Abstract
Objective
To examine whether polygenic susceptibility for body mass index (BMI) interacts with cumulative stress exposure, potentially exacerbating and buffering the effects of chronic stress, to predict obesity during childhood.
Methods
Data were analyzed from an established prospective puberty cohort in Anhui province, China. A total of 1000 children (421 boys and 579 girls, mean (standard deviation) age 8.97 (0.86) years) who had complete DNA genotyping, hair cortisol concentration and BMI were eligible for the study. The polygenic susceptibility score (PSS) was computed based on 11 SNPs derived from a published genome-wide association study for child obesity.
Results
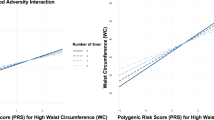
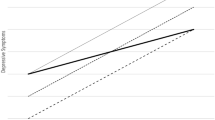
Children with different obesity polygenic susceptibility did not differ in BMI, obesogenic behaviors and HCC. The positive association between HCC with BMI was only found among children with highest PSS (r = 0.269, P < 0.001). When exposed in cumulative stress, children with highest PSS have higher BMI (β = 1.46, 95% CI: 0.63, 2.29; P = 0.001) than those having lowest PSS. The reverse pattern was found among children without cumulative stress exposure, those with highest PSS showed lowest BMI (β = −1.27, 95% CI: −2.17, −0.38; P = 0.001), compared to lowest PSS groups. Re-parameterized regression models provide strong support for the differential susceptibility hypothesis.
Conclusions
The findings underlie the importance of shifting perspectives from gene vulnerability to gene plasticity in the field of childhood obesity prevention. Children carrying additional BMI-raising alleles are at heightened risk of obesity are at heightened risk of obesity; however, they seem to be protected against obesity when the adverse psychosocial environment is removed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
NCD Risk Factor Collaboration (NCD-RisC). Worldwide trends in body-mass index, underweight, overweight, and obesity from 1975 to 2016: a pooled analysis of 2416 population-based measurement studies in 128.9 million children, adolescents, and adults. Lancet. 2017;390:2627–42.
Popkin BM, Slining MM. New dynamics in global obesity facing low- and middle-income countries. Obes Rev. 2013;14:11–20.
Global BMI Mortality Collaboration, Di Angelantonio E, Bhupathiraju ShN, Wormser D, et al. Body-mass index and all-cause mortality: individual-participant-data meta-analysis of 239 prospective studies in four continents. Lancet. 2016;388:776–86.
Quek YH, Tam WWS, Zhang MWB, Ho RCM. Exploring the association between childhood and adolescent obesity and depression: a meta-analysis. Obes Rev. 2017;18:742–54.
Singh AS, Mulder C, Twisk JW, van Mechelen W, Chinapaw MJ. Tracking of childhood overweight into adulthood: a systematic review of the literature. Obes Rev. 2008;9:474–88.
Goodarzi MO. Genetics of obesity: what genetic association studies have taught us about the biology of obesity and its complications. Lancet Diabetes Endocrinol. 2017;6:223–36.
Hesketh T, Zhen Y, Lu L, Dong ZX, Jun YX, Xing ZW. Stress and psychosomatic symptoms in Chinese school children: cross-sectional survey. Arch Dis Child. 2010;95:136–40.
Siervo M, Wells JC, Cizza G. The contribution of psychosocial stress to the obesity epidemic: an evolutionary approach. Horm Metab Res. 2009;41:261–70.
Razzoli M, Bartolomucci A. The dichotomous effect of chronic stress on obesity. Trends Endocrinol Metab. 2016;27:504–15.
Singh A, Babyak MA, Nolan DK, Brummett BH, Jiang R, Siegler IC, et al. Gene by stress genome-wide interaction analysis and path analysis identify EBF1 as a cardiovascular and metabolic risk gene. Eur J Hum Genet. 2015;23:854–62.
Singh A, Babyak MA, Brummett BH, Jiang R, Watkins LL, Barefoot JC, et al. Computing a synthetic chronic psychosocial stress measurement in multiple datasets and its application in the replication of G×E interactions of the EBF1 gene. Genet Epidemiol. 2015;39:489–97.
Belsky J. Theory testing, effect-size evaluation, and differential susceptibility to rearing influence: the case of mothering and attachment. Child Dev. 1997;8:598–600.
Ellis BJ, Boyce WT. Differential susceptibility to the environment: toward an understanding of sensitivity to developmental experiences and context. Dev Psychopathol. 2011;23:1–5.
Belsky J, Hartman S. Gene-environment interaction in evolutionary perspective: differential susceptibility to environmental influences. World Psychiatry. 2014;13:87–89.
Fox E, Beevers CG. Differential sensitivity to the environment: contribution of cognitive biases and genes to psychological wellbeing. Mol Psychiatry. 2016;21:1657–62.
Silveira PP, Gaudreau H, Atkinson L, Fleming AS, Sokolowski MB, Steiner M, et al. Genetic differential susceptibility to socioeconomic status and childhood obesogenic behavior: why targeted prevention may be the best societal investment. JAMA Pediatr. 2016;170:359–64.
Sullivan PF, Daly MJ, O’Donovan M. Genetic architectures of psychiatric disorders: the emerging picture and its implications. Nat Rev Genet. 2012;13:537–51.
International Schizophrenia Consortium, Purcell SM, Wray NR, Stone JL, et al. Common polygenic variation contributes to risk of schizophrenia and bipolar disorder. Nature. 2009;460:748–52.
Khera AV, Emdin CA, Drake I, Natarajan P, Bick AG, Cook NR, et al. Genetic risk, adherence to a healthy lifestyle, and coronary disease. N Engl J Med. 2016;375:2349–58.
Dalle Molle R, Fatemi H, Dagher A, Levitan RD, Silveira PP, Dubé L. Gene and environment interaction: is the differential susceptibility hypothesis relevant for obesity? Neurosci Biobehav Rev. 2017;73:326–39.
Levitan RD, Jansen P, Wendland B, Tiemeier H, Jaddoe VW, Silveira PP, et al. A DRD4 gene by maternal sensitivity interaction predicts risk for overweight or obesity in two independent cohorts of preschool children. J Child Psychol Psychiatry. 2017;58:180–8.
Belsky J, Beaver KM. Cumulative-genetic plasticity, parenting and adolescent self-regulation. J Child Psychol Psychiatry. 2011;52:619–26.
Raul JS, Cirimele V, Ludes B, Kintz P. Detection of physiological concentrations of cortisol and cortisone in human hair. Clin Biochem. 2004;37:1105–11.
Felix JF, Bradfield JP, Monnereau C, van der Valk RJ, Stergiakouli E, Chesi A, et al. Genome-wide association analysis identifies three new susceptibility loci for childhood body mass index. Hum Mol Genet. 2016;25:389–403.
Belsky DW, Moffitt TE, Caspi A. Genetics in population health science: strategies and opportunities. Am J Public Health. 2013;103:S73–S83.
Veldhorst MA, Noppe G, Jongejan MH, Kok CB, Mekic S, Koper JW, et al. Increased scalp hair cortisol concentrations in obese children. J Clin Endocrinol Metab. 2014;99:285–90.
Li H, Zong XN, Ji CY, Mi J. Body mass index cut-offs for overweight and obesity in Chinese children and adolescents aged 2–18 years. Zhonghua Liu Xing Bing Xue Za Zhi. 2010;31:616–20.
Ma J, McKeown NM, Hwang SJ, Hoffmann U, Jacques PF, Fox CS. Sugar-sweetened beverage consumption is associated with change of visceral adipose tissue over 6 years of follow-up. Circulation. 2016;133:370–7.
Belsky J, Pluess M, Widaman KF. Confirmatory and competitive evaluation of alternative gene-environment interaction hypotheses. J Child Psychol Psychiatry. 2013;54:1135–43.
Widaman KF, Helm JL, Castro-Schilo L, Pluess M, Stallings MC, Belsky J. Distinguishing ordinal and disordinal interactions. Psychol Methods. 2012;17:615–22.
Hemmingsson E. A new model of the role of psychological and emotional distress in promoting obesity: conceptual review with implications for treatment and prevention. Obes Rev. 2014;15:769–79.
Mitchell C, Hobcraft J, McLanahan SS, Siegel SR, Berg A, Brooks-Gunn J, et al. Social disadvantage, genetic sensitivity, and children’s telomere length. Proc Natl Acad Sci USA. 2014;111:5944–9.
Loos RJ. Genetic determinants of common obesity and their value in prediction. Best Pract Res Clin Endocrinol Metab. 2012;26:211–26.
Park S, Daily JW, Zhang X, Jin HS, Lee HJ, Lee YH. Interactions with the MC4R rs17782313 variant, mental stress and energy intake and the risk of obesity in Genome Epidemiology Study. Nutr Metab. 2016;13:38.
Acknowledgements
We acknowledge funding from the National Natural Science Foundation of China (81673188 for YS), Key Project of Natural Science Foundation of Anhui Education (KJ2016A338 for YS).
Author contributions
Study concept and design: YS, FT. Acquisition, analysis, or interpretation of data: YS, JF, YW, JH, YX, FT. DNA genotype: JF. Hair cortisol extraction: YX, JH. Drafting of the manuscript: Sun. Critical revision of the manuscript for important intellectual content: YS, FT. Statistical analysis: YS, JF. Study supervision: FT.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Sun, Y., Fang, J., Wan, Y. et al. Polygenic differential susceptibility to cumulative stress exposure and childhood obesity. Int J Obes 42, 1177–1184 (2018). https://doi.org/10.1038/s41366-018-0116-z
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-018-0116-z
This article is cited by
-
Interaction effects of cumulative genetic score and psychological distress on excessive gaming: A 2-year longitudinal study
Current Psychology (2024)
-
The weight of childhood adversity: evidence that childhood adversity moderates the impact of genetic risk on waist circumference in adulthood
International Journal of Obesity (2022)