Abstract
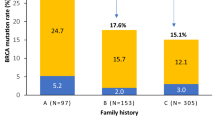
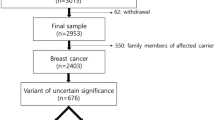
BRCA1/2 pathogenic variant prevalence in Japanese breast cancer is unclear. Here, we analyzed BRCA1/2 pathogenic variant prevalence with a particular focus on age factors, using the Japanese HBOC consortium database. All registered subjects were Japanese individuals who underwent BRCA1/2 genetic testing from January 1996 to July 2017 according to the Japanese HBOC consortium database. Cases were extracted and analyzed for each evaluation item. Overall BRCA1 and BRCA2 pathogenic variant prevalence was 11.2% and 9.0% in the cohort of 2366 proband patients, respectively. The age at onset of breast cancer for patients with BRCA1/2 pathogenic variants was significantly lower than that for patients without a BRCA1/2 pathogenic variant. In both BRCA1/2 patients, ages at onset were not statistically significantly different between two subtype groups (ER-positive vs. TNBC). We analyzed the BRCA1/2 pathogenic variant prevalence among age groups in patients with no family history of breast or ovarian cancer. In the TNBC group, the rate of genetic variants was more frequent among younger patients. Our results demonstrated that early breast cancer onset is associated with a BRCA1/2 pathogenic variant in the Japanese population. Younger TNBC patients were more likely to have a BRCA1/2 pathogenic variant irrespective of a family history of breast or ovarian cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Breast Cancer Risk and Prevention. https://www.cancer.org/cancer/breast-cancer/risk-and-prevention.html. 2020.
Valencia OM, Samuel SE, Viscusi RK, Riall TS, Neumayer LA, Aziz H. The role of genetic testing in patients with breast cancer: a review. JAMA Surg. 2017;152:589–94.
Bradbury AR, Olopade OI. Genetic susceptibility to breast cancer. Rev Endocr Metab Disord. 2007;8:255–67.
SEER Stat Fact Sheets. Female Breast Cancer. https://seer.cancer.gov/statfacts/html/breast.html. 2015–2017.
National Cancer Center Japan. https://ganjoho.jp/reg_stat/statistics/stat/summary.html. (2017).
Antoniou AC, Cunningham AP, Peto J, Evans DG, Lalloo F, Narod SA, et al. The BOADICEA model of genetic susceptibility to breast and ovarian cancers: updates and extensions. Br J Cancer. 2008;98:1457–66.
Antoniou A, Pharoah PD, Narod S, Risch HA, Eyfjord JE, Hopper JL, et al. Average risks of breast and ovarian cancer associated with BRCA1 or BRCA2 mutations detected in case Series unselected for family history: a combined analysis of 22 studies. Am J Hum Genet. 2003;72:1117–30.
Begg CB, Haile RW, Borg A, Malone KE, Concannon P, Thomas DC, et al. Variation of breast cancer risk among BRCA1/2 carriers. JAMA. 2008;299:194–201.
Brohet RM, Velthuizen ME, Hogervorst FB, Meijers-Heijboer HE, Seynaeve C, Collée MJ, et al. Breast and ovarian cancer risks in a large series of clinically ascertained families with a high proportion of BRCA1 and BRCA2 Dutch founder mutations. J Med Genet. 2014;51:98–107.
Chen S, Iversen ES, Friebel T, Finkelstein D, Weber BL, Eisen A, et al. Characterization of BRCA1 and BRCA2 mutations in a large United States sample. J Clin Oncol. 2006;24:863–71.
Evans DG, Shenton A, Woodward E, Lalloo F, Howell A, Maher ER. Penetrance estimates for BRCA1 and BRCA2 based on genetic testing in a Clinical Cancer Genetics service setting: risks of breast/ovarian cancer quoted should reflect the cancer burden in the family. BMC Cancer. 2008;8:155.
Ford D, Easton DF, Stratton M, Narod S, Goldgar D, Devilee P, et al. Genetic heterogeneity and penetrance analysis of the BRCA1 and BRCA2 genes in breast cancer families. The Breast Cancer Linkage Consortium. Am J Hum Genet. 1998;62:676–89.
Gabai-Kapara E, Lahad A, Kaufman B, Friedman E, Segev S, Renbaum P, et al. Population-based screening for breast and ovarian cancer risk due to BRCA1 and BRCA2. Proc Natl Acad Sci USA. 2014;111:14205–10.
Kuchenbaecker KB, Hopper JL, Barnes DR, Phillips KA, Mooij TM, Roos-Blom MJ, et al. Risks of breast, ovarian, and contralateral breast cancer for BRCA1 and BRCA2 mutation carriers. JAMA. 2017;317:2402–16.
Arai M, Yokoyama S, Watanabe C, Yoshida R, Kita M, Okawa M, et al. Genetic and clinical characteristics in Japanese hereditary breast and ovarian cancer: first report after establishment of HBOC registration system in Japan. J Hum Genet. 2018;63:447–57.
Lynch HT, Lynch PM. The cancer-family syndrome: a pragmatic basis for syndrome identification. Dis Colon Rectum. 1979;22:106–10.
Vasen HF, Mecklin JP, Khan PM, Lynch HT. The International Collaborative Group on Hereditary Non-Polyposis Colorectal Cancer (ICG-HNPCC). Dis Colon Rectum. 1991;34:424–5.
Nomizu T, Abe R, Tsuchiya A, Utsunomiya J, Watanabe F, Yamaki Y, editors. A clinical study of familial cancer in Japan. Berlin, Heidelberg: Springer Berlin Heidelberg; 1992.
Nomizu T, Tsuchiya A, Kanno M, Katagata N, Watanabe F, Yamaki Y, et al. Clinicopathological features of hereditary breast cancer. Breast Cancer (Tokyo, Jpn). 1997;4:239–42.
Foulkes WD, Brunet JS, Stefansson IM, Straume O, Chappuis PO, Begin LR, et al. The prognostic implication of the basal-like (cyclin E high/p27 low/p53+/glomeruloid-microvascular-proliferation+) phenotype of BRCA1-related breast cancer. Cancer Res. 2004;64:830–5.
Nicoletto MO, Donach M, De Nicolo A, Artioli G, Banna G, Monfardini S. BRCA-1 and BRCA-2 mutations as prognostic factors in clinical practice and genetic counselling. Cancer Treat Rev. 2001;27:295–304.
Chen H, Wu J, Zhang Z, Tang Y, Li X, Liu S, et al. Association between BRCA status and triple-negative breast cancer: a meta-analysis. Front Pharmacol. 2018;9:909.
Sugano K, Nakamura S, Ando J, Takayama S, Kamata H, Sekiguchi I, et al. Cross-sectional analysis of germline BRCA1 and BRCA2 mutations in Japanese patients suspected to have hereditary breast/ovarian cancer. Cancer Sci. 2008;99:1967–76.
Frank TS, Deffenbaugh AM, Reid JE, Hulick M, Ward BE, Lingenfelter B, et al. Clinical characteristics of individuals with germline mutations in BRCA1 and BRCA2: analysis of 10,000 individuals. J Clin Oncol. 2002;20:1480–90.
Couch FJ, Hart SN, Sharma P, Toland AE, Wang X, Miron P, et al. Inherited mutations in 17 breast cancer susceptibility genes among a large triple-negative breast cancer cohort unselected for family history of breast cancer. J Clin Oncol. 2015;33:304–11.
Hall MJ, Reid JE, Burbidge LA, Pruss D, Deffenbaugh AM, Frye C, et al. BRCA1 and BRCA2 mutations in women of different ethnicities undergoing testing for hereditary breast-ovarian cancer. Cancer. 2009;115:2222–33.
Weitzel JN, Clague J, Martir-Negron A, Ogaz R, Herzog J, Ricker C, et al. Prevalence and type of BRCA mutations in Hispanics undergoing genetic cancer risk assessment in the southwestern United States: a report from the Clinical Cancer Genetics Community Research Network. J Clin Oncol. 2013;31:210–6.
Palomba G, Budroni M, Olmeo N, Atzori F, Ionta MT, Pisano M, et al. Triple-negative breast cancer frequency and type of BRCA mutation: clues from Sardinia. Oncol Lett. 2014;7:948–52.
Ghadirian P, Robidoux A, Nassif E, Martin G, Potvin C, Patocskai E, et al. Screening for BRCA1 and BRCA2 mutations among French-Canadian breast cancer cases attending an outpatient clinic in Montreal. Clin Genet. 2014;85:31–5.
Tung N, Battelli C, Allen B, Kaldate R, Bhatnagar S, Bowles K, et al. Frequency of mutations in individuals with breast cancer referred for BRCA1 and BRCA2 testing using next-generation sequencing with a 25-gene panel. Cancer. 2015;121:25–33.
Kang E, Seong MW, Park SK, Lee JW, Lee J, Kim LS, et al. The prevalence and spectrum of BRCA1 and BRCA2 mutations in Korean population: recent update of the Korean Hereditary Breast Cancer (KOHBRA) study. Breast Cancer Res Treat. 2015;151:157–68.
Kast K, Rhiem K, Wappenschmidt B, Hahnen E, Hauke J, Bluemcke B, et al. Prevalence of BRCA1/2 germline mutations in 21401 families with breast and ovarian cancer. J Med Genet. 2016;53:465–71.
Susswein LR, Marshall ML, Nusbaum R, Vogel Postula KJ, Weissman SM, Yackowski L, et al. Pathogenic and likely pathogenic variant prevalence among the first 10,000 patients referred for next-generation cancer panel testing. Genet Med. 2016;18:823–32.
Buys SS, Sandbach JF, Gammon A, Patel G, Kidd J, Brown KL, et al. A study of over 35,000 women with breast cancer tested with a 25-gene panel of hereditary cancer genes. Cancer. 2017;123:1721–30.
Wen WX, Allen J, Lai KN, Mariapun S, Hasan SN, Ng PS, et al. Inherited mutations in BRCA1 and BRCA2 in an unselected multiethnic cohort of Asian patients with breast cancer and healthy controls from Malaysia. J Med Genet. 2018;55:97–103.
Momozawa Y, Iwasaki Y, Parsons MT, Kamatani Y, Takahashi A, Tamura C, et al. Germline pathogenic variants of 11 breast cancer genes in 7,051 Japanese patients and 11,241 controls. Nat Commun. 2018;9:4083.
Kemp Z, Turnbull A, Yost S, Seal S, Mahamdallie S, Poyastro-Pearson E, et al. Evaluation of cancer-based criteria for use in mainstream BRCA1 and BRCA2 genetic testing in patients with breast cancer. JAMA Netw Open. 2019;2:e194428.
Center for Cancer Control and Information Services NCC. Cancer Statistics in Japan ‘17. 2017. https://ganjoho.jp/data/reg_stat/statistics/brochure/2017/cancer_statistics_2017.pdf.
NCCN Clinical Practice Guidelines in Oncology (NCCN Guidelines). Genetic/familial high-risk assessment: breast and ovarian Version 1.2020. 2019.
Kurian AW. BRCA1 and BRCA2 mutations across race and ethnicity: distribution and clinical implications. Curr Opin Obstet Gynecol. 2010;22:72–8.
Armstrong N, Ryder S, Forbes C, Ross J, Quek RG. A systematic review of the international prevalence of BRCA mutation in breast cancer. Clin Epidemiol. 2019;11:543–61.
Tung N, Lin NU, Kidd J, Allen BA, Singh N, Wenstrup RJ, et al. Frequency of germline mutations in 25 cancer susceptibility genes in a sequential series of patients with breast cancer. J Clin Oncol. 2016;34:1460–8.
Atchley DP, Albarracin CT, Lopez A, Valero V, Amos CI, Gonzalez-Angulo AM, et al. Clinical and pathologic characteristics of patients with BRCA-positive and BRCA-negative breast cancer. J Clin Oncol. 2008;26:4282–8.
Honrado E, Benitez J, Palacios J. The molecular pathology of hereditary breast cancer: genetic testing and therapeutic implications. Mod Pathol. 2005;18:1305–20.
Musolino A, Bella MA, Bortesi B, Michiara M, Naldi N, Zanelli P, et al. BRCA mutations, molecular markers, and clinical variables in early-onset breast cancer: a population-based study. Breast. 2007;16:280–92.
Song Y, Barry WT, Seah DS, Tung NM, Garber JE, Lin NU. Patterns of recurrence and metastasis in BRCA1/BRCA2-associated breast cancers. Cancer. 2020;126:271–80.
Wong ES, Shekar S, Chan CH, Hong LZ, Poon SY, Silla T, et al. Predictive Factors for BRCA1 and BRCA2 genetic testing in an Asian clinic-based population. PLoS ONE. 2015;10:e0134408.
Engel C, Rhiem K, Hahnen E, Loibl S, Weber KE, Seiler S, et al. Prevalence of pathogenic BRCA1/2 germline mutations among 802 women with unilateral triple-negative breast cancer without family cancer history. BMC Cancer. 2018;18:265.
Robson M, Im SA, Senkus E, Xu B, Domchek SM, Masuda N, et al. Olaparib for metastatic breast cancer in patients with a germline BRCA mutation. N Engl J Med. 2017;377:523–33.
Chen S, Parmigiani G. Meta-analysis of BRCA1 and BRCA2 penetrance. J Clin Oncol. 2007;25:1329–33.
Acknowledgements
Registration Committee, Japanese HBOC Consortium [Committee]: Seigo Nakamura (Showa University), Takayuki Enomoto (Niigata University), Tadashi Nomizu (Hoshi General Hospital), Akihiro Sakurai (Sapporo Medical University), Masayuki Sekine (Niigata University), Hiroyuki Nomura (Fujita Medical University), Megumi Ohkawa (St. Luke’s International Hospital), Junko Yotsumoto (International University of Health and Welfare), [Data center] Chie Watanabe (Sophia University), [Office] Shiro Yokoyama (Showa University). Participating Facilities of Nationwide registration projects: Showa Medical University Hospital, St. Lukes Hospital, Cancer Institute Hospital, Hoshi General Hospital, Shikoku Cancer Center, Hokkaido Cancer Center, Sapporo Medical Center, Niigata University Faculty of Medicine, Keio University, Kitano Hospital, Kochi University Faculty of Medicine, Tawara IVF Clinic, Kochi Medical Center, Nagoya University Hospital, St. Marianna University School of Medicine, Asahikawa Medical University, Aichi Cancer Center Hospital, Saku Medical Center, Tsukuba Medical University Hospital, Yokohama City University Hospital, Fujita Medical University Hospital, Ehime University Hospital, Gunma Prefectural Cancer Center, Nagasaki University Hospital, Shinshu University Hospital, Juntendo University Hospital, Kitazato University Hospital, Aichi Cancer Center Aichi Hospital, Okayama University Hospital, Saitama Medical University International Medical Center, Tokyo Medical Center, Tokyo Metropolitan Komagome Hospital, Japanese Red Cross Ishinomaki Hospital, Nagoya City University Hospital, Kawasaki Medical School Hospital, Yamanashi Prefectural Central Hospital, Nara Medical University Hospital, Kanagawa Cancer Center, Shiga Medical University, Shizuoka Cancer Center, Gifu University Hospital, Hiroshima Prefectural Hospital, Niigata Cancer Center Hospital, Japanese Red Cross Nagoya Daiichi Hospital, Tottori University Hospital, Kansai Rosai Hospital, Kokura Medical Center, Nippon Medical School Musashi Kosugi Hospital, Kansai Medical University Hospital, Sagara Hospital Breast Center, Chiba University Hospital, Ibaraki Prefectural Hospital, Fukui University Hospital, Hokkaido University Hospital, Saitama Medical Center, Osaka University, Japanese Red Cross Yamaguchi Hospital, Kyoto University Hospital, Konan Kosei Hospital, Japanese Red Cross Medical Center, Shonan Memorial Hospital, Shizuoka General Hospital, Hiroshima University Hospital, National Hospital Organization Kyoto Medical Center, Shiroyama Hospital, Saitama Cancer Center, National Hospital Organization Osaka National Hospital, Kitakyushu Municipal Medical Center, Iwate Medical University, and Tokuyama Central Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Okano, M., Nomizu, T., Tachibana, K. et al. The relationship between BRCA-associated breast cancer and age factors: an analysis of the Japanese HBOC consortium database. J Hum Genet 66, 307–314 (2021). https://doi.org/10.1038/s10038-020-00849-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s10038-020-00849-y
This article is cited by
-
The Japanese Breast Cancer Society clinical practice guidelines for epidemiology and prevention of breast cancer, 2022 edition
Breast Cancer (2024)
-
A transcriptional response to replication stress selectively expands a subset of Brca2-mutant mammary epithelial cells
Nature Communications (2023)
-
A Japanese case of ovarian mucinous adenocarcinoma with germline double variants of MSH2 and BRCA2
Journal of Human Genetics (2023)
-
Clinical risk management of breast, ovarian, pancreatic, and prostatic cancers for BRCA1/2 variant carriers in Japan
Journal of Human Genetics (2023)
-
Promoters of BRCA testing under insurance coverage for non-metastatic breast cancer patients in Japan: a retrospective cohort study
Breast Cancer (2023)