Abstract
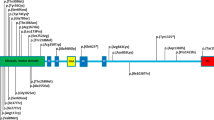
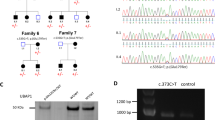
Hereditary spastic paraplegias (HSPs) are characterized by lower extremity spasticity and weakness. HSP is often caused by mutations in SPG genes, but it may also be produced by inborn errors of metabolism. We performed next-generation sequencing of 4813 genes in one adult twin pair with HSP and severe muscular weakness occurring at the same age. We found two pathogenic compound heterozygous variants in MTHFR, including a variant not referenced in international databases, c.197C>T (p.Pro66Leu) and a known variant, c.470G>A (p.Arg157Gln), and two heterozygous pathogenic variants in POLG, c.1760C>T (p.Pro587Leu) and c.752C>T (p.Thr251Ile). MTHFR and POLG mutations were consistent with the severe muscle weakness and the metabolic changes, including hyperhomocysteinemia and decreased activity of both N(5,10)methylenetetrahydrofolate reductase (MTHFR) and complexes I and II of the mitochondrial respiratory chain. These data suggest the potential role of MTHFR and POLG mutations through consequences on mitochondrial dysfunction in the occurrence of spastic paraparesis phenotype with combined metabolic, muscular, and neurological components.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Kara E, Tucci A, Manzoni C, Lynch DS, Elpidorou M, Bettencourt C, et al. Genetic and phenotypic characterization of complex hereditary spastic paraplegia. Brain. 2016;139:1904–18.
Hensiek A, Kirker S, Reid E. Diagnosis, investigation and management of hereditary spastic paraplegias in the era of next-generation sequencing. J Neurol. 2015;262:1601–12.
Sedel F, Fontaine B, Saudubray JM, Lyon-Caen O. Hereditary spastic paraparesis in adults associated with inborn errors of metabolism: a diagnostic approach. J Inherit Metab Dis. 2007;30:855–64.
Hedera P. Hereditary Spastic Paraplegia Overview. In: Adam MP, Ardinger HH, Pagon RA, Wallace SE, Bean LJH, editors. GeneReviews®. Seattle (WA): University of Washington, Seattle; 1993–2019.
Perna A, Masciullo M, Modoni A, Cellini E, Parrini E, Ricci E, et al. Severe 5,10-methylenetetrahydrofolate reductase deficiency: a rare, treatable cause of complicated hereditary spastic paraplegia. Eur J Neurol. 2018;25:602–5.
MacArthur DG, Manolio TA, Dimmock DP, Rehm HL, Shendure J, Abecasis GR, et al. Guidelines for investigating causality of sequence variants in human disease. Nature. 2014;508:469–76.
Singleton MV, Guthery SL, Voelkerding KV, Chen K, Kennedy B, Margraf RL, et al. Phevor combines multiple biomedical ontologies for accurate identification of disease-causing alleles in single individuals and small nuclear families. Am J Hum Genet. 2014;94:599–610.
Schwarz JM, Cooper DN, Schuelke M, Seelow D. MutationTaster2: mutation prediction for the deep-sequencing age. Nat Methods. 2014;11:361–2.
Shihab HA, Gough J, Cooper DN, Stenson PD, Barker GL, Edwards KJ, et al. Predicting the functional, molecular, and phenotypic consequences of amino acid substitutions using hidden Markov models. Hum Mutat. 2013;34:57–65.
Dong C, Wei P, Jian X, Gibbs R, Boerwinkle E, Wang K, et al. Comparison and integration of deleteriousness prediction methods for nonsynonymous SNVs in whole exome sequencing studies. Hum Mol Genet. 2015;24:2125–37.
Kumar P, Henikoff S, Ng PC. Predicting the effects of coding non-synonymous variants on protein function using the SIFT algorithm. Nat Protoc. 2009;4:1073–81.
Choi Y, Chan AP. PROVEAN web server: a tool to predict the functional effect of amino acid substitutions and indels. Bioinformatics. 2015;31:2745–7.
Quang D, Chen Y, Xie X. DANN: a deep learning approach for annotating the pathogenicity of genetic variants. Bioinformatics. 2015;31:761–3.
Richards S, Aziz N, Bale S, Bick D, Das S, Gastier-Foster J, et al. Standards and guidelines for the interpretation of sequence variants: a joint consensus recommendation of the American College of Medical Genetics and Genomics and the Association for Molecular Pathology. Genet Med. 2015;17:405–24.
Forges T, Chery C, Audonnet S, Feillet F, Gueant JL. Life-threatening methylenetetrahydrofolate reductase (MTHFR) deficiency with extremely early onset: characterization of two novel mutations in compound heterozygous patients. Mol Genet Metab. 2010;100:143–8.
Garcia MM, Gueant-Rodriguez RM, Pooya S, Brachet P, Alberto JM, Jeannesson E, et al. Methyl donor deficiency induces cardiomyopathy through altered methylation/acetylation of PGC-1alpha by PRMT1 and SIRT1. J Pathol. 2011;225:324–35.
Goyette P, Sumner JS, Milos R, Duncan AM, Rosenblatt DS, Matthews RG, et al. Human methylenetetrahydrofolate reductase: isolation of cDNA, mapping and mutation identification. Nat Genet. 1994;7:195–200.
Ferrari G, Lamantea E, Donati A, Filosto M, Briem E, Carrara F, et al. Infantile hepatocerebral syndromes associated with mutations in the mitochondrial DNA polymerase-gammaA. Brain. 2005;128:723–31.
Scuderi C, Borgione E, Castello F, Lo Giudice M, Santa Paola S, Giambirtone M, et al. The in cis T251I and P587L POLG1 base changes: description of a new family and literature review. Neuromuscul Disord. 2015;25:333–9.
Lek M, Karczewski KJ, Minikel EV, Samocha KE, Banks E, Fennell T, et al. Analysis of protein-coding genetic variation in 60,706 humans. Nature. 2016;536:285–91.
Haworth JC, Dilling LA, Surtees RA, Seargeant LE, Lue-Shing H, Cooper BA, et al. Symptomatic and asymptomatic methylenetetrahydrofolate reductase deficiency in two adult brothers. Am J Med Genet. 1993;45:572–6.
Bathgate D, Yu-Wai-Man P, Webb B, Taylor RW, Fowler B, Chinnery PF. Recessive spastic paraparesis associated with complex I deficiency due to MTHFR mutations. J Neurol Neurosurg Psychiatry. 2012;83:115.
Lossos A, Teltsh O, Milman T, Meiner V, Rozen R, Leclerc D, et al. Severe methylenetetrahydrofolate reductase deficiency: clinical clues to a potentially treatable cause of adult-onset hereditary spastic paraplegia. JAMA Neurol. 2014;71:901–4.
Lin N, Jiang N, Dai Y, Gao J, Wang L. Adult-onset severe methylenetetrahydrofolate reductase deficiency characterized by reversible spastic paraplegia with a novel mutation. Neurol Sci. 2016;37:1735–7.
Iida S, Nakamura M, Asayama S, Kunieda T, Kaneko S, Osaka H, et al. Rapidly progressive psychotic symptoms triggered by infection in a patient with methylenetetrahydrofolate reductase deficiency: a case report. BMC Neurol. 2017;17:47.
Gueant JL, Namour F, Gueant-Rodriguez RM, Daval JL. Folate and fetal programming: a play in epigenomics? Trends Endocrinol Metab. 2013;24:279–89.
Milone M, Massie R. Polymerase gamma 1 mutations: clinical correlations. Neurologist. 2010;16:84–91.
Van Goethem G, Schwartz M, Lofgren A, Dermaut B, Van Broeckhoven C, Vissing J. Novel POLG mutations in progressive external ophthalmoplegia mimicking mitochondrial neurogastrointestinal encephalomyopathy. Eur J Hum Genet. 2003;11:547–9.
DeBalsi KL, Longley MJ, Hoff KE, Copeland WC. Synergistic effects of the in cis T251I and P587L mitochondrial DNA polymerase gamma disease mutations. J Biol Chem. 2017;292:4198–209.
Milone M, Tang S, Sorenson E, Zhiyv N, Wong L-j. POLG-related disorders: muscle biopsy findings, mitochondrial DNA content and deletions (P07.206). Neurology. 2012;78:P07.206.
Hasselmann O, Blau N, Ramaekers VT, Quadros EV, Sequeira JM, Weissert M. Cerebral folate deficiency and CNS inflammatory markers in Alpers disease. Mol Genet Metab. 2010;99:58–61.
Froese DS, Huemer M, Suormala T, Burda P, Coelho D, Gueant JL, et al. Mutation update and review of severe methylenetetrahydrofolate reductase deficiency. Hum Mutat. 2016;37:427–38.
Acknowledgements
Institutional grants of INSERM UMR_S 1256 were received from INSERM (French National Institute of Health and Medical Research) and the Region of Lorraine (France). MRB is supported by the Swiss National Science Foundation (SNSF 31003A_138521) and the Rare Disease Initiative Zurich (radiz), a clinical research priority program for rare diseases of the University of Zurich, Switzerland.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Wiedemann, A., Chery, C., Coelho, D. et al. Mutations in MTHFR and POLG impaired activity of the mitochondrial respiratory chain in 46-year-old twins with spastic paraparesis. J Hum Genet 65, 91–98 (2020). https://doi.org/10.1038/s10038-019-0689-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s10038-019-0689-y
This article is cited by
-
Predictors of the utility of clinical exome sequencing as a first-tier genetic test in patients with Mendelian phenotypes: results from a referral center study on 603 consecutive cases
Human Genomics (2023)
-
Diagnostic yield of clinical exome sequencing as a first-tier genetic test for the diagnosis of genetic disorders in pediatric patients: results from a referral center study
Human Genetics (2022)
-
Expanding the clinical spectrum of STIP1 homology and U-box containing protein 1-associated ataxia
Journal of Neurology (2021)