Abstract
Ghrelin, an enteric hormone with potent appetite stimulating effects, also stimulates growth hormone release. We hypothesized that altered levels of total ghrelin (TG) or acylated ghrelin (AG) could affect growth by altering growth hormone secretion, subsequently affecting insulin-like growth factor-1 (IGF-1) generation or by altering appetite and food intake. After institutional review board approval, 52 children presenting for evaluation of chronic gastrointestinal symptoms (group 1), poor weight gain (group 2), or poor linear growth (group 3) were evaluated for fasting TG and AG levels in addition to their regular evaluation. Serum ghrelin, IGF-1, and prealbumin were compared between groups. No difference was observed for mean fasting TG between groups. However, mean fasting AG was highest in patients in group 2 (465 ± 128 pg/mL) versus group 1 (176 ± 37 pg/mL) and group 3 (190 ± 34 pg/mL). IGF-1 was lowest in patients in group 2 despite similar prealbumin levels among the three groups. We conclude that serum AG levels are highest in children with isolated poor weight gain compared with children with short stature or chronic gastrointestinal symptoms, suggesting the possibility of resistance to AG in underweight children. Additional studies are needed to further clarify ghrelin's role in growth and appetite.
Similar content being viewed by others
Main
Many children are referred to pediatric endocrinologists and gastroenterologists for evaluation of poor growth. There is often considerable overlap in the clinical presentation of patients given the diagnosis of “failure-to-thrive,” or “growth failure” with some patients presenting with poor linear growth, others with poor weight gain, and some with both. In addition, children with poor linear growth are often poor eaters and have gastrointestinal symptoms (1).
Extensive workup, including a broad panel of screening laboratories looking for the causes of poor growth, often fails to reveal an underlying diagnosis. Therefore, there has been considerable interest in finding a definable link between poor weight gain and poor linear growth. Ghrelin, a hormone that is not routinely measured in this clinical setting, could theoretically have a role in both poor growth and gastrointestinal disease.
Ghrelin is an enteric hormone with potent orexigenic and adipogenic effects, and it is also a potent stimulator of growth hormone release, mediated by the growth hormone secretagogue receptor (GHSR) type 1A (2). Ghrelin is produced predominately by the stomach and serves to stimulate appetite and regulate positive energy balance (2,3). In addition to serving as a potent stimulator of growth hormone release in synergy with growth hormone releasing hormone, ghrelin stimulates prolactin and adrenocorticotropic hormone (ACTH) secretion, modulates insulin secretion and sensitivity, and stimulates gastrointestinal tract motility (3).
Studies have reported a potential role for ghrelin in children with Helicobacter pylori infection, a gastrointestinal disease that has been associated with poor growth (4). Some studies have shown that tissue concentrations of ghrelin are decreased in the stomach in the presence of H. pylori infection, whereas others have shown that serum levels of acylated ghrelin (AG), the active form of the peptide, are decreased (5–7). Other studies dispute these findings (8). Of particular interest, there are several other gastrointestinal diseases in children that may present with poor growth as a presenting symptom, including celiac disease and inflammatory bowel disease. Many patients with these disorders have nonspecific symptoms such as abdominal pain, dyspepsia, or poor appetite (9). It is still unknown how ghrelin levels are altered in these disease states. Thus, the potential relationships between gastrointestinal disease, ghrelin, growth, and appetite are still unclear.
Underweight children have been found to have elevated ghrelin levels, but only one study has shown low height SD score (SDS) as an independent determinant of elevated AG levels in children with idiopathic short stature (10,11). Recently, in several patients, however, a missense mutation resulting in a complete loss of GHSR constitutive activity has been implicated in short stature with dominant transmission (12). A syndrome of recessive isolated growth hormone deficiency caused by mutations in the ghrelin receptor has also been reported (13).
We hypothesized that ghrelin could affect growth by two separate mechanisms: 1) by altering growth hormone secretion and subsequently affecting insulin-like growth factor (IGF)-1 generation or 2) by stimulating appetite and food intake. The goal of this study was to test the first part of this hypothesis by determining how total ghrelin (TG), AG, and IGF-1 levels are altered in children with short stature and/or poor weight gain. Therefore, we measured serum TG, AG, and IGF-1 levels to determine whether they are altered in children with these conditions. Currently, it is thought that AG is more important than TG as a marker of ghrelin activity (14).
METHODS
Patients and measurements.
All children who presented over a 6-mo period for their initial evaluation of isolated gastrointestinal symptoms, poor linear growth, or poor weight gain to the Tripler Army Medical Center pediatric endocrinology and pediatric gastroenterology clinics and who subsequently required additional fasting laboratory workup were evaluated for fasting serum TG and AG levels in addition to their standard of care workup. All ghrelin levels were drawn fasting at 0800 h. Children who presented for similar symptoms but who did not require additional laboratory workup or who did not require fasting laboratories were excluded.
Patients were divided into three groups according to their presenting symptoms: 1) isolated gastrointestinal symptoms without affects on growth or weight gain, 2) failure-to-thrive (predominantly poor weight gain), and 3) short stature (or proportionally small height and weight). Patients with chronic gastrointestinal symptoms, defined as symptoms of gastrointestinal disease for greater than 6 wk or recurrent symptoms but normal stature and growth, were included in group 1.
To be included in the failure-to-thrive group (group 2), subjects must have had poor weight gain, defined as weight less than −2 SD for gender and age or less than expected rate of weight gain for gender and age. To be included in the short stature group (group 3), subjects must have had short stature, defined as height less than −2 SD for gender and age or an abnormal growth velocity for gender and age.
Patients who were affected in both weight and height were stratified by which measurement was more severely affected, with poor weight gain being the primary problem in the failure-to-thrive grouping (group 2) and poor linear growth being the primary problem in the short stature group (group 3). Patients who were proportionally small, in that their height and weight were both affected to an equal degree, were included in group 3, as they were not underweight for their height percentile.
Routine data collected on all patients to rule out treatable causes of poor growth included IGF-1, thyroid-stimulating hormone (TSH), free thyroxine (FT4), complete blood count (CBC), chemistry, prealbumin, and celiac disease testing, which at our institution includes tissue transglutaminase IgA and total IgA. In addition, because H. pylori disease has been associated with poor growth and possibly lower ghrelin levels, H. pylori antibody was measured on all patients. Additional studies sent on each patient were determined by the patient's provider, including bone age or perceived need for further workup (karyotype for females, endoscopy, etc.).
The study protocol was approved by the institutional review board (IRB) at Tripler Army Medical Center. Written informed consent was obtained from legal guardians of children recruited into the study. Written assent was also obtained from all children older than 7 y as required by our IRB. Investigators adhered to the policies for protection of human subjects as prescribed in 45 CFR 46.
Hormonal assays.
TG and AG levels in patient serum were determined via commercial kits using RIA (catalog numbers GHRT-89HK and GHRA-88HK, respectively; Linco Research, St. Charles, MO) using a standard curve of known concentration of purified 125I-labeled ghrelin peptide. Intra- and interassay coefficients of variation reported by the manufacturer were 4.4–10% and 14.7–16.7% for TG, respectively, and 6.5–9.5% and 9.6–16.2% for AG, respectively (for conversion to SI units: pg/mL × 3.371 = pmol/L for active ghrelin; pg/mL × 3.189 for des-AG − total ghrelin measures both AG and des-AG). IGF-1 serum levels were determined by immunochemiluminometric assay at Quest Diagnostics Nichols Institute (San Juan Capistrano, CA). Serum prealbumin levels were run at the Tripler Army Medical Center main laboratory by immunoturbidimetric assay. The remainder of the routine screening tests was run in the Tripler Army Medical Center main laboratory.
Statistical analysis.
Based on a previous study, it is assumed that the normative mean for ghrelin in Tanner I subjects will be 900 pg/mL with a SD of 200 pg/mL (15). It is also assumed that the SD of ghrelin levels within the three patient groups could be as high as 300 pg/mL. Controlling for the probability of a type I error at α = 0.05, analysis showed that up to 20 subjects in each group could be needed to give a power of 80% to detect a difference in ghrelin levels between one of the study groups and the normative value.
The primary outcome variables were measurements of TG and AG in each of the three groups. Serum ghrelin levels were compared between groups by Kruskal–Wallis nonparametric, one-way ANOVA, comparing all three groups as a whole. Comparison between individual groups to determine specific differences between groups 1 and 2, 1 and 3, and 2 and 3 was completed using a t test.
In addition, age-, race-, and gender-adjusted height, weight, and BMI z-scores were calculated for each patient in the study using the formula from the National Health and Nutrition Examination Survey. Comparison of height, weight, and BMI SDS to ghrelin levels was performed to determine whether they were independently associated with ghrelin levels.
Additional analysis was performed to determine whether there was a difference in IGF-1 and prealbumin levels among the three groups. Finally, subgroup analysis of ghrelin levels was performed to compare patients who were eventually given an underlying diagnosis. All data are reported as the mean ± SEM.
RESULTS
Fifty-two patients were recruited into the study. Eleven had chronic gastrointestinal symptoms without growth issues (group 1). Eight patients had poor weight gain (failure-to-thrive), with weight significantly more affected than height (group 2). Thirty-three patients had short stature, with height being more affected than weight or were proportionally small, with height and weight at similar percentiles (group 3). Except for two patients in group 1 and one in group 3, all patients were prepubertal. Demographic data for all patients, including mean height and weight SDS scores for each group, is summarized in Table 1.
No difference was observed for mean fasting TG levels between groups 1, 2, and 3 (1157 ± 105 pg/mL, 1264 ± 245 pg/mL and 1063 ± 77 pg/mL, respectively, p = 0.217). These values are similar to those reported by Soriano-Guillén et al. (894 ± 26 pg/mL) for Tanner I normal children (15).
However, mean fasting AG levels were significantly different for the three groups by ANOVA, with higher levels found in patients who had primarily poor weight gain (group 2, 465 ± 128 pg/mL), versus those with isolated gastrointestinal symptoms (group 1, 176 ± 37 pg/mL) and those with short stature (group 3, 190 ± 34 pg/mL; p = 0.021). Comparison between specific groups using t test confirmed a difference in mean AG levels only between groups 1 and 2 (p = 0.023) and groups 2 and 3 (p = 0.003) but not between groups 1 and 3. TG and AG values for all three groups are displayed in Figs. 1 and 2.
Prealbumin levels were 19.6 ± 1.6 mg/dL, 23.3 ± 1.5 mg/dL, and 21.8 ± 1.5 mg/dL for groups 1, 2, and 3, respectively. Comparison among the three groups (1 versus 2, 1 versus 3, and 2 versus 3) showed no difference (p = 0.14, p = 0.37, and p = 0.63, respectively). A comparison of all three groups is displayed in Fig. 3.
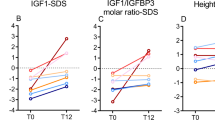
IGF-1 levels were significantly lower in patients with poor weight gain (group 2, 51.9 ± 10.4 ng/mL) versus the short stature group (group 3, 122.9 ± 15.2 ng/mL, p = 0.02), as shown in Fig. 4. However, all groups had normal range IGF-1 when adjusted for the mean age of their group. Comparison of height, weight, and BMI z-scores to TG and AG levels showed no correlation based on linear regression analysis.
Subgroup analysis was performed to compare ghrelin levels based on the eventual underlying diagnosis given to each patient. For diagnoses with a sufficient number of patients for analysis (growth hormone deficiency and idiopathic short stature), comparison of these patients with the means for their group showed no differences in mean TG or AG levels. Results from all patients given an underlying diagnosis are summarized in Table 2.
DISCUSSION
Ghrelin, the natural ligand of the GHSR type 1A, was first discovered in 1999 (16). In addition to being a potent stimulator of growth hormone release, premeal increases of circulating ghrelin suggest ghrelin plays a role as a hunger signal. AG triggers meal initiation, increasing food intake and activating brain appetite centers by acting mainly on the arcuate nucleus, stimulating neuropeptide Y and agouti-related protein neurons expressing the GHSR type 1A (17–20). Thus, ghrelin may not only have a role in triggering growth hormone release but could also contribute to positive energy balance by increasing appetite and that these effects, together or separately, could affect growth and weight gain.
Our clinical dilemma is that there is often much overlap in the clinical entities of poor weight gain, short stature, and normal variants of growth. Herein, we describe patients with poor weight gain as their presenting complaint as failure-to-thrive, recognizing that many of these patients eventually have linear growth affected should they continue to gain weight poorly for prolonged periods of time. In addition, idiopathic short stature likely represents a combination of genetic and environmental factors, with many children growing poorly also having a history of poor appetite and being “picky eaters” (1,21). Depending on the primary concern of the parents and referring provider, patients may present for evaluation for one or all of these symptoms, creating a complex clinical dilemma. Ghrelin has the potential to link these diagnoses together, as alterations in circulating ghrelin levels could be hypothesized to affect appetite, linear growth, or both in this population of patients.
Our results show that TG levels do not differ in patients with poor linear growth, poor weight gain, or isolated gastrointestinal symptoms. This result is not surprising in that much of the growth hormone releasing and other endocrine actions of ghrelin are thought to be due to its acylated form (14,20).
We found that serum AG levels were significantly higher in patients with predominantly poor weight gain than in patients with poor linear growth. Previous studies have shown that circulating AG levels are increased by fasting and energy restriction and decreased by food intake (22). Circulating ghrelin levels are also increased in adults with anorexia and cachexia, suggesting ghrelin secretion is up-regulated under conditions of negative energy balance (23). This finding has been postulated to represent a compensatory response to poor caloric intake and may reflect a ghrelin-resistance syndrome in cachexia (24). Our data show that despite often having symptoms of poor appetite and poor eating, children with poor weight gain have elevated fasting AG, reflecting a state of negative energy balance consistent with findings in cachectic adults.
As shown in one other study of children with idiopathic short stature (11), we found that children with elevated AG levels had the lowest IGF-1 levels (Fig. 4). However, other studies of children with idiopathic short stature and growth hormone deficiency have failed to show any relation between IGF-1 and ghrelin levels (25). In our study, despite similar prealbumin levels among the three groups (Fig. 3), we believe that it would be premature to conclude that poor nutrition was not the underlying cause for the lower IGF-1 levels found in the poor weight gain grouping for a number of reasons. First, when adjusted for the mean age of the group, the mean IGF-1 in group 2 was at the lower end of normal, although a wide range for IGF-1 is seen at this age. We also studied only a small number of patients who were primarily underweight, many of whom also had poor linear growth. In addition, our patient population was not homogeneous and included patients with a number of different diagnoses. As our study was not designed to measure appetite and feeding behavior, we cannot distinguish among these or other possible explanations for how nutritional status may have affected IGF-1 and overall energy balance. Thus, the relationship between ghrelin and IGF-1 is still unclear.
Our data showed that height, weight, and BMI z-scores did not correlate with ghrelin levels, suggesting that there are clinically important differences in the presentation of the proportionally short and thin child versus a child who is only underweight. In fact, eight of the 33 patients in the short stature group (group 3) were found to have growth hormone deficiency based on growth hormone stimulation testing and/or MRI findings. Many of these patients were also underweight, but their mean AG levels were lower than the patients with isolated poor weight gain (Table 2).
Although previous studies have shown that exogenous administration of growth hormone secretagogues can increase 24 h growth hormone secretion (26), there is no convincing evidence to our knowledge that ghrelin is important for physiologic growth. Our study suggests that ghrelin levels do not correlate with linear growth and that elevated AG levels characterize isolated poor weight gain and not short stature in children. If the exact role of ghrelin in this and other conditions can be elucidated, ultimately there may be a role for ghrelin analogs in treating cachectic states, although circulating ghrelin levels are high in this situation. Animal studies have shown that exogenous ghrelin administration may be useful in restoring normal body weight (27,28). Limited data in humans treated with oral ghrelin mimetics show that growth hormone secretagogues can safely produce dose-related weight gain (29) and even increase hunger in anorexic patients, although not all patients with anorexia responded equally (30). If it can be proven that children with poor weight gain have resistance to ghrelin that can be overcome, then we may have identified a cohort for future consideration of treatment with growth hormone secretagogues.
We conclude that poor weight gain in children is characterized by elevated fasting levels of AG compared with children with short stature or chronic gastrointestinal symptoms. Additional studies of ghrelin in normal and abnormal children are needed to further clarify its potential role in growth and energy balance.
Abbreviations
- AG:
-
acylated ghrelin
- GHSR:
-
growth hormone secretagogue receptor
- SDS:
-
SD score
- TG:
-
total ghrelin
REFERENCES
Wudy SA, Hagemann S, Dempfle A, Ringler G, Blum WF, Berthold LD, Alzen G, Gortner L, Hebebrand J 2005 Children with idiopathic short stature are poor eaters and have decreased body mass index. Pediatrics 116: e52–e57
van der Lely AJ, Tschop M, Heiman ML, Ghigo E 2004 Biological, physiological, pathophysiological, and pharmacological aspects of ghrelin. Endocr Rev 25: 426–457
Muccioli G, Tschöp M, Papotti M, Deghenghi R, Heiman M, Ghigo E 2002 Neuroendocrine and peripheral activities of ghrelin: implications in metabolism and obesity. Eur J Pharmacol 440: 235–254
Patel P, Mendall MA, Khulusi S, Northfield TC, Strachan DP 1994 Helicobacter pylori infection in childhood: risk factors and effect on growth. BMJ 309: 1119–1123
Osawa H, Nakazato M, Date Y, Kita H, Ohnishi H, Ueno H, Shiiya T, Satoh K, Ishino Y, Sugano K 2005 Impaired production of gastric ghrelin in chronic gastritis associated with Helicobacter pylori. J Clin Endocrinol Metab 90: 10–16
Plonka M, Bielanski W, Konturek SJ, Targosz A, Sliwowski Z, Dobrzanska M, Kaminska A, Sito E, Konturek PC, Brzozowski T 2006 Helicobacter pylori infection and serum gastrin, ghrelin and leptin in children of Polish shepherds. Dig Liver Dis 38: 91–97
Isomoto H, Nakazato M, Ueno H, Date Y, Nishi Y, Mukae H, Mizuta Y, Ohtsuru A, Yamashita S, Kohno S 2004 Low plasma ghrelin levels in patients with Helicobacter pylori-associated gastritis. Am J Med 117: 429–432
Gokcel A, Gumurdulu Y, Kayaselcuk F, Serin E, Ozer B, Ozsahin AK, Guvener N 2003 Helicobacter pylori has no effect on plasma ghrelin levels. Eur J Endocrinol 148: 423–426
Salardi S, Cacciari E, Volta U, Santoni R, Ragni L, Elleri D, Cicognani A, Vaira D 2005 Growth and adult height in atypical coeliac patients, with or without growth hormone deficiency. J Pediatr Endocrinol Metab 18: 769–775
Tannenbaum GS, Ramsay M, Martel C, Samia M, Zygmuntowicz C, Porporino M, Ghosh S 2009 Elevated circulating acylated and total ghrelin concentrations along with reduced appetite scores in infants with failure to thrive. Pediatr Res 65: 569–573
Camurdan MO, Bideci A, Demirel F, Cinaz P 2006 Serum ghrelin, IGF-1 and IGF-BP3 levels in children with normal variant short stature. Endocr J 53: 479–484
Pantel J, Legendre M, Cabrol S, Hilal L, Hajaji Y, Morisset S, Nivot S, Vie-Luton MP, Grouselle D, de Kerdanet M, Kadiri A, Epelbaum J, Le Bouc Y, Amselem S 2006 Loss of constitutive activity of the growth hormone secretagogue receptor in familial short stature. J Clin Invest 116: 760–768
Pantel J, Legendre M, Nivot S, Morisset S, Vie-Luton MP, le Bouc Y, Epelbaum J, Amselem S 2009 Recessive isolated growth hormone deficiency and mutations in the ghrelin receptor. J Clin Endocrinol Metab 94: 4334–4341
Fehrentz JA, Martinez J, Boeglin D, Guerlavais V, Deghenghi R 2002 Growth hormone secretagogues: past, present and future. IDrugs 5: 804–814
Soriano-Guillén L, Barrios V, Chowen JA, Sánchez I, Vila S, Quero J, Argente J 2004 Ghrelin levels from fetal life through early adulthood: relationship with endocrine and metabolic and anthropometric measures. J Pediatr 144: 30–35
Kojima M, Hosoda H, Date Y, Nakazato M, Matsuo H, Kangawa K 1999 Ghrelin is a growth-hormone-releasing acylated peptide from stomach. Nature 402: 656–660
Cummings DE, Purnell JQ, Frayo RS, Schmidova K, Wisse BE, Weigle DS 2001 A preprandial rise in plasma ghrelin levels suggests a role in meal initiation in humans. Diabetes 50: 1714–1719
Wren AM, Seal LJ, Cohen MA, Brynes AE, Frost GS, Murphy KG, Dhillo WS, Ghatei MA, Bloom SR 2001 Ghrelin enhances appetite and increases food intake in humans. J Clin Endocrinol Metab 86: 5992–5995
Lawrence CB, Snape AC, Baudoin FM, Luckman SM 2002 Acute central ghrelin and GH secretagogues induce feeding and activate brain appetite centers. Endocrinology 143: 155–162
Gasco V, Beccuti G, Marotta F, Benso A, Granata R, Broglio F, Ghigo E 2010 Endocrine and metabolic actions of ghrelin. Endocr Dev 17: 86–95
Savage MO, Camacho-Hübner C, David A, Metherell LA, Hwa V, Rosenfeld RG, Clark AJ 2007 Idiopathic short stature: will genetics influence the choice between GH and IGF-I therapy?. Eur J Endocrinol 157: S33–S37
Tassone F, Broglio F, Destefanis S, Rovere S, Benso A, Gottero C, Prodam F, Rossetto R, Gauna C, van der Lely AJ, Ghigo E, Maccario M 2003 Neuroendocrine and metabolic effects of acute ghrelin administration in human obesity. J Clin Endocrinol Metab 88: 5478–5483
Shiiya T, Nakazato M, Mizuta M, Date Y, Mondal MS, Tanaka M, Nozoe S, Hosoda H, Kangawa K, Matsukura S 2002 Plasma ghrelin levels in lean and obese humans and the effect of glucose on ghrelin secretion. J Clin Endocrinol Metab 87: 240–244
Castañeda TR, Tong J, Datta R, Culler M, Tschop MH 2010 Ghrelin in the regulation of body weight and metabolism. Front Neuroendocrinol 31: 44–60
Ghizzoni L, Mastorakos G, Vottero A, Ziveri M, Ilias I, Bernasconi S 2004 Spontaneous growth hormone (GH) secretion is not directly affected by ghrelin in either short normal prepubertal children or children with GH neurosecretory dysfunction. J Clin Endocrinol Metab 89: 5488–5495
Maccario M, Veldhuis JD, Broglio F, Vito LD, Arvat E, Deghenghi R, Ghigo E 2002 Impact of two or three daily subcutaneous injections of hexarelin, a synthetic growth hormone (GH) secretagogue, on 24-h GH, prolactin, adrenocorticotropin and cortisol secretion in humans. Eur J Endocrinol 146: 310–318
Yukawa M, Weigle DS, Davis CD, Marck BT, Woolden-Hanson T 2008 Peripheral ghrelin treatment stabilizes body weights of senescent male Brown Norway rats at baseline and after surgery. Am J Physiol Regul Integr Comp Physiol 294: R1453–R1460
Dornonville de la Cour C, Lindqvist A, Egecioglu E, Tung YC, Surve V, Ohlsson C, Jansson JO, Erlanson-Albertsson C, Dickson SL, Håkanson R 2005 Ghrelin treatment reverses the reduction in weight gain and body fat in gastrectomised mice. Gut 54: 907–913
Garcia JM, Polvino WJ 2007 Effect on body weight and safety of RC-1291, a novel, orally available ghrelin mimetic and growth hormone secretagogue: results of a phase I, randomized, placebo-controlled, multiple-dose study in healthy volunteers. Oncologist 12: 594–600
Broglio F, Gianotti L, Destefanis S, Fassino S, Abbate Daga G, Mondelli V, Lanfranco F, Gottero C, Gauna C, Hofland L, Van der Lely AJ, Ghigo E 2004 The endocrine response to acute ghrelin administration is blunted in patients with anorexia nervosa, a ghrelin hypersecretory state. Clin Endocrinol (Oxf) 60: 592–599
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by the Tripler Army Medical Center Department of Clinical Investigation.
The views expressed in this manuscript are those of the authors and do not reflect the official policy or position of the Department of the Army, Department of Defense, or the U.S. Government.
This study is registered at ClinicalTrials.gov, study number NCT01070173.
Rights and permissions
About this article
Cite this article
Pinsker, J., Ondrasik, D., Chan, D. et al. Total and Acylated Ghrelin Levels in Children With Poor Growth. Pediatr Res 69, 517–521 (2011). https://doi.org/10.1203/PDR.0b013e3182181b2c
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e3182181b2c