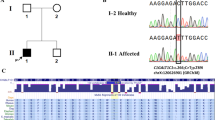
Abstract
Although genetic defect of complement factor H (CFH) is a common cause of atypical hemolytic uremic syndrome (aHUS), development of autoantibodies to CFH (CFH-Ab) is also known to be an acquired cause of aHUS. Recently, a correlation between the development of CFH-Ab and the deficiency of the CFH-related proteins, CFHR1 and CFHR3, was identified. In this study, plasma complement profiles were measured and genetic analysis of the CFH, CFI, MCP, CFHR1, and CFHR3 genes were performed in three female patients diagnosed with aHUS with positive CFH-Ab. Acute stage plasmas of all the three patients revealed low C3, low or low-normal CFH antigenic levels, and high titers of CFH-Ab. All the patients also showed complete plasma CFHR1 deficiency and homozygous genomic deletion of CFHR1/CFHR3, but none had CFH, CFI, or MCP mutations. All the patients were treated with plasmapheresis, and two patients required additional immunosuppressive therapy. These patients had a novel subgroup of aHUS characterized by a combination of genetic (a homozygous deletion of CFHR1/CFHR3) and acquired (development of CFH-Ab) factors. Patients with this disease may need intensive immunosuppressive therapy in addition to plasmapheresis. Screening for CFH-Ab and the CFHR1/CFHR3 deficiency should be included in the diagnostic tests for patients with aHUS.
Similar content being viewed by others
Main
Hemolytic uremic syndrome (HUS) is a clinical syndrome characterized by microangiopathic hemolytic anemia, thrombocytopenia, and acute renal failure (1). In ∼90% of childhood cases, HUS follows a prodrome of diarrhea, which is typically caused by verocytotoxin-producing Escherichia coli (1). However, atypical cases (aHUS) without preceding diarrhea also occur. These cases show a tendency to relapse, to occur in families, and to have a poor outcome (1,2). Recent advances have shown that aHUS is a disease of complement dysregulation, and that loss-of-function mutations were detected in ∼50% of cases in one of the three complement regulator genes: the CFH gene encoding complement factor H (CFH), the CFI gene encoding complement factor I, and the MCP gene encoding membrane cofactor protein (CD46) (3,4). In addition, few cases of aHUS were associated with gain-of-function mutations in complement activation proteins, complement factor B and C3, as described (5,6). Among these mutations, CFH mutations are the most common and account for 14–30% of aHUS cases (3,4,7–10).
In addition to genetic defects associated with aHUS, acquired functional defects of CFH due to the development of anti-CFH autoantibodies (CFH-Ab) have been observed in 6–11% of aHUS cases (11–13). In 2008, Józsi et al.(13) isolated a strong correlation between the occurrence of CFH-Ab and the genetic deletion of the CFHR1 and CFHR3 genes by identifying 16 patients (11%) with both defects in a cohort of 147 aHUS patients. The CFHR1 and CFHR3 genes, which are tightly linked to the CFH gene, encode CFH-related protein 1 and 3 (CFHR1 and CFHR3), respectively (14,15).
Here, we report three additional cases of aHUS positive for CFH-Ab with deficiency of CFHR1/CFHR3. Although the mechanism involved in how CFHR1/CFHR3 deficiency leads to the generation of CFH-Ab is currently unknown, it is clinically important to detect CFH-Ab in deciding the treatment option for patients with aHUS. In patients with positive CFH-Ab, plasma infusion or plasmapheresis alone may be insufficient to restore hematologic and renal disturbances and need additional immunosuppressive treatments in the early phase of disease to reduce CFH-Ab production.
MATERIALS AND METHODS
Patients.
All the three patients were clinically diagnosed as aHUS, and stool culture and multiplex PCR tests for verotoxin-producing E. coli in their stools were negative. This study was approved by the Ethics Committee of Seoul National University Hospital, Seoul, Korea, and informed consent of parents of the each patient was obtained before DNA analysis.
Complement Assays.
Plasma concentrations of the complement components C3, C4, and factor B antigens were measured by nephelometry (Dade Behring, Paris La Defense, France). CFH and complement factor I antigen concentrations were measured by an ELISA method as described previously (16).
CFH-Ab Assessment.
Presence of plasma CFH-Ab was detected by using an ELISA method as previously described (16). Briefly, ELISA plates were coated with 0.3 μg of purified human CFH (Calbiochem, Meudon, France). After washing and blocking free reactive sites with PBS containing 1% BSA, serially diluted sample plasmas were added to the ELISA plates for 1 h at room temperature. After washing, the plates were incubated for 1 h at room temperature with a horseradish peroxidase-conjugated goat anti-human IgG antibody (Sigma-Aldrich Chemical, Steinheim, Germany). After additional washing, enzymatic activity was revealed using the orthophenyldiamine substrate. Antibody titers were expressed as arbitrary units per mL (AU/mL) calculated as (S − B) × 1000/(P − B), where S is OD of the test sample diluted at 1:200, B is absorbency of the blank, and P is absorbency of the reference positive plasma diluted (1:200) given an arbitrary titer of 1000 AU/mL.
Western Blot Analysis.
Plasma samples of the patients and their available family members were investigated by Western blotting by using an enhanced chemiluminescent kit (Amersham Life Science, Buckinghamshire, UK). Goat polyclonal anti-human CFH (Calbiochem, San Diego, CA) was used as a primary antibody (1:2500 dilution) and a horseradish peroxidase-conjugated donkey anti-goat IgG (Santa Cruz Biotechnology, Santa Cruz, CA) as a secondary antibody (1:2500 dilution). The pooled plasma of five healthy volunteers was used as a normal control. There are two differently glycosylated forms of CFHR1 protein, CFHR1α (one carbohydrate residue) and CFHR1β (two carbohydrate residues). Western blot analysis of the plasma of the control subjects revealed three strong bands. According to the binding capacity of the primary antibody, which can bind CFH and factor H like protein-1 (CFHL-1, an alternative splicing product of CFH) strongly and also bind CFHR1–5 weakly, the largest band represents CFH (150 kD) and two smaller bands represent CFHR1α (37 kD) and a mixture of CFHL-1 and CFHR1β (43 kD). Specific antibodies against CFHR1 and CFHR3 were not available for this study.
Genomic DNA Analysis.
The entire coding exons of CFH, MCP, and CFI were amplified from peripheral blood genomic DNA by PCR and directly sequenced in all the three patients. In addition, to screen the homozygous deletion of CFHR1/CFHR3, genomic DNA was amplified by PCR using eight specific primer pairs (R1–R8 primer pairs described in Ref. 14) that cover the 100-kb region downstream of the CFH gene. We screened 100 control Korean subjects with this method, and the homozygous deletion of CFHR1/CFHR3 was detected in two subjects.
RESULTS
Patient 1.
A 7-y-old girl was admitted to the hospital with abdominal pain, vomiting, gross hematuria, with a blood pressure of 110/64 mm Hg. Laboratory tests revealed microangiopathic hemolytic anemia (Hb 64 g/L, reticulocyte count 11.5%, serum haptoglobin <0.07 g/L), thrombocytopenia (20 × 109/L), and azotemia [serum creatinine 274 μM, estimated GFR by Schwartz formula (17) 23 mL · min−1 · 1.73 m−2]. Her spot urine protein/creatinine ratio [Pr/Cr, (mg/dL)/(mg/dL)] was 31.9. A stool culture and multiplex PCR test for verotoxin-producing E. coli in the stool were both negative. An antinuclear antibody (ANA) test was negative. The hemolytic process was not controlled by 10 sessions of daily plasmapheresis followed by a week of intermittent plasmapheresis (three times per week) and hemodialysis. Therefore, oral corticosteroid treatment (2 mg · kg−1 · d−1) was started at day 18 and i.v. immunoglobulin (1 g/kg) was administered twice at days 38 and 39. The steroid and immunoglobulin treatment brought clinical improvement without further plasmapheresis. However, aHUS recurred at day 58 with abdominal pain and jaundice (serum total and direct bilirubin levels were 180 and 106 μM). The serum levels of hepatic (alanine aminotransferase 708 U/L) and pancreatic enzymes (amylase 193 U/L) were elevated, and abdominal ultrasonography revealed mildly swollen pancreas and fluid collection with septation in the peripancreatic space. Although the hepatic and pancreatic symptoms were relieved after 1 wk of supportive care and total restriction of oral intake, the hemolytic process was unresponsive to 1 wk of daily plasmapheresis but the addition of oral azathioprine (2 mg · kg−1 · d−1) to the treatment regimen resulted in a complete remission with the discontinuation of plasmapheresis. Laboratory tests conducted 5 mo after onset of symptoms revealed no evidence of hemolysis, but moderate renal insufficiency (serum creatinine 115 μM, estimated GFR 23 mL · min−1 · 1.73 m−2) with mild proteinuria. Oral corticosteroid treatment is currently being tapered (Table 1 and Fig. 1A).
Patients 2 and 3.
These two patients, when compared with patient 1, showed milder but very similar clinical features and laboratory findings, which were summarized in Fig. 1B, Fig. 1C, and Tables 1 and 2. Both patients had preceding nonbloody diarrhea with stools negative for enterohemorrhagic E. coli and verotoxin. In patient 2, stool was positive for norovirus RNA by RTPCR.
Complement and CFH-Ab assay.
Table 2 summarizes the plasma complement profiles of these three patients. In all the three patients, the plasma C3 levels were decreased in the acute stage but normalized once in remission. The antigenic levels of CFH were low (Patients 1 and 3) or low normal (patient 2) during the acute stage; however, these levels were also normalized later during follow-up. The initial titers of the CFH-Ab were extremely elevated in all patients. After 3–11 mo of follow-up examinations, the CFH-Ab titers decreased markedly but still above normal.
Western blot and genomic DNA analysis.
When compared with three strong bands detected in the plasma of the control subjects, the 37 kD band (CFHR1α) was completely lacking and the 43 kD band (a mixture of CFHL-1 and CFHR1β) was weaker in all the three patients, while the 150 kD band (CFH) was comparable. These findings suggest that the patients have a homozygous depletion of CFHR1 in their plasmas. The 37 and 43 kD bands of the parents of patient 1 were weaker than those of the controls, which suggests a heterozygous deletion (Fig. 2).
Western blot analysis of plasma using a commercial polyclonal anti-human CFH antibody. Three bands are seen in lane 1 (pooled control plasmas); CFH of 150 kD, CFH-related protein 1α (CFHR1α) of 37 kD, and a mixture of CFH-like protein-1 (FHL-1) and CFHR1β of 43 kD. The 37 kD band was completely lacking and the 43 kD band was weaker in all the three patients (lanes 2, 5, and 6, respectively), which suggests a complete lack of CFHR1α/CFHR1β. The parents of patient 1 (lanes 3 and 4) showed weaker 37 and 43 kD bands than the controls, which suggests a heterozygous deficiency of CFHR1α/CFHR1β. Lane 7 is the plasma of a patient with a CFH mutation.
Finally, the homozygous deletion of the CFHR1/CFHR3 genes was confirmed by failure of PCR amplification of the genomic DNA fragments within or near both genes in all the three patients (Fig. 3).
Panel A: A partial map of the human RCA gene cluster on chromosome 1q32 showing four genes (CFH, CFHR3, CFHR1, and CFHR4) in tandem arrangement. Exons are indicated as gray vertical lines, and the positions of the two duplicated homologous segments (B and B′) and the eight primer pairs (R1–R8) are shown. Panel B: Failure to amplify DNA downstream of CFH (R2–R6) was noted in all the three patients (Pt 1, Pt 2 and Pt 3), whereas the DNA was amplified in the control subjects (C). These results suggest a homozygous genomic deletion of CFHR1/CFHR3 due to recombination between segments B and B′. M, molecular size markers.
No pathogenic mutations of the CFH, CFI, and MCP genes were detected in any of the patients.
DISCUSSION
CFH, a serum glycoprotein, is composed of 20 consecutive homologous units called complement control protein modules, each comprising ∼60 amino acids (18). CFH is a central fluid-phase regulator of the alternative pathway of complement, having both cofactor and decay-accelerating activity (19). The majority (60–70%) of CFH mutations is heterozygous missense mutations that cluster in the C-terminal region of CFH, a heparin binding domain (20–22). Such mutants show decreased binding for glycosaminoglycans, endothelial cells, and C3b, the CFH ligand (20,23–25). In addition to genetic defects involving CFH or other complement regulator genes, aHUS may also result from an acquired defect such as the development of CFH-Ab (11–13). The binding epitopes of the CFH-Ab are localized to the C-terminal recognition region of CFH, which is a hot spot for genetic mutations (11,12).
The role of CFHRs has also been studied as a cause of aHUS. The genes for CFH and CFHR1–5 are all tightly linked in the regulators of complement activation (RCA) gene cluster at chromosome 1q32. This site is a hot spot for gene conversion events as well as genomic rearrangements (26–28), and a role for gene conversion in generation of CFH mutants associated with aHUS was proved (28). In addition, it is recently known that a haplotype containing a deletion of CFHR1/CFHR3, which may result from a nonallelic homologous recombination between CFH and CFHR1, is detected in ∼2% of normal population (11), and this polymorphism has been demonstrated to increase the risk of aHUS (29).
Finally, in 2008, Józsi et al. (13) identified a strong correlation between the occurrence of CFH-Ab and the absence or reduction of plasma CFHR1/CFHR3. In a large cohort of 147 patients with aHUS, they found 22 (15%) patients had total or near total CFHR1/CFHR3 deficiency and 16 (11% of the total) of those patients were positive for CFH-Ab. Furthermore, no patients developed CFH-Ab that did not have a CFHR1/CFHR3 deficiency. These findings suggest that CFHR1/CFHR3 deficiency may favor the development of CFH autoantibody. However, the mechanism by which the CFHR1/CFHR3 deficiency leads to the generation of CFH-Ab is currently unknown. Small portion of healthy control subjects and some patients with aHUS have CFHR1/CFHR3 deficiency but not CFH-Ab (11,13). Several clinically unaffected family members of the patients with CFHR1/CFHR3 deficiency and CFH-Ab also showed CFHR1/CFHR3 deficiency without CFH-Ab (13). These findings suggest that the CFHR1/CFHR3 deficiency itself is not sufficient for the development of CFH-Ab and aHUS.
Since three French cases of aHUS associated with CFH-Ab were first described by Dragon-Durey et al. in 2005 (12), a total of 24 patients with aHUS associated with CFH-Ab have been reported with the frequency of 6–11% among patients with aHUS (11–13). However, the CFHR1/CFHR3 genes were studied in 16 patients of the latest study (13) only, and all 16 have deletion of both genes. Our study presents three additional cases with aHUS associated with a CFH-Ab and a homozygous deletion of CFHR1/CFHR3.
Almost all the previously reported patients with CFH-Ab positive aHUS as well as our patients were juvenile, suggesting a preferential age in preadolescent children (11–13). Conversely, aHUS associated with CFH mutations starts earlier in children, including the neonatal period (4). In addition, the three cases reported here and two of the three French cases (12) showed extra-renal involvements, especially in the liver and pancreas. Conversely, extrarenal involvement in patients with other forms of aHUS has been reported uncommon (4).
In the three French cases (12), the CFH assays were not performed during the acute phase for two of the patients and their plasma CFH activity decreases, whereas their plasma CFH antigenic levels were normal. Conversely, although the CFH activity was not measured in our cases, the CFH antigenic levels were low or low normal in plasma samples collected during the acute stage but were normalized in plasma collected during the convalescent stage. Based on these results, one can speculate that rapid development of a very large amount of CFH-Ab may lead to a transient decrease in circulating CFH. Therefore, a decreased plasma CFH antigenic level in a patient with aHUS does not exclude the possibility of CFH-Ab-associated aHUS.
All the three French patients were ANA positive (12). Similarly, ANA is frequently detected in adult patients with idiopathic thrombotic microangiopathies associated with acquired ADAMST-13 deficiency (30). Conversely, none of the patients in our study exhibited ANA. However, we currently have no explanation for this difference.
In majority of patients with aHUS with/without known genetic mutations, the illness is preceded by a triggering condition such as a nonspecific infection (3). Indeed, all the three patients in our study as well as the three French cases (12) involved a preceding diarrheal illness and/or gastrointestinal symptoms. Therefore, it is likely that a triggering nonspecific infection alters the immunologic response of the host and leads to the development of autoantibodies. This phenomenon is probably more likely to occur in hosts with a genetic defect of CFHR1/CFHR3.
Genetic diagnosis of patients with aHUS can provide relevant information that can be used to predict survival, renal recovery, and transplant outcome. Overall, patients with MCP mutations have a milder form of the disease than those with either CFH or CFI mutations, and many of these patients recover without plasma therapy (3). In addition, screening for CFH-Ab in aHUS patients would be helpful for planning a therapeutic strategy, as patients with CFH-Ab may require intensive immunosuppressive therapy as well as plasma infusion or plasmapheresis. Plasma therapy, which is the mainstay of treatment of aHUS, can remove circulating CFH-Ab, but such treatment cannot block ongoing production of the autoantibodies. The required intensity of immunosuppressive therapy for individual patients may be proportional to the degree of CFH-Ab production of each patient. All the three patients reported here and the three French patients (12) had recurrences of aHUS, when plasma therapy was stopped. Most likely, this was due to a rebound of CFH-Ab, which was subsequently prevented by the addition of steroid and/or azathioprine to plasma therapy in four of them. These findings suggest that more aggressive immunosuppressive treatment should be started earlier to prevent this sequel and tapering if this treatment should be guided by serial determination of the antibody titers. In addition, determination of CFH-Ab is also necessary if kidney transplantation is necessary to prevent posttransplant HUS recurrence (31,32).
In conclusion, we present three additional patients with a novel subgroup of aHUS that is characterized by a peculiar combination of genetic (a homozygous deletion of CFHR1/CFHR3) and acquired (development of CFH-Ab) factors. For patients with aHUS, determination of CFH-Ab is necessary not only for correct diagnosis but also for planning a therapeutic strategy.
Abbreviations
- aHUS:
-
atypical hemolytic uremic syndrome
- ANA:
-
antinuclear antibody
- CCP:
-
complement control protein module
- CFH:
-
complement factor H
- CFH-Ab:
-
anticomplement factor H autoantibodies
- CFHR:
-
complement factor H-related protein
- HUS:
-
hemolytic uremic syndrome
References
Noris M, Remuzzi G 2005 Hemolytic uremic syndrome. J Am Soc Nephrol 16: 1035–1050
Kavanagh D, Goodship TH, Richards A 2006 Atypical haemolytic uraemic syndrome. Br Med Bull 77-78: 5–22
Caprioli J, Noris M, Brioschi S, Pianetti G, Castelletti F, Bettinaglio P, Mele C, Bresin E, Cassis L, Gamba S, Porrati F, Bucchioni S, Monteferrante G, Fang CJ, Liszewski MK, Kavanagh D, Atkinson JP, Remuzzi G 2006 Genetics of HUS: the impact of MCP, CFH, and IF mutations on clinical presentation, response to treatment, and outcome. Blood 108: 1267–1279
Sellier-Leclerc AL, Frémeaux-Bacchi V, Dragon-Durey MA, Macher MA, Niaudet P, Guest G, Boudailliez B, Bouissou F, Deschenes G, Gie S, Tsimaratos M, Fischbach M, Morin D, Nivet H, Alberti C, Loirat C 2007 Differential impact of complement mutations on clinical characteristics in atypical hemolytic uremic syndrome. J Am Soc Nephrol 18: 2392–2400
Goicoechea de Jorge E, Harris CL, Esparza-Gordillo J, Carreras L, Arranz EA, Garrido CA, Lopez-Trascasa M, Sanchez-Corral P, Morgan BP, Rodriguez de Cordoba S 2007 Gain-of-function mutations in complement factor B are associated with atypical hemolytic uremic syndrome. Proc Natl Acad Sci USA 104: 240–245
Frémeaux-Bacchi V, Miller EC, Liszewski MK, Strain L, Blouin J, Brown AL, Moghal N, Kaplan BS, Weiss RA, Lhotta K, Kapur G, Mattoo T, Nivet H, Wong W, Gie S, Hurault de Ligny B, Fischbach M, Gupta R, Hauhart R, Meunier V, Loirat C, Dragon-Durey MA, Fridman WH, Janssen BJ, Goodship TH, Atkinson JP 2008 Mutations in complement C3 predispose to development of atypical hemolytic uremic syndrome. Blood 112: 4948–4952
Neumann HP, Salzmann M, Bohnert-Iwan B, Mannuelian T, Skerka C, Lenk D, Bender BU, Cybulla M, Riegler P, Konigsrainer A, Neyer U, Bock A, Widmer U, Male DA, Franke G, Zipfel PF 2003 Haemolytic uraemic syndrome and mutations of the factor H gene: a registry-based study of German speaking countries. J Med Genet 40: 676–681
Dragon-Durey MA, Frémeaux-Bacchi V 2005 Atypical haemolytic uraemic syndrome and mutations in complement regulator genes. Springer Semin Immunopathol 27: 359–374
Frémeaux-Bacchi V, Kemp EJ, Goodship JA, Dragon-Durey MA, Strain L, Loirat C, Deng HW, Goodship TH 2005 The development of atypical haemolytic-uraemic syndrome is influenced by susceptibility factors in factor H and membrane cofactor protein: evidence from two independent cohorts. J Med Genet 42: 852–856
Esparza-Gordillo J, Goicoechea de Jorge E, Buil A, Carreras Berges L, Lopez-Trascasa M, Sanchez-Corral P, Rodriguez de Cordoba S 2005 Predisposition to atypical hemolytic uremic syndrome involves the concurrence of different susceptibility alleles in the regulators of complement activation gene cluster in 1q32. Hum Mol Genet 14: 703–712
Józsi M, Strobel S, Dahse HM, Liu WS, Hoyer PF, Oppermann M, Skerka C, Zipfel PF 2007 Anti factor H autoantibodies block C-terminal recognition function of factor H in hemolytic uremic syndrome. Blood 110: 1516–1518
Dragon-Durey MA, Loirat C, Cloarec S, Macher MA, Blouin J, Nivet H, Weiss L, Fridman WH, Fremeaux-Bacchi V 2005 Anti-Factor H autoantibodies associated with atypical hemolytic uremic syndrome. J Am Soc Nephrol 16: 555–563
Józsi M, Licht C, Strobel S, Zipfel SL, Richter H, Heinen S, Zipfel PF, Skerka C 2008 Factor H autoantibodies in atypical hemolytic uremic syndrome correlate with CFHR1/CFHR3 deficiency. Blood 111: 1512–1514
Male DA, Ormsby RJ, Ranganathan S, Giannakis E, Gordon DL 2000 Complement factor H: sequence analysis of 221 kb of human genomic DNA containing the entire fH, fHR-1 and fHR-3 genes. Mol Immunol 37: 41–52
Zipfel PF, Jokiranta TS, Hellwage J, Koistinen V, Meri S 1999 The factor H protein family. Immunopharmacology 42: 53–60
Dragon-Durey MA, Frémeaux-Bacchi V, Loirat C, Blouin J, Niaudet P, Deschenes G, Coppo P, Herman Fridman W, Weiss L 2004 Heterozygous and homozygous factor H deficiencies associated with hemolytic uremic syndrome or membranoproliferative glomerulonephritis: report and genetic analysis of 16 cases. J Am Soc Nephrol 15: 787–795
Schwartz GJ, Haycock GB, Edelmann CM Jr, Spitzer A 1976 A simple estimate of glomerular filtration rate in children derived from body length and plasma creatinine. Pediatrics 58: 259–263
Kristensen T, Tack BF 1986 Murine protein H is comprised of 20 repeating units, 61 amino acids in length. Proc Natl Acad Sci USA 83: 3963–3967
Atkinson JP, Liszewski MK, Richards A, Kavanagh D, Moulton EA 2005 Hemolytic uremic syndrome: an example of insufficient complement regulation on self-tissue. Ann N Y Acad Sci 1056: 144–152
Jokiranta TS, Cheng ZZ, Seeberger H, Jozsi M, Heinen S, Noris M, Remuzzi G, Ormsby R, Gordon DL, Meri S, Hellwage J, Zipfel PF 2005 Binding of complement factor H to endothelial cells is mediated by the carboxy-terminal glycosaminoglycan binding site. Am J Pathol 167: 1173–1181
Hellwage J, Jokiranta TS, Friese MA, Wolk TU, Kampen E, Zipfel PF, Meri S 2002 Complement C3b/C3d and cell surface polyanions are recognized by overlapping binding sites on the most carboxyl-terminal domain of complement factor H. J Immunol 169: 6935–6944
Kavanagh D, Richards A, Atkinson J 2008 Complement regulatory genes and hemolytic uremic syndromes. Annu Rev Med 59: 293–309
Józsi M, Heinen S, Hartmann A, Ostrowicz CW, Halbich S, Richter H, Kunert A, Licht C, Saunders RE, Perkins SJ, Zipfel PF, Skerka C 2006 Factor H and atypical hemolytic uremic syndrome: mutations in the C-terminus cause structural changes and defective recognition functions. J Am Soc Nephrol 17: 170–177
Vaziri-Sani F, Holmberg L, Sjöholm AG, Kristoffersson AC, Manea M, Fremeaux-Bacchi V, Fehrman-Ekholm I, Raafat R, Karpman D 2006 Phenotypic expression of factor H mutations in patients with atypical hemolytic uremic syndrome. Kidney Int 69: 981–988
Manuelian T, Hellwage J, Meri S, Caprioli J, Noris M, Heinen S, Jozsi M, Neumann HP, Remuzzi G, Zipfel PF 2003 Mutations in factor H reduce binding affinity to C3b and heparin and surface attachment to endothelial cells in hemolytic uremic syndrome. J Clin Invest 111: 1181–1190
Lupski JR, Stankiewicz P 2005 Genomic disorders: molecular mechanisms for rearrangements and conveyed phenotypes. PLoS Genet 1: e49
Heinen S, Sanchez-Corral P, Jackson MS, Strain L, Goodship JA, Kemp EJ, Skerka C, Jokiranta TS, Meyers K, Wagner E, Robitaille P, Esparza-Gordillo J, Rodriguez de Cordoba S, Zipfel PF, Goodship TH 2006 De novo gene conversion in the RCA gene cluster (1q32) causes mutations in complement factor H associated with atypical hemolytic uremic syndrome. Hum Mutat 27: 292–293.
Venables JP, Strain L, Routledge D, Bourn D, Powell HM, Warwicker P, Diaz-Torres ML, Sampson A, Mead P, Webb M, Pirson Y, Jackson MS, Hughes A, Wood KM, Goodship JA, Goodship TH 2006 Atypical haemolytic uraemic syndrome associated with a hybrid complement gene. PLoS Med 3: e431
Zipfel PF, Edey M, Heinen S, Józsi M, Richter H, Misselwitz J, Hoppe B, Routledge D, Strain L, Hughes AE, Goodship JA, Licht C, Goodship TH, Skerka C 2007 Deletion of complement factor H-related genes CFHR1 and CFHR3 is associated with atypical hemolytic uremic syndrome. PLoS Genet 3: e41
Coppo P, Bengoufa D, Veyradier A, Wolf M, Bussel A, Millot GA, Malot S, Heshmati F, Mira JP, Boulanger E, Galicier L, Durey-Dragon MA, Fremeaux-Bacchi V, Ramakers M, Pruna A, Bordessoule D, Gouilleux V, Scrobohaci ML, Vernant JP, Moreau D, Azoulay E, Schlemmer B, Guillevin L, Lassoued K 2004 Severe ADAMTS13 deficiency in adult idiopathic thrombotic microangiopathies defines a subset of patients characterized by various autoimmune manifestations, lower platelet count, and mild renal involvement. Medicine (Baltimore) 83: 233–244
Kwon T, Dragon-Durey M-A, Macher M-A, Baudouin V, Maisin A, Peuchmaur M, Fremeaux-Bacchi V, Loirat C 2008 Successful pre-transplant management of a patient with anti-factor H autoantibodies-associated haemolytic uraemic syndrome. Nephrol Dial Transplant 23: 2088–2090
Le Quintrec M, Zuber J, Noel LH, Thervet E, Frémeaux-Bacchi V, Fridman WH, Legendre C, Dragon-Durey MA 2009 Anti-factor H-auto-antibodies in a fifth renal transplant recipient with atypical hemolytic and uremic syndrome. Am J Transplant 9: 1223–1229
Author information
Authors and Affiliations
Additional information
Supported by a Grant A080588 from the Korea Healthcare technology R&D Project, Ministry for Health, Welfare and Family Affairs, Republic of Korea and a Grant 06-2008-192-9 from the Seoul National University Hospital.
Rights and permissions
About this article
Cite this article
Lee, B., Kwak, S., Shin, J. et al. Atypical Hemolytic Uremic Syndrome Associated With Complement Factor H Autoantibodies and CFHR1/CFHR3 Deficiency. Pediatr Res 66, 336–340 (2009). https://doi.org/10.1203/PDR.0b013e3181b1bd4a
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e3181b1bd4a
This article is cited by
-
Mutations in the alternative complement pathway in multiple myeloma patients with carfilzomib-induced thrombotic microangiopathy
Blood Cancer Journal (2023)
-
Genotypic analysis of a large cohort of patients with suspected atypical hemolytic uremic syndrome
Journal of Molecular Medicine (2023)
-
Systematic review of atypical hemolytic uremic syndrome biomarkers
Pediatric Nephrology (2022)
-
Deficiency of CFHR plasma proteins and autoantibody positive hemolytic uremic syndrome: treatment rationale, outcomes, and monitoring
Pediatric Nephrology (2021)
-
Altered Peripheral Blood Leucocyte Phenotype and Responses in Healthy Individuals with Homozygous Deletion of FHR1 and FHR3 Genes
Journal of Clinical Immunology (2019)