Abstract
To test the neuroprotective effects of the nonpsychoactive cannabinoid cannabidiol (CBD), piglets received i.v. CBD or vehicle after hypoxia-ischemia (HI: temporary occlusion of both carotid arteries plus hypoxia). Nonhypoxic-ischemic sham-operated piglets remained as controls. Brain damage was studied by near-infrared spectroscopy (NIRS) and amplitude-integrated electroencephalography (aEEG) and by histologic assessment (Nissl and FluoroJadeB staining). In HI+vehicle, HI led to severe cerebral hemodynamic and metabolic impairment, as reflected in NIRS by an increase in total Hb index (THI) and a decrease in the fractional tissue oxygenation extraction (FTOE); in HI+CBD the increase of THI was blunted and FTOE remained similar to SHAM. HI profoundly decreased EEG amplitude, which was not recovered in HI+vehicle, indicating cerebral hypofunction; seizures were observed in all HI+vehicle. In HI+CBD, however, EEG amplitude recovered to 46.4 ± 7.8% baseline and seizures appeared only in 4/8 piglets (both p < 0.05). The number of viable neurons decreased and that of degenerating neurons increased in HI+vehicle; CBD reduced both effects by more than 50%. CBD administration was free from side effects; moreover, CBD administration was associated with cardiac, hemodynamic, and ventilatory beneficial effects. In conclusion, administration of CBD after HI reduced short-term brain damage and was associated with extracerebral benefits.
Similar content being viewed by others
Main
Several studies have pointed to cannabinoids as substances with a high potential as neuroprotective treatments in ischemic or traumatic brain damage (1,2). Lately, our group has demonstrated that the cannabinoid receptor agonist WIN55212–2 induces signs of neuroprotection in both in vitro and in vivo models of neonatal hypoxic-ischemic encephalopathy (NHIE) in rats (3,4). Because the production of psychoactive effects is likely to limit the therapeutic value of compounds such as WIN55212–2, we have now also performed experiments with cannabidiol (CBD), a major nonpsychoactive constituent of cannabis. Importantly, CBD has been found to induce neuroprotective effects in both in vitro and in vivo studies (5–9). These neuroprotective effects are thought to rely mainly on the potent antiinflammatory and antioxidant properties of CBD (6,9,10), although inhibition of calcium transport across membranes, inhibition of anandamide uptake and enzymatic hydrolysis, and inhibition of iNOS protein expression and NF-κB activation (6,9,11) might also account for CBD-induced neuroprotection.
The aim of the present work was to study the neuroprotective effect of CBD by using the temporary occlusion of both carotid arteries combined with hypoxia animal model, considered as very close to actual perinatal asphyxia in human neonates (12). In addition, we aimed to test the protective effect of CBD by using the two best devices available for actual bedside studies in asphyxiated newborns: near-infrared spectroscopy (NIRS), a noninvasive optical technique for assessing circulation and oxygenation in brain, and amplitude-integrated electroencephalography (aEEG). Neuroprotection by CBD was also assessed by histologic study. Finally, we also aimed to test whether CBD administration was free of significant clinical side effects.
METHODS
Animal preparation.
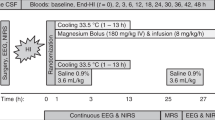
The experimental protocol met European and Spanish regulations for animal research (EU 86/609 and RD 1201/2005). Piglets 3 to 5-d old were anesthetized with a perfusion of phentanil, propofol, and midazolam in dextrose 5% (0.004, 3, and 0.5 mg/kg/h, respectively) and paralyzed by a perfusion of vecuronium (3 mg/kg/h) administered through an ear vein. Animals were then intubated and positive pressure ventilated (Bourns BP200, CA); lung tidal volume (Vt), dynamic compliance (Cdyn), and Oxygenation Index [OI: mean airway pressure (cm H2O) × fraction of inspired oxygen (FiO2)/Pao2 (mm Hg)] were monitored by computerized pneumotacography (Chart5 Powerlab, ADI Instr., CO). Continuous three-lead ECG was recorded. The right common carotid flow (Qcar) was measured by an ultrasonic flow probe (Transonic Systems Inc., NY), as a representation of cerebral blood flow (CBF) (13). Catheters were inserted into femoral arteries to record intraarterial oxygen saturation (SaO2) (Oximetric System, Abbott Laboratories, IL), mean blood pressure (MBP) (Ominare CMS24, HP, Göblingen, Germany) and take blood samples, and into the right jugular vein to record cardiac output (CO) (PiCCO Plus, Pulsion, München, Germany). Rectal temperature was maintained between 37.5 and 38.5°C with heating lamps.
Experimental procedures.
Hypoxia-ischemia (HI) was induced by clamping both carotid arteries with vascular occluders and lowering FiO2 to 8–10% over 20 min. Fifteen and 240 min later, piglets received i.v. 1 mL of saline (HI+VEH group, n = 8, age 4.3 ± 0.3 d h, weight 2.3 ± 0.2 kg) or of a solution containing CBD (Tocris Bioscience, Bristol, UK) 0.1 mg/kg (HI+CBD, n = 8, age 4.6 ± 0.3 d h, weight 2.1 ± 0.1 kg). This dose was selected as it was the lowest tested in previous in vivo studies with CBD (7,8). CBD was dissolved in emulphor/ethanol/saline 1:1:18 (5). Other piglets were similarly anesthetized and intubated but were kept normoxemic with their carotids unclamped (SHAM, n = 3, age 4.5 ± 0.4 d, and weight 2.6 ± 0.4 kg). Six hours after HI, or the equivalent period in SHAM, the piglets were euthanized with an i.v. injection of potassium chloride. Then, the brain was perfused via the carotid arteries with heparin in cold saline, removed, fixed with 4% paraformaldehide, and then stored at 4°C.
Data acquisition and analysis. Physiologic assessment.
Deviations from acceptable blood gases values (ABL5, Radiometer, Copenhagen, Denmark) (Pao2 90–110 mm Hg, Paco2 35–45 mm Hg, and pH 7.35–7.45) were corrected by changing ventilator parameters and/or by adding sodium bicarbonate or Tris as needed. MBP was maintained over 50 mm Hg and blood glucose levels over 40 mg/dL by administering a perfusion of dopamine (0.6 mg/mL in 5% dextrose) or 25% dextrose, respectively, when needed. Blood samples were collected at baseline and 0, 3, and 6 h postinsult. Cardiac troponin T (cTnT), a marker of myocardial ischemia, was measured by ELISA (Elecsys Analyzer, Roche Diagnostics, Mannheim, Germany).
Neurophysiological assessment.
Tissue oxygen index (TOI) and variations in total Hb index (THI) were continuously monitored using a NIRS-system (NIRO-200, Hamamatsu Photonics KK, Joko Cho, Japan). The NIRS sensor was placed on the skull in the midline fronto-parietally and fixed with bandages. TOI represents the tissue oxygen saturation and is measured in percent; it was used to calculate the fractional tissue oxygen extraction (FTOE) (14): FTOE = (SaO2 − TOI)/SaO2. Normalized tissue Hb index (nTHI) is an absolute figure of the total Hb (tHb) content in brain (15); its changes from one measuring point to another are measured as a percentage.
Brain activity (integrated amplitude) and impedance were monitored using a two-channel bed EEG monitor (BRM2, BrainZ Instruments, Auckland, New Zealand). The “raw” EEG traces were manually reviewed for seizures (periods of sudden increase in voltage, accompanied by a narrowing of the band of aEEG activity and followed by a brief period of suppression).
Histologic study.
Fixed brains were cut into sections 5 mm in width and embedded in paraffin. Coronal sections (4 μm) were cut and mounted on a glass slide to be stained. To assess brain damage, consecutive pairs of brain sections were stained by two different methods (16): First, Nissl staining to determine early neuronal necrosis. Areas of 1 mm2 in the central three lobes of the parietal cortex and in the CA1 area of hippocampus were examined using a light microscope (×400) by an investigator blinded to the experimental group, using a grid of 50 compartments, calculating the mean of 5 compartments. Parietal cortex and hippocampus are known to be particularly sensitive to HI-induced tissue damage (17,18); both were counted at 3.00 mm in the posterior plane, as shown in a stereotaxic atlas of pig brain (19). Apparently normal neurons were morphologically identified by the presence of typical nuclei with clear nucleoplasm and a distinct nucleolus, surrounded by purple-stained cytoplasm. Neurons were defined as damaged when no distinction could be made between nucleus and cytoplasm (pyknotic or necrotic). Second, to determine the presence of degenerating neurones, brain sections were stained with FluoroJade B (FJB) (16); these sections were examined using a fluorescence microscope (I3 filter cube for an FITC, excitation band of 450–490 nm).
Statistical analysis.
SPSS 11.0.0 was used for all statistical analyses. Mean values have been compared using the Kruskal-Wallis test for unpaired data and the Wilcoxon signed rank test for paired data. Bonferroni correction for multiple testing was performed when appropriate. A p value <0.05 was considered to be significant. All data are presented as means ± SE.
RESULTS
Neurophysiological assessment.
Hypoxic-ischemic insult induced a hyperaemic response in brain circulation, as shown by the dramatic increase of Qcar (Fig. 1A). Afterward, Qcar remained stable and similar to SHAM. Similarly, an increase of nTHI just after the HI insult was observed by NIRS (Fig. 1B). In HI+CBD, nTHI returned to baseline in approximately 30 min, then remaining similar to SHAM, whereas in HI+VEH, nTHI remained higher than SHAM. In contrast, FTOE fell dramatically during HI, subsequently rising again in the first hour postinsult (Fig. 1C). In HI+CBD, FTOE reached values similar to SHAM during the first 3 h, slightly decreasing afterward; in HI+VEH, in contrast, FTOE remained significantly lower than SHAM from the end of HI and lower than HI+CBD from 1 h postinsult.
Cerebral hemodynamic and metabolic changes induced by HI in piglets and its modification by postinsult administration of cannabidiol 0.1 mg/kg i.v. A, changes in carotid blood flow; B, changes in nTHI determined by NIRS; C, changes in FTOE calculated from NIRS. VEH (•): HI piglets treated with vehicle (n = 8). CBD (○): HI piglets treated with cannabidiol (n = 8). SHAM (▪): operated piglets without HI. B: baseline. H: HI insult. D: drug administration. (*) Kruskall-Wallis p < 0.05 vs SHAM; (†) Kruskall-Wallis p < 0.05 vs VEH.
During HI, EEG amplitude was reduced to 14.5 ± 4.3% and 16.9 ± 2.3% baseline in HI+VEH and HI+CBD, respectively (Fig. 2A). This severely depressed activity remained unchanged in HI+VEH but partially recovered from 1 h postinsult in HI+CBD (Fig. 2A); thus, at the end of the experiment, amplitude was 20.5 ± 4.8% and 46.4 ± 7.8% baseline in HI+VEH and HI+CBD, respectively (p < 0.05). None of HI+VEH regained an EEG amplitude over 4 μV, whereas that amplitude was regained in 6/8 HI+CBD (p < 0.05). The EEG traces indicate the presence of seizures in all piglets from HI+VEH but only in 4/8 HI+CBD (p < 0.05).
Changes in cerebral amplitude (A) and impedance (B) induced by HI in piglets and its modification by postinsult administration of cannabidiol 0.1 mg/kg i.v., determined by amplitude-integrated EEG. VEH (•): HI piglets treated with vehicle (n = 8). CBD (○): HI piglets treated with cannabidiol (n = 8). SHAM (▪): operated piglets without HI. B: baseline. H: HI insult. D: drug administration. (*) Kruskall-Wallis p < 0.05 vs SHAM; (†) Kruskall-Wallis p < 0.05 vs VEH.
Cerebral impedance increased 1 h postinsult in HI+VEH, reaching values 2-fold higher than baseline (Fig. 2B); in HI+CBD, the increase of impedance was very modest and only significantly different from SHAM at the end of the experiment (Fig. 2B).
Histologic analysis.
Nissl staining revealed a decrease in the number of apparently normal neurons in cortex and hippocampus of HI+VEH piglets (Fig. 3) (371 ± 21 per mm2 in cortex and 82 ± 27 per mm2 in hippocampus versus 653 ± 6 per mm2 and 240 ± 5 per mm2, respectively, in SHAM, both p < 0.05). In addition, a number of pyknotic neurons appeared in HI+VEH, mainly in the deeper layers of cortex but also in hippocampus. In HI+CBD, the loss of normal neurons was blunted and the appearance of pyknotic cells prevented (Fig. 3); thus, normal neurons were 482 ± 21 per mm2 in cortex and 160 ± 25 per mm2 in hippocampus in HI+CBD (p < 0.05 versus HI+VEH and versus SHAM).
Representative light microphotographs of Nissl-stained brain sections, obtained after sham operation (SHAM) or after HI from piglets receiving VEH or CBD 0.1 mg/kg. C: parietal cortex; H: hippocampus. In brain from HI+VEH there is a decrease in number of viable neurons and an increase in number of pyknotic cells (arrows). Administration of CBD reduced the loss of viable neurons and the presence of pyknotic cells. Original magnification ×200, bar: 100 μm.
FJB staining revealed the appearance of a number of degenerating neurons in HI+VEH in cortex and hippocampus (Fig. 4) (298 ± 29 per mm2 in cortex and 260 ± 44 per mm2 in hippocampus, versus 10 ± 3 per mm2 in cortex and 5 ± 2 per mm2 in hippocampus in SHAM, both p < 0.05). The number of degenerating neurons was reduced by CBD (96 ± 21 per mm2 in cortex and 116 ± 23 per mm2 in hippocampus in HI+CBD, p < 0.05 versus HI+VEH and versus SHAM).
Representative light microphotographs of FluoroJade B stained brain sections, obtained after sham operation (SHAM) or after HI from piglets receiving VEH or CBD 0.1 mg/kg. C: parietal cortex; H: hippocampus. Administration of CBD reduced the number of degenerating—FJB-stained—cells. Original magnification ×200, bar: 100 μm.
Physiologic data.
Blood pressure fell after HI, more severely in HI+VEH than in HI+CBD (Table 1) even though the former were receiving at the end of the experiment more dopamine than the latter (16.9 ± 3.8 μg/kg/min versus 8.1 ± 2.2 μg/kg/min, p < 0.05). Decrease of MBP was compensated for by a significant increase in heart rate, to maintain CO stable (Table 1). cTnT was undetectable in SHAM and in the other groups at baseline. HI led to an immediate and sustained increase in cTnT that was greater in VEH than in CBD, so that from 3 h after HI cTnT levels were greater in VEH than in CBD (Table 1).
HI led to a similar decrease of Pao2 in HI+VEH and HI+CBD (31.1 ± 2.5 and 28.9 ± 1.6 mm Hg, respectively). HI insult induced a profound decrease in pH, similar in HI+VEH and HI+CBD (Table 1). In all HI+CBD piglets, normal pH was regained by 1 h postinsult; in HI+VEH, normal pH was regained only in six of eight piglets beyond 3 h postinsult. Similarly, Paco2 increased after HI in both groups (Table 1); HI+CBD regained normal levels by 2 h postinsult whereas in HI+VEH, five of eight piglets were still showing supra-normal values at the end of the experiment.
The HI insult led to an early increase of O2 needs, as demonstrated by the enhancement of OI in both HI groups (Table 1). Mechanical ventilation induced lung damage, as suggested even in SHAM animals by the progressive increase of OI and decrease of Vt and compliance (Table 1). CBD demonstrated some lung protective effects, as both Vt and compliance remained stable throughout the experiment, unlike HI+VEH piglets, which showed a decrease of both parameters parallel to that observed in CTL animals. Moreover, OI decreased during the experimental period in HI+CBD to values even lower than in SHAM, whereas in HI+VEH OI values increased to reach statistical significance at the end of the experiment.
DISCUSSION
Our present investigation demonstrated that CBD, administered after HI in newborn piglets, could display neuroprotective activity without inducing significant side effects. To the best of our knowledge, this is the first study demonstrating short-term neuroprotection by CBD in newborn animals, and supports previous studies in adult rodent models of stroke (5,7,8). Importantly, CBD protected against ischemic brain injury when administered after the insult, which renders CBD a feasible tool for clinical use, as NHIE is currently unpredictable (20). Another point favoring a possible clinical use of CBD is its lack of psychoactive effects because CBD does not activate CB1 receptors (6). In our study, CBD was neuroprotectant at a dose (0.1 mg/kg) below that reported for adult rodents (1–5 mg/kg) (5,7,8). This difference might be due to species- or age-related differences in sensitivity to CBD and/or to the use of a different route for drug. The absence of significant side effects with CBD in our study does, however, warrant further investigation directed at examining the effects of higher doses of this cannabinoid.
After the HI episode, we did not observe any difference in Qcar between SHAM and HI+VEH piglets, as reported previously (21), nor between HI+VEH and HI+CBD. Previous studies indicate that CBD increases CBF in cortex during ischemia in mice (7), an effect that may reflect the ability of CBD to dilate cerebral arteries in rodents via the activation of vanilloid receptors (6). This difference might be due to the low dose of CBD we used, as CBD has been demonstrated to be a full vanilloid receptor agonist at concentrations attained after its administration at doses almost 100 times higher (22). Nevertheless, changes in regional CBF by CBD cannot be ruled out in our experiments, as we measured Qcar. In NIRS, HI+VEH showed an increase in nTHI. nTHI provides an absolute measure of tHb in brain (15), changes in which reflect changes in cerebral blood volume (CBV) (13). Increased CBV may indicate pronounced vasodilation in cerebral microcirculation due to exhausted autoregulatory vasodilation (14,23). Another factor influencing the increase in THI is the increase in oxygenated Hb content that results from decreased cerebral oxygen utilization caused by increased brain damage (24). Accordingly, FTOE was decreased in HI+VEH piglets, as reported previously (14). The association of an increase in CBV and a decrease in uptake of oxygen by the brain is considered as particularly ominous for asphyxiated newborns (23). Administration of CBD prevented that increase in THI to occur and blunted the decrease of FTOE. Normal CBV together with increased uptake of oxygen by the brain reflects less severe cerebral hemodynamic impairment in human newborns and is associated with a more favorable outcome (23).
The pattern of aEEG in piglets after HI resembles best the situation in the human newborn affected by perinatal asphyxia (12). The immediate drop in amplitude we observed at the start of the HI period, similar in VEH and CBD, reflects the severity of the insult (13,25) and is due to the decrease in neuronal metabolism that protects the brain cells against further injury (12). Sustained severely reduced EEG amplitude despite oxygenation and hemodynamic recovery, as we observed in HI+VEH, suggests neuronal hypofunction with lower brain oxygen utilization (12,13). This agrees with the low FTOE we observed during this period in HI+VEH. None of HI+VEH piglets did recover EEG amplitude over 4 μV and all of them showed seizure activity, both effects that signal an unfavourable outcome in human newborns (26,27). In contrast, CBD administration led to a significant recovery of amplitude, with six of eight piglets regaining EEG amplitude by more than 4 μV at the end of the experiment. Improvement in aEEG pattern is considered a good predictor of favorable outcome in newborns (26). In addition, only half of HI+CBD piglets had significant seizures; a similar reduction of seizures occurs in HI piglets in response to high doses of the anticonvulsant topiramate (18). This finding is in line with previous reports that CBD is an anticonvulsant (6).
Finally, EEG studies also demonstrated a dramatic postinsult increase in impedance in HI+VEH, which indicates the presence of cerebral edema (28). Impedance increase starts as early as 10 min postHI and is strongly associated with poor neurologic outcome (28). Administration of CBD blunted this progressive increase in impedance. Progressing edema indicates a failure in brain capacity to reestablish cellular homoeostasis (28), being known as cytotoxic edema (20). Antiedema activity has been described for other cannabinoids after close brain injury (1), but to the best of our knowledge, no data on CBD exist.
The neuroprotective effect of CBD was confirmed by histology. In HI+VEH, the viable cell count was reduced to 57 and 34% of SHAM in cortex and hippocampus, respectively. Administration of CBD reduced HI-induced viable cell loss by 60% in cortex and by 50% in hippocampus. Also, CBD reduced the number of neurones undergoing degeneration in response to HI, as indicated by FJB staining; CBD administration reduced the number of FJB-positive cells observed after HI by 78% in cortex and 56% in hippocampus. Similar histologic protective effects have been reported in HI piglets treated with high-dose topiramate (18), but not with other neuroprotective substances such as the antioxidants deferoxamine or allopurinol (17).
We did not detect any side effects in piglets treated with CBD, supporting that CBD is essentially nontoxic and free from short- or long-term side effects (5–9). CBD at doses up to 5 mg/kg does not induce changes in blood pressure or ventilatory parameters in rodents (8,29), whereas in artificially ventilated anesthetized adult dogs CBD 1 mg/kg i.v decreases lung compliance and CO (6). Possibly because of the low dose of CBD used in our experiments or because of species- or age-related differences in extracerebral sensitivity to CBD, no negative hemodynamic or ventilatory effects were observed in HI+CBD. Instead, we observed significant beneficial extra cerebral effects. After HI, arterial pH fell because of poor peripheral circulation (20), returning to normal 3 h postinsult as reported previously (21). Normalization of arterial pH was quicker in HI+CBD, suggesting a beneficial effect of CBD on systemic circulation. This is supported by our finding that the dose of dopamine needed in HI+CBD to maintain MBP was less than half of that required in HI+VEH. In addition, CBD showed cardioprotective effects, as suggested by its effect on cTnT levels, a marker of myocardial damage after HI (20). Although myocardial ischemia was greater in the CBD than the VEH group, as indicated by the higher cTnT levels at drug administration, CBD blunted subsequent rises of cTnT at both 3 h and 6 h after HI. Protective effects of CBD against myocardial ischemic reperfusion injury have also been detected in adult rats (30). Mechanical ventilation progressively damaged piglet lung, as shown by the decrease in lung compliance observed in SHAM piglets throughout the experiment; a similar decrease was observed in HI+VEH. In HI+CBD, in contrast, lung compliance remained stable and Vt improved throughout the experiment. Although we did not analyze lung tissue because this was not an endpoint of the study, this effect of CBD could be attributed to its robust antiinflammatory effect (6). Thus, in HI+VEH, there was both a progressive increase in the OI, indicating a progressive impairment of oxygenation, and an increase in Paco2, indicating an impairment of ventilation. Consequently, it is likely that after HI, gas diffusion in the lung decreased over time, that this decrease occurred because the alveolar wall became progressively damaged by inflammation (31) and that CBD acted to reduce this inflammation. It is worth noting, however, that despite the aforementioned differences, hemodynamic or gasometrical parameters in HI+VEH and HI+CBD did not reach values known to modify CBF (20). Thus, these differences are unlikely to have a decisive influence on the neuroprotective effect of CBD.
In conclusion, administration of CBD after a HI insult in newborn piglets reduced short-term brain damage, in a manner that can be attributed to a CBD-induced reduction of cerebral hemodynamic impairment, improvement of brain metabolic activity postinsult, reduction of brain edema, and reduction of seizures. These neuroprotective effects were not only free from side effects but also associated with some cardiac, hemodynamic, and ventilatory benefits. Consequently, because other promising compounds with neuroprotective activity that have been tested in animals, for example topiramate or erythropoietin, have not displayed such extracerebral benefits (18,32), and because the simplicity and feasibility of administering CBD in the clinic has apparent advantages over more sophisticated and complex strategies such as hypothermia, we consider CBD to be a serious candidate for future clinical trials with asphyxiated newborns. However, before any clinical trials with humans are performed, it will be important to perform further experiments with piglets to establish an optimal dosing regimen for CBD and to characterize its long-term effects.
Abbreviations
- aEEG:
-
amplitude-integrated EEG
- CBD:
-
cannabidiol
- CBF:
-
cerebral blood flow
- CBV:
-
cerebral blood volume
- FJB:
-
FluoroJadeB staining
- FTOE:
-
fractional tissue oxygenation extraction
- HI:
-
hypoxia-ischemia
- NIRS:
-
near-infrared spectroscopy
- nTHI:
-
normalized total haemoglobin index
- OI:
-
oxygenation index
- Qcar:
-
common carotid artery flow
- VEH:
-
vehicle
- Vt:
-
lung tidal volume
References
Mechoulam R, Panikashvili D, Shohami E 2002 Cannabinoids and brain injury: therapeutic implications. Trends Mol Med 8: 58–61
Nagayama T, Sinor AD, Simon RP, Chen J, Graham SH, Jin K, Greenberg DA 1999 Cannabinoids and neuroprotection in global and focal cerebral ischemia and in neuronal cultures. J Neurosci 19: 2987–2995
Fernandez-Lopez D, Martinez-Orgado J, Nunez E, Romero J, Lorenzo P, Moro MA, Lizasoain I 2006 Characterization of the neuroprotective effect of the cannabinoid agonist WIN-55212 in an in vitro model of hypoxic-ischemic brain damage in newborn rats. Pediatr Res 60: 169–173
Fernandez-Lopez D, Pazos MR, Tolon RM, Moro MA, Romero J, Lizasoain I, Martinez-Orgado J 2007 The cannabinoid agonist WIN55212 reduces brain damage in an in vivo model of hypoxic-ischemic encephalopathy in newborn rats. Pediatr Res 62: 255–260
Braida D, Pegorini S, Arcidiacono MV, Consalez GG, Croci L, Sala M 2003 Post-ischemic treatment with cannabidiol prevents electroencephalographic flattening, hyperlocomotion and neuronal injury in gerbils. Neurosci Lett 346: 61–64
Pertwee RG 2004 The pharmacology and therapeutic potential of cannabidiol. Di Marzo V Cannabinoids. Kluwer Academic/Plenum Publishers, New York pp 32–83
Mishima K, Hayakawa K, Abe K, Ikeda T, Egashira N, Iwasaki K, Fujiwara M 2005 Cannabidiol prevents cerebral infarction via a serotonergic 5-hydroxytryptamine1A receptor-dependent mechanism. Stroke 36: 1077–1082
Hayakawa K, Mishima K, Nozako M, Hazekawa M, Irie K, Fujioka M, Orito K, Abe K, Hasebe N, Egashira N, Iwasaki K, Fujiwara M 2007 Delayed treatment with cannabidiol has a cerebroprotective action via a cannabinoid receptor-independent myeloperoxidase-inhibiting mechanism. J Neurochem 102: 1488–1496
Mechoulam R, Peters M, Murillo-Rodriguez E, Hanus LO 2007 Cannabidiol—recent advances. Chem Biodivers 4: 1678–1692
Marsicano G, Moosmann B, Hermann H, Lutz B, Behl C 2002 Neuroprotective properties of cannabinoids against oxidative stress: role of the cannabinoid receptor CB1. J Neurochem 80: 448–456
Esposito G, De Filippis D, Maiuri MC, De Stefano D, Carnuccio R, Iuvone T 2006 Cannabidiol inhibits inducible nitric oxide synthase protein expression and nitric oxide production in beta-amyloid stimulated PC12 neurons through p38 MAP kinase and NF-kappaB involvement. Neurosci Lett 399: 91–95
Ioroi T, Peeters-Scholte C, Post I, Leusink C, Groenendaal F, van Bel F 2002 Changes in cerebral haemodynamics, regional oxygen saturation and amplitude-integrated continuous EEG during hypoxia-ischaemia and reperfusion in newborn piglets. Exp Brain Res 144: 172–177
Gavilanes AW, Vles JS, von Siebenthal K, Reulen JP, Nieman FH, van Sprundel R, Blanco CE 2001 Electrocortical brain activity, cerebral haemodynamics and oxygenation during progressive hypotension in newborn piglets. Clin Neurophysiol 112: 52–59
Toet MC, Lemmers PM, van Schelven LJ, van Bel F 2006 Cerebral oxygenation and electrical activity after birth asphyxia: their relation to outcome. Pediatrics 117: 333–339
Nagdyman N, Fleck TP, Ewert P, Abdul-Khaliq H, Redlin M, Lange PE 2003 Cerebral oxygenation measured by near-infrared spectroscopy during circulatory arrest and cardiopulmonary resuscitation. Br J Anaesth 91: 438–442
Martinez-Orgado J, Fernandez-Frutos B, Gonzalez R, Romero E, Uriguen L, Romero J, Viveros MP 2003 Neuroprotection by the cannabinoid agonist WIN-55212 in an in vivo newborn rat model of acute severe asphyxia. Brain Res Mol Brain Res 114: 132–139
Peeters-Scholte C, Braun K, Koster J, Kops N, Blomgren K, Buonocore G, Buul-Offers S, Hagberg H, Nicolay K, van Bel F, Groenendaal F 2003 Effects of allopurinol and deferoxamine on reperfusion injury of the brain in newborn piglets after neonatal hypoxia-ischemia. Pediatr Res 54: 516–522
Schubert S, Brandl U, Brodhun M, Ulrich C, Spaltmann J, Fiedler N, Bauer R 2005 Neuroprotective effects of topiramate after hypoxia-ischemia in newborn piglets. Brain Res 1058: 129–136
Felix B, Leger ME, Albe-Fessard D, Marcilloux JC, Rampin O, Laplace JP 1999 Stereotaxic atlas of the pig brain. Brain Res Bull 49: 1–137
Volpe JJ 2001 Hypoxic-ischemic encephalopathy: clinical aspects. Volpe JJ Neurology of the Newborn. WB Saunders Co, Philadelphia pp 331–394
Tichauer KM, Brown DW, Hadway J, Lee TY, St Lawrence K 2006 Near-infrared spectroscopy measurements of cerebral blood flow and oxygen consumption following hypoxia-ischemia in newborn piglets. J Appl Physiol 100: 850–857
Bisogno T, Hanus L, De Petrocellis L, Tchilibon S, Ponde DE, Brandi I, Moriello AS, Davis JB, Mechoulam R, Di Marzo V 2001 Molecular targets for cannabidiol and its synthetic analogues: effect on vanilloid VR1 receptors and on the cellular uptake and enzymatic hydrolysis of anandamide. Br J Pharmacol 134: 845–852
Derdeyn CP, Videen TO, Yundt KD, Fritsch SM, Carpenter DA, Grubb RL, Powers WJ 2002 Variability of cerebral blood volume and oxygen extraction: stages of cerebral haemodynamic impairment revisited. Brain 125: 595–607
Peeters-Scholte C, van den Tweel E, Ioroi T, Post I, Braun K, Veldhuis W, Nicolay K, Groenendaal F, van Bel F 2002 Pharmacological interventions in the newborn piglet in the first 24 h after hypoxia-ischemia. A hemodynamic and electrophysiological perspective. Exp Brain Res 147: 200–208
Gavilanes AW, Vles JS, von Siebenthal K, van Sprundel R, Reulen JP, Blanco CE 2004 Neonatal electrocortical brain activity and cerebral tissue oxygenation during non-acidotic, normocarbic and normotensive graded hypoxemia. Clin Neurophysiol 115: 282–288
Shah DK, Lavery S, Doyle LW, Wong C, McDougall P, Inder TE 2006 Use of 2-channel bedside electroencephalogram monitoring in term-born encephalopathic infants related to cerebral injury defined by magnetic resonance imaging. Pediatrics 118: 47–55
Toet MC, Hellstrom-Westas L, Groenendaal F, Eken P, de Vries LS 1999 Amplitude integrated EEG 3 and 6 hours after birth in full term neonates with hypoxic-ischaemic encephalopathy. Arch Dis Child Fetal Neonatal Ed 81: F19–F23
Lingwood BE, Dunster KR, Healy GN, Ward LC, Colditz PB 2003 Cerebral impedance and neurological outcome following a mild or severe hypoxic/ischemic episode in neonatal piglets. Brain Res 969: 160–167
McQueen DS, Bond SM, Smith PJ, Balali-Mood K, Smart D 2004 Cannabidiol lacks the vanilloid VR1-mediated vasorespiratory effects of capsaicin and anandamide in anaesthetised rats. Eur J Pharmacol 491: 181–189
Durst R, Danenberg H, Gallily R, Mechoulam R, Meir K, Grad E, Beeri R, Pugatsch T, Tarsish E, Lotan C 2007 Cannabidiol, a nonpsychoactive Cannabis constituent, protects against myocardial ischemic reperfusion injury. Am J Physiol Heart Circ Physiol 293: H3602–H3607
Tollofsrud PA, Medbo S, Solas AB, Drevon CA, Saugstad OD 2002 Albumin mixed with meconium attenuates pulmonary dysfunction in a newborn piglet model with meconium aspiration. Pediatr Res 52: 545–553
Sola A, Wen TC, Hamrick SE, Ferriero DM 2005 Potential for protection and repair following injury to the developing brain: a role for erythropoietin?. Pediatr Res 2005: 110R–117R
Acknowledgements
The authors thank Carolina Herranz for excellent technical assistance.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supported by grants from FIS-PI060839 (F.J.A.), FIS-PI061085 (J.M.-O.), S-SAL/0261/2006 and SAF 2007–61565 (J.R.).
Rights and permissions
About this article
Cite this article
Alvarez, F., Lafuente, H., Carmen Rey-Santano, M. et al. Neuroprotective Effects of the Nonpsychoactive Cannabinoid Cannabidiol in Hypoxic-Ischemic Newborn Piglets. Pediatr Res 64, 653–658 (2008). https://doi.org/10.1203/PDR.0b013e318186e5dd
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/PDR.0b013e318186e5dd
This article is cited by
-
A narrative review of the therapeutic and remedial prospects of cannabidiol with emphasis on neurological and neuropsychiatric disorders
Journal of Cannabis Research (2024)
-
N-Methyl-D-aspartate (NMDA) and cannabinoid CB2 receptors form functional complexes in cells of the central nervous system: insights into the therapeutic potential of neuronal and microglial NMDA receptors
Alzheimer's Research & Therapy (2021)
-
Cannabidiol reduces withdrawal symptoms in nicotine-dependent rats
Psychopharmacology (2021)
-
Neuroprotective Effects of Cannabidiol Under Cerebral Ischemic Conditions
Revista Brasileira de Farmacognosia (2021)
-
Cannabidiol and Sports Performance: a Narrative Review of Relevant Evidence and Recommendations for Future Research
Sports Medicine - Open (2020)