Abstract
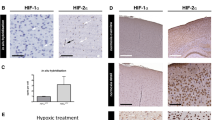
Oxidative stress is closely related to inflammation, a pathologic process characterized by activation of the transcriptional factor nuclear factor-kappa B (NF-κB). We have used transgenic NF-κB luciferase reporter mice to assess brain NF-κB activity noninvasively in living mice. We have studied NF-κB activation in hypoxic mice reoxygenated with either 21% O2 (room air) or 100% O2. Forty-one mice exposed for 2 h to 4% oxygen and then randomized to reoxygenation with pure oxygen or room air were investigated. A control mouse was dedicated to every mouse exposed to hypoxia. In vivo luminescence originated from brain was measured from mice 2 d before hypoxia, and 3 h after reoxygenation. A change in luminescence between the mouse exposed to hypoxia and its control demonstrates an alteration in NF-κB activity. Because of high mortality among males, only females were included. Six female mice died. Nineteen female mice were reoxygenated with room air, 16 with pure oxygen. We observed a significantly higher luminescence in the brain of the 100% O2 group versus the 21% O2 group. Our data indicate that brain NF-κB activity is increased in mice subjected to 4% oxygen followed by reoxygenation with 100% oxygen. However, when reoxygenation occurs with 21% O2 (room air), no elevation in NF-κB activity is observed. Thus, reoxygenation with room air may induce less brain inflammation than reoxygenation with pure oxygen.
Similar content being viewed by others
Main
In several pathologic conditions, such as brain edema, ischemia, traumatic brain injury, birth asphyxia, and circulatory arrest, oxygen delivery to the brain or specific brain regions may be compromised and severe hypoxic (Po2 < 0.1 kPa) or anoxic areas develop. Such interruption of oxygen delivery rapidly damages the metabolically active brain tissue. Paradoxically, restoration of blood flow to the hypoxic or anoxic tissues initiates a cascade of pathology that leads to additional cell or tissue injury. It is well documented that hypoxia/reoxygenation damage is a potent inducer of a number of inflammatory mediators (1).
The NF-κB transcription factors are known to be of utmost importance in orchestrating inflammatory responses. The NF-κB family includes a number of different proteins [p65 (RelA), p50, p52, RelB and c-Rel], which form homo- and heterodimers that are normally sequestered in the cytosol by a protein called IκB. Upon activation, IκB is phosphorylated and degraded, which, in turn, releases NF-κB, permitting translocation into the nucleus where it can bind to target sequences in DNA and activate transcription of specific genes (2–5).
Resuscitation after birth asphyxia is a common procedure that exposes the newborn child to more, or less, oxygen, depending on the protocol used. We have recently shown that resuscitation of hypoxic newborn piglets with pure oxygen induces inflammatory changes in the brain, heart, and the lungs (6,7). Hypoxic events in adults have also been shown to enhance inflammation through activated cytotoxic functions of the neutrophil cells (8). There is growing evidence indicating that room air is as safe in the resuscitation procedure of newborn infants as pure oxygen (9,10). Further, accumulating data indicate that pure oxygen may be disadvantageous, leading to not only an inflammatory response in the sensitive tissues of the newborn (6,7,11) but also a prolonged oxidative stress. The observed inflammation is believed to result from an oxidative burst as a consequence of too much oxygen delivered to the tissues (12).
To assess the NF-κB activation under various inflammatory conditions in vivo we have generated transgenic NF-κB reporter mice, which express luciferase under the control of NF-κB DNA binding sites, enabling noninvasive imaging of NF-κB activation in living animals. Following injection of the substrate D-luciferin into such mice, the cells that express the transgene (i.e. luciferase) will metabolize the substrate in a reaction that yields light. A sensitive CCD (charge-coupled device) camera is used to detect NF-κB activation as light escaping from various regions.
The aim of our study was to establish a mouse model of hypoxia and reoxygenation, and to use luciferase mice to study the effect of resuscitation with 21% or 100% oxygen on brain NF-κB activity.
METHODS
Hypoxia/reoxygenation.
A transparent plastic chamber measuring 30 × 30 × 40 cm, large enough for two small mouse cages, was used to expose the mice to hypoxia and reoxygenation. Gas introduced in the chamber was premixed by the gas company AGA (Oslo, Norway) in different concentrations of oxygen (8, 6, 5, and 4%) mixed with nitrogen and stored in 50-L bottles. The oxygen concentration was within a 5% mixing level and 1% analyzing level. Before entering the hypoxia/reoxygenation chamber, the gas passed through a heating and humidifier device (Respirator humidifier MR 730, Fisher & Paykel Healthcare, Greenmount, Auckland, New Zealand), keeping the temperature and the humidity nearly constant (23–25°C, 50–60%). Inside the chamber there were continuous measurements of oxygen concentration, carbon dioxide concentration, temperature, relative humidity, and dew point. Gas was evacuated through a long tube, keeping the pressure in the box at one atmosphere. The chamber was airtight and the gas concentrations were stable during the hypoxia period. Flow was set to maintain carbon dioxide concentration below 0.3%.
Animals.
We used female transgenic luciferase reporter mice for NF-κB activation, age 4–8 wk. The transgene contains three NF-kB binding sites from the Igκ-light chain promoter coupled to the gene encoding firefly luciferase. The transgene is flanked by insulator sequences from the chicken β-globin gene (13) to reduce interference from the genome. The resulting transgenic founder, which was the basis of these experiments, was the result of screening of several founders. The genetic background is an F2 mix of C57BL6/J and CBA. To every mouse exposed to hypoxia, we assigned one control mouse coming from the same litter. The control mouse was only exposed to room air. Differences in luciferase activity were compared between the hypoxia mouse and its control. For better detection of light emerging from the animals, fur was removed by shaving the backside of the skull and the ventral side of thorax and abdomen. At least 2 d before hypoxia, basal luminescence was recorded. Animals with a high basal luminescence (>2 SD above mean of all mice) were excluded. Such basal activity indicated a not controllable reason for NF-κB activation, such as an infection. All animal experiments were performed according to national guidelines for animal welfare, and approved by the Norwegian Animal Experimental Board.
In vivo imaging.
Mice were anesthetized with either hypnorm/dormicum (Jansen, Beerse, Belgium; Roche, Basel, Switzerland) or isoflurane (0.25 L/min; 2.5–3%) and placed in the light-tight imaging chamber, where anesthesia was maintained throughout the imaging session. The mice being exposed to hypoxia and their controls were always anesthetized and imaged at the same time and with the same type of anesthesia. Four milligrams (150 mg/kg) of the substrate D-luciferin (Biosynth, Staad, Switzerland) dissolved in 200 μL PBS, pH 7.8 was injected intraperitoneally to each mouse. Eight minutes later, photons were sampled from the ventral side during 4 min, followed by 4 min of exposure from the dorsal side. The imaging system used was IVIS-100 (Xenogen Corp., Alameda, CA). This system includes a CCD camera, an imaging chamber, a cryogenic refrigeration unit, a camera controller, and a computer with the necessary software, including Living Image (Xenogen Corporation, Alameda, CA) for image analysis. Photons emitted from a defined region of the mouse were expressed as photons/s/cm2/steradian. Changes in NF-κB activity were calculated after comparing, the differences of luminescence before and after hypoxia between the hypoxia mouse and its control. Figure 1 shows the same mouse imaged before and after exposure of 2 h of 4% hypoxia and 30 min of reoxygenation with 100% oxygen. The color scale is the same for the two pictures and reflects the amount of light emerging from the mouse. The colors of the picture to the left, marked “before 4% hypoxia,” show the basal luminescence reflecting the basal activity of NF-κB. The colors of the picture to the right, marked “after 4% hypoxia,” indicate an increased NF-κB activity. The Living Image software provides a numeric value by calculating the number of photons registered in a defined area.
Luminescence measurements in reporter mice for NF-κB activity. The figure shows two pictures of the same mouse imaged before and after exposure of two hours of 4% hypoxia and 30 minutes of reoxygenation with 100% oxygen. The color scale is the same for the two pictures and reflects the amount of light emerging from the mouse. The colors registered on the picture to the left, marked “before 4% hypoxia”, reflects the basal luminescence referring to the basal activity of the transcriptional factor NF-κB. The colors of the picture to the right marked “after 4% hypoxia”, indicates an increased NF-κB activity. The Living Image® software provides a numeric value by calculating the number of photons registered in a desired area.
Experimental model.
To establish a model of hypoxia/reoxygenation, 4–8-wk-old mice were exposed to different levels of 2 h hypoxemia: 8% (n = 6), 6% (n = 11), and 5% (n = 14) of oxygen mixed with nitrogen. All experiments started at about 8.00 h. On the first day of hypoxia, two or three mice were kept in a small mouse cage with free access to drinking water and food. The cage was placed in the air-tight chamber and hypoxia was introduced with air flow at 15 L per minute. Oxygen concentration in the chamber was constantly monitored and compared with previous experiments. Corrections were made to the gas flow to ensure stabilization at a desired oxygen level after approximately 15 min. When the desired oxygen concentration was reached, flow was reduced to a minimum, keeping the concentration of carbon dioxide below 0.3%. All mice were monitored by respiration rate during the hypoxemia session. After 2 h of hypoxia, the animals were reoxygenated for 30 min with pure oxygen.
A protocol of 4% oxygen was initiated with the same procedures as described. Forty-two transgenic, female mice were enrolled. Only female mice were used because of better survival. Exclusion criteria were extremely high basal luminescence, defined by more than 2 SD above the average luminescence of all mice measured (n = 61), and death during hypoxia. The mice were randomized to reoxygenation either by room air or by 100% oxygen. The randomization was performed by opening of one of initially 50 envelopes. When reoxygenating with room air, the cover of the air-tight chamber was removed, allowing room air to enter the box. Monitoring proved 21% oxygen to be established in the cage within 2 min. When reoxygenation was performed with 100% oxygen, the box was flushed with 15 L per minute during 10 min, by this time oxygen concentration in the box reached 98–100%. The flow was then reduced to 3 L/min, leaving an oxygen concentration >98% for 20 min. All control mice were monitored in their original cages. The mice were free to move in the cages, with access to drinking water and food. The monitoring was visual, counting the respiration rate, and recording the level of activity. Immediately after the hypoxia period, some mice were killed to measure the acid-base balance. The transcriptional factor NF-κB is rapidly activated, and the expressed luciferase reporter has a relatively short half life (t1/2 ~ 2–3 h) (14,15). In accordance with previous studies (16), we recorded luminescence 3 h after the end of reoxygenation. The luminescence was recorded in the mice exposed to hypoxia and in the controls at the same time.
Statistics.
Statistical analysis was performed with the SPSS for Windows (version 12.0.1, SPSS Inc., Chicago, IL). For evaluation of luminescence data, a Mann-Whitney U test was used to compare parameters form different groups of mice.
RESULTS
Respiration rate and acid base balance.
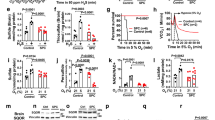
During the initial studies to establish the hypoxic model, mice were exposed to 8%, 6%, and 5% oxygen. Only the mice exposed to 5% oxygen were seriously affected. They all lay down, and breathed initially with a frequency of over 240 breaths per minute. Respiration frequency gradually decreased during hypoxia. Arterial pH in a selected number of mice (n = 12) immediately after the hypoxia period proved a strong correlation with respiration frequency by the end of hypoxia, with a Pearson's correlation of 0.8 (p < 0.01) (Fig. 2). Seven of these 12 mice had pH >7.3. In the protocol with 4% oxygen, all mice were visually and metabolically seriously affected. We found no correlation between respiration frequency and pH in the 4% group. Acid-base balance immediately after 2 h of 4% and 5% hypoxemia is presented in Table 1.
Mortality rate.
All mice exposed to 8%, 6%, or 5% oxygen for 2 h survived. Hypoxia with Fio2 of 4% resulted in an overall mortality of 27% (n = 97). Male mice had a mortality rate of 50% compared with 17% in females (p < 0.003).
Luciferase measurements.
Luciferase measurements are presented in Figure 3. Three groups were reoxygenated with pure oxygen 6% (n = 11), 5% (n = 17), and 4% (n = 16). Only the 4% oxygen group had significantly increased luminescence compared with the controls (p < 0.001).
Luciferase measurements after two hours of hypoxia and 30 minutes of reoxygenation. Luciferase measurements recorded from the brain in mice that have been exposed to two hours of hypoxia. After the hypoxia, the first three groups (6% (n = 11), 5% (n = 17), and 4% (n = 16)) were reoxygenated for 30 minutes with 100% oxygen. Only the 4% group proved a significant increase (p < 0.001). The last group (n=19) was exposed to 4% hypoxia, and reoxygenated with room air. There is a significant difference between the two groups exposed to 4% hypoxia indicating that NF-κB is more activated when pure oxygen is used for reoxygenation (p = 0.016).
In the protocol with 42 female mice exposed to 4% hypoxia and reoxygenated with either room air or pure oxygen, 1 mouse was excluded because of strong basal luminescence, and 6 others died during hypoxia. The room air study group and the 100% oxygen group comprised 19 and 16 mice, respectively. The results presented in Figure 3 reveal a significantly augmented level of luminescence in the group reoxygenated with pure oxygen compared with room air (p = 0.016). No increase was found in the room air group.
DISCUSSION
In this study of transgenic luciferase mice reporting the NF-κB activity, exposure to 8% or 6% oxygen and reoxygenation with 100% oxygen did not affect the mice much. Fio2 of 5% oxygen and reoxygenation with 100% oxygen affected most mice according to reduced physical activity, but there were large differences between the mice, both in activity and in acid-base balance immediately after the hypoxia period. Because of the strong correlation between the respiratory frequency and the pH balances, it would have been possible to consider only the mice most affected as detected by a low respiration rate. By choosing only the mice with respiration of less than 120 breaths per minute, mice with pH <7.2 could be sorted out. This procedure would have excluded three quarters of the study population exposed to 5% oxygen. However, with 4% oxygen, all mice were affected both physically and metabolically.
Mice exposed to 4% oxygen were studied with luciferase assessment from the brain, showing increased luminescence when 100% oxygen was used for reoxygenation. No such increase was found in animals reoxygenated with room air. This indicates that the transcriptional factor NF-κB was activated by pure oxygen by contrast to room air.
NF-κB is involved in numerous signaling pathways in the cells. Studies have proven high activity during normal mouse development (17) and in the control of neuronal survival and plasticity (18). Furthermore, it is an active mediator of inflammation, initiating the production of a number of cytokines necessary for the acute inflammatory process (2–5). NF-κB also plays an essential part in the development of chronic inflammatory diseases like asthma and inflammatory bowel disease (19,20). In our study, we have not directly measured any known markers of inflammation, but the increased NF-κB activity observed is most likely a response to the oxidative stress provoked in the mice. The increase in luminescence after hypoxia and reoxygenation was on average 2-fold. This corresponds to what has been observed when identical mice have been stimulated by well-known NF-κB inducers like tumor necrosis factor-α or lipopolysaccharide directly in the brain (H. Carlsen, unpublished results).
The measuring of luminescence was standardized with the IVIS system, delivering comparable numeric values. Emitted photons come from the whole mouse, but the fur blocks them and light emerging from deeper layers is not easily assessed, so only luminescence emerging from selected, shaved areas of the mouse can be assessed. From the back of the skull, we measured high luciferase activity. As the brain is located superficially, is easily demarked from surrounding tissue, and because os cranii has minor luciferase activity (data not shown), the luminescence measured from the head most probably reflects luciferase activity predominantly from the brain. Control measurements of NF-κB activity in brain tissue homogenates show large individual variations, and we did not find differences among the groups studied. The luciferase method of measuring NF-κB activity enables several measurements of the same animal and is suitable for detecting relative changes in activity. To further reduce the effect of fluctuations in NF-κB activity, we assigned a control mouse among one of the sisters of the hypoxia mouse. Because of these measures taken to reduce unknown factors in our model, we believe the luciferase method is the better of the two in detecting changes in NF-κB activity.
There was no mortality until reaching a 4% level of hypoxia. This is less than reported by other groups, which found that half of the mice died after 10 min in 5% oxygen, and 100% died after less than 200 s in 4% oxygen (21–23). We exposed mice to 2 h of 4% oxygen concentration and registered an overall mortality of 27%. In agreement with others (23–25), we registered a marked difference between genders. The mouse strain and level of stress are other factors that impact on survival. The mice were calmer when they recognized the examiner based on several exposures. If mice from different cages were put together, or if there were too many mice in the cage, stress was apparent, and the outcome was worse. If the oxygen concentration was brought down to the desired level too quickly, more mice died. The experiments were therefore strictly standardized; the hypoxic gas was introduced slowly, using 15 min to establish the desired level of hypoxia, and stress was reduced to a minimum.
In this study, we performed luminescence measurements on sedated animals. The measurements were gentle, with no more demands than a shaving and a 15-min anesthesia, which is standardized with isoflurane gas. The procedure can be performed repeatedly, making it possible to monitor an inflammatory response over several days.
There is growing evidence that the use of 100% oxygen worsens the outcome after resuscitating sick newborn infants (26–28). Our findings indicate that tissue exposed to hypoxia may be further damaged if exposed to pure oxygen immediately after hypoxia. It should be specifically noted that we have recorded changes occurring in the brain only. All cells have the ability to produce NF-κB, both in newborn and adult animals (29). Our study was performed on adult mice (4–8 wk), and care must be taken to apply the results to resuscitation procedures in neonates.
With the use of this hypoxia model it is possible to study therapeutic approaches in mice exposed to hypoxia and reoxygenation. Because reactive oxygen species (ROS) can cause oxidative damage, and pure oxygen is a source of ROS, it is possible to test the efficacy of different antioxidants in this mouse model. This model also allows studies of toxicity of different oxygen concentrations during reoxygenation.
CONCLUSION
We have established a model exposing mice to extreme levels of hypoxia. With transgenic reporter mice for NF-κB activity we have proven an induction when pure oxygen is used for reoxygenation after hypoxia, in contrast to room air.
Abbreviations
- IκB:
-
inhibitor kappa B
- NF-κB:
-
nuclear factor-kappa B
References
Ishibashi N, Prokopenko O, Reuhl KR, Mirochnitchenko O 2002 Inflammatory response and glutathione peroxidase in a model of stroke. J Immunol 168: 1926–1933
Li ZW, Rickert RC, Karin M 2004 Genetic dissection of antigen receptor induced-NF-kappaB activation. Mol Immunol 41: 701–714
Ghosh S, May MJ, Kopp EB 1998 NF-kappa B and Rel proteins: evolutionarily conserved mediators of immune responses. Annu Rev Immunol 16: 225–260
Ghosh S, Karin M 2002 Missing pieces in the NF-kappaB puzzle. Cell 109( suppl): S81–S96
Senftleben U, Karin M 2002 The IKK/NF-kappaB pathway. Crit Care Med 30: S18–S26
Munkeby BH, Borke WB, Bjornland K, Sikkeland LI, Borge GI, Halvorsen B, Saugstad OD 2004 Resuscitation with 100% O2 increases cerebral injury in hypoxemic piglets. Pediatr Res 56: 783–790
Borke WB, Munkeby BH, Halvorsen B, Bjornland K, Tunheim SH, Borge GI, Thaulow E, Saugstad OD 2004 Increased myocardial matrix metalloproteinases in hypoxic newborn pigs during resuscitation: effects of oxygen and carbon dioxide. Eur J Clin Invest 34: 459–466
Tamura DY, Moore EE, Partrick DA, Johnson JL, Offner PJ, Silliman CC 2002 Acute hypoxemia in humans enhances the neutrophil inflammatory response. Shock 17: 269–273
Saugstad OD, Rootwelt T, Aalen O 1998 Resuscitation of asphyxiated newborn infants with room air or oxygen: an international controlled trial: the Resair 2 study. Pediatrics 102: e1
Ramji S, Rasaily R, Mishra PK, Narang A, Jayam S, Kapoor AN, Kambo I, Mathur A, Saxena BN 2003 Resuscitation of asphyxiated newborns with room air or 100% oxygen at birth: a multicentric clinical trial. Indian Pediatr 40: 510–517
Vento M, Asensi M, Sastre J, Lloret A, Garcia-Sala F, Minana JB, Vina J 2002 Hyperoxemia caused by resuscitation with pure oxygen may alter intracellular redox status by increasing oxidized glutathione in asphyxiated newly born infants. Semin Perinatol 26: 406–410
Saugstad OD 2003 Bronchopulmonary dysplasia-oxidative stress and antioxidants. Semin Neonatol 8: 39–49
Bell AC, West AG, Felsenfeld G 1999 The protein CTCF is required for the enhancer blocking activity of vertebrate insulators. Cell 98: 387–396
Ignowski JM, Schaffer DV 2004 Kinetic analysis and modeling of firefly luciferase as a quantitative reporter gene in live mammalian cells. Biotechnol Bioeng 86: 827–834
Thompson JF, Hayes LS, Lloyd DB 1991 Modulation of firefly luciferase stability and impact on studies of gene regulation. Gene 103: 171–177
Carlsen H, Moskaug JO, Fromm SH, Blomhoff R 2002 In vivo imaging of NF-kappa B activity. J Immunol 168: 1441–1446
Schmidt-Ullrich R, Memet S, Lilienbaum A, Feuillard J, Raphael M, Israel A 1996 NF-kappaB activity in transgenic mice: developmental regulation and tissue specificity. Development 122: 2117–2128
Mattson MP, Culmsee C, Yu Z, Camandola S 2000 Roles of nuclear factor kappaB in neuronal survival and plasticity. J Neurochem 74: 443–456
Desmet C, Gosset P, Pajak B, Cataldo D, Bentires-Alj M, Lekeux P, Bureau F 2004 Selective blockade of NF-kappa B activity in airway immune cells inhibits the effector phase of experimental asthma. J Immunol 173: 5766–5775
Hollenbach E, Neumann M, Vieth M, Roessner A, Malfertheiner P, Naumann M 2004 Inhibition of p38 MAP kinase- and RICK/NF-kappaB-signaling suppresses inflammatory bowel disease. FASEB J 18: 1550–1552
Endoh H, Taga K, Yamakura T, Sato K, Watanabe I, Fukuda S, Shimoji K 1999 Effects of naloxone and morphine on acute hypoxic survival in mice. Crit Care Med 27: 1929–1933
Sato Y, Kitani K, Kanai S, Nokubo M, Ohta M 1991 Differences in tolerance to hypoxia/anoxia in mice of different ages. Res Commun Chem Pathol Pharmacol 73: 209–220
Saiyed M, Riker WK 1993 Cholinergic and anticholinergic drug effects on survival during hypoxia: significant gender differences. J Pharmacol Exp Ther 264: 1146–1153
Vannucci SJ, Willing LB, Goto S, Alkayed NJ, Brucklacher RM, Wood TL, Towfighi J, Hurn PD, Simpson IA 2001 Experimental stroke in the female diabetic, db/db, mouse. J Cereb Blood Flow Metab 21: 52–60
Knoferl MW, Jarrar D, Schwacha MG, Angele MK, Cioffi WG, Bland KI, Chaudry IH 2000 Severe hypoxemia in the absence of blood loss causes a gender dimorphic immune response. Am J Physiol Cell Physiol 279: C2004–C2010
Saugstad OD, Ramji S, Vento M 2005 Resuscitation of depressed newborn infants with ambient air or pure oxygen: a meta-analysis. Biol Neonate 87: 27–34
Tan A, Schulze A, O'Donnell CP, Davis PG 2004 Air versus oxygen for resuscitation of infants at birth. Cochrane Database Syst Rev CD002273
Davis PG, Tan A, O'Donnell CP, Schulze A 2004 Resuscitation of newborn infants with 100% oxygen or air: a systematic review and meta-analysis. Lancet 364: 1329–1333
Karin M, Ben Neriah Y 2000 Phosphorylation meets ubiquitination: the control of NF-[kappa]B activity. Annu Rev Immunol 18: 621–663
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was supported by grants from the Norwegian Research Council, the Norwegian Cancer Society, the Johan Throne Holst Foundation, the National Hospital of Norway, and the University of Oslo. Xenogen Corp. (Alameda, CA) generously supported the work by providing the IVIS-100 imaging system.
Rights and permissions
About this article
Cite this article
Døhlen, G., Carlsen, H., Blomhoff, R. et al. Reoxygenation of Hypoxic Mice with 100% Oxygen Induces Brain Nuclear Factor-kappa B. Pediatr Res 58, 941–945 (2005). https://doi.org/10.1203/01.PDR.0000182595.62545.EE
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/01.PDR.0000182595.62545.EE
This article is cited by
-
Real-Time Noninvasive Bioluminescence, Ultrasound and Photoacoustic Imaging in NFκB-RE-Luc Transgenic Mice Reveal Glia Maturation Factor-Mediated Immediate and Sustained Spatio-Temporal Activation of NFκB Signaling Post-Traumatic Brain Injury in a Gender-Specific Manner
Cellular and Molecular Neurobiology (2021)
-
Extracellular mtDNA activates NF-κB via toll-like receptor 9 and induces cell death in cardiomyocytes
Basic Research in Cardiology (2016)
-
Making the Brain Glow: In Vivo Bioluminescence Imaging to Study Neurodegeneration
Molecular Neurobiology (2013)
-
Diet-induced obesity increases NF-κB signaling in reporter mice
Genes & Nutrition (2009)
-
Brief Exposure to Hyperoxia Depletes the Glial Progenitor Pool and Impairs Functional Recovery after Hypoxic-Ischemic Brain Injury
Journal of Cerebral Blood Flow & Metabolism (2008)