Abstract
Immunologic consequences of exposure to HIV-1 in utero are still poorly understood. This study investigates relationships between type-1 [interferon-γ (IFN-γ)] and type-2 (IL-10) cytokine production and maternal-infant HIV-1 transmission. Cord blood leukocytes from deliveries of 71 HIV-1–infected and 11 uninfected mothers were tested for in vitro IFN-γ and IL-10 production after phytohemagglutinin (PHA) stimulation. The infants of these HIV-1–infected mothers were followed prospectively after birth to determine HIV vertical transmission, and IFN-γ and IL-10 production was measured again at 6 mo. Median PHA-stimulated IFN-γ production was 210 pg/mL in cord blood cells from infected and 73 pg/mL from uninfected mothers (p = 0.12), and median PHA-stimulated IL-10 production was 491 pg/mL in cord blood cells from infected and 161 pg/mL from uninfected mothers (p = 0.004). PHA-stimulated IFN-γ and IL-10 production alone were not significantly associated with transmission, but relationships between the two cytokines differed among infected and uninfected infants of HIV-1–infected mothers. PHA-stimulated IFN-γ and IL-10 production was positively correlated among infected (r = 0.7, p = 0.12 in cord blood and r = 0.66, p = 0.03 at 6 mo) but not uninfected infants, and stronger relative production of IFN-γ to IL-10 was observed among exposed uninfected than among infected infants (p = 0.04). Exposure in utero to HIV-1 may augment production of IL-10 detectable in fetal cord blood. Stronger relative production of IFN-γ to IL-10 in cord blood cells from infants of HIV-1–infected mothers may be associated with protection against perinatal HIV infection.
Similar content being viewed by others
Main
Most infants of HIV-1–infected mothers do not acquire HIV-1 infection themselves. Protection from maternal-infant HIV-1 transmission is associated with less advanced maternal disease, particularly lower maternal viral loads (1), antiretroviral treatment (2), cesarean delivery before rupture of membranes (3), and absence of breast-feeding (4). The most likely explanation for the benefits of these factors is reduction in the duration or dose of viral exposure, although other mechanisms may also be involved.
Less well elucidated are fetal and neonatal host factors that may be critical for protection against vertical transmission upon viral exposure. More than a third of uninfected infants of HIV-1–infected mothers elicit memory helper T-cell responses to HIV-1 peptides at birth, and these cell-mediated responses have been correlated with protection from perinatal infection (5–7). Helper T-cell responses to HIV-1 have also been observed in uninfected adult populations sexually exposed to HIV-1 (8, 9), including those repeatedly exposed and thought to be resistant (10). HIV-1–specific CTL responses have also been observed in uninfected adults exposed to HIV-1 (11, 12). However, HIV-specific CTL responses are more difficult to elicit in infants but have been detected in some uninfected infants of infected mothers (13–18). The reports that protection against both maternal-infant (19) and sexual transmission in female sex workers (20) is associated with HLA class I and II alleles suggest that HLA complex will also contribute to protection. Overall, the balance of evidence supports the notion that acquired cellular, rather than humoral, immune responses (at least at a systemic level) are needed for protective immunity to HIV-1. Other processes may be operational at local mucosal sites (9).
Development of a strong cellular response to an antigen is influenced by the cytokine milieu. Type-1 cytokines, including IFN-γ, IL-2, and IL-12, enhance the development of cellular responses, whereas type-2 cytokines, including IL-4, IL-5, IL-6, and IL-10, stimulate humoral responses (21). Hence, we hypothesized that type-1 predominance in cytokine production may be one of the factors associated with protection from HIV-1 infection in HIV-1–exposed populations, including infants of HIV-1–infected mothers. In this study, we investigated whether IFN-γ (type 1) and IL-10 (type 2) production in cord blood of infants of HIV-1–infected mothers would predict which infants were subsequently found to have acquired infection and which were not.
METHODS
Study population.
The mother-child pairs included in this study were participants in a randomized clinical trial of vitamin A supplementation that is described in more detail elsewhere (22, 23). In brief, HIV-1–seropositive women attending prenatal clinics at two hospitals in Durban, South Africa, were recruited with written informed consent during pregnancy. Women were counseled about the risks of breast-feeding transmission and about the health risks of formula-feeding and were encouraged to make an informed choice. No woman in the study was treated with antiretroviral therapy. This study was done before the results of the short-course antiretroviral drug trials were available. The study was approved by the Institutional Review Boards of the University of Natal and Columbia University.
Samples collected.
As part of the clinical trial protocol, a maternal blood sample was drawn at enrollment for CD4+ and CD8+ T-lymphocyte counts and for quantification of HIV-1 RNA in plasma. Neonatal and obstetric information was recorded at delivery. Mother-child pairs were followed after delivery with regular clinical examinations. Venous blood was drawn from infants on the day of birth, at 1 wk, 6 wk, and 3 mo of age and thereafter every 3 mo until 18 mo for HIV-1 diagnostic tests. If children were breast-fed beyond 15 mo, an additional sample was drawn at least 3 mo after complete cessation of breast-feeding.
Over a specified period of time, cord blood was collected when possible depending on staff availability from the clinical trial participants. Cord blood was collected by cordocentesis to avoid maternal contamination immediately after delivery of the placenta. Cytokine production was measured in cord blood samples and in venous blood samples collected from infants at 6 mo of age if sufficient sample remained after the sample for the HIV-1 diagnostic tests had been prepared. All blood samples were drawn into ethylenediamine tetraacetate tubes. Cord blood was also collected from a sample of infants of HIV-seronegative women as controls, but these infants were not followed after birth. Sample volumes were not sufficient to complete in vitro cytokine measurement on all samples. The number of samples included in each analysis is recorded in “Results.”
In vitro IFN-γ and IL-10 production.
Within 24 h of sample collection, mononuclear cells were separated on Ficoll-Hypaque, washed twice in PBS, and the number of viable leukocytes determined by trypan blue exclusion. Cells were resuspended at 3 × 106/mL in RPMI 1640 containing 100 U/mL penicillin and 2 mM glutamine. Three × 106 cells in suspension were placed in flat-bottom wells of a microtiter culture plate. For each sample, stimulated and unstimulated (control) wells were set up in triplicate. PHA at a final concentration of 1:100 was used as the stimulus. Pooled human plasma was added to each well an hour after sensitization. The cells were cultured at 37°C in a moist 7% CO2 atmosphere for 48 h. Culture supernatants were harvested, frozen, and stored at −20°C until assayed for IFN-γ and IL-10 production. Cytokine production was measured using commercially available ELISA assays for human IFN-γ and IL-10 (R&D Systems, Minneapolis, MN, U.S.A.) run according to the manufacturer's instructions. The numerical value for the amount of cytokine was calculated from the standard curve. For all statistical analyses, the level of stimulated IFN-γ and IL-10 was estimated by subtracting from the stimulated value the unstimulated value (truncated to 0 if unstimulated exceeded stimulated values).
Determination of infant HIV-1 status.
Plasma from infant samples collected at 6 mo or younger was tested for HIV-1 RNA using PCR (Roche Molecular Systems, Branchburg, NJ, U.S.A.) with an analytic limit of detection of ∼10 RNA copies (approximately 400 copies/mL). Samples collected at older ages were tested for HIV-1 antibody (Abbott Laboratories, Chicago, IL, U.S.A.). Infants with at least one positive PCR test were classified as HIV-1 infected. All children classified as infected in this study, except one who was lost to follow-up, tested PCR positive on two or more different specimens. Cord blood was not used for HIV diagnosis. Infants testing negative on their last available sample and who had no positive PCR results were classified as uninfected. Infected children were further stratified into those presumed to have acquired infection intrauterine if the PCR test on their venous blood sample collected on the day of birth was positive, those presumed to have acquired infection intrapartum or during the early postnatal period if the PCR test on the day of birth was negative but was positive by 6 wk of age, and those presumed to have acquired infection during the late postnatal period through breast-feeding if the PCR at 6 wk was negative but was positive at older ages.
Statistical methods.
Nonparametric statistics were used throughout because IFN-γ and IL-10 levels were not normally distributed. Differences in IFN-γ and IL-10 levels were tested using the Mann-Whitney U test for 2-group comparisons or the Kruskal-Wallis test for greater than 2-group comparisons. Differences between cord blood and 6-mo results were tested with a paired Wilcoxon signed rank test. Spearman's rank correlation coefficient was used to estimate associations between IFN-γ and IL-10 production. Proportions with IFN-γ and IL-10 levels above threshold levels were tested using the χ2 test. All p values were 2-sided.
RESULTS
Infants of HIV-1–infected and uninfected mothers.
The median level of PHA-stimulated IFN-γ measured was 210 pg/mL (25th–75th percentile, 17–1479) in cord blood leukocytes of 71 infants of HIV-1–infected mothers compared with 73 pg/mL (2–196) among 11 infants of uninfected mothers, but this trend did not reach significance (p = 0.12). PHA-stimulated IFN-γ production in cord blood cells ranged from 0 to more than 500,000 pg/mL among the infants of HIV-1–infected mothers, with 18 (25.4%) having levels above 1396 pg/mL—the maximum value observed in the infants of uninfected mothers (p = 0.059). PHA-stimulated IL-10 production was significantly higher (p = 0.004) in cord blood leukocytes from 70 infants of HIV-1–infected mothers (median, 491 pg/mL) than among 11 controls (median, 161 pg/mL) (Table 1). After excluding HIV-infected infants, significantly higher levels of PHA-stimulated IL-10 (p = 0.004) production in cord blood cells was observed among uninfected infants of HIV-infected mothers than among uninfected infants of uninfected mothers.
HIV-1–infected and uninfected infants of HIV-1–infected mothers.
PHA-stimulated IFN-γ production in cord blood leukocytes was not statistically significantly different among seven infants later established to be infected and 62 uninfected infants (p = 0.27), although median levels tended to be higher in the uninfected (217 pg/mL) than in the infected group (89 pg/mL). Two of the seven infected infants were presumed to have acquired infection intrauterine because they had detectable HIV-1 RNA in peripheral blood samples collected on the day of birth. The other five were presumed to have acquired infection intrapartum or during the early postnatal period: four had positive PCR results by 6 wk of age, and one was negative at 6 wk but positive when next tested at 3 mo. PHA-stimulated IL-10 production in cord blood cells was similar among eight infected (median, 653 pg/mL) and 60 uninfected (median, 491 pg/mL) infants of HIV-infected mothers (p = 0.96) (Table 1).
HIV-1–infected and uninfected infants at 6 mo.
Quantities of PHA-stimulated IFN-γ production in PBMC collected at 6 mo of age among the cohort of infants of HIV-1–infected mothers were similarly high to quantities observed in cord blood cells (p = 0.85), but quantities of IL-10 production had significantly declined at 6 mo (p = 0.001) (Table 1).
No significant differences in PHA-stimulated IFN-γ or IL-10 production in PBMC from infected and uninfected infants of HIV-infected mothers at 6 mo of age were observed (Table 1). One child with 6-mo cytokine results of the 12 who were classified as infected was PCR negative at 6 mo but positive when retested at 7 mo. The others had tested PCR positive on samples collected at ages younger than 6 mo. No significant differences were observed in PHA-stimulated IFN-γ or IL-10 production in PBMC between breast-fed and never breast-fed children, but numbers of nonbreast-fed children were small.
Correlation between IFN-γ and IL-10 production.
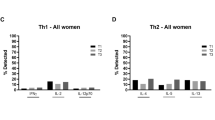
The relationship between PHA-stimulated IFN-γ production and IL-10 production in cord blood cells differed among HIV-infected and uninfected infants. In cord blood cells, production of these two cytokines was positively correlated among six infected infants of HIV-1–infected mothers with both cytokines measured (r = 0.7, p = 0.12), i.e. individuals with high IFN-γ production in vitro after PHA stimulation tended to have high IL-10 production and individuals with low IFN-γ production had low IL-10 production. However, no association between production of the two cytokines was observed among 58 uninfected infants (r = 0.06, p = 0.66) with these two cytokines measured in cells from the same blood specimen. A similar pattern was observed at 6 mo:r = 0.66, p = 0.028 among 11 infected and r = 0.27, p = 0.083 among 44 uninfected (Fig. 1). No correlation between IFN-γ and IL-10 production in cord blood cells was observed among control infants of HIV-seronegative mothers (r = 0.08, p = 0.821).
Scatterplot of IFN-γ and IL-10 production after stimulation with PHA in cord blood cells or in PBMC at 6 mo of age among infected (solid dots) and uninfected (open dots) infants of HIV-infected mothers. The lines indicate the best-fitting lines through the data points based on a linear regression model among the infected (solid line) and the uninfected (dashed line) infants. (A) Cord blood results; (B) venous blood at 6 mo.
Relative production of IFN-γ to IL-10.
Because a predominant type-1 cytokine milieu supportive of cell-mediated immunity may depend not only on individual cytokine production but also on relative production of type-1 to type-2 cytokines, we also investigated the relative production of IFN-γ to IL-10. Relative production was measured by calculating the ratio of PHA-stimulated IFN-γ:IL-10 production. The number 1 was added to the cytokine quantity to avoid division by 0. Among infants of HIV-1–infected mothers, the ratio of PHA-stimulated IFN-γ to IL-10 production in cord blood cells was higher (median = 0.563, 25th–75th percentile, 0.08–2.80) in those 58 infants who escaped infection compared with those six who acquired infection (median = 0.16, 25th–75th percentile, 0.002–0.808). Two of the six were presumed intrauterine infections and four intrapartum or early postnatal infections. Cord blood cells from none of the six infants of HIV-1–infected mothers who became infected produced more IFN-γ than IL-10 in vitro after PHA stimulation, whereas 25/58 (43.1%) of the uninfected infants did (p = 0.04).
Association of vertical transmission with maternal HIV RNA levels.
The quantity of maternal HIV-1 RNA in plasma was significantly higher among infants who acquired infection than among those who remained uninfected (p = 0.002). Maternal viral load did not, however, appear to explain any associations with the cytokines measured because HIV-1 RNA copy numbers did not correlate with in vitro production of PHA-stimulated IFN-γ, IL-10, or the ratio of these two cytokines in cord blood cells of infants of HIV-infected mothers.
DISCUSSION
We observed elevated levels of IL-10 production in response to mitogen stimulation in cord blood leukocytes from infants of HIV-1–infected mothers compared with infants from uninfected control mothers. Levels of IFN-γ tended to be elevated, too, but did not reach significance. Elevations could not be explained by HIV-1 infection per se among the infants and were observed among the majority of infants of HIV-1–infected mothers who did not themselves acquire infection. Elevations in IL-10 production among the HIV-exposed infants declined by 6 mo of age. These results suggest that the intrauterine experience with an HIV-1–infected mother may be associated with augmented IL-10 (and possibly IFN-γ) production detectable in fetal cord blood. A limitation of our study is the small control group. Hence, we are unable to definitively rule out conditions other than HIV that may account for these differences. However, the control group was an unselected sample of uninfected women delivering at the same hospital during the same period and from the same communities as the HIV-1–infected women.
These results are consistent with other studies that have observed immunologic changes in newborns exposed to HIV in utero. A recent study reported reduced Staphylococcus aureus Cowan (SAC)-stimulated IL-12 production by cord blood from uninfected deliveries of HIV-infected mothers, demonstrating the influence of the HIV-infected maternal environment on in utero immunologic development (24). Another study reported increased proportions of activated (HLA-DR+ CD38+) and memory (CD45RA- RO+) CD4+ T lymphocytes among uninfected infants of HIV-1–infected mothers compared with infants of uninfected mothers (25). Antigen stimulation in utero may decrease the pool of naive lymphocytes enhancing cytokine production in the newborn.
The relative production of IFN-γ to IL-10 appeared to be associated with maternal-infant HIV-1 transmission rather than the independent production of either cytokine alone. In the infected, IFN-γ and IL-10 production was positively correlated, i.e. either both high or both low production of the two cytokines tended to occur together in the same individual. No infant subsequently found to be infected produced more IFN-γ than IL-10 after PHA stimulation regardless of maternal viral load, whereas 43% of uninfected infants did. These results are consistent with the hypothesis that the failure to establish a polarized type-1 response is associated with an increased risk of transmission. Although fully mature type-1 responses can be achieved in neonates, neonatal T cells tend to be poor producers of type-1 cytokines under neutral conditions (26, 27). More costimulation and augmentation of antigen-presenting cell function, which tends to be immature in fetal cord blood, are necessary to achieve vigorous type-1 responses in newborns (26, 27). Further understanding of the conditions promoting robust type-1 responses is critical to elucidating protective immunity to HIV-1 among infants of HIV-1–infected mothers.
Type-1 and type-2 cytokine production has been investigated in several studies of HIV-1–infected children, mostly to consider associations with disease progression (28–32). Similar to studies in adults, progression of pediatric HIV-1–infection tends to be associated with declines in type-1 cytokines and elevations in type-2 cytokines, although these profiles are not consistently observed depending on the methods used to measure cytokine production (28–32). Even if type-1 predominance can be shown to be associated with slower disease progression among infected children, it does not necessarily follow that a nonspecific type-1 predominance will help protect against infection in the first place. Given the dynamic changes in cytokine production that occur over time among infected children, it is difficult on the basis of these previous studies (even those that included some samples from uninfected infants of HIV-1–infected mothers) to make any inferences about transmission. A strength of our study is that samples from both infected and uninfected children were collected at the same ages and that all the offspring of HIV-1–infected mothers were followed prospectively to determine transmission. However, we cannot rule out that the associations we observed are secondary to HIV-1 infection rather than relevant to transmission because we had insufficient numbers of cord blood samples from study subjects who acquired infection intrapartum or during the postnatal period to consider these subgroups separately. An inherent difficulty in studying immunologic factors associated with vertical transmission is that immunologic data need to be collected before transmission occurs because HIV infection itself has multidimensional immunologic consequences.
Our findings suggest intrauterine exposure to HIV-1 may result in detectable increases in IL-10 production after PHA stimulation in fetal cord blood leukocytes and suggest that, among infants of HIV-1–infected mothers, greater IFN-γ production relative to IL-10 production in cord blood leukocytes after PHA stimulation may be associated with lack of HIV infection. These findings are consistent with that observed in a study of adult i.v. drug users who were known to have shared needles with HIV-infected partners but who, despite intensive follow-up for many years, remained seronegative. Among this high-risk exposed uninfected population, increased PHA-stimulated IFN-γ production in PBMC and decreased IL-4 and IL-10 production were observed (33). Further study of a wider range of type-1 and type-2 cytokines and of chemokines and their associations with HIV-specific cell-mediated immune responses is needed to clarify these relationships. Better understanding of the spectrum of immune responses that may occur after HIV-1 exposure among individuals who do not themselves develop a chronic HIV infection may assist the development of an effective HIV-1 vaccine. Uninfected infants of HIV-1–infected mothers are a special case of such an exposed uninfected population and are an important group to study to better understand processes of natural immunity to HIV.
Abbreviations
- IFN-γ:
-
interferon-γ
- PHA:
-
phytohemagglutinin
- CTL:
-
cytotoxic T lymphocyte
- PBMC:
-
peripheral blood mononuclear cells
References
Cao Y, Krogstad P, Korber BT, Koup RA, Muldoon M, Macken C, Song JL, Jin Z, Zhao JQ, Clapp S, Chen IS, Ho DD, Ammann AJ 1997 Maternal HIV-1 viral load and vertical transmission of infection: the Ariel Project for the prevention of HIV transmission from mother to infant. Nat Med 3: 549–552
Connor EM, Sperling RS, Gelber R, Kiselev P, Scott G, O'Sullivan MJ, VanDyke R, Bey M, Shearer W, Jacobson RL, Jimenez E, O'Neill E, Bazin B, Delfraissy JF, Culnane M, Coombs R, Elkins M, Moye J, Stratton P, Balsley J 1994 Reduction of maternal-infant transmission of human immunodeficiency virus type 1 with zidovudine treatment. N Engl J Med 331: 1173–1180
International Perinatal HIV Group 1999 The mode of delivery and the risk of vertical transmission of human immunodeficiency virus type 1: a meta-analysis of 15 prospective cohort studies. N Engl J Med 340: 977–987
Dunn DT, Newell ML, Ades AE, Peckham CS 1992 Risk of human immunodeficiency virus type 1 transmission through breastfeeding. Lancet 340: 585–588
Clerici M, Sison AV, Berzofsky JA, Rakusan TA, Brandt CD, Ellaurie M, Villa ML, Colie C, Venzon DJ, Sever JL, Shearer GM 1993 Cellular immune factors associated with mother-to-infant transmission of HIV. AIDS 7: 1427–1433
Wasik TJ, Bratosiewicz J, Wierzbicki A, Whiteman VE, Rutstein RR, Starr SE, Douglas SD, Kaufman D, Sison AV, Polansky M, Lischner HW, Kozbor D 1999 Protective role of beta-chemokines associated with HIV-specific Th responses against perinatal HIV transmission. J Immunol 162: 4355–4364
Kuhn L, Coutsoudis A, Moodley D, Trabattoni D, Mngqundaniso N, Shearer GM, Clerici M, Coovadia HM, Stein Z 2001 T-helper cell responses to HIV envelope peptides in cord blood: protection against intrapartum and breast-feeding transmission. AIDS 15: 1–9
Clerici M, Giorgi JV, Chou CC, Gudeman VK, Zack JA, Gupta P, Ho HN, Mishanian PG, Berzofsky JA, Shearer GM 1992 Cell-mediated immune response to human immunodeficiency virus (HIV) type 1 in seronegative homosexual men with recent sexual exposure to HIV-1. J Infect Dis 165: 1012–1019
Mazzoli S, Trabattoni D, Lo Caputo S, Piconi S, Ble C, Meacci F, Ruzzante S, Salvi A, Semplici F, Longhi R, Fusi ML, Tofani N, Biasin M, Villa ML, Mazzotta F, Clerici M 1997 HIV-specific mucosal and cellular immunity in HIV-seronegative partners of HIV-seropositive individuals. Nat Med 3: 1250–1257
Kaul R, Trabattoni D, Bwayo J, Arienti D, Zagliani A, Mwangi FM, Kariuki C, Ngugi EN, MacDonald KS, Ball TB, Clerici M, Plummer FA 1999 HIV-1-specific mucosal IgA in a cohort of HIV-1-resistant Kenyan sex workers. AIDS 13: 23–29
Rowland-Jones S, Sutton J, Ariyoshi K, Dong T, Gotch F, McAdam S, Whitby D 1996 HIV-specific cytotoxic T-cells in HIV-exposed but uninfected Gambian women. Nat Med 1: 59–64
Bernard NF, Yannakis CM, Lee JS, Tsoukas CM 1999 Human immunodeficiency virus (HIV)-specific cytotoxic T lymphocyte activity in HIV-exposed seronegative persons. J Infect Dis 179: 538–547
Rowland-Jones SL, Nixon DF, Aldhous MC, Gotch F, Ariyoshi K, Hallam N, Kroll JS, Froebel K, McMichael A 1993 HIV-specific cytotoxic T-cell activity in an HIV-exposed but uninfected infant. Lancet 341: 860–861
Cheynier R, Langlade-Demoyen P, Marescot MR, Blanche S, Blondin G, Wain-Hobson S, Griscelli C, Vilmer E, Plata F 1992 Cytotoxic T lymphocyte responses in the peripheral blood of children born to human immunodeficiency virus-1-infected mothers. Eur J Immunol 22: 2211–2217
Aldhous MC, Watret KC, Mok JY, Bird AG, Froebel KS 1994 Cytotoxic T lymphocyte activity and CD8 subpopulations in children at risk of HIV infection. Clin Exp Immunol 97: 61–67
De Maria A, Cirillo C, Moretta L 1994 Occurrence of human immunodeficiency virus type 1 (HIV-1)-specific cytolytic T cell activity in apparently uninfected children born to HIV-1-infected mothers. J Infect Dis 170: 1296–1299
McFarland EJ, Harding PA, Luckey D, Conway B, Young RK, Kuritzkes DR 1994 High frequency of Gag- and envelope-specific cytotoxic T lymphocyte precursors in children with vertically acquired human immunodeficiency virus type 1 infection. J Infect Dis 170: 766–774
Luzuriaga K, Koup RA, Pikora CA, Brettler DB, Sullivan JL 1991 Deficient human immunodeficiency virus type 1-specific cytotoxic T cell responses in vertically infected children. J Pediatr 119: 230–236
MacDonald KS, Embree J, Njenga S, Nagelkerke NJD, Ngatia I, Mohammed Z, Barber BH, Ndinya-Achola J, Bwayo J, Plummer FA 1998 Mother-child class I HLA concordance increases perinatal human immunodeficiency virus type 1 transmission. J Infect Dis 177: 551–556
MacDonald KS, Fowke KR, Kimani J, Dunand VA, Nagelkerke NJD, Ball TB, Oyugi J, Njagi E, Gaur LK, Brunham RC, Wade J, Luscher MA, Krausa P, Rowland-Jones S, Ngugi E, Bwayo J, Plummer F 2000 Influence of HLA supertypes on susceptibility and resistance to human immunodeficiency virus type 1 infection. J Infect Dis 181: 1581–1589
Clerici M, Shearer GM 1994 The Th1-Th2 hypothesis of HIV infection: new insights. Immunol Today 15: 575–581
Coutsoudis A, Pillay K, Spooner E, Kuhn L, Coovadia HM 1999 Randomized trial testing effect of vitamin A supplementation on pregnancy outcomes and early mother-to-child transmission of HIV-1 in Durban, South Africa. AIDS 13: 1517–1524
Coutsoudis A, Pillay K, Spooner E, Kuhn L, Coovadia HM 1999 Influence of infant feeding patterns on early mother-to-child transmission of HIV-1 in Durban, South Africa. Lancet 354: 471–476
Chougnet CA, Kovacs A, Baker R, Mueller BU, Luban NLC, Liewehr DJ, Steinberg SM, Thomas EK, Shearer GM 2000 Influence of human immunodeficiency virus-infected maternal environment on development of infant interleukin-12 production. J Infect Dis 181: 1590–1597
Rich K, Siegel JN, Jennings C, Rydman RJ, Landay AL 1997 Function and phenotype of immature CD4+ lymphocytes in healthy infants and early lymphocyte activation in uninfected infants of human immunodeficiency virus-infected mothers. Clin Diagn Lab Immunol 4: 354–361
Adkins B 1999 T-cell function in newborn mice and humans. Immunol Today 20: 330–335
Trivedi HN, HayGlass KT, Gangur V, Allardice JG, Embree J, Plummer F 1997 Analysis of neonatal T cell and antigen presenting cell functions. Hum Immunol 57: 69–79
Vigano A, Balotta C, Trabattoni D, Salvaggio A, Riva C, Bricalli D, Crupi L, Colombo MC, Principi N, Galli M, Clerici M 1996 Virologic and immunologic markers of disease progression in pediatric HIV infection. AIDS Res Hum Retroviruses 12: 1255–1262
Vigano A, Principi N, Villa ML, Riva C, Crupi L, Trabattoni D, Shearer GM, Clerici M 1995 Immunologic characterization of children vertically infected with human immunodeficiency virus, with slow or rapid disease progression. J Pediatr 126: 368–374
Hyjek E, Lischner HW, Hyslop T, Bartkowiak J, Kubin M, Trinchieri G, Kozbor D 1995 Cytokine patterns during progression to AIDS in children with perinatal HIV infection. J Immunol 155: 4060–4071
Lee BN, Lu JG, Kline MW, Paul M, Doyle M, Kozinetz C, Shearer WT, Reuben JM 1996 Type 1 and type 2 cytokine profiles in children exposed to or infected with vertically transmitted human immunodeficiency virus. Clin Diagn Lab Immunol 3: 493–499
Than S, Hu R, Oyaizu N, Romano J, Wang X, Sheikh S, Pahwa S 1997 Cytokine pattern in relation to disease progression in human immunodeficiency virus-infected children. J Infect Dis 175: 47–56
Barcellini W, Rizzardi GP, Velati C, Borghi MO, Fain C, Lazzarin A, Meroni PL 1995 In vitro production of type 1 and type 2 cytokines by peripheral blood mononuclear cells from high-risk HIV-negative intravenous drug users. AIDS 9: 691–694
Acknowledgements
The authors thank Drs. Elizabeth Spooner and Kerry Uebel of McCord Hospital, Durban, for assistance with patients; Dr. Gill Sinclair of the National Institutes of Virology, Johannesburg, and Dr. Sharon Cassol from the University of Ottawa, Ontario, for HIV RNA tests; and Dr. Zena Stein for helpful advice.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kuhn, L., Coutsoudis, A., Moodley, D. et al. Interferon-Gamma and Interleukin-10 Production Among HIV-1–Infected and Uninfected Infants of HIV-1–Infected Mothers. Pediatr Res 50, 412–416 (2001). https://doi.org/10.1203/00006450-200109000-00018
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200109000-00018