Abstract
Plasma concentrations of endothelin-1 (ET-1) are increased in children with congenital heart disease associated with increased pulmonary blood flow. However, the role of ET-1 in the pathophysiology of pulmonary hypertension remains unclear. Preproendothelin-1 gene expression is increased in adults with advanced pulmonary hypertension. To characterize potential early molecular alterations in the ET-1 cascade induced by increased pulmonary blood flow and pulmonary hypertension, fetal lambs underwent in utero placement of an aortopulmonary vascular graft (shunt). RNase protection assays and Western blot analysis were performed on lung tissue prepared from 4-wk-old shunt lambs and age-matched controls. Endothelin-converting enzyme-1 [the enzyme responsible for the production of active ET-1 from big ET-1, mRNA (411%, p < 0.05)] and protein (170%, p < 0.05) were increased in lung tissue prepared from shunt lambs, compared with age-matched controls. Endothelin type A receptor (the receptor that mediates vasoconstriction), mRNA (246%, p < 0.05), and protein (176%, p < 0.05) also were increased in lung tissue prepared from shunt lambs compared with age-matched controls. Conversely, endothelin type B receptor (the receptor that mediates vasodilation), mRNA (46%, p < 0.05), and protein (65%, p < 0.05) were decreased in shunt lambs. Both the mRNA and protein levels for preproendothelin-1 were unchanged. Thus we conclude that increased pulmonary blood flow and pulmonary hypertension induce early alterations in the ET-1 cascade that result in increased ET-1 production, increased ET-1-mediated vasoconstriction, and decreased vasodilation. These early alterations in gene expression may contribute to the development of pulmonary hypertension and its associated enhanced pulmonary vascular reactivity.
Similar content being viewed by others
Main
The development of pulmonary hypertension and its associated increased vascular reactivity is a common accompaniment of congenital heart disease with increased pulmonary blood flow (1). After birth, the presence of a systemic-to-pulmonary communication results in increased pulmonary blood flow, increased pulmonary arterial pressure, and the progressive development of structural and functional abnormalities of the pulmonary vascular bed (2, 3). Recent evidence suggests that normal pulmonary vascular tone and vascular smooth muscle cell proliferation are regulated by a complex interaction of vasoactive substances that are produced locally by the vascular endothelium (4–7). Endothelial injury secondary to increased pulmonary blood flow and/or pressure may disrupt these regulatory mechanisms and is a potential factor in the development of pulmonary hypertension (8).
ET-1 is a 21-amino acid polypeptide—produced by vascular endothelial cells—that has potent vasoactive properties and is mitogenic for vascular smooth muscle cells (7, 9). The gene for human ET-1 is located on chromosome 6 and is translated to a 203-amino acid peptide precursor (preproET-1) which is then cleaved to form proendothelin-1. Proendothelin (big ET-1) is then cleaved by the metalloprotease ECE-1 into its functional form (10). The complex pulmonary vasoactive effects of ET-1, which may include pulmonary vasoconstriction and/or pulmonary vasodilation, are mediated by at least two different receptors, ETA and ETB. ETA receptors and a subpopulation of ETB receptors mediate vasoconstriction and are located on vascular smooth muscle cells. A second subpopulation of ETB receptors mediate vasodilation and are located on vascular endothelial cells (11–13).
Several studies demonstrate increased ET-1 plasma concentrations in children with congenital heart disease associated with increased pulmonary blood flow and pulmonary hypertension (14–16). In addition, adults with advanced pulmonary hypertension have increased preproET-1 expression within pulmonary vascular endothelial cells (17). However, because most patients who undergo histologic evaluation have advanced pulmonary hypertension, it has been difficult to investigate early alterations in the ET-1 cascade and their potential role in the development of pulmonary hypertension secondary to increased pulmonary blood flow.
Using aortopulmonary shunt placement in the fetal lamb, we recently established a unique animal model of pulmonary hypertension that mimics congenital heart disease with increased pulmonary blood flow (18). As early as 4 wk of age, these lambs have physiologic alterations in the ET-1 cascade, as displayed by loss of ETB receptor-mediated pulmonary vasodilation, increased ETA receptor-mediated pulmonary vasoconstriction, and increased plasma concentrations of ET-1 (19). The purpose of the present study was to characterize the early molecular alterations in the ET-1 cascade induced by increased pulmonary blood flow. Using RNase protection assays and Western blot analysis, we compared preproET-1, ECE-1, ETA receptor, and ETB receptor mRNA and protein in 4-wk-old lambs with increased pulmonary blood flow (shunt lambs) with that of age-matched control lambs.
METHODS
Surgical Preparations and Care
Ewes.
Ten mixed-breed Western pregnant ewes (137–141 d gestation, term = 145 d) were operated on under sterile conditions as previously described (18). Through a left lateral fetal thoracotomy, an 8.0-mm Gore-tex vascular graft (2 mm long) (W. L. Gore and Assos., Milpitas, CA) was anastomosed between the ascending aorta and main pulmonary artery of the fetus with 7.0 proline (Ethicon Inc., Somerville, NJ), using a continuous suture technique as previously described (18). Because we showed previously that unoperated and sham-operated control lambs are physiologically and morphologically similar, we used unoperated twin fetal lambs as the control group in these studies (18). After recovery from anesthesia, the ewe was returned to the cage with free access to food and water. Antibiotics (2 million units of penicillin G potassium and 100 mg of gentamicin sulfate) were administered to the ewe during surgery and daily thereafter until 2 d after spontaneous delivery of the lamb.
Lambs.
After spontaneous delivery, antibiotics (1 million units of penicillin G potassium and 25 mg of gentamicin sulfate) were administered intramuscularly (i.m.) for 2 d. The lambs were weighed daily, and the respiratory and heart rates were obtained. Furosemide (1 mg/kg, i.m.) was administered daily. Elemental iron (50 mg, i.m.) was given weekly. At 4 wk of age, the lambs were anesthetized with ketamine hydrochloride (∼1 mg/kg/min), intubated with a 5.5-mm OD endotracheal tube, and were mechanically ventilated with a Healthdyne pediatric time-cycled, pressure-limited ventilator (Healthdyne Inc., Marietta, GA). A mid-sternotomy incision was performed, and the pericardium was incised. Polyurethane catheters were then inserted into the left and right atrium, main pulmonary artery distal to the vascular graft, and the femoral artery. An ultrasonic flow probe (Transonics Systems, Inc., Ithaca, NY) was placed around the left pulmonary artery to measure left pulmonary blood βow. After a 30-min recovery period, blood was obtained from the left and right atria, distal pulmonary artery, right ventricle, and descending aorta for Hb and oxygen saturation determinations, and the baseline systemic and pulmonary arterial pressures, pulmonary blood flow, heart rate, and right and left atrial pressures were determined. The lambs were then killed by an i.v. injection of pentobarbital sodium (Euthanasia CII, Central City Medical, Union City, CA) followed by bilateral thoracotomy. The lungs were removed and prepared for RNase protection assays and Western blot analysis. All procedures and protocols were approved by the Committee on Animal Research of the University of California, San Francisco.
Measurements
Pulmonary and systemic arterial, and right and left atrial pressures were measured with Statham P23Db pressure transducers (Statham Instruments, Hato Rey, PR). Mean pressures were obtained by electrical integration. Heart rate was measured by a cardiotachometer triggered from the phasic systemic arterial pressure pulse wave. Left pulmonary blood flow was measured on an ultrasonic flow meter (Transonic Systems, Ithaca, NY). Systemic arterial blood gases and pH were measured on a Corning 158 pH/blood gas analyzer (Corning Medical and Scientific, Medfield, MA). Hb concentration and oxygen saturation were measured by a hemoximeter (model OSM 2, Radiometer, Copenhagen, Denmark). The ratio of pulmonary to systemic blood flow (Qp/Qs) was calculated by the Fick equation. Standard formulas were used to calculate pulmonary vascular resistance.
Tissue Preparation
To prepare total RNA, lung tissue was snap-frozen in liquid nitrogen and stored at −70°C until used. The snap-frozen lung tissue was pulverized, then was briefly homogenized in 4 M guanidinium isothiocyanate. Total RNA was extracted as previously described (20).
Generation of Ovine cDNA
Total ovine fetal lung RNA was used in reverse transcriptase-polymerase chain reactions (kit from Perkin-Elmer, Foster City, CA). The generated cDNA fragment of interest (see below) was then cloned directly into the pCR II vector (Invitrogen, San Diego, CA), sequenced (Sequenase kit from USB, Cleveland, OH), and then subcloned into pBluescript KS+ (Stratagene, La Jolla, CA).
PreproET-1.
Oligonucleotides were synthesized by using the 522-bp cDNA fragment of ovine preproET-1 as a template (21). The sequences of the oligonucleotides were 5′-CCTGAATTCCTCTGCTGTTTGTGGCTT-3′ for oligonucleotide #1 and 5′-GAAGAATTCGCTGTTGCTGATGGCCTC-3′ for oligonucleotide #2.
ECE-1.
Oligonucleotides were synthesized using the bovine ECE-1 cDNA as a template (22). The sequences of the oligonucleotides were 5′-AGCTCCATCTTGAGTTCCATG-3′ for oligonucleotide #1 and 5′-CTGGAAGTTGTCCTTGTCCCA-3′ for oligonucleotide #2. The region amplified (338 bp) corresponds to amino acids 97 to 209 of the ECE-1 protein.
Endothelin receptors.
Regions of minimal homology between the rat ETA and ETB receptors were identified (11, 12). Oligonucleotides were synthesized (using the rat ET receptors as a template) to allow amplification of these regions within the ovine ETA and ETB receptor sequences. The sequences of the oligonucleotides for the ETA receptor were 5′-CTCATCTATGGCGCCAAGCATGCCTGG-3′ for oligonucleotide #1, and 5′-AGTTGTCACAGTAGTCACGGACGCCGA-3′ for oligonucleotide #2. The region amplified (309 bp) corresponds to amino acids 127 to 232 of the ETA receptor protein. The sequences of the oligonucleotides for ETB receptor were 5′-CTCATCTATGGCGCCAAGCATGCCTGG-3′ for oligonucleotide #1 and 5′-AGTTGTCACAGTAGTCACGGACGCCGA-3′ for oligonucleotide #2. The region amplified (291 bp) corresponds to amino acids 148 to 247 of the ETB receptor protein.
RNA Probe Synthesis and RNase Protection Assay
The plasmid containing the cDNA fragment of interest was linearized with the appropriate restriction enzyme (GIBCO-BRL, Grand Island, NY). Antisense 32P-UTP-radiolabeled cRNA probes (New England Nuclear, Boston, MA) were synthesized by in vitro transcription, using either T3 or T7 RNA polymerases (Boerhinger-Mannheim, Indianapolis, IN) in the presence of cold rCTP, rGTP, and rATP (20).
RNase protection assays were performed as previously described (20). Antisense radiolabeled cRNA probes were hybridized overnight at 42°C with total RNA isolated from ovine fetal lung (50 μg) in 80% formamide, 50 mM piperazine-N,N′-bis(2-ethanesulphonic acid (PIPES) (pH 6.4), 0.4 M NaCl, and 1 mM EDTA. Single-stranded RNA was digested for 1 h at 37°C with an RNase A/T1 mixture (Ambion, Austin, TX). After phenol/CHCl3 extraction and ethanol precipitation, the protected fragments were analyzed by electrophoresis on a 6% denaturing polyacrylamide gel. Also included was a probe for 18S to serve as a control for the amount of input total RNA and the recovery of protected probe fragments.
Generation of Ovine ETA-Specific Antisera
The ETA cDNA fragment was subcloned in frame into the pET23c expression vector (Novagen, Madison, WI) to overexpress the corresponding ETA protein fragment (20). After confirming the reading frame at both the 5′- and 3′-ends, the pET23a clone was transformed into the bacterial strain BL21(DE3)plys S, which contains a lysogen of T7 bacteriophage and a plasmid-encoding lysozyme to reduce constitutive expression of the T7 RNA polymerase. One-liter cultures were grown from a single colony under ampicillin selection until the OD600 reached ∼0.6; isopropyl thiogalactoside was then added (final concentration, 0.4 mM). After 3 h, the cells were pelleted, resuspended in 1/10th volume of imidazole buffer, and sonicated to disrupt the cell membranes and shear chromosomal DNA. The lysate was cleared by centrifugation, passed over a Ni2+ column, washed, and eluted with 1 M imidazole. The eluted fraction was concentrated by passage through a concentrator with the addition of sterile distilled water to reduce the imidazole concentration. The resultant partially purified ETA protein fragment was then injected into New Zealand White rabbits (Animal Pharm Services, Healdsberg, CA) to produce a polyclonal ETA antiserum. The specificity of the antiserum was assessed by Western blot analysis on protein extracts prepared from a variety of tissues.
Western Blot Analysis
Western blot analysis was performed as previously described (20). Protein extracts were separated on 6% denaturing polyacrylamide gels for ECE-1, 10% denaturing polyacrylamide gels for ETA and ETB receptors, or 4–20% denaturing polyacrylamide gradient gels for preproET-1. All gels were electrophoretically transferred to Hybond-PVDF membranes (Amersham, Arlington Heights, IL). The membranes were blocked with 5% nonfat dry milk in Tris-buffered saline containing 0.1% Tween. After blocking, the membranes were incubated at room temperature with the appropriate dilution of the antiserum of interest (1: 250 for ECE-1, 1:1,000 for ETA, 1:25 for ETB, or 1:500 for preproET-1), washed with triethanolamine-buffered saline containing 0.1% Tween, and then incubated with either a goat anti-rabbit IgG-horseradish peroxidase conjugate (for ETA and ETB receptors) or a goat anti-mouse IgG-horseradish peroxidase conjugate (for ECE-1 and preproET-1). After washing, chemiluminescence was used to detect the protein bands.
The ECE-1 antisera was provided by Adel Giaid (McGill University, Montreal, Canada) (23). The ETB receptor antiserum was obtained from Maine Biotechnology Services (Portland, ME). The preproET-1 antibody was obtained from Affinity Bioreagents (Golden, CO). The specificity of the preproET-1 antibody was verified with a preincubation step with purified ET-1 (50 ng ET–1/15 μL of antiserum) protein. The purified ET-1 was purchased from Sigma Chemical Co. (St. Louis, MO).
Data Analysis
The means ± SD were calculated for the baseline hemodynamic variables, and for systemic arterial blood gases and pH. The general hemodynamic variables, systemic arterial blood gases, and pH were compared between study groups by unpaired t test.
Quantification of autoradiographic results was performed by scanning (Hewlett Packard SCA Jet IICX, Hewlett-Packard, Inc., Palo Alto, CA) the bands of interest into an image-editing software program (Adobe Photoshop, Adobe Systems, Mt. View, CA). Band intensities from RNase protection assays and Western blot analysis were analyzed densitometrically on a MacIntosh computer (model 9500, Apple Computer, Inc., Cupertino, CA) using the public domain National Institutes of Health Image Program (developed at the National Institutes of Health and available on the Internet at http://rsb.info.nih.gov/nih-image). For RNase protection assays to control for the amount of input RNA and the recovery of protected probe fragments, the mRNA signal of interest was normalized to the corresponding 18S signal for each lane. Because the relative signals of the 18S and test probes were substantially different, multiple exposures were prepared and scanned to ensure that all signals were in the linear range of the autoradiographic film. Results from control lamb lungs were assigned the value of 1 (relative mRNA of interest). For Western blot analysis, to ensure equal protein loading, duplicate polyacrylamide gels were run. One was stained with Coomassie blue. Results from control lamb lungs were assigned the value of 1 (relative protein of interest). The means ± SEM were calculated for the relative mRNA and the relative protein of interest from control and shunt lamb lungs, and results were compared by unpaired t test. A p < 0.05 was considered statistically significant.
RESULTS
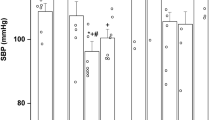
At 4 wk of age, all shunted lambs had a continuous murmur and an increase in oxygen saturation between the right ventricle and distal pulmonary artery. The pulmonary-to-systemic blood flow ratio (Qp/Qs) was 2.6 ± 0.8. Compared with age-matched controls, mean pulmonary arterial pressure was increased (26.4 ± 8.0 versus 14.8 ± 3.8 mm Hg, p < 0.05) to 49% of systemic values. This was associated with an increase in left pulmonary blood flow (158.4 ± 29.3 versus 34.8 ± 18.9 mL/kg/min, p < 0.05) and left atrial pressure (8.4 ± 3.6 versus 4.8 ± 1.0 mm Hg, p < 0.05). Mean systemic arterial pressure was decreased (56.4 ± 7.8 versus 69.4 ± 10.7 mm Hg). Heart rate, right atrial pressure, left pulmonary vascular resistance, systemic arterial blood gases, and pH were unchanged.
Increased pulmonary blood flow and pulmonary hypertension induced changes in the expression of the members of the ET-1 cascade. RNase protection assays demonstrated that preproET-1 mRNA expression was similar in 4-wk-old shunt and control lambs (Fig. 1, A and B). Similarly, Western blot analysis with an ET-1-specific MAb demonstrated no significant alterations in preproET-1 protein levels in 4-wk-old shunt or control lambs (Fig. 1, C and D). Studies using ECE-1-specific probes demonstrated that ECE-1 mRNA and protein expression was increased by 411% and 170%, respectively, in shunt lambs compared with normal 4-wk-old control lambs (*p < 0.05) (Fig. 2).
RNase protection assay (panels A and B) and Western blot analysis (panels C and D) for preproET-1 in lung tissue from 4-wk-old lambs (Control), and after insertion of an aorta-to-pulmonary artery vascular graft in utero (Shunt). Panel A: a cRNA probe for ovine preproET-1 was hybridized overnight to 50 μg of total lung RNA prepared from two 4-wk-old lambs (one Control and one Shunt). There was no change in preproET-1 mRNA expression between 4-wk-old Shunt and Control lambs. No protected fragments were detected in the lanes in which the probe was hybridized without RNA (PA) or in the presence of tRNA. ET-1 is undigested probe. A cRNA for ovine 18S was also hybridized to serve as a control for RNA loading (panel A). Panel B: the densitometric values for relative preproET-1 mRNA (normalized to 18S mRNA and to control) from five Control and eight Shunt lambs. In Shunt lambs, relative preproET-1 mRNA expression was similar to that in Control lambs. Values are mean ± SEM (panel B). Panel C: protein extracts (100 μg) prepared from lung tissue from six 4-wk-old lambs (three Control and three Shunt) were separated on a 4–20% denaturing polyacrylamide gradient gel, electrophoretically transferred to Hybond membranes, and analyzed with a specific antiserum raised against preproET-1. There was no change in preproET-1 protein expression between 4-wk-old Shunt and Control lambs (panel C). Panel D: the densitometric values for relative preproET-1 protein (normalized to control) from five Control and eight Shunt lambs. In Shunt lambs, relative preproET-1 mRNA expression was not significantly different from that in Control lambs. Values are mean ± SEM (panel D).
RNase protection assay (panels A and B) and Western blot analysis (panels C and D) for endothelin-converting enzyme-1 (ECE-1) in lung tissue from 4-wk-old lambs (Control), and after insertion of an aorta-to-pulmonary artery vascular graft in utero (Shunt). Panel A: cRNA probe for ovine ECE-1 was hybridized overnight to 50 μg of total lung RNA prepared from two 4-wk-old lambs (one Control and one Shunt). There was an increase in ECE-1 mRNA expression in Shunt lambs. No protected fragments were detected in the lanes in which the probe was hybridized without RNA (PA) or in the presence of tRNA. ECE-1 is undigested probe. A cRNA for ovine 18S was also hybridized to serve as a control for RNA loading (panel A). Panel B: the densitometric values for relative ECE-1 mRNA (normalized to 18S mRNA and to control) from four Control and eight Shunt lambs. In Shunt lambs, relative ECE-1 mRNA increased by 411% (p < 0.05). Values are mean ± SEM. *p < 0.05, Control vs Shunt (panel B). Panel C: protein extracts (100 μg) prepared from lung tissue from six 4-wk-old lambs (three Control and three Shunt) were separated on a 6% denaturing polyacrylamide gel, electrophoretically transferred to Hybond membranes, and analyzed with a specific antiserum raised against endothelin- converting enzyme-1. There was an increase in ECE-1 protein expression in Shunt lambs (panel C). Panel D: the densitometric values for relative ECE-1 protein (normalized to control) from six Control and eight Shunt lambs. In Shunt lambs, relative ECE-1 protein expression was increased by 170% (p < 0.05). Values are mean ± SEM (panel D).
Subsequently, we also measured the mRNA and protein levels ETA and ETB receptors in 4-wk-old shunt and control lambs. We found that ETA receptor mRNA and protein expression was increased by 246% and 176%, respectively, in shunt lambs compared with normal 4-wk-old control lambs (*p < 0.05) (Fig. 3). Conversely, ETB receptor mRNA and protein expression were decreased by 54% and 35%, respectively, in shunt lambs compared with normal 4-wk-old control lambs (*p < 0.05) (Fig. 4).
RNase protection assay (panels A and B) and Western blot analysis (panels C and D) for the ETA receptor in lung tissue from 4-wk-old lambs (Control), and after insertion of an aorta-to-pulmonary artery vascular graft in utero (Shunt) . cRNA probe for the ovine ETA receptor was hybridized overnight to 50 μg of total lung RNA prepared from two 4-wk-old lambs (one Control and one Shunt). There was an increase in ETA mRNA expression in Shunt lambs. No protected fragments were detected in the lanes where the probe was hybridized without RNA (PA) or in the presence of tRNA. ETA Receptor is undigested probe. A cRNA for ovine 18S was also hybridized to serve as a control for RNA loading (panel A). Panel B: the densitometric values for relative ETA mRNA (normalized to 18S mRNA and to control) from four Control and eight Shunt lambs. In Shunt lambs, relative ETA mRNA increased by 246% (p < 0.05). Values are mean ± SEM. *p < 0.05, Control vs Shunt (panel B). Panel C: protein extracts (100 μg), prepared from lung tissue from two 4-wk-old lambs (one Control and one Shunt), were separated on a 10% denaturing polyacrylamide gel, electrophoretically transferred to Hybond membranes, and analyzed with a specific antiserum raised against the ETA receptor. There was an increase in ETA receptor protein expression in Shunt lambs (panel C). Panel D: the densitometric values for relative ETA receptor protein (normalized to control) from six Control and eight Shunt lambs. In Shunt lambs, relative ETA receptor protein expression was increased by 176% (p < 0.05). Values are mean ± SEM (panel D).
RNase protection assay (panels A and B) and Western blot analysis (panels C and D) for the ETB receptor in lung tissue from 4-wk-old lambs (Control), and after insertion of an aorta-to-pulmonary artery vascular graft in utero (Shunt). Panel A: a cRNA probe for the ovine ETB receptor was hybridized overnight to 50 μg of total lung RNA prepared from two 4-wk-old lambs (one Control and one Shunt). There was a decrease in ETB receptor mRNA expression in Shunt lambs. No protected fragments were detected in the lanes where the probe was hybridized without RNA (PA) or in the presence of tRNA. ETB Receptor is undigested probe. A cRNA for ovine 18S was also hybridized to serve as a control for RNA loading (panel A). Panel B: the densitometric values for relative ETB receptor mRNA (normalized to 18S mRNA and to control) from six Control and 10 Shunt lambs. Relative ETB receptor mRNA was decreased by 54% (p < 0.05). Values are mean ± SEM. *p < 0.05 Control vs Shunt (panel B). Panel C: protein extracts (100 μg), prepared from lung tissue from four 4-wk-old lambs (two Control and two Shunt), were separated on a 10% denaturing polyacrylamide gel, electrophoretically transferred to Hybond membranes, and analyzed with a specific antiserum raised against the ETB receptor. There was a decrease in ETB receptor protein expression in Shunt lambs (panel C). Panel D: the densitometric values for relative ETB receptor protein (normalized to control) from six Control and eight Shunt lambs. In Shunt lambs, relative ETB receptor protein expression was decreased by 35% (p < 0.05). Values are mean ± SEM (panel D).
DISCUSSION
Children with congenital heart disease and increased pulmonary blood flow may suffer significant morbidity and mortality from the development of pulmonary hypertension (24). The ET-1 cascade is an important mediator of pulmonary vascular reactivity and smooth muscle mitogenesis (6, 7). Although preproET-1 gene expression is increased in the lungs of patients with late, irreversible pulmonary hypertension, potential early molecular alterations in the ET-1 cascade that may play a crucial role in the pathophysiology of pulmonary hypertension have not been identified (17). Therefore, the purpose of the present study was to determine whether pulmonary hypertension with increased pulmonary blood flow induces early changes in the expression of genes of the ET-1 cascade in the lung. For this study, we used a novel model of pulmonary hypertension with increased pulmonary blood flow in the lamb after in utero placement of an aortopulmonary vascular graft. At 4 wk of age, these lambs have a pulmonary-to-systemic blood flow ratio of ∼2:1, a mean pulmonary arterial pressure that is 50–75% of mean systemic arterial pressure, and pulmonary vascular remodeling that is characteristic of children with pulmonary hypertension with increased pulmonary blood flow (18). In addition, we observed increased plasma ET-1 concentrations and an alteration in the vasoactive response to exogenous ET-1 from pulmonary vasodilation to vasoconstriction. This was associated with loss of ETB-mediated vasodilation and increased ETA-mediated vasoconstriction (19). In the present study, we found alterations in gene expression that correlated with the physiologic alterations; ECE-1 and ETA receptor mRNA and protein were up-regulated in the lungs of 4-wk-old shunted lambs, whereas ETB receptor mRNA and protein were down-regulated. These early alterations in gene expression may result in increasing ET-1-induced pulmonary vasoconstriction and mitogenesis and might thereby contribute significantly to the development of pulmonary hypertension secondary to increased pulmonary blood flow.
An association between ET-1 and early pulmonary hypertensive disorders in humans has been based previously on reports of increased plasma ET-1 concentrations in patients with pulmonary hypertension. For example, several studies demonstrate increased ET-1 concentrations in children with congenital heart disease associated with increased pulmonary blood flow and pulmonary hypertension. In addition, some patients with pulmonary hypertension demonstrate an increase in plasma ET-1 concentrations between the right ventricle and pulmonary vein, suggesting increased local production of ET-1 within the pulmonary circulation (14–16) However, the correlations between plasma ET-1 concentrations and pulmonary hemodynamics have been inconsistent (14). Recent animal studies have supported an early role for ET-1-induced vasoconstriction and mitogenesis in the pathophysiology of pulmonary hypertension induced by a variety of etiologies. For example, chronic blockade of the ETA receptor attenuates the development of pulmonary hypertension induced by chronic hypoxia, monocrotaline, or in utero ductal ligation (25–27). The findings of the present study further implicate a role for alterations in the ET-1 cascade in the pathophysiology of pulmonary hypertension secondary to increased pulmonary blood flow.
Surprisingly, despite increased plasma ET-1 concentrations, preproET-1 mRNA and protein were unchanged in 4-wk-old lambs with increased pulmonary blood flow and pulmonary hypertension. These data are in contrast to the increased preproET-1 mRNA found in humans with advanced pulmonary hypertension secondary to a variety of etiologies and in lambs with persistent PPHN after in utero ligation of the ductus arteriosus (17, 28). Factors responsible for the regulation of preproET-1 gene expression in vivo remain unknown. In vitro, shear stress regulates ET-1 gene expression, a factor that may be responsible for the differences noted in this study from results of previous in vivo studies. Because the pulmonary circulation of shunt lambs is exposed to increased pulmonary blood flow and the pulmonary arteries have a decreased internal radius secondary to vascular remodeling, shear stress probably is increased in shunt lambs (18). In vitro data suggest that the regulation of preproET-1 expression by shear stress is dependent on a variety of factors, including the level and duration of the stimulus (29). Although both humans with advanced pulmonary vascular disease and lambs with PPHN have increased shear stress, the duration, level, and timing of the stimulus differ. For example, all of the human data represent changes in advanced pulmonary vascular disease that have occurred over several years. The early effects of increased pulmonary blood flow on preproET-1 gene expression in humans have not been studied. Similarly, the exposure in lambs with PPHN subsequent to in utero ductal ligation is exclusively prenatal, whereas the exposure in the current model is predominantly postnatal. In vitro data also suggest that ET-1 gene expression is regulated by NO. For example, in human umbilical vein endothelial cells, NO suppresses preproET-1 gene expression, and inhibition of NO increases preproET-1 mRNA (30). In both humans with advanced pulmonary hypertension and lambs with PPHN, production of NO is decreased (31, 32). However, previous physiologic and molecular evidence suggests that basal NO production is increased in lambs with increased pulmonary blood flow (33). Therefore, this increased NO production in shunt lambs may also explain, in part, why preproET-1 gene expression is not increased, in contrast to lambs with PPHN and humans with advanced pulmonary hypertension.
Our results demonstrate that both ETB receptor mRNA and protein are down-regulated in lambs with increased pulmonary blood flow. This correlates with our previous physiologic data in which the pulmonary vasodilating response to ETB receptor agonists was abolished (19). The down-regulation of ETB receptor mRNA has also been demonstrated in pulmonary hypertension produced by monocrotaline and by in utero ligation of the ductus arteriosus (28, 34, 35). In vitro data suggest that increased ET-1 exposure down-regulates ETB receptor mRNA (36). Increased circulating levels of ET-1 are found in lambs with increased pulmonary blood flow, as well as in rats after injections of monocrotaline and in lambs after in utero ligation of the ductus arteriosus (19, 37, 38). Therefore, increased ET-1 production may contribute to the down-regulation of the ETB receptor in these models of pulmonary hypertension. Conversely, because the ETB receptor participates in the clearance of ET-1, down-regulation of the ETB receptor may contribute to the increase in ET-1 levels secondary to decreased clearance (39).
When the ETB receptor is down-regulated, ET-1 activates the ETA receptor, producing vascular smooth muscle contraction and pulmonary vasoconstriction. In our present study, ETA receptor mRNA and protein were up-regulated in lambs with increased pulmonary blood flow. That correlates, also, with our previous physiologic data which demonstrated increased ETA receptor-mediated pulmonary vasoconstriction in shunt lambs (19). The up-regulation of ETA receptors has also been demonstrated in pulmonary hypertension produced by in utero ligation of the ductus arteriosus (28). Factors responsible for the regulation of ETA receptor gene expression in vivo remain unknown. However, in vitro data suggest that NO-cGMP production increases ETA receptors in vascular smooth muscle cells (40). In vitro data also suggest that basic fibroblast growth factor increases ETA receptors (41). Both NO-cGMP and basic fibroblast growth factor are increased in these lambs with increased pulmonary blood flow (33, 42). However, their role, if any, in up-regulating ETA receptor gene expression in lambs with increased pulmonary blood flow remains to be determined.
ECE-1 exhibited the most dramatic alteration in gene expression induced by increased pulmonary blood flow. ECE-1 mRNA was up-regulated 4-fold, whereas ECE-1 protein was increased 2-fold (it is unclear why there is this discrepancy between the ECE-1 mRNA and protein data). ECE-1 is a membrane-bound metalloprotease homologous to neutral endopeptidase 24.11. It has been shown to be expressed in a variety of organs, including the lung, and most abundantly in vascular endothelial cells (10, 22). Several studies suggest that ECE-1 activity regulates tissue and plasma ET-1 levels. For example, plasma molar levels of big ET-1 (the inactive precursor to ET-1) are much higher than those of ET-1 in humans and animals (43). In addition, in rats, congestive heart failure significantly increases plasma levels of ET-1, whereas big ET-1 levels remain unchanged, suggesting that the majority of big ET-1 within vascular endothelial cells is not converted to ET-1 (44). Because preproET-1 mRNA is unchanged in lambs with increased pulmonary blood flow, the up-regulation of ECE-1 is probably responsible for the increased plasma concentrations of ET-1 noted in these lambs with increased pulmonary blood flow. Although factors responsible for the regulation of ECE-1 in vivo remain unknown, ECE-1 is up-regulated following balloon injury of the coronary artery endothelium (45). In vitro data also suggest that VEGF increases ECE-1 gene expression (46). Our initial studies showed that VEGF expression is increased in the shunt lambs with increased pulmonary blood flow (42). However, the possible role of endothelial injury and/or increased VEGF expression in the up-regulation of ECE-1 is speculative and remains to be elucidated.
Within the lung, ET-1 may be synthesized by a variety of cell types that include bronchial and alveolar epithelial cells, neuroendocrine cells, macrophages, smooth muscle cells, and endothelial cells (47). Because the present study was performed in whole lung, the changes noted cannot be isolated to particular types of cells. However, it is noteworthy that the changes in gene expression correlated with the physiologic alterations previously noted within the pulmonary circulation, suggesting that the changes occurred, at least in part, within the vasculature. In addition, we have previously demonstrated that shunt lambs have approximately twice the number of pulmonary vessels as age-matched control lambs (18). Although the decrease in ETB receptor expression and the large increase in ECE-1 expression should not be affected, explaining differences in vessel densities cannot be excluded from the differences noted in ETA receptor expression.
In conclusion, the present study demonstrates an alteration of genes of the ET-1 cascade over the first 4 wk of life in a lamb model of pulmonary hypertension secondary to increased pulmonary blood flow. Increased pulmonary blood flow and pulmonary hypertension increased the expression of ETA receptor and ECE-1 mRNA and protein and decreased the expression of ETB receptor mRNA and protein. The net result of these gene alterations is increased production of ET-1, increased ET-1-mediated pulmonary vasoconstriction, and decreased ET-1-mediated pulmonary vasodilation. These early alterations in gene expression may contribute to the development of pulmonary hypertension and its associated enhanced pulmonary vascular reactivity. A better understanding of the mechanisms responsible for these changes in gene expression could lead to better prevention and treatment strategies for children with congenital heart disease and increased pulmonary blood flow.
Abbreviations
- NO:
-
nitric oxide
- PreproET-1:
-
preproendothelin-1
- ET-1:
-
endothelin-1
- ECE-1:
-
endothelin-converting enzyme-1
- ETA:
-
endothelin type A receptor
- ETB:
-
endothelin type B receptor
- PPHN:
-
pulmonary hypertension of the newborn
- VEGF:
-
vascular endothelial growth factor
References
Hoffman JIE, Rudolph AM, Heymann MA 1981 Pulmonary vascular disease with congenital heart lesions: pathologic features and causes. Circulation 64: 873–877.
Heath D, Edwards JE 1958 The pathology of hypertensive pulmonary vascular disease. Circulation 18: 533–547.
Rabinovitch M, Haworth SG, Castenada AR, Nadas AS, Reid LM 1978 Lung biopsy in congenital heart disease: a morphometric approach to vascular disease. Circulation 58: 1107–1122.
Furchgott RF, Vanhoutte PM 1989 Endothelium-derived relaxing and contracting factors. FASEB J 3: 2007–2018.
Wiklund NP, Persson MG, Gustafsson LE, Moncada S, Hedqvist P 1990 Modulatory role of endogenous nitric oxide in pulmonary circulation in vivo. Eur J Pharmacol 185: 123–124.
Fineman JR, Soifer SJ, Heymann MA 1995 Regulation of pulmonary vascular tone in the perinatal period. Annu Rev Physiol 57: 115–134.
Hassoun PM, Thappa V, Landman MJ, Fanburg BL 1992 Endothelin 1: mitogenic activity on pulmonary artery smooth muscle cells and release from hypoxic endothelial cells. Proc Exp Biol Med 199: 165–170.
Rabinovitch M, Bothwell T, Hayakawa BN, Williams WG, Trusler GA, Rowe RD, Olley PM, Cutz E 1986 Pulmonary artery endothelial abnormalities in patients with congenital heart defects and pulmonary hypertension. Lab Invest 6: 632–653.
Yanagisawa M, Kurihara H, Kimura S, Tomobe Y, Kobayashi M, Mitsui Y, Yazaki Y, Goto K, Masaki T 1988 A novel potent vasoconstrictor peptide produced by vascular endothelial cells. Nature 332: 411–415.
Turner AJ, Murphy LJ 1996 Molecular pharmacology of endothelin converting enzymes. Biochem Pharmacol 51: 91–102.
Arai H, Hori S, Aramori I, Ohkubo H, Nakanishi S 1990 Cloning and expression of a cDNA encoding an endothelin receptor. Nature 348: 730–732.
Sakurai T, Yanagisawa M, Takuwa Y, Miyazaki H, Kimura S, Goto K, Masaki T 1990 Cloning of a cDNA encoding a non-isopeptide-selective subtype of the endothelin receptor. Nature 348: 732–735.
Shetty SS, Toshikazu O, Webb RL, DelGrande D, Lapp RW 1993 Functionally distinct endothelin b receptors in vascular endothelium and smooth muscle. Biochem Biophys Res Commun 191: 459–464.
Vincent JA, Ross RD, Kassab J, Hsu JM, Pinsky WW 1993 Relation of elevated plasma endothelin in congenital heart disease to increased pulmonary blood flow. Am J Cardiol 71: 1204–1207.
Yamamoto K, Ikeda U, Mito H, Fujikawa H, Sekiguchi H, Shimada K 1994 Endothelin production in pulmonary circulation of patients with mitral stenosis. Circulation 89: 2093–2098.
Yoshibayashi M, Nishioka K, Nakao K, Saito Y, Matsumura M, Ueda T, Temma S, Shirakami G, Imura H, Mikawa H 1991 Plasma endothelin concentrations in patients with pulmonary hypertension associated with congenital heart disease. Circulation 84: 2280–2285.
Giaid A, Yanagisawa M, Langleben D, Michel RP, Levy R, Shennib H, Kimura S, Masaki T, Duguid WP, Stewart DJ 1993 Expression of endothelin-1 in the lungs of patients with pulmonary hypertension. N Engl J Med 328: 1732–1739.
Reddy VM, Meyrick B, Wong J, Khoor A, Liddicoat JR, Hanley FL, Fineman JR 1995 In utero placement of aortopulmonary shunts: a model of postnatal pulmonary hypertension with increased pulmonary blood flow in lambs. Circulation 92: 606–613.
Wong J, Reddy VM, Hendricks-Munoz K, Liddicoat JR, Gerrets R, Fineman JR 1995 Endothelin-1 vasoactive responses in lambs with pulmonary hypertension and increased pulmonary blood flow. Am J Physiol 269: H1965–H1972.
Black SM, Johengen MJ, Ma ZD, Bristow J, Soifer SJ 1997 Ventilation and oxygenation induce endothelial nitric oxide synthase gene expression in the lungs of fetal lambs. J Clin Invest 100: 1–11.
Donahue DM, Lee ME, Suen HC, Quertermous T, Wain JC 1994 Pulmonary hypoxia increases endothelin-1 gene expression in sheep. J Surg Res 57: 280–283.
Xu D, Emoto N, Giaid A, Slaughter C, Kaw S, deWit D, Yanagisawa M 1994 ECE-1: a membrane-bound metalloprotease that catalyzes the proteolytic activation of big endothelin-1. Cell 78: 473–485.
Furukawa K, Saleh D, Bayan F, Emoto N, Kaw S, Yanagisawa M, Giaid A 1996 Co-expression of endothelin-1 and endothelin converting enzyme-1 in patients with chronic rhinitis. Am J Resp Cell Mol Biol 14: 248–253.
Burrows FA, Klinck JR, Rabinovitch M, Bohn DJ 1986 Pulmonary hypertension in children: perioperative management. Can Anaesth Soc J 33: 606–628.
Miyauchi T, Yorikane R, Sakai S, Sakurai T, Okada M, Nishikibe M, Yano M, Yamaguchi I, Sugishita Y, Goto K 1993 Contribution of endogenous endothelin-1 to the progression of cardiopulmonary alterations in rats with monocrotaline-induced pulmonary hypertension. Circ Res 73: 887–897.
Bonvallet ST, Zamora MR, Hasunuma K, Sato K, Hanasato N, Anderson D, Sato K, Stelzner TJ 1994 BQ 123, an ETA-receptor antagonist, attenuates hypoxic pulmonary hypertension in rats. Am J Physiol 266: H1327–H1331.
Ivy DD, Parker TA, Ziegler JW, Galan HL, Kinsella JP, Tuder RM, Abman SH 1997 Prolonged endothelin A receptor blockade attenuates chronic pulmonary hypertension in the ovine fetus. J Clin Invest 99: 1179–1186.
Ivy DD, Le Cras TD, Horan MP, Abman SH 1998 Increased lung preproET-1 and decreased ETB-receptor gene expression in fetal pulmonary hypertension. Am J Physiol 274: L535–L541.
Kuchan MJ, Frangos JA 1993 Shear stress regulates endothelin-1 release via protein kinase C and cGMP in cultured endothelial cells. Am J Physiol 264: H150–H156.
Kourembanas S, McQuillan LP, Leung GK, Faller DV 1993 Nitric oxide regulates the expression of vasoconstrictors and growth factors by vascular endothelium under normoxia and hypoxia. J Clin Invest 92: 99–104.
Giaid A, Saleh D 1995 Reduced expression of endothelial nitric oxide synthase in the lungs of patients with pulmonary hypertension. N Engl J Med 333: 214–221.
Shaul P, Yuhanna LS, German Z, Chen Z, Steinhorn RH, Morin IFC 1997 Pulmonary endothelial NO synthase gene expression is decreased in fetal lambs with pulmonary hypertension. Am J Physiol 272: L1005–L1012.
Black SM, Fineman JR, Steinhorn RH, Bristow J, Soifer SJ 1998 Increased endothelial NO synthase in lambs with increased pulmonary blood flow and hypertension. Am J Physiol 275: H1643–H1651.
Yorikane R, Miyauchi T, Sakai S, Sakurai T, Yamaguchi I, Sugishita Y, Goto K 1993 Altered expression of ETB-receptor mRNA in the lung of rats with pulmonary hypertension. J Cardiovasc Pharmacol 22: S336–S338.
Black SM, Johengen MJ, Soifer SJ 1998 Coordinated regulation of genes of the nitric oxide and endothelin pathways during the development of pulmonary hypertension in fetal lambs. Pediatr Res 44: 821–830.
Clozel M, Loffler BM, Breu V, Hilfiger L, Maire JP, Butscha B 1993 Downregulation of endothelin receptors by autocrine production of endothelin-1. Am J Physiol 265: C188–C192.
Mathew R, Zeballos GA, Tun H, Gewitz MH 1995 Role of nitric oxide and endothelin-1 in monocrotaline-induced pulmonary hypertension. Cardiovasc Res 30: 739–746.
Ivy DD, Ziegler JW, Dubus MF, Fox JJ, Kinsella JP, Abman SH 1996 Chronic intrauterine pulmonary hypertension alters endothelin receptor activity in the ovine fetal lung. Pediatr Res 39: 435–442.
Fukuroda T, Fujikawa T, Ozaki S, Ishikawa K, Yano M, Nishikibe M 1994 Clearance of circulating endothelin-1 by ETb receptors in rats. Biochem Biophys Res Commun 199: 1461–1465.
Redmond EM, Cahill PA, Hodges R, Zhang S, Sitzman JV 1996 Regulation of endothelin receptors by nitric oxide in cultured rat vascular smooth muscle cells. J Cell Physiol 166: 469–479.
Cristiani C, Volpi D, Landonio A, Bertolero F 1994 Endothelin-1-selective binding sites are downregulated by transforming growth factor-β and upregulated by basic fibroblast growth factor in a vascular smooth muscle-derived cell line. J Cardiovasc Pharmacol 23: 988–994.
Black SM, Fineman JR, Johengen MJ, Ma ZD, Soifer SJ 1996 Alterations in pulmonary blood flow in the lamb induces changes in pulmonary vascular morphology and growth factor expression. Pediatr Res 39: 23A
Suzuki N, Matsumoto H, Kitada C, Kimura S, Miyauchi T, Fujino M 1992 A sandwich-type enzyme immunoassay to detect immunoreactive big-endothelin-1 and endothelin-1 in human, rat, and rabbit plasma. Biochem Int 27: 755–761.
Teerlink JR, Loffler BM, Hess P, Maire JP, Clozel M, Clozel JP 1994 Role of endothelin in the maintenance of blood pressure in conscious rats with chronic heart failure: acute effects of the endothelin receptor antagonist Ro 47:0203 (Bosentan). Circulation 90: 2510–2518.
Minamino T, Kurihara H, Takahashi M, Shimada K, Maemura K, Oda H, Ishikawa T, Uchiyama T, Tanzawa K, Yazaki Y 1997 Endothelin-converting enzyme expression in the rat vascular injury model and human coronary atherosclerosis. Circulation 95: 221–230.
Matsuura A, Kawashima S, Yamochi W, Hirata K, Yamaguchi T, Emoto N, Yokoyama M 1997 Vascular endothelial growth factor increases endothelin-converting-enzyme expression in vascular endothelial cells. Biochem Biophys Res Commun 235: 713–716.
Michael JR, Markewitz BA 1996 Endothelins and the lung. Am J Respir Crit Care Med 154: 555–581.
Author information
Authors and Affiliations
Additional information
This research was supported by grant 97–212 from the American Heart Association, Western States Affiliates (S.M.B.), grant HL60190 from the National Heart, Lung, and Blood Institute (S.M.B.), grant 9640010N EIA from the American Heart Association (J.R.F.), grant FY97–0175 from the March of Dimes (J.R.F.), and grant HL 35518 from the National Heart, Lung, and Blood Institute (S.J.S.).
Rights and permissions
About this article
Cite this article
Black, S., Bekker, J., Johengen, M. et al. Altered Regulation of the ET-1 Cascade in Lambs with Increased Pulmonary Blood Flow and Pulmonary Hypertension. Pediatr Res 47, 97 (2000). https://doi.org/10.1203/00006450-200001000-00018
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200001000-00018
This article is cited by
-
Pulmonary hypertension associated with vein of Galen malformation. Fetal cardiac hemodynamic findings and physiological considerations
Journal of Perinatology (2022)
-
HIF-1α promotes cellular growth in lymphatic endothelial cells exposed to chronically elevated pulmonary lymph flow
Scientific Reports (2021)
-
Plasma endothelin-1 and nitrate levels in Down’s syndrome with complete atrioventricular septal defect-associated pulmonary hypertension: a comparison with non-Down’s syndrome children
European Journal of Pediatrics (2009)