Abstract
Neonates are unusually susceptible to herpes simplex virus infection, which may be explained in part by defects in killing of herpes simplex virus–infected cells by natural killer (NK) cell cytotoxicity and antibody-dependent cellular cytotoxicity. The mechanism for these defects remains poorly defined. We have for the first time used immunomagnetically enriched NK cells to explore neonatal NK cell phenotype and target cell adhesion. CD56-positive neonatal NK cells had markedly lower CD57 expression, but adult level expression of adhesive glycoproteins (CD18, CD44) and Fc receptor for IgG (CD16). Although the cells conjugated normally with target cells in the absence of antibody, antibody-mediated conjugation was significantly lower than that of NK cells from adults (p< 0.002). These results demonstrate intact adhesion in neonatal NK cell cytotoxicity. In contrast, defective neonatal antibody-dependent cellular cytotoxicity is caused, in part, by an adhesion defect in the presence of antibody.
Similar content being viewed by others
Main
Human and many animal neonates are unusually susceptible to severe infection caused by HSV (1). The increased susceptibility is caused by multiple defects in the ability of their immune systems to contain and then cure the viral infection (2). Among these defects is included the ability of NK cells to destroy viral-infected cells in the absence of antibody, termed NKC, and in the presence of transplacentally acquired antiviral antibody, or ADCC (2, 3).
Although it has been well substantiated that human neonatal cells are deficient in NKC and ADCC, the underlying defects have not been delineated. This is in part because of the lack of reliable techniques for obtaining good yields of enriched neonatal NK cells. Indeed, almost all previous work on human neonatal NK cell function has used Ficoll-Hypaque–enriched PBMC preparations. In the work presented in this article, we used an immunomagnetic separation technique to obtain enriched neonatal NK cell preparations. We then explored the neonatal NK cell phenotype and binding ability to HSV-infected cells. Although neonatal CD56-positive NK cells had phenotypically intact IgG FcR, their ability to bind antibody-coated HSV-infected cells was markedly diminished.
METHODS
Target cells.
Chang liver cells were infected 18 h before use with HSV-HE strain type 1 at a multiplicity of infection of approximately two as previously described (4) in minimal essential media containing 10% heat-inactivated FCS (Atlanta Biologic, Norcross, GA), 100 U/mL penicillin, 100 μg/mL streptomycin, and 2 mM glutamine.
Preparation of adult and umbilical cord blood mononuclearcells.
Overnight adult buffy coat and cord blood samples were collected at the Stanford Blood Bank and Advanced Biologic Technologies Inc. (Alameda, CA), respectively. Cells were used within 8 h of collection. PBMC were isolated by density-gradient centrifugation with Ficoll-Hypaque (Pharmacia, Piscataway, NJ) as previously described (5). Cells were washed three times in PBS solution (without Ca2+ and Mg2+) and suspended in PBS supplemented with 5% FCS.
Enrichment of NK cells.
We followed the manufacturer's instruction to enrich NK cells from mononuclear cell preparation by high-affinity negative selection to minimize potential activation of cells associated with positive selection techniques (Stem Cell Technology, Vancouver, BC). NK cells were isolated using sensitization with bispecific tetrameric antibody cocktails to sensitize unwanted cells by subsequent coating of targeted cells with dextran-coated colloidal iron that were then bound to an iron-mesh column by a powerful magnet (Stem Cell Technology). Briefly, 10 × 107 PBMC in 1 mL PBS and 5% FCS were incubated for 15 min with 100 μL of NK cell enrichment bispecific antibody cocktail (containing antibodies to CD3, CD4, CD8, CD14, CD19, CD66, glycophorin A, and dextran). The mixture was then incubated for another 15 min at room temperature with 60 μL of colloid iron coated with dextran. For magnetic cell separation, samples were loaded into a primed and washed iron-mesh column and suspended in a magnet. The flow through containing NK-enriched cells was collected.
Flow cytometry.
Purified NK cells were incubated with FITC- or phycoerythrin-conjugated mouse anti-human MAb to CD3, CD4, CD16, CD 44, CD56, and CD57 (Coulter Immunotech, Miami, FL) and CD18 and NKB1 (Becton Dickinson, San Jose, CA) for 15 min at room temperature. Cells were washed in FACS buffer (PBS:1% FCS:0.01% sodium azide) and fixed in 0.5% paraformaldehyde. Stained cells were analyzed with a FACS flow cytometer (Becton Dickinson). Quadrants were set by analysis of cells incubated with FITC- and phycoerythrin-conjugated isotype-matched control antibodies.
Single cell binding assay.
Effector (NK) and HSV-infected target cells (at 6 × 105/mL) were added to Eppendorf microcentrifuge tubes at 1:1 effector to target cell ratio in 90 μL of volume each. Anti-HSV sera was a pool of sera from three individuals with recurrent oral HSV. It was positive for HSV antibody by ADCC (titer 10−4) and neutralization (titer 1:32). The HSV-negative sera was a pool of sera from three individuals without a history of HSV and no reaction in ADCC or neutralization. Anti-HSV antibody-negative and -positive sera were then added in a volume of 20 mL for a final dilution of 1:1000. Preliminary experiments determined this as the optimal dilution for conjugation without target cell agglutination. Concentration of antibody of 1:100 or less caused spontaneous target cell adhesion to target cells. Concentrations of 1:10 000 resulted in lower target cell binding. The mixture was centrifuged for 5 min at 200 ×g. Ninety microliters of supernatant was removed, and the pellet was gently resuspended. A counting chamber was loaded with an aliquot of a 1:1 mixture of the cell suspension in trypan blue. Total number of effector cells and bound effector cells to target cells were counted. One hundred effector cells were counted.
Percent of NK cell binding to target cells were calculated as MATH Corrected adhesion was calculated as MATH Percent adhesion index was calculated as MATH



Statistics.
Comparison of paired data were by the two-tailed paired t test. All results reported are from separate adult and cord blood samples.
RESULTS
NK cell enrichment.
Table 1 delineates the purity and recovery of CD56-positive NK cells from adult and cord blood PBMC by immunomagnetic separation. Beginning with 5–10% NK cells in PBMC, the enrichment was typically 10-fold, with no significant difference in purity between cord blood and adult blood enriched NK cells as defined by CD56-positive cells (Table 1). Of interest was the almost 100% increased recovery of cord blood compared with adult NK cells from PBMC (p< 0.005). Thus this separation proved to be a reliable and practical one to obtain a high-yield and relative high-purity population of neonatal NK cells.
NK cell phenotype.
Table 2 delineates the phenotype of immunomagnetically enriched NK cells from adult and cord blood. There was a markedly lower expression of CD57 on cord blood NK cells compared with NK cells from adults (p< 0.006). The expression of the IgG FcR (CD16), the adhesive molecules CD44, and of the β-2 integrin family (represented by the common β-chain CD18) was nearly identical in adult and cord blood NK cells and was exhibited on almost all NK cells (Table 2). Similarly, the expression of the KIR, NKB1, was slightly but not significantly lower in cord NK cells compared with adult NK cells (Table 2).
Adhesion of NK cells to HSV-1 infected target cells.
NK cells were tested for their ability to adhere to HSV-1–infected target cells in the absence of antibody (the initiation of NKC) and the presence of antibody (the initiation of ADCC). Table 3 delineates the antibody-independent adhesion of enriched NK cells. Both adhesion of NK cells and adhesion corrected by NK purity were similar for adult and cord blood immuomagnetically enriched NK cell populations. Thus, no defect was noted in antibody-independent adhesion to HSV-infected cells.
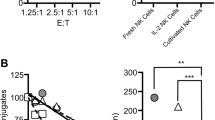
Table 4 delineates the antibody-mediated adhesion of enriched NK cells of cord and adult blood. In contrast to the results in the absence of antibody, there was a 2.3-fold increase in adult NK cell adhesion in the presence of antibody and only a 1.4-fold increase in cord NK cell adhesion (Table 4). The adhesion, corrected adhesion, and adhesion index were all statistically significantly lower in cord blood enriched NK cell preparations (Table 4). Figure 1 is a graphic representation of the binding of the NK preparations in the presence of HSV-negative and -positive antibody. Again, the binding in the absence of antibody is similar with cord and adult NK cells. The additional target cell binding in the presence of anti-HSV antibody with adult but not cord blood NK cell preparations can be easily appreciated (Fig. 1).
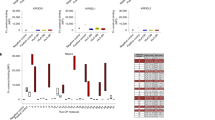
Because CD16 is one of the main determinants of antibody-mediated binding, and initial results revealed similar expression of CD16 on cord and adult NK cells (Table 2), further analysis of CD16 expression was performed. Figure 2 illustrates the expression of CD16 by FACS analysis of cord and adult NK cells with diminishing dilutions of anti-CD16 antibody. There was clearly no deficiency of CD16 expression of cord blood NK cells even at low concentrations of anti-CD16 antibody (Fig. 2), excluding defective expression of CD16 as the cause of diminished antibody-mediated target cell binding.
Expression of CD16 on NK cells of cord and adult NK cell preparations. The expression of CD16 by FACS analysis (fraction positive) on cord (closed squares) and adult (open circles) NK cell preparations (mean ± SEM of four experiments from different samples) is shown at dilutions of anti-CD16 antibody of 5 to 0.005 μL/mL.
DISCUSSION
NK cell activity is believed to be an important part of the immune response to viral infection (2, 3, 6). Neonates (2, 3, 7, 8) and others such as renal transplant patients (9) or individuals with absent NK cells (10) or absent NK cell killing (11) are unusually susceptible to HSV infection. Multiple studies have documented low NK cytotoxic function in neonates using bulk PBMC preparations (2, 3, 5–8, 12–17). The defects are magnified in preterm infants who are exceptionally susceptible to viral infection (18).
Neonates have similar or higher percentages of NK cells in their blood as determined by morphologic and phenotypic markers (CD56, CD16) (19–21). Although one study reported that low levels of NK cells in neonatal PBMC preparations were associated with low NKC (19), we could not confirm those results using enriched NK cell preparations. In two experiments involving enriched NK cell preparations at an effector ratio of 30:1 from adults and neonates, both with 25% CD56-positive cells, the NKC to HSV-infected cells was 0 ± 0 for cord cells and 10 ± 7.0 for adult cells, whereas the ADCC was 27.5% ± 3.5 for cord cells and 45% ± 0 for adult cells. Similar results were seen at effector ratios of 60:1 and using K562 cells (cord, 10% NKC; adult, 25% NKC; in one experiment). Thus, the analysis of defective NKC must rely on delineation of cellular function.
In the studies reported here, immunomagnetic enrichment of CD56-positive NK cells is used. We have demonstrated this to be a rapid and practical technique to obtain a high yield of relatively enriched neonatal NK cells (Table 1). Indeed, the yields were higher from neonatal than adult PBMC preparations. Although this may raise the possibility that a subpopulation of adult NK cells were lost, this did not seem to be the case, as demonstrated by phenotypic analysis compared with neonatal cells (Table 2).
Phenotypic analysis confirmed previous work demonstrating a markedly lower expression of CD57 in cord blood NK cells (21–23). CD57 is an oligosaccharide with no known function or ligands at this writing. Antibody to CD57 does not block NKC activity (Ryan J, personal communication). Thus, low CD57 expression is not likely to explain defective neonatal NK cell function. Expression of adhesive glycoproteins CD18 and CD44, which are important adhesive glycoproteins for cytotoxicity (24, 25), and of the immunoglobulin receptor (FcRIII, CD16) on neonatal NK cells was equivalent to that of adults, and nearly uniform on CD56-positive cells (Table 2, Fig. 2). Thus, our finding of antibody-mediated adhesive defects remains undefined (Table 4).
This is the first well-substantiated description of an antibody-mediated recognition or adhesive defect in enriched neonatal CD56-positive NK cells, although we previously provided preliminary data of a similar defect using neonatal PBMC (26). With an adhesion percentage of only 2–3%, those data were much less robust. This finding of an adhesion defect in part explains low ADCC to HSV-infected cells, an antibody-mediated phenomenon. It would be logical to assume this defect to be related to FcRIII in neonatal NK cells. Neonatal FcR expression has been only recently studied. El-Mohandes et al. (27) have reported low expression of FcRII on neonatal monocytes, and Payne and Fleit (28) have reported low FcRIII (CD16) on polymorphonuclear leukocytes of extremely low birth weight neonates. Our report of normal expression of FcRIII on cord blood NK cells does not preclude functional defects. Indeed, it has been shown in a patient with severe HSV infections that enumeration of FcRIII using the same MAb (3G8) as we used may miss a functional defect, when analyzed by other antibodies (29). This would necessitate hypothesizing a generalized expression of a functionally defective FcRIII in neonates that then shifts to a functional molecule with age. Although unlikely, further analysis of neonates' NK cell CD16 by other antibodies and IgG binding techniques could test this hypothesis.
Analysis of binding of neonatal NK cells to target cells in the absence of antibody has been controversial and hampered by the use of bulk PBMC. Studies have shown both diminished and normal binding (23, 26, 30–32). Our studies demonstrated adult levels of binding to HSV-1 target cells (Table 3, Fig. 1), confirming more recent reports pointing toward a defect in the lytic machinery of NKC. Indeed, several older studies using PBMC of neonates have reported decreased expression of the ill-defined NKC factor (30) and of cytoplasmic granules in large granular lymphocytes (33). Neonates' PBMC have been shown able to up-regulate mRNA expression for perforin and granzymes A and B, components of lytic activity (32), but this has not been quantitatively compared with their adult counterparts.
Of recent interest has been the description of KIRs, which interact with HLA molecules of self to inhibit NKC (34). One possible mechanism for defective neonatal NKC activity would be overexpression of KIR or hyperactivity of KIR. At least by phenotypic analysis of one common KIR, NKB1, overexpression of KIR does not seem to account for low neonatal NKC (Table 2). This does not exclude hyperactivity of KIR or overexpression of other KIR molecules, such as CD 94/NKG. It is also of interest that HSV interferes with the transport of HLA class 1 to cell surfaces (35). Although not directly measured in this cell system, it may account for high NKC to HSV-infected cells.
Thus, we can hypothesize a signal transduction or lytic defect in neonatal NKC and at least a recognition or binding defect in neonatal ADCC. Further molecular analysis of these defects using purified cell populations will likely delineate the underlying molecular mechanisms. This may point toward cytokine reconstitution of these defects with possible amelioration of the risks of severe HSV infection in high-risk neonates.
Abbreviations
- HSV:
-
herpes simplex virus
- NK:
-
natural killer
- NKC:
-
natural killer cell cytotoxicity
- ADCC:
-
antibody-dependent cellular cytotoxicity
- PBMC:
-
peripheral blood mononuclear cells
- FcR:
-
Fc receptor
- FACS:
-
fluorescent activated cell sorter
- KIR:
-
killer inhibitory receptor
- NKB1:
-
subtype of killer inhibitory receptor
References
Kohl S 1997 Neonatal herpes simplex virus infections. Clin Perinatol 24: 129–150
Kohl S 1989 The neonatal human immune response to herpes simplex virus: a critical review. Pediatr Infect Dis J 8: 67–74
Kohl S 1991 Role of antibody-dependent cellular cytotoxicity in defense against herpes simplex virus infection. Rev Infect Dis 13: 108–114
Kohl S, Stryndaka NCJ, Hodges RS, Pereira L 1990 Analysis of the role of antibody activity in murine neonatal herpes simplex virus infection with antibodies to synthetic peptides of glycoprotein D and monoclonal antibodies to glycoprotein B. J Clin Invest 86: 273–278
Jenkins M, Mills J, Kohl S 1993 Natural killer cytotoxicity of HIV-infected cells by leukocytes form human neonates and adults. Pediatr Res 33: 469–474
Trinchieri G 1989 Biology of natural killer cells. Adv Immunol 47: 187–376
Kohl S, Shaban SS, Starr SE, Wood PA, Nahmias AJ 1978 Human neonatal and maternal monocyte-macrophage and lymphocyte-mediated antibody–dependent cytotoxicity to cells infected with herpes simplex. J Pediatr 93: 206–210
Kohl S, Harmon MW 1983 Human neonatal leukocyte interferon production and natural killer cytotoxicity in response to herpes simplex virus. J Interferon Res 3: 401–463
Greenberg MS, Friedman M, Cohen SG, Oh SH, Laster L, Starr S 1983 A comparative study of herpes simplex infections in renal transplant and leukemic patients. J Infect Dis 156: 280–287
Biron CA, Byron KS, Sullivan JL 1989 Severe herpes virus infections in an adolescent without natural killer cells. N Engl J Med 320: 1731–1735
Komiyama A, Kawai H, Akihiko Y, Yanagisawa M, Miyagawa Y, Ota M, Hasekura H, Akabane T 1990 Natural killer cell deficiency in siblings: defective killing in the absence of natural killer cytotoxic factor activity in natural killer and lymphokine-activated killer cytotoxicities. Pediatrics 85: 323–330
Kohl S, Loo LS 1980 Ontogeny of murine cellular cytotoxicity to herpes simplex virus-infected cells. Infect Immun 30: 847–850
McConnachie PR, Rachelefsky G, Stiehm ER, Terasake PJ 1973 Antibody-dependent lymphocyte killer function and age. Pediatrics 52: 795–800
Kaplan J, Shope TC, Bollinger RO, Smith J 1982 Human newborns are deficient in natural killer activity. J Clin Immunol 2: 350–355
Uksila J, Lassila O, Hirvonnen T 1982 Natural killer cell function of human neonatal lymphocytes. Clin Exp Immunol 48: 649–654
Lubens RG, Gard SE, Soderberg-Warner M, Stiehm ER 1982 Lectin dependent T-lymphocyte and natural killer cell cytotoxic deficiencies in human newborns. Cell Immunol 74: 40–53
Chin TW, Ank BJ, Murakami D, Gill M, Spina C, Strom S, Stiehm ER 1986 Cytotoxic studies in human newborns: lessened allogeneic cell-induced (augmented) cytotoxicity but strong lymphokine-activated cytotoxicity of cord mononuclear cells. Cell Immunol 103: 241–251
Merrill JD, Sigaroudinia M, Kohl S 1996 Characterization of natural killer and antibody-dependent cellular cytotoxicity of preterm infants against human immunodeficiency virus-infected cells. Pediatr Res 40: 498–503
Sancho L, de la Hera A, Casas J, Vaquer S, Matrinez C, Alvarez MM 1991 Two different maturational stages of natural killer lymphocytes in human newborn infants. J Pediatr 119: 446–454
McDonald T, Sneed J, Valenski WR, Dockter M, Cooke R, Herrod HG 1992 Natural killer cell activity in very low birth weight infants. Pediatr Res 31: 376–380
Abo T, Miller CA, Balch CM 1984 Characterization of human granular lymphocyte subpopulations expressing HNK-1 (Leu-7) and Leu-11 antigens in the blood and lymphoid tissues from fetuses, neonates and adults. Eur J Immunol 14: 616–623
Bradstock KF, Luxford C, Grimsely PG 1993 Functional and phenotypic assessment of neonatal human leucocytes expressing natural killer cell-associated antigens. Immunol Cell Biol 71: 535–542
Yabuhara A, Kawai H, Komiyama A 1990 Development of natural killer cytotoxicity during childhood: marked increases in number of natural killer cells with adequate cytotoxic abilities during infancy to early childhood. Pediatr Res 28: 316–322
Matsumoto G, Nghiem MP, Nozaki N, Schmits R, Penninger JM 1998 Cooperation between CD44 and LFA-1/CD11a adhesion receptors in lymphokine-activated killer cell cytotoxicity. J Immunol 158: 5781–5789
Yago T, Tsukuda M, Fukushima H, Yamaoka H, Kurata-Miura K, Nishi T, Minami IL 1998 IL-12 promotes the adhesion of NK cells to endothelial selectins under flow conditions. J Immunol 161: 1140–1145
Kohl S, Loo LS, Gonick B 1984 Analysis in human neonates of defective antibody-dependent cellular cytotoxicity and natural killer cytotoxicity to herpes simplex virus infected cells. J Infect Dis 150: 14–19
El-Mohandes AA, Rivas RA, Kiang E, Wahl LM, Katona IM 1995 Membrane antigen and ligand receptor expression on neonatal monocytes. Biol Neonate 68: 308–317
Payne NR, Fleit HB 1996 Extremely low birth weight infants have lower Fc gamma RIII (CD16) plasma levels and their PMN produce less Fc gamma RIII compared to adults. Biol Neonate 69: 235–242
de Vries E, Koene HR, Vossen JM, Gratama JW, von dem Borne AEGK, Waaijer JLM, Haraldsson A, de Haas M, van Tol MJD 1996 Identification of an unusual Fc gamma receptor IIIa (CD16) on natural killer cells in a patient with recurrent infections. Blood 88: 3022–3027
Nair MPN, Schwartz SA, Menon M 1985 Association of decreased natural and antibody-dependent cellular cytotoxicity and production of natural killer cytotoxic factor and interferon in neonates. Cell Immunol 94: 159–171
Baley JE, Schacter BZ 1985 Mechanisms of diminished natural killer cell activity in pregnant women and neonates. J Immunol 134: 3043–3048
Webb BJ, Bochan MR, Montel A, Padilla LM, Brahmi Z 1994 The lack of NK cytotoxicity associated with fresh HUCB may be due to the presence of soluble HLA in the serum. Cell Immunol 159: 246–361
Abo T, Cooper MD, Balch CM 1982 Postnatal expansion of the natural killer and killer cell population in humans identified by the monoclonal HNK-1 antibody. J Exp Med 155: 321–326
Lanier LL 1997 Natural killer cells: from no receptor to too many. Immunity 6: 371–378
Hill AB, Barnett BC, McMichael AJ, McGeach DJ 1994 HLA class I molecules are not transported to the cell surface in cells infected with herpes simplex virus types 1 and 2. J Immunol 152: 2736–2741
Acknowledgements
The authors thank Terry Olesen for fine manuscript preparation, Patty Lovelace and Annika vanVollhoven for FACS analysis, and Luis Soares and Alberto Rivas for technical suggestions.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Kohl, S., Sigouroudinia, M. & Engleman, E. Adhesion Defects of Antibody-Mediated Target Cell Binding of Neonatal Natural Killer Cells. Pediatr Res 46, 755 (1999). https://doi.org/10.1203/00006450-199912000-00018
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199912000-00018
This article is cited by
-
Does IVIg administration yield improved immune function in very premature neonates?
Journal of Perinatology (2010)