Abstract
Pulmonary hypoplasia has been found in the human neonatal autopsy population and has been attributed to an alteration in epithelial-mesenchymal interactions during development of the lung. Pulmonary acinar aplasia is a very rare and severe form of pulmonary hypoplasia. The transforming growth factor-betas (TGF-β) are multifunctional regulatory peptides that are secreted by a variety of normal and malignant cells and are expressed in developing organs including the lung; their tissue distribution patterns have possible significance for signaling roles in many epithelial-mesenchymal interactions. Here, we report our examination of TGF-β in the lungs of a term female infant diagnosed with pulmonary acinar aplasia whose autopsy revealed extremely hypoplastic lungs with complete absence of alveolar ducts and alveoli. Immunohistochemical and in situ hybridization analyses were used to localize and measure the proteins and mRNA, respectively, for TGF-β1, TGF-β2, TGF-β3, and TGF-β type I and type II receptors (TGF-β RI and RII) in formalin-fixed and paraffin-embedded sections of these hypoplastic lungs and normal lungs. Immunostaining for TGF-β1, TGF-β2, and TGF-β RI and RII was significantly lower in the bronchial epithelium and muscle of the hypoplastic lungs than in normal lungs, whereas no difference was detected in staining for other proteins including Clara cell 10-kD protein, adrenomedullin, hepatocyte growth factor/scatter factor, and hepatocyte growth factor receptor/Met in the hypoplastic and normal lungs or in the liver and kidneys of this infant compared with normal liver and kidney. In addition, in situ hybridization showed that TGF-β1 and TGF-β RI transcripts were considerably reduced in the bronchial epithelium of the hypoplastic lung compared with normal lung. These results show that there is a selective reduction of TGF-β in pulmonary acinar aplasia and suggest that the signaling action of TGF-β in epithelial-mesenchymal interactions in the lungs of this developmental condition may be compromised.
Similar content being viewed by others
Main
The lung is impressive both for its high rate of biosynthetic activity and for its high level of functional stability(1,2). The preservation of a steady equilibrium in the presence of the intense metabolic rate of the lung requires a fine-tuned interplay of many different cell types. Respiratory epithelial cells of the lung undergo dramatic morphologic and biochemical differentiation during the different phases of development. Distinct cell types are generated from the undifferentiated cuboidal epithelial cells lining the respiratory tract of the fetal lung, ultimately producing a variety of cell types including ciliated, mucous, basal, and nonciliated Clara cells, and alveolar type I and type II cells. Many of the cell-cell interactions in the lung are thought to be mediated by polypeptide growth factors, which control a wide range of cellular activities including proliferation, differentiation, chemotaxis, and extracellular matrix production(3). The transforming growth factor-β (TGF-β) family of proteins represents one set of growth factors that regulates cellular activities in the lung [for a review, see Pelton and Moses(4)]. There highly homologous, yet distinct, isoforms of TGF-β, TGF-β1, TGF-β2, and TGF-β3, have been identified in humans [for reviews, see Roberts and Sporn(5) and Massague(6)]. The activities of TGF-β in the lung are many and diverse and included both stimulatory and inhibitory effects. The temporal and differential cellular localization of TGF-β mRNA synthesis and protein expression in lung tissue provides evidence for a regulatory role for TGF-β in cellular processes in the lung(4).
Many different types of cells have been demonstrated to synthesize TGF-β, and essentially all cells have been shown to have a specific set of receptors for this growth factor. The TGF-β exert their effects through binding to these specific cell surface receptor proteins. Three major types of TGF-β receptors, type I (RI), type II (RII), and type III (RIII), have been identified in most cells and have been defined by their ability to bind and cross-link 125I-TGF-β [for reviews, see Derynck(7), Massague(8), and Hoodless and Wrana(9)]. Both TGF-β RI and RII have been determined to be required for TGF-β-induced signaling(10,11). In contrast, TGF-β RIII may be involved in presenting TGF-β ligand to TGF-β RI and RII, but does not directly mediate TGF-β signaling(12). TGF-β RI and RII have the ability to interact and form a tetrameric complex in the presence of ligand, and this heteromeric complex is thought to be the signaling unit responsible for mediating the biologic responses of TGF-β(13,14).
A number of patterns of maldevelopment of pulmonary tissue before birth have been described, ranging from the extremely rare condition of bilateral pulmonary agenesis to congenital cystic adenomatoid malformation (CCAM), which may occupy an entire lung, and pulmonary hypoplasia of varying degrees of severity(15–18). In the neonatal autopsy population, the most common form of pulmonary maldevelopment is hypoplasia. Although hypoplasia is a multifaceted and multicausal phenomenon, most forms of pulmonary hypoplasia are characterized at the morphologic level by a reduction in the number of generations of bronchi, small lungs, and, with the exception of decreased radial alveolar counts, relatively normal histologic development(19). This may be accompanied by a decrease in the number or size of terminal respiratory units.
Pulmonary acinar aplasia is a very rare and severe form of pulmonary hypoplasia. It was termed acinar dysplasia by Rutledge and Jensen in 1986(20) when a term neonate died of respiratory failure and autopsy revealed small lungs. Chambers reported in 1991(21) a case termed acinar aplasia in another term infant who also died of respiratory failure in which the lungs at autopsy were characterized by almost total failure of development of terminal respiratory units; this case suggested an arrest of pulmonary growth early in the second trimester. Similarly, Davidson et al.(22) reported a case of congenital acinar dysplasia and concluded that this malformation is a sporadic, lethal developmental defect. CCAM of the lung also encompasses a variety of variably cystic developmental anomalies histologically characterized by immature lung tissue(16–18,23,24).
In the present study, we examined the expression of the proteins and mRNA for the TGF-β ligands and receptors using immunohistochemical staining and in situ hybridization analyses, respectively, in a term neonate who died of pulmonary acinar aplasia and whose autopsy revealed extremely hypoplastic lungs with complete absence of alveolar ducts and alveoli. This is the first description of the localization of the TGF-β ligands and receptors in this developmental condition. Our data show significantly reduced immunostaining for TGF-β1, TGF-β2, and TGF-β RI and RII proteins and for TGF-β1 and TGF-β RI mRNA in the bronchial epithelium of the hypoplastic lungs compared with normal lungs. No significant difference was detected for expression of the TGF-β ligand and receptor proteins and mRNA in the liver or kidneys of the neonate with hypoplastic lungs compared with normal neonatal liver and kidney. Our results indicate that the signaling action of TGF-β in the lungs of this developmental condition may be compromised, suggesting that deregulation of TGF-β expression may be involved in the cause of hypoplastic lung malformation.
METHODS
Clinical history. A 2730-g female infant was born to a 23-y-old gravida 2, para 0, abortus 1, mother at 37-wk gestational age. The maternal history was unremarkable, with normal fetal ultrasound examination. The delivery was performed with low forceps, and Apgar scores were 2, 3, and 4 at 1, 5, and 10 min, respectively. Immediate respiratory resuscitation was necessary, and despite all efforts, the infant died at 2 h 24 min after birth. Autopsy was performed 24 h after death. A second term infant who died to asphyxia from placental infarction was used as a control. Portions of the lungs, liver, and kidneys were removed, immersed in 10% neutral buffered formalin for 24 h, dehydrated, embedded in paraffin, and cut in 5-µm sections. The sections were mounted onto slides treated with poly-L-lysine or silane for immunohistochemical staining and in situ hybridization analyses, respectively. One section from each lung, liver, and kidney was stained with hematoxylin and eosin and examined for histologic diagnosis by light microscopy. Human studies were approved by the National Cancer Institute Institutional Review Board.
Immunohistochemistry. For the immunocytochemical localization of TGF-β ligands and receptors in paraffin sections, the avidin-biotin complex technique was used (Vector Laboratories, Burlingame, CA). Affinity-purified polyclonal antibodies were purchased from Santa Cruz Biotechnology (Santa Cruz, CA) and included TGF-β1(V) for TGF-β1, TGF-β2(V) for TGF-β2, TGF-β3(III) for TGF-β3, TGF-βRI(V-22) for TGF-β RI, TGF-β RII(L-21) for TGF-β RII, C-20 for hepatocyte growth factor (HGF)/scatter factor (SF), and C-28 for HGF receptor (HGFR)/Met. Polyclonal antibodies to Clara cell 10-kD protein (CC10; urine protein 1; A0257) were purchased from Dako (Carpinteria, CA). A previously reported, well-characterized rabbit antiserum (No. 2343) was used to localize adrenomedullin (AM) immunoreactivity(25). After deparaffinization and blocking of endogenous peroxidase in hydrogen peroxide/methanol, the sections were blocked with 1.5% normal goat serum/0.5% BSA, incubated overnight at 4°C with affinity-purified antisera at 0.5 µg/mL, washed extensively, and then incubated with biotinylated goat anti-rabbit IgG and avidin-enzyme complex. Sections were stained with 3,3′-diaminobenzidine (Sigma Chemical Co, St. Louis, MO) and hydrogen peroxide for 4 min, and counterstained with Mayer's hematoxylin. Hypoplastic and normal lung sections were stained with each antibody at the same time using identical conditions. After immunostaining, the tissues were viewed, analyzed, and photographed on an Olympus microscope with imaging attachments (Millerville, NY). A control included using primary antisera preincubated with a 20-fold excess of the appropriate peptide.
Reverse transcription-polymerase chain reaction amplification. The oligonucleotide primers were synthesized using a MilliGen/Biosearch 8700 DNA synthesizer (Millipore, Marlborough, MA). Primer sets were as follows: TGF-β1 (precursor and mature): 448-bp product (1447-1894), sense: 5′-CGGAGTTGTGCGGCAGTGGTTGA-3′, antisense: 5′-GGCGCCCGGGTTATGCTGGTTGTA-3′; TGF-β2 (5′UTR): 439-bp product (-379-60), sense: 5′-TCCGCACCCGAGACTGACA-3′, antisense: 5′-GCTGAGCGCGACCGTGACCA-3′; TGF-β3 (3′UTR): 435-bp product (1762-2196), sense: 5′-TGGGGATAGAGGAAAGGGATGGTA-3′, antisense: 5′-GAGGGCAGACAGGAGAGGGTTGAT-3′; TGF-β RI (intracellular): 420-bp product (799-1218), sense: 5′-GTGGTTCCGTGAGGCAGAGATTTA-3′, antisense: 5′-GGGGCCATGTACCTTTTTGTTCC-3′; and TGF-β RII (intracellular): 410-bp product (903-1312), sense: 5′-CGCGTTAACCGGCAGCAGAAG-3′, antisense: 5′-GCGGTGATCAGCCAGTATTGTTT-3′.
Reverse transcription-polymerase chain reaction amplification (RT-PCR) was performed using 2 µg of total RNA from human normal bronchial epithelial cells (Clonetics, San Diego, CA) and the GeneAmp RNA PCR kit according to the manufacturer's directions (Perkin Elmer/Cetus, Norwalk, CT). The reverse transcription (RT) procedure was performed using the antisense primers with the following conditions: RT at 42°C for 50 min, inactivation of reverse transcriptase at 70°C for 15 min, and RNase H digestion at 37°C for 20 min. After RT, PCR was performed using the sense primers in a Perkin Elmer 9600 thermal cycler as follows: 94°C for 15 s, 60°C for 15 s, and 72°C for 1 min for 30 cycles followed by a 10-min incubation at 72°C. To visualize the PCR products, the samples were subjected to electrophoresis on 2% agarose gels containing ethidium bromide. The authenticity of the products was confirmed by Southern blot hybridization with nested internal primers and DNA sequencing.
In situ hybridization. Detection of the mRNA for the TGF-β ligands and receptors was performed using in situ hybridization as described previously(26). The cDNA generated using RT-PCR as outlined previously for the TGF-β ligands and receptors were ligated into the pcDNA1 vector (Invitrogen, San Diego, CA) following the manufacturer's procedures and used to generate riboprobes. The plasmids were linearized with EcoRV and BamHI and used as templates to synthesize digoxigenin-labeled sense and antisense RNA transcripts. Hybridization was performed in a moist chamber at 65°C for 20 h in a 50-µL volume containing the antisense probes. After stringency washes, visualization of digoxigenin was performed using a digoxigenin detection kit (Boehringer Mannheim, Indianapolis, IN). Sense probes were used as controls. Hypoplastic and normal lung sections were hybridized with cRNA probes and detection of digoxigenin staining was performed at the same time using identical conditions.
Statistical analysis. The data were expressed as the mean and SEM. Statistical significance between hypoplastic and normal lung values was tested by t test.
RESULTS
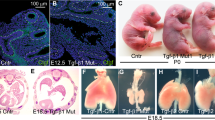
Autopsy and hematoxylin and eosin staining. Autopsy revealed an externally normal term female infant with extremely hypoplastic lungs. In addition, there was a cystic dysplastic right kidney and focal dysplasia in the cerebral and cerebellar cortices. Microscopically, Figure 1,A and C, shows hematoxylin and eosin staining of a representative portion of the lung of this infant. The lung showed virtually complete absence of airway development beyond the level of small bronchioles, which were normal and lined by ciliated cuboidal to ciliated columnar cells. There was complete absence of alveolar ducts and alveoli, and expansion of the interstitium with capillaries and prominent hematopoietic infiltrates. Cartilaginous rings were also unusually prominent around the bronchi. Bronchovascular bundles appeared to be haphazard in the parenchyma. Electron microscopic examination revealed the presence of normal cellular components of terminal bronchioles with no discernible alveolar epithelial differentiation (data not shown). Figure 1,B and D, shows hematoxylin and eosin staining of a normal lung of an infant for comparison. This lung shows the presence of normal alveoli, bronchi, and bronchioles.
TGF-β ligand and receptor immunohistochemistry. To investigate the localization of the TGF-β ligand proteins in these neonatal hypoplastic lungs, we examined the immunohistochemical staining patterns of TGF-β1, TGF-β2, and TGF-β3 using specific antibodies. Figure 2,A,E,and I, shows the immunohistochemical staining pattern of TGF-β1, TGF-β2, and TGF-β3, respectively, in the hypoplastic lung. Immunostaining for the three TGF-β isoforms was detected in the bronchiolar epithelium and interstitium, with that of TGF-β3 being more intense than that of TGF-β1 and TGF-β2. In comparison, Figure 2,B,C,F,G,J, and K, shows positive immunostaining for the three TGF-β isoforms in a normal neonatal lung. Intense positive staining for the three TGF-β isoforms was detected in the bronchial epithelium and developing respiratory epithelium. Less intense immunostaining was also detected in the smooth muscle cells surrounding the normal bronchi as well as in the surrounding alveoli (data not shown); staining for the three TGF-β isoforms in these structures was more intense in the normal lung than in the hypoplastic lung.
Expression of TGF-β1, TGF-β2, and TGF-β3 in neonatal hypoplastic and normal lung. Immunohistochemical detection of TGF-β1 (A-C), TGF-β2 (E-G), and TGF-β3 (I-K) in hypoplastic (A, E, and I) and normal lung (B, C, F, G, J, and K). Absorption controls for TGF-β1 (D), TGF-β2 (H), and TGF-β3 (L). Immunostaining in this and subsequent figures is representative of two separate experiments. Magnification: B, F, J ×40; A, C, D, E, G, H, I, K, L ×100.
The relative intensity of diaminobenzidine peroxidase product from TGF-β immunohistochemical analysis was measured by image analysis. Although image analysis is by no means quantitative or linear with respect to the amount of TGF-β protein present, this technique does provide a means to determine relative differences in staining intensity. Figure 3 shows that image analysis of TGF-β immunostaining provided values that confirmed the qualitative visual examination of the staining intensity in that there were statistically significant decreases (TGF-β1, 4,8-fold; TGF-β2, 5-fold; p < 0.05) in expression of TGF-β1 and TGF-β2 in the hypoplastic bronchi compared with normal bronchi. The 1.4-fold decrease in the staining intensity of TGF-β3 in the hypoplastic lung compared with normal lung was not significantly different. Immunohistochemical staining for TGF-β1, TGF-β2, and TGF-β3 was completely blocked when the antibodies were preincubated with solutions of peptides against which they were raised (Fig. 2,D,H, and L).
To examine the localization of TGF-β RI and RII in the neonatal hypoplastic lungs, the immunohistochemical staining patterns of TGF-β RI and RII were examined using specific antibodies. Figure 4,A and E, shows the immunohistochemical staining pattern of TGF-β RI and RII in the hypoplastic lungs. Like the TGF-β ligands, positive staining for TGF-β RI and RII was detected in the bronchial epithelium and interstitium. In comparison, Figure 4,B,C,F, and G, shows intense staining for TGF-β RI and RII in the normal bronchial epithelium and developing respiratory epithelium. Less intense immunostaining for both TGF-β receptors was also detected in the smooth muscle surrounding the bronchi; staining for TGF-β RI and RII was considerably more intense in the bronchial epithelium of the normal lung than in the hypoplastic lung. Like the TGF-β ligands, Figure 3 shows that image analysis of TGF-β RI and RII immunostaining provided values that confirmed the visual examination of the staining intensity, with statistically significant decreases (TGF-β RI, 8-fold; TGF-β RII, 4.4-fold; p < 0.05) in expression of both TGF-β receptors in the hypoplastic bronchi compared with normal bronchi. Immunohistochemical staining for TGF-β RI and RII was completely blocked when the antibodies were preincubated with solutions of peptides against which they were raised (Fig. 4,D and H).
In situ hybridization. To examine the tissue-specific distribution of the mRNA for the TGF-β ligands and receptors, in situ hybridization was performed on these hypoplastic and normal lung sections using nonradioactive digoxigenin-labeled cRNA probes. Hybridization with antisense and sense (negative control) cRNA probes and washing were performed at high stringency to ensure specific hybridization. Negative control sections were hybridized with sense TGF-β ligand and receptor cRNA probes. Figure 5,A,E, and G, shows prominent hybridization, as a purple precipitate, to TGF-β1, TGF-β RI, and TGF-β RII mRNA, respectively, in the bronchial epithelium of the hypoplastic lung. Expression of TGF-β RI and RII transcripts was also prominent in the surrounding smooth muscle of these lungs whereas that of TGF-β1 mRNA was not evident. Figure 5,C,G, and K, shows prominent hybridization to TGF-β1, TGF-β RI, and TGF-β RII mRNA in the bronchial epithelium and developing respiratory epithelium in the normal lung, with hybridization to TGF-β1 and TGF-β RI mRNA being more prominent in these structures in the normal lung than in the hypoplastic lung. Expression of TGF-β RII mRNA was similar in the bronchial epithelium of the hypoplastic and normal lung. However, expression of TGF-β RI and RII mRNA was more prominent in the smooth muscle surrounding the bronchi in the hypoplastic lung than in the normal lung. Although the pattern of localization of hybridization of TGF-β2 and TGF-β3 mRNA was similar to that of TGF-β1 mRNA in the hypoplastic and normal lung (data not shown), no difference was evident in expression of these TGF-β mRNA in hypoplastic and normal lung. Hybridization was also performed using digoxigenin-labeled sense TGF-β1 and TGF-β RI and RII cRNA probes as controls for specificity; Figure 5, B, D, F, H, J, and L, shows the absence of hybridization of these probes to the hypoplastic and normal lungs.
Expression of TGF-β1, TGF-β RI, and TGF-β RII mRNA in neonatal hypoplastic and normal lung. In situ hybridization for TGF-β1 mRNA (A and C), TGF-β RI mRNA (E and G), and TGF-β RII mRNA (I and K) in hypoplastic (A, E, and I) and normal (C, G, and K) lung. Sense controls for TGF-β1 (B and D), TGF-β RI (F and H), and TGF-β RII (J and L) in hypoplastic (B, F, and J) and normal (D, H, and L) lung. In situ hybridization in this figure is representative of three separate experiments. Magnification: A-L ×40.
Immunohistochemistry of other proteins. In addition to the TGF-β ligands and receptors, we also examined the immunohistochemical staining patterns of other proteins in the hypoplastic and normal lungs. The immunostaining patterns of CC10, AM, and HGFR/Met in hypoplastic (Fig. 6,A,C, and E) and normal (Fig. 6,B,D, and F) neonatal lung were examined. No differences were observed in the staining patterns of these three proteins in the hypoplastic and normal lungs. Also, no difference was observed in the staining pattern of HGF/SF in the hypoplastic and normal lung as well (data not shown). In addition to the lungs, expression of the TGF-β ligands and receptors was examined in the liver and kidneys of the infant with hypoplastic lungs and compared with that of a normal infant. No difference was detected in expression of the TGF-β ligands and receptors in these tissues (data not shown).
DISCUSSION
In the present study, we have examined the case of an extreme form of pulmonary maldevelopment of a term infant characterized by almost total failure of development of terminal respiratory units. During normal human embryonic development, the lung demonstrates distinct histologic and temporal phases of growth and differentiation after formation of the lung buds at 4 wk after conception(27). In the pseudoglandular phase, the lung buds branch and produce lobules composed of epithelial-lined tubules in loose mesenchyme, which takes place to the 14th week of gestation. This is followed by the canalicular phase, which occurs in the second trimester, in which there is an increase in the caliber of peripheral airways, an increase in muscularization of acini, vascularization of the mesenchyme, and the appearance of air spaces as saccular structures. After about 28 wk, there is a decrease in saccular wall thickness, in the amount of interstitial tissue, and in the size of distal air spaces, which subdivide and form the alveoli beginning after about 32 wk. If a disturbance occurs in any of these phases, lung maldevelopment may occur.
Three cases of pulmonary acinar aplasia have been previously reported(20–22). Ours is the fourth case of this rare and severe congenital condition. As in the previous cases, the infant was a term female with unaffected older siblings. Like the second and third reported cases(21,22), the lungs showed complete absence of alveolar structures and expansion of the interstitium with capillaries. Like the first and second case(20,21), our case showed prominent hematopoietic infiltrates in the lungs that were absent in the third case(22). Although the infant described in our study has some pathologic features that are similar to CCAM, this infant also has features that are different from this condition. These include the absence of pulmonary cysts, the presence of bronchiole-like structures with no cartilage or goblet cells, and the presence of prominent vascularity(24). Also, as was true of the three previous cases of pulmonary acinar aplasia, the infant in our study was female, whereas CCAM has been shown to display a slight male preference(17,18). In addition, the hypoplastic lungs described in our study were solid and showed an entire arrest of growth at the level of bronchioles, not just a partial arrest as has been shown in the majority of CCAM cases(16–18,23,24). These differences suggest that the infant described in our study is an example of pulmonary acinar aplasia and not of CCAM. Nonetheless, congenital lung abnormalities dominated by errors in histogenesis are infrequent. In our study, the arrest of pulmonary growth occurred at an early stage of development, very likely early during the pseudoglandular phase as in the other cases. It has been suggested that the defect may involve a failure of the peripheral mesenchyme to induce development of the terminal respiratory unit(20). The failure of this induction may, in turn, result from a defect in the ability of the epithelium to receive or respond to the inducing signals from the mesenchyme(20,24).
Epithelial-mesenchymal interactions have been implicated in branching morphogenesis of embryonic lung. Lung development begins with the outgrowth of paired lung buds from the foregut endoderm that invade the surrounding mesenchyme in a genetically predetermined pattern of branching morphogenesis and lung-specific cell differentiation [reviewed in Hilfer(28)]. The histogenesis of the lung is intimately dependent on proper interaction between epithelial elements and the macro-molecules of the extracellular matrix forming the mesenchyme(29). The branching morphogenesis of the lung, as well as that of the kidney and pancreas, is greatly influenced by the specific types of mesenchyme with which the epithelium may interact. Alterations of these interactions, or of one or more macromolecules important in pulmonary morphogenesis, may result in a halt in development.
A number of soluble polypeptide growth factors are potential mediators instructing primitive lung epithelial branching morphogenesis. In general, the growth factors that activate cognate receptors with tyrosine kinase intracellular signaling domains, such as epidermal growth factor, fibroblast growth factor, IGF, keratinocyte growth factor, platelet-derived growth factor, and HGF and its receptor HGFR/Met, exert inductive influences on lung development(30–36), whereas those growth factors that function through receptors with serine/threonine kinase signaling domains, such as the TGF-β, are inhibitory(37–39). Secreted signaling molecules such as TGF-β regulate cell growth, differentiation, and tissue morphogenesis through autocrine/paracrine signaling mechanisms(5–9). TGF-β induces growth arrest in several types of cells including lung epithelial cells, and expression of a wide array of proteins, some of which are deposited in the lung extracellular matrix. Expression of TGF-β in the lung has been studied for the most part in the mouse lung, and expression of the TGF-β ligands and receptors has been detected in the embryonic mouse lung at critical times during development(40,41). Specifically, during the pseudoglandular stage, TGF-β protein accumulates in the stroma along the proximal airways and underlying cleft points of epithelial branching and colocalizes with extracellular matrix proteins including fibronectin and type I and III collagen(40). It has been shown in several previous reports dealing with mouse, and in human embryos as well, that the TGF-β are expressed in embryonic epithelia undergoing intense morphogenetic interactions with the underlying mesenchyme(38,40–50). The expression of TGF-β1 in these structures is tightly regulated and restricted to particular cell types in any given stage of embryogenesis. In all cases in which TGF-β1 mRNA has been detected in epithelia, the protein has been found to be deposited in the underlying mesenchyme. This has led to the suggestion that TGF-β1 is involved in paracrine interactions with the underlying mesenchyme and that TGF-β1 facilitates epithelial-mesenchymal interactions in regions of morphogenesis. The expression pattern and known biologic activities of TGF-β suggest an important role for this growth factor in tracheobronchial development.
In the present study, we have examined the expression and localization of the TGF-β ligand and receptor proteins and their corresponding mRNA in neonatal pulmonary acinar aplasia and compared this with normal neonatal lung. We have shown that there is a reduction in expression of two TGF-β isoforms (TGF-β1 and TGF-β2) in the bronchial epithelium of the hypoplastic lungs compared with normal lung. In addition, there is a reduction in expression of TGF-β RI and RII proteins in the bronchial epithelium of the hypoplastic lungs compared with normal lung as well. The reduction in expression of the TGF-β ligands and receptors was shown to be localized and confined to the hypoplastic lungs; no difference was observed in the TGF-β ligands and receptors in the liver and kidneys of the infant with the hypoplastic lungs compared with normal neonatal liver and kidney. That reduction of the TGF-β ligands and receptors in the lungs was a specific event, and not merely a reduction of protein expression in general, was demonstrated by similar levels of expression of at least four other proteins that have been shown to be expressed in bronchial epithelium, including AM, CC10, HGF, and HGFR(25,51,52), in the hypoplastic and normal neonatal lung. This suggests that there are factors specifically influencing the developmental expression of TGF-β in the lung.
Reduction of TGF-β in the lung at an early time in embryogenesis may influence the pattern of morphogenesis of the lung. For example, endodermal branching is one of the major events in lung morphogenesis that is known to depend on the interaction of the epithelium with the mesenchyme and on the formation of an extracellular matrix at the interface of these tissues. It has been shown that branching does not occur in the absence of either the mesenchyme(53) or the extracellular matrix(54). Among the components of the extracellular matrix that have been implicated as being necessary for branching are the collagens, which are associated with the mesenchyme and the basement membrane of the epithelium(55,56), and the sulfated glycosaminoglycans, which are major components of mesenchyme and epithelial matrices(57). These extracellular matrix components are necessary for the initiation of endodermal branching and for the stabilization and maintenance of the newly formed tissue structures(58). Many of the actions of TGF-β are related to its ability to regulate the formation of extracellular matrix by mechanisms including increasing synthesis of the major components of the extracellular matrix, controlling their proteolytic degradation, and modulating the synthesis of integrin receptors that are important in the regulation of cell-matrix interactions(59–61). The presence of TGF-β1 at the epithelial-mesenchymal interfaces of lung branching at a time when extracellular matrix proteins can be first visualized in these areas in mouse lung embryogenesis suggests a direct participation of TGF-β in the development of the basic architecture of the lung. A reduction of TGF-β ligands and receptors at this time may likely influence the resulting architecture of the lung so that these extracellular matrix proteins may not be able to be induced at the correct time and in the correct quantity to permit normal development.
Although our study has shown reduced expression of TGF-β in pulmonary acinar aplasia, proof of a causal connection between reduction of TGF-β expression and inhibition of lung development will require additional studies. It is also possible that because the TGF-β and their receptors are spatially and temporally regulated, the reduced levels of their expression that were detected here at birth may not reflect the critical changes that resulted in pulmonary dysgenesis in this infant. Rather, this infant may possibly have a natural mutation of one of the many other genes that are critical in initiating the canalicular stage of lung development. The reduced expression of TGF-β may be the consequence and not the cause of such a mutation. Nevertheless, this is the first description of the localization of the TGF-β ligands and receptors in this developmental condition. The reduction in expression of the TGF-β ligand and receptor mRNA and proteins may be characteristic of this developmental anomaly. Our study suggests that other cases of pulmonary hypoplasia should be examined to determine whether dysregulation of TGF-β is an underlying theme of this condition. In addition, a number of mouse models involving targeted disruption of oncogenes and growth factors including N-myc, keratinocyte growth factor, HGF, and TGF-β3 have shown that these proteins have roles in branching morphogenesis of the embryonic mouse lung(38,52,62–64). Targeted expression of a dominant negative fibroblast growth factor receptor has been shown to block branching morphogenesis and epithelial differentiation in the mouse lung(22). To determine whether reduction of TGF-β is a cause or consequence of pulmonary acinar aplasia, it will be necessary to examine animal model systems of pulmonary hypoplasia along with future infant cases of this developmental condition.
Abbreviations
- TGF-β:
-
transforming growth factor-β
- AM:
-
adrenomedullin
- TGF-β RI and RII:
-
transforming growth factor-β receptor type I and II
- CC10:
-
Clara cell 10-kD protein
- CCAM:
-
congenital cystic adenomatoid malformation
- RT-PCR:
-
reverse transcription polymerase chain reaction
- HGF:
-
hepatocyte growth factor
- SF:
-
scatter factor
References
Fowler RW 1985 Aging and lung function. Age Aging 14: 209–215
Kelley J, Stirewilt WS, Chrin L 1985 Protein synthesis in rat lung: measurements in vivo based on leucyl-tRNA and rapidly turning-over procollagen. Biochem J 222: 77–83
King RJ, Jones MB, Minoo P 1989 Regulation of lung cell proliferation by polypeptide growth factors. Am J Physiol 257:L23–L38
Pelton RW, Moses HL 1990 The β type transforming growth factors: mediators of cell regulation in the lung. Am Rev Respir Dis 142:S31–S35
Roberts AB, Sporn MB 1990 The transforming growth factor-βs. In: Sporn MB, Roberts AB (eds) Handbook of Experimental Pharmacology. Peptide Growth Factors and Their Receptors. Springer-Verlag, Heidelberg, FRG, vol 95/I, pp 419–472
Massague J 1990 The transforming growth factor-β family. Annu Rev Cell Biol 6: 597–641
Derynck R 1994 TGF-β receptor-mediated signaling. Trends Biochem Sci 19: 548–553
Massague J 1996 TGFβ signaling: receptors, transducers and Mad proteins. Cell 85: 947–950
Hoodless PA, Wrana JL 1998 Mechanism and function of signaling by the TGFβ superfamily. Curr Top Microbiol Immunol 228: 235–272
Laiho M, Weis FM, Massague J 1990 Concomitant loss of transforming growth factor (TGF)- receptor types I and II in TGF- resistant cell mutants implicates both receptor types in signal transduction. J Biol Chem 265: 18518–18524
Laiho M, Weis FM, Boyd FT, Ignotz RA, Massague J 1991 Responsiveness to transforming growth factor-β (TGF-β) restored by genetic complementation between cells defective in TGF-β receptors I and II. J Biol Chem 266: 9108–9112
Lopez-Casillas F, Cheifetz S, DoodyJ, Andres JL, Lane WS, Massague J 1991 Structure and expression of the transmembrane proteoglycan betaglycan, a component of the TGF- receptor system. Cell 67: 785–795
Wrana JL, Attisano L, Carcamo J, Zentella A, Doody J, Laiho M, Wang X-F, Massague J 1992 TGF-β signals through a heteromeric protein kinase receptor complex. Cell 71: 1003–1014
Wrana JL, Attisano L, Wieser R, Ventura F, Massague J 1994 Mechanism of activation of the TGF-β receptor. Nature 370: 341–347
Ostor AG, Stillwell R, Fortune DW 1978 Bilateral pulmonary agencies. Pathology 10: 243–248
Ch'in KY, Tang MY 1949 Congenital adenomatoid malformation of one lobe of a lung with general anasarca. Arch Pathol 48: 221–229
Stocker JT, Madewell JE, Drake RM 1977 Congenital cystic adenomatoid malformation of the lung: classification and morphological spectrum. Hum Pathol 8: 155–171
Stocker JT 1994 Congenital and developmental diseases. In: Dail DH, Hammar SP (eds) Pulmonary Pathology. Springer-Verlag, New York, pp 155–190
Hislop A, Hay E, Reid L 1979 The lungs in congenital renal agenesis and dysplasia. Arch Dis Child 54: 32–38
Rutledge JC, Jensen P 1986 Acinar dysplasia: a new form of pulmonary maldevelopment. Hum Pathol 17: 1290–1293
Chambers H 1991 Congenital acinar aplasia: an extreme form of pulmonary maldevelopment. Pathology 23: 69–71
Davidson LA, Batman P, Fagan DG 1998 Congenital acinar dysplasia: a rare case of pulmonary hypoplasia. Histopathology 32: 57–59
Van Dijk C, Wagenvoort CA 1972 The various types of congenital adenomatoid malformation of the lung. J Pathol 110: 131–134
Cangiarella J, Greco A, Askin F, Perlman E, Goswami S, Jagirdar J 1995 Congenital cystic adenomatoid malformation of the lung: insights into the pathogenesis utilizing quantitative analysis of vascular marker CD34 (QBEND-10) and cell proliferation marker MIB-1. Mod Pathol 8: 913–918
Montuenga LM, Martinez A, Miller MJ, Unsworth EJ, Cuttitta F 1997 Expression of adrenomedulin and its receptor during embryogenesis suggests autocrine or paracrine modes of action. Endocrinology 138: 440–451
Jakowlew S, Moody TW, You L, Mariano J 1998 Reduction in transforming growth factor-β type II receptor in mouse lung carcinogenesis. Mol Carcinogen 22: 46–56
Langston C, Thurlbeck WM 1982 Lung growth and development in late gestation and early postnatal life. Perspec Pediatr Pathol 7: 203–210
Hilfer SR 1996 Morphogenesis of the lung: control of embryonic and fetal branching. Annu Rev Physiol 58: 93–113
Trelsteand RL 1984 The Role of Extracellular Matrix in Development. Allen R Liss, New York
Minoo P, King RJ 1994 Epithelial-mesenchymal interactions in lung development. Annu Rev Physiol 56: 13–45
Warburton D, Seth R, Shum L, Horcher PJ, Hall FL, Werb Z, Slavkin HC 1992 Epigenetic role of epidermal growth factor expression and signaling in embryonic mouse lung morphogenesis. Dev Biol 149: 123–133
Peters K, Werner S, Liao X, Wert S, Whitsett J, Williams L 1994 Targeted expression of a dominant negative FGF receptor blocks branching morphogenesis and epithelial differentiation of the mouse lung. EMBO J 13: 3296–3301
Souza P, Kuliszewski M, Wang J, Tseu I, Tanswell AK, Post M 1995 PDGF-AA and its receptor influence early lung branching via an epithelial-mesenchymal interaction. Development 121: 2559–2567
Miettinen PJ, Berger JE, Meneses J, Phung Y, Pederson RA, Werb Z, Derynck R 1995 Epithelial immaturity and failure in mice lacking epidermal growth factor receptor. Nature 376: 337–341
Miettinen PJ, Warburton D, Bu D, Zhao J, Berger JE, Minoo P, Koivisto T, Allen L, Dobbs L, Werb Z, Derynck R 1997 Impaired lung branching morphogenesis in the absence of functional EGF receptor. Dev Biol 186: 224–236
Shiratori M, Oshika E, Ling PU, Singh G, Shinozuka H, Warburton D, Michalopoulos G, Katyal S 1996 Keratinocyte growth factor and embryonic rat lung morphogenesis. Am J Respir Cell Mol Biol 15: 328–338
Serra R, Pelton RW, Moses HL 1994 TGF beta 1 inhibits branching morphogenesis and N-myc expression in lung bud organ cultures. Development 120: 2153–2161
Kaartinen V, Voncken JW, Schuler C, Warburton D, Bu D, Heisterkamp N, Groffen J 1995 Abnormal lung development and cleft palate in mice lacking TGF-beta 3 indicates detects of epithelial-mesenchymal interaction. Nat Genet 11: 415–421
Zhao J, Bu D, Lee M, Slavkin HC, Hall FL, Warburton D 1996 Abrogation of transforming growth factor-β type II receptor stimulates embryonic mouse lung branching morphogenesis in culture. Dev Biol 180: 242–257
Heine UI, Munoz EF, Flanders KC, Roberts AB, Sporn MB 1990 Colocalization of TGF-beta 1 and collagen I and III, fibronectin and glycosaminoglycans during lung branching morphogenesis. Development 109: 29–36
Pelton RW, Johnson MD, Perkett EA, Gold LI, Moses HL 1991 Expression of transforming growth factor-β1, -β2, and -β3 mRNA and protein in the murine lung. Am J Respir Cell Mol Biol 5: 522–530
Heine UI, Flanders KC, Roberts AB, Munoz EF, Sporn MB 1987 Role of transforming growth factor-β in the development of the mouse embryo. J Cell Biol 105: 2861–2876
Lehnert SA, Akhurst RJ 1988 Embryonic expression of pattern of TGF-beta type 1 RNA suggests both paracrine and autocrine mechanisms of action. Development 104: 263–273
Fitzpatrick DR, Denhez F, Kondaiah P, Akhurst RJ 1990 Differential expression of TGF-beta isoforms in murine palatogenesis. Development 109: 585–595
Gatherer D, ten Dijke P, Baird DT, Akhurst RJ 1990 Expression of TGFβ isoforms during first trimester human embryogenesis. Development 110: 445–460
Pelton RW, Dickenson ME, Moses HL, Hogan BLM 1990 In situ hybridization analysis of TGF-β3 RNA expression during mouse development: comparative studies with TGF-β1 and β2. Development 110: 609–620
Pelton RW, Nomura S, Moses HL, Hogan BLM 1990 Expression of transforming growth factor-β2 during murine embryogenesis. Development 110: 759–767
Pelton RW, Saxena B, Jones M, Moses HL, Gold LI 1991 Immunohistochemical localization of TGF-beta 1, TGF-beta 2 and TGF-beta 3 in the mouse embryo-expression patterns suggest multiple roles during embryonic development. J Cell Biol 115: 1091–1105
Millan FA, Denhez F, Kondaiah P, Akhurst RJ 1991 Embryonic gene expression patterns of TGF beta-1, beta-2 and beta-3 suggest different developmental functions in vivo. Development 111: 131–144
Schmid P, Cox D, Bilbe G, Maier R, McMaster GK 1991 Differential expression of TGF β1, β2 and β3 genes during mouse embryogenesis. Development 111: 117–130
Ray MK, Wang G, Barrish J, Finegold MJ, DeMayo FJ 1996 Immunohistochemical localization of mouse Clara cell 10 kd protein using antibodies raised against the recombinant protein. J Histochem Cytochem 44: 919–927
Ohmichi H, Koshimizu U, Matsumoto K, Nakamura T 1998 Hepatocyte growth factor (HGF) acts as a mesenchyme-derived morphogenic factor during fetal lung development. Development 125: 1315–1324
Rudnick D 1933 Developmental capacities of the chick lung in chorioallantoic grafts. J Exp Zool 66: 125–154
Bernfield MR 1981 Organization and remodeling of the extracellular matrix in morphogenesis. In: Connelly TG, Brinkley LL, Carlson BM (eds) Morphogenesis and Pattern Formation. Raven Press, New York, pp 139–161
Fukuda Y, Masuda Y, Kishi J-I, Hashimoto Y, Hayakawa T, Nogawa H, Nakanishi Y 1988 The role of interstitial collagens in cleft formation of mouse embryonic submandibular gland during initial branching. Development 103: 259–267
Nakanishi Y, Nogawa H, Hashimoto Y, Kishi J-I, Hayakawa T 1988 Accumulation of collagen III at the cleft points of developing mouse submandibular epithelium. Development 104: 51–59
Silberstein GB, Daniel CW 1982 Glycosaminoglycans in the basal lamina and extracellular matrix of the mouse mammary duct. Dev Biol 90: 215–222
Blum JL, Zeigler ME, Wicha MS 1987 Regulation of rat mammary gene expression by extracellular matrix components. Exp Cell Res 173: 322–340
Ignotz RA, Massague J 1987 Cell adhesion protein receptors as targets for transforming growth factor-. Cell 51: 189–197
Edwards DR, Murphy G, Reynolds JJ 1987 Transforming growth factor β modulates the expression of collagenase and metalloproteinase inhibitor. EMBO J 6: 1899–1904
Keski-Oja J, Raghow R, Sawdey M, Loskutoff DJ, Postlethwaite AE, Kang AH, Moses HL 1988 Regulation of mRNA for type-1 plasminogen activator inhibitor, fibronectin, and type 1 procollagen by transforming growth factor-β. J Biol Chem 263: 3111–3115
Moens CB, Auerbach AB, Conlon RA, Joyner AL, Rossant J 1992 A targeted mutation reveals a role for N-myc in branching morphogenesis in the embryonic mouse lung. Genes Dev 6: 691–704
Moens CB, Stanton BR, Parada LF, Rossant J 1993 Defects in heart and lung development in compound heterozygotes for two different targeted mutations at the N-myc locus. Development 119: 485–499
Post M, Souzza P, Liu J, Tseu I, Wang J, Kuliszewski M, Tanswell AK 1996 Keratinocyte growth factor and its receptor are involved in regulating early lung branching. Development 122: 3107–3115
Acknowledgements
The authors thank Drs. M. Tsao (University of Toronto), L. Montuenga (National Cancer Institute), and J. Letterio (National Cancer Institute) for helpful suggestions in writing.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Chen, MF., Gray, K., Prentice, M. et al. Human Pulmonary Acinar Aplasia: Reduction of Transforming Growth Factor-β Ligands and Receptors. Pediatr Res 46, 61–70 (1999). https://doi.org/10.1203/00006450-199907000-00011
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199907000-00011
This article is cited by
-
Mesenchyme-specific deletion of Tgf-β1 in the embryonic lung disrupts branching morphogenesis and induces lung hypoplasia
Laboratory Investigation (2019)