Abstract
Mammalian epithelial surfaces are remarkable for their ability to provide critical physiologic functions in the face of frequent microbial challenges. The fact that these mucosal surfaces remain infection-free in the normal host suggests that highly effective mechanisms of host defense have evolved to protect these environmentally exposed tissues. Throughout the animal and plant kingdoms, endogenous genetically encoded antimicrobial peptides have been shown to be key elements in the response to epithelial compromise and microbial invasion. In mammals, a variety of such peptides have been identified, including the well-characterized defensins and cathelicidins. A major source of these host defense molecules is circulating phagocytic leukocytes. However, more recently, it has been shown that resident epithelial cells of the skin and respiratory, alimentary, and genitourinary tracts also synthesize and release antimicrobial peptides. Both in vitro and in vivo data support the hypothesis that these molecules are important contributors to intrinsic mucosal immunity. Alterations in their level of expression or biologic activity can predispose the organism to microbial infection. The regulatory and developmental aspects of antimicrobial peptide synthesis are discussed from a perspective that emphasizes the possible relevance to pediatric medicine.
Similar content being viewed by others
Main
A striking feature of evolution in the animal kingdom is the development of highly specialized epithelial surfaces. These sites of host-environment interaction provide vital physiologic functions including gas exchange, nutrient absorption, water conservation, and reproduction. The low incidence of infectious and inflammatory complications at epithelial surfaces suggests that local host immunity includes highly effective, broad-spectrum, noninflammatory antimicrobial defenses.
As a general paradigm, antimicrobial defenses can be divided into two systems: clonal (acquired) immunity and innate (nonacquired) immunity(1). The clonal immune system uses B and T lymphocytes to mediate and amplify antigen-specific humoral and cellular responses. These responses require days to weeks for maximal activity, involve somatic gene rearrangement, and lead to immunologic memory. Although the acquired immune system represents the "crowning accomplishment of vertebrate immunity"(2) and has been the focus of significant clinically related research (10 Nobel Prizes awarded), evidence now suggests that the function of the acquired immune system is intimately tied to and complemented by the evolutionarily ancient but less highly glorified innate immune system(3,4).
Innate immunity encompasses a complex of first-line host-defense elements. This host-defense system can provide for (i) recognition of microbial organisms as foreign(5–10); (ii) incapacitation and elimination of pathogens(11); and (iii) adjuvant magnification of the acquired immune response when such a response is warranted(3,4,12–14). The elements of innate immunity do not function in isolation, but interact to ensure that the magnitude of the host response reflects the severity of the microbial threat. Components of innate immunity range in complexity from simple inorganic molecules such as nitric oxide to phagocytic and natural killer cells.
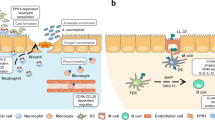
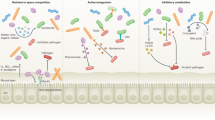
In contrast to the acquired immune system in which an effective response involves gene rearrangements and is developed over a period of days, the innate system remains ever-ready or immediately inducible. In the innate immune system, the ability to discriminate self from nonself is "hard-wired" in the genome, a result of selective pressures of evolution to optimize both recognition and effector molecules. The working hypotheses for much current immunologic research highlight the role of the innate immune system in host defense of epithelial surfaces in humans and other animals (Fig. 1).
Microbial challenge at wet mucosal epithelia, a model. The model suggests that defense of mammalian wet mucosal surfaces includes inducible and constitutive expression of antimicrobial peptides, generation of simple inorganic molecules with antimicrobial activity, and proteins that can directly inhibit microbial survival. These antimicrobial factors are made locally by epithelial cells at mucosal surfaces but, in some cases, may also be derived from circulating cells and plasma. These factors coupled with barrier properties and clearance mechanisms constitute the local defense response. The model then suggests that this local response to microbial challenges effectively deals with the vast majority of encounters with microbes to prevent local infection. Only if the local defenses are overwhelmed will secondary lines of defense be called into play. Factors that may lead to the overwhelming of local defenses include pathogenicity of specific microbes, sheer number of microbes, or inadequate host responses due to genetic predisposition, developmental immaturity, or systemic disease.
Recent investigations have uncovered a large and remarkably varied collection of antimicrobial peptides (arbitrarily defined as <100 amino acids in size) that comprise a widespread effector arm of the innate immune system. Antimicrobial peptides have been identified in organisms as diverse as humans, frogs, insects, plants, and protozoa. Their cellular origin includes granulocytes, platelets, specialized epithelial glands, wet mucosal epithelia including intestinal Paneth cells, fetal membranes, leaves, flowers, and seeds. Chemically divergent in structure (Fig. 2), they are microbicidal at micromolar concentrations against a wide range of target organisms. In this review, we will focus on the properties of those antimicrobial peptides known to be present in tissues of mammalian species (Fig. 3), especially as they may relate to human innate immunity at wet mucosal surfaces. The interested reader is directed to recent reviews that emphasize other aspects of antimicrobial peptide structure and biology(15–21).
Chemical structural classification of some well-studied mammalian antimicrobial peptides. The primary sequence of some characterized mammalian peptides are organized on the basis of distinguishing structural features, similar to a classification by Boman(15). Several of these peptides [LL-37(130), protegrins(119,124), sheep cathelin-associated peptide 5 (SC5)(111), and CRAMP(131), PR-39(35,118), bactenecin peptide 5 (BAC5)(109), and indolicidin(117)] are derived from a precursor protein containing a cathelin-like domain and may be classified alternatively as cathelicidins.
Sites of antimicrobial expression. WBC: Mammalian antimicrobial peptides were first identified in circulating phagocytes(174). Members of the defensin(69,70) and cathelicidin(132) families of peptides have been identified in human neutrophils. Defensins were also detected in rabbit(175) and bovine(176) lung macrophages but have not been reported in human macrophages. Tongue: The tongue(93,94) and gingival mucosa(103) are known sites of β-defensin expression. Airways: The first β-defensin, TAP, was isolated from bovine tracheal mucosa(89). Expression of β-defensins(54,90,91,167) and LL-37(133) have been detected in human AEC. Anionic heptapeptides with antibacterial activity have been isolated from ovine airway surface fluid(138). Colon: Recently, β-defensin expression was discovered in colonic mucosa of cattle(97) and sheep(98). Reproductive Tract: Defensins are expressed in human urogenital mucosa(77,96). Defensin and cathelicidin mRNA have been detected in testicular tissue(130,141,177). Skin: Human skin is the site of expression for both defensin(54,134,178) and cathelicidins(134). Small Intestine: Defensins are expressed in the small intestinal epithelium(67,68,71,73,98,142,179,180). In humans, only defensins HD-5 and HD-6 have been detected at this site(74). Kidney: In kidney tissue, both α- and β-defensins have been detected(41,60,90,96,101,181). HBD-1 has been isolated from human urine(96).
BASIC PROPERTIES
Mechanism of activity. Antimicrobial peptides generally are microbicidal rather than static agents, with the most detailed information on their mechanism of action derived from anti-bacterial studies [for reviews, see(15,16,22)]. Bacterial killing occurs in minutes and in most cases requires bacterial cell growth. Addition of purified cecropin, magainin, or defensin peptides to artificial membrane systems leads to pore formation and membrane depolarization, suggesting a possible mechanism of their microbicidal activity(23–30). Other peptides, e.g. some members of the cathelicidin family, seem to act via disruption of bacterial energy metabolism or biosynthetic pathways(31,32).
Gene encoding. Unlike most other antibiotics in nature that are products of multienzyme cascades, these molecules are products of prototypical genes(18) (Fig. 4). Families of anti-microbial peptide genes are generally tightly clustered and typically have two or more exons. Families of structurally similar antimicrobial peptides map to syntenic chromosomal segments in different mammalian species, consistent with their distant evolution from an ancestral gene(33–41). In some cases, the genes are adjacent to repetitive sequence elements that may provide a mechanism for gene family expansion and diversification through homologous but unequal cross-over during meiosis(42). There has been only an isolated report of alternative splicing as a mechanism of gene diversification(43).
The primary translational product is a prepropeptide with a putative N-terminal endoplasmic reticulum targeting (signal) sequence that has been conserved within specific gene families. Adjacent to this signal peptide is a pro segment, which is often anionic in charge and may be important for neutralization/processing/folding of the cationic C-terminal peptide(44–47). A proposed function for the propeptide segment is that of rendering the cationic peptide inactive through charge interaction as a means of protecting the host cell. Some propeptides (e.g. neutrophil defensins; see Major Classes of Mammalian Antimicrobial Peptides, β-Defensins) are processed by post-translational cleavage steps leading to intracellular peptide storage in lysosomal-type granules, whereas others (e.g. cathelicidins; see Major Classes of Mammalian Antimicrobial Peptides, Cathelicidins) are stored as propeptides with posttranslational cleavage occurring extracellularly. The posttranslational processing steps include proteolytic cleavage that liberates the mature peptide and, in some cases, formation of intramolecular disulfide bonding, C-terminal amidation, and/or N-terminal formation of pyroglutamate.
Sites of expression. (i) Granules of mammalian neutrophils contain high levels of cysteine-rich defensins (humans, rabbits, rats, guinea pigs, and cattle; see Major Classes of Mammalian Antimicrobial Peptides, Defensins) and/or cathelicidins (cattle, sheep, rabbits, and pigs; see Major Classes of Mammalian Antimicrobial Peptides, Cathelicidins). The mouse is a notable exception in which neutrophil granules contain no defensins and only low levels of cathelicidins(48–50). (ii) Antimicrobial peptides present at epithelial surfaces are derived either from in situ synthesis by resident cells or from mobilized storage depots present in circulating cells (granulocytes, monocytes, platelets)(50,51). Examples of in situ synthesis include constitutive expression of α-defensins (in Paneth cell granules of mouse, rat, and human small intestine)(52) and inducible expression of β-defensins (in bovine airway and human skin)(53,54). Examples of systemic delivery include neutrophil localization and release of intragranular peptides in pig skin (PR-39)(55,56) and human lung (α-defensins)(57).
MAJOR CLASSES OF MAMMALIAN ANTIMICROBIAL PEPTIDES
Defensins. Mammalian defensins are cationic antimicrobial peptides characterized by the presence of three intramolecular disulfide bonds [for more detailed reviews, see(17,19,22)]. Defensins interact with and disrupt microbial membranes, resulting in cell death(23). In standardized assays conducted in the presence of low salt concentrations, defensins are microbicidal at 10-100 µg/mL (3-30 µM)(22). However, their activity is inhibited at higher salt concentrations (≥ ∼ 75 mM NaCl).
Mammalian defensins can be subdivided into two general classes, the α-defensins(17,22) and the β-defensins(21), based on (i) alternative spacing of their six cysteine residues; (ii) differences in the alignment of the disulfide bridges(58,59); and (iii) variation in the length of the pro segment. Both classes have been described in humans and rodents, whereas only α-defensins have been reported in rabbits and guinea pigs and only β-defensins have been described in cattle, sheep, and pigs. In humans and mice, genes encoding α- and β-defensin peptides map to the same chromosomal segment(38,41,60), consistent with their derivation from a common ancestral sequence. Despite their differences in sequence and disulfide bond pattern, the α- and β-defensins share a similar three-dimensional structure in solution(61).
α-Defensins. The α-defensins are 29-35 amino acids in length containing three disulfide bridges in a 1-6, 2-4, 3-5 alignment (Fig. 5)(58). Structural studies of α-defensins show a triple-stranded β-sheet and a β-hairpin loop containing cationic charged residues(62,63). α-Defensins are found in great abundance in intracellular granules of circulating neutrophils (5-18% of total protein)(64–66) and in granule-containing Paneth cells of the small intestine(67,68). The human α-defensin family consists of four defensins isolated from neutrophils, HD-1-HD-4 [often referred to as human neutrophil peptide (HNP)-1-HNP-4](65,69,70), and two defensins expressed in Paneth cells of the small intestine, HD-5(68,71,72) and HD-6(73,74). Recently, it has been shown that HD-5 is expressed also at multiple sites within the female reproductive tract, placenta, and fetal membranes(75–77).
Structure of α- and β-defensin peptides. Mammalian defensins may be grouped into two distinct structural subfamilies designated α- and β-defensins. (see Major Classes of Mammalian Antimicrobial Peptides, Defensins). The primary structure for the known human peptides is shown, the consensus residues for each family is highlighted in yellow, and the disulfide linkages defined by Selsted et al.(58,59) are indicated.
The human α-defensins are synthesized as 93-100 amino acid prepropeptides with a predicted 19-amino acid signal peptide and a 41-51-amino acid anionic pro segment(66,78). The pro segment has been shown to be necessary for accurate processing and transport of the defensin peptide(44–46), but its removal is thought to be necessary for expression of antimicrobial activity(44,47). Human neutrophil defensins associate as amphiphilic dimers(28,63,79) and, when incubated with model membranes, form voltage-dependent channels that are weakly anion-selective(24). The induction of Cl--specific channels has been shown also upon incubation of murine α-defensins with cultured T84 gastrointestinal epithelial cells(80).
Individual α-defensins have unique spectra of antibacterial activity against both Gram-positive and Gram-negative species including intracellular and extracellular organisms [for review, see(22)], antiviral activity with effects on propagation of enveloped virus including members of the Herpes family(81), antifungal activity targeting Candida albicans(82–84), and antiparasitic activity including anti-Giardia(85) and antitreponemal effects(86,87).
β-Defensins. The β-defensins are 36-42 amino acids in length with six cysteines in a spacing pattern and a disulfide alignment (1-5, 2-4, 3-6)(59), differing from that of the α-defensins (Fig. 5). A subset of ruminant β-defensins has been shown to contain an N-terminal pyroglutamate residue(88). In cattle neutrophils, there are at least 13 different β-defensin peptides(88), although none have been reported in sheep and human neutrophils. β-defensins are synthesized at epithelial surfaces including the upper respiratory tract(42,89–92), nasal mucosa(42), tongue(93,94), kidney(90,95,96), pancreas(90), colon(97,98), female reproductive tract(96), and conjunctiva(92).
The β-defensins are synthesized as 64-68 amino acid pre-propeptides with the 26-32 amino acids at the N-terminus comprising putative signal and propeptide segments. The intracellular processing, storage, and release pathways remain to be defined. Limited data are available on the spectrum of β-defensin antimicrobial activity, although several peptides of the family have been shown to be active against Gram-positive and Gram-negative bacteria as well as C. albicans and Aspergillus fumigatus(41,54,88,89,93,96,99–101). In most tissues, the constitutive level of β-defensin expression seems to be low. However, expression of at least four different β-defensins has been shown to be inducible: β-defensins TAP(53), enteric β-defensin(97), lingual antimicrobial peptide (LAP)(92,93,102), and HBD-2(54). Bovine tracheal epithelial cells exposed to lipopolysaccharide up-regulate transcription of both the TAP and lingual antimicrobial peptide genes in a dose- and time-dependent fashion(102). NF-κB recognition elements are present upstream of the TAP coding sequences that may mediate the induction(42,53).
Two HBD peptides have been identified to date, HBD-1(95,96) and HBD-2(54). The former was identified initially as a 36-amino acid peptide purified from blood filtrate(95). The gene encoding HBD-1 has been shown to be expressed in epithelial tissues including kidney, lung (both upper respiratory tract and parenchyma), pancreas, testis, gingival tissue, and vagina(90,91,95,96,103,104). Several isoforms of HBD-1 that represent N-terminal extensions of the 36-amino acid peptide have been identified in urine and vaginal mucosal secretions(96). Urine concentrations are increased in pregnancy and isoform differences exist between males and females. The various isoforms may represent alternative processing of the prepropeptide and suggest that proteolytic cleavage may be an important site of biologic regulation. In contrast with the bovine airway β-defensins, HBD-1 expression does not seem to be inducible(90,96).
HBD-2 is a 41-amino acid peptide purified from lesional psoriatic skin based on its binding to a whole Escherichia coli affinity column. In addition to skin, expression of HBD-2 was detected also in the tracheal mucosa(54,105–107). HBD-2 is bactericidal in vitro against both Pseudomonas aeruginosa and C. albicans but relatively ineffective against Gram-positive Staphylococcus aureus. All three organisms induce HBD-2 transcription in foreskin-derived keratinocytes, as does the cytokine TNF-α.
Cathelicidins. The cathelicidins are a remarkably diverse collection of molecules that derive from prepropeptides sharing a highly conserved N-terminal propeptide segment (Fig. 6)(108). The conserved propeptide segment of approximately 100 amino acids shares sequence similarity with the porcine protein cathelin, a putative cysteine protease inhibitor, and hence the family name(109–111). Cathelicidins are stored in neutrophil granules as propeptides (nonantimicrobial)(112,113), with neutrophil activation leading to elastase-mediated endoproteolytic cleavage and generation of the C-terminal antimicrobial peptide(114,115).
Structure of cathelicidin precursors. A diverse collection of antimicrobial peptides are synthesized at the carboxyl-terminal portion of precursors with a highly conserved amino-terminal domain, approximately 100 amino acid residues in size, termed "cathelin." The active peptide is released after proteolytic cleavage(114,115). Examples of this collection of antimicrobial peptides are found in humans(130,132,182), cattle(129,183–185), sheep(39,111), rabbits(186,110), mice(131), and pigs(121,187–190), and the primary structure for several of these peptides is shown in Figure 2.
The cathelicidin gene families of pigs, cattle, and sheep are large and diverse(109,111,116–129), whereas those of humans and mice are limited to one or two genes(130,131). The human cathelicidin, referred to alternatively as FALL-39/hCAP18/LL-37/CAMP, in its mature form is a 37-amino acid amphiphilic α-helical peptide(132). Expression of LL-37 has been detected not only in neutrophils(132) but also in testes(130) and respiratory epithelia(133) and in keratinocytes at sites of inflammation(134).
Others. Antimicrobial peptides have been shown in platelets(135), salivary secretions(136), amniotic fluid(137), and lung fluid(138,139). As circulating blood elements, platelets would be an ideal cell type for the delivery of antimicrobial agents to sites of vascular compromise accompanying epithelial injury. Preliminary characterization of the amniotic-fluid and lung-fluid activity showed the presence of a unique, Zn-dependent antimicrobial anionic peptide(138,139).
ONTOGENY OF ANTIMICROBIAL PEPTIDE EXPRESSION
Antimicrobial peptide gene expression is developmentally regulated and occurs in tissue patterns that are species-specific. As examples, human α-defensins are expressed in neutrophils and Paneth cells but not in macrophages, whereas rabbit α-defensins are found in both neutrophils and macrophages and mouse α-defensins are present in Paneth cells and testes. Further, macrophage expression of rabbit α-defensins is absent in neonates but present in adults and is detectable in lung-derived but not in peritoneal-derived cells(140).
Paneth cell α-defensins. Human α-defensins HD-5 and HD-6 are expressed in the developing fetus as early as 13.5-wk gestation (detected by RT-PCR), with HD-5 present in both small intestine and colon and HD-6 present only in small intestine(74). By 17-wk gestation, PCR-based detection of both isoforms is limited to the small intestine, and at 24 wk, enteric defensin expression has reached levels detectable by Northern blot hybridization. At this point in gestation (late second trimester), both the number of Paneth cells and the level of enteric α-defensin transcription are significantly lower than in the adult. In contrast, mouse α-defensins of the small intestine (cryptdins) are expressed at low levels before birth, with a rapid increase during the weaning period(141–143). Interestingly, transgenic mice carrying the HD-5 gene express the peptide in Paneth cells in the same developmental sequence as the endogenous mouse genes (Salzman N, Bevins CL, Huttner KM 1996 Abstract 132/E-53. American Society of Microbiology, New Orleans, LA).
β-Defensins. HBD-1 is developmentally regulated in lung parenchyma, with detection by RNase-protection assay in postnatal and adult samples but not in 15- and 22-wk gestation fetal tissue(91). The cattle β-defensin TAP is developmentally regulated antenatally as well, as assayed by Northern blot hybridization on airway RNA samples from 4-mo gestation, 6-mo gestation, and adult animals(42). In sheep, β-defensin expression was detected by nested RT-PCR at d 115 of gestation (145-150 d term) in trachea, tongue, stomach, and uterus, and by Northern analysis at d 127 in ileum and colon(98). Using primer pairs specific for the two sheep β-defensin isoforms, we found that tissues express both SBD-1 and SBD-2 at 115 and 127 d of gestation (Fig. 7). In contrast, SBD-1 is the predominant or exclusive β-defensin in all adult tissues assayed with the exception of SBD-2 in the ileum (based on sequencing of multiple cDNA species).
β-Defensin isoform expression during sheep gestation and adulthood. RNA was isolated from indicated sheep tissues and analyzed by RT-PCR using gene specific primers. Primer pairs specific for exon 2 of SBD-1 and SBD-2 produced products visualized by ethidium bromide fluorescence. [Reproduced with permission from Huttner et al. (1998) Antimicrobial peptide expression is developmentally regulated in the ovine gastrointestinal tract. J Nutr 128:297S-299S.]
Cathelicidins. Developmental regulation of the human cathelicidin LL-37 remains to be investigated. However, expression of the mouse cathelicidin CRAMP was detected by Northern blot hybridization both in adult bone marrow and in whole embryo extracts as early as embryonic d 12(131).
STRATEGY OF ANTIMICROBIAL PEPTIDES AS AGENTS OF HOST DEFENSE
The ubiquity of antimicrobial peptide expression in every plant and animal species examined suggests that these molecules function as highly effective host-defense elements(15). Facing a resurgence of antibiotic-resistant organisms in the clinical arena, what might we learn from the strategies used by these peptides that are conserved through evolution?
1. Target microbial structures essential for survival and not readily altered by simple genetic changes. The majority of antimicrobial peptides work by selectively disrupting the membrane of target microorganisms through channel or pore formation(23–30). Attempts to select out resistant bacterial strains from sensitive ones have been unsuccessful, suggesting that the bacterial target represents a structure fundamental for survival.
2. Use a combination of agents to increase effectiveness. Within most epithelial tissues studied to date, one can show the presence of multiple peptides from a single family or peptides and proteins from distinct families with unrelated structures and overlapping spectra of antimicrobial activity. Specific examples of antibacterial synergy between differing antimicrobial peptides or between antimicrobial peptides and other host-defense proteins have been reported(83,144,145).
3. Develop multifunctional agents. In addition to their direct microbicidal activity, antimicrobial peptides are agents that can modulate inflammatory response, wound repair, cell division, and adaptive immune response. One intriguing example is the porcine cathelicidin PR-39 that can localize to the site of skin wounds, sterilize the break in epithelial integrity, and additionally stimulate the wound-repair process(55). Other examples include defensin-mediated inactivation of serine proteinase inhibitors(146), defensin and cathelicidin chemotactic activity(147–149), defensin stimulation of epithelial cell proliferation(150), defensin antagonism of ACTH-stimulated glucocorticoid release(151,152), defensin inhibition of fibrinolysis(153), and enhancement of binding plasminogen and lipoprotein (a) to endothelial cells(153,154).
POSSIBLE LINKS TO HUMAN DISEASE
An abundance of circumstantial evidence supports the hypothesis that antimicrobial peptides are an integral component of innate immunity in vivo including their sites of expression (Fig. 3); evolutionary ubiquity preceding development of the vertebrate adaptive immune system(15,155,156); up-regulation by epithelial compromise, infection, and/or inflammation(53,92,93,97,134,157); broad-spectrum rapid antimicrobial activity(15,22); and an association of Salmonella virulence with resistance to antimicrobial peptides(67,158–161). Direct evidence of in vivo effectiveness is available in insects and plants. In Drosophila, blocked induction of the antifungal peptide drosomycin results in overwhelming spontaneous fungal infection(162,163). In transgenic plants, overexpression of antimicrobial peptides enhances host-defense responses(164). Comparable direct and conclusive evidence from a mammalian system is not yet available.
In the common inherited disorder CF, recurrent infection is a devastating component of the disease process but, curiously, is strictly limited to the respiratory tract(165). This suggests that a deficiency in local lung host defense results either directly or indirectly from the mutations identified in the CFTR. Recently, studies using cultures of AEC grown in primary culture have suggested that genetic defects in the CFTR impair the capacity for airway surface fluid to kill Pseudomonas bacteria(166). A model to explain these findings was suggested by Smith et al.(166) and proposes that low molecular weight factors are secreted by AEC (both from controls and CF patients) but that defective function of the CFTR in CF cells impairs the antimicrobial activity of these factors. Indirect evidence for the role of HBD-1 in this setting was provided by studies of human AEC maintained in a xenograft mouse model system(167). Antisense oligonucleotides directed specifically against HBD-1 inhibited antimicrobial activity of epithelial secretions, yet control oligonucleotides had no inhibitory effect. An important area of future investigation will be to elucidate more clearly the local host-defense factors of the airway epithelium and to better define the possible role of HBD-1 and other lung antimicrobial peptides [for example, HBD-2(54) and LL-37(133)] in the pathogenesis of CF. New therapeutic strategies to treat the lung infections of CF patients may emerge from these studies.
The genetic mapping assignments of the human α- and β-defensins to chromosome 8p23.1-p23.2(33,36,38,40,168) and of the human cathelicidin LL-37 to chromosome 3p21.3(35) will allow investigators to search for colocalization of genetic syndromes that predispose to infection. The same is true for the mouse defensin(34) and cathelicidin(131) mapping assignments and mouse models of infection susceptibility. It has been shown in human population surveys that there is polymorphic expression of α-defensins, with 10% of individuals lacking expression of the HD-3 peptide(169). A possible explanation for this finding stems from evidence for the existence of variable numbers of defensin genes at the defensin locus within the human population(170). Whether there is a phenotype that is coinherited with HD-3 deficiency or with mutations in any of the antimicrobial peptide genes may be a fruitful area for future investigations.
A LOOK TO THE FUTURE
As pediatricians, what role will antimicrobial peptides play in the well-being of our patients? Considering the rapidity with which new antimicrobial peptides are being discovered and how little we yet know of their in vivo properties, it may be premature to overly speculate on details. However, with the current information, we predict the following:
-
1
Antimicrobial peptides will be found in nearly all human mucosal secretions, contributing to host defense in the respiratory, gastrointestinal, and genitourinary tracts as well as throughout the oropharynx and ocular surfaces.
-
2
Insufficient expression of antimicrobial peptides will predispose to disease. A deficiency in antimicrobial peptide levels (or activity) may contribute to patient subpopulations being at higher risk for neonatal sepsis, otitis media, conjunctivitis, dental caries, nasopharynx carriage of potential pathogens, urinary tract infections, etc. Antimicrobial peptide levels may be reduced in our youngest and least mature patients, the preterm infants, secondary to their developmental state. Alternatively, changes in the local environment in which these peptides should function may impair antimicrobial activity and compromise host defense, as proposed in CF airway surface fluid(166,167).
-
3
Common therapeutic interventions and pharmacologic agents may alter natural defenses involving antimicrobial peptides. As examples, in the intubated patient, air-borne pathogens can bypass the antimicrobial peptide-rich upper airway epithelium. In the gastrointestinal tract, surgical resection or bypass of the distal ileum may lead to altered lumenal bacteria from omission of Paneth cell α-defensins. Further, glucocorticoids, used frequently in clinical practice, block inducible expression of immune and inflammation-associated genes (via inhibition of NF-κB signaling(171)) and may result in reduced host immunity. In one model system, frogs exposed to systemic or topical glucocorticoids suffered a 93% reduction in antimicrobial peptide expression, resulting in at least a 10-fold increase in oral bacterial counts(172).
-
4
Antimicrobial peptides may earn a place in our armamentarium of topical or systemic agents used in treating infections. Clinical trials of a magainin derivative (Xenopus laevis antimicrobial peptide), a recombinant bactericidal permeability-increasing protein fragment (rabbit), and a protegrin (pig cathelicidin) are underway as novel therapeutic agents(173).
Abbreviations
- AEC:
-
airway epithelial cells
- CAMP and CRAMP:
-
cathelin-related antimicrobial peptide
- CF:
-
cystic fibrosis
- CFTR:
-
cystic fibrosis transmembrane regulator
- FALL-39:
-
39-amino acid cathelicidin-associated peptide with amino terminal sequence: Phe-Ala-Leu-Leu
- HBD:
-
human β-defensin
- HD:
-
human defensin
- LL-37:
-
37-amino acid cathelin-associated peptide with amino terminal sequence: Leu-Leu
- NF-κB:
-
nuclear factor kappa B
- PR-39:
-
39-amino acid cathelin-associated peptide with amino terminal sequence: pro-arg
- RT-PCR:
-
reverse transcriptase polymerase chain reaction
- SBD:
-
sheep β-defensin
- TAP:
-
tracheal antimicrobial peptide
References
Janeway CA Jr, Travers P 1997 Immunobiology: The Immune System in Health and Disease, 3rd Ed. Current Biology, Ltd, London, 1.5–1.11.
Fearon DT 1997 Seeking wisdom in innate immunity. Nature 388: 323–324.
Janeway CA 1989 Approaching the asymptote? Evolution and revolution in immunology. Cold Spring Harbor Symp Quant Biol 54: 1–13.
Fearon DT, Locksley RM 1996 The instructive role of innate immunity in the acquired immune response. Science 272: 50–54.
Mosser 1994 Receptors on phagocytic cells involved in microbial recognition. Immunol Ser 60: 99–114.
Ulevitch RJ, Tobias PS 1994 Recognition of endotoxin by cells leading to transmembrane signaling. Curr Opin Immunol 6: 125–130.
Epstein J, Eichbaum Q, Sheriff S, Ezekowitz RA 1996 The collectins in innate immunity. Curr Opin Immunol 8: 29–35.
Pearson AM 1996 Scavenger receptors in innate immunity. Curr Opin Immunol 8: 20–28.
Medzhitov R, Janeway CA Jr 1997 Innate immunity: the virtues of a nonclonal system of recognition. Cell 91: 295–298.
Janeway CA 1992 The immune system evolved to discriminate infectious nonself from noninfectious self. Immunol Today 13: 11–16.
Wright SD, Unkeless JC 1993 Fatal attraction: recognition and killing mechanisms in innate immunity. Curr Opin Immunol 5: 57–58.
Janeway CA, Bottomly K 1994 Signals and signs for lymphocyte responses. Cell 76: 275–285.
Medzhitov R, Janeway CA Jr 1996 On the semantics of immune recognition. Res Immunol 147: 208–214.
Medzhitov R, Janeway CA Jr 1997 Innate immunity: impact on the adaptive immune response. Curr Opin Immunol 9: 4–9.
Boman HG 1995 Peptide antibiotics and their role in innate immunity. Annu Rev Immunol 13: 61–92.
Hancock REW, Falla T, Brown M 1995 Cationic bactericidal peptides. Adv Microb Physiol 37: 135–175.
Martin E, Ganz T, Lehrer RI 1995 Defensins and other endogenous peptide antibiotics of vertebrates. J Leuk Biol 58: 128–136.
Nissen-Meyer J, Nes IF 1997 Ribosomally synthesized antimicrobial peptides: their function, structure, biogenesis, and mechanism of action. Arch Microbiol 167: 67–77.
Lehrer RI, Bevins CL, Ganz T 1998 Defensins and other antimicrobial peptides. In: Ogra PL, Mestecky J, Lamm ME, Strober WM, Bienstock J (eds) Mucosal Immunology. Academic Press, New York, 89–99.
Boman HG 1998 Gene-encoded peptide antibiotics and the concept of innate immunity: an update review. Scand J Immunol 48: 15–25.
Diamond G, Bevins CL 1998 beta-Defensins: endogenous antibiotics of the innate host defense response. Clin Immunol Immunopathol 88: 221–225.
Lehrer RI, Lichtenstein AK, Ganz T 1993 Defensins: antimicrobial and cytotoxic peptides of mammalian cells. Annu Rev Immunol 11: 105–128.
Lehrer RI, Barton A, Daher KA, Harwig SS, Ganz T, Selsted ME 1989 Interaction of human defensins with Escherichia coli. Mechanism of bactericidal activity. J Clin Invest 84: 553–561.
Kagan BL, Selsted ME, Ganz T, Lehrer RI 1990 Antimicrobial defensin peptides form voltage-dependent ion-permeable channels in planar lipid bilayer membranes. Proc Natl Acad Sci USA 87: 210–214.
Wimley WC, Selsted ME, White SH 1994 Interactions between human defensins and lipid bilayers: evidence for formation of multimeric pores. Protein Sci 3: 1362–1373.
Ludtke SJ, He K, Heller WT, Harroun TA, Yang L, Huang HW 1996 Membrane pores induced by magainin. Biochemistry 43: 13723–13728.
Silvestro L, Gupta K, Weiser JN, Axelsen PH 1997 The concentration-dependent membrane activity of cecropin A. Biochemistry 36: 11452–11460.
Hristova K, Selsted ME, White SH 1996 Interactions of monomeric rabbit neutrophil defensins with bilayers: comparison with dimeric human defensin HNP-2. Biochemistry 35: 11888–11894.
Lohner K, Latal A, Lehrer RI, Ganz T 1997 Differential scanning microcalorimetry indicates that human defensin, HNP-2, interacts specifically with biomembrane mimetic systems. Biochemistry 36: 1525–1531.
Hristova K, Selsted ME, White SH 1997 Critical role of lipid composition in membrane permeabilization by rabbit neutrophil defensins. J Biol Chem 272: 24224–24233.
Boman HG, Agerberth B, Boman A 1993 Mechanisms of action on Escherichia coli of cecropin P1 and PR-39, two antibacterial peptides from pig intestine. Infect Immun 61: 2978–2984.
Falla TJ, Karunartne N, Hancock REW 1996 Mode of action of the antimicrobial peptide indolicidin. J Biol Chem 271: 19298–19303.
Sparkes RS, Kronenberg M, Heinzmann C, Daher KA, Klisak I, Ganz T, Mohandas T 1989 Assignment of defensin gene(s) to human chromosome 8p23. Genomics 5: 240–244.
Ouellette AJ, Pravtcheva D, Ruddle FH, James M 1989 Localization of the cryptdin locus on mouse chromosome 8. Genomics 5: 233–239.
Gudmundsson GH, Magnusson KP, Chowdhary BP, Johansson M, Andersson L, Boman HG 1995 Structure of the gene for porcine peptide antibiotic PR-39, a cathelin gene family member: comparative mapping of the locus for the human peptide antibiotic FALL-39. Proc Natl Acad Sci USA 92: 7085–7089.
Bevins CL, Jones DE, Dutra A, Schaffzin J, Muenke MM 1996 Human enteric defensin genes: chromosomal map position and a model of possible evolutionary relationships. Genomics 31: 95–106.
Iannuzzi L, Gallagher DS, Di Meo MeoGP, Diamond G, Bevins CL, Womack JE 1996 High resolution FISH mapping of beta-defensin genes to river buffalo and sheep chromosomes suggests a chromosome discrepancy in cattle standard karyotypes. Cytogenet Cell Genet 75: 10–13.
Liu L, Zhao C, Heng HH, Ganz T 1997 The human beta-defensin-1 and alpha-defensins are encoded by adjacent genes: two peptide families with differing disulfide topology share a common ancestry. Genomics 43: 316–320.
Huttner KM, Lambeth MR, Burkin HR, Burkin DJ, Broad TE 1998 Localization and genomic organization of sheep antimicrobial peptide genes. Gene 206: 85–91.
Harder J, Siebert R, Zhang Y, Matthiesen P, Christophers E, Schlegelberger B, Schroder JM 1997 Mapping of the gene encoding human beta-defensin-2 (DEFB2) to chromosome region 8p22-p 23:1. Genomics 46: 472–475.
Morrison GM, Davidson DJ, Kilanowski FM, Borthwick DW, Crook K, Maxwell AI, Govan JRW, Dorin JR 1998 Mouse beta defensin-1 is a functional homolog of human beta defensin-1. Mamm Genome 9: 453–457.
Diamond G, Jones DE, Bevins CL 1993 Airway epithelial cells are the site of expression of a mammalian antimicrobial peptide gene. Proc Natl Acad Sci USA 90: 4596–4600.
Scocchi M, Wang S, Gennaro R, Zanetti M 1998 Cloning and analysis of a transcript derived from two contiguous genes of the cathelicidin family. Biochim Biophys Acta 1398: 393–396.
Michaeklson D, Rayner J, Couto M, Ganz T 1992 Cationic defensins arise from charge neutralized propeptides: a mechanism for avoiding leukocyte autotoxicity?. J Leuk Biol 51: 634–639.
Ganz T, Liu L, Valore E, Oren A 1993 Posttranslational processing and targeting of transgenic human defensin in murine granulocyte, macrophage, fibroblast, pituitary adenoma cell lines. Blood 82: 641–650.
Liu L, Ganz T 1995 The pro region of human neutrophil defensin contains a motif that is essential for normal subcellular sorting. Blood 85: 1095–1103.
Valore EV, Martin E, Harwig SS, Ganz T 1996 Intramolecular inhibition of human defensin HNP-1 by its propiece. J Clin Invest 97: 1624–1629.
Eisenhauer PB, Lehrer RI 1992 Mouse neutrophils lack defensins. Infect Immun 60: 3446–3447.
Levy O 1996 Antibiotic proteins of polymorphonuclear leukocytes. Eur J Haematol 56: 263–277.
Ganz T, Weiss J 1997 Antimicrobial peptides of phagocytes and epithelia. Semin Hematol 34: 343–354.
Bevins CL 1994 Antimicrobial peptides as agents of mucosal immunity. In: Marsh J, Goode JA, Boman H (eds) Antimicrobial Peptides (Ciba Foundation Symposium 186). John Wiley and Sons, Chichester, UK, 250–269.
Ouellette AJ 1997 Paneth cells and innate immunity in the crypt microenvironment. Gastroenterology 113: 1779–1784.
Diamond G, Russell JP, Bevins CL 1996 Inducible expression of an antibiotic peptide gene in lipopolysaccharide-challenged tracheal epithelial cells. Proc Natl Acad Sci USA 93: 5156–5160.
Harder J, Bartels J, Christophers E, Schroder JM 1997 A peptide antibiotic from human skin. Nature 387: 861
Gallo RL, Ono M, Povsic T, Page C, Eriksson E, Klagsbrun M, Bernfield M 1994 Syndecans, cell surface heparin sulfate proteoglycans, are induced by proline-rich antimicrobial peptide from wounds. Proc Natl Acad Sci USA 91: 11035–11039.
Shi J, Ganz T 1998 The role of protegrins and other elastase-activated polypeptides in the bactericidal properties of porcine inflammatory fluids. Infect Immun 66: 3611–3617.
Soong LB, Ganz T, Ellison A, Caughey GH 1997 Purification and characterization of defensins from cystic fibrosis sputum. Inflamm Res 46: 98–102.
Selsted ME, Harwig SS 1989 Determination of the disulfide array in the human defensin HNP-2. A covalently cyclized peptide. J Biol Chem 264: 4003–4007.
Tang YQ, Selsted ME 1993 Characterization of the disulfide motif in BNBD-12, an antimicrobial beta-defensin peptide from bovine neutrophils. J Biol Chem 268: 6649–6653.
Huttner KM, Kozak CA, Bevins CL 1997 The mouse genome encodes a single homolog of the antimicrobial peptide human beta-defensin 1. FEBS Lett 413: 45–49.
Zimmermann GR, Legault P, Selsted ME, Pardi A 1995 Solution structure of bovine neutrophil beta-defensin-12: the peptide fold of the beta-defensins is identical to that of the classical defensins. Biochemistry 34: 13663–13671.
Pardi A, Hare DR, Selsted ME, Morrison RD, Bassolino DA, Bach AC II 1988 Solution structures of the rabbit neutrophil defensin NP-5. J Mol Biol 201: 625–636.
Hill CP, Yee J, Selsted ME, Eisenberg D 1991 Crystal structure of defensin HNP-3, an amphiphilic dimer: mechanisms of membrane permeabilization. Science 251: 1481–1485.
Rice WG, Ganz T, Kinkade JMJ, Selsted ME, Lehrer RI, Parmley RT 1987 Defensin-rich dense granules of human neutrophils. Blood 70: 757–765.
Gabay JE, Scott RW, Campanelli D, Griffith J, Wilde C, Marra MN, Seeger M, Nathan CF 1989 Antibiotic proteins of human polymorphonuclear leukocytes. Proc Natl Acad Sci USA 86: 5610–5614.
Harwig SSL, Park ASK, Lehrer RI 1992 Characterization of defensin precursors in mature human neutrophils. Blood 79: 1532–1537.
Selsted ME, Miller SI, Henschen AH, Ouellette AJ 1992 Enteric defensins: antibiotic peptide components of intestine host defense. J Cell Biol 118: 929–936.
Porter E, Liu L, Oren A, Anton P, Ganz T 1997 Localization of human intestinal defensin 5 in Paneth cell granules. Infect Immun 65: 2389–2395.
Ganz T, Selsted ME, Szklarek D, Harwig SS, Daher K, Bainton DF, Lehrer RI 1985 Defensins. Natural peptide antibiotics of human neutrophils. J Clin Invest 76: 1427–1435.
Wilde CG, Griffith JE, Marra MN, Snable JL, Scott RW 1989 Purification and characterization of human neutrophil peptide 4, a novel member of the defensin family. J Biol Chem 264: 11200–11203.
Jones DE, Bevins CL 1992 Paneth cells of the human small intestine express an antimicrobial peptide gene. J Biol Chem 267: 23216–23225.
Porter EM, Poles MA, Lee JS, Naitoh J, Bevins CL, Ganz T 1998 Isolation of human intestinal defensins from ileal neobladder urine. FEBS Lett 434: 272–276.
Jones DE, Bevins CL 1993 Defensin-6 mRNA in human Paneth cells: implications for antimicrobial peptides in host defense of the human bowel. FEBS Lett 315: 187–192.
Mallow EB, Harris A, Salzman N, Russell JP, DeBerardinis JR, Ruchelli E, Bevins CL 1996 Human enteric defensins: gene structure and developmental expression. J Biol Chem 271: 4038–4045.
Svinarich DM, Wolf NA, Gomez R, Gonik B, Romero R 1997 Detection of human defensin 5 in reproductive tissues. Am J Obstet Gynecol 176: 470–475.
Svinarich DM, Gomez R, Romero R 1997 Detection of human defensins in the placenta. Am J Reprod Immunol 38: 252–255.
Quayle AJ, Porter EM, Nussbaum AA, Wang YM, Brabec C, Yip KP, Mok SC 1998 Gene expression, immunolocalization, and secretion of human defensin-5 in human female reproductive tract. Am J Pathol 152: 1247–1258.
Valore EV, Ganz T 1992 Posttranslational processing of defensins in immature human myeloid cells. Blood 79: 1538–1544.
Zhang XL, Selsted ME, Pardi A 1992 NMR studies of defensin antimicrobial peptides. 1. Resonance assignment and secondary structure determination of rabbit NP-2 and human HNP-1. Biochemistry 31: 11348–11356.
Lencer WI, Cheung G, Strohmeier GR, Currie MG, Ouellette AJ, Selsted ME, Madara JL 1997 Induction of epithelial chloride secretion by channel-forming cryptins 2 and 3. Proc Natl Acad Sci USA 94: 8585–8589.
Daher KA, Selsted ME, Lehrer RI 1986 Direct inactivation of viruses by human granulocyte defensins. J Virol 60: 1068–1074.
Lehrer RI, Szzklarek D, Ganz T, Selsted ME 1985 Correlation of binding of rabbit granulocyte peptides to Candida albicans: correlation with candacidal activity. Infect Immun 49: 207–211.
Lehrer RI, Szklarek D, Ganz T, Selsted ME 1986 Synergistic activity of rabbit granulocyte peptides against Candida albicans. Infect Immun 52: 902–904.
Lehrer RI, Ganz T, Szklarek D, Selsted ME 1988 Modulation of the in vitro candidacidal activity of human neutrophil defensins by target cell metabolism and divalent cations. J Clin Invest 81: 1829–1835.
Aley SB, Zimmerman M, Hetsko M, Selsted ME, Gillin FD 1994 Killing of Giardia lambia by cryptdins and cationic neutrophil peptides. Infect Immun 62: 5397–5403.
Borenstein LA, Selsted ME, Lehrer RI, Miller JN 1991 Antimicrobial activity of rabbit leukocyte defensins against Treponema pallidum subsp. pallidum. Infect Immun 59: 1359–1367.
Borenstein LA, Selsted ME, Lehrer RI, Miller JN 1991 Contribution of rabbit leukocyte defensins to the host response in experimental syphilis. Infect Immun 59: 1368–1377.
Selsted ME, Tang YQ, Morris WL, McGuire PA, Novotny MJ, Smith W, Henschen AH, Cullor JS 1993 Purification, primary structures, and antibacterial activities of beta-defensins, a new family of antimicrobial peptides from bovine neutrophils. J Biol Chem 268: 6641–6648.
Diamond G, Zasloff M, Eck H, Brasseur M, Maloy WL, Bevins CL 1991 Tracheal antimicrobial peptide, a novel cysteine-rich peptide from mammalian tracheal mucosa: peptide isolation and cloning of a cDNA. Proc Natl Acad Sci USA 88: 3952–3956.
Zhao C, Wang I, Lehrer RI 1996 Widespread expression of beta-defensin hBD-1 in human secretory glands and epithelial cells. FEBS Lett 396: 319–322.
McCray PB Jr, Bentley L 1997 Human airway epithelia express a beta-defensin. Am J Respir Cell Mol Biol 16: 343–349.
Stolzenberg ED, Anderson GM, Ackermann MR, Whitlock RH, Zasloff M 1997 Epithelial antibiotic induced in states of disease. Proc Natl Acad Sci USA 94: 8686–8690.
Schonwetter BS, Stolzenberg ED, Zasloff MA 1995 Epithelial antibiotics induced at sites of inflammation. Science 267: 1645–1648.
Zhang G, Wu H, Shi J, Ganz T, Ross CR, Blecha F 1998 Molecular cloning and tissue expression of porcine beta-defensin-1. FEBS Lett 424: 37–40.
Bensch KW, Raida M, Mägert HJ, Schulz-Knappe P, Forssmann WG 1995 hBD-1: a novel β-defensin from human plasma. FEBS Lett 368: 331–335.
Valore EV, Park CH, Quayle AJ, Wiles KR, McCray PB Jr, Ganz T 1998 Human β-defensin-1: an antimicrobial peptide of urogenital tissues. J Clin Invest 101: 1633–1642.
Tarver AP, Clark DP, Diamond G, Cohen KM, Erdjument-Bromage H, Jones DE, Sweeney R, Wines M, Hwang S, Tempst P, Bevins CL 1998 Enteric β-defensin: molecular cloning and characterization of a gene with inducible intestinal epithelial expression associated with Cryptospiridium parvum expression. Infect Immun 66: 1045–1056.
Huttner KM, Brezinski-Caliguri DJ, Mahoney MM, Diamond G 1998 Antimicrobial peptide expression is developmentally regulated in the ovine gastrointestinal tract. J Nutr 128: 297S–299S.
Harwig SSL, Swiderek KM, Kokryakov VN, Tan L, Lee TD, Panyutich EA, Aleshina GM, Shamova OV, Lehrer RI 1994 Gallinacins: cysteine-rich antimicrobial peptides of chicken leukocytes. FEBS Lett 342: 281–285.
Lawyer C, Pai S, Watabe M, Bakir H, Eagleton L, Watabe K 1996 Effects of synthetic form of tracheal antimicrobial peptide on respiratory pathogens. J Antimicrob Chemother 37: 599–604.
Bals R, Goldman MJ, Wilson JM 1998 Mouse beta-defensin 1 is a salt-sensitive antimicrobial peptide present in epithelia of the lung and urogenital tract. Infect Immun 66: 1225–1232.
Russell JP, Diamond G, Tarver A, Bevins CL 1996 Coordinate induction of two antibiotic genes in tracheal epithelial cells exposed to the inflammatory mediators lipopolysaccharide and tumor necrosis factor-α. Infect Immun 64: 1565–1568.
Krisanaprakornkit S, Weinberg A, Perez CN, Dale BA 1998 Expression of the peptide antibiotic human beta-defensin 1 in cultured gingival epithelial cells and gingival tissue. Infect Immun 66: 4222–4228.
Schnapp D, Harris A 1998 Antibacterial peptides in bronchoalveolar lavage fluid. Am J Respir Cell Mol Biol 19: 352–356.
Bals R, Wang X, Wu Z, Freeman T, Bafna V, Zasloff M, Wilson JM 1998 Human β-defensin 2 is a salt-sensitive peptide antibiotic expressed in human lung. J Clin Invest 102: 874–880.
Hiratsuka T, Nakazato M, Date Y, Ashitani J, Minematsu T, Chino N, Matsukura S 1998 Identification of human beta-defensin-2 in respiratory tract and plasma and its increase in bacterial pneumonia. Biochem Biophys Res Commun 249: 943–947.
Singh PK, Jia HP, Wiles K, Hesselberth J, Liu L, Conway BA, Greenberg EP, Valore EV, Welsh MJ, Ganz T, Tack BF, McCray PB Jr 1998 Production of beta-defensins by human airway epithelia. Proc Natl Acad Sci USA 95: 14961–14966.
Zanetti M, Gennaro R, Romeo D 1995 Cathelicidins: a novel protein family with a common proregion and a variable C-terminal antimicrobial domain. FEBS Lett 374: 1–5.
Zanetti M, Del Sal, Storici P, Schneider C, Romeo D 1993 The cDNA of the neutrophil antibiotic BAC5 predicts a pro-sequence homologous to a cysteine proteinase inhibitor that is common to other neutrophil antibiotics. J Biol Chem 268: 522–526.
Levy O, Weiss J, Zarember K, Ooi CE, Elsbach P 1993 Antibacterial 15-kDa protein isoforms (p15s) are members of a novel family of leukocyte proteins. J Biol Chem 268: 6058
Mahoney MM, Lee AY, Brezinski-Caliguri DJ, Huttner KM 1995 Molecular analysis of the sheep cathelin family reveals a novel antimicrobial peptide. FEBS Lett 377: 519–522.
Zanetti M, Litteri L, Gennaro R, Horstmann H, Romeo D 1990 Bactenecins, defense polypeptides of bovine neutrophils, are generated from precursor molecules stored in the large granules. J Cell Biol 111: 1363–1371.
Storici P, Tossi A, Lenarcic B, Romeo D 1996 Purification and structural characterization of bovine cathelicidins, precursors of antimicrobial peptides. Eur J Biochem 238: 769–776.
Scocchi M, Skerlavaj B, Romeo D, Gennaro R 1992 Proteolytic cleavage by neutrophil elastase converts inactive storage proforms to antibacterial bactenecins. Eur J Biochem 209: 589–595.
Panyutich A, Shi J, Boutz PL, Zhao C, Ganz T 1997 Porcine polymorphonuclear leukocytes generate extracellular microbicidal activity by elastase-mediated activation of secreted proprotegrins. Infect Immun 65: 978–985.
Storici P, Del Sal, Schneider C, Zanetti M 1992 cDNA sequence analysis of an antibiotic dodecapeptide from neutrophils. FEBS Lett 314: 187–190.
Del Sal, Storici P, Schneider C, Romeo D, Zanetti M 1992 cDNA cloning of the neutrophil bactericidal peptide indolicidin. Biochem Biophys Res Commun 187: 467–472.
Storici P, Zanetti M 1993 A cDNA derived from pig bone marrow cells predicts a sequence identical to the intestinal antibacterial peptide PR-39. Biochem Biophys Res Commun 196: 1058–1065.
Storici P, Zanetti M 1993 A novel cDNA sequence encoding a pig leukocyte antimicrobial peptide with a cathelin-like pro-sequence. Biochem Biophys Res Commun 196: 1363–1368.
Zhao C, Liu L, Lehrer RI 1994 Identification of a new member of the protegrin family by cDNA cloning. FEBS Lett 346: 285–288.
Zanetti M, Storici P, Tossi A, Scocchi M, Gennaro R 1994 Molecular cloning and chemical synthesis of a novel antibacterial peptide derived from pig myeloid cells. J Biol Chem 269: 7855–7858.
Scocchi M, Romeo D, Zanetti M 1994 Molecular cloning of Bac7, a proline- and arginine-rich antimicrobial peptide from bovine neutrophils. FEBS Lett 352: 197–200.
Storici P, Scocchi M, Tossi A, Gennaro R, Zanetti M 1994 Chemical synthesis and biological activity of a novel antibacterial peptide deduced from a pig myeloid cDNA. FEBS Lett 337: 303–307.
Zhao C, Ganz T, Lehrer RI 1995 The structure of porcine protegrin genes. FEBS Lett 368: 197–202.
Bagella L, Scocchi M, Zanetti M 1995 cDNA sequences of three sheep myeloid cathelicidins. FEBS Lett 376: 225–228.
Tossi A, Scocchi M, Zanetti M, Storici P, Gennaro R 1995 PMAP-37, a novel antibacterial peptide from pig myeloid cells. cDNA cloning, chemical synthesis and activity. Eur J Biochem 228: 941–946.
Zhao C, Ganz T, Lehrer RI 1995 Structures of genes for two cathelin-associated antimicrobial peptides: prophenin-2 and PR-39. FEBS Lett 376: 130–134.
Skerlavaj B, Gennaro R, Bagella L, Merluzzi L, Risso A, Zanetti M 1996 Biological characterization of two novel cathelicidin-derived peptides and identification of structural requirements for their antimicrobial and cell lytic activities. J Biol Chem 271: 28375–28381.
Scocchi M, Wang S, Zanetti M 1997 Structural organization of the bovine cathelicidin gene family and identification of a novel member. FEBS Lett 417: 311–315.
Agerberth B, Gunne H, Odeberg J, Kogner P, Boman HG, Gudmundsson GH 1995 FALL-39, a putative human peptide antibiotic, is cysteine-free and expressed in bone marrow and testis. Proc Natl Acad Sci USA 92: 195–199.
Gallo RL, Kim KJ, Bernfield M, Kozak CA, Zanetti M, Merluzzi L, Gennaro R 1997 Identification of CRAMP, a cathelin-related antimicrobial peptide expressed in the embryonic and adult mouse. J. Biol Chem 272: 13088–13093.
Gudmundsson G, Agerberth B, Odeberg J, Bergman T, Olsson B, Salcedo R 1996 The human gene FALL39 and processing of the cathelin precursor to the antibacterial peptide LL-37 in granulocytes. Eur J Biochem 238: 325–332.
Bals R, Wang X, Zasloff M, Wilson JM 1998 The peptide antibiotic LL-37/hCAP-18 is expressed in epithelia of the human lung where it has broad antimicrobial activity at the airway surface. Proc Natl Acad Sci USA 95: 9541–9546.
Frohm M, Agerberth B, Ahangari G, Stahle-Backdahl M, Liden S, Wigzell H, Gudmundsson GH 1997 The expression of the gene coding for the antibacterial peptide LL-37 is induced in human keratinocytes during inflammatory disorders. J Biol Chem 272: 15258–15263.
Yeaman MR, Tang YQ, Shen AJ, Bayer AS, Selsted ME 1997 Purification and in vitro activities of rabbit platelet microbicidal proteins. Infect Immun 65: 1023–1031.
Xu T, Levitz SM, Diamond RD, Oppenheim FG 1991 Anticandidial activity of major human salivary histatins. Infect Immun 59: 2549–2554.
Schlievert P, Johnson W, Galask RP 1976 Isolation of a low-molecular-weight antibacterial system from human amniotic fluid. Infect Immun 14: 1156–1166.
Brogden KA, De Lucca, Bland J, Elliott S 1996 Isolation of an ovine pulmonary surfactant-associated anionic peptide bactericidal for Pasteurella haemolytica. Proc Natl Acad Sci USA 93: 412–416.
Brogden KA, Ackermann M, Huttner KM 1997 Small, anionic, and charge-neutralizing propeptide fragments of zymogens are antimicrobial. Antimicrob Agents Chemother 41: 1615–1617.
Ganz T, Rayner JR, Valore EV, Tumolo A, Talmadge K, Fuller F 1989 The structure of the rabbit macrophage defensin genes and their organ-specific expression. J Immunol 143: 1358–1365.
Ouellette AJ, Cordell B 1988 Accumulation of abundant messenger ribonucleic acids during postnatal development of mouse small intestine. Gastroenterology 94: 114–121.
Ouellette AJ, Greco RM, James M, Frederick D, Naftilan J, Fallon JT 1989 Developmental regulation of cryptdin, a corticostatin/defensin precursor mRNA in mouse small intestinal crypt epithelium. J Cell Biol 108: 1687–1695.
Darmoul D, Brown D, Selsted ME, Ouellette AJ 1997 Cryptdin gene expression in developing mouse small intestine. Am J Physiol 272:G197–G206.
Levy O, Ooi CE, Weiss J, Lehrer RI, Elsbach P 1994 Individual and synergistic effects of rabbit granulocyte proteins on Escherichia coli. J Clin Invest 94: 672–682.
Westerhoff HV, Zasloff M, Rosner JL, Hendler RW, DeWaal A, VazGomez A, Jongsma APM, Riethorst A, Juretic D 1995 Functional synergism of the magainins PGLa and magainin-2 in E. coli, tumor cells, and liposomes. Eur J Biochem 228: 257–264.
Panyutich AV, Hiemstra PS, van Wetering, Ganz T 1995 Human neutrophil defensin and serpins form complexes and inactivate each other. Am J Respir Cell Mol Biol 12: 351–357.
Territo MC, Ganz T, Selsted ME, Lehrer R 1989 Monocyte-chemotactic activity of defensins from human neutrophils. J Clin Invest 84: 2017–2020.
Huang HJ, Ross CR, Blecha F 1997 Chemoattractant properties of PR-39, a neutrophil antibacterial peptide. J Leukoc Biol 61: 624–629.
Chertov O, Michiel DF, Xu L, Wang JM, Tani L, Murphy WJ, Longo DL, Taub DD, Oppenheim JJ 1996 Identification of defensin-1, defensin-2, and CAP37/azurocidin as T-cell chemoattractant proteins released from interleukin-8-stimulated neutrophils. J Biol Chem 271: 2935–2940.
Murphy CJ, Foster BA, Mannis MJ, Selsted ME, Reid TW 1993 Defensins are mitogenic for epithelial cells and fibroblasts. J Cell Physiol 155: 408–413.
Zhu Q, Singh AV, Bateman A, Esch F, Solomon S 1987 The corticostatic (anti-ACTH) and cytotoxic activity of peptides isolated from fetal, adult, and tumor-bearing lung. J Ster Biochem 27: 1017–1022.
Singh A, Bateman A, Zhu QZ, Shimasaki S, Esch F, Solomon S 1988 Structure of a novel human granulocyte peptide with anti-ACTH activity. Bioch Biophys Res Commun 155: 524–529.
Higazi AAR, Ganz T, Kariko K, Cines DB 1996 Defensin modulates tissue-type plasminogen activator and plasminogen binding to fibrin and endothelial cells. J Biol Chem 271: 17650–17655.
Higazi AA, Lavi E, Bdeir K, Ulrich AM, Jamieson DG, Rader DJ, Usher DC, Kane W, Ganz T, Cines DB 1997 Defensin stimulates the binding of lipoprotein (a) to human vascular endothelial and smooth muscle cells. Blood 89: 4290–4298.
Zhao C, Liaw L, Lee IH, Lehrer RI 1997 cDNA cloning of Clavanins: antimicrobial peptides of tunicate hemocytes. FEBS Lett 410: 490–492.
Zhao C, Liaw L, Lee IH, Lehrer RI 1997 cDNA cloning of three cecropin-like antimicrobial peptides (Styelins) from the tunicate, Styela clava. FEBS Lett 412: 144–148.
Salzman NH, Polin RA, Harris MC, Ruchelli E, Hebra A, Zirin-Butler S, Jawad A, Martin Porter, Bevins CL 1998 Enteric defensin expression in necrotizing enterocolitis. Pediatr Res 44: 20–26.
Groisman EA, Chiao E, Lipps CJ, Heffron F 1989 Salmonella typhimurium phoP virulence gene is a transcriptional regulator. Proc Natl Acad Sci USA 86: 7077–7081.
Miller SI, Pulkkinen WS, Selsted ME, Mekalanos JJ 1990 Characterization of defensin resistance phenotypes associated with mutations in the phoP virulence regulon of Salmonella typhinurium. Infect Immun 58: 3706–3710.
Gunn JS, Miller SI 1996 PhoP-PhoQ activates transcription of pmrAB, encoding a two-component regulatory system involved in Salmonella typhimurium antimicrobial peptide resistance. J Bacteriol 178: 6857–6864.
Porter E, van Dam, Valore E, Ganz T 1997 Broad spectrum antimicrobial activity of human intestinal defensin 5. Infect Immun 65: 2396–2401.
Lemaitre B, Nicolas E, Michaut L, Reichhart JM, Hoffmann JA 1996 The dorsoventral regulatory gene cassette spatzle/Toll/cactus controls the potent antifungal response in drosophila adults. Cell 86: 973–983.
Hoffmann JA, Reichart JM 1997 Drosophila immunity. Trends Cell Biol 7: 309–316.
Epple P, Apel K, Bohlmann H 1997 Overexpression of an endogenous thionin enhances resistance of Arabidopsis against Fusarium oxysporum. Plant Cell 9: 509–520.
Davis PB, Drumm M, Konstan MW 1996 Cystic fibrosis. Am J Respir Crit Care Med 154: 1229–1256.
Smith JJ, Travis SM, Greenberg EP, Welsh MJ 1996 Cystic fibrosis airway epithelia fail to kill bacteria because of abnormal airway surface fluid. Cell 85: 229–236.
Goldman MJ, Anderson GM, Stolzenberg ED, Kari UP, Zasloff M, Wilson JM 1997 Human beta-defensin-1 is a salt-sensitive antibiotic in lung that is inactivated in cystic fibrosis. Cell 88: 553–560.
Palfree RG, Sadro LC, Solomon S 1993 The gene encoding the human corticostatin HP-4 precursor contains a recent 86-base duplication and is located on chromosome 8. Mol Endocrinol 7: 199–205.
Ganz T, Selsted ME, Lehrer RI 1990 Defensins. Eur J Haematol 44: 1–8.
Mars WM, Stellrecht CM, Stass S, Frazier ML, Saunders GF 1987 Localization of an abundant myeloid mRNA to individual leukocytes in mixed cell populations. Leukemia 1: 167–172.
Auphan N, DiDonato JA, Rosette C, Helmberg A, Karin M 1995 Immunosuppression by glucocorticoids: inhibition of NF-kB activity through induction of IkB synthesis. Science 270: 286–290.
Simmaco M, Boman A, Mangoni ML, Mignogna G, Miele R, Barra D, Boman HG 1997 Effect of glucocorticoids on the synthesis of antimicrobial peptides in amphibian skin. FEBS Lett 416: 273–275.
Kelley KJ 1996 Using host defenses to fight infectious diseases. Nature Biotech 14: 587–590.
Spitznagel JK 1997 Origins and development of peptide antibiotic research. From extracts to abstracts to contracts. Methods Mol Biol 78: 1–14.
Selsted ME, Brown DM, DeLange RJ, Harwig SSL, Lehrer RI 1985 Primary structures of six antimicrobial peptides of rabbit peritoneal neutrophils. J Biol Chem 260: 4579–4585.
Ryan LK, Rhodes J, Bhat M, Diamond G 1996 Expression of beta-defensin genes in bovine alveolar macrophages. Infect Immun 66: 878–881.
Ouellette AJ, Lualdi JC 1990 A novel mouse gene family coding for cationic, cysteine-rich peptides. J Biol Chem 265: 9831–9837.
Fulton C, Anderson GM, Zasloff M, Bull R, Quinn AG 1997 Expression of natural peptide antibiotics in human skin. Lancet 350: 1750–1751.
Ouellette AJ, Miller SI, Henschen AH, Selsted ME 1992 Purification and primary structure of murine cryptdin-1, a Paneth cell defensin. FEBS Lett 304: 146–148.
Eisenhauer PB, Harwig SSSL, Lehrer RI 1992 Cryptdins: antimicrobial defensins of the murine small intestine. Infect Immun 60: 3556–3565.
Bateman A, MacLeod RJ, Lembessis P, Hu J, Esch F, Solomon S 1996 The isolation and characterization of a novel corticostatin/defensin-like peptide from the kidney. J Biol Chem 271: 10654–10659.
Cowland JB, Johnsen AH, Borregaard N 1995 hCAP-18, a cathelin/pro-bactenecin-like protein of human neutrophil specific granules. FEBS Lett 368: 173–176.
Romeo D, Skerlavaj B, Bolognesi M, Gennaro R 1988 Structure and bactericidal activity of an antibiotic dodecapeptide purified from bovine neutrophils. J Biol Chem 263: 9573–9575.
Gennaro R, Skerlavaj B, Romeo D 1989 Purification, composition, and activity of two bactenecins, antibacterial peptides of bovine neutrophils. Infect Immun 57: 3142–3146.
Selsted ME, Novotny MJ, Morris WL, Tang YQ, Smith W, Cullor JS 1992 Indolicidin, a novel bactericidal tridecapeptide amide from neutrophils. J Biol Chem 267: 4292–4295.
Tossi A, Scocchi M, Skerlavaj B, Gennaro R 1994 Identification and characterization of a primary antibacterial domain in CAP18, a lipopolysaccharide binding protein from rabbit leukocytes. FEBS Lett 339: 108–112.
Agerberth B, Lee JY, Bergman T, Carlquist M, Boman HG, Mutt V, Jörnvall H 1991 Amino acid sequence of PR-39, isolation from pig intestine of a new member of the family of proline-arginine-rich antibacterial peptides. Eur J Biochem 202: 849–854.
Kokryakov VN, Harwig SS, Panyutich EA, Shevchenko AA, Aleshina GM, Shamova OV, Korneva HA, Lehrer RI 1993 Protegrins: leukocyte antimicrobial peptides that combine features of corticostatic defensins and tachyplesins. FEBS Lett 315: 231–236.
Pungercar J, Strukelj B, Kopitar G, Renko M, Lenarcic B, Gubensek F, Turk V 1993 Molecular cloning of a putative homolog of proline/arginine-rich antibacterial peptides from porcine bone marrow. FEBS Lett 336: 284–288.
Harwig SS, Kokryakov VN, Swiderek KM, Aleshina GM, Zhao C, Lehrer RI 1995 Prophenin-1, an exceptionally proline-rich antimicrobial peptide from porcine leukocytes. FEBS Lett 362: 65–69.
Harwig SS, Waring A, Yang HJ, Cho Y, Tan L, Lehrer RI 1996 Intramolecular disulfide bonds enhance the antimicrobial and lytic activities of protegrins at physiological sodium chloride concentrations. Eur J Biochem 240: 352–357.
Selsted ME, Harwig SS, Ganz T, Schilling JW, Lehrer RI 1985 Primary structures of three human neutrophil defensins. J Clin Invest 76: 1436–1439.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Huttner, K., Bevins, C. Antimicrobial Peptides as Mediators of Epithelial Host Defense. Pediatr Res 45, 785–794 (1999). https://doi.org/10.1203/00006450-199906000-00001
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199906000-00001
This article is cited by
-
Expression and characterization of the new antimicrobial peptide AP138L-arg26 anti Staphylococcus aureus
Applied Microbiology and Biotechnology (2024)
-
Associations of PART1 and DEFB1 polymorphisms with Dental Caries in twelve-year-old children in Southern China: a cross-sectional study
BMC Pediatrics (2023)
-
Campylobacter jejuni infection of conventionally colonized mice lacking nucleotide-oligomerization-domain-2
Gut Pathogens (2017)
-
Immune responses upon Campylobacter jejuni infection of secondary abiotic mice lacking nucleotide-oligomerization-domain-2
Gut Pathogens (2017)
-
Purification and characterization of a novel antimicrobial peptide from sheep reproductive tract
Biotechnology Letters (2015)