Abstract
Employing immunohistochemical and Western blot analyses, we investigated the cellular localization (22-d fetal and 14-d postnatal animals) and concentrations (22-d fetal to 21-d postnatal animals) of rat hepatic glucose transporters (Glut 1 and Glut 2) and glucokinase in response to development and uteroplacental insufficiency with IUGR. Glut 1, the predominant fetal hematopoietic cellular isoform, persisted in postnatal hematopoietic islands and was noted minimally in fetal hepatic cellular membranes. A ≈40% extrauterine decline in Glut 1 levels paralleled the decline in hematopoietic cells. IUGR increased the fetal hepatic Glut 1 levels in parallel with an expanded hematopoietic cell mass (p < 0.05). In contrast, IUGR failed to alter the 2-fold increase in extrauterine Glut 2 concentrations(1-7-d postnatal animals), the isoform found in fetal and postnatal hepatocytic cell membranes. Glucokinase, the nuclear enzyme, increased 25% postnatally. IUGR caused a 16% increase in fetal glucokinase levels and a≈25% decline at postnatal d 1 (p < 0.05) without a comparable change in the hepatocytic cell number (92 ± 6 versus 86± 4). We conclude that hepatic Glut 1 concentrations reflect the extramedullary hematopoietic cellular mass, whereas extrauterine Glut 2 changes herald the need for enhanced flexibility in hepatocytic glucose transport with the initiation of food ingestion. The age-related alteration along with the IUGR-induced compensatory changes in the nuclear-mitochondrial glucokinase levels attributes a critical role for this enzyme in perinatal hepatocytic glucose homeostasis.
Similar content being viewed by others
Main
IUGR has profound adverse effects on fetal physiology and metabolism. Among the changes described are an imbalance in fetal and postnatal glucose homeostasis secondary to a restricted nutrient supply(1, 2). In addition to low fetal plasma glucose levels, IUGR is associated with depletion of liver glycogen stores, delayed induction of gluconeogenesis, and a change in liver glucose utilization rate(2–6). These responses suggest that transport of glucose and its entry into intermediary metabolism by the liver and production of glucose and its exit from the liver may be influenced by uteroplacental insufficiency leading to IUGR.
As in many tissues, glucose transport in the liver is a process of facilitated diffusion mediated by a family of structurally related, membrane spanning glycoproteins called glucose transporters(7, 8). Of the six major facilitative isoforms cloned to date, Glut 2, the high Km (15 to 20 mM) isoform, which facilitates bidirectional transport of glucose, is predominantly expressed in adult hepatocytes(9–11). Glut 1, the low Km(1-2 mM) ubiquitous isoform, is expressed only by the adult periportal and perivenular hepatocytes(12, 13). Although glucose transport in insulin-responsive adult tissues has been observed to be rate-limiting(14, 15), it has become apparent that Glut 2 mediated cellular glucose transport is not rate-limiting(16, 17). Once glucose has been transported into adult cells expressing Glut 2, intracellular glucose phosphorylation mediated by the enzyme glucokinase has proven to be the rate-limiting step in this process(18). Studies in the adult rat have observed that circulating glucose concentrations form a powerful stimulus for Glut 2 and Glut 1 transcription and expression in other tissues(19, 20). Starvation-induced hypoglycemia caused an increase in liver Glut 1 protein with no effect upon Glut 2 protein concentrations. However, removal of this nutrient restriction with refeeding led to an increase in both the hepatic Glut 1 and Glut 2 concentrations(21).
In contrast to these adult studies, although conditions of nutrient restriction exist in the fetus(1, 2), there are no studies to date examining the cell-specific localization and concentrations of these two glucose transporter isoforms in the intact fetal liver. Further, the level of Glut 1, Glut 2, and the glucokinase enzyme proteins in fetal, neonatal, and juvenile livers has not been characterized. In addition, the effect of a nutrient restrictive environment causing IUGR upon fetal hepatic Glut 1, Glut 2, and glucokinase protein levels has not been explored. Similarly, the intrauterine restrictive effect upon hepatic glucose transporter isoform and glucokinase amounts in the neonatal and juvenile progeny after the removal of the in utero nutrient restrictive environment has not been investigated. Based upon this lack of information we hypothesized that normal development and uteroplacental insufficiency associated with IUGR will cause perturbations in fetal hepatic glucose transporter and glucokinase enzyme levels, which will revert to baseline after the postnatal removal of the nutritively restricted environment. To test this hypothesis we undertook the present study and investigated the effect of development and maternal uterine artery ligation upon fetal, neonatal, and juvenile hepatic Glut 1, Glut 2, and glucokinase protein levels and the cell-specific localization of these proteins in the fetal and postnatal rat livers.
METHODS
Materials. All chemicals were obtained from commercial vendors and were of molecular biology grade.
Animals. Time-dated pregnant Sprague-Dawley rats were obtained from Taconic Laboratories (Germantown, NY). Pregnant rats were housed in individual cages and allowed ad libitum access to rat chow and maintained in 12-h light/dark cycles. The use and care of animals was approved by the Institutional Animal Care Committee in accordance with the guidelines established by the National Institutes of Health.
IUGR model. The pregnant rats were starved 2 h before surgery. Timed 19-d pregnant rats (fertilization = 1 d; term ≈22-23 d) underwent laparotomy with methoxyflurane inhalational anesthesia. The uterus was exteriorized, and complete bilateral uterine artery ligation was performed(IUGR). Sham-operated control animals underwent the same procedure, including exteriorization of the uterus, except that uterine artery ligation was not performed. The animals recovered with in 20-30 min of the procedure and were returned to their respective cages and allowed free access to standard laboratory chow (Purina Co., St. Louis, MO) and water(22).
Fetal studies. On d 22 of pregnancy the dams were given intraperitoneal pentobarbital (60 mg/kg), and the fetuses were delivered by hysterotomy. Fetuses from a single litter were pooled, and the fetal body weight was determined. Brains and livers were quickly removed and placed in ice-cold PBS. The pooled livers and brains were weighed, frozen rapidly under liquid nitrogen, and stored at -70°C. Pooled blood from either a single litter or two litters was collected on ice at decapitation, and the plasma was separated by centrifugation at 4°C and saved in aliquots at -70°C for further analyses.
Postnatal studies. Animals operated on d 19 of pregnancy were allowed to proceed to term (22-23 d) and deliver spontaneously. The number of pups was maintained at nine per litter for both IUGR and control progeny by culling or pooling litters if necessary. Close attention was paid to maternal nesting and maternal/neonatal feeding behavior in control and IUGR animals. Pups that appeared to be not feeding well, or to be severely runted in comparison with litter-mates, were excluded from the study. On d 1, 7, 14, and 21 of postnatal life, blood and livers were obtained from both the study groups, as above, and stored at -70°C.
Plasma assays. Plasma had to be pooled from two litters at times to obtain adequate amounts to assess glucose, insulin, and corticosterone concentrations. Fetal and neonatal plasma glucose concentrations were measured by a standard glucose oxidase method using a Beckman 2 glucose analyzer (Beckman, Fullerton, CA)(23). Plasma corticosterone and insulin concentrations were measured by RIAs as described previously(23, 24).
Immunohistochemistry. Liver tissues from sham-operated and IUGR 22-d fetal and 14-d postnatal animals were snap frozen in liquid nitrogen. Histologic examination and immunostaining were undertaken in portions of frozen liver that were thawed in 10% buffered formaldehyde, sliced into 2-mm sections, and processed for paraffin embedding. Six-micron thick paraffin sections were obtained on Super Frost Plus glass slides (Fisher Scientific, Pittsburgh, PA) and stained with hematoxylin and eosin or with different antibodies as outlined below. The affinity-purified antibodies used were each raised in rabbit against the rat Glut 1 COOH-terminal peptide(25), GST-rat Glut 2 COOH-terminal peptide fusion protein(26) (Charles River Pharmservices, Southbridge, MA), and the human glucokinase enzyme(27). In addition, an antibody raised in sheep against the GST rat glucokinase fusion peptide was also used(28).
After hematoxylin-eosin staining of liver sections, hematopoietic and hepatic cells in a total of 10 high power fields (magnification, ×250) from each treatment group at fetal d 22 and postnatal d 14 were manually counted. A minimum of a single high power field per representative section from different fetal and postnatal litters was included. In addition to absolute numbers, the hematopoietic to hepatocytic cellular ratio was calculated to determine the relative change in cell numbers from fetal to postnatal age and due to IUGR.
The immunostaining procedure was essentially similar to that described previously(26). Briefly, after deparaffinization, the sections were immersed in a 4% solution of paraformaldehyde in PBS, pH 7.4, for 5 min. The sections were then treated with 0.05% trypsin in 0.1% calcium chloride for 15 min at 37°C. After two washes in PBS for 5 min each, the sections were incubated in 3% hydrogen peroxide for 10 min. After three washes in PBS of 5 min each, the sections were blocked with normal goat serum (1:5 dilution in PBS) for 20 min. The sections were overlaid with the primary antibody diluted in PBS, covered with strips of Parafilm, and placed in a moist chamber for incubation overnight at 4°C. Negative controls included incubation with preimmune rabbit or sheep serum, the corresponding peptide preabsorbed primary antibody, or omission of the primary antibody. After three washes in PBS of 5 min each, the blocking step was repeated for 10 min, and the sections were then incubated with goat anti-rabbit or anti-sheep IgG conjugated with horseradish peroxidase (Bio-Rad, Richmond, CA), diluted 1:20 in PBS, for 20 min at room temperature. After three rinses in PBS for 5 min each, the sections were covered with a solution of 3,3′-diaminobenzidine tetrahydrochloride (Sigma Chemical Co. St. Louis, MO) in PBS (6 mg of 3,3′-diaminobenzidine tetrahydrochloride in 30 mL of PBS) to which 60μL of 3% hydrogen peroxide was added immediately before use. After a 10-min incubation, the sections were washed three times in PBS for 5 min each. Staining intensification was undertaken by exposing the sections to 1% osmium tetroxide in PBS for 15 min. After three more washes in PBS, the sections were counterstained in a 1% solution of Fast Green for 5 min. The sections were dehydrated through graded alcohols, cleared in xylene, and mounted in Canada balsam.
Western blot analysis. Hepatic tissue homogenates were prepared by mechanical homogenization using a Tissuemizer (Tekmar, Cincinnati, OH). Protein content was determined by the Bio-Rad protein dye binding assay(Bio-Rad, Richmond, CA). Protein, 75 μg per tissue sample, was subjected to discontinuous 10% SDS-PAGE followed by electroblot transfer to nitrocellulose(Nytran, Schleicher & Schuell, Keene, NH). Equality of loading and efficiency of transfer were assessed by Coomassie Blue staining of the gel and by Ponceau S staining of the filters. The nitrocellulose filters were incubated overnight at 4°C in 5% nonfat dry milk in PBS to decrease nonspecific binding of the antibody. This was followed by incubation with either the affinity-purified rabbit anti-rat Glut 1 (0.5 mg/mL)(25), anti-GST-rat Glut 2 (0.75 mg/mL)(26) (Charles River Pharmservices, South-bridge, MA) COOH-terminal peptides, sheep anti-GST-rat glucokinase (1:500 dilution)(28) IgGs, or rabbit anti-human glucokinase(27) IgG (1:500 dilution) for 16 h at room temperature. After washing in PBS/1% Triton X-100, the filters were incubated with 2.5× 105 cpm/mL of 125I-labeled goat anti-rabbit IgG (12.5 mCi/mg) or anti-sheep IgG/protein A (ICN, Irvine, CA) for 2 h at 23°C. After extensive washing, the blots were air-dried and subjected to autoradiography for 2-7 d. The areas of the filters corresponding to the glucose transporter and glucokinase bands as seen on the autoradiographs were cut out, and the radioactivity was measured using a Beckman γ-counter. Background activity was measured in blank areas of the filters and subtracted from the glucose transporter or glucokinase protein band-associated radioactivity. Interlane loading variability was standardized as previously described(23).
Data analysis. All data are presented as mean ± SEM. A t test was used to compare two age-matched groups, which consist of the IUGR and sham-operated control animals. When more than two groups were compared as in the developmental study, one-way analysis was used, and intergroup differences were detected by the post hoc Newman-Kuel's multiple comparison test.
RESULTS
Asymmetrical growth restriction was produced in the 22-d fetus and 1-d newborn by bilateral uterine artery ligation (Table 1) as seen by the ≈25% reduction in body and liver weights with no change in brain weights. By 7 d of postnatal age, body and liver weights were comparable, indicating catch-up growth. No differences in liver protein or RNA per g of tissue were observed between sham-operated control and IUGR animals except for a catch-up compensatory increase in RNA in the 7-d postnatal IUGR group when compared with age-matched control animals (Table 1). The total fetal loss rate due to uteroplacental insufficiency was≈30% in the ligated animals compared with 3% in the sham-operated control animals. As has been described previously(1) our present model also resulted in fetal hypoglycemia, which resolved in the postnatal 1-d-old animals (Table 2). No statistically significant change in fetal or postnatal plasma insulin concentrations was observed between the two groups, despite a trend toward lower fetal insulin concentrations in the IUGR group. Similarly, no difference was observed between the two groups in fetal plasma corticosterone concentrations.
Quantitation of hematopoietic and hepatocytic cells per given high power field revealed a 15-fold decline in hematopoietic cells from the 22-d fetal to the 14-d postnatal stages, with a 50% increase in hepatocytic cells(Table 3). IUGR caused a 2-fold increase in fetal hematopoietic cells, which did not persist postnatally. In contrast, IUGR was not associated with any change in fetal or postnatal hepatocytic cell numbers(Table 3). These differences in the two cell populations resulted in an IUGR-induced 2-fold increase in the fetal hematopoietic to hepatocytic cellular ratio with no effect upon the corresponding postnatal cellular ratio (Table 3).
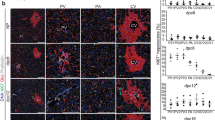
In keeping with the quantitation results, hematoxylin-eosin-stained morphology of liver sections revealed a visual increase in hematopoietic cells within the liver of the IUGR fetus (Fig. 1A) when compared with the age-matched sham-operated control (Fig. 1B). In the 14-d postnatal stage, mere islands of hematopoietic cells remained in the liver of the IUGR group (Fig. 1C), whereas none to minimal hematopoietic cells were observed in the age-matched sham-operated control liver sections (Fig. 1D). Immunolocalization experiments demonstrated that Glut 1 was primarily observed in hematopoietic cells found with in the fetal livers along with minimal amounts in the hepatocytic plasma membranes (Fig. 2,A and B). The IUGR fetal liver section demonstrated a visual increase in Glut 1 immunoreactive hematopoietic cells (Fig. 2A) when compared with the fetal sham-operated controls (Fig. 2B). These fetal Glut 1 stained hematopoietic cells visually diminished at 14-d postnatal age and were similar in both the IUGR (not shown) and sham-operated control (Fig. 2C) groups. No postnatal hepatocytic Glut 1 staining was observed (Fig. 2C) in either treatment groups. In contrast, Glut 2 was localized only to the fetal (Fig. 3A) and postnatal (Fig. 3B) hepatocytic plasma membranes. No difference in the localization or intensity of the Glut 2 immunoreactivity was noted between the age-matched IUGR and sham-operated controls. Thus only a representative fetal sham-operated and a postnatal IUGR liver sections were included in Figure 3. Glucokinase immunoreactivity was observed concentrated in a select few of the fetal hepatocytic nuclei in the IUGR (Fig. 4A) and sham-operated control (Fig. 4B) groups. During the 14-d postnatal stage, glucokinase enzyme in certain cells was found more in the hepatocytic nuclear membrane (seen as peripheral nuclear staining with a central clear area) in both the IUGR group (Fig. 4C) and sham-operated controls (Fig. 4D). No other nonhepatocytic parenchymal cells found in the fetal and postnatal liver revealed Glut 1, Glut 2, or glucokinase immunoreactivity.
Hematoxylin- and eosin-stained liver sections. Hematoxylin and eosin staining of 22-d fetal (A and B) and 14-d postnatal (C and D) IUGR (A and C) and sham-operated control (B and D) livers. The 22-d fetal liver contains many islands of hematopoiesis (arrows)(B), which are generally absent from hepatic sinusoids and portal areas in the 14-d postnatal liver (D). The IUGR 22-d fetal liver shows abundant hematopoiesis within hepatic sinusoids (arrows) (A), and in the 14-d postnatal liver occasional islands of hematopoiesis persist(arrows) (C). (Original magnification, ×312.)
Immunohistochemistry-Glut 1 in liver sections. Immunoperoxidase staining for Glut 1 (antibody dilution = 1:100) in the 22-d fetal liver sections reveals immunoreactivity in hematopoietic cells (larger arrows) and some linear staining of the plasma membranes of hepatocytes(smaller arrows). The Glut 1 immunoreactive hematopoietic cells are increased in the IUGR liver sections (A) as opposed to the sham-operated controls (B). In the 14-d postnatal liver section, minimal Glut 1-stained hematopoietic cellular islands are noted (larger arrows) with no hepatocytic Glut 1 immunoreactivity. No difference in Glut 1 immunoreactivity was observed between the IUGR and the sham-operated control liver sections(C). (Original magnification, ×196.)
Immunohistochemistry-Glut 2 in liver sections. Immunoperoxidase staining for Glut 2 (antibody dilution = 1:100) in the liver sections. The 14-d postnatal and 22-d fetal liver sections demonstrate intense Glut 2 immunoreactivity in hepatocytic plasma membranes (smaller arrows) with no staining of the hematopoietic cells (larger arrows). No difference in Glut 2 staining was observed between the IUGR and the sham-operated control 22-d fetal and the 14-d postnatal liver sections. Representative 22-d fetal sham-operated control (A) and 14-d postnatal IUGR (B) liver sections are shown. (Original magnification, ×196.)
Immunohistochemistry-glucokinase in liver sections. Immunoperoxidase staining for glucokinase (antibody dilution = 1:50) in liver sections from the 22-d fetal (A and B) and the 14-d postnatal (C and D) IUGR (A and C) animals and sham-operated controls (B and D). Glucokinase immunoreactivity (small arrows) is noted in select hepatocytic nuclei in the IUGR (A) and sham-operated (B) fetuses. The glucokinase-stained hepatocytic nuclei are increased in the IUGR section(A) when compared with the sham-operated (B) fetal liver sections. Similar numbers of hepatocytic nuclear membranes demonstrate glucokinase immunoreactivity in the 14-d postnatal IUGR (C) and sham-operated (D) postnatal animals. (Original magnification×196.)
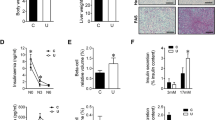
Western blot analyses of liver homogenates demonstrated a decline in hepatic ≈45-50-kD Glut 1 protein concentrations at the 1-d postnatal age when compared with the fetus (Figs. 5,top panel,and 6A). Hepatic Glut 1 levels in the 1-d postnatal rat were no different from that of the 7-, 14-, and 21-d-old postnatal rats (Fig. 6A). In contrast, fetal liver Glut 2 protein concentrations were low in the fetus, peaking in the postnatal period between ages 1 and 7 d, followed by a decline to the levels noted in the 14- and 21-d-old animals (Figs. 5,middle panel,and 6B). Glucokinase protein concentrations were similar in the 22-d fetal and 1- and 7-d postnatal livers (Figs. 5,bottom panel,and 6C). The levels of glucokinase protein in the 14- and 21-d livers were higher than that of the fetus and 1- and 7-d-old postnatal livers. Unlike the single glucokinase protein band noted in the fetal and 1-, 7-, and 14-d-old livers, two distinct protein bands were noted in the 21-d-old livers (Fig. 5, bottom panel).
Western blot analysis-Glut 1, Glut 2, and glucokinase. Western blot analyses demonstrates the 45-50-kD Glut 1 protein (top panel), the ≈45-kD Glut 2 protein (middle panel), and the ≈50-kD glucokinase(GSK) protein (bottom panel) bands in the sham-operated control(C) and the IUGR (I) groups in the 22-d fetus and at the 1-, 7-, 14-, and 21-d postnatal ages.
Quantitation of Western blots-Glut 1, Glut 2, and glucokinase. Quantitative analysis of the Western blots (A) Glut 1 concentrations at the different ages between the sham-operated controls(□) and IUGR groups (▪). A t test comparing the IUGR group with the age-matched control group at a single age = *p < 0.05. ANOVA (p < 0.0003) followed by the Neuman-Kuel's test revealed a difference at p < 0.05 between Glut 1 levels in the 22-d fetus when compared with the 1-, 7-, 14-, and 21- d sham-operated controls. No other intergroup differences were noted. A t test revealed a difference(*p < 0.05) between the 22-d fetal sham-operated control and the corresponding age-matched IUGR groups. (B) Glut 2 concentrations at different ages between sham-operated controls and the IUGR groups. No differences were observed between the two groups at all ages per a t test. ANOVA with Neuman Kuel's test revealed a difference at a p< 0.05 between d-22 fetus, 14-d postnatal age, and d 1-, 7-, and 21-d postnatal ages among the sham-operated controls and the IUGR group.(C) Comparison of glucokinase concentrations among the sham-operated control group at different ages revealed a difference at p < 0.00097 (ANOVA), with Newman-Kuel's test demonstrating differences between the 22-d fetus, 1- and 7-d, and the 14- and 21-d postnatal stages. A t test revealed a difference (*p < 0.05) between the 22-d fetal and the 1-d postnatal sham-operated control and the corresponding age-matched IUGR groups. The number (n) for quantitation of all three proteins: 22-d fetus sham-operated(7), IUGR(10); 1-d postnatal sham-operated(6), IUGR(9); 7-d sham-operated(6), IUGR(6); 14-d sham-operated(5), IUGR(5); 21-d sham-operated(5), IUGR(5).
In response to uteroplacental insufficiency causing IUGR, a 2-fold increase in fetal hepatic Glut 1 protein levels was observed when compared with the age-matched sham-operated control animals (Figs. 5,top panel,and 6A). This difference in fetal liver Glut 1 protein concentrations normalized postnatally from 1 d through 21 d of age. In contrast, no detectable effect of IUGR was noted upon fetal and postnatal hepatic Glut 2 protein levels (Figs. 5, middle panel,and 6B). However, a slight increase in fetal hepatic glucokinase protein concentrations was observed in the IUGR fetus when compared with the age-matched sham-operated control counterpart. This fetal increase was followed by a one-third decline in the 1-d-old hepatic glucokinase protein level in the IUGR group when compared with the sham-operated group. At subsequent postnatal ages of 7, 14, and 21 d, there was no difference in hepatic glucokinase protein levels (Fig. 6C).
DISCUSSION
IUGR produced by maternal uterine artery ligation has been shown to increase fetal liver glucose utilization(6). Other models of IUGR produced by maternal starvation(2) showed a decrease in hepatic glucose utilization. These seemingly incongruent effects of IUGR prompted us to more thoroughly examine the effect of uteroplacental insufficiency with IUGR upon the mechanisms that mediate hepatic glucose uptake. In the present model, 72 h of maternal uterine artery ligation resulted in an environment that was nutritively and metabolically restrictive(1, 22).
Previous studies have shown the presence of Glut 1 mRNA and protein in fetal liver(29, 30) but have not identified the cell type in situ that expresses Glut 1. These previous investigations observed developmental changes in rat liver Glut 1 mRNA and protein concentrations(29, 30) and rat and rabbit liver cytochalasin B binding(31–33), indicating high fetal glucose transporter concentrations that decline postnatally. Based upon the Km of the cytochalasin B binding experiments, an extrauterine switch over to the “adult type” of liver glucose transporter was implicated(31–33). Although in our present investigation we examined the developmental changes in sham-operated controls, the pattern mimicked that of unmanipulated animals from previous reports(29–33). We observed an age-related decline in liver Glut 1 protein concentrations along with an increase in Glut 2 (adult type) in the immediate postnatal period. Because our localization experiments demonstrated Glut 1 predominantly in hematopoietic cells found within the fetal liver, this developmental decline in Glut 1 protein concentrations paralleled the extrauterine diminution in hepatic hematopoietic tissue. Although we noted minimal Glut 1 immunoreactivity in fetal hepatocytic plasma membranes, previous studies have observed considerable amounts of Glut 1 in freshly isolated fetal hepatocytes(34). This difference may stem from the lower glucose concentrations which were present in the collagenase-containing buffers that were used in the cell isolation procedure. Extracellular glucose concentrations reciprocally regulate cellular Glut 1 concentrations(35). Given the lower Km of Glut 1 compared with Glut 2(7, 8), the minimal presence of Glut 1 in fetal hepatocytes versus postnatal hepatocytes provides an efficient glucose transport system, which helps fuel the process of glycogen synthesis that is characteristic of the late gestation fetal liver(36).
We also observed an IUGR-induced increase in fetal liver Glut 1 levels that is consistent with an expanded hematopoietic cell mass in the fetal liver due to extramedullary hematopoiesis. IUGR, however, does not appear to enhance the fetal hepatocytic Glut 1 concentrations. Increased hematopoiesis secondary to hypoxic-ischemia has been described in small for gestational age human infants(37, 38). Our present findings supportive of increased extramedullary hematopoiesis confirms the reduction in placental perfusion with resultant nutritive restriction and fetal ischemic-hypoxia causing IUGR in the rat maternal uterine artery ligation model. Although the larger fetal hematopoietic cells demonstrated Glut 1, neither in a previous study(23) nor in the present one, did we observe Glut 1 in the mature postmitotic fetal rat erythrocytes. This observation allows Glut 1 to serve as a cellular marker for the immature mitotic hematopoietic cells found in fetal liver. In keeping with the increase in the hematopoietic cellular mass and the enhanced amounts of the Glut 1 isoform, which is primarily an unidirectional transporter with the Vmax for the influx being greater than the Vmax for the efflux, an increase in fetal liver [3H]D-glucose uptake has been reported(6, 11).
In contrast to these findings with Glut 1, fetal Glut 2, the isoform with a high Km and the ability to mediate bidirectional glucose transport (influx Vmax = efflux Vmax)(7, 11), was localized to the hepatocytic plasma membrane. Previous investigations in vitro have demonstrated the presence of the Glut 2 protein in freshly isolated and cultured fetal hepatocytes(34, 35); however, our current observations have specifically localized Glut 2 in situ to the fetal hepatocytic plasma membranes. Given the low affinity for glucose, Glut 2 is able to accommodate differing concentrations of glucose in the circulation. This quality is of benefit particularly in the adult, when the portal circulation clears from the intestines a wide range of glucose loads based upon whether the animal is in a preprandial or postprandial state(10, 12, 13). A similar situation does not exist in the nonfeeding fetus where a constant ingestion of amniotic fluid occurs. Therefore fetal liver Glut 2 levels were low and uteroplacental insufficiency did not alter the basal fetal liver Glut 2 concentrations. Postnatally upon initiation of oral ingestion, a 2-fold increase in the sham-operated liver Glut 2 concentrations was observed along with only a 50% increase in the hepatocytic cell mass. This confirms an additional increase in Glut 2 per given hepatocyte. Further, no perturbation in liver Glut 2 amounts was noted as a long-term consequence of the in utero“nutritive restriction” and ischemic-hypoxia.
These IUGR-induced changes in fetal and postnatal liver glucose transporter isoforms are similar to those of previous reports in the adult rat, where starvation-induced hypoglycemia increased the number of hepatic periportal and perivenular hepatocytes that expressed the Glut 1 protein without changing Glut 2, which is found in a bulk of the adult hepatocytes(12, 13, 21). Subsequent removal of the nutritive restriction by refeeding led to alterations in Glut 1 and Glut 2 levels(21). These observations in the adult liver are distinctly different from the effect of circulating glucose concentrations upon pancreatic β-islet cellular glucose transporter protein levels(19, 20), attesting to the presence of tissue specificity in this regard. Although isolated hypoxia in other adult tissues is known to augment Glut 1 levels(39), the effect of ischemichypoxia upon adult or fetal liver Glut 1 or Glut 2 levels has not been examined previously.
Studies in transgenic mice have demonstrated that Glut 2-mediated glucose transport does not constitute the rate-limiting step in cellular glucose uptake(16, 17). Instead the intracellular glucose phosphorylation catalyzed by glucokinase is rate-limiting(18). In our present investigation we noted the presence of the glucokinase protein as early as the 22-d fetus. This observation is contrary to previous reports in which glucokinase nascent transcripts measured in isolated rat hepatocytes were not evident at postnatal d 10(40). Further, no spectrophotometrically assessed glucokinase enzyme activity was observed until postnatal d 15(30). Our present report has for the first time detected glucokinase protein in fetal rat hepatocytes by employing affinity-purified high titer anti-glucokinase antibodies with highly sensitive antigen-antibody detection systems and prolonged autoradiographic exposure times (7 d). The presence of fetal hepatocytic glucokinase was confirmed separately with the use of two different anti-glucokinase antibodies(27, 41) and by two different methods, namely Western blot and immunohistochemical analyses. The discrepancy between our present study and previous reports may stem from the fact that spectrophotometric analysis of glucokinase separate from the abundantly present hexokinase I in fetal liver may not be sensitive in detecting minimal amounts of biologically active enzyme levels(30, 42). Further, in vitro transcription in isolated hepatocytes will detect only newly synthesized enzyme transcripts but not the steady state accumulation of glucokinase enzyme transcripts(40). However, previous investigations aimed at assessing steady state glucokinase mRNA levels in fetal rat livers used total RNA rather than poly(A)+ RNA compromising the sensitivity of detection(30). In addition, the limited autoradiographic exposure times (4-48 h) that were used(30) hindered detection of small amounts of glucokinase mRNA present in fetal rat livers, becoming evident on 7 d of autoradiographic exposure (our unpublished observation). The significance of two glucokinase protein bands at postnatal d 21 remains unknown and does not represent cross-reactivity with other hexokinase isoforms, because hexokinase I(25, 41), the other hepatic isoform, is not expressed to a major extent in the 21-d postnatal liver(30).
In our present investigation, although no changes in fetal and postnatal liver Glut 2 amounts were noted, an IUGR-induced mild increase in the fetal hepatocytic glucokinase protein concentrations was observed despite no change in the hepatocytic cell numbers. Postnatally, subsequent to the removal of the“nutritively restrictive” and ischemic-hypoxic environment, a compensatory decline in the mass of this enzyme was noted at postnatal d 1, which subsequently normalized at later postnatal stages. In keeping with these changes in concentrations, glucokinase, which is a mitochondrial enzyme, was noted primarily in the fetal hepatocytic nucleus as opposed to the postnatal hepatocytic nuclear membrane. This postnatal hepatocytic glucokinase localization pattern in certain cells is similar to that previously observed in adult rat pancreatic β-islet cells, where hyperglycemia led to a translocation of glucokinase from the nucleus to the cytoplasm for biologic action(43). In our present study localization of glucokinase to the postnatal hepatocytic nuclear membranes may be due to the relatively higher postnatal circulating glucose concentrations versus the lower fetal values. Localization to nuclear membranes represents transit of glucokinase from the nucleus to the cytoplasm to mediate the increased need for intracellular glucose phosphorylation(44). This increased necessity for glucokinase action postnatally may be in response to enhanced Glut 2-mediated glucose transport into hepatocytes. Although localization and quantitation of the glucokinase protein does not translate into enzyme activity, an IUGR-induced increase in fetal enzyme levels indirectly suggests a mild increase in glucose entry into fetal hepatocytes secondary to uteroplacental insufficiency. Thus, the IUGR-induced increase in hematopoietic Glut 1 levels and the hepatocytic glucokinase concentrations both contribute toward the net increase in fetal liver glucose uptake and utilization(7). These changes serve to protect the fetal cellular glucose supply and oxidative metabolism in the presence of a nutritively restrictive and ischemic-hypoxic in utero environment. In contrast, initiation of oral ingestion postnatally leads to enhanced Glut 2-mediated hepatic glucose transport, warranting a need for increased glucose phosphorylation.
We conclude that normal development induces a differential change in liver Glut 1 and Glut 2 protein concentrations, suggestive of an extrauterine switch between the fetal Glut 1 and the adult Glut 2 liver isoforms. This switch in isoforms reflects the disappearance of the Glut 1-expressing hematopoietic cells and the enhanced need for Glut 2 in increasing numbers of hepatocytes upon initiation of oral feeds. Uteroplacental insufficiency causing IUGR doubles fetal hematopoietic Glut 1 levels due to expanding hematopoietic cell mass, and mildly elevates hepatocytic glucokinase concentrations, without affecting the hepatocytic Glut 2 amounts and cell number. Postnatally, no change in liver Glut 1 or Glut 2 levels was observed; however, an immediate compensatory decline in hepatocytic glucokinase enzyme amounts was present with no subsequent change. We speculate that the changes in liver glucokinase rather than Glut 2 implicate a critical role for the former rather than the latter in regulating hepatocytic glucose entry in this rat model of IUGR.
Abbreviations
- IUGR:
-
intrauterine growth restriction
- GST:
-
glutathione S-transferase
References
Ogata ES, Bussey ME, Finley S 1986 Altered gas exchange, limited glucose and branched amino acids, and hypoinsulinism retard fetal growth in the rat. Metabolism 35: 970–977
Leturque A, Haugle S, Revelli J-P, Burnol A-F, Kandle J, Girard J 1989 Fetal glucose utilization in response to maternal starvation and acute hyperketonemia. Am J Physiol 256:E699–E703
Pollak A, Susa JB, Stonestreet BS, Schwartz R, Oh W 1979 Phosphoenolpyruvate carboxykinase in experimental intrauterine growth retardation in rats. Pediatr Res 13: 175–179
Bussey ME, Finley S, LaBarbera A, Ogata ES 1985 Hypoglycemia in the newborn growth-retarded rat: Delayed phosphoenolpyruvate carboxykinase induction despite increased glucagon availability. Pediatr Res 19: 363–367
Oh W, D'Amadio, Yap L 1970 Carbohydrate metabolism in experimental intrauterine growth retardation in rats. Am J Obstet Gynecol 108: 415–421
Lueder FL, Ogata ES 1990 Uterine artery ligation in the maternal rat alters fetal tissue glucose utilization. Pediatr Res 28: 464–468
Devaskar SU, Mueckler M 1992 The mammalian glucose transporters. Pediatr Res 31: 1–12
Bell GI, Burant CF, Takeda J, Gould GW 1993 Structure and function of mammalian facilitative sugar transporters. J Biol Chem 268: 19161–19164
Thorens B, Sarkar HK, Kaback HR, Lodish HF 1988 Cloning and functional expression in bacteria of a novel glucose transporter present in liver, intestine, kidney, and beta pancreatic islet cells. Cell 55: 281–290
Thorens B 1992 Molecular and cellular physiology of Glut 2, a high Km facilitated diffusion glucose transporter. Int Rev Cytol 137: 209–238
Gould GW, Thomas HM, Jess TJ, Bell GI 1991 Expression of human glucose transporters in xenopus oocytes: kinetic characterization and substrate specificities of the erythrocyte, liver, and brain isoforms. Biochemistry 30: 5139–5145
Tal M, Schneider DL, Thorens B, Lodish HF 1990 Restricted expression of the erythroid/brain glucose transporter isoform to perivenous hepatocytes in rats. J Clin Invest 86: 986–992
Bilir BM, Gong TWL, Kwasiborski V, Shen CS, Fillmore CS, Berkowitz CM, Cumucio JJ 1993 Novel control of the position-dependent expression of genes in hepatocytes. J Biol Chem 268: 19776–1978
Hansen PA, Gulve EA, Marshall BA, Gao J, Pessin JE, Holloszy JO, Mueckler M 1995 Skeletal muscle glucose transport and metabolism are enhanced in transgenic mice overexpressing the Glut 4 glucose transporter. J Biol Chem 270: 1679–1684
Mueckler M, Holman G 1995 Homeostasis without a Glut. Nature 377: 100–101
Tal M, Wu Y-J, Leiser M, Surana M, Lodish H, Fleischer N, Weir G, Efrat S 1992 [Val12]H Ras downregulates Glut 2 in β cells of transgenic mice without affecting glucose homeostasis. Proc Natl Acad Sci USA 89: 5744–5748
Ishihara H, Asano T, Tsukuda K, Katagiri H, Inukai K, Anai M, Yazaki Y, Miyazaki J-I, Kikuchi M, Oka Y 1995 Human Glut 2 overexpression does not affect glucose-stimulated insulin secretion in MIN6 cells. Am J Physiol 269:E897–E902
Grupe A, Hultgren B, Ryan A, Ma YH, Bauer M, Stewart TA 1995 Transgenic knockouts reveal a critical requirement for pancreatic cell glucokinase in maintaining glucose homeostasis. Cell 83: 69–78
Chen L, Alam T, Johnson JH, Hughes S, Newgard CB, Unger RH 1990 Regulation of β-cell glucose transporter gene expression. Proc Natl Acad Sci USA 87: 4088–4092
Giddings SJ, Carnaghi LR, Shalwitz RA 1993 Hypoglycemia but not hyperglycemia induces rapid changes in pancreatic -cell gene transcription. Am J Physiol 265:E259–E266
Thorens B, Flier JS, Lodish HF, Kahn BB 1990 Differential regulation of two glucose transporters in rat liver by fasting and refeeding and by diabetes and insulin treatment. Diabetes 39: 712–719
Tracy T Jr, Bailey P, Goerke M, Sadiq F, Devaskar S, Connors R, Weber T 1989 A new model of intrauterine growth retardation. Reprod Biol Surg Forum 15: 645–647
Schroeder RE, Doria-Medina CL, Das UG, Sivitz WI, Devaskar SU 1997 Effect of maternal diabetes upon fetal rat myocardial and skeletal muscle glucose transporters. Pediatr Res 41: 11–19
Devaskar S, Ganguli S, Devaskar U, Sperling MA 1982 Glucocorticoids and hypothyroidism modulate development of fetal lung insulin receptors. Am J Physiol 242:E385–E391
Devaskar SU, Devaskar UP, Schroeder RE, deMello DE, Fiedorek FT Jr, Mueckler M 1994 Expression of genes involved in placental glucose uptake and transport in the nonobese diabetic mouse pregnancy. Am J Obstet Gynecol 171: 1316–1323
Devaskar SU, deMello DE 1996 Cell-specific localization of glucose transporter proteins in mammalian lung. J Clin Endocrinol Metab 81: 4373–4378
Brown KS, Kalinowski WW, Megill JR, Durham SK, Mookhtiar KA 1997 Glucokinase regulatory protein may interact with glucokinase in the hepatocyte nucleus. Diabetes 46: 179–186
Jetton T, Magnuson MA 1992 Heterogeneous distribution of glucokinase in B-cells of pancreatic islet. Proc Natl Acad Sci USA 89: 2619–2624
Werner H, Adamo M, Lowe WL Jr, Roberts CT, LeRoith D 1989 Developmental regulation of rat brain/Hep G2 glucose transporter gene expression. Mol Endocrinol 3: 272–279
Postic C, Leturque AE, Printz RL, Maulard P, Loizeau M, Granner DK, Girard J 1994 Development and regulation of glucose transporter and hexokinase expression in rat. Am J Physiol 266:E548–E559
Axelrod JD, Pilch PF 1983 Unique cytochalasin B binding characteristics of the hepatic glucose carrier. Biochemistry 22: 2222–2227
Wang C, Brennan WA Jr 1988 Rat skeletal muscle, liver and brain have different fetal and adult forms of the glucose transporter. Biochim Biophys Acta 946: 11–18
Chundu K, Devaskar S 1988 The ontogeny of the rabbit hepatic glucose transporter. Biochem Biophys Res Commun 155: 173–180
Levitsky LL, Zheng Q, Mink K, Rhoads DB 1994 Glut 1 and Glut 2 mRNA, protein, and glucose transporter activity in cultured fetal and adult hepatocytes. Am J Physiol 267:E88–E94
Zheng Q, Levitsky LL, Mink K, Rhoads DB 1995 Glucose regulation of glucose transporters in cultured adult and fetal hepatocytes. Metabolism 44: 1553–1558
Bourbon J, Gilbert M 1981 Role of fetal insulin in glycogen metabolism in the liver of the rat fetus. Biol Neonate 40: 38–45
Stockman JA, deAlarcan PA 1992 Hematopoiesis and Granulopoiesis. In: Polin RA, Fox WW (eds) Fetal and Neonatal Physiology. WB Saunders, Philadelphia, pp 1327–1363
Wirth FH, Goldberg KE, Lubchenco LO 1979 Neonatal hyperviscosity. I. Incidence, J Pediatr 63: 833–836
Doria-Medina CL, Lund DD, Pasley A, Sandra A, Sivitz WI 1993 Immunolocalization of Glut-1 glucose transporter in rat skeletal muscle and in normal and hypoxic cardiac tissue. Am J Physiol E454–E464
Bossard P, Decaux J-F, Juanes M, Girard J 1994 Initial expression of glucokinase gene in cultured hepatocytes from suckling rats is linked to the synthesis of an insulin-dependent protein. Eur J Biochem 223: 371–380
Schroeder RE, Devaskar UP, Trail SE, deMello DE, Cole DP, Devaskar SU 1993 Effect of maternal diabetes on the expression of genes regulating fetal brain glucose uptake. Diabetes 42: 1487–1496
Spears G, Sneyd JGT, Loten EG 1971 A method for deriving kinetic constants for two enzymes acting on the same substrate. Biochem J 125: 1149–1151
Noma Y, Bonner-Weir S, Latimer JB, Davalli AM, Weir GC 1996 Translocation of glucokinase in pancreatic β-cells during acute and chronic hyperglycemia. Endocrinology 137: 1485–1491
Hariharan N, Farrelly D, Hagan D, Hillyer D, Arbeeny C, Sabrah T, Treloar A, Brown K, Kalinowski S, Mookhtiar K 1997 Expression of human hepatic glucokinase in transgenic mice liver results in decreased glucose levels and reduced body weight. Diabetes 46: 11–16
Acknowledgements
The authors thank Dr. Mike Mueckler(Washington University, St. Louis, MO) for the Glut 1 antibody, and Dr. David James (formerly at Washington University, St. Louis, MO, now at the University of Queensland, Australia) for the rabbit anti-GST rat Glut 2 fusion protein antibody that was used in some of the experiments, whereas the commercially purchased anti-GST-Glut 2 antibody was used in others. We acknowledge Dr. Mark Magnusson (Vanderbilt University, Nashville, TN) for the sheep anti-GST rat glucokinase antibody and Dr. Kasim Mookhtiar (Bristol-Myers Squibb, PRI, Princeton, NJ) for the rabbit anti-human glucokinase antibody, both of which were used in the present studies.
Author information
Authors and Affiliations
Additional information
Supported by the Fleur-de-Lis Funds, St. Louis, MO (H.F.S.), American Diabetes Association (S.U.D.), and National Institutes of Health Grants HD25024 (S.U.D.), HD33997 (S.U.D.), and HL55600 (D.E.d).
Rights and permissions
About this article
Cite this article
Sadiq, H., Demello, D. & Devaskar, S. The Effect of Intrauterine Growth Restriction upon Fetal and Postnatal Hepatic Glucose Transporter and Glucokinase Proteins. Pediatr Res 43, 91–100 (1998). https://doi.org/10.1203/00006450-199801000-00014
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199801000-00014