Abstract
In full-term newborns, permanent closure of the ductus arteriosus is associated with the formation of a neointima that is characterized by extracellular matrix deposition and smooth muscle cell migration. Transforming growth factor-β (TGF-β), a potent modulator of extracellular matrix deposition and smooth muscle cell migration, has been found to play a role in the remodeling associated with several forms of vascular disease. We examined the protein and mRNA expression of the three mammalian isoforms of TGF-β(TGF-β1, TGF-β2, and TGF-β3) during ductus arteriosus closure in full-term lambs. We found that the temporal changes and cellular localization of the proteins and mRNAs of all three TGF-β isoforms were similar. TGF-β proteins and mRNAs were present in very low levels in the late-gestation fetal ductus. Within 24 h of delivery, there was enhanced expression of TGF-β in the newly forming neointima and outer muscle media; this continued to increase over the next 10 d. Increased expression of TGF-β in the inner muscle media and adventitia lagged behind that of the neointima and outer muscle media. TGF-β was not found in the luminal endothelial cells at any time. In contrast to the pattern described above, the appearance of TGF-β protein differed from that of mRNA in the vasa vasorum of the ductus wall. After delivery, there was an increase in TGF-β immunoreactivity in the smooth muscle cell layers of the vasa vasorum without any concurrent mRNA expression. The appearance of TGF-β at the time of ductus closure suggests an important role for this growth factor in the reorganization of the ductus wall after birth.
Similar content being viewed by others
Main
Anatomical closure of the ductus arteriosus is a necessary adaptation to extrauterine life. In full-term animals and humans, anatomical closure of the ductus arteriosus follows initial vessel constriction (functional closure) and is directly related to the loss of luminal blood flow(1, 2). The subsequent ischemia of the inner vessel wall produces acellular necrosis (of the inner muscle media) and the formation of a neointima, composed of ECM and migrating medial SMC. Unlike the full-term ductus arteriosus, the preterm ductus is more resistant to the ischemic damage that occurs during functional closure(3) and is therefore less likely to undergo reorganization and permanent anatomical closure.
The processes that initiate ductus arteriosus remodeling after birth are unknown. Certain parallels, however, can be drawn between anatomical closure of the ductus arteriosus and other models of vascular disease such as pulmonary hypertension, hypertensive atherosclerosis, and restenosis lesions after balloon angioplasty(4–7). Although unique mechanisms initiate the vascular changes associated with each of these disorders, all are characterized by the formation of a neointima, narrowing of the vessel lumen, and the increased appearance of TGF-β in the vessel wall(4–7). Because TGF-β is induced by hypoxia and ischemia(8, 9), we hypothesize that it may play an early critical role in the process of ductus remodeling.
TGF-β, a 25-kD disulfide-linked homodimer, belongs to a family of proteins that regulates the growth and differentiation of a wide variety of cells in culture(10). TGF-β is also a potent modulator of vascular SMC migration and ECM deposition in cultured cells(11–13). TGF-β is synthesized and released from cells as a latent complex that requires activation; the active TGF-β is then available to bind to specific cell membrane receptors.
There isoforms of TGF-β (TGF-β1, TGF-β2, and TGF-β3) have been characterized in mammals. Although they are thought to have qualitatively similar activities when added to cells in culture, several differences in their biologic potencies have been reported(14). In addition, the distinct isoforms have been reported to have different affinities for their receptors(15).
The following study was designed to understand the potential roles of TGF-β1, TGF-β2, and TGF-β3 during ductus arteriosus remodeling. We examined the sequential temporal and spacial changes of the three TGF-β proteins and mRNAs in the fetus and during the 1st wk of life in the full-term ovine ductus arteriosus. Understanding the events that occur during normal closure of the ductus should serve as a basis for studying the preterm patent ductus arteriosus in the future.
METHODS
Tissue fixation. Late-gestation fetal and newborn lambs were given an overdose of pentobarbital sodium. The chest was opened immediately, and the ductus arteriosus was excised and fixed as described below. Tissues were obtained from animals of the following ages: fetus (0.93-0.97 gestation,n = 5); newborn: <24 h old (n = 3); 1 d old(n = 5); 2 d old (n = 3); 4 d old (n = 4); 8 d old (n = 3); 10 d old (n = 1). Different antibodies required unique tissue preparations; therefore, the ductus arteriosus was processed by three separate protocols: 1) fixation for 16 h in fresh 4% paraformaldehyde, dehydration, and paraffin embedding; 2) fixation for 16 h in 4% paraformaldehyde, equilibration in 10% sucrose before freezing in Tissue Tek OCT (Miles Laboratories, Elkhart, IN) by isopentanol chilled in liquid N2; 3) fixation in methyl Carnoy's fixative for 24 h followed by dehydration and paraffin embedding.
Immunohistochemistry. The protocol for immunohistochemical studies of TGF-β was similar to methods we have previously reported(6). The preparation and characterization of the rabbit polyclonal antibodies to the specific TGF-β isoforms have been previously reported(16, 17). These antisera have previously been shown to be specific for each TGF-β isoform and have been used for immunohistochemistry of murine, porcine, and ovine tissues(6, 16, 17). Five-micrometer thick sections of lamb ductus arteriosus were cut from paraffin blocks, dewaxed, and hydrated through graded alcohol. The sections were incubated in PBS with 0.3% (vol/vol) Triton X-100 for 15 min, followed by incubation in methanol/0.3% hydrogen peroxide (vol/vol) for 30 min to quench endogenous peroxidase. Next, the sections were treated with hyaluronidase (1 mg/mL) in 100 mM sodium acetate, 0.85% (wt/vol) NaCl for 30 min. Nonspecific binding was blocked with normal goat serum (5%). The antibodies to each TGF-β isoform were diluted with blocking serum to 2.5 μg/mL and applied to the sections overnight at 4°C. The following day the sections were incubated with goat anti-rabbit secondary antibody (1:200 dilution: Vectastain ABC Elite kit: Vector Laboratory, Burlingame, CA) for 60 min. The sections were then exposed to avidin-biotin complex (ABC Elite kit; Vector Laboratories) and reacted with diaminobenzidine according to the manufacturer's recommendations. Finally, sections were counterstained with hematoxylin. Normal rabbit IgG was used instead of primary rabbit antibody as control.
For identification of von Willebrand factor, a similar protocol to the one described above was used. Sections were treated with trypsin (0.125%) in PBS for 15 min instead of hyaluronidase, and incubated with rabbit polyclonal antibodies to von Willebrand factor (Dakopatts, Denmark). For identification of α-SMC actin, ductus tissue that had been fixed with methyl Carnoy's fixative was used. No enzymatic digestion was necessary, and the sections were incubated with mouse MAb to α-SMC actin (Sigma Chemical Co., St. Louis, MO) and reacted with goat anti-mouse secondary antibody. Similar concentrations of an irrelevant mouse MAb were used as a control.
Probes. Previously published murine TGF-β cDNA constructs in pGEM vectors were used as templates for making isoform-specific riboprobes(18–20). The TGF-β1 construct included nucleotides 421 through 1395, whereas the TGF-β2 and TGF-β3 constructs included nucleotides 1511-1953 and 821-1440, respectively. The 35S-labeled riboprobes were prepared using Riboprobe Gemini System II (Promega, Madison, WI). The mouse cDNA fragments of TGF-β1(18). TGF-β2(20), and TGF-β3(19) were obtained from H. L. Moses (Vanderbilt University, Nashville, TN). They were cloned into the multicloning site of plasmid pGEM3Z (Promega) and used as templates for the preparation of single-stranded RNA probes using the SP6 and T7 polymerases and 35S-UTP. The radiolabeled probes were reduced by limited alkaline hydrolysis to an average size of 200-250 bp. Previous studies have shown that each probe recognizes specific TGF-β isoforms and does not cross-hybridize with other TGF-β transcripts(6).
In situ hybridization. The protocol was modified slightly from previously published methods(6). Paraformaldehydefixed tissue sections in OCT were dried at 55°C for 30 min and postfixed in 4% paraformaldehyde in PBS for 20 min. Sections were treated with proteinase K(20 μg/mL) in 50 mM Tris (pH 7.5), 5 mM EDTA at 37°C for 7.5 min, followed by retreatment in 4% paraformaldehyde in PBS. Sections were then acetylated in 0.1 M triethanolamine, pH 8, 25 mM acetic anhydride for 20 min. The sections were dehydrated through graded ethanol and air-dried for 30 min.
Tissue sections were hybridized with labeled RNA probes (0.6 × 106 counts/section) in 50% formamide, 300 mM NaCl, 10 mM Tris-HCl (pH 7.5), 5 mM EDTA, 10 mM Na2PO4, 0.02% Ficoll 400, 0.02% polyvinylpyrrolidone, 0.02% BSA, 10% dextran sulfate, 8 mM DTT, and 2% transfer RNA (10 μg/μl). Hybridization proceeded overnight at 55°C in a humidified incubator. After hybridization, the sections were washed in 5× SSC (1 × SSC = 150 mM NaCl, 15 mM sodium citrate), 10 mM DTT at 50°C for 15 min, followed by 2 × SSC containing 50% formamide, 100 mM DTT at 50°C for 60 min. The slides were then washed in TEN buffer (10 mM Tris, pH 7.5, 5 mM EDTA, 0.5 M NaCl) twice, followed by treatment with RNase A (20 μg/mL) at 37°C for 30 min. The slides were then rinsed in 2× SSC at 50°C for 30 min and 0.1 × SSC at 50°C for 30 min. Finally, the sections were dehydrated through graded ethanol containing 0.3 M ammonium acetate and dried in a desiccator for 1 h. RNase A was obtained from Boehringer Mannheim (Indianapolis, IN), whereas all other reagents were purchased from Sigma.
The dried slides were coated in melted Ilford K.5 photoemulsion (diluted 1:1 with sterile water at 42°C) and slowly dried and desiccated for 2-4 wk, depending on the experiment. Slides were then developed (Kodak D-19; Eastman Kodak, Rochester, NY) and counterstained with hematoxylin and eosin. The sections were visualized using a Leitz Orthoplan 2 brightfield and darkfield microscope.
RESULTS
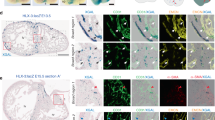
The late-gestation fetal ductus arteriosus comprises a single layer of endothelial cells separated from the smooth muscle media by a continuous internal elastic lamina. Before delivery, occasional SMC penetrate beyond the internal elastic lamina and lie directly beneath the luminal endothelial cells(Fig. 1A). Within 6 h of delivery, SMC migrate from the tunica media to the subendothelium, forming a two to six-cell layer-thick neointima (Fig. 1B). Over the next several days, the luminal endothelial cells begin to proliferate (data not shown), and migrating endothelial cells, which originate from the luminal endothelium, join the invading SMC as part of the neointima (Fig. 1C). Ultimately, the ductus lumen is obliterated by endothelial cells, migrating SMC, and ECM components (e.g. hyaluronic acid, collagen, elastin, fibronectin)(21). After cessation of luminal blood flow, the inner muscle media becomes ischemic; this is associated with cytolytic necrosis and cell loss(22, 23)(Fig. 1D). In the fetal ductus, vasa vasorum, originating from the adventitia, do not penetrate beyond the outer muscle media(Fig. 1E). In contrast, within 2 d after birth, vasa vasorum invades the vessel wall as far as the inner media(Fig. 1F), and the entire outer media becomes hyperemic(24).
Identification of endothelial cells and SMC in the ductus arteriosus. Ductus arteriosus tissue sections were incubated with antibodies to von Willebrand factor to identify endothelial cells, or antibodies to α-SMC actin to identify SMC. Cell nuclei were counterstained with hematoxylin. (A) Fetal ductus arteriosus showing a predominance of α-SMC actin staining SMC in the tunica media(M) below the internal elastic lamina (IEL) (indicated by dashed line), and nonstaining endothelial cells (EC) lining the vessel's lumen (L). Note that in several areas (arrows), SMC have penetrated beyond the internal elastic lamina and lie directly beneath the luminal endothelial cells. Magnification, 45×. (B) Six-hour-old ductus arteriosus showing α-SMC actin staining SMC invading the subendothelium, forming a neointima (NI). Magnification, 45×. (C) One-day-old ductus arteriosus stained for von Willebrand factor. Lumen has been almost completely obliterated. Former luminal endothelial cells (Lum EC) from opposite walls of the vessel have been pushed together forming a two-cell layer. Migrating endothelial cells invade the neointima. Magnification, 49×. (D) Ten-day-old ductus arteriosus with von Willebrand factor staining of the endothelial cells that form a portion of the neointima. Note the area of cell loss (CL) (with absence of hematoxylin-stained nuclei) just beyond the inner media (IM). OM, outer media. Magnification, 28×. (E) Fetal ductus arteriosus showing von Willebrand factor staining of endothelial cells lining the ductus lumen and those of the vasa vasorum (VV) lying in the adventitia (A). Magnification, 5.3×. (F) Two-day-old ductus arteriosus showing von Willebrand factor staining of new vasa vasorum invading the muscle media of the ductus wall. Magnification, 6.2×.
Immunohistochemistry. Figure 4 summarizes the changes in TGF-β protein expression in the closing full-term ductus arteriosus. The changes that occur after delivery in the expression of all three isoforms of TGF-β follow a steady progression from d 1 to 10. For ease of presentation, representative time points are illustrated for TGF-β2. TGF-β is present in very low levels in the late-term fetal ductus arteriosus (Fig. 2A). Within 24 h of delivery, TGF-β protein expression is increased throughout the vessel wall (Fig. 2B). No significant protein staining is noted in the endothelial cells that continue to line the former vessel lumen(Fig. 2D). During the first postnatal week, TGF-β expression increases especially in the thickened neointima and in the outer muscle media (Figs. 2C and4). TGF-β staining in the inner muscle media and adventitia also increases during ductus closure, but to a lesser extent than observed in the outer media and neointima(Figs. 2C and4).
Summary of protein expression of TGF-β isoforms(represented by β1, β2, and β3) in the closing ductus arteriosus. TGF-β is present in low levels in the fetal ductus arteriosus. There is enhanced protein expression in the vesell wall within 24 h of delivery; this continues to increase over the next 10 d. TGF-β protein is most concentrated in the neointima and outer muscle media. There is no protein expressed in the luminal endothelial cells. Vasa vasorum that penetrate the muscle media of the fetal ductus arteriosus also stain for TGF-β; after ductus closure, vasa vasorum in both the muscle media and adventitia stain for TGF-β (N/A, not applicable).
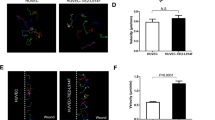
Immunohistochemistry of TGF-β2. All three TGF-β proteins showed a similar pattern of localization by immunohistochemistry. Because there were no differences in the patterns of expression of the three isoforms, only data for TGF-β2 are presented. Tissue sections were stained with TGF-β2 isoform antibody (brown pigment) and counterstained with hematoxylin. (A) Fetal ductus arteriosus demonstrating minimal immunoreactivity to TGF-β2 in the vessel wall (L, lumen; IM, internal tunica muscularis). Magnification, 45×. (B) Six-hour-old ductus arteriosus showing enhanced protein expression of TGF-β2, especially in reoriented, migrating SMC (arrows)(IEL, internal elastic lamina). Magnification, 45×.(C) Ten-day-old ductus arteriosus showing enhanced protein expression of TGF-β2, especially in the neointima (NI) and outer muscle media (OM), with loss of SMC (CL) from the inner smooth muscle media (IM). Magnification, 4.8×.(D) One-to two-day-old ductus arteriosus showing TGF-β2 staining of cells and matrix of the neointima. Note that there is no TGF-β2 staining of the endothelial cells (Lum EC) that line the former lumen of the vessel. New vasa vasorum (VV) have formed within the neointima. Magnification, 45×. (E) Luminal portion of the aorta from a 10-d-old newborn demonstrating the lack of immunoreactivity to TGF-β2. Magnification, 24×.(F) Outer media and adventitia (A) from a 10-d-old aorta depicting the lack of immunoreactivity to TGF-β2 in the vessel wall and vasa vasorum. Magnification, 24×. (G) Four-hour-old ductus arteriosus showing immunostaining of TGF-β2 in the invading vasa vasorum of the muscle media (vec, vasa vasorum endothelial cells; vsm, vasa vasorum SMC). Magnification, 112×.(H) Four-hour-old ductus arteriosus demonstrating the lack of TGF-β2 immunoreactivity in the vasa vasorum of the adventitia(n = nerve). Magnification, 45×. (I) Eight-day-old ductus arteriosus demonstrating intense immunostaining of TGF-β2 in the medial and adventitial vasa vasorum, as well as in the vessel wall. Compare with structures in aorta in F. Magnification, 24×.
In the fetus, the SMC of the medial vasa vasorum show increased staining for TGF-β when compared with the surrounding smooth muscle of the ductus wall; the vasa vasorum that runs through the adventitia of the ductus arteriosus does not stain with antibodies against TGF-β. With advancing postnatal age, TGF-β staining increases in both the vasa vasorum that penetrate into the muscle media and those that course through the adventitia(Fig. 2,G-I). At the same time, there is increased TGF-β immunoreactivity in the vessel wall (Fig. 2I).
The patterns of expression of TGF-β1, TGF-β2, and TGF-β3 follow the same progression throughout ductus closure; TGF-β2 expression, however, appears earlier and with greater intensity than either TGF-β1 or TGF-β3 in the muscle media (Fig. 4).
Immunohistochemical staining for TGF-β was also performed in descending aortas obtained from the same animals. The fetal aorta had the same, minimal amount of TGF-β staining as was found in the in the fetal ductus arteriosus. In contrast to the marked changes in TGF-β expression in the postnatal ductus arteriosus, the expression of TGF-β in the postnatal aorta did not change perceptibly from the pattern seen in the fetus(Fig. 2,E andF).
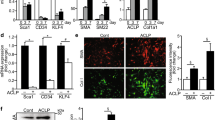
In situ hybridization. The changes that occur in TGF-β mRNA expression (Fig. 5) follow a pattern similar to the changes we observed in TGF-β protein expression (Fig. 4). In general, hybridization with the TGF-β2 riboprobe is more pronounced in the muscle media than hybridization with either the TGF-β1 or TGF-β3 riboprobes at all time points. Similar to protein expression, TGF-β mRNA expression is minimal in the fetal ductus arteriosus (Fig. 3A); TGF-β mRNA increases in the neointima (Fig. 3B) and outer muscle media within the first 24 h after birth, and it continues to increase throughout the first postnatal week (Fig. 3,C andD). There is modest TGF-β mRNA expression in the inner muscle media, which increases slightly during ductus closure. Similarly, TGF-β is only modestly expressed in cells of the adventitia, and expression remains at low levels throughout the 1st wk of life. In contrast to the increased presence of TGF-β protein, TGF-β mRNA is not observed in the muscle layers of the medial and adventitial vasa vasorum (Fig. 3E). However, TGF-β mRNA can occasionally be seen in endothelial cells of the vasa vasorum with advancing postnatal age (Fig. 3E).
Summary of mRNA expression of TGF-β isoforms(represented by β1, β2, and β3) in the closing ductus arteriosus. TGF-β mRNA expression is minimal in the fetal ductus arteriosus. TGF-β mRNA levels increase in the neointima and outer muscle media shortly after birth, and continue to increase throughout the first postnatal week. TGF-β mRNA expression in the inner muscle media and adventitia is modest and does not change significantly throughout ductus closure. There is no TGF-β mRNA expression in the luminal endothelial cells. Unlike TGF-β protein expression, there is no TGF-βmRNA expression in the muscle layers of the vasa vasorum that penetrate either the muscle media or adventitia of the ductus after birth (N/A, not applicable).
In situ hybridization of TGF-β2 in the ductus arteriosus. All three TGF-β mRNAs showed a similar pattern of hybridization. Because there were no differences in the pattern of staining for the three isoforms, only data for TGF-β2 are presented. Ductus arteriosus sections were hybridized with TGF-β2-labeled riboprobe(white dots), counterstained with hematoxylin and eosin, and photographed using darkfield microscopy. (A) Fetal ductus arteriosus viewed using darkfield microscopy showing low level hybridization of TGF-β2 uniformly throughout the ductus wall. Under darkfield microscopy, elastin(internal elastic lamina (arrowheads) and elastin bands in the muscular media (arrows)) appear as broad white bands (L, lumen; M, tunica muscularis). Silver grain counts/1000μm2: vessel media = 20 ± 3.8 (m ± SD); lumen(background) = 4 ± 2. Magnification, 24×. (B) One-day-old ductus arteriosus viewed using darkfield microscopy demonstrating increased mRNA expression of TGF-β2 in the forming neointima(NI). Silver grain counts/1000 μm2: neointima = 47± 2; inner media = 18 ± 3. Magnification, 24×.(C) Eight-day-old ductus arteriosus viewed using darkfield microscopy showing continued increased mRNA expression of TGF-β2 in the neointima. Arrowheads outline the duplicated internal elastic lamina. Silver grain counts/1000 μm2: neointima = 74 ± 7; inner media = 38 ± 4. Magnification, 24×. (D) Necrotic region (CL) and outer muscle media (OM) of an 8-d-old ductus arteriosus viewed using darkfield microscopy. Note the lack of hybridization in the acellular, necrotic region, with enhanced TGF-β2 mRNA expression in the neighboring outer muscle media. Silver grain counts/1000 μm2: acellular region = 11 ± 2; outer media = 67 ± 7. Magnification, 24×. (E) Adventitial vasa vasorum (VV) in an 8-d-old ductus arteriosus viewed using darkfield microscopy. Note the lack of TGF-β2 mRNA expression in the muscle wall (m) of the vasa vasorum (ec, endothelial cells). Magnification, 45×. (F) Eight-day-old ductus arteriosus after hybridization with a sense-oriented TGF-β2 riboprobe (control), viewed using darkfield microscopy. Note the lack of TGF-β2 hybridization using the sense riboprobe (compare withC). Silver grain counts/1000 μm2: neointima = 20 ± 6; inner media = 19 ± 5. Magnification, 24×.
In situ hybridization of descending aortas from the same animals showed a pattern of expression similar to that seen for TGF-β protein(see above). TGF-β mRNA is only minimally expressed in aortas obtained from fetal and neonatal lambs (data not shown).
DISCUSSION
In our study, we found that within hours of delivery, TGF-β expression was markedly increased in the vessel wall of the ductus arteriosus. In contrast to other models of vascular disease(4–6), we noted a similar temporal pattern of appearance of all three isoforms of TGF-β.
In many other injury models, inflammatory cells and platelets contribute significantly to TGF-β production(7). In the closing ductus arteriosus, however, macrophages and polymorphonuclear cells do not invade the muscle media or the neointima. Platelets (a principal source of exogenous TGF-β) occasionally can be seen adhering to the luminal endothelial cells of the ductus within the first 24 h after delivery. Thrombi also may be seen in the lumen around the third postnatal day (our unpublished observations). It is unlikely, however, that these cells are responsible for the increased expression of TGF-β found in the closing ductus arteriosus because their presence is infrequent and sporadic. In our study, the proteins and mRNAs of the three TGF-β isoforms co-localized predominantly in the cells of the neointima and outer muscle media. During ductus closure, proliferating endothelial cells originating from the lining of the vessel's lumen invade the neointima, which is composed primarily of SMC. Additionally, endothelial cells from the adventitial vasa vasorum invade the outer muscle media as new vasa vasorum. These findings suggest that SMC, and perhaps invading endothelial cells, are the principal source(s) of TGF-β in the closing ductus arteriosus. Previous reports have suggested that, in vivo, TGF-β is produced only by SMC and not by quiescent endothelial cells(17, 25). However, proliferating endothelial cells have been reported to produce TGF-β in vitro(26); in addition, endothelial cells have increased immunostaining for the TGF-β isoforms during bovine vessel remodeling(5) and during epidermal wound-induced angiogenesis(27). Therefore, endothelial cells may be responsible for a fraction of the increased TGF-β observed in the neointima and outer muscle media of the closing ductus arteriosus.
We also found a marked increase in immunoreactive TGF-β in the SMC layer of the vasa vasorum that course through the adventitia of the ductus after birth; this occurred without an apparent increase in TGF-β mRNA. Translational control of TGF-β production could account for this discrepancy between mRNA abundance and protein production(28, 29). The abundance of TGF-β mRNA also may have been below the level of detection for our hybridization assay. Alternatively, changes in the ECM composition of the rapidly proliferating vasa vasorum could alter the capacity of the vasa vasorum to bind TGF-β. The ECM acts as a repository for TGF-β proteins; therefore, TGF-β could accumulate in the ECM that surrounds the SMC.
The factors that initiate TGF-β release are currently unknown. Loss of luminal blood flow and tissue ischemia seem to be crucial factors in initiating reorganization of the ductus arteriosus after birth. Hypoxia and ischemia, which stimulate TGF-β synthesis, also may be principal factors in the induction of TGF-β in the ductus(8, 9). After the initial burst in TGF-β synthesis, continued TGF-β production may occur via autoinduction(30, 31).
TGF-β is secreted from cells in a latent form that is inactive. The antibodies used in our study do not distinguish between active TGF-β and the latent peptide. Therefore, the presence of TGF-β protein in the ductus arteriosus does not necessarily correlate with TGF-β activity. Latent TGF-β can be activated by treatment with acid(32). Similarly, co-culture of endothelial and SMC results in TGF-β activation via the activation of proteases like plasmin(33). In the neointima of the closing ductus arteriosus, latent TGF-β may be activated by the coexistence of invading endothelial cells and migrating SMC. In the muscle media, latent TGF-β may be activated by the release of proteases from the ischemic region of the muscle wall.
TGF-β may play numerous roles in the process of ductus closure. TGF-β appears to have a unique effect on ductus arteriosus SMC studiedin vitro(34). TGF-β increases the anchoring of ductus SMC to the ECM(34). By increasing SMC adhesiveness to the surrounding ECM, TGF-β may help to maintain the tension necessary to sustain ductal contracture during remodeling. At the same time, TGF-β may also stimulate the release of PDGF and endothelin (potent vasoconstrictors)(35, 36) to aid in maintaining ductus arteriosus constriction after birth. TGF-β also enhances matrix production during vascular remodeling(4, 37); TGF-β stimulates fibronectin production and matrix remodeling when added to ductus arteriosus SMC in culture(34). Although TGF-β acts as a chemoattractant for SMC isolated from the aorta(11), it has no such effect on SMC of the ductus arteriosus(34). Instead, TGF-β appears to promote SMC migration toward another growth factor, PDGF, by increasing the synthesis of PDGF-β receptors in the ductus SMC (our unpublished observations). Consequently, TGF-β may play a role in neointimal thickening by increasing the accumulation of ECM and stimulating the chemotaxis of SMC toward the PDGF gradient created by luminal platelets and neointimal cells(our unpublished observations).
Closure of the ductus arteriosus is also associated with the appearance of new vessels (vasa vasorum) in the muscle media and adventitia(Fig. 1F)(24). TGF-β may play an indirect role in new vessel formation by stimulating the release of potent angiogenic factors like basic fibroblast growth factor(36) and vascular endothelial growth factor(38).
The results of this study and our previous study(34) support a role for TGF-β in the vascular remodeling of the full-term ductus arteriosus after birth. We hypothesize that in the preterm infant, persistent patency of the ductus arteriosus may be due to a failure of TGF-β induction after delivery. Further studies will address this issue.
Abbreviations
- cDNA:
-
complimentary DNA
- ECM:
-
extracellular matrix
- PDGF:
-
platelet-derived growth factor
- SMC:
-
smooth muscle cell
- SSC:
-
sodium chloride, sodium citrate
- TGF-β:
-
transforming growth factor-β
References
Clyman R, Mauray F, Roman C, Heyman M, Payne B 1983 Factors determining the loss of ductus arteriosus responsiveness to prostaglandin E2 . Circulation 68: 433–436.
Weiss H, Cooper B, Brook M, Schlueter M, Clyman R Factors determining ductus arteriosus reopening after successful closure with indomethacin. J Pediatr (in press)
Ruffle T, Olsen E, Graven S, Zachman R 1975 Oxygen consumption in the fetal rabbit ductus arteriosus. Proc Soc Exp Biol Med 148: 593–595.
Majesky M, Lindner V, Twardzik D, Schwartz S, Reidy M 1991 Production of transforming growth factor-β1 during repair of arterial injury. J Clin Invest 88: 904–910.
Botney M, Bahadori L, Gold L 1994 Vascular remodeling in primary pulmonary hypertension; potential role for transforming growth factor-β. Am J Pathol 144: 286–295.
Perkett E, Pelton R, Meyrick B, Gold L, Miller D 1994 Expression of transforming growth factor- mRNAs and proteins in pulmonary vascular remodeling in the sheep air embolization model of pulmonary hypertension. Am J Respir Cell Mol Biol 11: 16–24.
Ross R 1993 The pathogenesis of atherosclerosis: a perspective for the 1990s. Nature 362: 801–809.
Falanga V, Quian S, Danielpour D, Katz M, Roberts A, Sporn M 1991 Hypoxia upregulates the synthesis of TGF-β1 by human dermal fibroblasts. J Invest Dermatol 97: 634–637.
Klempt N, Sirimanne E, Gunn A, Klempt M, Singh K, Williams C, Gluckman P 1992 Hypoxia-ischemia induces transforming growth factor-β1 mRNA in the infant rat brain. Brain Res Mol Brain Res 13: 93–101.
Massague J 1987 The TGF- family of growth and differentiation factors. Cell 49: 437–438.
Koyama N, Koshikawa T, Morisaki N, Naito Y, Yoshida S 1990 Bifunctional effects of transforming growth factor- on migration of cultured rat aortic smooth muscle cells. Biochem Biophys Res Commun 169: 725–729.
Ignotz R, Massague J 1986 Transforming growth factor- stimulates the expression of fibronectin and collagen and their incorporation into the extracellular matrix. J Biol Chem 261: 4337–4345.
Basson C, Kocher O, Basson M, Asis A, Madri J 1992 Differential modulation of vascular cell integrin and extracellular matrix expression in vitro by TGF-β1 correlates with reciprocal effects on cell migration. J Cell Physiol 153: 118–128.
Burmester J, Qian S, Roberts A, Huang A, Amatayakul-Chantler S, Suardet L, Odartchenko M, Madri J, Sporn M 1993 Characterization of distinct functional domains of transforming growth factor. Proc Natl Acad Sci USA 90: 8628–8632.
Massaque J 1992 Receptors for the TGF- family. Cell 69: 1067–1070.
Pelton R, Saxena B, Jones M, Moses H, Gold L 1991 Immunohistochemical localization of TGF-β1, TGF-β2 and TGF-β2 in the mouse embryo: expression patterns suggest multiple roles during embryonic development. J Cell Biol 115: 1091–1105.
Pelton R, Johnson M, Perkett E, Gold L, Moses H 1991 Expression of transforming growth factor-β1, β2, andβ3 mRNA and protein in the murine lung. Am J Respir Cell Biol 5: 522–530.
Derynck R, Jarrett J, Chen E, Goeddel D 1986 The murine transforming growth factor- precursor. J Biol Chem 261: 4377–4379.
Miller D, Lee A, Matsui Y, Chen E, Moses H, Derynck R 1989 Complementary DNA cloning of the murine transforming growth factor-β3 (TGF-β3) precursor and the comparative expression of TGF-β3 and TGF-β1 messenger RNA in murine embryos and adult tissue. Mol Endocrinol 3: 1926–1934.
Miller D, Lee A, Pelton R, Chen E, Moses H, Derynck R 1989 Murine transforming growth factor-β2 cDNA sequence and expression in adult tissues and embryos. Mol Endocrinol 3: 1108–1114.
Broccoli F, Carinci P 1973 Histological and histochemical analysis of the obliteration processes of ductus arteriosus Botalli. Acta Anat 85: 69–83.
Gittenberger-de-Groot AC 1977 Persistent ductus arteriosus: most probably a primary congenital malformation. Br Heart J 39: 610–618.
Yoder MJ, Baumann FG, Grover-Johnson NM, Brick I, Imparato AM 1978 A morphological study of early cellular changes in the closure of the rabbit ductus arteriosus. Anat Rec 192: 19–39.
Clarke JA 1965 An x-ray microscopic study of the vasa vasorum of the human ductus arteriosus. J Anat 99: 527–537.
Sarzani R, Brecher P, Chobanian A 1989 Growth factor expression in aorta of normotensive and hypertensive rats. J Clin Invest 83: 1404–1408.
Hannan R, Kourembanas S, Flanders K, Rogelj S, Roberts A, Faller D, Klagsbrun M 1988 Endothelial cells synthesize basic fibroblast growth factor and transforming growth factor-. Growth Factors 1: 7–17.
McMullen H, Longaker M, Cabrera R, Sung J, Canete J, Siebert J, Lorenz H, Gold L Spacial and temporal expression of TGF-β isoforms (TGF-β1, TGF-β2, TGF-β3) during ovine excisional and incisional wound repair. Wound Repair and Regeneration(in press)
Kim S, Park K, Koeller D, Kim K, Wakefield L, Sporn M, Roberts A 1992 Post-transcriptional regulation of the human transforming growth factor-β1 gene. J Biol Chem 267: 13702–13707.
Scotto L, Assoian R 1993 A GC-rich domain with bifunctional effects on mRNA and protein levels: implications for control of transforming growth factor-β1 expression. Mol Cell Biol 13: 3588–3597.
Van Obberghen-Schilling E, Roche N, Flanders K, Sporn M, Roberts A 1988 Transforming growth factor-β1 positively regulates its own expression in normal and transformed cells. J Biol Chem 263: 7741–7746.
Kim S, Angel P, Lafyatis R, Hattori K, Kim K, Sporn M, Karin M, Roberts A 1990 Autoinduction of transforming growth factor-β1 is mediated by the AP-1 complex. Mol Cell Biol 10: 1492–1497.
Sporn M, Roberts A, Wakefield L, Assolian R 1986 Transforming growth factor-β: biological function and chemical structure. Science 233: 532–534.
Flaumenhaft R, Abe M, Sato Y, Miyazono K, Harpel J, Heldin C, Rifkin D 1993 Role of the latent TGF- binding protein in the activation of latent TGF- by co-cultures of endothelial and smooth muscle cells. J Cell Biol 120: 995–1002.
Tannenbaum JE, Waleh N, Mauray F, Breuss J, Pytela R, Kramer R, Clyman RI 1995 Transforming growth factor-β1 inhibits fetal ductus arteriosus smooth muscle cell migration. Pediatr Res 37: 561–570.
Kurihara H, Yoshizumi M, Sugiyama T, Takaku F, Yanagisawa M, Masaki T, Hamaoki M, Kato H, Yazaki Y 1989 Transforming growth factor-β stimulates the expression of endothelin mRNA by vascular endothelial cells. Biochem Biophys Res Commun 159: 1435–1440.
Majack R, Majesky M, Goodman L 1990 Role of PDGF-A expression in the control of vascular smooth muscle cell growth by transforming growth factor-β. J Cell Biol 111: 239–247.
Roberts A, Sporn M, Assoain R, Smith J, Roche N, Wakefield L, Heine U, Liotta L, Falanga V, Kehrl J, Fauci A 1986 Transforming growth factor type beta: rapid induction of fibrosis and angiogenesis in vivo and stimulation of collagen formation in vitro. Proc Natl Acad Sci USA 83: 4167–4171.
Risau W 1990 Angiogenic growth factors. Prog Growth Factor Res 2: 71–79.
Acknowledgements
We wish to thank Mr. Paul Sagan for his skillful help in the preparation of this manuscript.
Author information
Authors and Affiliations
Additional information
This work was supported by a grant from the U.S. Public Health Service, National Heart, Lung and Blood Institute HL46691 and by a gift from the Perinatal Associates Research Foundation.
Rights and permissions
About this article
Cite this article
Tannenbaum, J., Waleh, N., Mauray, F. et al. Transforming Growth Factor-β Protein and Messenger RNA Expression Is Increased in the Closing Ductus Arteriosus. Pediatr Res 39, 427–434 (1996). https://doi.org/10.1203/00006450-199603000-00009
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199603000-00009