Abstract
The quality of serum LH was assessed during pubertal maturation in boys by measuring immunoreactive (I) LH by a time-resolved immunofluorometric assay(IFMA, Delfia), and bioactive (B) LH by a sensitized in vitro bioassay. Seven samples were collected at 3-mo intervals from 14 healthy boys(median starting age 11.8 y) during pubertal maturation from Tanner stage I-III or II-IV (n = 7 for each). The mouse Leydig cell in vitro bioassay was sensitized 10-fold, to 0.05-0.1 IU/L, by including 1.5μmol/L of forskolin in the incubation medium. The I- and B-LH levels showed good linear correlation throughout the concentration range analyzed. Mean I-LH increased between the pubertal stages I-IV from 0.42 to 2.24 IU/L and that of B-LH from 1.35 to 5.04 IU/L. No concomitant change occurred in the B-LH/I-LH(B/I) ratio, which was 2.84 ± 0.54 in stage I and 2.58 ± 0.48 in stage IV (mean ± SEM, n = 7). Although the B/I ratios of LH varied from 0.59 to 5.85 in the samples analyzed, the intraindividual variation was small (mean coefficient of variance, 22%). In conclusion, IFMA and sensitized in vitro bioassay showed in healthy boys a similar 4-5-fold increase in the mean LH concentration during pubertal maturation, with no concomitant change in the B/I ratio. The sensitized in vitro bioassay of LH is useful for analysis of the low peripubertal LH levels. The good correlation between the I-LH and B-LH levels, and the lack of change in LH B/I ratio, indicate that IFMA correctly estimates the LH levels upon evaluation of pubertal maturation.
Similar content being viewed by others
Main
Numerous studies report on qualitative changes of LH in various physiologic and clinical conditions, as reflected by alterations in the ratio of biologic to immunologic activity of the hormone, i.e. its B/I ratio (for reviews, seeRefs. 1–3). However, the biochemical features of the LH molecules, responsible for such changes, have largely remained unidentified. With the advent of immunometric assays with improved sensitivity it has become apparent that many, although not all, of the previous findings on changes of the B/I ratio of LH have been due to a bias introduced by the conventional RIA methods, which overestimate low hormone concentrations(4–6). Therefore, the B/I ratios of LH at low hormone levels are erroneously low, and whenever there is an increase in LH concentrations, a greater fold-increase occurs in B-LH, resulting in artifactual elevation of the B/I ratio. We have earlier demonstrated the existence of this type of bias in the B/I ratios estimated during the pulsatile LH secretion, after gonadotropin-releasing hormone stimulation and during treatment with its agonists(5, 6). One of the earlier findings which needs reevaluation is the increase of the B/I ratio of LH during pubertal maturation(7–13). Because this finding is now widely cited in textbooks on endocrinology, it is important to test whether it can be verified by using the recent assay methods with improved sensitivity and specificity. In addition, we report here that in agreement with Debertin and Pomerantz(13), forskolin in a carefully selected concentration increases the sensitivity of mouse Leydig cells to LH stimulation, and it can be used to increase the sensitivity of thein vitro bioassay of human serum LH.
METHODS
Subjects. Fourteen healthy boys entering puberty were studied. Their ages at the beginning of the study ranged from 11 y, 5 mo, to 12 y(median, 11.8 y). The boys were examined every 3 mo for the stage of puberty[according to Marshall and Tanner(14)] for a total time of 18 mo. A peripheral blood sample was taken for hormone measurements at each visit. Seven of the boys were in pubertal stages G1 and 7 in stage G2 at the time of the first visit, and at the time of the last visit, the boys had advanced two stages, half of them being in stages G3 and G4. Duration of each pubertal stage was correlated and compared with the longitudinal standards af pubertal development(14). All subjects had pubertal progression within normal limits. Some data on the physical and endocrine maturation of the subjects during the course of the study are presented inTable 1. Testicular volume of 2 cm3 was considered the limit of stages G1 and G2. The length and width of each testis was measured for mean testis volume(15). The study was approved by the Ethical Committee of The Children's Hospital, University of Helsinki.
Hormone measurements. I-LH was measured using an IFMA (LH spec, Delfia, Wallac OY, Turku, Finland). The assay has a sensitivity of 0.04 IU/L, and intraassay CV of 5.4% at normal LH level (1-5 IU/L). All samples were analyzed in the same assay run.
B-LH was measured by the mouse interstitial cell in vitro bioassay, essentially as described by us before(16, 17), with the following modifications. LH-free serum from healthy men treated with testosterone enanthate (200 mg/wk, intramuscularly)(18) for contraception was used to equalize the serum content of all standard and unknown bioassay samples. The LH-free serum had unmeasurable (<0.04 IU/L) level of LH as assayed by IFMA. The sensitivity of the assay was improved, as demonstrated recently by Debertin and Pomerantz(13), by inclusion of 1.5 μmol/L forskolin in the incubation medium. This increased the sensitivity of the assay about 10-fold, when the dose response curves of incubations in the presence and absence of forskolin were compared (see Fig. 1). The interassay CV of the improved bioassay was 20.2% and that of intraassay 9.1% at normal LH levels (1-5 IU/L). The sensitivity of the individual assays ranged from 0.005 to 0.01 mIU/tube (0.05 to 0.1 IU/L), which is 5-10-fold higher than the sensitivity of the LH in vitro bioassay in the absence of forskolin(16). Upon setting up the sensitized in vitro bioassay, multiple dilutions of unknown serum samples were assayed, and they displayed parallelism of testosterone responses with those of the LH standards. Therefore, when the study material was analyzed, duplicate serum samples at two dilutions ranging from 1:2 to 1:10 were assayed. Hence, the amount of serum per incubation tube ranged from 5 to 25%. The dilutions were selected according to the expected concentration (on the basis of IFMA). If parallelism of the unknown serum dilutions did not occur with the standards, the sample was reassayed.
The same standard, WHO 2nd International standard 80/552 was used in both assays, and the LH concentrations were expressed as international units per liter (IU/L).
The serum levels (in Table 1) of FSH were measured by an immunofluorometric assay kit (Delfia, Wallac OY), and those of testosterone using a RIA after chromatographic separation(19).
Statistical analyses. The data are expressed as mean ± SEM. The statistical analysis was performed using one-way analysis of variance, followed by Duncan's new multiple range test to identify the groups differing. A p value less than 0.05 was considered statistically significant.
RESULTS AND DISCUSSION
The effect of forskolin on sensitivity of the in vitro bioassay is demonstrated in Fig. 1. Inclusion of a 1.5 μmol/L concentration of forskolin in the incubations increased the sensitivity of the assay about 10-fold, in the presence of 10% serum to 0.005 mIU/assay tube (or 0.05 IU/L). It is also seen that increasing the percentage of serum in the bioassay tubes decreased the sensitivity. This is due to as yet unidentified inhibitory factors in the peripheral serum(16). We find it therefore important to include the same amount of serum in each assay tube, including the standards. This is achieved by equalizing the serum content of all standard and unknown samples with LH-free human male serum(16). In this way the dose response curves of standards and serum samples at different dilutions are parallel. The net effect of forskolin on the sensitivity is thus about 10-fold when standard curves containing the same amounts of serum are compared. The increased sensitivity by forskolin increased the variability of the assay. The intra- and interassay CV values (9 and 20%, respectively) are still tolerable, although 2-fold higher than in assays performed without forskolin(16). The increased sensitivity of this assay is an asset which is not offered by the other recent developments in in vitro bioassays of LH, using either Leydig tumor cells(20) or cell lines expressing recombinant LH receptor(21).
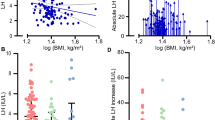
We also paid special attention to evaluating the linearity of the B-LH and I-LH responses (Fig. 2). When the B-LH and I-LH levels of all samples analyzed were correlated, the coefficient was moderate(r = 0.72). However, when we took into account the fact that there was considerable interindividual variation in the B/I ratios of LH (see below), and grouped the subjects according to their average B/I ratio (<2, 2-3.4, and >3.5), good correlation coefficients (r = 0.90-0.95) were found between the two measurements (Fig. 2). The correlation was linear, and neither of the assays appeared to over- or underestimate the low hormone concentrations, i.e. the regression lines crossed the axes at or near the origin. Hence, the B/I ratio measurements are not influenced by bias in the absolute LH levels, which are lowest in the early stages of puberty. We have previously shown that the lack of such linear correlation throughout the concentration range of LH measured results in biased B/I ratio measurements(5, 22).
Correlation between the B-LH and I-LH concentrations measured in the serum samples of 14 peripubertal boys (n = 98). All results are presented in panel A (r = 0.72). Inpanels B-D, the observations are grouped according to the mean B/I ratio of each subject. Those with B/I ratio < 2 are in panel B(r = 0.92), those between 2 and 3.5 in panel C(r = 0.95), and those above 3.5 in panel D (r = 0.90). All correlations were significant at the p level < 0.001.
The mean levels of B-LH, I-LH, and the B/I ratios at the different stages of puberty are presented in Fig. 3. I-LH increased between pubertal stages I and IV from 0.42 ± 0.13 to 2.24 ± 0.34 IU/L (p < 0.01) and B-LH from 1.35 ± 0.49 to 5.04 ± 0.78 IU/L (p < 0.01), but no concomitant changes occurred in the mean B/I ratios of LH (2.58-2.84). The same was apparent when data on the individual subjects are inspected (Fig. 4). Although the B/I ratio of the individual samples varied between 0.6 and 5.9, the variation of this parameter within the samples of one subject was rather small. The CV percentages ranged between 9 and 40, with the mean for the whole group of 14 subjects being 22%. The large interindividual variation in the B/I ratios of LH has been suggested to be due to individual differences in the composition of LH isoforms with differing carbohydrate moieties and intrinsic bioactivities(1–3), but it is also possible that there are substances in the peripheral serum that modify the activity of LH molecules at the receptor site [for references, see Huhtaniemi(23)]. Although we measured the LH levels in single serum samples, we trust that they reflect reliably the overall B/I ratio of LH in the subjects. We have previously shown that, using our assay methods, the B/I ratio of LH does not change during the LH secretion pulses(6).
The mean (± SEM) levels of B-LH (top panel), I-LH (middle panel), and the B/I ratios (bottom panel) of the 14 peripubertal boys studied according to their stage of puberty (I-IV). The number of subjects analyzed at each pubertal stage is presented in brackets at the bottom of bars of the bottom panel. When different letters are above the bars these results differ significantly from each other (p < at least 0.05).
The B/I ratios of LH in the individual serum samples of the 14 peripubertal boys with advancing chronologic age, indicating a large interindividual, but small intraindividual, variation of the ratio. The lines connect the samples of each individual. The numbers in the lines indicate the pubertal stage at the individual sampling times as follows: 1-1, stage I; 2-2, stage II; 3-3, stage III; 4-4, stage IV.
The increase in I-LH between stages I and IV was 5-fold(Fig. 3). It was somewhat less that the over 10-fold increase between stages I and IV that was recently demonstrated by Garibaldiet al.(24) using a sensitive immunoradiometric assay. This is explained by the fact that our subjects were at the late phase of pubertal stage I, because truly prepubertal boys have LH levels below 0.3 IU/L when monitored by IFMA(25, 26). The concomitant increase in LH between stage I and IV is only 2-3-fold when measured using conventional RIA(8–10, 12, 24). We have considered this previously the main reason why the B/I ratios tend to increase when the absolute LH levels increase, as monitored by RIA. However, we also identified another difference. The B-LH increase was in our measurements 4-fold, whereas the three earlier studies on LH bioactivity during pubertal maturation demonstrated 8-12-fold increases(8–10, 12). Dissimilar assay sensitivities are the most likely reasons for the difference. Our assay had a sensitivity below 0.1 IU/L, whereas that of the previous studies was 0.5 IU/L(12) or over 1 IU/L(8–10). The low levels are therefore subject to greater error in the previous studies. Another clear difference is the greater increase of B-LH in the earlier studies beyond pubertal stage I. The different standards used, different approaches to eliminate the confounding effects of the serum matrix, different species of interstitial cells (mouse or rat), and their preparations may be additional confounding factors. Many of the LH bioactivity measurements in pubertal children have been carried out using the rat interstitial cell in vitro bioassay(7–9, 11, 12). However, we have previously shown that there is a good correlation between the B-LH levels measured with the rat and mouse bioassays(27).
We paid special attention to testing the linearity of the B- and I-LH responses in our assays (Fig. 2) and found no apparent changes in the B/I ratio of LH during pubertal maturation from pre- to mid- and late stages, where the steepest increase in the ratio has previously been reported(7–11). Therefore, in contrast to earlier reports, we conclude that the pubertal maturation is not contributed to by increased intrinsic bioactivity (i.e. B/I ratio) of LH. Our different finding was obtained using an immunoassay with improved sensitivity and specificity and an in vitro bioassay with improved sensitivity and good correlation with I-LH measurements. In our opinion, the previous contention that the quality of LH changes during pubertal maturation may need reevaluation. The current in vitro bioassays of LH are still suboptimal in sensitivity, precision, and accuracy, and further method development is needed before the overall value of gonadotropin bioactivity/immunoreactivity relationships can be judged. The good correlation between B-LH and I-LH levels in the present measurements, together with the lack of changes in B/I ratios of LH during puberty, indicates that the highly sensitive IFMA of LH gives a correct estimate of LH bioactivity as well, emphasizing the clinical usefulness of this assay for evaluation of the pubertal process.
Abbreviations
- B:
-
bioactive
- CV:
-
coefficient of variation
- I:
-
immunoreactive
- IFMA:
-
immunofluorometric assay
References
Dufau ML, Veldhuis JD 1987 Pathophysiological relationships between the biological and immunological activities of luteinizing hormone. Baillieres Clin Endocrinol Metab 1: 153–176
Beitins IZ, Padmanabhan V 1991 Bioactivity of gonadotropins. Endocrinol Metab Clin North Am 20: 85–120
Tsatsoulis A, Shalet SM, Robertson WR 1991 Bioactive gonadotrophin secretion in man. Clin Endocrinol 35: 193–206
Chappel S 1990 Biological to immunological ratios: reevaluation of a concept. J Clin Endocrinol Metab 70: 1494–1495
Jaakkola T, Ding Y-Q, Kellokumpu-Lehtinen P, Valavaara R, Martikainen H, Tapanainen J, Rönnberg L, Huhtaniemi I 1990 The ratios of serum bioactive/immunoreactive luteinizing hormone and follicle-stimulating hormone in various clinical conditions with increased and decreased gonadotropin secretion: reevaluation by a highly sensitive immunometric assay. J Clin Endocrinol Metab 70: 1496–1505
Huhtaniemi I, Ding Y-Q, Tähtelä R, Välimäki M 1992 The bio/immuno ratio of plasma luteinizing hormone does not change during the endogenous secretion pulse; reanalysis on the concept using improved immunometric techniques. J Clin Endocrinol Metab 75: 1442–1445
Rich BH, Rosenfield RL, Moll GW, Lucky AW, Roche-Bender N, Fang V 1982 Bioactive luteinizing hormone pituitary reserves during normal and abnormal male puberty. J Clin Endocrinol Metab 55: 140–146
Lucky AW, Rich BH, Rosenfield RL, Fang VS, Roche-Bender N 1980 LH bioactivity increases more than immunoreactivity during puberty. J Pediatr 97: 205–213
Reiter EO, Beitins IZ, Ostrea T, Gutai JP 1982 Bioassayable luteinizing hormone during childhood and adolescence and in patients with delayed pubertal development. J Clin Endocrinol Metab 54: 155–161
Dunger DB, Villa AK, Matthews DR, Edge JA, Jones J, Rothwell C, Preece MA, Robertson WR 1991 Pattern of secretion of bioactive and immnoreactive gonadotrophins in normal pubertal children. Clin Endocrinol 35: 267–275
Kasa-Vubu JZ, Padmanabhan V, Kletter GB, Brown MB, Reiter EO, Sizonenko PC, Beitins IZ 1993 Serum bioactive luteinizing and follicle-stimulating hormone concentrations in girls increase during puberty. Pediatr Res 34: 829–833
Kletter GB, Padmanabhan V, Brown MB, Reiter EO, Sizonenko PC, Beitins IZ 1993 Serum bioactive gonadotropins during male puberty: a longitudinal study. J Clin Endocrinol Metab 76: 432–438
Debertin WJ, Pomerantz DK 1992 Improved sensitivity of the mouse interstitial cell testosterone assay with the addition of forskolin. Can J Physiol Pharmacol 70: 866–871
Marshall WA, Tanner JM 1970 Variations in the pattern of pubertal changes in boys. Arch Dis Child 45: 13–23
Hansen P 1952 Clinical measurements of the testis in boys and men. Acta Med Scand 142( suppl 266): 457–465
Ding Y-Q, Huhtaniemi I 1989 Human serum LH inhibitor(s): behavior and contribution to in vitro bioassay of LH using dispersed mouse Leydig cells. Acta Endocrinol 121: 46–54
Haavisto A-M, Pettersson K, Bergendahl M, Virkamäki A, Huhtaniemi I 1995 Occurrence and biological properties of a common genetic variant of luteinizing hormone. J Clin Endocrinol Metab 80: 1257–1263
Apter D, Jänne O, Karvonen P, Vihko R 1976 Simultaneous determination of five sex hormones in human serum by radioimmunoassay after chromatography on Lipidex-5000. Clin Chem 22: 32–38
WHO Task Force on Methods for the Regulation of Male Fertility 1990 Contraceptive efficacy of testosterone induced azoospermia in normal men. Lancet 336: 955–959
Dahl KD, Sarkissian A 1993 Validation of an improvedin vitro bioassay to measure LH in diverse species. J Androl 14: 124–129
Jia X-C, Perlas E, Su J-GJ, Moran F, Lasley BL, Ny T, Hsueh AJW 1993 Luminescence luteinizing hormone/choriogonadotropin (LH/CG) bioassay: measurement of serum bioactive LH/CG during early pregnancy in human and macaque. Biol Reprod 49: 1310–1316
Huhtaniemi I, Venho P, Jacobi G, Rannikko S 1991 Response of circulating gonadotropin levels to GnRH agonist treatment in prostatic cancer. J Androl 12: 46–53
Huhtaniemi I 1993 Hormonal control mechanisms of Leydig cells. In: De Kretser D (ed) Molecular Biology of the Male Reproductive System. Academic Press, San Diego, pp 383–410
Garibaldi LR, Picco P, Magier S, Chevli R, Aceto T Jr 1991 Serum luteinizing hormone concentrations, as measured by a sensitive immunoradiometric assay, in children with normal, precocious or delayed pubertal development. J Clin Endocrinol Metab 72: 888–898
Haavisto A-M, Dunkel L, Pettersson K, Huhtaniemi I 1990 LH measurements by in vitro bioassay and a highly sensitive immunofluorometric assay improve the distinction between boys with constitutional delay of puberty and hypogonadotropic hypogonadism. Pediatr Res 27: 211–214
Dunkel L, Alfthan H, Stenman U-H, Selstam G, Rosberg S, Albertsson-Wikland K 1992 Developmental changes in 24-hour profiles of luteinizing hormone and follicle-stimulating hormone from prepuberty to midstages of puberty in boys. J Clin Endocrinol Metab 74: 890–897
Ding Y-Q, Ranta T, Nikkanen V, Huhtaniemi I 1991 Discordant levels of serum bioactive LH in man as measured in different in-vitro bioassay systems using rat and mouse interstitial cells and human granulosa-luteal cells. J Endocrinol 128: 131–137
Acknowledgements
The skillful technical assistance of Tarja Laiho is gratefully acknowledged.
Author information
Authors and Affiliations
Additional information
Supported by grants from the Academy of Finland, the Turku University Foundation, and the Ahokas Foundation.
Rights and permissions
About this article
Cite this article
Huhtaniemi, I., Haavisto, AM., Anttila, R. et al. Sensitive Immunoassay and in Vitro Bioassay Demonstrate Constant Bioactive/Immunoreactive Ratio of Luteinizing Hormone in Healthy Boys during the Pubertal Maturation. Pediatr Res 39, 180–184 (1996). https://doi.org/10.1203/00006450-199601000-00030
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199601000-00030