Abstract
To determine the effects of chronic maternal undernutrition on postnatal somatic growth and blood pressure, pregnant dams were randomly assigned to one of two dietary treatment groups. A control group was fed ad libitum throughout pregnancy and a restricted group was fed 30% of ad libitum intake. From birth, feeding was ad libitum in both groups, and litter size was adjusted to eight pups per litter. Litter size was not significantly altered by the reduced maternal intake. Offspring of the restricted fed group were significantly smaller than offspring from the ad libitum fed group from birth until 12 wk of age, but by 30 wk had similar body weights. Blood pressure was measured by tail cuff plethysmography. Offspring from the restricted fed group were found to have significantly (p < 0.05) elevated systolic blood pressure (5-8 mm Hg) at 30, 48, and 56 wk of age. These data demonstrate that nutritional deprivation in the pregnant rat leads to changes in postnatal allometric growth patterns, to delayed catch-up growth, and to elevated blood pressure in adulthood. The data are consistent with the hypothesis that poor maternal nutrition in pregnancy may irreversibly alter programming of the development of cardiovascular homeostasis.
Similar content being viewed by others
Main
Epidemiologic studies have provided evidence that certain major adult noncommunicable diseases may have their origins in fetal life through exposure to an adverse intrauterine environment. A number of studies have shown associations between low birth weight and increased risk of developing hypertension(1–4), noninsulin-dependent diabetes(1, 5), and ischemic heart disease(6). Barker et al.(1) proposed that these apparent associations are a consequence of adverse periconceptual or intrauterine influences, which can alter fetal growth and determine the “programming” of the developing cardiovascular and endocrine/metabolic control systems. Thus a suboptimum intrauterine environment might lead to both an abnormal birth size phenotype and to altered cardiovascular and/or metabolic homeostasis. In further reports, inadequate maternal nutrition, in particular, has been implicated as an important determinant of the risk for the subsequent development of hypertension in the offspring(7, 8).
Supplies of nutrients and oxygen are known to be major determinants of fetal growth(9, 10). Chronic maternal undernutrition during pregnancy leads to reduced birth weight in many mammalian species(11, 12). Recently, it has been suggested that the impact of altered nutrient availability varies at different stages of gestation, and both the timing and degree of undernutrition are important in determining how fetal growth is affected(13). Maternal dietary restriction has been associated with altered placental and fetal growth and composition(14–16). Moreover, dietary supplementation in late gestation human pregnancy can enhance postnatal growth(17).
At present, the physiologic basis for the observed association between low birth weight and increased risk of developing hypertension in adulthood is unknown. Because none of the human studies which relate birth weight to adult blood pressure has actually measured nutritional intake in mothers or babies, their nutritional status has been inferred only indirectly from measurements of birth weight. In animals, experimental evidence linking prenatal events to postnatal cardiovascular sequelae is limited and has been confined to observations made during puberty or young adulthood. In guinea pigs, induction of IUGR by maternal uterine artery ligation led to raised blood pressures in the offspring at 3-4 mo of age(18). Elevated systolic blood pressures were also observed in the adolescent and young adult offspring of rats exposed to a protein-deficient diet shortly before and during pregnancy(19).
We have recently developed a model in the rat of IUGR by restricting maternal food intake throughout gestation. Reductions of 20-30% in fetal and placental weights were noted during the final third of gestation when maternal dietary intake was restricted to 30% of ad libitum fed controls(20). The present study was designed to determine whether such restriction of maternal nutrition throughout gestation affects blood pressure in the offspring during mid to late adult life. We observed significantly higher systolic blood pressures measured from 30 to 56 wk of age in the offspring of nutritionally restricted dams. The study thus provides evidence to support the proposal that maternal undernutrition during pregnancy is associated with raised blood pressure in the adult offspring.
METHODS
Animals and study design. Timed matings were performed in Wistar rats (age range 70-100 d) using a rat estrus cycle monitor (Fine Science Tools Inc., North Vancouver, BC, Canada) to assess the stage of estrus of the animals, before introducing the males. Day 1 of pregnancy was determined by the presence of spermatozoa after a vaginal smear. After confirmation that mating had occurred, the animals were housed individually in standard rat cages containing wood shavings as bedding with free access to water. The room was maintained at a constant temperature (25 °C) and with a 12-h light-dark cycle.
Dams were randomly assigned to one of two dietary treatment groups. A control group was fed ad libitum (diet 86: protein 18%, fat 4%, fiber 3%, ash 7%, carbohydrates 58%, Skellerup Stock Foods, Auckland, New Zealand) throughout pregnancy, and a restricted group was fed 30% of the ad libitum intake, determined by the amount of food consumed by the control group on the previous day from d 1 of pregnancy until parturition (23 d). The degree of food restriction had been determined in a pilot study. Fetal and placental weights were determined by sacrificing subgroups of pregnant dams after 22 d of gestation.
At parturition, feeding was ad libitum in both groups, and litter size was adjusted to eight pups per litter. The pups were weaned at 3 wk of age on to rat chow (diet 86, Skellerup Stock Foods, Auckland, NZ)) and were housed in either pairs (males) or triplets (females). Animals were weighed weekly from weaning until 90 d of age and monthly thereafter. All adult offspring were killed at 62 wk of age by decapitation under halothane anesthesia. Body weight, body lengths (nose-rump and nose-tail), and tail circumferences were measured. This study was approved by the Animal Ethics Committee of the University of Auckland.
Blood pressure measurements. Systolic blood pressure was measured in a total of 58 conscious male and female offspring from eight litters (four ad libitum and four restricted fed) by using tail cuff plethysmography (blood pressure analyzer IITC, Life Science, Woodland Hills, CA) as previously validated(21). Rats were placed in a clear Perspex restraint tube, maintained in a darkened room at 28-29 °C. After allowing 15 min for each animal to acclimatize in the tube, a 18- or 11-mm cuff was placed around the tail of male and female rats, respectively, and inflated to 240 mm Hg. Pulses were recorded during deflation at a rate of 3 mm Hg/s. Systolic pressure was recorded as the pressure at the point when the first tail pulse was detected, but it was not possible to obtain reliable measurements of diastolic pressure. Heart rate was calculated as beats/min by counting the number of pulses registering over a 2-s period and multiplying by 30. Training for indirect tail-cuff blood pressure determination began when the rats were 25 wk old, and blood pressure measurements were recorded at 30, 40, 48, and 56 wk of age. Blood pressure was determined in triplicate for each animal, with average systolic pressure and heart rate recorded as the mean of three readings.
Statistical analyses. All analyses were carried out using the Sigma Stat statistical package (Jandel Scientific, San Rafael, CA). A preliminary multivariate analysis showed no litter effect, and differences between groups were evaluated using analysis of variance with age as a repeated measure. When significant differences were found, post hoc comparisons of the means were made using a Bonferroni multiple comparison test. Data are shown as mean ± SEM.
RESULTS
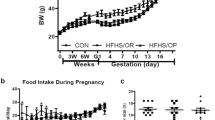
Maternal effects of nutritional restriction during pregnancy. Average daily food intake during pregnancy was 20.7 ± 2.8 g/d in ad libitum controls and 6.2 ± 0.8 g/day in the nutritionally restricted dams. There was a significant (p < 0.05) effect of maternal nutritional restriction on maternal weight gain during pregnancy. Maternal body weight in ad libitum controls increased from 234.6± 3.9 g at mating to 338.7 ± 6.7 g at parturition, but in the restricted dams maternal weight fell from 238.5 ± 3.9 g to 211.0± 4.4 g between conception and d 15 of pregnancy before returning to their premating weight at delivery (227.6 ± 8.72 g).
Nutritional restriction did not affect litter size (ad libitum 11.95 ± 0.75 pups/litter; 30% ad libitum 11.56 ± 0.79 pups/litter). No differences were observed in maternal nursing behavior between the nutritionally restricted and ad libitum mothers, and no pups were eaten by their mothers in either group. However, the mortality rate between birth and weaning was higher among the pups of nutritionally restricted dams. After standardizing all litters at birth to eight pups per litter, four of 32 pups born to nutritionally restricted dams died before weaning, but there were no deaths among the control pups.
Postnatal somatic growth. Maternal undernutrition resulted in IUGR which was reflected by a significant decrease in fetal weight(p < 0.01) and placental weight (p < 0.01) in the restricted fed groups at d 22 of gestation (Table 1). In the offspring from restricted dams, body weights were significantly reduced by 25% at birth (p < 0.05) and by 15% when weaned at 21 d of age(p < 0.05; Table 1). The sex of the pups could not be determined with certainty until they were weaned. The ad libitum control group comprised 18 males and 14 females, compared with 17 males and 11 females in the nutritionally restricted offspring. Body weights recorded at regular intervals from weaning onward are shown in Figure 1. By 8 wk of age, males were significantly heavier than females, a difference which progressively increased with advancing age. For both males and females, pups from ad libitum fed dams were significantly heavier (p < 0.05) than the offspring from restricted fed dams until 12 wk of age. Progeny from the restricted fed group showed catch-up in growth between 12 and 30 wk of age (Fig. 1). When the animals were killed at 62 wk of age, body length (nose-rump and nose-tail) was significantly shorter in the females of both groups compared with the males, but there was no effect of maternal nutritional group on body length in either sex (Table 2). Similarly, heart and kidney weights were both significantly less in females than in males of each group, but maternal nutrition did not have a significant effect (Table 2).
Body weight from 21 until 390 d of age in offspring from ad libitum (n = 4 litters) and 30% ad libitum (n = 4 litters) dams. Ad libitum males(open circles), ad libitum females (open squares), 30% ad libitum males (solid circles), 30%ad libitum females (solid squares). Values are mean± SEM. *p < 0.05 compared with ad libitum offspring from 21 until 90 d of age by analysis of variance followed by a Bonferroni test.
Systolic blood pressure in adult offspring. The first measurements of systolic blood pressure and heart rate were made when the offspring were 30 wk of age (Fig. 2), an age by which body weights were identical in the two groups. Subsequent measurements were made at 40, 48, and 56 wk of age. Tail circumferences were similar between nutritional groups, thus validating comparison by tail cuff methodology(Table 2). No sex differences were observed in blood pressure measurements between males and females in either nutritional group(ad libitum males versus females p < 0.3; 30%ad libitum males versus females p < 0.2).
Systolic blood pressure was significantly (p < 0.05) higher in the offspring of nutritionally restricted dams (119.7 ± 1.32 mm Hg) compared with the offspring of ad libitum fed group (114.1 ± 0.24 mm Hg). Post hoc comparison revealed that systolic pressure was significantly elevated at 30, 48, and 56 wk of age in the nutritionally restricted offspring (Fig. 2), but the difference was not significant at 40 wk of age. In both groups of offspring there was a trend toward a small decrease in systolic pressure with advancing age, but this was not significant. The effect of prior exposure as a fetus to maternal undernutrition was greatest at 48 wk after birth when systolic pressure was 8.1 mm Hg higher in the nutritionally restricted group compared with the control offspring. At 30 wk of age the difference in systolic pressure between the two groups was 6.8 mm Hg, and at 56 wk the difference was 5.0 mm Hg. At 30 wk of age systolic pressure was negatively correlated with birth weight(r = -0.27; p < 0.05), but this association was not significant at older ages.
Heart rate of adult offspring. Heart rates calculated from the pulses detected during blood pressure measurement are shown in Table 3. There was no effect of age on heart rate in either group, but there was a trend toward a higher heart rate in the offspring of nutritionally restricted dams which was significant (p< 0.05) at 48 wk of age.
DISCUSSION
In this study we used chronic maternal undernutrition throughout pregnancy to induce fetal growth retardation in the rat. We demonstrated that low birth weight is associated with raised systolic pressure in adult life. Our measurements were made when the offspring were aged between 30 and 56 wk of age and during the period when body size and weights were similar between nutritionally restricted and control offspring. Given that the average life span of the rat is 18 mo, our blood pressure recordings were made in mid to late adult life. This is an age comparable with human population studies in which blood pressure measured in adults of both sexes aged 46-54 y and 60-71 y was inversely related to birth weight(22). The influence of maternal undernutrition on the blood pressure of the offspring may be apparent at an earlier age, as was reported in female offspring of protein restricted dams at 9 wk of age(19), but was not evaluated in our study.
The degree of fetal growth retardation we observed by restricting maternal diet only during the period of gestation was comparable to that reported with other experimental models of IUGR in the rat(23–25). This level of maternal undernutrition also limited placental growth to a similar degree, with no evidence of any compensatory hypertrophy as suggested in human pregnancies when poor maternal nutrition is associated with iron-deficiency anemia(26). Postnatally, pups from restricted fed dams showed persistent growth failure and remained markedly smaller than the offspring of ad libitum fed dams from birth until 13 wk of age. After weaning, growth rates were similar between the two groups from 21 to 90 d of age but catch-up growth did not occur until between 13 and 30 wk of age.
The persistent elevation of adult blood pressure in the IUGR offspring, together with the failure to show catch-up growth until adult life, both emphasize the profound influence of maternal diet during pregnancy. In contrast to a previous study where maternal protein intake was restricted for 2 wk before conception as well as throughout gestation(19), the aim of the present study was to determine the effect on the offsprings' adult blood pressure of maternal undernutrition during pregnancy alone. Thus the nutritionally restricted dams were allowed ad libitum feeding until there was a positive mating, and the ad libitum diet was provided again immediately after parturition. In the present study we did not cross-foster from nutritionally restricted dams onto ad libitum fed mothers after birth. However, we consider it unlikely that any effects that undernutrition during pregnancy may have on milk supply or composition after birth would contribute significantly to either the observed postnatal growth failure or the elevated blood pressure in late adult life. This is because, first, litter size was reduced immediately after birth to assure that maternal milk supply would not be a limiting factor. Second, we have evidence from an unrelated study that, when nutritionally restricted offspring are cross-fostered at birth onto ad libitum fed mothers, the failure to show any catch-up in growth still occurs (our unpublished observations). This suggests that the postnatal growth failure occurs as a result of maternal undernutrition during pregnancy rather than through any failure in lactation after ad libitum feeding is reestablished. Although we attempted to measure the amount and composition of maternal milk, the data we obtained was inconsistent due to technical difficulties with harvesting procedures.
Our observations provide direct experimental support for the theory, derived from human epidemiologic studies, that adult hypertension may originate during fetal life as a result of exposure to a suboptimal intrauterine environment(27). Population studies have described associations between low birth weight and increased risk of cardiovascular disease including hypertension(2, 28), ischemic heart disease and stroke(6, 29), and syndrome X(30). A further report indicated that placental weight predicts adult hypertension more strongly than reduced birth weight, such that babies born light relative to their placenta are at greatest risk of hypertension(31). Barker(32) has proposed that such associations are evidence that the pathogenesis of cardiovascular disease is “programmed” during critical periods of intrauterine development. Programming is a general process whereby a stimulus or insult at a critical period of development has lasting or lifelong significance(33). The favored hypothesis elaborated by Barker and colleagues in recent years is that it is poor or inadequate maternal nutrition during pregnancy which provides the suboptimal intrauterine environment, or insult, which both impairs fetal growth and alters the programming of fetal cardiovascular and metabolic control systems(1). However, this proposition is based on retrospective epidemiologic observations, and maternal nutritional intake has not actually been measured in any human studies. Even though the 5-8 mm Hg rise in systolic pressure observed in the present study is small in absolute terms, the finding is notable because it provides a clear demonstration that blood pressure can be significantly elevated over a prolonged period from mid to late adult life after fetal exposure to controlled restriction of maternal nutritional intake during pregnancy.
Two previous experimental studies reported that an adverse intrauterine environment leads to raised blood pressure in the offspring, but in both studies, blood pressure was measured only in adolescent or young adult animals. IUGR, induced in guinea pigs by ligation of a uterine artery in midgestation, was associated with an increase in mean blood pressure of 7 mm Hg in those with severe, but not moderate, IUGR(18). The same study also noted an inverse correlation between heart rate and birth weight, and the trend we observed toward higher heart rates in the nutritionally restricted offspring is consistent with this. In rats, graded restriction of maternal protein intake, which was continued from 2 wk before conception until parturition, was associated with raised systolic pressure from 9 to 21 wk of age, but these observations were made only on the female offspring(19) and heart rates were not reported. In that study, systolic pressure at 9 wk of age was inversely related to both maternal protein intake and maternal energy intake. These authors also noted that, in all nutritional groups, blood pressure declined significantly between 9 and 21 wk of age. In the present study, we measured systolic pressures in both male and female offspring, and at later ages, but we observed a similar trend. The reasons for this fall in blood pressure are unclear, because in humans and many other mammals arterial pressure increases progressively with advancing age and increasing weight. In humans, it is also suggested that raised blood pressure initiated in utero is progressively amplified throughout life(22). Despite this, it is notable that in both the present study as well as that of Langley and Jackson(19) systolic pressure continued to be higher in the nutritionally restricted offspring at all ages except at 40 wk. The absence of a difference in blood pressure at this one age is unlikely to be of physiologic significance and may suggest that the age-related decline in blood pressure was slightly delayed in the ad libitum offspring.
The mechanisms by which maternal undernutrition during pregnancy can lead to hypertension in the adult offspring remain to be elucidated. It has been proposed that the changes in the intrauterine environment which alter fetal, and possibly placental, growth may also affect the programming of cardiovascular and metabolic control systems(1). Many hormones important in fetal adaptation to an adverse intrauterine environment have well known pressor effects, for example catecholamines, vasopressin, and angiotensin II. Fluctuations in fetal blood pressure may initiate the pathophysiologic changes which alter the set points of autonomic nervous control of the cardiovascular system. This would be consistent with Folkow's(34) proposal that hypertension develops when an initiating event which raises blood pressure acutely is followed by a continuing amplification process which progressively magnifies the differences long after the initial stimulus has disappeared. There is now also some evidence that exposure of the fetus to excessive glucocorticoid levels may be involved in the reprogramming of cardiovascular control systems. The hypertensive effects of glucocorticoids are well recognized, and exposure of rat fetuses to exogenous glucocorticoids leads to reduced birth weight and subsequent hypertension in the offspring(35). Normally, placental 11β-hydroxysteroid dehydrogenase protects the fetus from the deleterious effects of maternal glucocorticoids by catalyzing the inactivation of cortisol and corticosterone(36). However, a recent report indicates that maternal protein deprivation during pregnancy is associated with reduced placental 11β-hydroxysteroid dehydrogenase activity, and this is suggested as a possible mechanism which could lead to both IUGR and hypertension in the offspring(37).
The observations of Barker and colleagues, although intriguing, have met with some controversy(38). The suggestion that inadequate maternal nutrition during pregnancy is a primary factor in the development of hypertension in the next generation has been criticized because it is based on retrospective epidemiologic studies in which maternal nutrition has never been measured. The present study provides direct experimental support for the hypothesis that maternal malnutrition can alter the development of cardiovascular control in the fetus and thereby lead to raised blood pressure in the adult offspring. This preparation should prove useful in clarifying the role of maternal nutrition in determining the cardiovascular health of subsequent generations.
Abbreviations
- IUGR:
-
intrauterine growth retardation
- IGF:
-
insulin-like growth factor
References
Barker DJP, Gluckman PD, Godfrey KM, Harding JE, Owens JA, Robinson JS 1993 Fetal nutrition and cardiovascular disease in adult life. Lancet 341: 938–941
Gennser G, Rymark P, Isberg PE 1988 Low birth weight and risk of high blood pressure in adulthood. BMJ 296: 1498–1500
Osmond C, Barker DJP, Winter PD, Fall CHD, Simmons SJ 1993 Early growth and death from cardiovascular disease. BMJ 307: 1519–1524
Whincup PH, Cook DG, Shaper AG 1989 Early influences on blood pressure: a study of children aged 5-7 years. BMJ 299: 587–591
Hales CN, Barker DJP, Clark PM, Cox LJ, Fall C, Osmond C, Winter CD 1991 Fetal and infant growth and impaired glucose tolerance at aged 64. BMJ 303: 1019–1022
Barker DJP, Winter PD, Osmond C, Margretts B, Simmonds SJ 1989 Weight in infancy and death from ischemic heart disease. Lancet 11: 577–580
Barker DJP, Fall C 1993 Fetal and infant origins of cardiovascular disease. Arch Dis Child 68: 797–799
Godfrey KM, Forrester T, Barker DJP, Jackson AA, Landman JP, Hall JS, Cox V, Osmond C 1994 Maternal nutritional status during pregnancy and blood pressure in childhood. Br J Obstet Gynaecol 101: 398–403
Owens JA, Owens PC, Robinson JS 1989 Experimental fetal growth retardation: metabolic and endocrine aspects. In: Gluckman PD, Johnston BM, Nathanielsz PW (eds) Advances in Fetal Physiology. Perinatology Press, Ithaca, NY, pp 263–262
Gluckman PD, Breier BH, Oliver MH, Harding JE, Bassett NS 1990 Fetal growth in late gestation: a constrained pattern of growth. Acta Paediatr Scand Suppl 1367: 105–110
Lederman SA, Rosso P 1980 Effects of food restriction of fetal and placental growth and maternal body composition. Growth 44: 77–88
Lechtig A, Yarbrough C, Delgado H, Habicht J-P, Martorell R, Klein RE 1975 Influence of maternal nutrition on birth weight. Am J Clin Nutr 28: 1223–1233
Harding JE, Johnston BM 1995 Nutrition and fetal growth. Reprod Fertil Dev 7: 639–645
Wunderlich SM, Baliga BS, Munro HN 1979 Rat placental protein synthesis and peptide hormone secretion in relation to malnutrition from protein deficiency or alcohol administration. J Nutr 109: 1534–1541
van Marthens E, Shimomaye SY 1978 In utero fetal and placental development following maternal protein repletion in rats. J Nutr 108: 959–966
Anderson GD, Ahokas RA, Lipshitz J, Dilts PV Jr 1980 Effect of maternal dietary restriction during pregnancy on maternal weight gain and fetal birth weight in the rat. J Nutr 110: 883–890
Kusin JA, Kardjati S, Houtkooper JM, Renqvist UH 1992 Energy supplementation during pregnancy and postnatal growth. Lancet 340: 623–626
Persson E, Jansson T 1992 Low birth weight is associated with elevated adult blood pressure in the chronically catheterized guinea-pig. Acta Physiol Scand 145: 195–196
Langley SC, Jackson AA 1994 Increased systolic blood pressure in adult rats induced by fetal exposure to maternal low protein diets. Clin Sci 86: 217–222
Woodall SM, Breier BH, Johnston BM, Gluckman PD 1996 A model of intrauterine growth retardation caused by chronic maternal undernutrition in the rat: effects on the somatotropic axis and postnatal growth. J Endocrinol 150: ( in press)
Buñag RD 1973 Validation in awake rats of a tail-cuff method for measuring systolic blood pressure. J Appl Physiol 34: 279–282
Law CM, de Swiet M, Osmond C, Fayers PM, Barker DJP, Cruddas AM, Fall CHD 1993 Initiation of hypertension in utero and its amplification throughout life. BMJ 306: 24–27
Unterman TG, Simmons RA, Glick RP, Ogata ES 1993 Circulating levels of insulin, insulin-like growth factor-I (IGF-I), IGF-II and IGF-binding proteins in the small for gestational age fetal rat. Endocrinology 132: 327–336
Straus DS, Ooi GT, Orlowski CC, Rechler MM 1991 Expression of the genes for insulin-like growth factor-I (IGF-I), IGF-II and IGF-binding proteins-1 and-2 in fetal rat under conditions of intra-uterine growth retardation caused by maternal fasting. Endocrinology 128: 518–525
Tapanainen PJ, Bang P, Wilson K, Unterman TG, Vreman HJ, Rosenfeld RG 1994 Maternal hypoxia as a model for intrauterine growth retardation: effects on insulin-like growth factors and their binding proteins. Pediatr Res 36: 152–158
Godfrey KM, Redman CW, Barker DJP, Osmond C 1991 The effect of maternal anemia and iron deficiency on the ratio of fetal weight to placental weight. Br J Obstet Gynaecol 98: 886–891
Barker DJP, Martyn CN 1992 The maternal and fetal origins of cardiovascular disease. J Epidemiol Community Health 46: 8–11
Barker DJP, Osmond C, Golding J, Kuh D, Wadsworth ME 1989 Growth in utero, blood pressure in childhood and adult life, and mortality from cardiovascular disease. BMJ 298: 564–567
Barker DJP, Osmond C, Simmonds SJ, Wield GA 1993 The relation of small head circumference and thinness at birth to death from cardiovascular disease in adult life. BMJ 306: 422–426
Barker DJP, Hales CN, Fall CH, Osmond C, Phipps K, Clark PM 1993 Type 2 (non-insulin dependent) diabetes mellitus, hypertension and hyperlipidaemia (syndrome X): relation to reduced fetal growth. Diabetologia 36: 62–67
Barker DJP, Bull AR, Osmond C, Simmonds SJ 1990 Fetal and placental size and risk of hypertension in adult life. BMJ 301: 259–262
Barker DJP 1992 The fetal origins of adult hypertension. J Hypertens 10( suppl 7): S39–S44
Lucas A 1991 Programming by early nutrition in man. In: The Childhood Environment and Adult Disease. [Ciba Foundation Symposium] Wiley, New York, pp 38–55
Folkow B 1978 Cardiovascular structural adaptation: its role in the initiation and maintenance of primary hypertension. Clin Sci Mol Med 55( suppl): 3S–22S
Benediktsson R, Lindsay RS, Noble J, Seckl JR, Edwards CRW 1993 Glucocorticoid exposure in utero: new model for adult hypertension. Lancet 341: 339–341
Murphy BEP, Clark SJ, Donald IR, Finsky M, Vedady D 1974 Conversion of maternal cortisol to cortisone during placental transfer to the human fetus. Am J Obstet Gynecol 118: 538–541
Langley-Evans SC, Phillips GJ, Benediktsson R, Gardner DS, Edwards CRW, Jackson AA, Seckl J 1996 Protein intake in pregnancy, placental glucocorticoid metabolism and the programming of hypertension. Placenta 17: 169–172
Paneth N, Susser M 1995 Early origin of coronary heart disease (the “Barker hypothesis”). BMJ 310: 411–412
Acknowledgements
The authors thank Rita Krishnamurthi for her assistance in measuring blood pressures.
Author information
Authors and Affiliations
Additional information
Funded by New Zealand Lottery Health and the Health Research Council of New Zealand.
Rights and permissions
About this article
Cite this article
Woodall, S., Johnston, B., Breier, B. et al. Chronic Maternal Undernutrition in the Rat Leads to Delayed Postnatal Growth and Elevated Blood Pressure of Offspring. Pediatr Res 40, 438–443 (1996). https://doi.org/10.1203/00006450-199609000-00012
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199609000-00012
This article is cited by
-
Effects on metabolic parameters in young rats born with low birth weight after exposure to a mixture of pesticides
Scientific Reports (2018)
-
Implications of maternal conditions and pregnancy course on offspring’s medical problems in adult life
Archives of Gynecology and Obstetrics (2016)
-
Maternal obesity and malnourishment exacerbate perinatal oxidative stress resulting in diabetogenic programming in F1 offspring
Journal of Endocrinological Investigation (2016)
-
Maternal salt and fat intake causes hypertension and sustained endothelial dysfunction in fetal, weanling and adult male resistance vessels
Scientific Reports (2015)
-
Programming of Essential Hypertension: What Pediatric Cardiologists Need to Know
Pediatric Cardiology (2015)