Abstract
Transient cerebral ischemia in fetal sheep is followed by a period of delayed cerebral injury associated with cerebral vasodilation. As nitric oxide(NO) can mediate both vasodilation and neuronal death, this study investigated whether inhibition of NO synthesis would attenuate the vasodilation and decrease cerebral injury. Eleven late gestation (range 122-133 d) fetal sheep were subjected to 30 min of transient cerebral ischemia in utero. Two hours later, treatment group (n = 5) received a continuous infusion of NG-nitro-L-arginine (L-NNA) at a dose of 50 mg·h-1 for 4 h followed by 20 mg·h-1 for the subsequent study period, a competitive inhibitor of NO synthase (NOS), whereas a control group (n = 6) received PBS. Inhibition of NOS activity was confirmed in the treatment group by 1) suppression of the fall in mean arterial blood pressure (MAP) associated with acetylcholine (p< 0.01), and 2) persistent increase in MAP after commencement of L-NNA (p < 0.05). Changes in cerebral blood volume (CBV) were observed for 3 d by measuring changes in concentration of total cerebral Hb([tHb]) using near infrared spectroscopy. The delayed increase in CBV commenced at 13.1 ± 1.0 h postischemia in the control and 12.7 ± 2.3 h in the treatment group. Maximum increase at 30-36 h was 0.5 ± 0.1 mL·100 g-1 in the treatment group and 1.2 ± 0.2 mL·100 g-1 in the control (p < 0.05). Final CBV was depressed below preischemic baseline in the treatment (-0.7 ± 0.2 mL·100 g-1) but not the control group (-0.1 ± 0.3 mL·100 g-1) (p < 0.05). Neuronal loss, quantified histologically 3 d postischemia, indicated that cerebral injury was increased in the treatment group (p < 0.05). The results indicate that after transient cerebral ischemia in fetal sheep, NOS inhibition attenuates the delayed rise in CBV but does not decrease the extent of cerebral injury.
Similar content being viewed by others
Main
Severe transient cerebral ischemia in fetal sheep is followed by two periods of cerebral vasodilation: an early period occurs immediately after the insult and lasts for 1 or 2 h and a second episode begins about 12 h later and continues for several hours(1). This second period of increased cerebral perfusion is coincident with a phase of delayed cerebral injury that can be demonstrated in fetal sheep by impaired cellular membrane function detected as an increase in CI and seizures(2). Delayed cerebral injury is an important feature of hypoxic-ischemic cerebral damage in the developing brain. It has been observed in rat pups, newborn piglets and asphyxiated infants with 31P magnetic resonance spectroscopy, as a delayed fall in the concentration of high energy phosphates, and in immature rats, as a delayed degradation of DNA(3–6).
Microdialysis studies have demonstrated that during delayed injury there is an increase in the extracellular concentration of citrulline(7). The latter is generated in the production of NO from L-arginine by NOS, and the finding suggests an increased production of NO. NO mediates cerebral vasodilation in the developing brain, and in the adult is thought to have a beneficial effect after cerebral ischemia by improving cerebral blood flow(8, 9). However, NO can also induce neuronal death through the generation of free radical species(10).
This study therefore investigated the hypothesis that delayed cerebral injury and delayed cerebral vasodilation after ischemia are mediated by increased NO production, and that inhibition of NO synthesis would reduce both delayed cerebral vasodilation and histologic injury. The effect of L-NNA, a competitive inhibitor of NOS, was investigated in late gestation fetal sheep. CI was recorded to determine the course and severity of the cerebral injury and NIRS was used to continuously measure changes in cerebral perfusion. The severity of cerebral injury was determined histologically at 3 d.
METHODS
Surgical procedure. Nineteen singleton Romney Suffolk fetal sheep of known gestational age (119-133 d) were operated on under 2% halothane/oxygen general anesthesia using sterile techniques. The general experimental approach has been described previously(2). Briefly, the 90-min procedure involved externalization of the fetal head, neck, and forelimbs and placement of polyvinyl catheters into the axillary arteries and amniotic cavity for measurement of MAP, and umbilical vein for drug administration. Through burr holes, three pairs of shielded stainless steel electrodes were placed on the dura overlying the parietal cortex-two pairs of ECoG electrodes (5 mm plus 15 mm anterior and 10 mm lateral to the bregma), and a third pair of stimulating electrodes to measure CI (10 mm anterior; 15 mm lateral to the bregma).
Cerebral blood supply was confined to the carotid arteries by ligation of the vertebro-occipital anastomoses, and on each carotid artery, a double ballooned inflatable cuff was positioned. Near infrared light was transmitted from laser diodes at four wavelengths (774, 826, 844, and 910 nm) and carried to and from the head via fiberoptic bundles. Optical prisms, at the ends of the bundles, were surgically fixed onto each side of the parietal region of the skull with dental cement at least 3.5 cm apart. The fetus was then returned to the uterus; the connecting lines were externalized through a uterine and maternal lateral skin incision, and muscle and skin layers were closed. After surgery the ewes were housed in metabolic cages at a constant temperature (16°C) and humidity (50%) and given free access to food and water. Antibiotics (gentamicin 80 mg i.v. to the fetus and penicillin 500 mg intramuscularly to the ewe) were administered daily for 3 d after surgery.
NIRS. The study used a commercial near infrared spectrophotometer (NIR 500 Hamamatsu Phototonics KK, Hamamatsu City, Japan). The technique depends on the transmission of near infrared light through tissue and its characteristic absorbance by three chromophores: HbO2, deoxyhemoglobin (Hb), and oxidized cytochrome aa3(11). Changes in chromophore concentration can be calculated from the changes in light absorption using a modification of the Beer Lambert law, which describes optical absorption in a highly scattering medium(12). Changes in [tHb], calculated as a sum of the changes in [Hb] and [HbO2] are related to changes in CBV by the cerebral hematocrit: CBV (mL·100 g brain-1) =[tHb]/(H·R) where H is the arterial Hb andR the cerebral-to-large vessel hematocrit ratio assumed to be 0.69(13).
Drug preparation. Ach (Sigma Chemical Co., St. Louis, MO) was diluted with sterile 0.9% normal saline (10 μg·mL-1). L-NNA(Sigma Chemical Co.) was dissolved in 0.1 M HCl and diluted with 1 M PBS (5 mg·mL-1) to a pH of 2.8-3.4.
Experimental protocol. Fetuses whose arterial blood gases and lactate were normal 2 d after surgery were entered into the study (Po2> 2.27 kPa, pH > 7.32, lactate < 1.2 mmol·L-1). NIRS, CI, MAP, and filtered ECoG recordings were commenced 12 h before the ischemic insult to obtain a baseline. During this period the hypotensive effect of a bolus i.v. injection of Ach (2 μg) was measured. Transient cerebral ischemia was induced by 30 min inflation of the bilateral carotid cuffs with saline and confirmed by an isoelectric ECoG and a rise in CI.
Two hours postischemia, fetuses were randomly assigned to treatment or control group. The treatment group received a continuous infusion of L-NNA into the umbilical vein at a dose of 50 mg·h-1 for the first 4 h followed by 20 mg·h-1 over the subsequent 3 d. The dose was shown in preliminary studies to attenuate the hypotensive effects of Ach, and attenuation was confirmed daily throughout the study period. The control group received equal volumes of 1 M PBS (pH 2.8-3.4) and Ach.
Sao2, Po2, Pco2, lactate, glucose, and Hb were measured before and immediately after the end of the occlusion, and at frequent intervals during the study period. Three days postischemia ewes were killed with an overdose of pentobarbital. All studies were approved by the Animal Ethical Committee of the University of Auckland.
Data collection. NIRS recordings of changes in [HbO2] and [Hb] were displayed on-line every 30 s during the study period and recorded on magnetic disks for later analysis.
ECoG was recorded continuously, and intensity spectra were obtained by real time spectral analysis as previously described(14). The ECoG signal was amplified 10 000 times, low pass filtered at 30 Hz, and sampled at 256 Hz. An eighth order Butterworth low pass filter was used with the cut-off frequency set with the -3 dB point at 30 Hz. A four-electrode technique was used to extract spectral ECoG (frequency) and CI signal from the ECoG(15). Increases in CI are associated with a fall in the extracellular space that occurs concomitantly with cytotoxic edema(2).
MAP, recorded from the brachial artery, was adjusted electronically for changes in amniotic pressure and thus changes in the ewe's posture. CI, ECoG, and corrected MAP recordings, displayed continuously on an analogue chart recorder running at 5 mm·min-1, were processed on-line, averaged over 1-min intervals, and recorded using a database acquisition program(Labview for Windows Version 2.5.1, National Instruments, Austin, TX).
Histologic assessment. Brains were fixed in 10% formalin and embedded in paraffin. As previously described, histologic sections were stained with thionine acid fuchsin, and scoring was performed on both hemispheres on coronal subserial sections (8 μm) by an independent neuropathologist experienced in the preparation (C.E.M.)(16). Dead cells were recognized by an acidophilic (red) cytoplasm and contracted nuclei, or just a small rim of red cytoplasm with a pyknotic nuclei, whereas all other cells were considered viable. The proportion of dead cells was assessed and scored, and a mean value was obtained from both hemispheres which was expressed as a percentage (neuronal score).
Data analysis and statistics. For analysis of NIRS variables, changes in the chromophore concentration were calculated from alterations in optical attenuation by least-squares multilinear regression using an algorithm that utilized accurate component spectra, took account of wavelength-dependent scattering, and calculated the changes in chromophore concentration(17). The distance between the optodes was determined during surgery and confirmed at postmortem using measuring callipers.
ECoG intensity data were log-transformed, and the onset of epileptiform activity was indicated by the development of intense (>-5 db), low frequency activity and confirmed by inspection of the chart recorder(18). Descriptive measurements of maxima, minima, 10% rise and fall times were made on data that had been median filtered over 500 s. Changes in the variables [HbO2], [Hb], MAP, CI, and ECoG activity for each fetus were averaged over 6-h time periods throughout the study period. Changes in CBV were calculated from [tHb] according to the arterial Hb that was measured throughout the study period(13). Changes in the averaged data within each group were determined by repeated measure analysis of variance with time as a repeated measure, and differences between the groups were determined by analysis of variance and Student-Newman-Keuls multiple comparisons test.
Linear regression analysis was used to determine the relation between histologic outcome and 1) the magnitude and duration of the delayed increase in CBV, 2) the final CBV at 66-72 h postischemia, and3) ECoG intensity at 66-72 h. The relation between CBV and ECoG intensity at 66-72 h was assessed.
Off line signal analyses were performed by Viewdac Data Acquisition, Version 2.1 (Keithley Data Acquisition Division, Keithley Instruments, Inc., Taunton, MA), and statistics were calculated by Sigmastat Statistical Analysis System, Version 1.02 (Jandel Scientific, Erkrath, Germany). Significant results (p value of < 0.05) are presented as the mean ± SEM. The end of the carotid artery occlusion is referred to as time zero.
RESULTS
Study groups. Nineteen subjects were investigated of which eight were rejected: three due to premature labor and five who died before the end of the study period. There was no difference in mortality between the treatment and control group. Eleven fetuses were allocated to control(n = 6) and treatment (n = 5) groups and were similar for gestational age (127 ± 1.2 d), weight (3.9 ± 0.2 kg), and head circumference (5.8 ± 0.1 cm). Table 1 shows the physiologic parameters throughout the study period. In both groups there was a rise in glucose and lactate and a fall in pH during the insult (p< 0.05). There was no difference in arterial blood gases, Hb, lactate, and glucose between the groups during the study period.
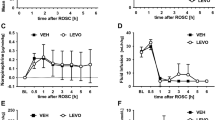
Evidence of NOS inhibition by L-NNA . Effect of L-NNA on the response to Ach. Figure 1 shows the change in MAP induced by 2 μg of Ach. In both groups Ach induced a fall in MAP before L-NNA treatment. In the control group, this effect was maintained throughout the study. However, it was suppressed in the treatment group after the administration of L-NNA (p < 0.001).
Changes in mean arterial blood pressure induced by Ach in control and L-NNA-treated group before and after cerebral ischemia. Shown are the changes in mean arterial blood pressure induced by the administration of 2 μg of Ach. Ach causes vasodilation and a fall in MAP through the release of NO, and the effect was attenuated in the treatment group(filled bars), after the commencement of L-NNA at 2 h (white bar) (*p < 0.001). Each bar represents the range and median at each time point for each group.
Effect of L-NNA on MAP. Changes in MAP throughout the study period are shown in Table 1. There was a rise in MAP during the insult in both groups (p < 0.001). This resolved in the control group after release of the occlusion and persisted in the treatment group after the commencement of L-NNA until 24 h postischemia(p < 0.05).
Cerebrovascular effects of L-NNA. Figure 2 shows the changes in CBV during and after cerebral ischemia. As previously shown, after transient cerebral ischemia there were two phases of increased CBV above preischemic baseline(1). The first phase immediately followed the insult and was similar in peak height and duration in the two groups.
Changes in CBV in control and L-NNA treatment groups during and after cerebral ischemia. The figure shows the changes in CBV(Δ CBV) during and after cerebral ischemia in control (○) and L-NNA-treated fetuses (•). There were two phases of increased CBV:1) an early phase immediately after the end of the ischemia and2) a delayed phase commencing several hours later. There was no difference in the early phase; however, the delayed phase was attenuated in the treated group (p < 0.01) (gray bar represents the period of L-NNA administration in the treatment group). Each symbol represents the mean (± SEM) of averaged data for each group.
The second phase commenced at 13.1 ± 1.0 h postischemia in the control group and 12.7 ± 2.3 h in the treatment group. However, the increase was attenuated in the treatment group (p < 0.01) and the maximum increase at 30-36 h was significantly different between control (1.2± 0.2 mL·100 g-1) and treatment group (0.5 ± 0.1 mL·100 g-1) (p < 0.05). Duration of the second increase in CBV was 43 ± 4 h in the control and 33 ± 2 h in the treatment group (p = 0.09). At the end of the study period (66-72 h postischemia), CBV was depressed below preischemic baseline in the treatment(-0.7 ± 0.2 mL·100 g-1; p < 0.05), but not in the control group (-0.1 ± 0.3 mL·100 g-1).
Linear regression analysis indicated that worse histologic outcome was related to: 1) shorter duration of the second increase in CBV(r = 0.8; p < 0.01; Fig. 3a) and2) lower final CBV (r = 0.8; p < 0.01;Fig. 3b).
The relation between the Δ CBV and histologic outcome after transient cerebral ischemia in control and L-NNA-treated fetuses. (a) The relation between duration of delayed increase in CBV (r = 0.7; p < 0.05) and (b) final CBV at the end of the study period (r = 0.8; p < 0.01) and neuronal score. A worse histologic outcome was related to a short-lived delayed increase in CBV and a more depressed final CBV.
Electrocortical activity and CI. Representative examples of the changes in ECoG 1) intensity and 2) CI in control and treatment group is shown in Figure 4.
Electrophysiologic variables after transient cerebral ischemia in a representative control and L-NNA-treated fetus. The time course of changes in (a) electrocortical (ECoG) intensity(upper) and (b) CI (lower) are shown in representative examples of a control fetus (left panel) and L-NNA-treated fetus (right panel). In both there is depression of ECoG intensity during ischemia accompanied by an acute rise in CI. Several hours after the insult, intense low frequency epileptiform activity developed and there was a delayed increase in CI. Greater depression of ECoG intensity by the end of the study period was evident in the treated animals.
ECoG intensity (Fig. 4a). ECoG intensity was depressed during and after ischemia. In both groups delayed cortical seizures were indicated by intense, low frequency ECoG activity and persisted for 20± 5 h in the control and 16 ± 3 h in the treatment group. In both groups ECoG intensity was depressed below preischemic baseline by the end of the study period and was more depressed in treatment (>19 ± 1 dB) compared with control group (>10 ± 2.0 dB) (p < 0.05).
The duration of seizures did not relate to histologic outcome. However, a more depressed final ECoG intensity at 66-72 h related to a lower final CBV(r = 0.8; p < 0.01) and a worse histologic outcome(r = 0.9; p < 0.01).
CI (Fig. 4b). This figure shows the two phases of increased CI above baseline: 1) during ischemia and2) commencing at 15 ± 3 h postischemia in the control group and 14 ± 4 h in the treatment group. The changes in CI throughout the study period are shown in Table 1. There was no difference in magnitude of the rise in CI during ischemia between the groups. Recovery CI at 2-6 h was 108 ± 2.7% in the control and 105 ± 1.4% in the treatment group, indicating no difference in the severity of the initial cerebral insult. The delayed increase in CI peaked to 140 ± 9% at 36± 2 h postischemia in the control group and 140 ± 6% at 42± 3 h in the treatment group.
Histologic outcome. Figure 5 gives the histologic results. The distribution of damage was similar in the two groups with laminar necrosis in the parasagittal region of the cortex and a lesser degree of injury in the lateral cortex, hippocampus, striatum and thalamus. There was increased cerebral injury in the treatment group in all regions assessed (p < 0.05).
Histologic outcome 3 d after transient cerebral ischemia in control and L-NNA-treated fetus. Neuronal loss was scored 3 d after transient cerebral ischemia in the parasagittal cortex (PsCx), lateral cortex (LtCx), striatum (Striat), amygdala(Amyg), thalamus (Thal), dentate gyrus (DG), subfields of the hippocampus (CA 1/2, 3, 4) and thalamus in control(□) and L-NNA-treated (□) animals. There was increased overall damage in the treated animals (p < 0.05). Each bar represents mean± SEM in each group.
DISCUSSION
In the present study treatment with the NOS inhibitor, L-NNA, attenuated the delayed cerebral vasodilation after transient cerebral ischemia in fetal sheep, led to cerebral vasoconstriction and was associated with more severe histologic injury.
NIRS allows continuous measurement of changes in cerebral vascular tone. When arterial [Hb] and the cerebral:peripheral hematocrit ratio remain constant, changes in [tHb] measured by NIRS, are a precise measure of changes in cerebral vascular volume(13). This reflects changes in cerebrovascular tone, which unlike measurements of cerebral blood flow(CBF), can be interpreted without considering changes in arterial blood pressure. The accuracy of NIRS for detecting alterations in [Hb] and[HbO2] has been described previously(12). Surgical fixation of the optodes to the fetal skull, which at this gestation has fused sutures, eliminated any alteration in optical path length due to movement. Changes in the scattering properties of the brain after ischemia have not been investigated, although they are unlikely to have any significant effect on the measurement of CBV(19). The experimental preparation thus permitted study of an isolated cerebral ischemic insult in an otherwise stable animal and eliminated the confounding factors of temperature control and anesthesia.
The severity of the ischemic insult is reflected by the residual increase in CI immediately after resuscitation and a greater increase predicts a worse cerebral injury(20). The residual CI was equal in control and treatment group (Table 1) and demonstrated that the severity of the ischemic insult was comparable in both groups.
L-NNA is an analog of L-arginine with a chemically altered guanidino moiety. The synthesis of NO involves oxidation of a guanidino-nitrogen moiety of L-arginine and L-NNA produces competitive and enantiomerically specific inhibition of the oxidation both in vitro and in vivo(21, 22). L-NNA does not have the antimuscarinic effects ascribed to the NOS inhibitors with alkyl ester substitutions at the carboxy terminal, and it inhibits both constitutively expressed and inducible NOS(23).
Inhibition of NOS within the systemic circulation was demonstrated by measuring the effect of Ach on MAP. NO is released by the endothelium in response to Ach, and stimulates soluble guanylate cyclase in smooth muscle resulting in a rise in cGMP and relaxation. Systemic vasodilation induces a transient fall in MAP and attenuation of the hypotensive effect of Ach has been used to confirm chronic NOS inhibition in fetal sheep(24). Accordingly, the treatment group received the dose of L-NNA used by Fineman et al.(24) and attenuation of the response to Ach was demonstrated throughout the study period. The dose required to achieve this effect (approximately 120 mg·kg-1·d-1) was greater that used in previous studies investigating the neuroprotective role of NO in perinatal animals(ranging from 1-100 mg·kg-1). In these studies the vascular effects of L-NNA were not assessed and may not have been achieved(25, 26). In the present study, L-NNA was continuously infused as it readily crosses the placenta and is eliminated through the maternal circulation(21).
The aim of this study was to examine the events associated with delayed cerebral injury, which is a critical period in the development of hypoxic-ischemic brain injury in the immature brain. Delayed injury has been demonstrated in human infants, piglets, and rat pups as a decline in cerebral high energy phosphates and in fetal sheep as an increase in CI(2–5). The magnitude of delayed injury correlates to severity of histologic damage and neurodevelopmental outcome in asphyxiated infants(27).
In fetal sheep, delayed injury is associated with a period of cerebral vasodilation, and with an increase in cerebral NO production(1, 7). As NO is able to mediate both vasodilation and neuronal cell death, we considered whether NO might be an important mediator of the delayed phase of cerebral injury. Inhibition of NO might be expected to reduce both cerebral vasodilation and cerebral damage.
The study found that NOS inhibition resulted in a reduction of cerebral vasodilation and an increase in histologic injury. There are several possible mechanisms which might explain this. The delayed increase in cerebral perfusion maybe a protective mechanism in part mediated by increased NO production. There is some evidence that increased NO production during, and for at least 1 h after cerebral ischemia is beneficial and NO donors improve the restoration of cerebral blood flow to ischemic tissue and reduce the extent of the infarction, although this effect has not been demonstrated in the developing brain(9, 28, 29). In this and previous studies, a greater injury is associated with a shorter delayed cerebral vasodilation and a lower final CBV whether or not the animal was treated with L-NNA(1). Reduction of cerebral vasodilation may be particularly detrimental during seizures when the metabolic demands of the brain are vastly increased(30, 31). Increased NO production may provide the link between neuronal activity and cerebral perfusion, and inhibiting NOS could limit substrate delivery and further jeopardize the survival of already compromised neurons(32–34).
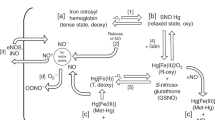
Another possibility is that the delayed production of NO is protective through its molecular and biochemical influence. Increasing evidence suggests that the redox versatility of NO allows it to form either protective or destructive species depending on the biologic milieu in which it is generated(35, 36). NO can exist as NO+ (nitrosonium ion), NO˙ (nitric oxide), and NO- (nitroxyl anion), and each respective species contains one additional electron. Under conditions favoring the formation of NO+, neuroprotection is incurred by the strong affinity of NO+ for the thiolate anion within NMDA receptors. NMDA receptor activity is down-regulated by S-nitrosylation and the subsequent inhibition of calcium influx is neuroprotective(37). NO can also protect against the cytotoxic effects of reactive oxygen species by scavenging the powerful oxidants and hydroxyl radicals(38). In addition, NO may protect by diverting superoxide radicals away from metal clusters toward sulfhydryl centers which are preferred targets for peroxynitrite formed from NO and superoxide(36).
There is also evidence that NO has anticonvulsant properties and NOS inhibitors can increase the intensity ofN-methyl-D-aspartate-induced seizures(39). NOS inhibition may increase cerebral injury by increasing seizure activity(40). However, in the present study there was no difference in the duration or magnitude of seizures in control and treatment group to explain the observed differences in histologic outcome.
Finally, there is a possibility that L-NNA is neurotoxic through a mechanism independent of NOS inhibition, but at present there is no published literature to substantiate this hypothesis.
Summary. NOS inhibition reduced the extent of delayed vasodilation and increased cerebral injury in fetal sheep after severe transient cerebral ischemia. NO production thus appears to have a protective action during the period of delayed cerebral injury, either by direct actions on neural functions or through its cerebrovascular effects. Further studies using more specific NOS inhibitors are required to distinguish these effects.
Abbreviations
- NIRS:
-
near infrared spectroscopy
- CI:
-
cortical impedance
- ECoG:
-
electrocorticographic activity
- [tHb]:
-
total cerebral Hb
- CBV:
-
cerebral blood volume
- NOS:
-
nitric oxide synthase
- NO:
-
nitric oxide
- L-NNA:
-
NG-nitro-L-arginine
- Sao2:
-
arterial oxygen saturation
- HbO2:
-
oxyhemoglobin
- MAP:
-
mean arterial blood pressure
- Ach:
-
acetylcholine
References
Marks KA, Mallard EC, Roberts I, Williams CE, Sirimanne ES, Johnston B, Gluckman PD, Edwards AD 1996 Delayed vasodilation and altered oxygenation after cerebral ischemia in fetal sheep. Pediatr Res 39: 48–54
Williams CE, Gunn AJ, Gluckman PD 1991 Time course of intracellular edema and epileptiform activity following prenatal cerebral ischemia in sheep. Stroke 22: 516–521
Blumberg RM, Cady EB, Wigglesworth JS, Edwards AD 1994 Delayed impairment of cerebral energy metabolism following transient focal hypoxia-ischemia in the 14 day old rat. Exp Brain Res ( in press)
Lorek A, Takei Y, Cady EB, Wyatt JS, Penrice J, Edwards AD, Peebles DM, Wylezinska M, Owen-Rees H, Kirkbride V, Cooper CE, Aldridge RF, Roth SC, Brown G, Delpy DT, Reynolds EOR 1994 Delayed (`secondary') cerebral energy failure following acute hypoxia-ischemia in the newborn piglet: continuous 48-hour studies by 31P magnetic resonance spectroscopy. Pediatr Res 36: 699–706
Wyatt JS, Edwards AD, Azzopardi D, Reynolds EOR 1989 Magnetic resonance and near infrared spectroscopy for the investigation of perinatal hypoxic ischaemic brain injury. Arch Dis Child 64: 953–963
Beilharz EJ, Williams CE, Dragunow M, Sirimanne ES, Gluckman PD 1995 Mechanisms of delayed cell death following hypoxic-ischemic injury in the immature rat: evidence for apoptosis during selective neuronal loss. Brain Res Mol Brain Res 29: 1–14
Tan WKM, Williams CE, During MJ, Mallard CE, Gunning MI, Gunn AJ, Gluckman PD 1996 Accumulation of cytotoxins during the development of seizures and edema after hypoxic-ischemic injury in late gestation fetal sheep. Pediatr Res 39: 791–797
Yamamoto S, Golanov EV, Berger SB, Reis DJ 1992 Inhibition of nitric oxide synthesis increases focal ischemic infarction in rat. J Cereb Blood Flow Metab 12: 717–726
Morikawa E, Moskowitz MA, Huang Z, Yoshida T, Irikura K, Dalkara T 1994 L-arginine infusion promotes nitric oxide-dependent vasodilation, increases regional cerebral blood flow, and reduces infarction volume in the rat. Stroke 25: 429–435
Beckman JS 1991 The double-edged role of nitric oxide in brain function and superoxide-mediated injury. J Dev Physiol 15: 53–59
Wray S, Cope M, Delpy DT, Wyatt JS, Reynolds EOR 1988 Characterization of the near infrared absorption spectra of cytochrome aa3 and haemoglobin for the non-invasive monitoring of cerebral oxygenation. Biochim Biophys Acta 933: 184–192
Reynolds EOR, Wyatt JS, Azzopardi D, Delpy DT, Cady EB, Cope M, Wray S 1988 New non-invasive methods for assessing brain oxygenation and haemodynamics. Br Med Bull 44: 1052–1075
Wyatt JS, Cope M, Delpy DT, Richardson CE, Edwards AD, Wray S, Reynolds EOR 1990 Quantitation of cerebral blood volume in human infants by near-infrared spectroscopy. J Appl Physiol 68: 1086–1091
Williams CE, Gluckman PD 1990 Real-time spectral intensity analysis of the EEG on a common microcomputer. J Neurosci Methods 32: 9–13
Robillard P, Poussart D 1979 Spatial resolution of four electrode array. IEEE Trans Biomed Eng 26: 465–470
Williams CE, Gunn AJ, Mallard C, Gluckman PD 1992 Outcome after ischemia in the developing sheep brain: an electroencephalographic and histological study. Ann Neurol 31: 14–21
Matcher SJ, Elwell CE, Cooper CE, Cope M, Delpy DT 1995 Performance comparison of several published tissue near-infrared spectroscopy algorithms. Ann Biochem 227: 54–68
Williams CE, Gunn AJ, Synek B, Gluckman PD 1990 Delayed seizures occurring with hypoxic-ischemic encephalopathy in the fetal sheep. Pediatr Res 27: 561–565
Wyatt JS, Cope M, Delpy DT, van der Zee P, Arridge S, Edwards AD, Reynolds EOR 1990 Measurement of optical path length for cerebral near-infrared spectroscopy in newborn infants. Dev Neurosci 12: 140–144
Gunn AJ, Parer JT, Mallard EC, Williams CE, Gluckman PD 1992 Cerebral histologic and electrocorticographic changes after asphyxia in fetal sheep. Pediatr Res 31: 486–491
Moncada S, Palmer RM, Higgs EA 1991 Nitric oxide: physiology, pathophysiology, and pharmacology. Pharmacol Rev 43: 109–142
Rees DD, Palmer RM, Schulz R, Hodson HF, Moncada S 1990 Characterisation of three inhibitors of endothelial nitric oxide synthasein vitro and in vivo. Br J Pharmacol 101: 746–752
Iadecola C, Pelligrino DA, Moskovitz MA, Lassen NA 1994 State of the art review: nitric oxide synthase inhibition and cerebrovascular regulation. J Cereb Blood Flow Metab 14: 175–192
Fineman JR, Wong J, Morin FC, Wild LM, Soifer SJ 1994 Chronic nitric oxide inhibition in utero produces persistent pulmonary hypertension in newborn lambs. J Clin Invest 93: 2675–2683
Hamada Y, Hayakawa T, Hattori H, Mikawa H 1994 Inhibitor of nitric oxide synthesis reduces hypoxic-ischemic brain damage in the neonatal rat. Pediatr Res 35: 10–14
Trifiletti RR 1992 Neuroprotective effects ofNG-nitro-L-arginine in focal stroke in the 7-day old rat. Eur J Pharmacol 218: 197–198
Azzopardi D, Wyatt JS, Cady EB, Delpy DT, Baudin J, Stewart AL, Hope PL, Hamilton PA, Reynolds EOR 1989 Prognosis of newborn infants with hypoxic-ischemic brain injury assessed by phosphorus magnetic resonance spectroscopy. Pediatr Res 25: 445–451
Zhang F, White JG, Iadecola C 1994 Nitric oxide donors increase blood flow and reduce brain damage in focal ischemia: evidence that nitric oxide is beneficial in the early stages of cerebral ischemia. J Cereb Blood Flow Metab 14: 217–226
Zhang F, Iadecola C 1994 Reduction of focal cerebral ischemic damage by delayed treatment with nitric oxide donors. J Cereb Blood Flow Metab 14: 574–580
Hill A, Volpe JJ 1981 Seizures, hypoxic-ischemic brain injury, and intraventricular hemorrhage in the newborn. Ann Neurol 10: 109–121
1992 Epilepsy, cerebral blood flow, and cerebral metabolic rate. Cerebrovasc Brain Metab Rev 4: 105–121
Iadecola C 1993 Regulation of the cerebral microcirculation during neural activity: is nitric oxide the missing link?. Trends Neurosci 16: 206–214
Faraci FM, Breese KR, Heistad DD 1993 Nitric oxide contributes to dilatation of cerebral arterioles during seizures. Am J Physiol 265:H2209–H2212
Rigaud Monnet AS, Pinard E, Borredon J, Seylaz J 1994 Blockade of nitric oxide synthesis inhibits hippocampal hyperemia in kainic acid-induced seizures. J Cereb Blood Flow Metab 14: 581–590
Lipton SA, Choi YB, Pan ZH, Lei SZ, Chen HS, Sucher NJ, Loscalzo J, Singel DJ, Stamler JS 1993 A redox-based mechanism for the neuroprotective and neurodestructive effects of nitric oxide and related nitroso-compounds. Nature 364: 626–632
Lipton SA, Singel DJ, Stamler JS 1994 Neuroprotective and neurodestructive effects of nitric oxide and redox congeners. Ann NY Acad Sci 738: 382–387
Stamler JS 1994 Redox signaling: nitrosylation and related target interactions of nitric oxide. Cell 78: 931–936
Beckman JS 1994 Peroxynitrite versus hydroxyl radical: the role of nitric oxide in superoxide-dependent cerebral injury. Ann NY Acad Sci 738: 69–75
Buisson A, Lakhmeche N, Verrecchia C, Plotkine M, Boulu RG 1993 Nitric oxide: an endogenous anticonvulsant substance. Neuroreport 4: 444–446
Wasterlain CG, Fujikawa DG, Penix L, Sankar R 1993 Pathophysiological mechanisms of brain damage from status epilepticus. Epilepsia 1( suppl 34): S37–S53
Author information
Authors and Affiliations
Additional information
Supported by The Wellcome Trust Grant M/92/4006), National Institutes of Health Grant HD 32752-021, and the Health Research Council of New Zealand.
Rights and permissions
About this article
Cite this article
Marks, K., Mallard, C., Roberts, I. et al. Nitric Oxide Synthase Inhibition Attenuates Delayed Vasodilation and Increases Injury after Cerebral Ischemia in Fetal Sheep. Pediatr Res 40, 185–191 (1996). https://doi.org/10.1203/00006450-199608000-00002
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199608000-00002
This article is cited by
-
Association Between rs3833912/rs16944 SNPs and Risk for Cerebral Palsy in Mexican Children
Molecular Neurobiology (2019)
-
Hypothermia for the treatment of infants with hypoxic–ischemic encephalopathy
Journal of Perinatology (2010)
-
Long-Term Neuroprotection with 2-Iminobiotin, An Inhibitor of Neuronal and Inducible Nitric Oxide Synthase, after Cerebral Hypoxia-Ischemia in Neonatal Rats
Journal of Cerebral Blood Flow & Metabolism (2005)
-
NO as a signalling molecule in the nervous system
British Journal of Pharmacology (2002)