Abstract
Background:
While older age is associated with higher tumor grade, it is unknown whether comorbid disease burden has a similar, independent association. We sought to evaluate the impact of comorbid disease burden on tumor grade at diagnosis as indicated by biopsy Gleason score.
Methods:
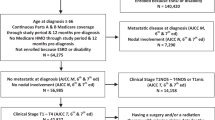
We conducted an observational cohort study of 1260 men newly diagnosed with non-metastatic prostate cancer from 1998 to 2004 at two Veterans Affairs Medical Centers. Multivariable ordinal and multinomial logistic regression were used to evaluate the association between Charlson Comorbidity Index score and biopsy Gleason score.
Results:
Men with Charlson scores of 2 (odds ratio (OR) 1.8, P<0.001) and 3+ (OR 1.8, P<0.001) had significantly greater odds of higher Gleason scores, compared with men with Charlson scores of 0. In a multinomial logistic regression model predicting Gleason 7 vs ⩾6, only men with Charlson scores of 2 (OR 1.6, P=0.01) had greater odds of having a Gleason 7 tumor, compared with those with Charlson scores of 0. In a multinomial logistic regression model predicting Gleason 8–10 vs ⩽6, those with Charlson scores of 1 (OR 1.6, P=0.047), 2 (OR 2.8, P=0.01) and 3+ (OR 2.9, P=0.001) had higher odds of having a Gleason 8–10 tumor.
Conclusions:
Moderate-to-heavy comorbid disease burden at diagnosis may be associated with high tumor grade, independent of age, and is a stronger predictor of Gleason 8–10 than Gleason 7 disease.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Daskivich TJ, Fan KH, Koyama T, Albertsen PC, Goodman M, Hamilton AS et al. Effect of age, tumor risk, and comorbidity on competing risks for survival in a U.S. population-based cohort of men with prostate cancer. Ann Intern Med 2013; 158: 709–717.
Albertsen PC, Moore DF, Shih W, Lin Y, Li H, Lu-Yao GL . Impact of comorbidity on survival among men with localized prostate cancer. J Clin Oncol 2011; 29: 1335–1341.
Alibhai SM, Leach M, Tomlinson G, Krahn MD, Fleshner N, Holowaty E et al. 30-day mortality and major complications after radical prostatectomy: influence of age and comorbidity. J Natl Cancer Inst 2005; 97: 1525–1532.
Ording AG, Horvath-Puho E, Lash TL, Ehrenstein V, Borre M, Vyberg M et al. Does comorbidity interact with prostate cancer to increase mortality? A Danish cohort study of 45 326 prostate cancer patients diagnosed during 1995-2011. Acta Oncol 2016; 55: 611–618.
Daskivich TJ, van de Poll-Franse LV, Kwan L, Sadetsky N, Stein DM, Litwin MS . From bad to worse: comorbidity severity and quality of life after treatment for early-stage prostate cancer. Prostate Cancer Prostatic Dis 2010; 13: 320–327.
Mohler JL, Armstrong AJ, Bahnson RR, D'Amico AV, Davis BJ, Eastham JA et al. Prostate cancer, version 1.2016. J Natl Compr Canc Netw 2016; 14: 19–30.
Heidenreich A, Bellmunt J, Bolla M, Joniau S, Mason M, Matveev V et al. EAU guidelines on prostate cancer. Part I: screening, diagnosis, and treatment of clinically localised disease. Actas Urol Esp 2011; 35: 501–514.
Thompson I, Thrasher JB, Aus G, Burnett AL, Canby-Hagino ED, Cookson MS et al. Guideline for the management of clinically localized prostate cancer: 2007 update. J Urol 2007; 177: 2106–2131.
Daskivich TJ, Lai J, Dick AW, Setodji CM, Hanley JM, Litwin MS et al. Questioning the ten-year life expectancy rule for high-grade prostate cancer: comparative effectiveness of aggressive vs. non-aggressive treatment of high-grade disease in older men with differing comorbid disease burdens. Urology 2016; 93: 68–76.
Bechis SK, Carroll PR, Cooperberg MR . Impact of age at diagnosis on prostate cancer treatment and survival. J Clin Oncol 2011; 29: 235–241.
Mandel P, Kriegmair MC, Kamphake JK, Chun FK, Graefen M, Huland H et al. Tumor characteristics and oncologic outcome after radical prostatectomy in men 75 years old or older. J Urol 2016; 196: 89–94.
Orozco R, O'Dowd G, Kunnel B, Miller MC, Veltri RW . Observations on pathology trends in 62,537 prostate biopsies obtained from urology private practices in the United States. Urology 1998; 51: 186–195.
Maurice MJ, Zhu H, Kiechle JE, Kim SP, Abouassaly R . Comorbid disease burden is independently associated with higher risk disease at prostatectomy in patients eligible for active surveillance. J Urol 2015; 95: 919–924.
Thomas JA 2nd, Gerber L, Banez LL, Moreira DM, Rittmaster RS, Andriole GL et al. Prostate cancer risk in men with baseline history of coronary artery disease: results from the REDUCE Study. Cancer Epidemiol Biomarkers Prev 2012; 21: 576–581.
Vidal AC, Howard LE, Moreira DM, Castro-Santamaria R, Andriole GL Jr., Freedland SJ . Obesity increases the risk for high-grade prostate cancer: results from the REDUCE study. Cancer Epidemiol Biomarkers Prev 2014; 23: 2936–2942.
Wu C, Moreira DM, Gerber L, Rittmaster RS, Andriole GL, Freedland SJ . Diabetes and prostate cancer risk in the REDUCE trial. Prostate Cancer Prostatic Dis 2011; 14: 326–331.
D'Amico AV, Whittington R, Malkowicz SB, Schultz D, Blank K, Broderick GA et al. Biochemical outcome after radical prostatectomy, external beam radiation therapy, or interstitial radiation therapy for clinically localized prostate cancer. JAMA 1998; 280: 969–974.
Charlson ME, Pompei P, Ales KL, MacKenzie CR . A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40: 373–383.
Daskivich TJ, Chamie K, Kwan L, Labo J, Palvolgyi R, Dash A et al. Overtreatment of men with low-risk prostate cancer and significant comorbidity. Cancer 2011; 117: 2058–2066.
Wilt TJ, Scardino PT, Carlsson SV, Basch E . Prostate-specific antigen screening in prostate cancer: perspectives on the evidence. J Natl Cancer Inst 2014; 106. dju010.
Bradley CJ, Dahman B, Anscher M . Prostate cancer treatment and survival: evidence for men with prevalent comorbid conditions. Med Care 2014; 52: 482–489.
Daskivich TJ, Lai J, Dick AW, Setodji CM, Hanley JM, Litwin MS et al. Questioning the 10-year life expectancy rule for high-grade prostate cancer: comparative effectiveness of aggressive vs nonaggressive treatment of high-grade disease in older men with differing comorbid disease burdens. Urology 2016; 93: 68–76.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
TJD is a consultant for Janssen Research & Development, LLC. The remaining authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Daskivich, T., Dru, C., Skarecky, D. et al. Association of comorbid disease burden at diagnosis with higher tumor grade in men with non-metastatic prostate cancer. Prostate Cancer Prostatic Dis 20, 343–347 (2017). https://doi.org/10.1038/pcan.2017.22
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2017.22
This article is cited by
-
Validation of the prostate cancer comorbidity index in predicting cause-specific mortality in men undergoing radical prostatectomy
Prostate Cancer and Prostatic Diseases (2023)