Abstract
Background:
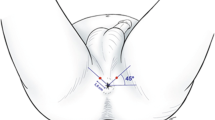
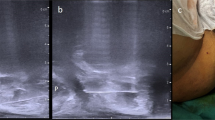
Despite high rates of disease misclassification and sepsis, the use of transrectal biopsy remains commonplace. Transperineal mapping biopsies mitigate these problems but carry increased cost and patient burden. Local anaesthetic, multiparametric magnetic resonance imaging (MRI)-targeted transperineal biopsy may offer an alternative. Here, we aim to determine the feasibility, tolerability and detection rates of clinically significant prostate cancer using a local anaesthetic, transperineal, MRI-targeted biopsy technique.
Methods:
Tertiary referral centre in which 181 consecutive men underwent local anaesthetic, transperineal MRI-targeted prostate biopsy (September 2014 to January 2016). A standardized local anaesthetic technique was used to obtain targeted biopsies using visual estimation with the number of targeted cores determined by each of a number of users. We assessed adverse events, patient visual analogue pain scores and detection rates of clinically significant cancer (defined by University College London (UCL) definitions one and two and separately by the presence of dominant and non-dominant Gleason pattern 4). We secondarily assessed detection of any cancer, rates of detection by MRI (Likert) score and by presenting PSA. Differences were assessed using Chi-squared tests (P<0.05).
Results:
One hundred eighty-one men with 243 lesions were included. There were no episodes of sepsis or re-admissions and one procedure was abandoned owing to patient discomfort. Twenty-three out of 25 (92%) men would recommend the procedure to another. Median visual analogue pain score was 1.0 (interquartile range: 0.0–2.4). A total 104/181 (57%) had UCL definition 1 disease (Gleason ⩾4+3 and/or maximum cancer length ⩾6 mm) and 129/181 (71%) had UCL definition 2 cancer (Gleason ⩾3+4 and/or maximum cancer length ⩾4 mm). Fifty-four out of 181 (30%) and 124/181 (69%) had dominant and non-dominant pattern 4 disease or greater (irrespective of cancer length). Any cancer was detected in 142/181 (78%). Significant disease was more likely in higher MRI-scoring lesions and in men with PSAs ⩾10 ng ml−1.
Conclusions:
This approach to prostate biopsy is feasible, tolerable and can be performed in ambulatory settings.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Han M, Chang D, Kim C, Lee BJ, Zuo Y, Kim HJ et al. Geometric evaluation of systematic transrectal ultrasound guided prostate biopsy. J Urol 2012; 188: 2404–2409.
Loeb S, Bjurlin MA, Nicholson J, Tammela TL, Penson DF, Carter HB et al. Overdiagnosis and overtreatment of prostate cancer. Eur Urol 2014; 65: 1046–1055.
Ahmed HU, El-Shater Bosaily A, Brown LC, Gabe R, Kaplan R, Parmar MK et al. Diagnostic accuracy of multi-parametric MRI and TRUS biopsy in prostate cancer (PROMIS): a paired validating confirmatory study. Lancet 2017; 389: 815–822.
Anastasiadis E, van der Meulen J, Emberton M . Hospital admissions after transrectal ultrasound-guided biopsy of the prostate in men diagnosed with prostate cancer: a database analysis in England. Int J Urol 2015; 22: 181–186.
Heidenreich A, Bastian PJ, Bellmunt J, Bolla M, Joniau S, van der Kwast T et al. EAU guidelines on prostate cancer. Part 1: screening, diagnosis, and local treatment with curative intent - update 2013. Eur Urol 2014; 65: 124–137.
Valerio M, Donaldson, Emberton M, Ehdale B, Hadaschik BA, Marks LS et al. Detection of clinically significant prostate cancer using magnetic resonance imaging-ultrasound fusion targeted biopsy: a systematic review. Eur Urol 2015; 68: 8–19.
Kasivisvanathan V, Dufour R, Moore CM, Ahmed HU, Abd-Alazeez M, Charman SC et al. Transperineal magnetic resonance image targeted prostate biopsy versus transperineal template prostate biopsy in the detection of clinically significant prostate cancer. J Urol 2013; 189: 860–866.
Grummet JP, Weerakoon M, Huang S, Lawrentschuk N, Frydenberg M, Moon DA et al. Sepsis and 'superbugs': should we favour the transperineal over the transrectal approach for prostate biopsy? BJU Int 2014; 114: 384–388.
Crawford ED, Rove KO, Barqawi AB, Maroni PD, Werahera PN, Baer CA et al. Clinical-pathologic correlation between trans- perineal mapping biopsies of the prostate and three-dimensional reconstruction of prostatectomy specimens. Prostate 2013; 73: 778.
Donaldson IA, Alonzi T, Barratt D, Berge V, Bott S, Bottomley D et al. Focal therapy: patients, interventions, and outcomes—a report from a consensus meeting. Eur Urol 2015; 67: 771–777.
Fütterer JJ, Briganti A, De Visschere P, Emberton M, Giannarini G, Kirkham A et al. Can clinically significant prostate cancer be detected with multiparametric magnetic resonance imaging? A systematic review of the literature. Eur Urol 2015; 68: 1045–1053.
Dickinson L, Ahmed HU, Allen C, Barentsz JO, Carey B, Futterer JJ et al. Scoring systems used for the interpretation and reporting of multiparametric mri for prostate cancer detection, localization, and characterization: could standardization lead to improved utilization of imaging within the diagnostic pathway? J Magn Reson Imaging 2013; 37: 48–58.
Kirkham A, Haslam P, Keanie JY, McCafferty I, Padhani AR, Punwani S et al. Prostate MRI: who, when, and how? Report from a UK consensus meeting. Clin Radiol 2013; 68: 1016–1023.
Rosenkrantz AB, Lim RP, Haghighi M, Somberg MB, Babb JS, Taneja SS . Comparison of interreader reproducibility of the prostate imaging reporting and data system and likert scales for evaluation of multiparametric prostate MRI. AJR Am J Roentgenol 2013; 201: W612–W618.
Ahmed HU, Hu Y, Carter T, Arumainayagam N, Lecornet E, Freeman A et al. Characterizing clinically significant prostate cancer using template prostate mapping biopsy. J Urol 2011; 186: 458–464.
Robertson NL, Hu Y, Ahmed HU, Freeman A, Barratt D, Emberton M . Prostate cancer risk inflation as a consequence of image-targeted biopsy of the prostate: a computer simulation study. Eur Urol 2014; 65: 628–634.
Abd-Alazeez M, Kirkham A, Ahmed HU, Arya M, Anastasiadis E, Charman SC et al. Performance of multiparametric MRI in men at risk of prostate cancer before the first biopsy: a paired validating cohort study using template prostate mapping biopsies as the reference standard. Prostate Cancer Prostatic Dis 2014; 17: 40–46.
Delongchamps NB, Lefevre A, Bouazza Z, Beuvon F, Legman P, Cornud F . Detection of significant prostate cancer with MR-targeted biopsies: should TRUS-MRI fusion guided biopsies alone be a standard of care? J Urol 2015; 193: 1198–1204.
Radtke JP, Schwab C, Wolf MB, Freitag MT, Alt CD, Kesch C et al. Multiparametric magnetic resonance imaging (MRI) and MRI-transrectal ultrasound fusion biopsy for index tumor detection: correlation with radical prostatectomy specimen. Eur Urol 2016; 70: 846–853.
Thompson JE, van Leeuwen PJ, Moses D, Shnier R, Brenner P, Delprado W . The diagnostic performance of multiparametric resonance imaging to detect significant prostate cancer. J Urol 2015; 195: 1428–1435.
Vargas HA, Akin O, Afaq A, Goldman D, Zheng J, Moskowitz CS et al. Magnetic resonance imaging for predicting prostate biopsy findings in patients considered for active surveillance of clinically low risk prostate cancer. J Urol 2012; 188: 1732–1738.
Hodge KK, McNeal JE, Terris MK, Stamey TA . Random systematic versus directed ultrasound guided transrectal core biopsies of the prostate. J Urol 1989; 142: 71–74.
Haas GP, Delongchamps N, Brawley OW, Wang CY, de la Roza G . The worldwide epidemiology of prostate cancer: perspectives from autopsy studies. Can J Urol 2008; 15: 3866–3871.
King CR, McNeal JE, Gill H, Presti J . Extended prostate biopsy scheme improves reliability of Gleason grading for radiotherapy patients. Int J Radiat Oncol Biol Phys 2004; 59: 386–391.
Puech P, Potiron E, Lemaitre L, Leroy X, Haber GP, Crouzet S et al. Dynamic contrast-enhanced- magnetic resonance imaging evaluation of intraprostatic prostate cancer: correlation with radical prostatectomy specimens. Urology 2009; 74: 1094–1099.
Kirkham APS, Emberton M, Allen C . How good is MRI at detecting and characterising cancer within the prostate? Eur Urol 2006; 50: 1163–1175.
Moore CM, Robertson N, Arsonious N, Middleton T, Villers A, Klotz L et al. Image-guided prostate biopsy using magnetic resonance imaging-derived targets: a systematic review. Eur Urol 2013; 63: 125–140.
Schoots IG, Roobol MJ, Nieboer D, Bangma CH, Steyerberg EW, Hunink MG . Magnetic resonance imaging-targeted biopsy may enhance the diagnostic accuracy of significant prostate cancer detection compared to standard transrectal ultrasound-guided biopsy: a systematic review and meta-analysis. Eur Urol 2015; 68: 438–450.
Grey A, Hartington T, KasiVisvanathan V, Arya M, Emberton M, Freeman A et al. Transperineal MRI visually-targeted prostate biopsies compared to template mapping biopsy in 534 men requiring further risk stratification. J Clin Urol 2016; 34 (suppl 9-77): (abstr P3-10).
Hamdy FC, Donovan JL, Lane JA, Mason M, Metcalfe C, Holding P et al. 10-Year outcomes after monitoring, surgery, or radiotherapy for localized prostate cancer. N Eng J Med 2016; 375: 1415–1424.
Novella G, Ficarra V, Galfano A, Ballario R, Novara G, Cavalleri S et al. Pain assessment after original transperineal prostate biopsy using a coaxial needle. Urology 2003; 62: 689–692.
Kubo Y, Kawakami S, Numao N, Takazawa R, Fujii Y, Masuda H et al. Simple and effective local anesthesia for transperineal extended prostate biopsy: application to three-dimensional 26-core biopsy. Int J Urol 2009; 16: 420–423.
Iremashvili VV, Chepurov AK, Kobaladze KM, Gamidov SI . Periprostatic local anesthesia with pudendal block for transperineal ultrasound-guided prostate biopsy: a randomized trial. Urology 2010; 75: 1023–1027.
Smith JB, Popert R, Nuttall MC, Vyas L, Kinsella J, Cahill D . Transperineal sector prostate biopsies: a local anesthetic outpatient technique. Urology 2014; 83: 1344–1349.
Wysock JS, Rosenkrantz AB, Huang WC, Stifelman MD, Lepor H, Deng FM et al. A prospective, blinded comparison of magnetic resonance (MR) imaging-ultrasound fusion and visual estimation in the performance of MR-targed prostate biopsy: the PROFUS trial. Eur Urol 2014; 66: 343–351.
Wegelin O, van Melick HH, Hooft L, Bosch JL, Reitsma HB, Barentsz JO et al. Comparing three different techniques for magnetic resonance imaging-targeted prostate biopsies: a systematic review of in-bore versus magnetic resonance imaging-transrectal ultrasound fusion versus cognitive registration. Is there a preferred technique? Eur Urol 2016; 71: 517–531.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Bass, E., Donaldson, I., Freeman, A. et al. Magnetic resonance imaging targeted transperineal prostate biopsy: a local anaesthetic approach. Prostate Cancer Prostatic Dis 20, 311–317 (2017). https://doi.org/10.1038/pcan.2017.13
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2017.13
This article is cited by
-
Landmarks in the evolution of prostate biopsy
Nature Reviews Urology (2023)
-
Pain control according to the periprostatic nerve block site in magnetic resonance imaging/transrectal targeted prostate biopsy
Scientific Reports (2022)
-
Are outpatient transperineal prostate biopsies without antibiotic prophylaxis equivalent to standard transrectal biopsies for patient safety and cancer detection rates?A retrospective cohort study in 222 patients
Patient Safety in Surgery (2021)
-
Transrectal versus transperineal prostate biopsy under intravenous anaesthesia: a clinical, microbiological and cost analysis of 2048 cases over 11 years at a tertiary institution
Prostate Cancer and Prostatic Diseases (2021)
-
Rationale and protocol for randomized study of transrectal and transperineal prostate biopsy efficacy and complications (ProBE-PC study)
Prostate Cancer and Prostatic Diseases (2021)