Abstract
Background:
Prostate cancer incidence and mortality vary dramatically by geographical location. Both are higher in developed countries. Some attribute this to westernized lifestyles of high-energy diets and limited physical activity with consequent obesity. Obesity and obesity-related diseases like diabetes cause hyperinsulinaemia, which upregulates pro-survival cell signalling. Previous work revealed diet-induced hyperinsulinaemia enhances prostate cancer xenograft growth in vivo. Metformin, an antidiabetic medication, reduces hyperinsulinaemia and also exhibits antineoplastic properties. Herein, we assess the potential additive benefit of combining bicalutamide antiandrogen therapy with metformin, in vitro and in vivo.
Methods:
Using clonogenic assays, we assessed the effect of bicalutamide and/or metformin on clonogenicity in prostate cancer cell lines. Western blot and cell cycle analyses were used to elucidate mechanisms of interaction between the drugs in androgen receptor (AR)-positive (LNCaP) and AR-negative (PC3) cell lines. The combination treatment regimen was assessed in vivo using an LNCaP murine xenograft model.
Results:
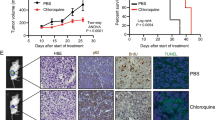
Micromolar bicalutamide or millimolar metformin caused a significant dose-dependent reduction in clonogenicity (P<0.001). Combination treatment further significantly reduced clonogenicity (P<0.005) with greater effects in AR-positive cells. Western blot and cell cycle analyses suggested differing mechanisms of interaction in AR-positive and -negative cell lines. Following combination treatment, LNCaP cells exhibited an altered cell proliferation (decreased phospho mammalian target of rapamycin expression) and perturbed cell cycle kinetics (G1/S cell cycle arrest). PC3 cells showed evidence of enhanced apoptosis (increased Bcl-2-associated X protein and decreased total caspase 3 expression). Markedly diminished tumour growth occurred following combination treatment in vivo (P<0.001).
Conclusions:
Combining bicalutamide and metformin significantly reduces prostate cancer cell growth further than either monotherapy. In AR-positive cells, this effect appeared to be mediated by reducing proliferation rates, whereas in AR-negative cells the combination treatment appeared to promote apoptosis. This combination drug regimen may improve prostate-cancer-specific survival by the direct antineoplastic properties outlined.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
American Cancer Society. Cancer Facts and Figures 2010. American Cancer Society: Atlanta, 2010.
Ogden CL, Carroll MD, Curtin LR, McDowell MA, Tabak CJ, Flegal KM . Prevalence of overweight and obesity in the United States, 1999–2004. JAMA 2006; 295: 1549–1555.
IARC. International Agency for Research in Cancer. Weight Control and Physical Activity. IARC press: Lyon, 2002.
MacInnis RJ, English DR, Haydon AM, Hooper JL, Gertig DM, Giles GG . Body size and composition and risk of rectal cancer (Australia). Cancer Causes Control 2006; 17: 1291–1297.
Freedland SJ, Platz EA, Presti Jr JC, Aronson WJ, Amling CL, Kane CJ et al. Obesity, serum prostate specific antigen and prostate size: implications for prostate cancer detection. J Urol 2006; 175: 500–504.
Gong Z, Neuhouser ML, Goodman PJ, Albanes D, Chi C, Hsing AW et al. Obesity, diabetes, and risk of prostate cancer: results from the prostate cancer prevention trial. Cancer Epidemiol Biomarkers Prev 2006; 15: 1977–1983.
Littman AJ, White E, Kristal AR . Anthropometrics and prostate cancer risk. Am J Epidemiol 2007; 165: 1271–1279.
Wright ME, Chang SC, Schatzkin A, Albanes D, Kipnis V, Mouw T et al. Prospective study of adiposity and weight change in relation to prostate cancer incidence and mortality. Cancer 2007; 109: 675–684.
Venkateswaran V, Haddad AQ, Fleshner NE, Fan R, Sugar LM, Nam R et al. Association of diet-induced hyperinsulinaemia with accelerated of prostate cancer (LNCaP) xenografts. J Natl Cancer Inst 2007; 99: 1793–1800.
Feller S, Boering H, Pischon T . Body mass index, waist circumference, and the risk of type 2 diabetes mellitus. Dtsch Arztebl Int 2010; 107: 470–476.
Guh DP, Zhang W, Bansback N, Amarsi Z, Birmingham CL, Anis AH . The incidence of co-morbidities related to obesity and overweight: a systematic review and meta-analysis. BMC Public Health 2009; 9: 88–107.
Fox CS, Pencina MJ, Meigs JB, Vasan RS, Levitzky YS, D’Agostino RB . Trends in the incidence of type 2 diabetes mellitus from the 1970 to the 1990s. The Framingham Heart Study. Circulation 2006; 113: 2914–2918.
Cusi K, Consoli A, DeFronza RA . Metabolic effects of metformin on glucose and lactate metabolism in noninsulin-dependent diabetes mellitus. J Clin Endocrinol Metab 1996; 81: 4059–4067.
Hundal RS, Krssak M, Dufour S, Laurent D, Lebon V, Chandramouli V et al. Mechanism by which metformin reduces glucose production in type 2 diabetes. Diabetes 2000; 49: 2063–2069.
Kahn B, Alquier T, Carling D, Hardie DG . AMP-activated protein kinase: ancient energy gauge provides clues to modern understanding of metabolism. Cell Metab 2005; 1: 15–25.
Sahra IB, Laurent K, Loubat A, Giorgetti-Peraldi S, Colosetti P, Auberger P et al. The antidiabetic drug metformin exerts an antitumoral effect in vitro and in vivo through a decrease of cyclin D1 level. Oncogene 2008; 27: 3576–3586.
Zakikhani M, Dowling R, Fabtus IG, Sonenberg N, Pollak M . Metformin is an AMP kinase–dependent growth inhibitor for breast cancer cells. Cancer Res 2006; 66: 10269–10273.
Zhuang Y, Mikimins WK . Cell cycle arrest in metformin treated breast cancer cells involves activation of AMPK, regulation of cyclin D1, and requires p27Kip1 or p21Cip1. J Mol Signal 2008; 3: 18–29.
Algire C, Zakikhani M, Blouin MJ, Shuai JH, Pollak M . Metformin attenuates the stimulatory effect of a high-energy diet on in vivo LLC1 carcinoma growth. Endocr-Relat Cancer 2008; 15: 833–839.
Zakikhani M, Dowling RJO, Sonenberg N, Pollak M . The effects of adiponectin and metformin on prostate and colon neoplasia involve activation of AMP-activated protein kinase. Cancer Prev Rev 2008; 15: 369–375.
Gotlieb WH, Samuet J, Beuchamp M-C, Gu J, Lau S, Pollak MN et al. In vitro metformin anti-neoplastic activity in epithelial ovarian cancer. Gynecol Oncol 2008; 110: 246–250.
Cantrell LA, Zhou C, Mendivil A, Molloy KM, Gehrig PA, Bae-Jump VL . Metformin is a potent inhibitor of endometrial cancer cell proliferation-implications for a novel treatment strategy. Gynecol Oncol 2010; 116: 92–98.
Agus DB, Cordon-Cardo C, Fox W, Drobnjak M, Koff A, Golde DW et al. Prostate cancer cell cycle regulators: response to androgen withdrawal and development of androgen independence. J Natl Cancer Inst 1999; 91: 1869–1876.
Knudsen KE, Arden KC, Cavenee WK . Multiple G1 regulatory elements control the androgen-dependent proliferation of prostatic carcinoma cells. J Biol Chem 1998; 273: 20213–20222.
McCrohan AM, Morrissey C, O’Keane, Mulligan N, Watson C, Smith J et al. Effects of the dual 5-alpha reductase inhibitor dutasteride on apoptosis in primary cultures of prostate cancer epithelial cells and cell lines. Cancer 2006; 106: 2743–2752.
Abramoff MD, Magelhaes PJ, Ram SJ . Image processing with ImageJ. Biophotonics International 2004; 11: 36–42.
Frid A, Sterner G, Londahl M, Wiklander C, Cato A, Vinge E et al. Novel assay of metformin levels in patients with type 2 diabetes and varying levels of renal function. Diabetes Care 2010; 33: 1291–1293.
Isakovic A, Harhaji L, Stevanovic D, Markovic Z, Sumarac-Dumanovic M, Starcevic V et al. Dual antiglioma action of metformin: cell cycle arrest and mitochondria-dependent apoptosis. Cell Mol Life Sci 2007; 64: 1290–1302.
Floyd MS, Teahan SJ, Fitzpatrick JM, Watson RW . Differential mechanisms of bicalutamide-induced apoptosis in prostate cell lines. Prostate Cancer Prostatic Dis 2009; 12: 25–33.
Hou M, Venier N, Sugar L, Musquera M, Pollak M, Kiss A et al. Protective effect of metformin in CD1 mice placed on a high carbohydrate-high fat diet. Biochem Biophys Res Commun 2010; 397: 537–542.
Acknowledgements
The authors gratefully acknowledge Prostate Cancer Canada and the Canadian Institute for Health Research to Dr Venkateswaran for generously funding this body of work.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Colquhoun, A., Venier, N., Vandersluis, A. et al. Metformin enhances the antiproliferative and apoptotic effect of bicalutamide in prostate cancer. Prostate Cancer Prostatic Dis 15, 346–352 (2012). https://doi.org/10.1038/pcan.2012.16
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2012.16
Keywords
This article is cited by
-
Efficacy of Bee Products (Anzer Honey, Pollen and Propolis) in Detection and Healing of Damage Induced by Antidiabetic Drug Vildagliptin/Metformin Hydrochloride in Healthy Human Pancreatic Cells: Cytotoxic, Genotoxic and Biochemical Studies
Current Medical Science (2023)
-
Metformin regulates multiple signaling pathways within castration-resistant human prostate cancer cells
BMC Cancer (2022)
-
A randomized phase 2 study of bicalutamide with or without metformin for biochemical recurrence in overweight or obese prostate cancer patients (BIMET-1)
Prostate Cancer and Prostatic Diseases (2022)
-
Association between metformin medication, genetic variation and prostate cancer risk
Prostate Cancer and Prostatic Diseases (2021)
-
Metformin enhances the radiosensitizing effect of cisplatin in non-small cell lung cancer cell lines with different cisplatin sensitivities
Scientific Reports (2019)