Abstract
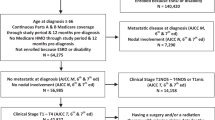
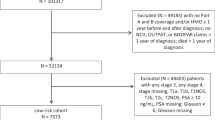
To quantify the downstream impact of PSA testing on cancer characteristics and utilization of cancer therapies among men aged 70 or older, we utilized patients diagnosed with prostate cancer in 2004–2005 in the Surveillance, Epidemiology and End Results (SEER)-Medicare and their Medicare claims before their cancer diagnosis during 2000–2005. Among men in the highest testing group (4–6 PSA tests), 75% were diagnosed with low- or intermediate-risk of disease, but 77% received treatments within 180 days of cancer diagnosis. More than 45% of newly diagnosed patients in 2004–2005 had 4–6 PSA tests before their cancer diagnosis during 2000–2005. Men in the high testing group were 3.57 times more likely to receive cancer treatments (either surgery, radiation or hormonal therapy) when compared with men who had no previous PSA testing during the same time period. Among men aged 75+ diagnosed with low-risk cancer, men in the high testing group were 78% more likely to receive treatment than those who had no previous PSA testing. In conclusion, given the lack of evidence of effective treatment for elderly patients diagnosed with low- and intermediate-risk prostate cancer and our inability to distinguish indolent from aggressive cancer, more frequent PSA testing among elderly population may exacerbate the risk of overdiagnosis and overtreatment.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Stamey TA, Yang N, Hay AR, McNeal JE, Freiha FS, Redwine E . Prostate-specific antigen as a serum marker for adenocarcinoma of the prostate. N Engl J Med 1987; 317: 909–916.
Lu-Yao G, Albertsen PC, Stanford JL, Stukel TA, Walker-Corkery ES, Barry MJ . Natural experiment examining impact of aggressive screening and treatment on prostate cancer mortality in two fixed cohorts from Seattle area and Connecticut. BMJ 2002; 325: 740.
Bill-Axelson A, Holmberg L, Ruutu M, Haggman M, Andersson SO, Bratell S et al. Radical prostatectomy versus watchful waiting in early prostate cancer. N Engl J Med 2005; 352: 1977–1984.
Kawachi MH, Bahnson RR, Barry M, Busby JE, Carroll PR, Carter HB et al. NCCN clinical practice guidelines in oncology: prostate cancer early detection. J Natl Compr Canc Netw 2010; 8: 240–262.
Bill-Axelson A, Holmberg L, Ruutu M, Garmo H, Stark JR, Busch C et al. Radical prostatectomy versus watchful waiting in early prostate cancer. N Engl J Med 2011; 364: 1708–1717.
Jemal A, Siegel R, Ward E, Hao Y, Xu J, Murray T et al. Cancer statistics, 2008. CA Cancer J Clin 2008; 58: 71–96.
Shao YH, Albertsen PC, Roberts CB, Lin Y, Mehta AR, Stein MN et al. Risk profiles and treatment patterns among men diagnosed as having prostate cancer and a prostate-specific antigen level below 4.0 ng/ml. Arch Intern Med 2010; 170: 1256–1261.
U.S. Preventive Services Task Force. Screening for prostate cancer: U.S. Preventive Services Task Force recommendation statement. Ann Intern Med 2008; 149: 185–191.
Schaeffer EM, Carter HB, Kettermann A, Loeb S, Ferrucci L, Landis P et al. Prostate specific antigen testing among the elderly--when to stop? J Urol 2009; 181: 1606–1614; discussion 1613–1604.
Walter LC, Bertenthal D, Lindquist K, Konety BR . PSA screening among elderly men with limited life expectancies. JAMA 2006; 296: 2336–2342.
Hudson SV, Ohman-Strickland P, Ferrante JM, Lu-Yao G, Orzano AJ, Crabtree BF . Prostate-specific antigen testing among the elderly in community-based family medicine practices. J Am Board Fam Med 2009; 22: 257–265.
Warren JL, Klabunde CN, Schrag D, Bach PB, Riley GF . Overview of the SEER-Medicare data: content, research applications, and generalizability to the United States elderly population. Med Care 2002; 40 (8 Suppl): IV-3-18.
Freeman JL, Klabunde CN, Schussler N, Warren JL, Virnig BA, Cooper GS . Measuring breast, colorectal, and prostate cancer screening with medicare claims data. Med Care 2002; 40 (8 Suppl): IV-36-42.
Charlson ME, Pompei P, Ales KL, MacKenzie CR . A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chronic Dis 1987; 40: 373–383.
Klabunde CN, Potosky AL, Legler JM, Warren JL . Development of a comorbidity index using physician claims data. J Clin Epidemiol 2000; 53: 1258–1267.
American Joint Committee on Cancer. Manual for Staging of Cancer, 5th edn. JB Lippincott: Philadelphia, 1997.
Hamilton AS, Gloeckler Ries L . Cancer of Prostate. In: Ries L, Young J, Keel G, Eisner M, YD L, M-J H (eds). SEER Survival Monograph: Cancer Survival Among Adults: U.S. SEER Program, 1988–2001, Patient and Tumor Characteristics. National Cancer Institute, SEER Program, NIH Pub: Bethesda, MD, 2007.
Mantel N, Haenszel W . Statistical aspects of the analysis of data from retrospective studies of disease. J Natl Cancer Inst 1959; 22: 719–748.
Mehta CR, Patel NR, Tsiatis AA . Exact significance testing to establish treatment equivalence with ordered categorical data. Biometrics 1984; 40: 819–825.
Advisory Committee on Cancer Prevention. Recommendations on cancer screening in the European Union. Eur J Cancer 2000; 36: 1473–1478.
van der Cruijsen-Koeter IW, Roobol MJ, Wildhagen MF, van der Kwast TH, Kirkels WJ, Schroder FH . Tumor characteristics and prognostic factors in two subsequent screening rounds with four-year interval within prostate cancer screening trial, ERSPC Rotterdam. Urology 2006; 68: 615–620.
Roobol MJ, Grenabo A, Schroder FH, Hugosson J . Interval cancers in prostate cancer screening: comparing 2- and 4-year screening intervals in the European Randomized Study of Screening for Prostate Cancer, Gothenburg and Rotterdam. J Natl Cancer Inst 2007; 99: 1296–1303.
Merenstein D . A piece of my mind. Winners and losers. JAMA 2004; 291: 15–16.
Linder SK, Hawley ST, Cooper CP, Scholl LE, Jibaja-Weiss M, Volk RJ . Primary care physicians’ reported use of pre-screening discussions for prostate cancer screening: a cross-sectional survey. BMC Fam Pract 2009; 10: 19.
Lin K, Lipsitz R, Miller T, Janakiraman S . Benefits and harms of prostate-specific antigen screening for prostate cancer: an evidence update for the U.S. Preventive Services Task Force. Ann Intern Med 2008; 149: 192–199.
Hayes JH, Ollendorf DA, Pearson SD, Barry MJ, Kantoff PW, Stewart ST et al. Active surveillance compared with initial treatment for men with low-risk prostate cancer: a decision analysis. JAMA 2010; 304: 2373–2380.
Barry MJ, Fleming C, Coley CM, Wasson JH, Fahs MC, Oesterling JE . Should Medicare provide reimbursement for prostate-specific antigen testing for early detection of prostate cancer? Part I: Framing the debate. Urology 1995; 46: 2–13.
Yabroff KR, Lamont EB, Mariotto A, Warren JL, Topor M, Meekins A et al. Cost of care for elderly cancer patients in the United States. J Natl Cancer Inst 2008; 100: 630–641.
Miles A, Cockburn J, Smith RA, Wardle J . A perspective from countries using organized screening programs. Cancer 2004; 101: 1201–1213.
Ross KS, Carter HB, Pearson JD, Guess HA . Comparative efficiency of prostate-specific antigen screening strategies for prostate cancer detection. JAMA 2000; 284: 1399–1405.
Lu-Yao GL, Albertsen PC, Moore DF, Shih W, Lin Y, DiPaola RS et al. Outcomes of localized prostate cancer following conservative management. JAMA 2009; 302: 1202–1209.
Acknowledgements
The study was supported by the following grants and awards: National Cancer Institute grant # RO1 CA 116399, Cancer Institute of New Jersey core grant NCI CA-72720-10 and Robert Wood Johnson foundation grant # 60624.
Authorship/disclaimer
All authors had access to the data and a role in writing the manuscript. This study used the linked SEER-Medicare database. The interpretation and reporting of these data are the sole responsibility of the authors. The content of the information does not reflect the position or policy of the Government or the employers, and no official endorsement should be inferred. The funding source had no role in the design, conduct, or analysis of this study or in the decision to submit the manuscript for publication.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Shao, YH., Albertsen, P., Shih, W. et al. The impact of PSA testing frequency on prostate cancer incidence and treatment in older men. Prostate Cancer Prostatic Dis 14, 332–339 (2011). https://doi.org/10.1038/pcan.2011.29
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2011.29
Keywords
This article is cited by
-
Intelligente Prostatakarzinomfrüherkennung 2021 – mehr Nutzen als Schaden
Der Urologe (2021)
-
Downstream tests, treatments, and annual direct payments in older men cared for by primary care providers with high or low prostate-specific antigen screening rates using 100 percent Texas U.S. Medicare public insurance claims data: a retrospective cohort study
BMC Health Services Research (2015)
-
Prognostic potential of ERG (ETS-related gene) expression in prostatic adenocarcinoma
International Urology and Nephrology (2013)