Abstract
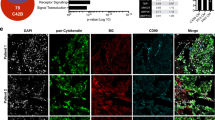
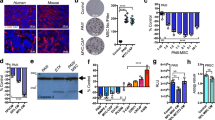
The growth of disseminated tumor cells into metastatic lesions depends on the establishment of a favorable microenvironment in the stroma of the target organs. Here we show that mice treated with anakinra, an antagonist of the interleukin (IL)-1β receptor (IL-1R), or harboring a targeted deletion of IL-1R are significantly less prone to develop bone tumors when inoculated in the arterial circulation with human prostate cancer (PCa) cells expressing IL-1β. Interestingly, human mesenchymal stem cells exposed in vitro to medium conditioned by IL-1β-expressing cancer cells responded by upregulating S100A4, a marker of cancer-associated fibroblasts (CAFs), and this effect was blocked by anakinra. Analogously, the stroma adjacent to skeletal metastases generated in mice by IL-1β-expressing cancer cells showed a dramatic increase in S100A4, COX-2 and the alteration of 30 tumor-related genes as measured by Nanostring analysis. These effects were not observed in the stroma associated with the rare and much smaller metastases generated by the same cells in IL-1R knockout animals, confirming that tumor-secreted IL-1β generates skeletal CAFs and conditions the surrounding bone microenvironment. In skeletal lesions from patients with metastatic PCa, histological and molecular analyses revealed that IL-1β is highly expressed in cancer cells in which the androgen receptor (AR) is not detected (AR−), whereas this cytokine is uniformly absent in the AR-positive (AR+) metastatic cells. The stroma conditioned by IL-1β-expressing cancer cells served as a supportive niche also for coexisting IL-1β-lacking cancer cells, which are otherwise unable to generate tumors after independently seeding the skeleton of mice. This niche is established very early following tumor seeding and hints to a role of IL-1β in promoting early colonization of PCa at the skeletal level.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Voronov E, Shouval DS, Krelin Y, Cagnano E, Benharroch D, Iwakura Y et al. IL-1 is required for tumor invasiveness and angiogenesis. Proc Natl Acad Sci USA 2003; 100: 2645–2650.
Lewis AM, Varghese S, Xu H, Alexander HR . Interleukin-1 and cancer progression: the emerging role of interleukin-1 receptor antagonist as a novel therapeutic agent in cancer treatment. J Transl Med 2006; 4: 48.
Valdivia-Silva JE, Franco-Barraza J, Silva ALE, Pont GD, Soldevila G, Meza I et al. Effect of pro-inflammatory cytokine stimulation on human breast cancer: implications of chemokine receptor expression in cancer metastasis. Cancer Lett 2009; 283: 176–185.
Dinarello CA . Why not treat human cancer with interleukin-1 blockade? Cancer Metastasis Rev 2010; 29: 317–329.
Liu Q, Russell MR, Shahriari K, Jernigan DL, Lioni MI, Garcia FU et al. Interleukin-1β promotes skeletal colonization and progression of metastatic prostate cancer cells with neuroendocrine features. Cancer Res 2013; 73: 3297–3305.
Eckhardt BL . Strategies for the discovery and development of therapies for metastatic breast cancer. Nat Rev Drug Discov 2012; 11: 479–497.
Wang M, Stearns ME . Isolation and characterization of PC-3 human prostatic tumor sublines which preferentially metastasize to select organs in S.C.I.D. mice. Differentiation 1991; 48: 115–125.
Russell MR, Jamieson WL, Dolloff NG, Fatatis A . The alpha-receptor for platelet-derived growth factor as a target for antibody-mediated inhibition of skeletal metastases from prostate cancer cells. Oncogene 2009; 28: 412–421.
Dinarello CA, Simon A, van der Meer JWM . Treating inflammation by blocking interleukin-1 in a broad spectrum of diseases. Nat Rev Drug Discov 2012; 11: 633–652.
Madar S, Goldstein I, Rotter V . ‘Cancer associated fibroblasts’ – more than meets the eye. Trends Mol Med 2013; 19: 447–453.
Orimo A, Gupta PB, Sgroi DC, Arenzana-Seisdedos F, Delaunay T, Naeem R et al. Stromal fibroblasts present in invasive human breast carcinomas promote tumor growth and angiogenesis through elevated SDF-1/CXCL12 secretion. Cell 2005; 121: 335–348.
Giannoni E, Bianchini F, Masieri L, Serni S, Torre E, Calorini L et al. Reciprocal activation of prostate cancer cells and cancer-associated fibroblasts stimulates epithelial-mesenchymal transition and cancer stemness. Cancer Res 2010; 70: 6945–6956.
Karagiannis GS, Poutahidis T, Erdman SE, Kirsch R, Riddell RH, Diamandis EP . Cancer-associated fibroblasts drive the progression of metastasis through both paracrine and mechanical pressure on cancer tissue. Mol Cancer Res 2012; 10: 1403–1418.
Li H-J, Reinhardt F, Herschman HR, Weinberg RA . Cancer-stimulated mesenchymal stem cells create a carcinoma stem cell niche via prostaglandin E2 signaling. Cancer Discov 2012; 2: 840–855.
Garrett SC, Varney KM, Weber DJ, Bresnick AR . S100A4, a mediator of metastasis. J Biol Chem 2006; 281: 677–680.
Weckermann D, Müller P, Wawroschek F, Harzmann R, Riethmüller G, Schlimok G . Disseminated cytokeratin positive tumor cells in the bone marrow of patients with prostate cancer: detection and prognostic value. J Urol 2001; 166: 699–703.
Xu J, Kalos M, Stolk JA, Zasloff EJ, Zhang X, Houghton RL et al. Identification and characterization of prostein, a novel prostate-specific protein. Cancer Res 2001; 61: 1563–1568.
Kalos M, Askaa J, Hylander BL, Repasky EA, Cai F, Vedvick T et al. Prostein expression is highly restricted to normal and malignant prostate tissues. Prostate 2004; 60: 246–256.
Sheridan T, Herawi M, Epstein JI, Illei PB . The role of P501S and PSA in the diagnosis of metastatic adenocarcinoma of the prostate. Am J Surg Pathol 2007; 31: 1351–1355.
Cindolo L, Franco R, Cantile M, Schiavo G, Liguori G, Chiodini P et al. NeuroD1 expression in human prostate cancer: can it contribute to neuroendocrine differentiation comprehension? Eur Urol 2007; 52: 1365–1373.
Komiya A, Suzuki H, Imamoto T, Kamiya N, Nihei N, Naya Y et al. Neuroendocrine differentiation in the progression of prostate cancer. Int J Urol 2009; 16: 37–44.
Bersani F, Lee J, Yu M, Morris R, Desai R, Ramaswamy S et al. Bioengineered implantable scaffolds as a tool to study stromal-derived factors in metastatic cancer models. Cancer Res 2014; 74: 7229–7238.
Drake JM, Gabriel CL, Henry MD . Assessing tumor growth and distribution in a model of prostate cancer metastasis using bioluminescence imaging. Clin Exp Metastasis 2005; 22: 674–684.
Drake JM, Danke JR, Henry MD . Bone-specific growth inhibition of prostate cancer metastasis by atrasentan. Cancer Biol Ther 2010; 9: 607–614.
Shen F, Zhang Y, Jernigan DL, Feng X, Yan J, Garcia FU et al. Novel small-molecule CX3CR1 antagonist impairs metastatic seeding and colonization of breast cancer cells. Mol Cancer Res 2016; 14: 518–527.
Cohen SB . The use of anakinra, an interleukin-1 receptor antagonist, in the treatment of rheumatoid arthritis. Rheum Dis Clin North Am 2004; 30: 365–380.
Boye K, Mælandsmo GM . S100A4 and metastasis. Am J Pathol 2010; 176: 528–535.
Goel HL, Li J, Kogan S, Languino LR . Integrins in prostate cancer progression. Endocr Relat Cancer 2008; 15: 657–664.
Hemingway F, Taylor R, Knowles HJ, Athanasou NA . RANKL-independent human osteoclast formation with APRIL, BAFF, NGF, IGF I and IGF II. Bone 2011; 48: 938–944.
Wai PY, Kuo PC . Osteopontin: regulation in tumor metastasis. Cancer Metastasis Rev 2008; 27: 103–118.
Yu D, Zhong Y, Li X, Li Y, Li X, Cao J et al. ILs-3, 6 and 11 increase, but ILs-10 and 24 decrease stemness of human prostate cancer cells in vitro. Oncotarget 2015; 6: 42687–42703.
Pio R, Corrales L, Lambris JD . The role of complement in tumor growth. Adv Exp Med Biol 2014; 772: 229–262.
Kim S, Iizuka K, Aguila HL, Weissman IL, Yokoyama WM . In vivo natural killer cell activities revealed by natural killer cell-deficient mice. Proc Natl Acad Sci USA 2000; 97: 2731–2736.
Childs RW, Carlsten M . Therapeutic approaches to enhance natural killer cell cytotoxicity against cancer: the force awakens. Nat Rev Drug Discov 2015; 14: 487–498.
Shariff AH, Ather MH . Neuroendocrine differentiation in prostate cancer. Urology 2006; 68: 2–8.
Jiborn T, Bjartell A, Abrahamsson PA . Neuroendocrine differentiation in prostatic carcinoma during hormonal treatment. Urology 1998; 51: 585–589.
Sun Y, Niu J, Huang J . Neuroendocrine differentiation in prostate cancer. Am J Transl Res 2009; 1: 148–162.
Beltran H, Rickman DS, Park K, Chae SS, Sboner A, MacDonald TY et al. Molecular characterization of neuroendocrine prostate cancer and identification of new drug targets. Cancer Discov 2011; 1: 487–495.
Sharma A, Yeow W-S, Ertel A, Coleman I, Clegg N, Thangavel C et al. The retinoblastoma tumor suppressor controls androgen signaling and human prostate cancer progression. J Clin Invest 2010; 120: 4478–4492.
Zhao Y, Tindall DJ, Huang H . Modulation of androgen receptor by FOXA1 and FOXO1 factors in prostate cancer. Int J Biol Sci 2014; 10: 614–619.
Fenton MJ . Review: transcriptional and post-transcriptional regulation of interleukin 1 gene expression. Int J Immunopharmacol 1992; 14: 401–411.
Klein CA . Selection and adaptation during metastatic cancer progression. Nature 2013; 501: 365–372.
Bedard PL, Hansen AR, Ratain MJ, Siu LL . Tumour heterogeneity in the clinic. Nature 2013; 501: 355–364.
Mickey DD, Stone KR, Wunderli H, Mickey GH, Vollmer RT, Paulson DF . Heterotransplantation of a human prostatic adenocarcinoma cell line in nude mice. Cancer Res 1977; 37: 4049–4058.
Tabassum DP, Polyak K . Tumorigenesis: it takes a village. Nat Rev Cancer 2015; 15: 473–483.
Wurth R, Tarn K, Jernigan D, Fernandez SV, Cristofanilli M, Fatatis A et al. A preclinical model of inflammatory breast cancer to study the involvement of CXCR4 and ACKR3 in the metastatic process. Transl Oncol 2015; 8: 358–367.
Jamieson-Gladney WL, Zhang Y, Fong AM, Meucci O, Fatatis A . The chemokine receptor CX3CR1 is directly involved in the arrest of breast cancer cells to the skeleton. Breast Cancer Res 2011; 13: R91.
Acknowledgements
We thank Dr Olimpia Meucci (Department of Pharmacology and Physiology at Drexel University College of Medicine) for invaluable advice, Dr Kevin Kelly (Medical Oncology) and all the other members of the Greater Philadelphia Prostate Cancer Working Group at the Sidney Kimmel Cancer Center, Thomas Jefferson University for insightful discussions, Dr Ruth Birbe (Pathology) at Thomas Jefferson University for providing the human specimens of skeletal metastases and Danielle Jernigan (Fatatis laboratory) for critical reading of the manuscript. This work was supported by NIH F30CA192896-01 grant to KS and in part by Department of Defense PC080987 Idea Award to AF.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Oncogene website
Supplementary information
Rights and permissions
About this article
Cite this article
Shahriari, K., Shen, F., Worrede-Mahdi, A. et al. Cooperation among heterogeneous prostate cancer cells in the bone metastatic niche. Oncogene 36, 2846–2856 (2017). https://doi.org/10.1038/onc.2016.436
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2016.436
This article is cited by
-
Subsets of cancer cells expressing CX3CR1 are endowed with metastasis-initiating properties and resistance to chemotherapy
Oncogene (2022)
-
Invasion front dynamics of interactive populations in environments with barriers
Scientific Reports (2022)
-
Metastasis-associated fibroblasts: an emerging target for metastatic cancer
Biomarker Research (2021)
-
YAP1 plays a key role of the conversion of normal fibroblasts into cancer-associated fibroblasts that contribute to prostate cancer progression
Journal of Experimental & Clinical Cancer Research (2020)