Abstract
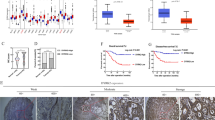
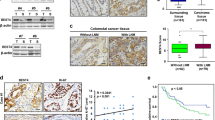
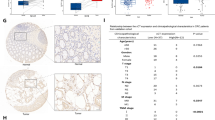
Colon cancer is the third leading cause of death from cancer worldwide with less than 10% survival rate at the late stage. Although mutations of certain genes have been implicated in familial colon cancer development, the etiology of the majority of colon cancer remains unknown. Herein, we identified TYRO3 as a potential oncogene. Immunohistochemical staining results demonstrated that levels of TYRO3 were markedly elevated in polyps and colon cancer cells and were negatively correlated with prognosis. Overexpression of TYRO3 enhanced cell motility, invasion, anchorage-independent growth and metastatic ability, while knockdown of TYRO3 impaired all these processes. Results from meta-analysis showed that TYRO3 was associated with epithelial–mesenchymal transition (EMT) signatures. Gain-of-function and loss-of-function experiments demonstrated that expression of SNAI1, the master regulator of EMT, was regulated by TYRO3 and played a major role in mediating TYRO3-induced EMT processes. The murine model also demonstrated that Tyro3 and Snai1 were upregulated in the early stage of colon cancer development. To provide a proof-of-concept that TYRO3 is a druggable target in colon cancer therapy, we raised anti-TYRO3 human antibodies and showed that treatment with the human antibody abolished TYRO3-induced EMT process. More importantly, administration of this anti-TYRO3 antibody increased drug sensitivity in primary cultured colon cancer cells and xenografted mouse tumors. These findings demonstrate that TYRO3 is a novel oncogene and a druggable target in colon cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Golan T, Urban D, Berger R, Lawrence YR . Changing prognosis of metastatic colorectal adenocarcinoma: differential improvement by age and tumor location. Cancer 2013; 119: 3084–3091.
Fearon ER, Vogelstein B . A genetic model for colorectal tumorigenesis. Cell 1990; 61: 759–767.
Groden J, Thliveris A, Samowitz W, Carlson M, Gelbert L, Albertsen H et al. Identification and characterization of the familial adenomatous polyposis coli gene. Cell 1991; 66: 589–600.
Takayama T, Katsuki S, Takahashi Y, Ohi M, Nojiri S, Sakamaki S et al. Aberrant crypt foci of the colon as precursors of adenoma and cancer. N Engl J Med 1998; 339: 1277–1284.
Petitjean A, Achatz MI, Borresen-Dale AL, Hainaut P, Olivier M . TP53 mutations in human cancers: functional selection and impact on cancer prognosis and outcomes. Oncogene 2007; 26: 2157–2165.
Chan HH, Tsai SJ, Sun HS . TAG: a comprehensive database for cancer research. Nucleic Acids Res 2007, Molecular Biology Database Collection: 922.
Lemke G, Rothlin CV . Immunobiology of the TAM receptors. Nat Rev Immunol 2008; 8: 327–336.
Stitt TN, Conn G, Gore M, Lai C, Bruno J, Radziejewski C et al. The anticoagulation factor protein S and its relative, Gas6, are ligands for the Tyro 3/Axl family of receptor tyrosine kinases. Cell 1995; 80: 661–670.
Schlessinger J . Cell signaling by receptor tyrosine kinases. Cell 2000; 103: 211–225.
Taylor IC, Roy S, Varmus HE . Overexpression of the Sky receptor tyrosine kinase at the cell surface or in the cytoplasm results in ligand-independent activation. Oncogene 1995; 11: 2619–2626.
Crosier KE, Crosier PS . New insights into the control of cell growth; the role of the AxI family. Pathology 1997; 29: 131–135.
Neubauer A, Burchert A, Maiwald C, Gruss HJ, Serke S, Huhn D et al. Recent progress on the role of Axl, a receptor tyrosine kinase, in malignant transformation of myeloid leukemias. Leuk Lymphoma 1997; 25: 91–96.
O'Bryan JP, Frye RA, Cogswell PC, Neubauer A, Kitch B, Prokop C et al. axl, a transforming gene isolated from primary human myeloid leukemia cells, encodes a novel receptor tyrosine kinase. Mol Cell Biol 1991; 11: 5016–5031.
Sun WS, Fujimoto J, Tamaya T . Clinical implications of coexpression of growth arrest-specific gene 6 and receptor tyrosine kinases Axl and Sky in human uterine leiomyoma. Mol Hum Reprod 2003; 9: 701–707.
Sawabu T, Seno H, Kawashima T, Fukuda A, Uenoyama Y, Kawada M et al. Growth arrest-specific gene 6 and Axl signaling enhances gastric cancer cell survival via Akt pathway. Mol Carcinog 2007; 46: 155–164.
Sun W, Fujimoto J, Tamaya T . Coexpression of Gas6/Axl in human ovarian cancers. Oncology 2004; 66: 450–457.
Gjerdrum C, Tiron C, Hoiby T, Stefansson I, Haugen H, Sandal T et al. Axl is an essential epithelial-to-mesenchymal transition-induced regulator of breast cancer metastasis and patient survival. Proc Natl Acad Sci USA 2010; 107: 1124–1129.
Song X, Wang H, Logsdon CD, Rashid A, Fleming JB, Abbruzzese JL et al. Overexpression of receptor tyrosine kinase Axl promotes tumor cell invasion and survival in pancreatic ductal adenocarcinoma. Cancer 2011; 117: 734–743.
Asiedu MK, Beauchamp-Perez FD, Ingle JN, Behrens MD, Radisky DC, Knutson KL . AXL induces epithelial-to-mesenchymal transition and regulates the function of breast cancer stem cells. Oncogene 2014; 33: 1316–1324.
Biesecker LG, Gottschalk LR, Emerson SG . Identification of four murine cDNAs encoding putative protein kinases from primitive embryonic stem cells differentiated in vitro. Proc Natl Acad Sci USA 1993; 90: 7044–7048.
Linger RM, Keating AK, Earp HS, Graham DK . TAM receptor tyrosine kinases: biologic functions, signaling, and potential therapeutic targeting in human cancer. Adv Cancer Res 2008; 100: 35–83.
De Vos J, Couderc G, Tarte K, Jourdan M, Requirand G, Delteil MC et al. Identifying intercellular signaling genes expressed in malignant plasma cells by using complementary DNA arrays. Blood 2001; 98: 771–780.
Avilla E, Guarino V, Visciano C, Liotti F, Svelto M, Krishnamoorthy G et al. Activation of TYRO3/AXL tyrosine kinase receptors in thyroid cancer. Cancer Res 2011; 71: 1792–1804.
Zhu S, Wurdak H, Wang Y, Galkin A, Tao H, Li J et al. A genomic screen identifies TYRO3 as a MITF regulator in melanoma. Proc Natl Acad Sci USA 2009; 106: 17025–17030.
Duijkers FA, Meijerink JP, Pieters R, van Noesel MM . Downregulation of Axl in non-MYCN amplified neuroblastoma cell lines reduces migration. Gene 2013; 521: 62–68.
Gerloff J, Korshunov VA . Immune modulation of vascular resident cells by Axl orchestrates carotid intima-media thickening. Am J Pathol 2012; 180: 2134–2143.
Budinska E, Popovici V, Tejpar S, D'Ario G, Lapique N, Sikora KO et al. Gene expression patterns unveil a new level of molecular heterogeneity in colorectal cancer. J Pathol 2013; 231: 63–76.
Goldenberg MM . Trastuzumab, a recombinant DNA-derived humanized monoclonal antibody, a novel agent for the treatment of metastatic breast cancer. Clin Ther 1999; 21: 309–318.
Caron PC, Schwartz MA, Co MS, Queen C, Finn RD, Graham MC et al. Murine and humanized constructs of monoclonal antibody M195 (anti-CD33) for the therapy of acute myelogenous leukemia. Cancer 1994; 73 (Suppl): 1049–1056.
Prewett M, Rockwell P, Rockwell RF, Giorgio NA, Mendelsohn J, Scher HI et al. The biologic effects of C225, a chimeric monoclonal antibody to the EGFR, on human prostate carcinoma. J Immunother Emphasis Tumor Immunol 1996; 19: 419–427.
Chien C-W, Lin S-C, Lai Y-Y, Lin B-W, Lin S-C, Lee J-C et al. Regulation of CD151 by hypoxia controls cell adhesion and metastasis in colorectal cancer. Clin Cancer Res 2008; 14: 8043–8051.
Lu RM, Chang YL, Chen MS, Wu HC . Single chain anti-c-Met antibody conjugated nanoparticles for in vivo tumor-targeted imaging and drug delivery. Biomaterials 2011; 32: 3265–3274.
Acknowledgements
We thank Miss Yi-Hsuan Yeh and Miss Yi-Chen Tang for technical assistance with IHC and animal study. This work was supported by grants from National Science Council of Taiwan (NSC 101-2321-B-006-020 and NSC 102-2321-B-006-011) and by Top University Grant of National Cheng Kung University (grant # D103-35A17).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Author contributions
CWC and PCH performed most experiments; HCW and YLC produced and tested human monoclonal antibody; SCL, BWL, JCL and YJC participated and conducted experiments using clinical samples; HSS and SJT conceived the project; and CWC, HSS and SJT wrote the manuscript. All authors read and approved the final version of manuscript.
Supplementary Information accompanies this paper on the Oncogene website
Supplementary information
Rights and permissions
About this article
Cite this article
Chien, CW., Hou, PC., Wu, HC. et al. Targeting TYRO3 inhibits epithelial–mesenchymal transition and increases drug sensitivity in colon cancer. Oncogene 35, 5872–5881 (2016). https://doi.org/10.1038/onc.2016.120
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2016.120
This article is cited by
-
LINC00858 promotes colon cancer progression through activation of STAT3/5 signaling by recruiting transcription factor RAD21 to upregulate PCNP
Cell Death Discovery (2022)
-
Circ_0000467 Exerts an Oncogenic Role in Colorectal Cancer via miR-330-5p-Dependent Regulation of TYRO3
Biochemical Genetics (2022)
-
Blocking antibody-mediated phosphatidylserine enhances cancer immunotherapy
Journal of Cancer Research and Clinical Oncology (2021)
-
circRAE1 promotes colorectal cancer cell migration and invasion by modulating miR-338-3p/TYRO3 axis
Cancer Cell International (2020)
-
Targeting TAM to Tame Pancreatic Cancer
Targeted Oncology (2020)