Abstract
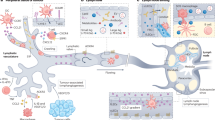
Most cancer patients die as a result of metastasis, thus it is important to understand the molecular mechanisms of dissemination, including intra- and extravasation. Although the mechanisms of extravasation have been vastly studied in vitro and in vivo, the process of intravasation is still unclear. Furthermore, how cells in the tumor microenvironment facilitate tumor cell intravasation is still unknown. Using high-resolution imaging, we found that macrophages enhance tumor cell intravasation upon physical contact. Macrophage and tumor cell contact induce RhoA activity in tumor cells, triggering the formation of actin-rich degradative protrusions called invadopodia, enabling tumor cells to degrade and break through matrix barriers during tumor cell transendothelial migration. Interestingly, we show that macrophage-induced invadopodium formation and tumor cell intravasation also occur in patient-derived tumor cells and in vivo models, revealing a conserved mechanism of tumor cell intravasation. Our results illustrate a novel heterotypic cell contact-mediated signaling role for RhoA, as well as yield mechanistic insight into the ability of cells within the tumor microenvironment to facilitate steps of the metastatic cascade.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Roussos ET, Balsamo M, Alford SK, Wyckoff JB, Gligorijevic B, Wang Y et al. Mena invasive (MenaINV) promotes multicellular streaming motility and transendothelial migration in a mouse model of breast cancer. J Cell Sci 2011; 124 (Pt 13): 2120–2131.
Patsialou A, Bravo-Cordero JJ, Wang Y, Entenberg D, Liu H, Clarke MF et al. Intravital multiphoton imaging reveals multicellular streaming as a crucial component of in vivo cell migration in human breast tumors. IntraVital 2013, (in press).
Wyckoff J, Wang W, Lin EY, Wang Y, Pixley F, Stanley ER et al. A paracrine loop between tumor cells and macrophages is required for tumor cell migration in mammary tumors. Cancer Res 2004; 64: 7022–7029.
Wyckoff JB, Wang Y, Lin EY, Li JF, Goswami S, Stanley ER et al. Direct visualization of macrophage-assisted tumor cell intravasation in mammary tumors. Cancer Res 2007; 67: 2649–2656.
Zervantonakis IK, Hughes-Alford SK, Charest JL, Condeelis JS, Gertler FB, Kamm RD . Three-dimensional microfluidic model for tumor cell intravasation and endothelial barrier function. Proc Natl Acad Sci USA 2012; 109: 13515–13520.
Robinson BD, Sica GL, Liu YF, Rohan TE, Gertler FB, Condeelis JS et al. Tumor microenvironment of metastasis in human breast carcinoma: a potential prognostic marker linked to hematogenous dissemination. Clin Cancer Res 2009; 15: 2433–2441.
Reymond N, Im JH, Garg R, Vega FM, Borda d'Agua B, Riou P et al. Cdc42 promotes transendothelial migration of cancer cells through beta1 integrin. J Cell Biol 2012; 199: 653–668.
Reymond N, Riou P, Ridley AJ . Rho GTPases and cancer cell transendothelial migration. Methods Mol Biol 2012; 827: 123–142.
Jin F, Brockmeier U, Otterbach F, Metzen E . New insight into the SDF-1/CXCR4 axis in a breast carcinoma model: hypoxia-induced endothelial SDF-1 and tumor cell CXCR4 are required for tumor cell intravasation. Molecular Cancer Res 2012; 10: 1021–1031.
Haidari M, Zhang W, Caivano A, Chen Z, Ganjehei L, Mortazavi A et al. Integrin alpha2beta1 mediates tyrosine phosphorylation of vascular endothelial cadherin induced by invasive breast cancer cells. J Biol Chem 2012; 287: 32981–32992.
Haidari M, Zhang W, Chen Z, Ganjehei L, Warier N, Vanderslice P et al. Myosin light chain phosphorylation facilitates monocyte transendothelial migration by dissociating endothelial adherens junctions. Cardiovascular Res 2011; 92: 456–465.
Voura EB, Sandig M, Kalnins VI, Siu C . Cell shape changes and cytoskeleton reorganization during transendothelial migration of human melanoma cells. Cell Tissue Res 1998; 293: 375–387.
Voura EB, Sandig M, Siu CH . Cell-cell interactions during transendothelial migration of tumor cells. Microscopy Res Tech 1998; 43: 265–275.
Stoletov K, Montel V, Lester RD, Gonias SL, Klemke R . High-resolution imaging of the dynamic tumor cell vascular interface in transparent zebrafish. Proc Nat Acad Sci USA 2007; 104: 17406–17411.
Tremblay PL, Auger FA, Huot J . Regulation of transendothelial migration of colon cancer cells by E-selectin-mediated activation of p38 and ERK MAP kinases Oncogene 2006; 25: 6563–6573.
Patsialou A, Wyckoff J, Wang Y, Goswami S, Stanley ER, Condeelis JS . Invasion of human breast cancer cells in vivo requires both paracrine and autocrine loops involving the colony-stimulating factor-1 receptor. Cancer Res 2009; 69: 9498–9506.
Das SK, Stanley ER, Guilbert LJ, Forman LW . Human colony-stimulating factor (CSF-1) radioimmunoassay: resolution of three subclasses of human colony-stimulating factors. Blood 1981; 58: 630–641.
Koop S, MacDonald IC, Luzzi K, Schmidt EE, Morris VL, Grattan M et al. Fate of melanoma cells entering the microcirculation: over 80% survive and extravasate. Cancer Res 1995; 55: 2520–2523.
Kramer RH, Nicolson GL . Interactions of tumor cells with vascular endothelial cell monolayers: a model for metastatic invasion. Proc Natl Acad Sci USA 1979; 76: 5704–5708.
Nicolson GL . Metastatic tumor cell attachment and invasion assay utilizing vascular endothelial cell monolayers. J Histochem Cytochem 1982; 30: 214–220.
Ohigashi H, Shinkai K, Mukai M, Ishikawa O, Imaoka S, Iwanaga T et al. In vitro invasion of endothelial cell monolayer by rat ascites hepatoma cells. Jap J Cancer Res 1989; 80: 818–821.
Proebstl D, Voisin MB, Woodfin A, Whiteford J, D'Acquisto F, Jones GE et al. Pericytes support neutrophil subendothelial cell crawling and breaching of venular walls in vivo. J Exp Med 2012; 209: 1219–1234.
Yu W, Chen J, Xiong Y, Pixley FJ, Dai XM, Yeung YG et al. CSF-1 receptor structure/function in MacCsf1r−/− macrophages: regulation of proliferation, differentiation, and morphology. J Leukoc Biol 2008; 84: 852–863.
Gligorijevic B, Wyckoff J, Yamaguchi H, Wang Y, Roussos ET, Condeelis J . N-WASP-mediated invadopodium formation is involved in intravasation and lung metastasis of mammary tumors. J Cell Sci 2012; 125 (Pt 3): 724–734.
Yamaguchi H . Pathological roles of invadopodia in cancer invasion and metastasis Eur J Cell Biol 2012; 91 (11-12): 902–907.
Saltel F, Daubon T, Juin A, Ganuza IE, Veillat V, Genot E . Invadosomes: intriguing structures with promise. Eur J Cell Biol 2011; 90 (2-3): 100–107.
Linder S, Wiesner C, Himmel M . Degrading devices: invadosomes in proteolytic cell invasion. Ann Rev Cell Dev Biol 2011; 27: 185–211.
Mader CC, Oser M, Magalhaes MA, Bravo-Cordero JJ, Condeelis J, Koleske AJ et al. An EGFR-Src-Arg-cortactin pathway mediates functional maturation of invadopodia and breast cancer cell invasion. Cancer Res 2011; 71: 1730–1741.
Oser M, Mader CC, Gil-Henn H, Magalhaes M, Bravo-Cordero JJ, Koleske AJ et al. Specific tyrosine phosphorylation sites on cortactin regulate Nck1-dependent actin polymerization in invadopodia. J Cell Sci 2010; 123 (Pt 21): 3662–3673.
Seals DF, Azucena EF Jr., Pass I, Tesfay L, Gordon R, Woodrow M et al. The adaptor protein Tks5/Fish is required for podosome formation and function, and for the protease-driven invasion of cancer cells. Cancer Cell 2005; 7: 155–165.
Bowden ET, Barth M, Thomas D, Glazer RI, Mueller SC . An invasion-related complex of cortactin, paxillin and PKCmu associates with invadopodia at sites of extracellular matrix degradation. Oncogene 1999; 18: 4440–4449.
Clark ES, Whigham AS, Yarbrough WG, Weaver AM . Cortactin is an essential regulator of matrix metalloproteinase secretion and extracellular matrix degradation in invadopodia. Cancer Res 2007; 67: 4227–4235.
Magalhaes MA, Larson DR, Mader CC, Bravo-Cordero JJ, Gil-Henn H, Oser M et al. Cortactin phosphorylation regulates cell invasion through a pH-dependent pathway. J Cell Biol 2011; 195: 903–920.
Beaty BT, Sharma VP, Bravo-Cordero JJ, Simpson MA, Eddy RJ, Koleske AJ et al. beta1 integrin regulates Arg to promote invadopodial maturation and matrix degradation. Mol Biol Cell 2013; 24: 1661–1675.
Bravo-Cordero JJ, Marrero-Diaz R, Megias D, Genis L, Garcia-Grande A, Garcia MA et al. MT1-MMP proinvasive activity is regulated by a novel Rab8-dependent exocytic pathway. EMBO J 2007; 26: 1499–1510.
Liu H, Patel MR, Prescher JA, Patsialou A, Qian D, Lin J et al. Cancer stem cells from human breast tumors are involved in spontaneous metastases in orthotopic mouse models. Proc Natl Acad Sci USA 2010; 107: 18115–18120.
Sakurai-Yageta M, Recchi C, Le Dez G, Sibarita JB, Daviet L, Camonis J et al. The interaction of IQGAP1 with the exocyst complex is required for tumor cell invasion downstream of Cdc42 and RhoA. J Cell Biol 2008; 181: 985–998.
Bravo-Cordero JJ, Oser M, Chen X, Eddy R, Hodgson L, Condeelis J . A novel spatiotemporal RhoC activation pathway locally regulates cofilin activity at invadopodia. Curr Biol 2011; 21: 635–644.
Lessey EC, Guilluy C, Burridge K . From mechanical force to RhoA activation. Biochemistry 2012; 51: 7420–7432.
Pertz O, Hodgson L, Klemke RL, Hahn KM . Spatiotemporal dynamics of RhoA activity in migrating cells. Nature 2006; 440: 1069–1072.
Blouw B, Seals DF, Pass I, Diaz B, Courtneidge SA . A role for the podosome/invadopodia scaffold protein Tks5 in tumor growth in vivo. Eur Cell Biol 2008; 87 (8-9): 555–567.
Lovett DH, Cheng S, Cape L, Pollock AS, Mertens PR . YB-1 alters MT1-MMP trafficking and stimulates MCF-7 breast tumor invasion and metastasis. Biochem Biophys Res Commun 2010; 398: 482–488.
Gil-Henn H, Patsialou A, Wang Y, Warren MS, Condeelis JS, Koleske AJ . Arg/Abl2 promotes invasion and attenuates proliferation of breast cancer in vivo. Oncogene 2013; 32: 2622–2630.
Hu Y, Kiely JM, Szente BE, Rosenzweig A, Gimbrone MA Jr. . E-selectin-dependent signaling via the mitogen-activated protein kinase pathway in vascular endothelial cells. J Immunol 2000; 165: 2142–2148.
Hu Y, Szente B, Kiely JM, Gimbrone MA Jr. . Molecular events in transmembrane signaling via E-selectin. SHP2 association, adaptor protein complex formation and ERK1/2 activation. J Biol Chem 2001; 276: 48549–48553.
Laferriere J, Houle F, Taher MM, Valerie K, Huot J . Transendothelial migration of colon carcinoma cells requires expression of E-selectin by endothelial cells and activation of stress-activated protein kinase-2 (SAPK2/p38) in the tumor cells. J Biol Chem 2001; 276: 33762–33772.
Rousseau S, Houle F, Landry J, Huot J . p38 MAP kinase activation by vascular endothelial growth factor mediates actin reorganization and cell migration in human endothelial cells. Oncogene 1997; 15: 2169–2177.
Walz G, Aruffo A, Kolanus W, Bevilacqua M, Seed B . Recognition by ELAM-1 of the sialyl-Lex determinant on myeloid and tumor cells. Science 1990; 250: 1132–1135.
Weiss TW, Mehrabi MR, Kaun C, Zorn G, Kastl SP, Speidl WS et al. Prostaglandin E1 induces vascular endothelial growth factor-1 in human adult cardiac myocytes but not in human adult cardiac fibroblasts via a cAMP-dependent mechanism. J Mol Cell Cardiol 2004; 36: 539–546.
Yoshida M, Takano Y, Sasaoka T, Izumi T, Kimura A . E-selectin polymorphism associated with myocardial infarction causes enhanced leukocyte-endothelial interactions under flow conditions. Arterioscler Thromb Vasc Biol 2003; 23: 783–788.
Li B, Zhao WD, Tan ZM, Fang WG, Zhu L, Chen YH . Involvement of Rho/ROCK signalling in small cell lung cancer migration through human brain microvascular endothelial cells. FEBS Letts 2006; 580: 4252–4260.
McGhee EJ, Morton JP, Von Kriegsheim A, Schwarz JP, Karim SA, Carragher NO et al. FLIM-FRET imaging in vivo reveals 3D-environment spatially regulates RhoGTPase activity during cancer cell invasion. Small GTPases 2011; 2: 239–244.
Timpson P, McGhee EJ, Morton JP, von Kriegsheim A, Schwarz JP, Karim SA et al. Spatial regulation of RhoA activity during pancreatic cancer cell invasion driven by mutant p53. Cancer Res 2011; 71: 747–757.
Carmona-Fontaine C, Matthews HK, Kuriyama S, Moreno M, Dunn GA, Parsons M et al. Contact inhibition of locomotion in vivo controls neural crest directional migration. Nature 2008; 456: 957–961.
Ponik SM, Trier SM, Wozniak MA, Eliceiri KW, Keely PJ . RhoA is down-regulated at cell-cell contacts via p190RhoGAP-B in response to tensional homeostasis. Mol Biol Cell 2013; 24: 1688–1699.
Witzel S, Zimyanin V, Carreira-Barbosa F, Tada M, Heisenberg CP . Wnt11 controls cell contact persistence by local accumulation of Frizzled 7 at the plasma membrane. J Cell Biol 2006; 175: 791–802.
Arthur WT, Noren NK, Burridge K . Regulation of Rho family GTPases by cell-cell and cell-matrix adhesion. Biol Res 2002; 35: 239–246.
Nethe M, de Kreuk BJ, Tauriello DV, Anthony EC, Snoek B, Stumpel T et al. Rac1 acts in conjunction with Nedd4 and dishevelled-1 to promote maturation of cell-cell contacts. J Cell Sci 2012; 125 (Pt 14): 3430–3442.
Omelchenko T, Hall A . Myosin-IXA regulates collective epithelial cell migration by targeting RhoGAP activity to cell-cell junctions. Curr Biol 2012; 22: 278–288.
Sharma VP, DesMarais V, Sumners C, Shaw G, Narang A . Immunostaining evidence for PI(4,5)P2 localization at the leading edge of chemoattractant-stimulated HL-60 cells. J Leukoc Biol 2008; 84: 440–447.
Sharma VP, Entenberg D, Condeelis J . High-resolution live-cell imaging and time-lapse microscopy of invadopodium dynamics and tracking analysis. Methods Mol Biol 2013; 1046: 343–357.
Lipschutz JH, O'Brien LE, Altschuler Y, Avrahami D, Nguyen Y, Tang K et al. Analysis of membrane traffic in polarized epithelial cells. Curr Protoc Cell BiolS 2001. 15.5.1–15.5.18.
Spiering D, Hodgson L . Multiplex imaging of Rho family GTPase activities in living cells. Methods Mol Biol 2012; 827: 215–234.
Acknowledgements
We thank Brian Beaty for advice regarding invadopodium experiments; David Entenberg, Vera Desmarais, Jeffrey Wyckoff and the Analytical Imaging Facility for help with microscopy; Richard Stanley, Fernando Macian, Esther Arwert, Allison Harney and Veronika Micolski for guidance and reagents; Yarong Wang for help with animal injections; and the Albert Einstein shRNA Core, the Flow Cytometry Core facility and the Histology and Comparative Pathology Core for help with experiments. We also thank Jeffrey Segall, Dianne Cox, Anne Bresnick and Aviv Bergmann for helpful discussions, and the Condeelis, Segall, Cox and Hodgson labs for advice and reagents. This work was funded by NIH CA150344 (JC), NIH CA100324 (AP), NIH GM093121 (LH and JJB-C), Post-doctoral fellowship from Susan G. Komen for the Cure© KG111405 (VPS) and NIH CA159663 (MRJ).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
JC holds equity in and is a member of the Scientific Advisory Board of MetaStat, Inc.
Additional information
Author Contributions
MR-J and JC conceived the project idea. MR-J, JJB-C and LH performed RhoA biosensor experiments; LH cloned RhoA mutant constructs; AP maintained TN1-GFP cells, created the MDA-MB-231 dtomato cell line and performed qRT-PCR; VPS optimized protocols regarding invadopodium assays and helped with microscopy; PG and MR-J performed IMARIS 3D reconstructions; and HL created the TN1-GFP cells. MR-J performed the rest of the experiments. All authors contributed to discussions related to the manuscript. MR-J and JC wrote the manuscript.
Supplementary Information accompanies this paper on the Oncogene website
Rights and permissions
About this article
Cite this article
Roh-Johnson, M., Bravo-Cordero, J., Patsialou, A. et al. Macrophage contact induces RhoA GTPase signaling to trigger tumor cell intravasation. Oncogene 33, 4203–4212 (2014). https://doi.org/10.1038/onc.2013.377
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2013.377
Keywords
This article is cited by
-
The Role of Tumor Epithelial-Mesenchymal Transition and Macrophage Crosstalk in Cancer Progression
Current Osteoporosis Reports (2023)
-
Invadopodia play a role in prostate cancer progression
BMC Cancer (2022)
-
Simple and automatic monitoring of cancer cell invasion into an epithelial monolayer using label-free holographic microscopy
Scientific Reports (2022)
-
Macrophages in multiple myeloma: key roles and therapeutic strategies
Cancer and Metastasis Reviews (2021)
-
A bi-directional dialog between vascular cells and monocytes/macrophages regulates tumor progression
Cancer and Metastasis Reviews (2021)