Abstract
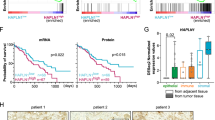
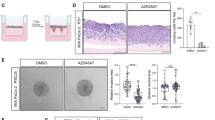
Heparan sulfate proteoglycans are an important and abundant component of the extracellular matrix, which undergo substantial remodeling throughout tumorigenesis via the enzymatic activity of heparanase. Heparanase has been shown to be upregulated in many human cancers; however, its specific functions in human pancreatic neuroendocrine tumors (PanNETs) and spontaneous mouse models of cancer have not been evaluated. Here, we investigated the role of heparanase in PanNETs using patient samples and the RIP1-Tag2 (RT2) PanNET-transgenic mouse model. High heparanase expression significantly correlated with more advanced tumor stage, higher tumor grade and the presence of distant metastasis in PanNET patients. We genetically manipulated heparanase levels in the RT2 model using heparanase-transgenic mice, which constitutively overexpress heparanase, and heparanase-knockout mice. Heparanase was found to have a critical role in promoting tumor invasion, through both macrophage and cancer cell sources in the tumor microenvironment. In addition, elevated heparanase levels significantly increased peritumoral lymphangiogenesis in vivo and promoted the trans-differentiation of macrophages into lymphatic endothelial cell-like structures in culture. Conversely, we found that heparanase deletion led to increased angiogenesis and pericyte coverage. Together, these data identify important roles for heparanase in regulating several critical aspects of tumorigenesis, demonstrating that heparanase represents a potential therapeutic target for PanNET patients.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Joyce JA, Pollard JW . Microenvironmental regulation of metastasis. Nat Rev Cancer 2009; 9: 239–252.
Vlodavsky I, Beckhove P, Lerner I, Pisano C, Meirovitz A, Ilan N et al. Significance of heparanase in cancer and inflammation. Cancer Microenvironment 2012; 5: 115–132.
Joyce JA, Freeman C, Meyer-Morse N, Parish CR, Hanahan D . A functional heparan sulfate mimetic implicates both heparanase and heparan sulfate in tumor angiogenesis and invasion in a mouse model of multistage cancer. Oncogene 2005; 24: 4037–4051.
Yao JC, Eisner MP, Leary C, Dagohoy C, Phan A, Rashid A et al. Population-based study of islet cell carcinoma. Ann Surg Oncol 2007; 14: 3492–3500.
Yao JC, Hassan M, Phan A, Dagohoy C, Leary C, Mares JE et al. One hundred years after "carcinoid": epidemiology of and prognostic factors for neuroendocrine tumors in 35,825 cases in the United States. J Clin Oncol 2008; 26: 3063–3072.
Jiao Y, Shi C, Edil BH, de Wilde RF, Klimstra DS, Maitra A et al. DAXX/ATRX, MEN1, and mTOR pathway genes are frequently altered in pancreatic neuroendocrine tumors. Science 2011; 331: 1199–1203.
Edge SB, Compton CC . The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol 2010; 17: 1471–1474.
Ferrone CR, Tang LH, Tomlinson J, Gonen M, Hochwald SN, Brennan MF et al. Determining prognosis in patients with pancreatic endocrine neoplasms: can the WHO classification system be simplified? J Clin Oncol 2007; 25: 5609–5615.
Nolan-Stevaux O, Truitt MC, Pahler JC, Olson P, Guinto C, Lee DC et al. Differential contribution to neuroendocrine tumorigenesis of parallel EGFR signaling in cancer cells and pericytes. Genes Cancer 2010; 1: 125–141.
Tuveson D, Hanahan D . Translational medicine: cancer lessons from mice to humans. Nature 2011; 471: 316–317.
Zcharia E, Jia J, Zhang X, Baraz L, Lindahl U, Peretz T et al. Newly generated heparanase knock-out mice unravel co-regulation of heparanase and matrix metalloproteinases. PloS One 2009; 4: e5181.
Zcharia E, Metzger S, Chajek-Shaul T, Aingorn H, Elkin M, Friedmann Y et al. Transgenic expression of mammalian heparanase uncovers physiological functions of heparan sulfate in tissue morphogenesis, vascularization, and feeding behavior. FASEB J 2004; 18: 252–263.
Lopez T, Hanahan D . Elevated levels of IGF-1 receptor convey invasive and metastatic capability in a mouse model of pancreatic islet tumorigenesis. Cancer Cell 2002; 1: 339–353.
Pyonteck SM, Gadea BB, Wang HW, Gocheva V, Hunter KE, Tang LH et al. Deficiency of the macrophage growth factor CSF-1 disrupts pancreatic neuroendocrine tumor development. Oncogene 2012; 31: 1459–1467.
Gocheva V, Wang HW, Gadea BB, Shree T, Hunter KE, Garfall AL et al. IL-4 induces cathepsin protease activity in tumor-associated macrophages to promote cancer growth and invasion. Genes Dev 2010; 24: 241–255.
Mandriota SJ, Jussila L, Jeltsch M, Compagni A, Baetens D, Prevo R et al. Vascular endothelial growth factor-C-mediated lymphangiogenesis promotes tumour metastasis. EMBO J 2001; 20: 672–682.
Zumsteg A, Christofori G . Myeloid cells and lymphangiogenesis. Cold Spring Harb Perspect Med 2012; 2: a006494.
Zumsteg A, Baeriswyl V, Imaizumi N, Schwendener R, Ruegg C, Christofori G . Myeloid cells contribute to tumor lymphangiogenesis. PloS One 2009; 4: e7067.
Maruyama K, Ii M, Cursiefen C, Jackson DG, Keino H, Tomita M et al. Inflammation-induced lymphangiogenesis in the cornea arises from CD11b-positive macrophages. J Clin Invest 2005; 115: 2363–2372.
Tammela T, Alitalo K . Lymphangiogenesis: molecular mechanisms and future promise. Cell 2010; 140: 460–476.
Parish CR, Freeman C, Brown KJ, Francis DJ, Cowden WB . Identification of sulfated oligosaccharide-based inhibitors of tumor growth and metastasis using novel in vitro assays for angiogenesis and heparanase activity. Cancer Res 1999; 59: 3433–3441.
Ori A, Wilkinson MC, Fernig DG . A systems biology approach for the investigation of the heparin/heparan sulfate interactome. J Biol Chem 2011; 286: 19892–19904.
Lindahl U, Li JP . Interactions between heparan sulfate and proteins-design and functional implications. Int Rev Cell Mol Biol 2009; 276: 105–159.
Arvatz G, Shafat I, Levy-Adam F, Ilan N, Vlodavsky I . The heparanase system and tumor metastasis: is heparanase the seed and soil? Cancer Metastasis Rev 2011; 30: 253–268.
Stenzel D, Nye E, Nisancioglu M, Adams RH, Yamaguchi Y, Gerhardt H . Peripheral mural cell recruitment requires cell-autonomous heparan sulfate. Blood 2009; 114: 915–924.
Cohen-Kaplan V, Naroditsky I, Zetser A, Ilan N, Vlodavsky I, Doweck I . Heparanase induces VEGF C and facilitates tumor lymphangiogenesis. Int J Cancer 2008; 123: 2566–2573.
Hanahan D . Heritable formation of pancreatic beta-cell tumours in transgenic mice expressing recombinant insulin/simian virus 40 oncogenes. Nature 1985; 315: 115–122.
Okabe M, Ikawa M, Kominami K, Nakanishi T, Nishimune Y . 'Green mice' as a source of ubiquitous green cells. FEBS Lett 1997; 407: 313–319.
Hu W, Feng Z, Modica I, Klimstra DS, Song L, Allen PJ et al. Gene Amplifications in well-differentiated pancreatic neuroendocrine tumors inactivate the p53 pathway. Genes Cancer 2010; 1: 360–368.
Mccullagh P . Regression-models for ordinal data. J Roy Stat Soc B Met 1980; 42: 109–142.
Acknowledgements
We thank members of the Joyce Lab; Drs Jacqueline Bromberg and Andrew Koff for discussion on this topic; and Robert Bowman, Daniela Quail, Alberto Schuhmacher and Hao-Wei Wang for reading the manuscript. We gratefully acknowledge Xiaoping Chen and Lin Song for excellent technical assistance; Marsha Quick and Karoline Dubin for project assistance; Elyn Reidel, MSKCC Epidemiology and Biostatistics Department for statistical analysis of RT2 tumor grades; Sho Fujisawa and the Molecular Cytology Core Facility for assistance with the MetaMorph lymphangiogenesis analysis; the MSKCC Flow Cytometry Core for technical assistance and advice; and Aisha Khan of the cGMP Cell Processing Facility, Cell Transplant Center, Diabetes Research Institute, University of Miami School of Medicine for providing normal islets. This research was funded by the National Cancer Institute R01 CA125162 and Cycle for Survival (JAJ). KEH was supported in part by a Grayer Fellowship.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Oncogene website
Supplementary information
Rights and permissions
About this article
Cite this article
Hunter, K., Palermo, C., Kester, J. et al. Heparanase promotes lymphangiogenesis and tumor invasion in pancreatic neuroendocrine tumors. Oncogene 33, 1799–1808 (2014). https://doi.org/10.1038/onc.2013.142
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2013.142
Keywords
This article is cited by
-
Identification of a novel lymphangiogenesis signature associated with immune cell infiltration in colorectal cancer based on bioinformatics analysis
BMC Medical Genomics (2024)
-
Extracellular matrix remodeling in tumor progression and immune escape: from mechanisms to treatments
Molecular Cancer (2023)
-
PTEN regulates invasiveness in pancreatic neuroendocrine tumors through DUSP19-mediated VEGFR3 dephosphorylation
Journal of Biomedical Science (2022)
-
Heparanase and the hallmarks of cancer
Journal of Translational Medicine (2020)
-
TAMing pancreatic cancer: combat with a double edged sword
Molecular Cancer (2019)