Abstract
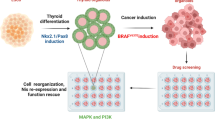
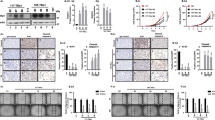
Thyroid cancers are the most common malignancy of the endocrine system in humans. To understand the molecular genetic events underlying thyroid carcinogenesis, we have generated a mouse model that spontaneously develops follicular thyroid carcinoma similar to human thyroid cancer (ThrbPV/PV mouse). This mutant mouse harbors a dominant-negative mutated thyroid hormone receptor β (denoted PV). The PV mutation was identified in a patient with resistance to thyroid hormone (TH). ThrbPV/PV mice exhibit highly elevated serum thyroid-stimulating hormone levels and increased TH. We have previously shown that thyroid-stimulating hormone is required, but not sufficient to induce metastatic follicular thyroid cancer in ThrbPV/PV mice. However, whether the elevated TH also contributes to the thyroid carcinogenesis of ThrbPV/PV mice was not elucidated. To understand the role of TH in thyroid carcinogenesis, we blocked the production of TH by treating ThrbPV/PV mice with propylthiouracil (ThrbPV/PV-PTU mice) and compared the development of thyroid cancer in ThrbPV/PV-PTU and untreated ThrbPV/PV mice. We found that thyroid tumor growth was reduced by ∼42% in ThrbPV/PV-PTU mice as compared with ThrbPV/PV mice. Analysis by bromodeoxyuridine-nuclear labeling showed decreased incorporation of bromodeoxyuridine in thyroid tumor cells of ThrbPV/PV-PTU mice, indicative of decreased tumor cell proliferation. However, cleaved-caspase 3 staining showed no apparent changes in apoptosis of tumor cells in ThrbPV/PV-PTU mice. Molecular studies identified a marked attenuation of the PI3K–AKT–β-catenin signaling pathway that led to decreased protein levels of cyclin D2, thereby decreasing tumor cell proliferation in ThrbPV/PV-PTU mice. Furthermore, matrix metalloproteinase-2, a downstream target of β-catenin and a key regulator during tumor invasion and metastasis, was also decreased. Thus, the present study uncovers a critical role of TH in promoting the thyroid carcinogenesis of ThrbPV/PV mice via membrane signaling events. Importantly, these findings suggest that anti-thyroid drugs could be considered as possible therapeutic agents of thyroid cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Abbosh PH, Nephew KP . (2005). Multiple signaling pathways converge on beta-catenin in thyroid cancer. Thyroid 15: 551–561.
Antico-Arciuch VG, Dima M, Liao XH, Refetoff S, Di Cristofano A . (2010). Cross-talk between PI3K and estrogen in the mouse thyroid predisposes to the development of follicular carcinomas with a higher incidence in females. Oncogene 29: 5678–5686.
Bergh JJ, Lin HY, Lansing L, Mohamed SN, Davis FB, Mousa S et al. (2005). Integrin alphaVbeta3 contains a cell surface receptor site for thyroid hormone that is linked to activation of mitogen-activated protein kinase and induction of angiogenesis. Endocrinology 146: 2864–2871.
Boelaert K, McCabe CJ, Tannahill LA, Gittoes NJ, Holder RL, Watkinson JC et al. (2003). Pituitary tumor transforming gene and fibroblast growth factor-2 expression: potential prognostic indicators in differentiated thyroid cancer. J Clin Endocrinol Metab 88: 2341–2347.
Cao X, Kambe F, Moeller LC, Refetoff S, Seo H . (2005). Thyroid hormone induces rapid activation of Akt/protein kinase B-mammalian target of rapamycin-p70S6K cascade through phosphatidylinositol 3-kinase in human fibroblasts. Mol Endocrinol 19: 102–112.
Castellone MD, De Falco V, Rao DM, Bellelli R, Muthu M, Basolo F et al. (2009). The beta-catenin axis integrates multiple signals downstream from RET/papillary thyroid carcinoma leading to cell proliferation. Cancer Res 69: 1867–1876.
Cheng SY, Leonard JL, Davis PJ . (2010). Molecular aspects of thyroid hormone actions. Endocr Rev 31: 139–170.
Cole AM, Myant K, Reed KR, Ridgway RA, Athineos D, Van den Brink GR et al. (2010). Cyclin D2-cyclin-dependent kinase 4/6 is required for efficient proliferation and tumorigenesis following Apc loss. Cancer Res 70: 8149–8158.
Davies L, Welch HG . (2006). Increasing incidence of thyroid cancer in the United States, 1973–2002. JAMA 295: 2164–2167.
Davis FB, Mousa SA, O'Connor L, Mohamed S, Lin HY, Cao HJ et al. (2004). Proangiogenic action of thyroid hormone is fibroblast growth factor-dependent and is initiated at the cell surface. Circ Res 94: 1500–1506.
Davis PJ, Davis FB, Lin H-Y, Mousa SA, Zhou M, Luidens MK . (2009). Translational implications of nongenomic actions of thyroid hormone initiated at its integrin receptor. Am J Physiol Endocrinol Metabol 297: E1238–E1246.
Fang D, Hawke D, Zheng Y, Xia Y, Meisenhelder J, Nika H et al. (2007). Phosphorylation of beta-catenin by AKT promotes beta-catenin transcriptional activity. J Biol Chem 282: 11221–11229.
Furumoto H, Ying H, Chandramouli GV, Zhao L, Walker RL, Meltzer PS et al. (2005). An unliganded thyroid hormone beta receptor activates the cyclin D1/cyclin-dependent kinase/retinoblastoma/E2F pathway and induces pituitary tumorigenesis. Mol Cell Biol 25: 124–135.
Furuya F, Hanover JA, Cheng SY . (2006). Activation of phosphatidylinositol 3-kinase signaling by a mutant thyroid hormone beta receptor. Proc Natl Acad Sci USA 103: 1780–1785.
Furuya F, Lu C, Willingham MC, Cheng SY . (2007). Inhibition of phosphatidylinositol 3-kinase delays tumor progression and blocks metastatic spread in a mouse model of thyroid cancer. Carcinogenesis 28: 2451–2458.
Glinskii AB, Glinsky GV, Lin HY, Tang HY, Sun M, Davis FB et al. (2009). Modification of survival pathway gene expression in human breast cancer cells by tetraiodothyroacetic acid (tetrac). Cell Cycle 8: 3554–3562.
Guigon CJ, Cheng SY . (2009). Novel non-genomic signaling of thyroid hormone receptors in thyroid carcinogenesis. Mol Cell Endocrinol 308: 63–69.
Guigon CJ, Kim DW, Zhu X, Zhao L, Cheng SY . (2010). Tumor suppressor action of liganded thyroid hormone receptor beta by direct repression of beta-catenin gene expression. Endocrinology 151: 5528–5536.
Guigon CJ, Zhao L, Lu C, Willingham MC, Cheng SY . (2008). Regulation of beta-catenin by a novel nongenomic action of thyroid hormone beta receptor. Mol Cell Biol 28: 4598–4608.
Hou P, Liu D, Shan Y, Hu S, Studeman K, Condouris S et al. (2007). Genetic alterations and their relationship in the phosphatidylinositol 3-kinase/Akt pathway in thyroid cancer. Clin Cancer Res 13: 1161–1170.
Kaneshige M, Kaneshige K, Zhu X, Dace A, Garrett L, Carter TA et al. (2000). Mice with a targeted mutation in the thyroid hormone beta receptor gene exhibit impaired growth and resistance to thyroid hormone. Proc Natl Acad Sci USA 97: 13209–13214.
Keniry M, Parsons R . (2008). The role of PTEN signaling perturbations in cancer and in targeted therapy. Oncogene 27: 5477–5485.
Kessenbrock K, Plaks V, Werb Z . (2010). Matrix metalloproteinases: regulators of the tumor microenvironment. Cell 141: 52–67.
Kim CS, Ying H, Willingham MC, Cheng SY . (2007). The pituitary tumor-transforming gene promotes angiogenesis in a mouse model of follicular thyroid cancer. Carcinogenesis 28: 932–939.
Liang J, Slingerland JM . (2003). Multiple roles of the PI3K/PKB (Akt) pathway in cell cycle progression. Cell Cycle 2: 339–345.
Lin HY, Sun M, Tang HY, Lin C, Luidens MK, Mousa SA et al. (2009). L-Thyroxine vs 3,5,3′-triiodo-L-thyronine and cell proliferation: activation of mitogen-activated protein kinase and phosphatidylinositol 3-kinase. Am J Physiol Cell Physiol 296: C980–C991.
Lin HY, Tang HY, Shih A, Keating T, Cao G, Davis PJ et al. (2007). Thyroid hormone is a MAPK-dependent growth factor for thyroid cancer cells and is anti-apoptotic. Steroids 72: 180–187.
Lu C, Cheng SY . (2011). Extranuclear signaling of mutated thyroid hormone receptors in promoting metastatic spread in thyroid carcinogenesis. Steroids 76: 885–891.
Lu C, Mishra A, Zhu YJ, Meltzer P, Cheng SY . (2011). Genomic profiling of genes contributing to metastasis in a mouse model of thyroid follicular carcinoma. Am J Cancer Res 1: 1–13.
Lu C, Zhao L, Ying H, Willingham MC, Cheng SY . (2010). Growth activation alone is not sufficient to cause metastatic thyroid cancer in a mouse model of follicular thyroid carcinoma. Endocrinology 151: 1929–1939.
Mousa SA, Davis FB, Mohamed S, Davis PJ, Feng X . (2006). Pro-angiogenesis action of thyroid hormone and analogs in a three-dimensional in vitro microvascular endothelial sprouting model. Int Angiol 25: 407–413.
Nikiforov YE . (2004). Genetic alterations involved in the transition from well-differentiated to poorly differentiated and anaplastic thyroid carcinomas. Endocr Pathol 15: 319–327.
Nikiforova MN, Nikiforov YE . (2009). Molecular diagnostics and predictors in thyroid cancer. Thyroid 19: 1351–1361.
Ono S, Schwartz ID, Mueller OT, Root AW, Usala SJ, Bercu BB . (1991). Homozygosity for a dominant negative thyroid hormone receptor gene responsible for generalized resistance to thyroid hormone. J Clin Endocrinol Metab 73: 990–994.
Parrilla R, Mixson AJ, McPherson JA, McClaskey JH, Weintraub BD . (1991). Characterization of seven novel mutations of the c-erbA beta gene in unrelated kindreds with generalized thyroid hormone resistance. Evidence for two ‘hot spot’ regions of the ligand binding domain. J Clin Invest 88: 2123–2130.
Puxeddu E, Romagnoli S, Dottorini ME . (2011). Targeted therapies for advanced thyroid cancer. Curr Opin Oncol 23: 13–21.
Rego-Iraeta A, Perez-Mendez LF, Mantinan B, Garcia-Mayor RV . (2009). Time trends for thyroid cancer in northwestern Spain: true rise in the incidence of micro and larger forms of papillary thyroid carcinoma. Thyroid 19: 333–340.
Rowlands TM, Pechenkina IV, Hatsell S, Cowin P . (2004). Beta-catenin and cyclin D1: connecting development to breast cancer. Cell Cycle 3: 145–148.
Saji M, Ringel MD . (2010). The PI3K-Akt-mTOR pathway in initiation and progression of thyroid tumors. Mol Cell Endocrinol 321: 20–28.
Sassolas G, Hafdi-Nejjari Z, Remontet L, Bossard N, Belot A, Berger-Dutrieux N et al. (2009). Thyroid cancer: is the incidence rise abating? Eur J Endocrinol 160: 71–79.
Sipos JA, Mazzaferri EL . (2010). Thyroid cancer epidemiology and prognostic variables. Clin Oncol (R Coll Radiol) 22: 395–404.
Sonderegger S, Haslinger P, Sabri A, Leisser C, Otten JV, Fiala C et al. (2010). Wingless (Wnt)-3A induces trophoblast migration and matrix metalloproteinase-2 secretion through canonical Wnt signaling and protein kinase B/AKT activation. Endocrinology 151: 211–220.
Suzuki H, Willingham MC, Cheng SY . (2002). Mice with a mutation in the thyroid hormone receptor beta gene spontaneously develop thyroid carcinoma: a mouse model of thyroid carcinogenesis. Thyroid 12: 963–969.
Verga Falzacappa C, Petrucci E, Patriarca V, Michienzi S, Stigliano A, Brunetti E et al. (2007). Thyroid hormone receptor TRbeta1 mediates Akt activation by T3 in pancreatic beta cells. J Mol Endocrinol 38: 221–233.
Weinberger PM, Adam BL, Gourin CG, Moretz 3rd WH, Bollag RJ, Wang BY et al. (2007). Association of nuclear, cytoplasmic expression of galectin-3 with beta-catenin/Wnt-pathway activation in thyroid carcinoma. Arch Otolaryngol Head Neck Surg 133: 503–510.
Xing M . (2010). Genetic alterations in the phosphatidylinositol-3 kinase/Akt pathway in thyroid cancer. Thyroid 20: 697–706.
Yalcin M, Bharali DJ, Dyskin E, Dier E, Lansing L, Mousa SS et al. (2010). Tetraiodothyroacetic acid and tetraiodothyroacetic acid nanoparticle effectively inhibit the growth of human follicular thyroid cell carcinoma. Thyroid 20: 281–286.
Ying H, Furuya F, Zhao L, Araki O, West BL, Hanover JA et al. (2006). Aberrant accumulation of PTTG1 induced by a mutated thyroid hormone beta receptor inhibits mitotic progression. J Clin Invest 116: 2972–2984.
Ying H, Suzuki H, Zhao L, Willingham MC, Meltzer P, Cheng SY . (2003). Mutant thyroid hormone receptor beta represses the expression and transcriptional activity of peroxisome proliferator-activated receptor gamma during thyroid carcinogenesis. Cancer Res 63: 5274–5280.
Ying H, Willingham MC, Cheng SY . (2008). The steroid receptor coactivator-3 is a tumor promoter in a mouse model of thyroid cancer. Oncogene 27: 823–830.
Acknowledgements
This research was supported by the Intramural Research Program of National Institutes of Health, National Cancer Institute, Center for Cancer Research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Oncogene website
Supplementary information
Rights and permissions
About this article
Cite this article
Lu, C., Zhu, X., Willingham, M. et al. Activation of tumor cell proliferation by thyroid hormone in a mouse model of follicular thyroid carcinoma. Oncogene 31, 2007–2016 (2012). https://doi.org/10.1038/onc.2011.390
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2011.390