Abstract
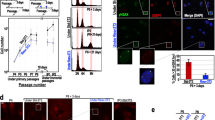
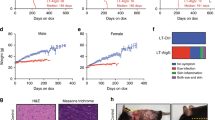
The function of the class III histone deacetylase, Sir2, in promoting lifespan extension is well established in small model organisms. By analogy, SirT1, the mammalian orthologue of Sir2, is a candidate gene to slow down aging and forestall the onset of age-associated diseases. We have used SirT1-null mice to study the function of SirT1 in susceptibility to tumorigenesis. The number of intestinal polyps induced in mice carrying the Apcmin mutation was unaffected by the SirT1 genotype although the average polyp size was slightly smaller in the SirT1-null animals. Similarly, the presence or absence of SirT1 had no effect on incidence and tumor load of skin papillomas induced by the classical two-stage carcinogenesis protocol. We found that resveratrol topically applied to the skin profoundly reduced tumorigenesis. This chemoprotective effect was significantly reduced but not ablated in SirT1-null mice, suggesting that part of the protection afforded by resveratrol requires the SirT1-encoded protein. Thus, our results suggest that SirT1 does not behave like a classical tumor-suppressor gene but the antitumor activity of resveratrol is mediated at least in part by SirT1.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 50 print issues and online access
$259.00 per year
only $5.18 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Abdelmohsen K, Pullmann Jr. R, Lal A, Kim HH, Galban S, Yang X et al. (2007). Phosphorylation of HuR by Chk2 regulates SIRT1 expression. Mol Cell 25: 543–557.
Araki T, Sasaki Y, Milbrandt J . (2004). Increased nuclear NAD biosynthesis and SIRT1 activation prevent axonal degeneration. Science 305: 1010–1013.
Boily G, Seifert EL, Bevilacqua L, He XH, Sabourin G, Estey C et al. (2008). SirT1 regulates energy metabolism and response to caloric restriction in mice. PLoS ONE 3: e1759.
Bordone L, Motta MC, Picard F, Robinson A, Jhala US, Apfeld J et al. (2006). Sirt1 regulates insulin secretion by repressing UCP2 in pancreatic beta cells. PLoS Biol 4: e31.
Borra MT, Smith BC, Denu JM . (2005). Mechanism of human SIRT1 activation by resveratrol. J Biol Chem 280: 17187–17195.
Bradbury CA, Khanim FL, Hayden R, Bunce CM, White DA, Drayson MT et al. (2005). Histone deacetylases in acute myeloid leukaemia show a distinctive pattern of expression that changes selectively in response to deacetylase inhibitors. Leukemia 19: 1751–1759.
Chen J, Zhou Y, Mueller-Steiner S, Chen LF, Kwon H, Yi S et al. (2005a). SIRT1 protects against microglia-dependent amyloid-beta toxicity through inhibiting NF-kappaB signaling. J Biol Chem 280: 40364–40374.
Chen WY, Wang DH, Yen RC, Luo J, Gu W, Baylin SB . (2005b). Tumor suppressor HIC1 directly regulates SIRT1 to modulate p53-dependent DNA-damage responses. Cell 123: 437–448.
Cheng HL, Mostoslavsky R, Saito S, Manis JP, Gu Y, Patel P et al. (2003). Developmental defects and p53 hyperacetylation in Sir2 homolog (SIRT1)-deficient mice. Proc Natl Acad Sci USA 100: 10794–10799.
Chua KF, Mostoslavsky R, Lombard DB, Pang WW, Saito S, Franco S et al. (2005). Mammalian SIRT1 limits replicative life span in response to chronic genotoxic stress. Cell Metab 2: 67–76.
Cucciolla V, Borriello A, Oliva A, Galletti P, Zappia V, Della Ragione F . (2007). Resveratrol: from basic science to the clinic. Cell Cycle 6: 2495–2510.
Dai JM, Wang ZY, Sun DC, Lin RX, Wang SQ . (2007). SIRT1 interacts with p73 and suppresses p73-dependent transcriptional activity. J Cell Physiol 210: 161–166.
Duan C, Xu Q . (2005). Roles of insulin-like growth factor (IGF) binding proteins in regulating IGF actions. Gen Comp Endocrinol 142: 44–52.
Firestein R, Blander G, Michan S, Oberdoerffer P, Ogino S, Campbell J et al. (2008). The SIRT1 deacetylase suppresses intestinal tumorigenesis and colon cancer growth. PLoS ONE 3: e2020.
Ford J, Jiang M, Milner J . (2005). Cancer-specific functions of SIRT1 enable human epithelial cancer cell growth and survival. Cancer Res 65: 10457–10463.
Fu M, Liu M, Sauve AA, Jiao X, Zhang X, Wu X et al. (2006). Hormonal control of androgen receptor function through SIRT1. Mol Cell Biol 26: 8122–8135.
Gerhart-Hines Z, Rodgers JT, Bare O, Lerin C, Kim SH, Mostoslavsky R et al. (2007). Metabolic control of muscle mitochondrial function and fatty acid oxidation through SIRT1/PGC-1alpha. EMBO J 26: 1913–1923.
Hida Y, Kubo Y, Murao K, Arase S . (2007). Strong expression of a longevity-related protein, SIRT1, in Bowen's disease. Arch Dermatol Res 299: 103–106.
Howitz KT, Bitterman KJ, Cohen HY, Lamming DW, Lavu S, Wood JG et al. (2003). Small molecule activators of sirtuins extend Saccharomyces cerevisiae lifespan. Nature 425: 191–196.
Huang J, Gan Q, Han L, Li J, Zhang H, Sun Y et al. (2008). SIRT1 overexpression antagonizes cellular senescence with activated ERK/S6k1 signaling in human diploid fibroblasts. PLoS ONE 3: e1710.
Huffman DM, Grizzle WE, Bamman MM, Kim JS, Eltoum IA, Elgavish A et al. (2007). SIRT1 is significantly elevated in mouse and human prostate cancer. Cancer Res 67: 6612–6618.
Jang KY, Hwang SH, Kwon KS, Kim KR, Choi HN, Lee NR et al. (2008). SIRT1 expression is associated with poor prognosis of diffuse large B-cell lymphoma. Am J Surg Pathol 32: 1523–1531.
Jang M, Cai L, Udeani GO, Slowing KV, Thomas CF, Beecher CW et al. (1997). Cancer chemopreventive activity of resveratrol, a natural product derived from grapes. Science 275: 218–220.
Kaeberlein M, McDonagh T, Heltweg B, Hixon J, Westman EA, Caldwell SD et al. (2005). Substrate-specific activation of sirtuins by resveratrol. J Biol Chem 280: 17038–17045.
Kaeberlein M, McVey M, Guarente L . (1999). The SIR2/3/4 complex and SIR2 alone promote longevity in Saccharomyces cerevisiae by two different mechanisms. Genes Dev 13: 2570–2580.
Kim D, Nguyen MD, Dobbin MM, Fischer A, Sananbenesi F, Rodgers JT et al. (2007). SIRT1 deacetylase protects against neurodegeneration in models for Alzheimer's disease and amyotrophic lateral sclerosis. EMBO J 26: 3169–3179.
Kitamura YI, Kitamura T, Kruse JP, Raum JC, Stein R, Gu W et al. (2005). FoxO1 protects against pancreatic beta cell failure through NeuroD and MafA induction. Cell Metab 2: 153–163.
Kundu JK, Shin YK, Surh YJ . (2006). Resveratrol modulates phorbol ester-induced pro-inflammatory signal transduction pathways in mouse skin in vivo: NF-kappaB and AP-1 as prime targets. Biochem Pharmacol 72: 1506–1515.
Kuzmichev A, Margueron R, Vaquero A, Preissner TS, Scher M, Kirmizis A et al. (2005). Composition and histone substrates of polycomb repressive group complexes change during cellular differentiation. Proc Natl Acad Sci USA 102: 1859–1864.
Langley E, Pearson M, Faretta M, Bauer UM, Frye RA, Minucci S et al. (2002). Human SIR2 deacetylates p53 and antagonizes PML/p53-induced cellular senescence. EMBO J 21: 2383–2396.
Lemieux ME, Yang X, Jardine K, He X, Jacobsen KX, Staines WA et al. (2005). The Sirt1 deacetylase modulates the insulin-like growth factor signaling pathway in mammals. Mech Ageing Dev 126: 1097–1105.
Lin SJ, Defossez PA, Guarente L . (2000). Requirement of NAD and SIR2 for life-span extension by calorie restriction in Saccharomyces cerevisiae. Science 289: 2126–2128.
Luo J, Nikolaev AY, Imai S, Chen D, Su F, Shiloh A et al. (2001). Negative control of p53 by Sir2alpha promotes cell survival under stress. Cell 107: 137–148.
McBurney MW, Yang X, Jardine K, Hixon M, Boekelheide K, Webb JR et al. (2003). The mammalian SIR2alpha protein has a role in embryogenesis and gametogenesis. Mol Cell Biol 23: 38–54.
Michishita E, Park JY, Burneskis JM, Barrett JC, Horikawa I . (2005). Evolutionarily conserved and nonconserved cellular localizations and functions of human SIRT proteins. Mol Biol Cell 16: 4623–4635.
Moser AR, Pitot HC, Dove WF . (1990). A dominant mutation that predisposes to multiple intestinal neoplasia in the mouse. Science 247: 322–324.
Moynihan KA, Grimm AA, Plueger MM, Bernal-Mizrachi E, Ford E, Cras-Meneur C et al. (2005). Increased dosage of mammalian Sir2 in pancreatic beta cells enhances glucose-stimulated insulin secretion in mice. Cell Metab 2: 105–117.
Muller-Decker K, Neufang G, Berger I, Neumann M, Marks F, Furstenberger G . (2002). Transgenic cyclooxygenase-2 overexpression sensitizes mouse skin for carcinogenesis. Proc Natl Acad Sci USA 99: 12483–12488.
Nemoto S, Fergusson MM, Finkel T . (2004). Nutrient availability regulates SIRT1 through a forkhead-dependent pathway. Science 306: 2105–2108.
Oberdoerffer P, Michan S, McVay M, Mostoslavsky R, Vann J, Park SK et al. (2008). SIRT1 redistribution on chromatin promotes genomic stability but alters gene expression during aging. Cell 135: 907–918.
Ono M, Kuwano M, Kung HF . (1991). Malignant transformation of mouse BALB/3T3 cells by polyoma middle T antigen requires epidermal growth factor receptor expression. Cell Growth Differ 2: 317–322.
Ota H, Tokunaga E, Chang K, Hikasa M, Iijima K, Eto M et al. (2006). Sirt1 inhibitor, Sirtinol, induces senescence-like growth arrest with attenuated Ras-MAPK signaling in human cancer cells. Oncogene 25: 176–185.
Parker JA, Arango M, Abderrahmane S, Lambert E, Tourette C, Catoire H et al. (2005). Resveratrol rescues mutant polyglutamine cytotoxicity in nematode and mammalian neurons. Nat Genet 37: 349–350.
Picard F, Kurtev M, Chung N, Topark-Ngarm A, Senawong T, Machado De Oliveira R et al. (2004). Sirt1 promotes fat mobilization in white adipocytes by repressing PPAR-gamma. Nature 429: 771–776.
Potente M, Ghaeni L, Baldessari D, Mostoslavsky R, Rossig L, Dequiedt F et al. (2007). SIRT1 controls endothelial angiogenic functions during vascular growth. Genes Dev 21: 2644–2658.
Qin W, Yang T, Ho L, Zhao Z, Wang J, Chen L et al. (2006). Neuronal SIRT1 activation as a novel mechanism underlying the prevention of Alzheimer disease amyloid neuropathology by calorie restriction. J Biol Chem 281: 21745–21754.
Rodgers JT, Puigserver P . (2007). Fasting-dependent glucose and lipid metabolic response through hepatic sirtuin 1. Proc Natl Acad Sci USA 104: 12861–12866.
Rogina B, Helfand SL . (2004). Sir2 mediates longevity in the fly through a pathway related to calorie restriction. Proc Natl Acad Sci USA 101: 15998–16003.
Sakatani T, Kaneda A, Iacobuzio-Donahue CA, Carter MG, de Boom Witzel S, Okano H et al. (2005). Loss of imprinting of Igf2 alters intestinal maturation and tumorigenesis in mice. Science 307: 1976–1978.
Stunkel W, Peh BK, Tan YC, Nayagam VM, Wang X, Salto-Tellez M et al. (2007). Function of the SIRT1 protein deacetylase in cancer. Biotechnol J 2: 1360–1368.
Tiano HF, Loftin CD, Akunda J, Lee CA, Spalding J, Sessoms A et al. (2002). Deficiency of either cyclooxygenase (COX)-1 or COX-2 alters epidermal differentiation and reduces mouse skin tumorigenesis. Cancer Res 62: 3395–3401.
Tissenbaum HA, Guarente L . (2001). Increased dosage of a sir-2 gene extends lifespan in Caenorhabditis elegans. Nature 410: 227–230.
van der Veer E, Ho C, O'Neil C, Barbosa N, Scott R, Cregan SP et al. (2007). Extension of human cell lifespan by nicotinamide phosphoribosyltransferase. J Biol Chem 282: 10841–10845.
Vaziri H, Dessain SK, Ng Eaton E, Imai SI, Frye RA, Pandita TK et al. (2001). hSIR2(SIRT1) functions as an NAD-dependent p53 deacetylase. Cell 107: 149–159.
Wang RH, Sengupta K, Li C, Kim HS, Cao L, Xiao C et al. (2008a). Impaired DNA damage response, genome instability, and tumorigenesis in SIRT1 mutant mice. Cancer Cell 14: 312–323.
Wang RH, Zheng Y, Kim HS, Xu X, Cao L, Luhasen T et al. (2008b). Interplay among BRCA1, SIRT1, and Survivin during BRCA1-associated tumorigenesis. Mol Cell 32: 11–20.
Wood JG, Rogina B, Lavu S, Howitz K, Helfand SL, Tatar M et al. (2004). Sirtuin activators mimic caloric restriction and delay ageing in metazoans. Nature 430: 686–689.
Wu Y, Yakar S, Zhao L, Hennighausen L, LeRoith D . (2002). Circulating insulin-like growth factor-I levels regulate colon cancer growth and metastasis. Cancer Res 62: 1030–1035.
Yeung F, Hoberg JE, Ramsey CS, Keller MD, Jones DR, Frye RA et al. (2004). Modulation of NF-kappaB-dependent transcription and cell survival by the SIRT1 deacetylase. EMBO J 23: 2369–2380.
Zhang QJ, Wang Z, Chen HZ, Zhou S, Zheng W, Liu G et al. (2008). Endothelium-specific overexpression of class III deacetylase SIRT1 decreases atherosclerosis in apolipoprotein E-deficient mice. Cardiovasc Res 80: 191–199.
Acknowledgements
We thank Christine Pratt for allowing us to use some of her chemicals. The projects were funded by the Canadian Institutes of Health Research. GB is a recipient of fellowship from the Fonds de Recherche en Santé du Québec (FRSQ).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Boily, G., He, X., Pearce, B. et al. SirT1-null mice develop tumors at normal rates but are poorly protected by resveratrol. Oncogene 28, 2882–2893 (2009). https://doi.org/10.1038/onc.2009.147
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/onc.2009.147
Keywords
This article is cited by
-
Antineoplastic activity of plant-derived compounds mediated through inhibition of histone deacetylase: a review
Amino Acids (2023)
-
Novel molecules as the emerging trends in cancer treatment: an update
Medical Oncology (2022)
-
p107 mediated mitochondrial function controls muscle stem cell proliferative fates
Nature Communications (2021)
-
Sirtuins transduce STACs signals through steroid hormone receptors
Scientific Reports (2020)
-
Combinatorial therapeutic effect of resveratrol and piperine on murine model of systemic lupus erythematosus
Inflammopharmacology (2020)