Abstract
Background/Objectives:
There is controversy regarding the existence of a body mass index (BMI) mortality paradox in diabetes, whereby the optimal BMI category is higher than it is in non-diabetic persons. To explore possible pathways to a mortality paradox, we examined the relationship of BMI with physical and mental health status in diabetic and non-diabetic persons.
Subjects/Methods:
We examined adjusted SF-12 Physical and Mental Component Summary (PCS-12 and MCS-12) scores by BMI (kg m−2) category (underweight, <20; normal weight, 20 to <25; overweight, 25 to <30; obese, 30 to <35; severely obese ⩾35) in adult diabetic and non-diabetic respondents to the 2000–2011 United States national Medical Expenditure Panel Surveys (N=119 161). Adjustors were age, sex, race/ethnicity, income, health insurance, education, smoking, comorbidity, urbanicity, geographic region and survey year.
Results:
In non-diabetic persons the adjusted mean PCS-12 score was highest (that is, most optimal) in the normal-weight category, whereas for diabetic persons the optimal adjusted mean PCS-12 score was in the overweight category (adjusted difference between non-diabetic and diabetic persons in the difference in PCS-12 means for overweight versus normal-weight category=0.8 points, 95% confidence interval; CI 0.1, 1.6; P=0.03). This paradoxical pattern was not evident for the MCS-12, and the adjusted difference between non-diabetic and diabetic persons in the difference in MCS-12 means for overweight versus obese persons was not significant (−0.3 points, 95% CI −0.9, 0.4; P=0.43). The findings were not significantly moderated by smoking status, cancer diagnosis or time period.
Conclusions:
The optimal BMI category for physical health status (but not mental health status) was higher among diabetic than non-diabetic persons. The findings are consistent with a BMI physical health status paradox in diabetes and, in turn, a mortality paradox.
Similar content being viewed by others

Introduction
Most studies examining the relationship of body mass index (BMI) with mortality in diabetic persons suggest a paradox: the BMI category with lowest associated mortality risk (overweight or obese) is higher than it is in non-diabetic persons (normal weight).1, 2, 3, 4, 5, 6, 7 Though apparently counterintuitive, genetic and physiological differences between leaner and heavier diabetic individuals could account for a BMI mortality paradox in diabetes,1, 4, 8, 9, 10, 11 particularly among those with Type 2 diabetes,12 which accounts for most cases in adults. However, in one high-profile study limited to persons with incident diabetes, normal weight was associated with the lowest mortality risk,13 re-igniting the long-standing controversy regarding the existence and potential health implications of a BMI mortality paradox in diabetes.14, 15, 16
Unstudied is whether a BMI health status paradox exists in diabetes, analogous to the BMI mortality paradox. Addressing this question is important in gauging the current net health impact of overweight and obesity in diabetes, and also has implications for the BMI mortality paradox debate, as health status influences mortality risk.17, 18, 19, 20, 21, 22 Heavier diabetic persons could have better health status than their leaner counterparts, owing to the same factors invoked in explaining the BMI mortality paradox,1, 8, 9, 10 or to uncharacterized factors. Alternatively, health status could be worse among heavier diabetic persons,23, 24, 25 owing to excess weight or its sequelae (for example, other metabolic conditions, osteoarthritis).26, 27
National studies comparing the health status of diabetic and non-diabetic persons across BMI categories are lacking. Prior studies of national samples show that health status tends to be lower among diabetic persons than among non-diabetic persons.24, 28, 29 However, the relationship of BMI with health status in diabetes is less clear, paralleling uncertainty regarding the relationship of BMI with mortality. Some studies find health status to be highest among normal-weight persons (including those with diabetes), whereas others find little influence of BMI on health status.24, 28, 30, 31, 32, 33, 34, 35 Reconciling these disparate findings is challenging owing to differences among the studies. Key differences include the type of health status examined (physical, mental, or overall), the degree of comorbidity adjustment, and the recency of the data employed, a particularly important issue given secular trends in BMI, diabetes and health status.36, 37, 38, 39, 40, 41, 42 As others have emphasized, the study of BMI paradoxes hinges on making comparisons between groups of individuals with and without a chronic health condition of interest.43 Thus, exploration of a possible BMI health status paradox in diabetes requires comparing physical and mental health status by BMI category in concurrent samples of diabetic and non-diabetic persons. Given that health status influences mortality risk,17, 19, 21, 22 including in diabetes,18, 20 the findings of such comparisons could suggest possible pathways to a BMI mortality paradox, informing the ongoing debate regarding its existence.
Using national data from the 2000–2011 United States national Medical Expenditure Panel Surveys (MEPS), we examined the relationship of BMI with physical and mental health status in diabetic and non-diabetic persons. The main analyses were adjusted for socio-demographic characteristics, chronic health conditions other than diabetes, smoking status and survey year (to account for secular trends). In additional analyses, we also explored whether smoking status, cancer diagnosis or time period moderated the relationship between BMI and diabetes and health status.
Subjects and methods
The MEPS is an annual national survey of health-care use and costs in the civilian, non-institutionalized population in the United States, employing an overlapping panel design.44 The analytic sample for the current study included persons aged 18–90 years old at entry. The study was exempted by the University of California Davis Institutional Review Board.
In the MEPS, the Household Component includes information on respondent socio-demographics and health insurance, and a self-administered questionnaire includes items on smoking and health conditions. The full-year response rate varied from 70.5 to 59.4% for the 2000–2011 panels.44
Measures
BMI in kg m−2 was constructed from self-reported height and weight. BMI categories employed in analyses were: <20 (underweight); 20–<25 (normal weight); 25–<30 (overweight); 30–<35 (obese); and ⩾35 (severely obese). These categories correspond to those widely employed by clinicians, except for the underweight and normal-weight categories, typically defined in clinical practice and most research prior to 2000 as <18.5 and 18.5–<25.45 A BMI of <20 was employed to distinguish underweight in the current analyses, as prior work indicates health status worsens sharply below that cut point, likely owing to the effects of concurrent illnesses.46 Classifying individuals with a BMI of 18.5–<20 as normal weight would artificially increase the risk of poor health status associated with normal weight and decrease the risk of poor health status associated with overweight and obesity.
Physical and mental health status were measured with the SF-12 Physical Component Summary (PCS-12) and Mental Component Summary (MCS-12) scales, respectively.47 Standardized scoring algorithms are employed to derive both scales, which range from 0 to 100, with higher scores indicating better self-rated health. Both summary scales were designed so that a representative sample of the US population would have a mean score of 50 with a standard deviation of 10.47
Health conditions and socio-demographics
Diabetes was self-reported (present or not), as were eight other chronic conditions: cancer, hypertension, coronary heart disease, myocardial infarction, cerebrovascular disease, asthma, emphysema and arthritis. Agreement between MEPS respondent-reported and clinician-reported health conditions is high.48 Self-reported smoking status was dichotomized as current smoker or not. Socio-demographic variables examined were: age in years; sex; race/ethnicity category (Hispanic (any race), non-Hispanic White, non-Hispanic Black or non-Hispanic other race); household income level as a percentage of Federal Poverty Level (<100%, 100–124%, 125–199%, 200–399%, or ⩾400%); health insurance status (uninsured, privately insured, or publicly insured); education level (less than high school (0–8 years of formal schooling), some high school (9–11years), high school graduate (12years), some college (13–15 years), or college graduate (⩾16 years)); US Census region (West, Midwest, Northeast, South); and urbanicity (living in a Metropolitan Statistical Area or not).
Data analysis
Data were analyzed using Stata 13.1 (Stata Corporation, College Station, TX, USA), adjusting for the complex survey design of MEPS. Data were analyzed using longitudinal strata and primary sampling unit identifiers and survey weights, to derive estimates representative of the US civilian, non-institutionalized adult population. The primary analyses examined associations of BMI category (the key independent variable) with the PCS-12 and MCS-12 scales (the dependent variables), in linear regression models that included diabetes status (present versus absent) as well as a diabetes(present) × BMI category interaction term. All models adjusted for socio-demographic characteristics (age, age squared, sex, race/ethnicity (reference category=non-Hispanic White), household income as a percentage of Federal Poverty Level (reference⩽100%), health insurance status (reference=private insurance), education (reference=less than high school), Census region (reference=Northeast) and urban residence); chronic health conditions other than diabetes (from a count of eight conditions); smoking status; and MEPS survey year, included as a categorical variable (reference=2000). To explore whether key potential confounders (smoking, cancer, or study time period (2000–2005 versus 2006–2011)) moderated the relationships between BMI and diabetes and health status, we conducted additional analyses including three-way interaction terms: key confounder × diabetes status × BMI category.
To facilitate interpretation of the net adjusted associations between BMI category and health status, the findings of all models are presented as adjusted predictive marginal effects, which estimate of the amount of change in health status score produced per change in BMI category.49 We examine the difference between the marginal health status score (physical or mental) for the BMI category associated with the lowest score in diabetic persons with that found among normal-weight diabetic persons. We contrast that difference with the difference observed between the same BMI categories among non-diabetic persons. We present the resulting 'difference in difference' in the Results text.
Results
There were 138 944 adults aged 18–90 entering the MEPS cohorts between 2000 and 2011; 119 161 (87.6%, population weighted) had complete data and were included in the current analyses. Table 1 summarizes the characteristics of the analytic sample by diabetes status. Compared with participants who did not report diabetes, those reporting diabetes were older and more likely to be Hispanic (any race) or non-Hispanic Black, have low household income and education, reside in the South and in non-urban areas, have more comorbid chronic health conditions, be non-smoking and be obese or severely obese. Participants reporting diabetes also had lower mean PCS-12 and MCS-12 scores than those not reporting diabetes.
Table 2 presents the unadjusted mean PCS-12 and MCS-12 scores of the analytic sample by BMI category and diabetes status. For both measures, across the range of study BMI categories, scores were lower among respondents with versus without diabetes. Among diabetic persons, for both measures the unadjusted mean scores were highest among those in the overweight category. By contrast, for non-diabetic persons, while unadjusted MCS-12 scores were again highest for those in the overweight category, unadjusted PCS-12 scores were highest in the normal-weight category.
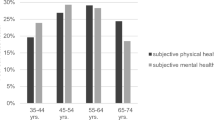
Table 3 and the Figure 1 show the adjusted PCS-12 and MCS-12 scores by BMI category and diabetes status. Across all study BMI categories, scores were lower for diabetic versus non-diabetic persons, with the most marked decrements for underweight diabetic persons. Among non-diabetic persons, for both health status measures, scores were lowest in the severely obese category. Among diabetic persons, the same pattern was observed for the PCS-12 (Table 3 and Figure 1, panel a), but for the MCS-12, scores were lowest in the underweight category (Table 3 and Figure 1, panel b).
Adjusted physical and mental health status by body mass index category among diabetic versus non-diabetic persons (N=119 161). Legend: Panel a: physical health status (PCS-12). Panel b: mental health status (MCS-12). Dark circles: point estimates for non-diabetic persons. Light diamonds: point estimates for diabetic persons. Bars around point estimates indicate 95% confidence intervals. Analyses adjusted for age, age squared, gender, race/ethnicity, family income, education, insurance coverage, number of chronic health conditions, smoking status, rurality, region, and panel year. Abbreviations: MCS-12, SF-12 Mental Component Summary score; PCS-12, SF-12 Physical Component Summary score.
For the PCS-12 (Table 3 and Figure 1, panel a), among non-diabetic persons scores were highest in the normal-weight group and significantly higher in that group than in the overweight group (0.4, 95% confidence interval (CI) 0.2, 0.5; P<0.001). Among diabetic persons scores were highest in the overweight group, though non-significantly higher than in the normal-weight group (0.5, 95% CI 0.3, 1.2; P=0.19). The adjusted difference between non-diabetic and diabetic persons in the difference in PCS-12 scores for the overweight versus the normal-weight category was significant (0.8, 95% CI 0.1, 1.6; P=0.03). The overall BMI category × diabetes status two-way interaction term also was significant (F(4445)=6.63; P<0.001).
For the MCS-12 (Table 3 and Figure 1, panel b), among non-diabetic persons, mean scores were highest in overweight persons, and significantly higher than in obese persons (0.3, 95% CI 0.1, 0.5; P=0.01). In diabetic persons, scores were also highest in the overweight group but non-significantly higher than in the obese group (0.0, 95% CI −0.6, 0.6; P=0.94). The adjusted difference between non-diabetic and diabetic persons in the difference in MCS-12 scores for the overweight versus the normal-weight category was not significant (−0.3, 95% CI −0.9, 0.4; P=0.43). The overall BMI category × diabetes status interaction term also was not significant (F(4445)=1.68; P=0.15).
In analyses exploring moderation of the associations of health status (PCS-12 or MCS-12) with BMI category in diabetes by smoking, cancer or time period, none of the respective three-way interaction terms were significant (data not shown, available from the authors).
Discussion
In a US national sample, we found evidence of a BMI physical health status paradox in diabetes, mirroring the previously described BMI mortality paradox. Consistent with prior work, physical and mental health status scores were lower for diabetic persons as compared with non-diabetic persons in our sample across all study BMI categories.24, 28, 29 However, for physical (but not mental) health status, the optimal BMI category was higher among individuals with diabetes (overweight) than among those without diabetes (normal weight). The findings in our diabetes sample are broadly consistent with those of a prior study of Type 2 diabetes, which found that 26 kg m−2 was the BMI associated with optimal overall health status, measured with the EQ-5D index.29 However, no prior studies have compared physical and mental health status by BMI category in concurrent samples of diabetic and non-diabetic persons.
Our findings should not be construed to mean that normal-weight individuals with diabetes should try to gain weight, or that overweight or obese diabetic persons should avoid losing weight.50 Also, the differences in physical health status scores that we observed for overweight versus normal-weight diabetic persons are small and unlikely to be clinically significant at the individual level. Prior work suggests that the minimum clinically important difference in scores for the PCS-12 measure is three points,51 whereas among diabetic persons we found an adjusted difference of less than one point between the optimal and next most optimal BMI category.
Nonetheless, the findings may have population level implications. Although the observational nature of our analyses precludes causal inference, the findings suggest that diabetes in the context of normal weight may involve more severe physical morbidity than diabetes associated with overweight, possibly driven by genetic and physiological differences between leaner and heavier diabetic persons.1, 4, 8, 9, 10, 11, 12 The MEPS data we employed did not permit us to distinguish whether patients had Type 1 or Type 2 diabetes. However, of the 25 million US adults who have diabetes, 90–95% have Type 2 diabetes, suggesting that most of the individuals in our sample reporting diabetes had Type 2 diabetes. Over 85% of persons with Type 2 DM are overweight or obese.52 Thus, despite the relatively small differences that we observed in health status scores for heavier versus thinner individuals with diabetes, our findings may have implications for the net public health impact of overweight and obesity in diabetes, particularly Type 2 diabetes.
The study findings may also bear on the long-standing controversy regarding the existence and implications of a BMI mortality paradox in diabetes.14, 15, 16 The controversy was newly driven by a recent study by Tobias et al.,13 in which normal weight was the BMI category of lowest mortality risk in a cohort of persons with incident diabetes. By contrast, all prior studies in this realm found that the overweight or obese diabetic persons had lower mortality risk than their normal-weight counterparts.1, 2, 3, 4, 5, 6, 7 Of note, rather than studying a broadly representative sample of individuals with varying durations of diabetes as did prior investigators, Tobias et al. studied a selected sample of nurses and physicians with incident diabetes who were free from cardiovascular disease and cancer at diagnosis. Such an approach excludes people with relatively earlier onset and potentially more severe diabetes, which could account for the differing findings of the study relative to others in this realm. In addition, the study by Tobias et al. and some others in this realm lacked a concurrent non-diabetic group,3, 5, 6, 7 yet such a comparison group is critical to examining the BMI mortality paradox.43 Of the two prior studies in this realm that did compare mortality risk by BMI category in concurrent diabetic and non-diabetic samples, both found evidence supporting a BMI mortality paradox in diabetes.2, 4 Given that physical health status has been shown to influence mortality risk,21, 22 including in diabetes,20 our findings suggest possible pathways that could contribute to a BMI mortality paradox.
Some have suggested the apparent BMI mortality paradox in diabetes is created by detrimental health habits (particularly smoking) and pre-existing conditions (especially cancer) leading to both lower BMI and increased mortality.13, 53 Thus, we examined whether the interaction of BMI category and diabetes in influencing physical health status was moderated by smoking or cancer. That we found no evidence of moderation by smoking or cancer does not exclude the possibility that they influenced the findings, as our observational study design precludes causal inference. In an attempt to address this issue, some researchers studying the BMI mortality paradox have excluded smokers and many or all persons with comorbid conditions.13, 53 We chose not to do so, as it would result in a much smaller, highly selected group of diabetic persons, limiting generalizability and statistical power.54 A robust examination of the potential role of smoking or cancer in explaining the BMI mortality paradox will require prospective studies of broadly representative samples that incorporate repeated weight, health status, health habits and comorbidity measurements over time.
Diabetic persons had worse physical and mental health status than non-diabetic persons across all BMI categories. However, the magnitudes of the differences were smaller for mental health status than for physical health status. Further, although decrements in both physical and mental health status associated with diabetes were progressively smaller from the underweight category through the overweight category, decrements in physical health status began to grow larger again in the obese category, whereas decrements in mental health status began to grow larger again only in severe obesity. These findings suggest the possibility of mental health status protective factors among heavier persons. Some genes conferring increased risk for both obesity and diabetes have variants associated with decreased risk for depression.12, 55 The findings further suggest that protective effects on mental health in heavier persons, if present, may be offset in severe obesity by detrimental factors. For example, whereas all degrees of increased BMI are stigmatized, in this era of prevalent overweight and obesity, the stigma of severe obesity is orders of magnitude greater, and may affect mental health.56 Research is needed to examine these hypotheses.
A strength of our study was the use of national data collected within the past 15 years from concurrent and broadly representative samples of diabetic and non-diabetic persons. Our study also had some limitations. As noted previously, the study was observational, so causal associations cannot be inferred, and the findings are susceptible to unmeasured confoundings, which could differ by diabetes status. Diabetes status was self-reported, and BMI was derived from self-reported height and weight. Prior studies suggest a complex relationship between self-reported and objectively measured BMI, with differences in BMI category misclassification resulting from self-reports based on socio-demographic characteristics (for example, country of residence, sex, race/ethnicity) and BMI category (for example, tendency to underestimate BMI among higher BMI persons versus overestimate BMI among lower BMI individuals).57, 58, 59 Further, people who perceive themselves as being normal weight are less likely to report impaired health status than those who perceive they are overweight, regardless of actual BMI.60 The net effects of such relationships on the BMI health status associations we observed are uncertain. Studies employing objectively measured BMI and diabetes are required to explore these issues. To explain the contrasting BMI health status relationships we observed for diabetic versus non-diabetic persons, there would also have to be a differential reporting bias by self-reported diabetes status.
In conclusion, in comparing physical and mental health status by BMI category in concurrent national samples of diabetic and non-diabetic persons, we found evidence of a physical (but not mental) health status paradox in diabetes. Physical health status was most optimal in the overweight category among diabetic persons, versus in the normal-weight category among non-diabetic persons. Given that physical health status influences mortality risk, the findings suggest possible pathways to a BMI mortality paradox in diabetes.
References
Carnethon MR, Rasmussen-Torvik LJ, Palaniappan L . The obesity paradox in diabetes. Curr Cardiol Rep 2014; 16: 446.
Jackson CL, Yeh HC, Szklo M, Hu FB, Wang NY, Dray-Spira R et al. Body-mass index and all-cause mortality in US adults with and without diabetes. J Gen Intern Med 2014; 29: 25–33.
Jerant A, Franks P . Body mass index, diabetes, hypertension, and short-term mortality: a population-based observational study, 2000-2006. J Am Board Fam Med 2012; 25: 422–431.
Lajous M, Bijon A, Fagherazzi G, Boutron-Ruault MC, Balkau B, Clavel-Chapelon F et al. Body mass index, diabetes, and mortality in French women: explaining away a "paradox". Epidemiology 2014; 25: 10–14.
McEwen LN, Karter AJ, Waitzfelder BE, Crosson JC, Marrero DG, Mangione CM et al. Predictors of mortality over 8 years in type 2 diabetic patients: Translating Research Into Action for Diabetes (TRIAD). Diabetes Care 2012; 35: 1301–1309.
Logue J, Walker JJ, Leese G, Lindsay R, McKnight J, Morris A et al. Association between BMI measured within a year after diagnosis of type 2 diabetes and mortality. Diabetes Care 2013; 36: 887–893.
Carnethon MR, De Chavez PJ, Biggs ML, Lewis CE, Pankow JS, Bertoni AG et al. Association of weight status with mortality in adults with incident diabetes. JAMA 2012; 308: 581–590.
Perry JR, Voight BF, Yengo L, Amin N, Dupuis J, Ganser M et al. Stratifying type 2 diabetes cases by BMI identifies genetic risk variants in LAMA1 and enrichment for risk variants in lean compared to obese cases. PLoS Genet 2012; 8: e1002741.
Coleman NJ, Miernik J, Philipson L, Fogelfeld L . Lean versus obese diabetes mellitus patients in the United States minority population. J Diabetes Complications 2013; 28: 500–505.
Vaag A, Lund SS . Non-obese patients with type 2 diabetes and prediabetic subjects: distinct phenotypes requiring special diabetes treatment and (or) prevention? Appl Physiol Nutr Metab 2007; 32: 912–920.
Kao YM, Chen JD . Inverse association between body mass index and chronic kidney disease in older diabetic adults. Ann Epidemiol 2013; 23: 255–259.
Xi B, Takeuchi F, Meirhaeghe A, Kato N, Chambers JC, Morris AP et al. Associations of genetic variants in/near body mass index-associated genes with type 2 diabetes: a systematic meta-analysis. Clin Endocrinol (Oxf) 2014; 81: 702–710.
Tobias DK, Pan A, Jackson CL, O'Reilly EJ, Ding EL, Willett WC et al. Body-mass index and mortality among adults with incident type 2 diabetes. N Engl J Med 2014; 370: 233–244.
Hainer V, Aldhoon-Hainerova I . Obesity paradox does exist. Diabetes Care 2013; 36: S276–S281.
Standl E, Erbach M, Schnell O . Defending the con side: obesity paradox does not exist. Diabetes Care 2013; 36: S282–S286.
Stevens J, Bradshaw PT, Truesdale KP, Jensen MD . Obesity Paradox should not interfere with public health efforts. Int J Obes (Lond) 2014; 39: 80–81.
DeSalvo KB, Bloser N, Reynolds K, He J, Muntner P . Mortality prediction with a single general self-rated health question. A meta-analysis. J Gen Intern Med 2006; 21: 267–275.
McEwen LN, Kim C, Haan MN, Ghosh D, Lantz PM, Thompson TJ et al. Are health-related quality-of-life and self-rated health associated with mortality? Insights from Translating Research Into Action for Diabetes (TRIAD). Prim Care Diabetes 2009; 3: 37–42.
Jerant A, Tancredi DJ, Franks P . Mortality prediction by quality-adjusted life year compatible health measures: findings in a nationally representative US sample. Med Care 2011; 49: 443–450.
Landman GW, van Hateren KJ, Kleefstra N, Groenier KH, Gans RO, Bilo HJ . Health-related quality of life and mortality in a general and elderly population of patients with type 2 diabetes (ZODIAC-18). Diabetes Care 2010; 33: 2378–2382.
Franks P, Gold MR, Fiscella K . Sociodemographics, self-rated health, and mortality in the US. Soc Sci Med 2003; 56: 2505–2514.
Haring R, Feng YS, Moock J, Volzke H, Dorr M, Nauck M et al. Self-perceived quality of life predicts mortality risk better than a multi-biomarker panel, but the combination of both does best. BMC Med Res Methodol 2011; 11: 103.
Muller-Nordhorn J, Muckelbauer R, Englert H, Grittner U, Berger H, Sonntag F et al. Longitudinal association between body mass index and health-related quality of life. PLoS One 2014; 9: e93071.
Jia H, Lubetkin EI . The impact of obesity on health-related quality-of-life in the general adult US population. J Public Health (Oxf) 2005; 27: 156–164.
Centers for Disease Control and Prevention (CDC). Self-rated fair or poor health among adults with diabetes—United States, 1996-2005. MMWR Morb Mortal Wkly Rep 2006; 55: 1224–1227.
Losina E, Walensky RP, Reichmann WM, Holt HL, Gerlovin H, Solomon DH et al. Impact of obesity and knee osteoarthritis on morbidity and mortality in older Americans. Ann Intern Med 2011; 154: 217–226.
Ul-Haq Z, Mackay DF, Fenwick E, Pell JP . Impact of metabolic comorbidity on the association between body mass index and health-related quality of life: a Scotland-wide cross-sectional study of 5,608 participants. BMC Public Health 2012; 12: 143.
Kearns B, Ara R, Young T, Relton C . Association between body mass index and health-related quality of life, and the impact of self-reported long-term conditions—cross-sectional study from the south Yorkshire cohort dataset. BMC Public Health 2013; 13: 1009.
Hunger M, Schunk M, Meisinger C, Peters A, Holle R . Estimation of the relationship between body mass index and EQ-5D health utilities in individuals with type 2 diabetes: evidence from the population-based KORA studies. J Diabetes Complications 2012; 26: 413–418.
Micciolo R, Canal L, Minniti A, Mazzali G, Fantin F, Corzato F et al. The association between excess weight and comorbidity and self-rated health in the Italian population. Ann Epidemiol 2013; 23: 172–178.
Korhonen PE, Seppala T, Jarvenpaa S, Kautiainen H . Body mass index and health-related quality of life in apparently healthy individuals. Qual Life Res 2014; 23: 67–74.
Bentley TG, Palta M, Paulsen AJ, Cherepanov D, Dunham NC, Feeny D et al. Race and gender associations between obesity and nine health-related quality-of-life measures. Qual Life Res 2011; 20: 665–674.
Bottone FG Jr, Hawkins K, Musich S, Cheng Y, Ozminkowski RJ, Migliori RJ et al. The relationship between body mass index and quality of life in community-living older adults living in the United States. J Nutr Health Aging 2013; 17: 495–501.
Ul-Haq Z, Mackay DF, Fenwick E, Pell JP . Meta-analysis of the association between body mass index and health-related quality of life among adults, assessed by the SF-36. Obesity (Silver Spring) 2013; 21: E322–E327.
Wee HL, Wu Y, Thumboo J, Lee J, Tai ES . Association of body mass index with Short-Form 36 physical and mental component summary scores in a multiethnic Asian population. Int J Obes (Lond) 2010; 34: 1034–1043.
Naess S, Eriksen J, Midthjell K, Tambs K . Diabetes mellitus and psychological well-being. Change between 1984-1986 and 1995-1997. Results of the Nord-Trondelag Health Study. J Diabetes Complications 2004; 18: 141–147.
Flegal KM, Carroll MD, Ogden CL, Curtin LR . Prevalence and trends in obesity among US adults, 1999-2008. JAMA 2010; 303: 235–241.
Centers for Disease Control and Prevention (CDC). State-specific incidence of diabetes among adults—participating states, 1995-1997 and 2005-2007. MMWR Morb Mortal Wkly Rep 2008; 57: 1169–1173.
Rabin D, Petterson SM, Bazemore AW, Teevan B, Phillips RL Jr, Dodoo MS et al. Decreasing self-perceived health status despite rising health expenditures. Am Fam Physician 2009; 80: 427.
Gregg EW, Cheng YJ, Narayan KM, Thompson TJ, Williamson DF . The relative contributions of different levels of overweight and obesity to the increased prevalence of diabetes in the United States: 1976-2004. Prev Med 2007; 45: 348–352.
Gregg EW, Cadwell BL, Cheng YJ, Cowie CC, Williams DE, Geiss L et al. Trends in the prevalence and ratio of diagnosed to undiagnosed diabetes according to obesity levels in the U.S. Diabetes Care 2004; 27: 2806–2812.
Fishman EI, Stokes A, Preston SH . The dynamics of diabetes among birth cohorts in the U.S. Diabetes Care 2014; 37: 1052–1059.
Childers DK, Allison DB . The 'obesity paradox': a parsimonious explanation for relations among obesity, mortality rate and aging? Int J Obes (Lond) 2010; 34: 1231–1238.
Agency for Healthcare Research and Quality. Medical Expenditure Panel Survey, 2010. http://www.meps.ahrq.gov/mepsweb/about_meps/survey_back.jsp (accessed 11 May 2014).
NHLBI Obesity Education Initiative Expert Panel on the Identification, Evaluation, and Treatment of Obesity in Adults. Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults. Report No. 98-4083. National Heart, Lung, and Blood Institute: Bethesda, MA, USA, 1998.
Muennig P, Lubetkin E, Jia H, Franks P . Gender and the burden of disease attributable to obesity. Am J Public Health 2006; 96: 1662–1668.
Ware J Jr, Kosinski M, Keller SD . A 12-Item Short-Form Health Survey: construction of scales and preliminary tests of reliability and validity. Med Care 1996; 34: 220–233.
Krauss N, Kass B Comparison of household and medical provider reports of medical conditions, Joint Statistical Meetings. Indianapolis, IN, USA 2000.
Graubard BI, Korn EL . Predictive margins with survey data. Biometrics 1999; 55: 652–659.
Schauer PR, Kashyap SR, Wolski K, Brethauer SA, Kirwan JP, Pothier CE et al. Bariatric surgery versus intensive medical therapy in obese patients with diabetes. N Engl J Med 2012; 366: 1567–1576.
Samsa G, Edelman D, Rothman ML, Williams GR, Lipscomb J, Matchar D . Determining clinically important differences in health status measures: a general approach with illustration to the Health Utilities Index Mark II. Pharmacoeconomics 1999; 15: 141–155.
Narayan KM, Boyle JP, Thompson TJ, Sorensen SW, Williamson DF . Lifetime risk for diabetes mellitus in the United States. JAMA 2003; 290: 1884–1890.
Preston SH, Stokes A . Obesity paradox: conditioning on disease enhances biases in estimating the mortality risks of obesity. Epidemiology 2014; 25: 454–461.
Flegal KM, Graubard BI, Williamson DF, Cooper RS . Reverse causation and illness-related weight loss in observational studies of body weight and mortality. Am J Epidemiol 2011; 173: 1–9.
Samaan Z, Anand SS, Zhang X, Desai D, Rivera M, Pare G et al. The protective effect of the obesity-associated rs9939609 A variant in fat mass- and obesity-associated gene on depression. Mol Psychiatry 2013; 18: 1281–1286.
Puhl RM, Heuer CA . The stigma of obesity: a review and update. Obesity (Silver Spring) 2009; 17: 941–964.
Gorber SC, Tremblay MS . The bias in self-reported obesity from 1976 to 2005: a Canada-US comparison. Obesity (Silver Spring) 2010; 18: 354–361.
Nyholm M, Gullberg B, Merlo J, Lundqvist-Persson C, Rastam L, Lindblad U . The validity of obesity based on self-reported weight and height: Implications for population studies. Obesity (Silver Spring) 2007; 15: 197–208.
Stommel M, Schoenborn CA . Accuracy and usefulness of BMI measures based on self-reported weight and height: findings from the NHANES & NHIS 2001-2006. BMC Public Health 2009; 9: 421.
Herman KM, Hopman WM, Rosenberg MW . Self-rated health and life satisfaction among Canadian adults: associations of perceived weight status versus BMI. Qual Life Res 2013; 22: 2693–2705.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution 4.0 International License. The images or other third party material in this article are included in the article’s Creative Commons license, unless indicated otherwise in the credit line; if the material is not included under the Creative Commons license, users will need to obtain permission from the license holder to reproduce the material. To view a copy of this license, visit http://creativecommons.org/licenses/by/4.0/
About this article
Cite this article
Jerant, A., Bertakis, K. & Franks, P. Body mass index and health status in diabetic and non-diabetic individuals. Nutr & Diabetes 5, e152 (2015). https://doi.org/10.1038/nutd.2015.2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nutd.2015.2