Abstract
Background:
Antibiotics, used for 60 years to promote weight gain in animals, have been linked to obesity in adults and in children when administered during early infancy. Lactobacillus reuteri has been linked to obesity and weight gain in children affected with Kwashiorkor using ready-to-use therapeutic food. In contrast, Escherichia coli has been linked with the absence of obesity. Both of these bacteria are resistant to vancomycin.
Objectives and methods:
We assessed vancomycin-associated weight and gut microbiota changes, and tested whether bacterial species previously linked with body mass index (BMI) predict weight gain at 1 year. All endocarditis patients treated with vancomycin or amoxicillin in our center were included from January 2008 to December 2010. Bacteroidetes, Firmicutes, Lactobacillus and Methanobrevibacter smithii were quantified using real-time PCR on samples obtained during the 4–6 weeks antibiotic regimen. L. reuteri, L. plantarum, L. rhamnosus, Bifidobacterium animalis and E. coli were quantified on stool samples obtained during the first week of antibiotics.
Results:
Of the193 patients included in the study, 102 were treated with vancomycin and 91 with amoxicillin. Vancomycin was associated with a 10% BMI increase (odds ratio (OR) 14.1; 95% confidence interval (CI; 1.03–194); P=0.047) and acquired obesity (4/41 versus 0/56, P=0.01). In patients treated with vancomycin, Firmicutes, Bacteroidetes and Lactobacillus increased, whereas M. smithii decreased (P<0.05). The absence of E. coli was an independent predictor of weight gain (OR=10.7; 95% CI (1.4–82.0); P=0.02). Strikingly, a patient with an 18% BMI increase showed a dramatic increase of L. reuteri but no increase of E. coli.
Conclusion:
The acquired obesity observed in patients treated with vancomycin may be related to a modulation of the gut microbiota rather than a direct antibiotic effect. L. reuteri, which is resistant to vancomycin and produces broad bacteriocins, may have an instrumental role in this effect.
Similar content being viewed by others
Introduction
Stokstad et al.1 first found that the administration of Streptomyces aureofaciens led to a twofold weight increase in chickens, and identified that one of its bacteriocins, chlortetracycline, was responsible for this effect. For over 60 years since then, antibiotics, including mainly glycopeptides, tetracycline, macrolides and penicillins, have been used at subtherapeutic levels to promote weight gain in animals. These continue to be widely used in the United States of America, where more than 13 000 tons of active ingredients have been sold in 2009.2 The Animal Health Institute of America (www.ahi.org) has estimated that without the use of growth promoting antibiotics, the USA would require an additional 452 million chickens, 23 million cattle and 12 million pigs to reach the levels of production attained with current practices.3 From the beginning of their use in agriculture in the 1950s, a similar effect on growth was reported in humans,4, 5, 6 but seems to have been neglected. The link recently identified between the gut microbiota, human obesity7 and malnutrition8, 9 has led researchers to reconsider the impact of antibiotics that are associated with obesity particularly when administered in early infancy (Table 1).
Glycopeptides, derived from bacteriocins secreted by bacteria of the Actinomycetales order, are antibiotics largely used in human medicine but linked with weight gain both in animals and humans. Indeed, avoparcin, originally isolated from Streptomyces candidus, was associated with weight gain in farm animals,10 whereas vancomycin, which is isolated from Amycolatopsis orientalis, was associated with significant weight gain and acquired obesity in humans11 in addition to increased adiposity in animals.12 In vitro, glycopeptides affect mainly Gram-positive bacteria due to inhibitory activity against peptidoglycan synthesis. However, Pediococcous and Lactobacillus are not susceptible to glycopeptides, with the notable exception of the L. acidophilus group. Even if the susceptibility depends on the bacterial species within the same genus, treatment with oral vancomycin in humans has been associated with a decrease in Clostridium, Enterococcus, Staphylococcus, Bacteroides and Bifidobacterium. However, an overgrowth of Lactobacillus, Pediococcus and Proteobacteria as Klebsiella, Enterobacter or Citrobacter has also been reported (Table 2).
In a previous study, we found an association between vancomycin and acquired obesity in humans, but gut microbiota was not analyzed.11 In this work, we have tested the weight gain effect associated with vancomycin in a new series of patients. In addition, we analyzed the change in the gut microbiota and tested whether bacterial species that were previously linked with body mass index (BMI)13, 14 were predictive of weight gain after vancomycin treatment.
Patients and methods
Patients
All endocarditis patients who were treated by vancomycin or amoxicillin (taken as a control group based on results of our previous study11) in the departments of Cardiology, Hospital de la Timone, Marseille, France were included (Figure 1) between January 2008 and December 2010. Endocarditis was defined using the modified Duke criteria.15 Patients were treated for at least 4 weeks with or without gentamycin. For each case of endocarditis, the decision for surgery was made by a multidisciplinary discussion following our protocol.16 The use of any antibiotic other than amoxicillin, vancomycin or gentamycin for more than 7 days and switching between vancomycin and amoxicillin were exclusion criteria. As all the patients were included after the diagnosis of endocarditis, samples were obtained from the first week after the start of antibiotics. The control group included 42 controls whose stools were analyzed in a previous study.14 Collection of data included age, sex, height, weight and type of antibiotic treatment, but other medications or diet were not collected. According to our published protocols,16 most of patients (>80%) received 6 weeks of treatment. Written consent was obtained from each participant and approved by the ethics committee of the Faculty of Medicine La Timone, Marseille, France under number 08–002.
Analysis of weight change
A standardized questionnaire was used to collect demographical, clinical and therapeutic data in all patients treated by antibiotics. The baseline weight (1 month before the onset of the disease), weight at 1 year and height were collected for each patient based on clinical records, systematic follow-up consultations or phone calls. The %deltaBMI, a %deltaBMI >10% and an acquired obesity (BMI becoming>30 at 1 year) were assessed comparing baseline BMI and BMI at 1 year. The %deltaBMI was calculated as follows: %deltaBMI=(BMI at 1 year−baseline BMI)/baseline BMI × 100.
Analysis of intestinal flora
Starting in April 2009, all patients with an endocarditis diagnosis were ask to provide a stool sample at diagnosis and as much as possible during the 4–6 weeks of treatment. DNA was isolated from the stool as described in Dridi et al.18 The purified DNA was eluted from samples to a final volume of 100 μl and stored at −80 °C until analysis. Real-time PCR analysis was performed on a Stratagene MX3000 (Agilent, Santa Clara, CA, USA) using the Quantitect PCR mix (Qiagen, Courtaboeuf, France) as previously described,19 which targeted Bacteroidetes, Firmicutes, Lactobacillus and M. smithii. Quantification of all bacteria was performed as previously described.18
A second analysis designed for the identification of gut bacteria predictive of weight gain was performed only for samples obtained during the first week of antibiotics in patients for whom both weight and gut flora data were available. A real-time PCR was performed on a Bio-Rad FLX96 and targeted L. reuteri, L. plantarum, L. rhamnosus, B. animalis and E. coli as previously reported.13
Statistical analysis
Student’s t-test or a Mann–Whitney test was used to compare continuous variables between the two groups according to the distribution assessed by the Kolmogorov–Smirnov test. Proportions were compared using a two-sided Barnard’s exact test.20 The analyses were performed using SPSS v21.0 (IBM, Paris, France).
In the first analysis, the changes of BMI at 1 year were compared between the two antibiotic groups (vancomycin or amoxicillin) for all patients with available information. A logistic regression analysis was performed, using a deltaBMI >10% or acquired obesity as the dependent variable. The regression was adjusted by age, sex, surgery and baseline BMI, and was systematically adjusted by antibiotic treatment (vancomycin or amoxicillin).
In the second analysis, the concentrations of Bacteroidetes, Firmicutes, M. smithii and Lactobacillus were compared between all samples by intervention group (vancomycin or amoxicillin) and controls for all patients with an available stool sample. In a preliminary univariate analysis, all significant comparisons were confirmed using Dunn’s multiple comparison test. To account for the intra-individual correlation within the repeated measures (one individual could have several fecal samples), a linear model with mixed effects and a random intercept was used, adjusted for age, sex and baseline BMI.
Finally, to identify a relationship between the initial gut microbiota and weight gain at 1 year, proportions of endocarditis patients with weight gain were compared between carriers and non-carriers for each bacterium analyzed on samples obtained during the first week of antibiotics. When comparing %deltaBMI at 1 year between carriers and non-carriers, a bilateral Student’s t-test was performed with Welch’s correction after the Kolmogorov–Smirnov test.
Results
Weight change study
Ninety-seven patients were analyzed for weight change at 1 year (Figure 1). The proportion of patients with an increase for more than 10% BMI was higher in the vancomycin group (5/41 (12.2%)) than in the amoxicillin group (1/56 (1.8%), P=0.038). This finding was confirmed using a logistic regression analysis, adjusted for age, sex, surgery and baseline BMI (Tables 3 and 4). It was not significant for an increase in BMI >5% (9/41 in the vancomycin group versus 7/56 in the amoxicillin group, P=0.23). Acquired obesity was observed in four individuals who had all been treated with vancomycin (P=0.01). One of the individuals with acquired obesity was initially lean (BMI 25) and gained 11 kg, whereas the other three have baseline BMI between 27 and 29.
Gut microbiota alteration during antibiotic treatment
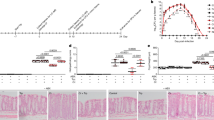
One-hundred and forty-nine patients were analyzed for gut microbiota alteration during antibiotic treatment (Figure 1). The amount of Firmicutes was significantly higher in the vancomycin group when compared with controls (P=0.007), whereas the amoxicillin group showed no significant difference compared with the control group (P=0.58) (Figure 2). The amount of Bacteroidetes was also increased in the vancomycin group when compared with controls (P<0.0001). Similarly, the amount of Bacteroidetes was higher in the amoxicillin group (P=0.002). Conversely, despite in vitro resistance to the use of antibiotics,21 the amount of M. smithii was significantly decreased in both groups of patients on antibiotics when compared with controls (P=0.01 for the vancomycin group and P=0.01 for the amoxicillin group). In addition, there was no significant difference in the amount of M. smithii between patients receiving vancomycin and amoxicillin (P=0.80). Lactobacillus was significantly increased in the vancomycin group compared with controls (P=0.04). There was no significant difference in the amount of Lactobacillus between the amoxicillin group and the control group. Finally, the total number of bacteria was increased in both groups of patients receiving antibiotics when compared with controls (P<0.0001 and P=0.001 for vancomycin and amoxicillin, respectively). No significant results were obtained in the multivariate analysis.
Case of a patient with acquired obesity while being initially lean
A 51-year-old woman treated with vancomycin after a valve replacement surgery presented a massive weight gain over the course of a year (height: 1.50 m; weight: 58 kg before endocarditis increasing to 69 kg at 1 year; BMI: 25.8 before the onset of the disease increasing to 30.6, 1 year after the treatment corresponding to an increase of 11 kg, 4.8 kg m−2 and 19% BMI). The analysis of her first stool sample collected promptly after the beginning of the vancomycin treatment was devoid of L. reuteri, L. plantarum, L. rhamnosus, B. animalis and E. coli. L. reuteri was found in high concentrations (4.7 log10 copies DNA per ml) for the first time in her second stool sample, which was collected 68 days after beginning the vancomycin treatment, no E. coli was detected and there was a decrease in Firmicutes (7.9–7.0 log c.f.u. per ml), Bacteroidetes (8.6–7.9 log c.f.u. per ml) and M. smithii (5.8–4.8 log c.f.u. per ml) between the two samples.
Absence of E. coli is predictive of weight gain under vancomycin
In the 21 patients treated with vancomycin for whom a stool sample obtained during the first week of antibiotics was available, the absence of E. coli in the initial gut microbiota was associated with an increase in BMI at 1 year (8/10 with a weight gain versus 3/11 without weight gain, P=0.03). A logistic regression model adjusted for age, sex and surgery identified an association between the absence of E. coli and weight gain at 1 year (odds ratio=10.7; 95% confidence interval 1.39–82.0); P=0.02). This was confirmed using %deltaBMI (mean±standard Error, 4.0±2.1 for patients without E. coli versus −3.4±2.0 for patients with E. coli, P=0.01, Figure 3). This was also true when one outlier (a patient with a BMI increase of 19%) was excluded (n=20, 2.5±1.6 versus −3.4±2.0, P=0.03). We did not find any other significant differences regarding other bacteria (L. plantarum, L. reuteri, L. rhamnosus, B. animalis, Firmicutes, Bacteroidetes, M. smithii and the Lactobacillus genus) or data from the amoxicillin-treated patients. However, the prevalence was extremely low for Lactobacillus and Bifidobacterium, as previously reported.13
Discussion
In this study, we confirmed that vancomycin was associated with a massive weight gain compared with the weight before the onset of the diseases (endocarditis) in 1/8 human individuals, whereas amoxicillin caused such a massive weight gain in <1 in 50 individuals. We found that the initial gut microbiota was a critical parameter for the identification of individuals more likely to gain weight under vancomycin. Indeed, the presence of E. coli at the beginning of treatment was predictive of weight loss, whereas its absence was predictive of weight gain. In contrast, the only patient with an acquired obesity while being initially lean showed a dramatic increase in L. reuteri. Finally, we confirmed a characteristic profile of the vancomycin gut microbiota with increased levels of Lactobacillus, increased Firmicutes and Bacteroidetes, but decreased levels of M. smithii.
Gut microbiota alterations associated with vancomycin have been previously reported using culture or large-scale molecular studies and included mainly an increase in the Proteobacteria and Lactobacillaceae, and a specific decrease in specific Firmicutes representatives, such as Clostridium, Staphylococcus and Enterococcus. One of the most striking difference between vancomycin and amoxicillin, the latter used in our study as a control, is the increase in Lactobacillus associated with vancomycin (Table 2).
Human obesity, which is promoted by antibiotics when administered in early infancy,22, 23 was associated with a specific profile of the digestive microbiota and a causal role was strongly suggested by the microbiota transplantation experiments.24 Clostridium perfringens,21, 25, 26 C. difficile,21 C. tetani,21 C. botulinum,21 E. coli13 and M. smithii13, 14, 17 have been linked with the absence of obesity. Conversely, Lactobacillus and especially L. reuteri or L. sakei have been linked with obesity.13, 14, 19, 27, 28 A very recent study21 comparing diabetic and nondiabetic women confirms the key role of Lactobacillus in weight regulation in humans as four species, L. fermentum, L. gasseri, L. johnsonii and L. crispatus were positively correlated with BMI, whereas a single species, L. casei was negatively correlated with BMI.21 Consistently, we had previously shown that L. fermentum was associated with weight gain,27 whereas L. casei or L. plantarum were associated with the absence of obesity.14, 27 In one study on mice, L. reuteri L6798 was associated with weight gain, whereas L. reuteri ATCC PTA 4659 was associated with weight loss.29 These results suggest a species and strain specificity in the effect of Lactobacillus probiotics on weight regulation.30 Overall, Lactobacillus provided a biological plausibility for the link between vancomycin and weight gain.
The acquired obesity associated with a dramatic L. reuteri increase, whereas treated by vancomycin in one patient suggest that bacteriocins could be critical in the link between weight and the profile of the gut microbiota. Indeed, Lactobacillus and particularly L. reuteri produce broad-spectrum bacteriocins, which allow for the elimination of various enteropathogens as Listeria monocytogenes, Staphylococcus aureus, Yersinia enterocolitica, Salmonella and E. coli, the latter being associated previously to the absence of obesity.31 In addition, the weight increase in children with Kwashiorkor under treatment with ready-to-use therapeutic food (RUTF) was correlated with an increase of L. reuteri and L. gasseri, and considered to be associated with bacteriocins secretion, resulting in a dramatic gut microbiota alteration.9 Consequently, the effectiveness of antibiotic treatment to combat severe malnutrition8, 32 also supports the role of bacteriocins, as they could increase the ability of the gut microbiota to extract energy from the diet, as found in experimental models.12
Our study includes some limitations. First, all patients had parenteral antibiotic administration. The administration routes have been shown to impact significantly the shift on the gut microbial populations with oral administration being associated with more pronounced alteration of the gut microbiota,33 but intravenous administration was also associated with dramatic gut microbiota changes notably in infants.34 As a confirmation, we found in this study using intravenous route a reproducible alteration previously obtained by oral administration as a Lactobacillus increase under vancomycin. In addition, although large-scale molecular methods became recently accurate at the species level,21 studies targeting bacterial species of interest in the human gut microbiome as in our work remain completely relevant.13, 14 As such, species-specific PCR avoids some biases of large-scale molecular methods such as the primer bias.35
In conclusion, the major weight gain and acquired obesity specifically observed in some patients treated with vancomycin could be related to the selection of resistant bacteria previously associated with obesity, such as an increase in Lactobacillus, and/or to the suppression of bacteria that are associated with the absence of obesity, such as C. perfringens,21, 25, 26 C. difficile,21 C. tetani,21 C. botulinum,21 E. coli13 or M. smithii.13, 14, 17 Bacteriocins, typically secreted by Lactobacillus,31 which are selected by vancomycin, may explain why the effect of an antibiotic on a complex microbial population is much wider than the expected direct ‘in vitro’ effect, by killing populations paradoxically resistant to the antibiotic when used ‘in vivo’. As demonstrated in experimental studies,36 we demonstrated that weight gain effect following antibiotic administration depends both on the initial gastrointestinal microbiota and the antibiotic used. From our results, it seems necessary to inform the patient of the risk of weight gain and obesity during long-term antibiotic treatment, especially when the patient is treated with vancomycin. More generally, this work supports the instrumental role of the human gut microbiota in the pro-obesity effect of antibiotics as recently reported,22, 23 and suggests bacteriocins as a keystone between gut microbiota and obesity.
References
Stokstad EL, Jukes TH . The multiple nature of the animal protein factor. J Biol Chem 1949; 180: 647–654.
Summary report on antimicrobials sold or distributed for use in food-producing animals. Food and drug administration, 2009.
Antibiotic resistance back in the news. Animal Health Institute (USA). AHI quaterly 1998; 19: 1–4.
Haight TH, Pierce WE . Effect of prolonged antibiotic administration of the weight of healthy young males. J Nutr 1955; 56: 151–161.
Ozawa E . Studies on growth promotion by antibiotics. II. Results of aurofac administration to infants. J Antibiot 1955; 8: 212–214.
Robinson P . Controlled trial of aureomycin in premature twins and triplets. Lancet 1952; 259: 52.
Ley RE, Turnbaugh PJ, Klein S, Gordon JI . Microbial ecology: human gut microbes associated with obesity. Nature 2006; 444: 1022–1023.
Trehan I, Goldbach HS, LaGrone LN, Meuli GJ, Wang RJ, Maleta KM et al. Antibiotics as part of the management of severe acute malnutrition. N Engl J Med 2013; 368: 425–435.
Smith MI, Yatsunenko T, Manary MJ, Trehan I, Mkakosya R, Cheng J et al. Gut microbiomes of Malawian twin pairs discordant for kwashiorkor. Science 2013; 339: 548–554.
Feighner SD, Dashkevicz MP . Subtherapeutic levels of antibiotics in poultry feeds and their effects on weight gain, feed efficiency, and bacterial cholyltaurine hydrolase activity. Appl Environ Microbiol 1987; 53: 331–336.
Thuny F, Richet H, Casalta JP, Angelakis E, Habib G, Raoult D . Vancomycin treatment of infective endocarditis is linked with recently acquired obesity. PLoS One 2010; 5: e9074.
Cho I, Yamanishi S, Cox L, Methe BA, Zavadil J, Li K et al. Antibiotics in early life alter the murine colonic microbiome and adiposity. Nature 2012; 488: 621–626.
Million M, Angelakis E, Maraninchi M, Henry M, Giorgi R, Valero R et al. Correlation between body mass index and gut concentrations of Lactobacillus reuteri, Bifidobacterium animalis, Methanobrevibacter smithii and Escherichia coli. Int J Obes 2013. e-pub ahead of print 5 March 2013; doi:10.1038/ijo.2013.20.
Million M, Maraninchi M, Henry M, Armougom F, Richet H, Carrieri P et al. Obesity-associated gut microbiota is enriched in Lactobacillus reuteri and depleted in Bifidobacterium animalis and Methanobrevibacter smithii. Int J Obes (Lond) 2012; 36: 817–825.
Li JS, Sexton DJ, Mick N, Nettles R, Fowler VG Jr, Ryan T et al. Proposed modifications to the Duke criteria for the diagnosis of infective endocarditis. Clin Infect Dis 2000; 30: 633–638.
Botelho-Nevers E, Thuny F, Casalta JP, Richet H, Gouriet F, Collart F et al. Dramatic reduction in infective endocarditis-related mortality with a management-based approach. Arch Intern Med 2009; 169: 1290–1298.
Schwiertz A, Taras D, Schafer K, Beijer S, Bos NA, Donus C et al. Microbiota and SCFA in lean and overweight healthy subjects. Obesity 2010; 18: 190–195.
Dridi B, Henry M, El KA, Raoult D, Drancourt M . High prevalence of Methanobrevibacter smithii and Methanosphaera stadtmanae detected in the human gut using an improved DNA detection protocol. PLoS One 2009; 4: e7063.
Armougom F, Henry M, Vialettes B, Raccah D, Raoult D . Monitoring bacterial community of human gut microbiota reveals an increase in Lactobacillus in obese patients and Methanogens in anorexic patients. PLoS One 2009; 4: e7125.
Barnard GA . A New test for 2 × 2 tables. Nature 1945; 156: 783–784.
Karlsson FH, Tremaroli V, Nookaew I, Bergstrom G, Behre CJ, Fagerberg B et al. Gut metagenome in European women with normal, impaired and diabetic glucose control. Nature 2013; 498: 99–103.
Trasande L, Blustein J, Liu M, Corwin E, Cox LM, Blaser MJ . Infant antibiotic exposures and early-life body mass. Int J Obes 2012; 37: 16–23.
Ajslev TA, Andersen CS, Gamborg M, Sorensen TI, Jess T . Childhood overweight after establishment of the gut microbiota: the role of delivery mode, pre-pregnancy weight and early administration of antibiotics. Int J Obes 2011; 35: 522–529.
Million M, Raoult D . The role of the manipulation of the gut microbiota in obesity. Curr Infect Dis Rep 2013; 15: 25–30.
Lev M, Forbes M . Growth response to dietary penicillin of germ-free chicks and of chicks with a defined intestinal flora. Br J Nutr 1959; 13: 78–84.
Cole JR Jr., Boyd FM . Fat absorption from the small intestine of gnotobiotic chicks. Appl Microbiol 1967; 15: 1229–1234.
Million M, Angelakis E, Paul M, Armougom F, Leibovici L, Raoult D . Comparative meta-analysis of the effect of Lactobacillus species on weight gain in humans and animals. Microb Pathog 2012; 53: 100–108.
Stsepetova J, Sepp E, Kolk H, Loivukene K, Songisepp E, Mikelsaar M . Diversity and metabolic impact of intestinal Lactobacillus species in healthy adults and the elderly. Br J Nutr 2011; 105: 1235–1244.
Fak F, Backhed F . Lactobacillus reuteri prevents diet-induced obesity, but not atherosclerosis, in a strain dependent fashion in Apoe−/− mice. PLoS One 2012; 7: e46837.
Million M, Raoult D . Species and strain specificity of Lactobacillus probiotics effect on weight regulation. Microb Pathog 2013; 55: 52–54.
Jacobsen CN, Rosenfeldt N,V, Hayford AE, Moller PL, Michaelsen KF, Paerregaard A et al. Screening of probiotic activities of forty-seven strains of Lactobacillus spp. by in vitro techniques and evaluation of the colonization ability of five selected strains in humans. Appl Environ Microbiol 1999; 65: 4949–4956.
Dubray C, Ibrahim SA, Abdelmutalib M, Guerin PJ, Dantoine F, Belanger F et al. Treatment of severe malnutrition with 2-day intramuscular ceftriaxone vs 5-day amoxicillin. Ann Trop Paediatr 2008; 28: 13–22.
Zhang L, Huang Y, Zhou Y, Buckley T, Wang HH . Antibiotic administration routes significantly influence the levels of antibiotic resistance in gut microbiota. Antimicrob Agents Chemother 2013; 57: 3659–3666.
Fouhy F, Guinane CM, Hussey S, Wall R, Ryan CA, Dempsey EM et al. High-throughput sequencing reveals the incomplete, short-term recovery of infant gut microbiota following parenteral antibiotic treatment with ampicillin and gentamicin. Antimicrob Agents Chemother 2012; 56: 5811–5820.
Turnbaugh PJ, Quince C, Faith JJ, McHardy AC, Yatsunenko T, Niazi F et al. Organismal, genetic, and transcriptional variation in the deeply sequenced gut microbiomes of identical twins. Proc Natl Acad Sci USA 2010; 107: 7503–7508.
Dubos R, Schaedler RW, Costello RL . The effect of antibacterial drugs on the weight of mice. J Exp Med 1963; 117: 245–257.
Pirzada OM, McGaw J, Taylor CJ, Everard ML . Improved lung function and body mass index associated with long-term use of Macrolide antibiotics. J Cyst Fibros 2003; 2: 69–71.
Saiman L, Mayer-Hamblett N, Anstead M, Lands LC, Kloster M, Goss CH et al. Open-label, follow-on study of azithromycin in pediatric patients with CF uninfected with Pseudomonas aeruginosa. Pediatr Pulmonol 2012; 47: 641–648.
Clement A, Tamalet A, Leroux E, Ravilly S, Fauroux B, Jais JP . Long term effects of azithromycin in patients with cystic fibrosis: a double blind, placebo controlled trial. Thorax 2006; 61: 895–902.
Mansi Y, Abdelaziz N, Ezzeldin Z, Ibrahim R . Randomized controlled trial of a high dose of oral erythromycin for the treatment of feeding intolerance in preterm infants. Neonatology 2011; 100: 290–294.
Lane JA, Murray LJ, Harvey IM, Donovan JL, Nair P, Harvey RF . Randomised clinical trial: Helicobacter pylori eradication is associated with a significantly increased body mass index in a placebo-controlled study. Aliment Pharmacol Ther 2011; 33/8: 922–929.
Kamada T, Hata J, Kusunoki H, Ito M, Tanaka S, Kawamura Y et al. Eradication of Helicobacter pylori increases the incidence of hyperlipidaemia and obesity in peptic ulcer patients. Dig Liver Dis 2005; 37: 39–43.
Patterson PR . Minocycline in the antibiotic regimen of cystic fibrosis patients: weight gain and clinical improvement. Clin Pediatr 1977; 16: 60–63.
Edlund C, Barkholt L, Olsson-Liljequist B, Nord CE . Effect of vancomycin on intestinal flora of patients who previously received antimicrobial therapy. Clin Infect Dis 1997; 25: 729–732.
Lund B, Edlund C, Barkholt L, Nord CE, Tvede M, Poulsen RL . Impact on human intestinal microflora of an Enterococcus faecium probiotic and vancomycin. Scand J Infect Dis 2000; 32: 627–632.
Van der Auwera P, Pensart N, Korten V, Murray BE, Leclercq R . Influence of oral glycopeptides on the fecal flora of human volunteers: selection of highly glycopeptide-resistant enterococci. J Infect Dis 1996; 173: 1129–1136.
Robinson CJ, Young VB . Antibiotic administration alters the community structure of the gastrointestinal micobiota. Gut Microbes 2010; 1: 279–284.
Yap IK, Li JV, Saric J, Martin FP, Davies H, Wang Y et al. Metabonomic and microbiological analysis of the dynamic effect of vancomycin-induced gut microbiota modification in the mouse. J Proteome Res 2008; 7: 3718–3728.
Swedish Study Group. A randomized multicenter trial to compare the influence of cefaclor and amoxycillin on the colonization resistance of the digestive tract in patients with lower respiratory tract infection. Infection 1991; 19: 208–215.
Brismar B, Edlund C, Nord CE . Impact of cefpodoxime proxetil and amoxicillin on the normal oral and intestinal microflora. Eur J Clin Microbiol Infect Dis 1993; 12: 714–719.
Floor M, van AF, Rozenberg-Arska M, Visser M, Kolsters A, Beumer H et al. Effect of loracarbef and amoxicillin on the oropharyngeal and intestinal microflora of patients with bronchitis. Scand J Infect Dis 1994; 26: 191–197.
Stark CA, Adamsson I, Edlund C, Sjosted S, Seensalu R, Wikstrom B et al. Effects of omeprazole and amoxycillin on the human oral and gastrointestinal microflora in patients with Helicobacter pylori infection. J Antimicrob Chemother 1996; 38: 927–939.
Schumann A, Nutten S, Donnicola D, Comelli EM, Mansourian R, Cherbut C et al. Neonatal antibiotic treatment alters gastrointestinal tract developmental gene expression and intestinal barrier transcriptome. Physiol Genomics 2005; 23: 235–245.
Million M, Lagier JC, Yahav D, Paul M . Gut bacterial microbiota and obesity. Clin Microbiol Infect 2013; 19: 305–313.
Markle JG, Frank DN, Mortin-Toth S, Robertson CE, Feazel LM, Rolle-Kampczyk U et al. Sex differences in the gut microbiome drive hormone-dependent regulation of autoimmunity. Science 2013; 339: 1084–1088.
Acknowledgements
We thank all the cardiology departments of the Hopital de La Timone for their assistance in recruiting endocarditis patients.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivs 3.0 Unported License. To view a copy of this license, visit http://creativecommons.org/licenses/by-nc-nd/3.0/
About this article
Cite this article
Million, M., Thuny, F., Angelakis, E. et al. Lactobacillus reuteri and Escherichia coli in the human gut microbiota may predict weight gain associated with vancomycin treatment. Nutr & Diabetes 3, e87 (2013). https://doi.org/10.1038/nutd.2013.28
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nutd.2013.28
Keywords
This article is cited by
-
Perilla, sunflower, and tea seed oils as potential dietary supplements with anti-obesity effects by modulating the gut microbiota composition in mice fed a high-fat diet
European Journal of Nutrition (2023)
-
Bacteria and Methanogens in the Human Microbiome: a Review of Syntrophic Interactions
Microbial Ecology (2022)
-
The antibiotic vancomycin induces complexation and aggregation of gastrointestinal and submaxillary mucins
Scientific Reports (2020)
-
Gut microbiome diversity and high-fibre intake are related to lower long-term weight gain
International Journal of Obesity (2017)
-
Antibiotics ameliorate lupus-like symptoms in mice
Scientific Reports (2017)