Key Points
-
Cytokines are major drivers of autoimmunity, and targeting cytokines has revolutionized the treatment of rheumatologic diseases
-
Despite their success, biologic agents that target key cytokines are not completely effective in all patients
-
Type I and II cytokines signal through the JAK–STAT pathway, and pharmacological inhibition of this signal transduction pathway with small molecules can block the actions of these cytokines
-
JAK inhibitors, or Jakinibs, are effective for rheumatoid arthritis and other immune-mediated diseases
-
Many of the adverse effects of Jakinibs can be linked to action of the cytokines that are blocked
-
Jakinibs are currently being investigated for a number of new indications, and second-generation selective Jakinibs are being developed and tested
Abstract
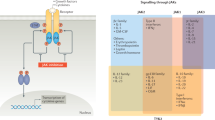
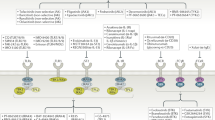
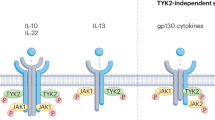
Cytokines are major drivers of autoimmunity, and biologic agents targeting cytokines have revolutionized the treatment of immune-mediated diseases. Despite the effectiveness of these drugs, they do not induce complete remission in all patients, prompting the development of alternative strategies — including targeting of intracellular signal transduction pathways downstream of cytokines. Many cytokines that bind type I and type II cytokine receptors are critical regulators of immune-mediated diseases and employ the Janus kinase (JAK) and signal transducer and activator of transcription (STAT) pathway to exert their effect. Pharmacological inhibition of JAKs blocks the actions of type I/II cytokines, and within the past 3 years therapeutic JAK inhibitors, or Jakinibs, have become available to rheumatologists. Jakinibs have proven effective for the treatment of rheumatoid arthritis and other inflammatory diseases. Adverse effects of these agents are largely related to their mode of action and include infections and hyperlipidemia. Jakinibs are currently being investigated for a number of new indications, and second-generation selective Jakinibs are being developed and tested. Targeting STATs could be a future avenue for the treatment of rheumatologic diseases, although substantial challenges remain. Nonetheless, the ability to therapeutically target intracellular signalling pathways has already created a new paradigm for the treatment of rheumatologic disease.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
McInnes, I. B. & Schett, G. The pathogenesis of rheumatoid arthritis. N. Engl. J. Med. 365, 2205–2219 (2011).
Lubberts, E. The IL-23–IL-17 axis in inflammatory arthritis. Nat. Rev. Rheumatol. 11, 415–429 (2015).
O'Shea, J. J., Ma, A. & Lipsky, P. Cytokines and autoimmunity. Nat. Rev. Immunol. 2, 37–45 (2002).
Bell, E. Inflammation: targeting TNF. Nat. Rev. Immunol. 9, 390–391 (2009).
Scott, D. L. Biologics-based therapy for the treatment of rheumatoid arthritis. Clin. Pharmacol. Ther. 91, 30–43 (2012).
O'Shea, J. J., Gadina, M. & Schreiber, R. D. Cytokine signaling in 2002. Cell 109, S121–S131 (2002).
Leonard, W. J. & O'Shea, J. J. JAKs and STATs: biological implications. Annu. Rev. Immunol. 16, 293–322 (1998).
O'Shea, J. J., Holland, S. M. & Staudt, L. M. JAKs and STATs in immunity, immunodeficiency, and cancer. N. Engl. J. Med. 368, 161–170 (2013).
Giovannoni, G. et al. Daclizumab high-yield process in relapsing-remitting multiple sclerosis (SELECTION): a multicentre, randomised, double-blind extension trial. Lancet Neurol. 13, 472–481 (2014).
Gold, R. et al. Daclizumab high-yield process in relapsing-remitting multiple sclerosis (SELECT): a randomised, double-blind, placebo-controlled trial. Lancet 381, 2167–2175 (2013).
McInnes, I. B. & Schett, G. Cytokines in the pathogenesis of rheumatoid arthritis. Nat. Rev. Immunol. 7, 429–442 (2007).
Rochman, Y., Spolski, R. & Leonard, W. J. New insights into the regulation of T cells by γc family cytokines. Nat. Rev. Immunol. 9, 480–490 (2009).
Spits, H. & Di Santo, J. P. The expanding family of innate lymphoid cells: regulators and effectors of immunity and tissue remodeling. Nat. Immunol. 12, 21–27 (2011).
Kaplan, M. H., Hufford, M. M. & Olson, M. R. The development and in vivo function of T helper 9 cells. Nat. Rev. Immunol. 15, 295–307 (2015).
Eto, D. et al. IL-21 and IL-6 are critical for different aspects of B cell immunity and redundantly induce optimal follicular helper CD4 T cell (Tfh) differentiation. PLoS ONE 6, e17739 (2011).
Kotlarz, D., Zietara, N., Milner, J. D. & Klein, C. Human IL-21 and IL-21R deficiencies: two novel entities of primary immunodeficiency. Curr. Opin. Pediatr. 26, 704–712 (2014).
Rasmussen, T. K. et al. Increased interleukin 21 (IL-21) and IL-23 are associated with increased disease activity and with radiographic status in patients with early rheumatoid arthritis. J. Rheumatol 37, 2014–2020 (2010).
Spolski, R. & Leonard, W. J. Interleukin-21: a double-edged sword with therapeutic potential. Nat. Rev. Drug Discov. 13, 379–395 (2014).
Papatriantafyllou, M. Cytokines: GM-CSF in focus. Nat. Rev. Immunol. 11, 370–371 (2011).
Burmester, G. R. et al. Efficacy and safety of mavrilimumab in subjects with rheumatoid arthritis. Ann. Rheum. Dis. 72, 1445–1452 (2013).
Cornelissen, C., Luscher-Firzlaff, J., Baron, J. M. & Luscher, B. Signaling by IL-31 and functional consequences. Eur. J. Cell Biol. 91, 552–566 (2012).
Hirahara, K. et al. Interleukin-27 priming of T cells controls IL-17 production in trans via induction of the ligand PD-L1. Immunity 36, 1017–1030 (2012).
Hirahara, K. et al. Mechanisms underlying helper T-cell plasticity: implications for immune-mediated disease. J. Allergy Clin. Immunol. 131, 1276–1287 (2013).
Hunter, C. A. & Kastelein, R. Interleukin-27: balancing protective and pathological immunity. Immunity 37, 960–969 (2012).
Griffiths, C. E. et al. Comparison of ustekinumab and etanercept for moderate-to-severe psoriasis. N. Engl. J. Med. 362, 118–128 (2010).
Neurath, M. F. Cytokines in inflammatory bowel disease. Nat. Rev. Immunol. 14, 329–342 (2014).
Higgs, B. W. et al. Patients with systemic lupus erythematosus, myositis, rheumatoid arthritis and scleroderma share activation of a common type I interferon pathway. Ann. Rheum. Dis. 70, 2029–2036 (2011).
Ronnblom, L. & Eloranta, M. L. The interferon signature in autoimmune diseases. Curr. Opin. Rheumatol 25, 248–253 (2013).
Crow, Y. J. Type I interferonopathies: a novel set of inborn errors of immunity. Ann. NY Acad. Sci. 1238, 91–98 (2011).
Rutz, S., Wang, X. & Ouyang, W. The IL-20 subfamily of cytokines — from host defence to tissue homeostasis. Nat. Rev. Immunol. 14, 783–795 (2014).
Senolt, L. et al. Efficacy and safety of anti-interleukin-20 monoclonal antibody in patients with rheumatoid arthritis: a randomized Phase IIa trial. Arthritis Rheumatol. 67, 1438–1448 (2015).
Huss, D. J. et al. In vivo maintenance of human regulatory T cells during CD25 blockade. J. Immunol. 194, 84–92 (2015).
Oh, J. et al. Daclizumab-induced adverse events in multiple organ systems in multiple sclerosis. Neurology 82, 984–988 (2014).
Ouyang, W., Rutz, S., Crellin, N. K., Valdez, P. A. & Hymowitz, S. G. Regulation and functions of the IL-10 family of cytokines in inflammation and disease. Annu. Rev. Immunol. 29, 71–109 (2011).
Greenhill, C. J. et al. Interleukin-10 regulates the inflammasome-driven augmentation of inflammatory arthritis and joint destruction. Arthritis Res. Ther. 16, 419 (2014).
Glocker, E. O., Kotlarz, D., Klein, C., Shah, N. & Grimbacher, B. IL-10 and IL-10 receptor defects in humans. Ann. NY Acad. Sci. 1246, 102–107 (2011).
da Rocha, L. F. Jr et al. Increased serum interleukin 22 in patients with rheumatoid arthritis and correlation with disease activity. J. Rheumatol 39, 1320–1325 (2012).
Shen, H., Xia, L., Xiao, W. & Lu, J. Increased levels of interleukin-27 in patients with rheumatoid arthritis. Arthritis Rheum. 63, 860–861 (2011).
Jones, G. W. et al. Interleukin-27 inhibits ectopic lymphoid-like structure development in early inflammatory arthritis. J. Exp. Med. 212, 1793–1802 (2015).
Gonzalez-Navajas, J. M., Lee, J., David, M. & Raz, E. Immunomodulatory functions of type I interferons. Nat. Rev. Immunol. 12, 125–135 (2012).
O'Shea, J. J. et al. The JAK–STAT pathway: impact on human disease and therapeutic intervention. Annu. Rev. Med. 66, 311–328 (2015).
Macchi, P. et al. Mutations of Jak-3 gene in patients with autosomal severe combined immune deficiency (SCID). Nature 377, 65–68 (1995).
Russell, S. M. et al. Mutation of Jak3 in a patient with SCID: essential role of Jak3 in lymphoid development. Science 270, 797–800 (1995).
Minegishi, Y. et al. Human tyrosine kinase 2 deficiency reveals its requisite roles in multiple cytokine signals involved in innate and acquired immunity. Immunity 25, 745–755 (2006).
Sigurdsson, S. et al. Polymorphisms in the tyrosine kinase 2 and interferon regulatory factor 5 genes are associated with systemic lupus erythematosus. Am. J. Hum. Genet. 76, 528–537 (2005).
Franke, A. et al. Genome-wide meta-analysis increases to 71 the number of confirmed Crohn's disease susceptibility loci. Nat. Genet. 42, 1118–1125 (2010).
Hu, K., Hou, S., Jiang, Z., Kijlstra, A. & Yang, P. JAK2 and STAT3 polymorphisms in a Han Chinese population with Behçet's disease. Invest. Ophthalmol. Vis. Sci. 53, 538–541 (2012).
Uzel, G. et al. Dominant gain-of-function STAT1 mutations in FOXP3 wild-type immune dysregulation-polyendocrinopathy-enteropathy-X-linked-like syndrome. J. Allergy Clin. Immunol. 131, 1611–1623 (2013).
Holland, S. M. et al. STAT3 mutations in the hyper-IgE syndrome. New Engl. J. Med. 357, 1608–1619 (2007).
Milner, J. D. et al. Early-onset lymphoproliferation and autoimmunity caused by germline STAT3 gain-of-function mutations. Blood 125, 591–599 (2015).
Cohen, A. C. et al. Cutting edge: decreased accumulation and regulatory function of CD4+CD25high T cells in human STAT5b deficiency. J. Immunol. 177, 2770–2774 (2006).
Kofoed, E. M. et al. Growth hormone insensitivity associated with a STAT5b mutation. N. Engl. J. Med. 349, 1139–1147 (2003).
Ellinghaus, D. et al. Combined analysis of genome-wide association studies for Crohn disease and psoriasis identifies seven shared susceptibility loci. Am. J. Hum. Genet. 90, 636–647 (2012).
Remmers, E. F. et al. STAT4 and the risk of rheumatoid arthritis and systemic lupus erythematosus. N. Engl. J. Med. 357, 977–986 (2007).
Duetsch, G. et al. STAT6 as an asthma candidate gene: polymorphism-screening, association and haplotype analysis in a Caucasian sib-pair study. Hum. Mol. Genet. 11, 613–621 (2002).
O'Shea, J. J., Kontzias, A., Yamaoka, K., Tanaka, Y. & Laurence, A. Janus kinase inhibitors in autoimmune diseases. Ann. Rheum. Dis. 72, ii111–ii115 (2013).
Changelian, P. S. et al. Prevention of organ allograft rejection by a specific Janus kinase 3 inhibitor. Science 302, 875–878 (2003).
Fleischmann, R. et al. Placebo-controlled trial of tofacitinib monotherapy in rheumatoid arthritis. N. Engl. J. Med. 367, 495–507 (2012).
Lee, E. B., Fleischmann, R. & Hall, S. Radiographic, clinical and functional comparison of tofacitinib monotherapy versus methotrexate in methotrexate-nai¨ve patients with rheumatoid arthritis [abstract]. Arthritis Rheum. 64 (Suppl. 10), S1049 (2012).
Burmester, G. R. et al. Tofacitinib (CP-690,550) in combination with methotrexate in patients with active rheumatoid arthritis with an inadequate response to tumour necrosis factor inhibitors: a randomised Phase 3 trial. Lancet 381, 451–460 (2013).
van der Heijde, D. et al. Tofacitinib (CP-690,550) in patients with rheumatoid arthritis receiving methotrexate: twelve-month data from a twenty-four-month Phase III randomized radiographic study. Arthritis Rheum. 65, 559–570 (2013).
van Vollenhoven, R. F. et al. Tofacitinib or adalimumab versus placebo in rheumatoid arthritis. N. Engl. J. Med. 367, 508–519 (2012).
Lee, E. B. et al. Tofacitinib versus methotrexate in rheumatoid arthritis. N. Engl. J. Med. 370, 2377–2386 (2014).
Conaghan, P. G. et al. Effects of tofacitinib on MRI enpoints in methotrexate-naive early rheumatoid arthritis: a Phase 2 MRI study with semi-quantitative and quantitative endpoints. Ann. Rheum. Dis. 74, 738 (2015).
Chiricozzi, A. et al. Tofacitinib for the treatment of moderate-to-severe psoriasis. Expert Rev. Clin. Immunol. 11, 443–455 (2015).
Bachelez, H. et al. Tofacitinib versus etanercept or placebo in moderate-to-severe chronic plaque psoriasis: a Phase 3 randomised non-inferiority trial. Lancet 386, 552–561 (2015).
Pfizer. Pfizer announces oral tofacitinib meets primary endpoints in pivotal Phase 3 psoriasis trials. Pfizer[online], (2015).
Pfizer. Pfizer receives complete response letter from FDA for oral XELJANZ® (tofacitinib citrate) supplemental new drug application for moderate to severe chronic plaque psoriasis. Pfizer[online], (2015).
Bissonnette, R. et al. Tofacitinib withdrawal and retreatment in moderate-to-severe chronic plaque psoriasis: a randomized controlled trial. Br. J. Dermatol. 172, 1395–1406 (2015).
Sandborn, W. J. et al. Tofacitinib, an oral Janus kinase inhibitor, in active ulcerative colitis. N. Engl. J. Med. 367, 616–624 (2012).
Sandborn, W. J. et al. A Phase 2 study of tofacitinib, an oral Janus kinase inhibitor, in patients with Crohn's Disease. Clin. Gastroenterol. Hepatol. 12, 1485–1493.e2 (2014).
Vincenti, F. et al. Evaluation of the effect of tofacitinib exposure on outcomes in kidney transplant patients. Am. J. Transplant 15, 1644–1653 (2015).
Fridman, J. S. et al. Selective inhibition of JAK1 and JAK2 is efficacious in rodent models of arthritis: preclinical characterization of INCB028050. J. Immunol. 184, 5298–5307 (2010).
Keystone, E. C. et al. Safety and efficacy of baricitinib at 24 weeks in patients with rheumatoid arthritis who have had an inadequate response to methotrexate. Ann. Rheum. Dis. 74, 333–340 (2015).
Smolen, J. S. et al. Patient-reported outcomes from a Phase 3 study of baricitinib in patients with rheumatoid arthritis (RA) and an inadequate response to tumor necrosis factor inhibitors. Ann. Rheum. Dis. 74, 785 (2015).
Genovese, M. C. et al. Baricitinib, an oral Janus kinase (JAK)1/JAK2 inhibitor, in patients with active rheumatoid arthritis (RA) and an inadequate response to TNF inhibitors: results of the Phase 3 RA-BEACON study [abstract OP0029]. Ann. Rheum. Dis. 74 (Suppl. 2), 75–76 (2015).
Dougados, M. et al. Baricitinib, an oral Janus kinase (JAK)1/JAK2 inhibitor, in patients with active rheumatoid arthritis (RA) and an inadequate response to cDMARD therapy: results of the Phase 3 RA-BUILD study [abstract LB0001]. Ann. Rheum. Dis. 74 (Suppl. 2), 79 (2015).
Cosgrove, S. B. et al. A blinded, randomized, placebo-controlled trial of the efficacy and safety of the Janus kinase inhibitor oclacitinib (Apoquel®) in client-owned dogs with atopic dermatitis. Vet. Dermatol. 24, 587–597 (2013).
Gonzales, A. J. et al. Oclacitinib (APOQUEL®) is a novel Janus kinase inhibitor with activity against cytokines involved in allergy. J. Vet. Pharmacol. Ther. 37, 317–324 (2014).
Kremer, J. M. et al. Evaluation of the effect of tofacitinib on measured glomerular filtration rate in patients with active rheumatoid arthritis: results from a randomised controlled trial. Arthritis Res. Ther. 17, 95 (2015).
Curtis, J. et al. Analysis of non-melanoma skin cancer across the tofacitinib rheumatoid arthritis clinical programme [abstract THU0174]. Ann. Rheum. Dis. 74 (Suppl. 2), 257 (2015).
Wollenhaupt, J. et al. Safety and efficacy of tofacitinib, an oral janus kinase inhibitor, for the treatment of rheumatoid arthritis in open-label, longterm extension studies. J. Rheumatol 41, 837–852 (2014).
He, Y. et al. Efficacy and safety of tofacitinib in the treatment of rheumatoid arthritis: a systematic review and meta-analysis. BMC Musculoskelet. Disord. 14, 298 (2013).
Winthrop, K. L. et al. Herpes zoster and tofacitinib therapy in patients with rheumatoid arthritis. Arthritis Rheumatol. 66, 2675–2684 (2014).
Freud, A. G., Yu, J. & Caligiuri, M. A. Human natural killer cell development in secondary lymphoid tissues. Semin. Immunol. 26, 132–137 (2014).
Valenzuela, F. et al. Effects of tofacitinib on lymphocyte sub-populations, CMV and EBV viral load in patients with plaque psoriasis. BMC Dermatol. 15, 8 (2015).
van Vollenhoven, R. F. et al. Relationship between NK cell count and important safety events in rheumatoid arthritis patients treated with tofacitinib [abstract THU0178]. Ann. Rheum. Dis. 74 (Suppl. 2), 258–259 (2015).
Winthrop, K. L. et al. The effect of tofacitinib on pneumococcal and influenza vaccine responses in rheumatoid arthritis. Ann. Rheum. Dis. http://dx.doi.org/10.1136/annrheumdis-2014-207191 (2015).
Vincenti, F. et al. Randomized Phase 2b trial of tofacitinib (CP-690,550) in de novo kidney transplant patients: efficacy, renal function and safety at 1 year. Am. J. Transplant. 12, 2446–2456 (2012).
Migita, K. et al. Effects of Janus kinase inhibitor tofacitinib on circulating serum amyloid A and interleukin-6 during treatment for rheumatoid arthritis. Clin. Exp. Immunol. 175, 208–214 (2014).
Scheller, J., Garbers, C. & Rose-John, S. Interleukin-6: from basic biology to selective blockade of pro-inflammatory activities. Semin. Immunol. 26, 2–12 (2014).
Souto, A. et al. Lipid profile changes in patients with chronic inflammatory arthritis treated with biologic agents and tofacitinib in randomized clinical trials: a systematic review and meta-analysis. Arthritis Rheumatol. 67, 117–127 (2015).
Kume, K. Tofacitinib improves arterial stiffness despite up-regulating serum cholesterol with chronic cardiovascular disease in methotrexate-resistant active rheumatoid arthritis patients. A cohort study [abstract 486]. ACRabstracts [online], (2014).
Charles-Schoeman, C. et al. Potential mechanisms leading to the abnormal lipid profile in patients with rheumatoid arthritis versus healthy volunteers and reversal by tofacitinib. Arthritis Rheumatol. 67, 616–625 (2015).
Moisan, A. et al. White-to-brown metabolic conversion of human adipocytes by JAK inhibition. Nat. Cell Biol. 17, 57–67 (2015).
Mittal, D., Gubin, M. M., Schreiber, R. D. & Smyth, M. J. New insights into cancer immunoediting and its three component phases — elimination, equilibrium and escape. Curr. Opin. Immunol. 27, 16–25 (2014).
U.S. Food and Drug Administration. FDA approves Actemra to treat rare form of juvenile arthritis. [online], (2011).
Genentech. Medicine offers a new option for the treatment of polyarticular juvenile idiopathic arthritis (PJIA). Genetech [online], (2013).
Salvarani, C. et al. Tocilizumab: a novel therapy for patients with large-vessel vasculitis. Rheumatology (Oxford) 51, 151–156 (2012).
Unizony, S. et al. Tocilizumab for the treatment of large-vessel vasculitis (giant cell arteritis, Takayasu arteritis) and polymyalgia rheumatica. Arthritis Care Res. (Hoboken) 64, 1720–1729 (2012).
Okuda, Y. et al. Comparison of the clinical utility of tocilizumab and anti-TNF therapy in AA amyloidosis complicating rheumatic diseases. Mod. Rheumatol. 24, 137–143 (2014).
Sieper, J., Porter-Brown, B., Thompson, L., Harari, O. & Dougados, M. Assessment of short-term symptomatic efficacy of tocilizumab in ankylosing spondylitis: results of randomised, placebo-controlled trials. Ann. Rheum. Dis. 73, 95–100 (2014).
Elhai, M. et al. Outcomes of patients with systemic sclerosis-associated polyarthritis and myopathy treated with tocilizumab or abatacept: a EUSTAR observational study. Ann. Rheum. Dis. 72, 1217–1220 (2013).
Narazaki, M. et al. Therapeutic effect of tocilizumab on two patients with polymyositis. Rheumatology (Oxford) 50, 1344–1346 (2011).
Jabbari, A. et al. Reversal of alopecia areata following treatment with the JAK1/2 inhibitor baricitinib. EBioMedicine 2, 351–355 (2015).
Craiglow, B. G. & King, B. A. Killing two birds with one stone: oral tofacitinib reverses alopecia universalis in a patient with plaque psoriasis. J. Invest. Dermatol. 134, 2988–2990 (2014).
Pieri, L., Guglielmelli, P. & Vannucchi, A. M. Ruxolitinib-induced reversal of alopecia universalis in a patient with essential thrombocythemia. Am. J. Hematol. 90, 82–83 (2015).
Xing, L. et al. Alopecia areata is driven by cytotoxic T lymphocytes and is reversed by JAK inhibition. Nat. Med. 20, 1043–1049 (2014).
Craiglow, B. G. & King, B. A. Tofacitinib citrate for the treatment of vitiligo: a pathogenesis-directed therapy. JAMA Dermatol. 151, 1110–1112 (2015).
Harel, S. et al. Pharmacologic inhibition of JAK–STAT signaling promotes hair growth. Sci. Adv. 1, e1500973–e1500973 (2015).
Bennett, L. et al. Interferon and granulopoiesis signatures in systemic lupus erythematosus blood. J. Exp. Med. 197, 711–723 (2003).
Banchereau, J. & Pascual, V. Type I interferon in systemic lupus erythematosus and other autoimmune diseases. Immunity 25, 383–392 (2006).
Hornung, T. et al. Remission of recalcitrant dermatomyositis treated with ruxolitinib. N. Engl. J. Med. 371, 2537–2538 (2014).
Liu, Y. et al. Activated STING in a vascular and pulmonary syndrome. N. Engl. J. Med. 371, 507–518 (2014).
Montealegre Sanchez, G. A. et al. Lipodystrophy and elevated temperatures (CANDLE): clinical characterization and initial response to Janus kinase inhibition with baricitinib [abstract]. Arthritis Rheum. 65 (Suppl. 10), S758–S759 (2013).
Liew, S. H. et al. Tofacitinib (CP-690,550), a Janus kinase inhibitor for dry eye disease: results from a Phase 1/2 trial. Ophthalmology 119, 1328–1335 (2012).
Vanhoutte, F. P. et al. Efficacy and safety of GLPG0634, a selective JAK1 inhibitor, after short-term treatment of rheumatoid arthritis; results of a Phase IIA trial [abstract OP0263]. Ann. Rheum. Dis. 71 (Suppl. 3), 145 (2012).
Fleischmann, R. M. et al. A randomized, double-blind, placebo-controlled, twelve-week, dose-ranging study of decernotinib, an oral selective JAK-3 inhibitor, as monotherapy in patients with active rheumatoid arthritis. Arthritis Rheumatol. 67, 334–343 (2015).
Genovese, M. C., van Vollenhoven, R. F., Pacheco-Tena, C., Zhang, Y. & Kinnman, N. VX-509 (decernotinib), an oral selective Janus kinase 3 inhibitor, in combination with methotrexate in patients with rheumatoid arthritis. Arthritis Rheumatol. http://dx.doi.org/10.1002/art.39473 (2015).
London, N. et al. Covalent docking of large libraries for the discovery of chemical probes. Nat. Chem. Biol. 10, 1066–1072 (2014).
Koo, M. Y. et al. Selective inhibition of the function of tyrosine-phosphorylated STAT3 with a phosphorylation site-specific intrabody. Proc. Natl Acad. Sci. USA 111, 6269–6274 (2014).
Santoni, M. et al. Investigational therapies targeting signal transducer and activator of transcription 3 for the treatment of cancer. Expert Opin. Investig. Drugs 24, 809–824 (2015).
Acknowledgements
The work of D.M.S., M.G. and J.J.O'S. is supported by the Intramural Research Program of the National Institute of Arthritis and Musculoskeletal and Skin Diseases of the NIH.
Author information
Authors and Affiliations
Contributions
All authors researched the data, provided a substantial contribution to discussions of the content, contributed to writing the article, and reviewed/edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
J.J.O'S. declares that he and the US Government receive royalties based on patents related to targeting Janus kinases. J.J.O'S. and M.G. and the US Government have had longstanding Cooperative Research and Development Agreements with Pfizer, which produces tofacitinib, a Janus kinase inhibitor.
Related links
FURTHER INFORMATION
Rights and permissions
About this article
Cite this article
Schwartz, D., Bonelli, M., Gadina, M. et al. Type I/II cytokines, JAKs, and new strategies for treating autoimmune diseases. Nat Rev Rheumatol 12, 25–36 (2016). https://doi.org/10.1038/nrrheum.2015.167
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrrheum.2015.167
This article is cited by
-
Evaluation of the effect of ozonated water in treatment of denture stomatitis associated with removable prosthetics
Bulletin of the National Research Centre (2024)
-
The efficacy and safety of deucravacitinib compared to methotrexate, in patients with vulvar lichen planus who have failed topical therapy with potent corticosteroids: a study protocol for a single-centre double-blinded randomised controlled trial
Trials (2024)
-
Impact of Upadacitinib on Laboratory Parameters and Related Adverse Events in Patients with RA: Integrated Data Up to 6.5 Years
Rheumatology and Therapy (2024)
-
Medicinal chemistry perspective of JAK inhibitors: synthesis, biological profile, selectivity, and structure activity relationship
Molecular Diversity (2024)
-
Evolving cognition of the JAK-STAT signaling pathway: autoimmune disorders and cancer
Signal Transduction and Targeted Therapy (2023)