Abstract
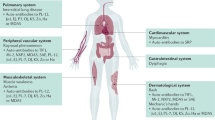
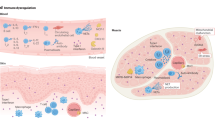
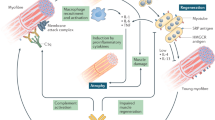
The inflammatory myopathies—collectively, myositis—are a heterogeneous group of chronic muscle disorders that differ in response to immunosuppressive treatment. Insufficient knowledge of the molecular pathways that drive pathogenesis (and underlie the clinical differences between subtypes) has hindered accurate classification, which in turn has been detrimental for clinical research. Nevertheless, new insights into pathogenesis are paving the way for improvements in diagnosis, classification and treatment. Accumulating data suggest that both immune and nonimmune mechanisms cause muscle weakness. Phenotyping of the T cells that accumulate in muscle tissue has identified proinflammatory, apoptosis resistant and cytotoxic CD4+ and CD8+ CD28null populations. Several myositis-specific autoantibodies have been identified, associated with distinct clinical phenotypes. Thus, adaptive immunity is involved in pathogenesis, and both T and B cells are interesting targets for therapy. Furthermore, genotyping has revealed activation of the type I interferon pathway in patients with dermatomyositis or with expression of particular autoantibodies. Decreased release of Ca2+ from the sarcoplasmic reticulum, as a consequence of release of proinflammatory cytokines and high mobility group protein B1, might contribute to muscle weakness, and nonimmune mechanisms potentially include a role for endoplasmic reticulum stress, autophagy and hypoxia. Deeper understanding, careful phenotyping of patients—and new classification criteria—will expedite clinical research.
Key Points
-
Myositis is a heterogeneous group of chronic inflammatory muscle disorders, the origins of which are not yet clear and for which efficient treatment is largely lacking
-
Recent findings suggest that both immune and nonimmune mechanisms are involved in the pathogenesis of myositis, and that different molecular pathways might predominate in different subsets of myositis
-
The immune mechanisms involve immune cells—T cells, B cells, dendritic cells and macrophages—and their products, such as cytokines and antibodies
-
Myositis-specific autoantibodies are helpful in the diagnosis of myositis, they identify different clinical subsets of myositis, and they might be important for differentiating pathogenic mechanisms between patients with myositis
-
Among nonimmune pathogenic mechanisms, there seem to be roles for endoplasmic reticulum stress, hypoxia and autophagy, contributing to the cause of muscle weakness
-
New classification criteria are needed to identify more homogenous subsets of patients, and subsets that are likely to share molecular pathways
-
Studying the outcomes of targeted therapies will facilitate understanding of disease mechanisms
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Dalakas, M. C. Polymyositis, dermatomyositis and inclusion-body myositis. N. Engl. J. Med. 325, 1487–1498 (1991).
Dalakas, M. C. & Hohlfeld, R. Polymyositis and dermatomyositis. Lancet 362, 971–982 (2003).
Plotz, P. H. et al. Current concepts in the idiopathic inflammatory myopathies: polymyositis, dermatomyositis, and related disorders. Ann. Intern. Med. 111, 143–157 (1989).
Li, C. K. et al. Overexpression of MHC class I heavy chain protein in young skeletal muscle leads to severe myositis: implications for juvenile myositis. Am. J. Pathol. 175, 1030–1040 (2009).
Nagaraju, K. et al. Activation of the endoplasmic reticulum stress response in autoimmune myositis: potential role in muscle fiber damage and dysfunction. Arthritis Rheum. 52, 1824–1835 (2005).
Askanas, V. & Engel, W. K. Inclusion-body myositis: a myodegenerative conformational disorder associated with Aβ, protein misfolding, and proteasome inhibition. Neurology 66, S39–S48 (2006).
Greenberg, S. A. How citation distortions create unfounded authority: analysis of a citation network. BMJ 339, b2680 (2009).
Christopher-Stine, L. et al. A novel autoantibody recognizing 200-kd and 100-kd proteins is associated with an immune-mediated necrotizing myopathy. Arthritis Rheum. 62, 2757–2766 (2010).
Hengstman, G. J. et al. Anti-signal recognition particle autoantibodies: marker of a necrotising myopathy. Ann. Rheum. Dis. 65, 1635–1638 (2006).
de Padilla, C. M. & Reed, A. M. Dendritic cells and the immunopathogenesis of idiopathic inflammatory myopathies. Curr. Opin. Rheumatol. 20, 669–674 (2008).
Reed, A. M. & Ernste, F. The inflammatory milieu in idiopathic inflammatory myositis. Curr. Rheumatol. Rep. 11, 295–301 (2009).
Szodoray, P. et al. Idiopathic inflammatory myopathies, signified by distinctive peripheral cytokines, chemokines and the TNF family members B-cell activating factor and a proliferation inducing ligand. Rheumatology (Oxford) 49, 1867–1877 (2010).
Englund, P., Lindroos, E., Nennesmo, I., Klareskog, L. & Lundberg, I. E. Skeletal muscle fibers express major histocompatibility complex class II antigens independently of inflammatory infiltrates in inflammatory myopathies. Am. J. Pathol. 159, 1263–1273 (2001).
Behrens, L. et al. Human muscle cells express a functional costimulatory molecule distinct from B7.1 (CD80) and B7.2 (CD86) in vitro and in inflammatory lesions. J. Immunol. 161, 5943–5951 (1998).
Hofbauer, M. et al. Clonal tracking of autoaggressive T cells in polymyositis by combining laser microdissection, single-cell PCR, and CDR3-spectratype analysis. Proc. Natl Acad. Sci. USA 100, 4090–4095 (2003).
Fasth, A. E. et al. T cell infiltrates in the muscles of patients with dermatomyositis and polymyositis are dominated by CD28null T cells. J. Immunol. 183, 4792–4799 (2009).
Pandya, J. M. et al. Expanded TCR-Vβ restricted T cells from sporadic inclusion body myositis patients are proinflammatory and cytotoxic CD28(null) T cells. Arthritis Rheum. 62, 3457–3466 (2010).
Fasth, A. E., Bjorkstrom, N. K., Anthoni, M., Malmberg, K. J. & Malmstrom, V. Activating NK-cell receptors co-stimulate CD4(+)CD28(–) T cells in patients with rheumatoid arthritis. Eur. J. Immunol. 40, 378–387 (2010).
Bettelli, E., Korn, T., Oukka, M. & Kuchroo, V. K. Induction and effector functions of T(H)17 cells. Nature 453, 1051–1057 (2008).
Page, G. et al. Plasma cell-like morphology of Th1-cytokine-producing cells associated with the loss of CD3 expression. Am. J. Pathol. 164, 409–417 (2004).
Chevrel, G. et al. Interleukin-17 increases the effects of IL-1β on muscle cells: arguments for the role of T cells in the pathogenesis of myositis. J. Neuroimmunol. 137, 125–133 (2003).
Waschbisch, A., Schwab, N., Ruck, T., Stenner, M. P. & Wiendl, H. FOXP3+ T regulatory cells in idiopathic inflammatory myopathies. J. Neuroimmunol. 225, 137–142 (2010).
Banica, L. et al. Quantification and molecular characterization of regulatory T cells in connective tissue diseases. Autoimmunity 42, 41–49 (2009).
Greenberg, S. A. et al. Plasma cells in muscle in inclusion body myositis and polymyositis. Neurology 65, 1782–1787 (2005).
De Bleecker, J. L., Engel, A. G. & Butcher, E. C. Peripheral lymphoid tissue-like adhesion molecule expression in nodular infiltrates in inflammatory myopathies. Neuromuscul. Disord. 6, 255–260 (1996).
Bradshaw, E. M. et al. A local antigen-driven humoral response is present in the inflammatory myopathies. J. Immunol. 178, 547–556 (2007).
Levine, T. D. Rituximab in the treatment of dermatomyositis: an open-label pilot study. Arthritis Rheum. 52, 601–607 (2005).
Majmudar, S., Hall, H. A. & Zimmermann, B. Treatment of adult inflammatory myositis with rituximab: an emerging therapy for refractory patients. J. Clin. Rheumatol. 15, 338–340 (2009).
Rios Fernandez, R., Callejas Rubio, J. L., Sanchez Cano, D., Saez Moreno, J. A. & Ortego Centeno, N. Rituximab in the treatment of dermatomyositis and other inflammatory myopathies. A report of 4 cases and review of the literature. Clin. Exp. Rheumatol. 27, 1009–1016 (2009).
Tournadre, A. et al. Polymyositis and pemphigus vulgaris in a patient: successful treatment with rituximab. Joint Bone Spine 75, 728–729 (2008).
Vandenbroucke, E. et al. Rituximab in life threatening antisynthetase syndrome. Rheumatol. Int. 29, 1499–1502 (2009).
Page, G., Chevrel, G. & Miossec, P. Anatomic localization of immature and mature dendritic cell subsets in dermatomyositis and polymyositis: interaction with chemokines and Th1 cytokine-producing cells. Arthritis Rheum. 50, 199–208 (2004).
Eloranta, M. L. et al. A possible mechanism for endogenous activation of the type I interferon system in myositis patients with anti-Jo-1 or anti-Ro 52/anti-Ro 60 autoantibodies. Arthritis Rheum. 56, 3112–3124 (2007).
Greenberg, S. A. et al. Interferon α/β-mediated innate immune mechanisms in dermatomyositis. Ann. Neurol. 57, 664–678 (2005).
McNiff, J. M. & Kaplan, D. H. Plasmacytoid dendritic cells are present in cutaneous dermatomyositis lesions in a pattern distinct from lupus erythematosus. J. Cutan. Pathol. 35, 452–456 (2008).
Civatte, M. et al. Expression of the β chemokines CCL3, CCL4, CCL5 and their receptors in idiopathic inflammatory myopathies. Neuropathol. Appl. Neurobiol. 31, 70–79 (2005).
Confalonieri, P. et al. Increased expression of β-chemokines in muscle of patients with inflammatory myopathies. J. Neuropathol. Exp. Neurol. 59, 164–169 (2000).
De Paepe, B. & De Bleecker, J. L. β-Chemokine receptor expression in idiopathic inflammatory myopathies. Muscle Nerve 31, 621–627 (2005).
Rostasy, K. M. et al. Monocyte/macrophage differentiation in dermatomyositis and polymyositis. Muscle Nerve 30, 225–230 (2004).
Stone, K. B. et al. Anti-Jo-1 antibody levels correlate with disease activity in idiopathic inflammatory myopathy. Arthritis Rheum. 56, 3125–3131 (2007).
Brouwer, R. et al. Autoantibody profiles in the sera of European patients with myositis. Ann. Rheum. Dis. 60, 116–123 (2001).
Mahouachi, R. et al. Antisynthetase syndrome [French]. Tunis Med. 86, 195–196 (2008).
Jordan Greco, A. S., Métrailler, J. C. & Dayer, E. The antisynthetase syndrome: a cause of rapidly progressive interstitial lung disease. Rev. Med. Suisse 3, 2675–2676, 2679–2681 (2007).
Gomard-Mennesson, E. et al. Clinical significance of anti-histidyl-tRNA synthetase (Jo1) autoantibodies. Ann. NY Acad. Sci. 1109, 414–420 (2007).
Genth, E. Inflammatory muscle diseases: dermatomyositis, polymyositis, and inclusion body myositis [German]. Internist (Berl.) 46, 1218–1232 (2005).
Legout, L. et al. The antisynthetase syndrome: a subgroup of inflammatory myopathies not to be unrecognized [French]. Rev. Med. Interne 23, 273–282 (2002).
Mammen, A. L. et al. Expression of the dermatomyositis autoantigen Mi-2 in regenerating muscle. Arthritis Rheum. 60, 3784–3793 (2009).
Kaji, K. et al. Identification of a novel autoantibody reactive with 155 and 140 kDa nuclear proteins in patients with dermatomyositis: an association with malignancy. Rheumatology (Oxford) 46, 25–28 (2007).
Targoff, I. N. et al. A novel autoantibody to a 155-kd protein is associated with dermatomyositis. Arthritis Rheum. 54, 3682–3689 (2006).
Sato, S. et al. RNA helicase encoded by melanoma differentiation-associated gene 5 is a major autoantigen in patients with clinically amyopathic dermatomyositis: association with rapidly progressive interstitial lung disease. Arthritis Rheum. 60, 2193–2200 (2009).
Levine, S. M. et al. Novel conformation of histidyl-transfer RNA synthetase in the lung: the target tissue in Jo-1 autoantibody-associated myositis. Arthritis Rheum. 56, 2729–2739 (2007).
Soejima, M. et al. Role of innate immunity in a model of histidyl-tRNA synthetase (Jo-1)-mediated myositis. Arthritis Rheum. (2010).
Katsumata, Y. et al. Species-specific immune responses generated by histidyl-tRNA synthetase immunization are associated with muscle and lung inflammation. J. Autoimmun. 29, 174–186 (2007).
Lovgren, T. et al. Induction of interferon-α by immune complexes or liposomes containing systemic lupus erythematosus autoantigen- and Sjögren's syndrome autoantigen-associated RNA. Arthritis Rheum. 54, 1917–1927 (2006).
Barbasso Helmers, S. et al. Sera from anti-Jo-1-positive patients with polymyositis and interstitial lung disease induce expression of intercellular adhesion molecule 1 in human lung endothelial cells. Arthritis Rheum. 60, 2524–2530 (2009).
Grundtman, C. et al. Immunolocalization of interleukin-1 receptors in the sarcolemma and nuclei of skeletal muscle in patients with idiopathic inflammatory myopathies. Arthritis Rheum. 56, 674–687 (2007).
Lundberg, I., Ulfgren, A. K., Nyberg, P., Andersson, U. & Klareskog, L. Cytokine production in muscle tissue of patients with idiopathic inflammatory myopathies. Arthritis Rheum. 40, 865–874 (1997).
St. Pierre, B. A., Kasper, C. E. & Lindsey, A. M. Fatigue mechanisms in patients with cancer: effects of tumor necrosis factor and exercise on skeletal muscle. Oncol. Nurs. Forum 19, 419–425 (1992).
Tateyama, M. et al. Expression of tumor necrosis factor-α in muscles of polymyositis. J. Neurol. Sci. 146, 45–51 (1997).
Krystufkova, O. et al. Increased serum levels of B cell activating factor (BAFF) in subsets of patients with idiopathic inflammatory myopathies. Ann. Rheum. Dis. 68, 836–843 (2009).
Walsh, R. J. et al. Type I interferon-inducible gene expression in blood is present and reflects disease activity in dermatomyositis and polymyositis. Arthritis Rheum. 56, 3784–3792 (2007).
Serrano, A. L., Baeza-Raja, B., Perdiguero, E., Jardi, M. & Munoz-Canoves, P. Interleukin-6 is an essential regulator of satellite cell-mediated skeletal muscle hypertrophy. Cell. Metab. 7, 33–44 (2008).
Scuderi, F., Mannella, F., Marino, M., Provenzano, C. & Bartoccioni, E. IL-6-deficient mice show impaired inflammatory response in a model of myosin-induced experimental myositis. J. Neuroimmunol 176, 9–15 (2006).
Sugiura, T. et al. Increased IL-15 production of muscle cells in polymyositis and dermatomyositis. Int. Immunol. 14, 917–924 (2002).
Suzuki, J. et al. Serum levels of interleukin 15 in patients with rheumatic diseases. J. Rheumatol. 28, 2389–2391 (2001).
Chiu, W. K., Fann, M. & Weng, N. P. Generation and growth of CD28nullCD8+ memory T cells mediated by IL-15 and its induced cytokines. J. Immunol. 177, 7802–7810 (2006).
Furmanczyk, P. S. & Quinn, L. S. Interleukin-15 increases myosin accretion in human skeletal myogenic cultures. Cell Biol. Int. 27, 845–851 (2003).
Andersson, U. & Harris, H. E. The role of HMGB1 in the pathogenesis of rheumatic disease. Biochim. Biophys. Acta 1799, 141–148 (2010).
Kokkola, R. et al. Successful treatment of collagen-induced arthritis in mice and rats by targeting extracellular high mobility group box chromosomal protein 1 activity. Arthritis Rheum. 48, 2052–2058 (2003).
Jiang, W. & Pisetsky, D. S. Mechanisms of disease: the role of high-mobility group protein 1 in the pathogenesis of inflammatory arthritis. Nat. Clin. Pract. Rheumatol. 3, 52–58 (2007).
Ulfgren, A. K. et al. Down-regulation of the aberrant expression of the inflammation mediator high mobility group box chromosomal protein 1 in muscle tissue of patients with polymyositis and dermatomyositis treated with corticosteroids. Arthritis Rheum. 50, 1586–1594 (2004).
Grundtman, C. et al. Effects of HMGB1 on in vitro responses of isolated muscle fibers and functional aspects in skeletal muscles of idiopathic inflammatory myopathies. FASEB J. 24, 570–578 (2010).
Alexanderson, H. et al. Patients with idiopathic inflammatory myopathies have low muscle endurance rather than low muscle strength [abstract 823]. Arthritis Rheum. 60 (Suppl.), S307 (2009).
Emslie-Smith, A. M. & Engel, A. G. Microvascular changes in early and advanced dermatomyositis: a quantitative study. Ann. Neurol. 27, 343–356 (1990).
Estruch, R. et al. Microvascular changes in skeletal muscle in idiopathic inflammatory myopathy. Hum. Pathol. 23, 888–895 (1992).
Grundtman, C., Tham, E., Ulfgren, A. K. & Lundberg, I. E. Vascular endothelial growth factor is highly expressed in muscle tissue of patients with polymyositis and patients with dermatomyositis. Arthritis Rheum. 58, 3224–3238 (2008).
Probst-Cousin, S., Neundorfer, B. & Heuss, D. Microvasculopathic neuromuscular diseases: lessons from hypoxia-inducible factors. Neuromuscul. Disord. 20, 192–197 (2010).
Dastmalchi, M. et al. Effect of physical training on the proportion of slow-twitch type I muscle fibers, a novel nonimmune-mediated mechanism for muscle impairment in polymyositis or dermatomyositis. Arthritis Rheum. 57, 1303–1310 (2007).
Nader, G. A. et al. A longitudinal, integrated, clinical, histological and mRNA profiling study of resistance exercise in myositis. Mol. Med. 16, 455–464 (2010).
Park, J. H. et al. Use of magnetic resonance imaging and P-31 magnetic resonance spectroscopy to detect and quantify muscle dysfunction in the amyopathic and myopathic variants of dermatomyositis. Arthritis Rheum. 38, 68–77 (1995).
Hamada, T. et al. Extracellular high mobility group box chromosomal protein 1 is a coupling factor for hypoxia and inflammation in arthritis. Arthritis Rheum. 58, 2675–2685 (2008).
Kim, I., Xu, W. & Reed, J. C. Cell death and endoplasmic reticulum stress: disease relevance and therapeutic opportunities. Nat. Rev. Drug Discov. 7, 1013–1030 (2008).
Hosoi, T. & Ozawa, K. Endoplasmic reticulum stress in disease: mechanisms and therapeutic opportunities. Clin. Sci. (Lond.) 118, 19–29 (2010).
Delaunay, A. et al. The ER-bound RING finger protein 5 (RNF5/RMA1) causes degenerative myopathy in transgenic mice and is deregulated in inclusion body myositis. PLoS ONE 3, e1609 (2008).
van der Pas, J., Hengstman, G. J., ter Laak, H. J., Borm, G. F. & van Engelen, B. G. Diagnostic value of MHC class I staining in idiopathic inflammatory myopathies. J. Neurol. Neurosurg. Psychiatry 75, 136–139 (2004).
Salomonsson, S. et al. Upregulation of MHC class I in transgenic mice results in reduced force-generating capacity in slow-twitch muscle. Muscle Nerve 39, 674–682 (2009).
Henriques-Pons, A. & Nagaraju, K. Nonimmune mechanisms of muscle damage in myositis: role of the endoplasmic reticulum stress response and autophagy in the disease pathogenesis. Curr. Opin. Rheumatol. 21, 581–587 (2009).
Askanas, V., Engel, W. K. & Nogalska, A. Inclusion body myositis: a degenerative muscle disease associated with intra-muscle fiber multi-protein aggregates, proteasome inhibition, endoplasmic reticulum stress and decreased lysosomal degradation. Brain Pathol. 19, 493–506 (2009).
Nagaraju, K. et al. The inhibition of apoptosis in myositis and in normal muscle cells. J. Immunol. 164, 5459–5465 (2000).
Shtifman, A. et al. Amyloid-β protein impairs Ca(2+) release and contractility in skeletal muscle. Neurobiol. Aging 31, 2080–2090 (2010).
Temiz, P., Weihl, C. C. & Pestronk, A. Inflammatory myopathies with mitochondrial pathology and protein aggregates. J. Neurol. Sci. 278, 25–29 (2009).
Nogalska, A., D'Agostino, C., Terracciano, C., Engel, W. K. & Askanas, V. Impaired autophagy in sporadic inclusion-body myositis and in endoplasmic reticulum stress-provoked cultured human muscle fibers. Am. J. Pathol. 177, 1377–1387 (2010).
Bohan, A. & Peter, J. B. Polymyositis and dermatomyositis (first of two parts). N. Engl. J. Med. 292, 344–347 (1975).
Tanimoto, K. et al. Classification criteria for polymyositis and dermatomyositis. J. Rheumatol. 22, 668–674 (1995).
Hoogendijk, J. E. et al. 119th ENMC international workshop: trial design in adult idiopathic inflammatory myopathies, with the exception of inclusion body myositis, 10–12 October 2003, Naarden, The Netherlands. Neuromuscul. Disord. 14, 337–345 (2004).
Engel, A. G. & Arahata, K. Mononuclear cells in myopathies: quantitation of functionally distinct subsets, recognition of antigen-specific cell-mediated cytotoxicity in some diseases, and implications for the pathogenesis of the different inflammatory myopathies. Hum. Pathol. 17, 704–721 (1986).
Arahata, K. & Engel, A. G. Monoclonal antibody analysis of mononuclear cells in myopathies. III: Immunoelectron microscopy aspects of cell-mediated muscle fiber injury. Ann. Neurol. 19, 112–125 (1986).
National Institue of Environmental Health Sciences. International Myositis Assessment and Clinical Research (IMACS) [online], (2011).
Dalakas, M. C. Immunotherapy of myositis: issues, concerns and future prospects. Nat. Rev. Rheumatol. 6, 129–137 (2010).
Vencovsky, J. et al. Cyclosporine A versus methotrexate in the treatment of polymyositis and dermatomyositis. Scand. J. Rheumatol. 29, 95–102 (2000).
Caramaschi, P., Volpe, A., Carletto, A., Bambara, L. M. & Biasi, D. Long-standing refractory polymyositis responding to mycophenolate mofetil: a case report and review of the literature. Clin. Rheumatol. 26, 1795–1796 (2007).
Gelber, A. C., Nousari, H. C. & Wigley, F. M. Mycophenolate mofetil in the treatment of severe skin manifestations of dermatomyositis: a series of 4 cases. J. Rheumatol 27, 1542–1545 (2000).
López de la Osa, A., Sánchez Tapia, C., Arias Díaz, M. & Terrancle de Juan, I. Antisynthetase syndrome with good response to mycophenolate mofetil [Spanish]. Rev. Clin. Esp. 207, 269–270 (2007).
Dalakas, M. C. et al. A controlled trial of high-dose intravenous immune globulin infusions as treatment for dermatomyositis. N. Engl. J. Med. 329, 1993–2000 (1993).
Barbasso Helmers, S. et al. Limited effects of high-dose intravenous immunoglobulin (IVIG) treatment on molecular expression in muscle tissue of patients with inflammatory myopathies. Ann. Rheum. Dis. 66, 1276–1283 (2007).
Wilkes, M. R., Sereika, S. M., Fertig, N., Lucas, M. R. & Oddis, C. V. Treatment of antisynthetase-associated interstitial lung disease with tacrolimus. Arthritis Rheum. 52, 2439–2446 (2005).
Haroon, M. & Devlin, J. Rituximab as a first-line agent for the treatment of dermatomyositis. Rheumatol. Int. doi:10.1007/S00296-010-1458-6.
Furlan, A., Botsios, C., Ruffatti, A., Todesco, S. & Punzi, L. Antisynthetase syndrome with refractory polyarthritis and fever successfully treated with the IL-1 receptor antagonist, anakinra: A case report. Joint Bone Spine 75, 366–367 (2008).
Dorph, C. et al. Anakinra in patients with refractory idiopathic inflammatory myopathies [abstract 589]. Arthritis Rheum. 60 (Suppl.) S218 (2009).
Dastmalchi, M. et al. A high incidence of disease flares in an open pilot study of infliximab in patients with refractory inflammatory myopathies. Ann. Rheum. Dis. 67, 1670–1677 (2008).
Alexanderson, H. Exercise effects in patients with adult idiopathic inflammatory myopathies. Curr. Opin. Rheumatol. 21, 158–163 (2009).
Alexanderson, H., Dastmalchi, M., Esbjornsson-Liljedahl, M., Opava, C. H. & Lundberg, I. E. Benefits of intensive resistance training in patients with chronic polymyositis or dermatomyositis. Arthritis Rheum. 57, 768–777 (2007).
de Salles Painelli, V. et al. The possible role of physical exercise on the treatment of idiopathic inflammatory myopathies. Autoimmun. Rev. 8, 355–359 (2009).
Author information
Authors and Affiliations
Contributions
M. Zong and I. E. Lundberg contributed equally to all aspects of the preparation of this manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Zong, M., Lundberg, I. Pathogenesis, classification and treatment of inflammatory myopathies. Nat Rev Rheumatol 7, 297–306 (2011). https://doi.org/10.1038/nrrheum.2011.39
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrrheum.2011.39
This article is cited by
-
Expansion of circulating peripheral TIGIT+CD226+ CD4 T cells with enhanced effector functions in dermatomyositis
Arthritis Research & Therapy (2021)
-
Inhibiting Interferon Pathways in Dermatomyositis: Rationale and Preliminary Evidence
Current Treatment Options in Rheumatology (2021)
-
The effect of a 24-week training focused on activities of daily living, muscle strengthening, and stability in idiopathic inflammatory myopathies: a monocentric controlled study with follow-up
Arthritis Research & Therapy (2021)
-
Biologics in refractory myositis: experience in juvenile vs. adult myositis; part II: emerging biologic and other therapies on the horizon
Pediatric Rheumatology (2019)
-
Physical therapy in adult inflammatory myopathy patients: a systematic review
Clinical Rheumatology (2019)