Abstract
B-cell depletion with unconjugated CD20 monoclonal antibody (mAb) is used to treat rheumatoid arthritis and other autoimmune diseases. CD20-targeted immunotherapy depletes mature B cells through monocyte-mediated antibody-dependent cellular cytotoxicity, but does not effectively deplete pre-B or immature B cells, certain peripheral B cell subpopulations, most antibody-producing cells, or their malignant counterparts. As immature B cells expressing autoreactive antigen receptors are not depleted by anti-CD20 mAb, a new strategy for eliminating autoantigen-selected B cells and for treating early lymphoblastic leukemias and/or lymphomas was developed using CD19-specific mAbs that induce Fcγ receptor-dependent and monocyte-dependent B-cell depletion. Preclinical studies using transgenic mice expressing human CD19 have shown that pre-B cells and their malignant counterparts, as well as pre-existing antibody-producing and autoantibody-producing cells, are depleted. Therefore, CD19-directed immunotherapy is expected to treat diverse pre-B-cell-related and plasmablast-related malignancies, and humoral transplant rejection. Moreover, in contrast to CD20-directed immunotherapies, CD19 mAbs could purge the B cell repertoire of autoreactive clones and reset the developmental clock to a point that curtails the extent of emerging self-reactivity, in addition to reducing autoreactive T-cell activation through the elimination of mature B cells. Humanized CD19 mAbs are expected to enter clinical trials in 2009, offering a new approach for the treatment of autoimmune disease that removes both immature B cells and antibodies with autoreactive specificities. CD19-directed immunotherapy could, therefore, offer a new horizon in B-cell depletion for the treatment of multiple autoimmune diseases.
Key Points
-
Autoreactive B cells have important pathogenic roles in autoimmune disorders beyond autoantibody production
-
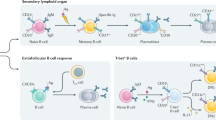
B cells exclusively express CD19, with continuous cell surface expression from the early pre-B cell stage of development through to the early stages of plasma cell differentiation
-
B-cell depletion with unconjugated CD19 monoclonal antibody (mAb) removes the majority of bone marrow, circulating and tissue B cells in human CD19 transgenic mice and primates, including pre-B cells and immature B cells
-
In human CD19 transgenic mice, CD19 mAb treatment substantially reduces serum autoantibody levels and autoantibody responses during pathogenic immune responses
-
Preclinical studies in mice and monkeys provide optimism for the future success of CD19 mAb therapy in patients with autoimmune diseases
-
Unconjugated CD19 mAbs will be entering phase I clinical trials for the treatment of autoimmune diseases in 2009
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
LeBien, T. W. & Tedder, T. F. B-lymphocytes: how they develop and function. Blood 112, 1570–1580 (2008).
Edwards, J. C. et al. Efficacy of B-cell-targeted therapy with rituximab in patients with rheumatoid arthritis. N. Engl. J. Med. 350, 2572–2581 (2004).
Yanaba, K. et al. B cell depletion delays collagen-induced arthritis in mice: arthritis induction requires synergy between humoral and cell-mediated immunity. J. Immunol. 179, 1369–1380 (2007).
Hamel, K. et al. Suppression of proteoglycan-induced arthritis by anti-CD20 B cell depletion therapy is mediated by reduction in autoantibodies and CD4+ T cell reactivity. J. Immunol. 180, 4994–5003 (2008).
Tedder, T. F. & Engel, P. CD20: a regulator of cell-cycle progression of B lymphocytes. Immunol. Today 15, 450–454 (1994).
Edwards, J. C. W. & Cambridge, G. Sustained improvement in rheumatoid arthritis following a protocol designed to deplete B lymphocytes. Rheumatology 40, 205–211 (2001).
Leandro, M. J., Edwards, J. C., Cambridge, G., Ehrenstein, M. R. & Isenberg, D. A. An open study of B lymphocyte depletion in systemic lupus erythematosis. Arthritis Rheum. 46, 2673–2677 (2002).
Silverman, G. J. & Weisman, S. Rituximab therapy and autoimmune disorders: prospects for anti-B cell therapy. Arthritis Rheum. 48, 1484–1492 (2002).
Hauser, S. L. et al. B-cell depletion with rituximab in relapsing-remitting multiple sclerosis. N. Engl. J. Med. 358, 676–688 (2008).
Bouaziz, J. D. et al. Therapeutic B cell depletion impairs adaptive and autoreactive CD4+ T cell activation in mice. Proc. Natl Acad. Sci. USA 104, 20882–20887 (2007).
Yanaba, K. et al. B-lymphocyte contributions to human autoimmune disease. Immunol. Rev. 223, 284–299 (2008).
Levesque, M. C. & St Clair, E. W. B cell-directed therapies for autoimmune disease and correlates of disease response and relapse. J. Allergy Clin. Immunol. 121, 13–21 (2008).
Taylor, R. P. & Lindorfer, M. A. Immunotherapeutic mechanisms of anti-CD20 monoclonal antibodies. Curr. Opin. Immunol. 20, 444–449 (2008).
DiLillo, D. J. et al. Maintenance of long-lived plasma cells and serological memory despite mature and memory B cell depletion during CD20 immunotherapy in mice. J. Immunol. 180, 361–371 (2008).
Anderson, K. C. et al. Expression of human B cell-associated antigens on leukemias and lymphomas: a model of human B cell differentiation. Blood 63, 1424–1433 (1984).
Loken, M. R., Shah, V. O., Dattilio, K. L. & Civin, C. I. Flow cytometric analysis of human bone marrow. II. Normal B lymphocyte development. Blood 70, 1316–1324 (1987).
Uckun, F. M. et al. Detailed studies on expression and function of CD19 surface determinant by using B43 monoclonal antibody and the clinical potential of anti-CD19 immunotoxins. Blood 71, 13–29 (1988).
Terstappen, L. W., Johnsen, S., Segers-Nolten, I. M. & Loken, M. R. Identification and characterization of plasma cells in normal human bone marrow by high-resolution flow cytometry. Blood 76, 1739–1747 (1990).
Nadler, L. M. et al. B4, a human B lymphocyte-associated antigen expressed on normal, mitogen activated, and malignant B lymphocytes. J. Immunol. 131, 244–250 (1983).
Scheuermann, R. H. CD19 antigen in leukemia and lymphoma diagnosis and immunotherapy. Leuk. Lymphoma 18, 385–397 (1995).
Tedder, T. F., Inaoki, M. & Sato, S. The CD19/21 complex regulates signal transduction thresholds governing humoral immunity and autoimmunity. Immunity 6, 107–118 (1997).
Fujimoto, M. et al. CD19 regulates Src-family protein tyrosine kinase activation in B lymphocytes through processive amplification. Immunity 13, 47–57 (2000).
Engel, P. et al. Abnormal B lymphocyte development, activation and differentiation in mice that lack or overexpress the CD19 signal transduction molecule. Immunity 3, 39–50 (1995).
Rickert, R. C., Rajewsky, K. & Roes, J. Impairment of T-cell-dependent B-cell responses and B-1 cell development in CD19-deficient mice. Nature 376, 352–355 (1995).
van Zelm, M. C. et al. An antibody-deficiency syndrome due to mutations in the CD19 gene. N. Engl. J. Med. 354, 1901–1912 (2006).
Inaoki, M., Sato, S., Weintraub, B. C., Goodnow, C. C. & Tedder, T. F. CD19-regulated signaling thresholds control peripheral tolerance and autoantibody production in B lymphocytes. J. Exp. Med. 186, 1923–1931 (1997).
Sato, S., Ono, N., Steeber, D. A., Pisetsky, D. S. & Tedder, T. F. CD19 regulates B lymphocyte signaling thresholds critical for the development of B-1 lineage cells and autoimmunity. J. Immunol. 157, 4371–4378 (1996).
Sato, S., Hasegawa, M., Fujimoto, M., Tedder, T. F. & Takehara, K. Quantitative genetic variation in CD19 expression correlates with autoimmunity. J. Immunol. 165, 6635–6643 (2000).
Tsuchiya, N. et al. Association of a functional CD19 polymorphism with susceptibility to systemic sclerosis (scleroderma). Arthritis Rheum. 50, 4002–4007 (2004).
Hasegawa, M. et al. A CD19-dependent signaling pathway regulates autoimmunity in Lyn-deficient mice. J. Immunol. 167, 2469–2478 (2001).
Westermann, J. & Pabst, R. Lymphocyte subsets in the blood: a diagnostic window on the lymphoid system? Immunol. Today 11, 406–410 (1991).
Uchida, J. et al. The innate mononuclear phagocyte network depletes B lymphocytes through Fc receptor-dependent mechanisms during anti-CD20 antibody immunotherapy. J. Exp. Med. 199, 1659–1669 (2004).
Hamaguchi, Y. et al. The peritoneal cavity provides a protective niche for B1 and conventional B lymphocytes during anti-CD20 immunotherapy in mice. J. Immunol. 174, 4389–4399 (2005).
Gong, Q. et al. Importance of cellular microenvironment and circulatory dynamics in B cell immunotherapy. J. Immunol. 174, 817–826 (2005).
Zhou, L.-J. et al. Tissue-specific expression of the human CD19 gene in transgenic mice inhibits antigen-independent B lymphocyte development. Mol. Cell. Biol. 14, 3884–3894 (1994).
Sato, S., Steeber, D. A., Jansen, P. J. & Tedder, T. F. CD19 expression levels regulate B lymphocyte development: human CD19 restores normal function in mice lacking endogenous CD19. J. Immunol. 158, 4662–4669 (1997).
Yazawa, N., Hamaguchi, Y., Poe, J. C. & Tedder, T. F. Immunotherapy using unconjugated CD19 monoclonal antibodies in animal models for B lymphocyte malignancies and autoimmune disease. Proc. Natl Acad. Sci. USA 102, 15178–15183 (2005).
Almasri, N. M., Duque, R. E., Iturraspe, J., Everett, E. & Braylan, R. C. Reduced expression of CD20 antigen as a characteristic marker for chronic lymphocytic leukemia. Am. J. Hematol. 40, 259–263 (1992).
Harada, H. et al. Phenotypic difference of normal plasma cells from mature myeloma cells. Blood 81, 2658–2663 (1993).
Hasegawa, M. et al. B-lymphocyte depletion reduces skin fibrosis and autoimmunity in the tight-skin mouse model for systemic sclerosis. Am. J. Pathol. 169, 954–966 (2006).
Horton, H. M. et al. Potent in vitro and in vivo activity of an Fc-engineered anti-CD19 monoclonal antibody against lymphoma and leukemia. Cancer Res. 68, 8049–8057 (2008).
Zalevsky, J. et al. The impact of Fc engineering on an anti-CD19 antibody: increased Fcγ receptor affinity enhances B-cell clearing in nonhuman primates. Blood 113, 3735–3743 (2009).
Tedder, T. F., Baras, A. & Xiu, Y. Fcγ receptor-dependent effector mechanisms regulate CD19 and CD20 antibody immunotherapies for B lymphocyte malignancies and autoimmunity. Sem. Pathol. 28, 351–364 (2006).
Hekman, A. et al. Initial experience with treatment of human B cell lymphoma with anti-CD19 monoclonal antibody. Cancer Immunol. Immunother. 32, 364–372 (1991).
Vlasveld, L. T. et al. Treatment of low-grade non-Hodgkin's lymphoma with continuous infusion of low-dose recombinant interleukin-2 in combination with the B-cell-specific monoclonal antibody CLB-CD19. Cancer Immunol. Immunother. 40, 37–47 (1995).
Grossbard, M. L. et al. A phase II study of adjuvant therapy with anti-B4-blocked ricin after autologous bone marrow transplantation for patients with relapsed B-cell non-Hodgkin's lymphoma. Clin. Cancer Res. 5, 2392–2398 (1999).
Kansas, G. S. & Tedder, T. F. Transmembrane signals generated through MHC class II, CD19, CD20, CD39, and CD40 antigens induce LFA-1-dependent and independent adhesion in human B cells through a tyrosine kinase-dependent pathway. J. Immunol. 147, 4094–4102 (1991).
Tedder, T. F., Wagner, N. & Engel, P. in Leukocyte Typing V: White Cell Differentiation Antigens Vol. 1. (eds Schlossman, S. F. et al.) 483–504 (Oxford University Press, Oxford, UK, 1995).
Gallagher, S. et al. Macrophages are required for anti-CD19 mAb mediated B cell depletion in mice. J. Immunol. 182, 50.16 (2009).
Carson, K. R. et al. Progressive multifocal leukoencephalopathy after rituximab therapy in HIV-negative patients: a report of 57 cases from the Research on Adverse Drug Events and Reports project. Blood 113, 4834–4840 (2009).
Calabrese, L. H., Molloy, E. S., Huang, D. & Ransohoff, R. M. Progressive multifocal leukoencephalopathy in rheumatic diseases: evolving clinical and pathologic patterns of disease. Arthritis Rheum. 56, 2116–2128 (2007).
Yanaba, K. et al. A regulatory B cell subset with a unique CD1dhiCD5+ phenotype controls T cell-dependent inflammatory responses. Immunity 28, 639–650 (2008).
Matsushita, T., Yanaba, K., Bouaziz, J.-D., Fujimoto, M. & Tedder, T. F. Regulatory B cells inhibit EAE initiation in mice while other B cells promote disease progression. J. Clin. Invest. 118, 3420–3430 (2008).
Goetz, M., Atreya, R., Ghalibafian, M., Galle, P. R. & Neurath, M. F. Exacerbation of ulcerative colitis after rituximab salvage therapy. Inflamm. Bowel Dis. 13, 1365–1368 (2007).
Dass, S., Vital, E. M. & Emery, P. Development of psoriasis after B cell depletion with rituximab. Arthritis Rheum. 56, 2715–2718 (2007).
Benedetti, L. et al. Relapses after treatment with rituximab in a patient with multiple sclerosis and anti myelin-associated glycoprotein polyneuropathy. Arch. Neurol. 64, 1531–1533 (2007).
Press, O. W., Farr, A. G., Borroz, K. I., Anderson, S. K. & Martin, P. J. Endocytosis and degradation of monoclonal antibodies targeting human B-cell malignancies. Cancer Res. 49, 4906–4912 (1989).
Schriever, F., Freeman, G. & Nadler, L. M. Follicular dendritic cells contain a unique gene repertoire demonstrated by single-cell polymerase chain reaction. Blood 77, 787–791 (1991).
Ghetie, M.-A. et al. Anti-CD19 inhibits the growth of human B-cell tumor lines in vitro and of Daudi cells in SCID mice by inducing cell cycle arrest. Blood 83, 1329–1336 (1994).
Acknowledgements
The author thanks Cynthia Magro, William St. Clair, Jonathan Poe, David Pisetsky, Karen Haas, Damian Maseda, and Takashi Matsushita for their assistance and suggestions. This work was supported by grants from the National Institutes of Health (AI56363, CA105001, CA96547, and AI057157).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
T. F. Tedder's research has centered on the development, activation, and functions of B cells with a specific focus on the identification of B cell-restricted cell surface molecules, their structural and biochemical features, and how these molecules regulate function in vivo. He obtained his PhD at the University of Alabama, Birmingham with Dr. Max Cooper, and was a postdoctoral fellow with Dr. Stuart Schlossman at Dana-Farber Cancer Institute/Harvard, before joining the faculty. He joined Duke University Medical Center as their first Chairman of a new Department of Immunology, where he remains as a Professor in the Department of Immunology.
Rights and permissions
About this article
Cite this article
Tedder, T. CD19: a promising B cell target for rheumatoid arthritis. Nat Rev Rheumatol 5, 572–577 (2009). https://doi.org/10.1038/nrrheum.2009.184
Issue Date:
DOI: https://doi.org/10.1038/nrrheum.2009.184
This article is cited by
-
Immune evasion in cell-based immunotherapy: unraveling challenges and novel strategies
Journal of Biomedical Science (2024)
-
Myasthenia gravis: the changing treatment landscape in the era of molecular therapies
Nature Reviews Neurology (2024)
-
Safety of AFM11 in the treatment of patients with B-cell malignancies: findings from two phase 1 studies
Trials (2023)
-
Enhanced CD19 activity in B cells contributes to immunodeficiency in mice deficient in the ICF syndrome gene Zbtb24
Cellular & Molecular Immunology (2023)
-
Antibody Therapies for Progressive Multiple Sclerosis and for Promoting Repair
Neurotherapeutics (2022)