Key Points
-
Depression is more common in patients with multiple sclerosis (MS) than in the general population, and substantially impairs quality of life; suicide rates are also elevated in patients with MS
-
To advance research and clinical practice, depression in patients with MS will require a rigorous definition based on quantitative assessment
-
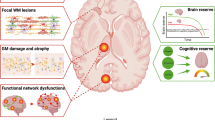
Structural brain changes on MRI account for almost 50% of the variance in the presence of MS-related depression; genetic, biochemical, immunological and psychosocial factors have also been implicated
-
Current disease-modifying therapies for MS do not seem to cause mood disorders
-
Treatment of MS-related depression requires further investigation: antidepressants are modestly effective, but adverse effects can preclude adequate dosing; cognitive–behavioural therapy is also effective
-
Randomized trials must address whether combining treatments improves outcomes
Abstract
Depression—be it a formal diagnosis based on consensus clinical criteria, or a collection of symptoms revealed by a self-report rating scale—is common in patients with multiple sclerosis (MS) and adds substantially to the morbidity and mortality associated with this disease. This Review discusses the prevalence and epidemiology of depression in patients with MS, before covering aetiological factors, including genetics, brain pathology, immunological changes, dysregulation of the hypothalamic–pituitary–adrenal axis, and psychosocial influences. Treatment options such as antidepressant drugs, cognitive–behavioural therapy, mindfulness-based therapy, exercise and electroconvulsive therapy are also reviewed in the context of MS-related depression. Frequent comorbid conditions, namely pain, fatigue, anxiety, cognitive dysfunction and alcohol use, are also summarized. The article then explores three key challenges facing researchers and clinicians: what is the optimal way to define depression in the context of diseases such as MS, in which the psychiatric and neurological symptoms overlap; how can current knowledge about the biological and psychological underpinnings of MS-related depression be used to boost the validity of this construct; and can intervention be made more effective through use of combination therapies with additive or synergistic effects, which might exceed the modest benefits derived from their individual components?
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Charcot, J. M. Lectures on the Diseases of the Nervous System. Delivered at the Infirmary of La Salpêtrière [English translation by Thomas Savill] 194–195 (New Sydenham Society, 1877).
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders 5th edn (American Psychiatric Publishing, 2013).
Beck, A. T., Steer, R. A. & Brown, G. K. Beck Depression Inventory (BDI)-II Manual (The Psychological Corporation, 1996).
Minden, S. L. et al. Evidence based guideline: assessment and management of psychiatric disorders in individuals with MS: report of the Guideline Development Subcommittee of the American Academy of Neurology. Neurology 82, 174–181 (2014).
Zigmond, A. S. & Snaith, R. P. The hospital anxiety and depression scale. Acta Psychiatr. Scand. 67, 361–370 (1983).
Beck, A. T., Steer, R. A. & Brown, G. K. BDI—Fast Screen for Medical Patients Manual (The Psychological Corporation, 2000).
Benedict, R. H., Fishman, I., McClellan, M. M., Bakshi, R. & Weinstock-Guttman, B. Validity of the Beck Depression Inventory—Fast Screen in multiple sclerosis. Mult. Scler. 9, 393–396 (2003).
Hornarmand, K. & Feinstein, A. Validation of the Hospital Anxiety and Depression Scale for use with multiple sclerosis patients. Mult. Scler. 15, 1518–1524 (2009).
Avarasala, J. R., Cross, A. H. & Trinkaus, K. Comparative assessment of Yale Single Question and Beck Depression Inventory Scale in screening for depression in multiple sclerosis. Mult. Scler. 9, 307–310 (2003).
Mohr, D. C., Hart, S. L., Julian, L. & Tasch, E. S. Screening for depression among patients with multiple sclerosis: two questions may be enough. Mult. Scler. 13, 215–219 (2007).
Kroenke, K., Spitzer, R. L., Williams, J. B. The PHQ-9: validity of a brief depression severity measure. J. Gen. Intern. Med. 16, 606–613 (2001).
Amtmann, D. et al. Comparing CESD-10, PHQ-9, and PROMIS depression instruments in individuals with multiple sclerosis. Rehabil. Psychol. 59, 220–229 (2014).
Sadnovik, A. D. et al. Depression and multiple sclerosis. Neurology 46, 628–632 (1996).
Kessler, R. C., Petukhova, M., Sampson, N. A., Zaslavsky, A. M. & Wittchen, H. U. Twelve-month and lifetime prevalence and lifetime morbid risk of anxiety and mood disorders in the United States. Int. J. Methods Psychiatr. Res. 21, 169–184 (2012).
Narrow, W. E., Rae, D. S., Robins, L. N. & Regier, D. A. Revised prevalence estimates of mental disorders in the United States: using a clinical significance criterion to reconcile 2 surveys' estimates. Arch. Gen. Psychiatry 59, 115–123 (2002).
Patten, S. B., Beck, C. A., Williams, J. V. A., Barbui, C. & Metz, L. M. Major depression in multiple sclerosis: a population-based perspective. Neurology 61, 1524–1527 (2003).
Chwastiak, L. et al. Depressive symptoms and severity of illness in multiple sclerosis: epidemiologic study of a large community sample. Am. J. Psychiatry 159, 1862–1868 (2002).
Marrie, R. A. et al. Mental comorbidity and multiple sclerosis: validating administrative data to support population-based surveillance. BMC Neurol. 13, 16 (2013).
Jones, K. H. et al. A large-scale study of anxiety and depression in people with multiple sclerosis: a survey via the web portal of the UK MS Register. PLoS ONE 7, e41910. (2012).
Marrie, R. A. et al. The burden of mental comorbidity in multiple sclerosis: frequent, underdiagnosed, and undertreated. Mult. Scler. 15, 385–392 (2009).
Schubert, D. S. & Foliart, R. H. Increased depression in multiple sclerosis: a meta-analysis. Psychosomatics 34, 124–130 (1993).
Thielscher, C., Thielscher, S. & Kostev, K. The risk of developing depression when suffering from neurological diseases. Ger. Med. Sci. 11, Doc02 (2013).
Ron, M. A. & Logsdail, S. J. Psychiatric morbidity in multiple sclerosis: a clinical and MRI study. Psychol. Med. 19, 887–895 (1987).
Leach, L. S., Christensen, H., Mackinnon, A. J., Windsor, T. D. & Butterworth, P. Gender differences in depression and anxiety across the adult lifespan: the role of psychosocial mediators. Soc. Psychiatry Psychiatr. Epidemiol. 43, 983–998 (2008).
Wood, B. et al. Prevalence and concurrence of anxiety, depression and fatigue over time in multiple sclerosis. Mult. Scler. 19, 217–224 (2013).
Dahl, O. P., Stordal, E., Lydersen, S. & Midgard, R. Anxiety and depression in multiple sclerosis. A comparative population-based study in Nord-Trøndelag County, Norway. Mult. Scler. 15, 1495–1501 (2009).
Blaschek, A. et al. Neuropsychological aspects of childhood multiple sclerosis: an overview. Neuropediatrics 43, 176–183 (2012).
Feinstein, A., Youl, B. & Ron, M. A. Acute optic neuritis: A cognitive and magnetic resonance imaging study. Brain 115, 1403–1415 (1992).
Feinstein, A., Kartsounis, L. D., Miller, D. H., Youl, B. D. & Ron, M. A. Clinically isolated lesions of the type seen in multiple sclerosis: a cognitive psychiatric and MRI follow up study. J. Neurol. Neurosurg. Psychiatry 55, 869–876 (1992).
Zabad, R. K., Patten, S. B. & Metz, L. M. The association of depression with disease course in multiple sclerosis. Neurology 64, 359–360 (2005).
Patten, S. B. & Metz, L. M. Hopelessness ratings in relapsing–remitting and secondary progressive multiple sclerosis. Int. J. Psychiatry Med. 32, 155–165 (2002).
Arnett, P. A. & Randolph, J. J. Longitudinal course of depression symptoms in multiple sclerosis. J. Neurol. Neurosurg. Psychiatry 77, 606–610 (2006).
Rabinowitz, A. R. & Arnett, P. A. A longitudinal analysis of cognitive dysfunction, coping, and depression in multiple sclerosis. Neuropsychology 23, 581–591 (2009).
Bianchi, V. et al. Mood and coping in clinically isolated syndrome and multiple sclerosis. Acta Neurol. Scand. 129, 374–381 (2014).
Moore, P. et al. Multiple sclerosis relapses and depression. J. Psychosom. Res. 73, 272–276 (2012).
O'Connor, A. B., Schwid, S. R., Herrmann, D. N., Markman, J. D. & Dwoekin, R. H. Pain associated with multiple sclerosis: systematic review and proposed classification. Pain 137, 96–111 (2008).
Edhe, D. M. et al. Chronic pain in a large community sample of persons with multiple sclerosis. Mult. Scler. 9, 605–611 (2003).
Alschuler, K. N., Ehde, D. M. & Jensen, M. P. The co-occurence of pain and depression in adults with multiple sclerosis. Rehabil. Psychol. 48, 217–221 (2013).
Kroenke, K. et al. Reciprocal relationship between pain and depression: a 12 month longitudinal analysis in primary care. J. Pain 12, 964–973 (2011).
Kroencke, D. C., Lynch, S. G. & Denney, D. R. Fatigue in multiple sclerosis: relationship to depression, disability and disease pattern. Mult. Scler. 6, 131–136 (2000).
Heesen, C. et al. Behavioral interventions in multiple sclerosis: a biopsychosocial perspective. Expert Rev. Neurother. 12, 1089–1100 (2012).
Korostil, M. & Feinstein, A. Anxiety disorders and their clinical correlates in multiple sclerosis patients. Mult. Scler. 13, 67–72 (2007).
Poder, K. et al. Social anxiety in a multiple sclerosis clinical population. Mult. Scler. 15, 393–398 (2009).
Giordano, A. et al. Anxiety and depression in multiple sclerosis patients around diagnosis. J. Neurol. Sci. 307, 86–91 (2011).
Burns, M. N., Nawacki, E., Siddique, J., Pelletier, D. & Mohr, D. C. Prospective examination of anxiety and depression before and during confirmed and pseudoexacerbations in patients with multiple sclerosis. Psychosom. Med. 75, 76–82 (2013).
Ó Donnchadha, S. et al. Symptom overlap in anxiety and multiple sclerosis. Mult. Scler. 19, 1349–1354 (2013).
Garfield, A. C. & Lincoln, N. B. Factors affecting anxiety in multiple sclerosis. Disabil. Rehabil. 34, 2047–2052 (2012).
Feinstein, A., O'Connor, P., Gray, T. & Feinstein, K. The effects of anxiety on psychiatric morbidity in patients with multiple sclerosis. Mult. Scler. 5, 323–326 (1999).
Quesnel, S. & Feinstein, A. Multiple sclerosis and alcohol: a study of problem drinking. Mult. Scler. 10, 197–201 (2004).
Goretti, B. et al. Anxiety state affects information processing speed in patients with multiple sclerosis. Neurol. Sci. 35, 559–563 (2014).
Rubio, J. M. et al. Epidemiology of chronic and nonchronic major depressive disorder: results from the national epidemiologic survey on alcohol and related conditions. Depress. Anxiety 28, 622–631 (2011).
Bombardier, C. H. et al. Alcohol and drug abuse among persons with multiple sclerosis. Mult. Scler. 10, 35–40 (2004).
Weiland, T. J. et al. The association of alcohol consumption and smoking with quality of life, disability and disease activity in an international sample of people with multiple sclerosis. J. Neurol. Sci. 336, 211–219, 2014.
Rao, S. M., Leo, G. J., Bernardin, L. & Unverzagt, F. Cognitive dysfunction in multiple sclerosis. I. Frequency, patterns and prediction. Neurology 41, 685–285 (1991).
Benedict, R. H. et al. Validity of the minimal assessment of cognitive function in multiple sclerosis (MACFIMS). J. Int. Neuropsychol. Soc. 12, 549–558 (2006).
Arnett, P. A. et al. Depression in multiple sclerosis: relationship to working memory capacity. Neuropsychology 13, 546–556 (1999).
Arnett, P. A. et al. Depressed mood in multiple sclerosis: relationship to capacity-demanding memory and attentional functioning. Neuropsychology 13, 434–446 (1999).
Arnett, P. A., Higginson, C. I. & Randolph, J. J. Depression in multiple sclerosis: relationship to planning ability. J. Int. Neuropsychol. Soc. 7, 665–674 (2001).
Lubrini, G., Perianez, J. A., Rios-Lago, M. & Frank, A. Velocidad de procesamiento en la esclerosis múltiple remitente recurrente: el papel de los síntomas depresivos [Spanish]. Rev. Neurol. 55, 585–592 (2012).
Fann, J. R., Uomoto, J. M. & Katon, W. J. Cognitive improvement with treatment of depression following mild traumatic brain injury. Psychosomatics 42, 48–54 (2001).
Kiy, G. et al. Decreased hippocampal volume, indirectly measured, is associated with depressive symptoms and consolidation deficits in multiple sclerosis. Mult. Scler. 17, 1088–1097 (2011).
Joffe, R. T., Lippert, G. P., Gray, T. A., Sawa, G. & Horvath, Z. Personal and family history of affective illness in patients with multiple sclerosis. J. Affect. Disord. 12, 63–65 (1987).
Minden, S. L., Orav, J. & Reich, P. Depression in multiple sclerosis. Gen. Hosp. Psychiatry 9, 426–434 (1987).
Schiffer, R. B., Weitkamp, L. R., Wineman, N. M. & Guttormsen, S. Multiple sclerosis and affective disorder. Family history, sex and HLA-DR antigens. Arch. Neurol. 45, 1345–1348 (1988).
Patten, S. B., Metz, L. M. & Reimer, M. A. Biopsychosocial correlates of lifetime major depression in a multiple sclerosis population. Mult. Scler. 6, 115–120 (2000).
Julian, L. J. et al. ApoE alleles, depression and positive affect in multiple sclerosis. Mult. Scler. 15, 311–315 (2009).
Pujol, J., Bello, J., Deus, J., Martí-Vilalta, J. L. & Capdevila, A. Lesions in the left arcuate fasciculus region and depressive symptoms in multiple sclerosis. Neurology 49, 1105–1110 (1997).
Pujol, J. et al Beck Depression Inventory factors related to demyelinating lesions of the left arcuate fasciculus region. Psychiatry Res. 99, 151–159 (2000).
Bakshi, R. et al. Brain MRI lesions and atrophy are related to depression in multiple sclerosis. Neuroreport 11, 1153–1158 (2000).
Feinstein, A. et al. Structural brain abnormalities in multiple sclerosis patients with major depression. Neurology 62, 586–590 (2004).
Zorzon, M. et al. Depressive symptoms and MRI changes in multiple sclerosis. Eur. J. Neurol. 9, 491–496 (2002).
Berg, D. et al. Lesion pattern in patients with multiple sclerosis and depression. Mult. Scler. 6, 156–162 (2000).
Feinstein, A. et al. Diffusion tensor imaging abnormalities in depressed multiple sclerosis patients. Mult. Scler. 16, 189–196 (2010).
Kern, S. et al. Circadian cortisol, depressive symptoms and neurological impairment in early multiple sclerosis. Psychoneuroendocrinology 36, 1505–1512 (2011).
Gold, S. M. et al. Smaller cornu ammonis 2–3/dentate gyrus volumes and elevated cortisol in multiple sclerosis patients with depressive symptoms. Biol. Psychiatry 68, 553–559 (2010).
Ysrraelit, M. C., Gaitán, M. I., Lopez, A. S. & Correale, J. Impaired hypothalamic-pituitary-adrenal axis activity in patients with multiple sclerosis. Neurology 71, 1948–1954 (2008).
Melief, J. et al. HPA axis activity in multiple sclerosis correlates with disease severity, lesion type and gene expression in normal appearing white matter. Acta Neuropathol. 126, 237–249 (2013).
Fassbender, K. et al. Mood disorders and dysfunction of the hypothalamic-pituitary-adrenal axis in multiple sclerosis: association with cerebral inflammation. Arch. Neurol. 55, 66–72 (1998).
Gold, S. M. et al. Detection of altered hippocampal morphology in multiple sclerosis-associated depression using automated surface mesh modeling. Hum. Brain Mapp. 35, 30–37 (2014).
Sabatini, U. et al. Involvement of the limbic system in multiple sclerosis patients with depressive disorders. Biol. Psychiatry 39, 970–975 (1996).
Passamonti, L. et al. Neurobiological mechanisms underlying emotional processing in relapsing–remitting multiple sclerosis. Brain 132, 3380–3391 (2009).
Altamura, A. C., Buoli, M. & Pozzoli, S. Role of immunological factors in the pathophysiology and diagnosis of bipolar disorder: comparison with schizophrenia. Psychiatry Clin. Neurosci. 68, 21–36 (2014).
Zunszain, P. A., Hepgul, N. & Pariante, C. M. Inflammation and depression. Curr. Top. Behav. Neurosci. 14, 135–151 (2013).
Lu, S. et al. Elevated specific peripheral cytokines found in major depressive disorder patients with childhood trauma exposure: a cytokine antibody array analysis. Compr. Psychiatry 54, 953–961 (2013).
Sukoff Rizzo, S. J. et al. Evidence for sustained elevation of IL-6 in the CNS as a key contributor of depressive-like phenotypes. Transl. Psychiatry 2, e199 (2012).
Gold, S. M. & Irwin, M. R. Depression and immunity: inflammation and depressive symptoms in multiple sclerosis. Neurol. Clin. 24, 507–519 (2006).
Kim, Y. K. et al. Cytokine imbalance in the pathophysiology of major depressive disorder. Prog. Neuropsychopharmacol. Biol. Psychiatry 31, 1044–1053 (2007).
Vaccarino, V. et al. Association of major depressive disorder with serum myeloperoxidase and other markers of inflammation: a twin study. Biol. Psychiatry 64, 476–483 (2008).
Serafini, G. et al. The role of inflammatory cytokines in suicidal behavior: a systematic review. Eur. Neuropsychopharmacol. 23, 1672–1686 (2013).
Karlović, D., Serreti, A., Vrkić, N., Martinac, M. & Marccˇinko, D. Serum concentrations of CRP, IL-6, TNF-α and cortisol in major depressive disorder with melancholic or atypical features. Psychiatry Res. 198, 74–80 (2012).
Hughes, M. M. et al. Tryptophan depletion in depressed patients occurs independent of kynurenine pathway activation. Brain Behav. Immun. 26, 979–987 (2012).
van Heesch, F. et al. Systemic tumor necrosis factor-α decreases brain stimulation reward and increases metabolites of serotonin and dopamine in the nucleus accumbens of mice. Behav. Brain Res. 253, 191–195 (2013).
Craddock, D. & Thomas, A. Cytokines and late-life depression. Essent. Psychopharmacol. 7, 42–52 (2006).
Gold, S. M. et al. Endocrine and immune substrates of depressive symptoms and fatigue in multiple sclerosis patients with comorbid major depression. J. Neurol. Neurosurg. Psychiatry 82, 814–818 (2011).
Pokryszko-Dragan, A. et al. Stimulated peripheral production of interferon-γ is related to fatigue and depression in multiple sclerosis. Clin. Neurol. Neurosurg. 114, 1153–1158 (2012).
Acharjee, S. et al. Altered cognitive–emotional behaviour in early experimental autoimmune encephalitis—cytokine and hormonal correlates. Brain Behav. Immun. 33, 164–172 (2013).
Peruja, I. et al. Inflammation modulates anxiety in an animal model of multiple sclerosis. Behav. Brain Res. 220, 20–29 (2011).
Haji, N. et al. TNF-α-mediated anxiety in a mouse model of multiple sclerosis. Exp. Neurol. 237, 296–303 (2012).
Pollak, Y., Ovadia, H., Orion, E. & Yirmiya, R. The EAE-associated behavioral syndrome: II. Modulation by anti-inflammatory treatments. J. Neuroimmunol. 137, 100–108 (2003).
Foley, F. W. et al. A prospective study of depression and immune dysregulation in multiple sclerosis. Arch. Neurol. 49, 238–244 (1992).
Feinstein, A., O'Connor, P. & Feinstein, K. J. Multiple sclerosis, inteferon β-1b and depression: a prospective investigation. J. Neurol. 249, 815–820 (2002).
Patten, S. B. et al. The relationship between depression and inteferon β-1a therapy in patients with multiple sclerosis. Mult. Scler. 11, 175–181 (2005).
Jongen, P. J. et al. Health-related quality of life in relapsing remitting multiple sclerosis: patients during treatment with glatiramer acetate: a prospective, observational, international, multi-centre study. Health Qual. Life Outcomes 8, 133 (2010).
Montalban, X. et al. Oral fingolimod (FTY720) in relapsing multiple sclerosis: impact on health-related quality of life in a phase II study. Mult. Scler. 17, 1341–1350 (2011).
Mendlewicz, J. et al. Shortened onset of action of antidepressants in major depression using acetylsalicylic acid augmentation: a pilot open-label study. Int. Clin. Psychopharmacol. 21, 227–231 (2006).
Müller, N. et al. The cyclooxygenase-2 inhibitor celecoxib has therapeutic effects in major depression: results of a double-blind, randomized, placebo controlled, add-on pilot study to reboxetine. Mol. Psychiatry 11, 680–684 (2006).
Tyring, A. et al. Etanercept and clinical outcomes, fatigue, and depression in psoriasis: double-blind placebo-controlled randomized phase III trial. Lancet 367, 29–35 (2006).
Lynch, S. G., Kroencke, D. C. & Denney, S. R. The relationship between disability and depression in multiple sclerosis: the role of uncertainty, coping and hope. Mult. Scler. 7, 411–416 (2001).
van der Werf, S. P., Evers, A., Jongen, P. J. & Bleijenberg, G. The role of helplessness as mediator between neurological disability, emotional instability, experienced fatigue and depression in patients with multiple sclerosis. Mult. Scler. 3, 89–94 (2003).
Voss, W. D. et al. Contributing factors to depressed mood in multiple sclerosis. Arch. Clin. Neuropsychol. 17, 103–115 (2002).
King, K. E. & Arnett, P. A. Predictors of dyadic adjustment in multiple sclerosis. Mult. Scler. 11, 700–707 (2005).
McCabew, M. P. & De Judicibus, M. The effects of economic disadvantage on psychological well-being and quality of life among people with multiple sclerosis. J. Health Psychol. 10, 163–173 (2005).
Goretti, B., Portaccio, E., Zipoli, V., Razzolini, L. & Amato, M. P. Coping strategies, cognitive impairment, psychological variables and their relationship with quality of life in multiple sclerosis. Neurol. Sci. 31 (Suppl. 2), S227–S230 (2010).
Mohr, D. C., Goodkin, D. E., Nelson, S., Cox, D. & Weiner, M. Moderating effects of coping on the relationship between stress and the development of new brain lesions in multiple sclerosis. Psychosom. Med. 64, 803–809 (2002).
Arnett, P., Barwick, F. H. & Beeney, J. E. Depression in multiple sclerosis: review and theoretical proposal. J. Int. Neuropsychol. Soc. 14, 691–724 (2008).
Hopman, W. M. et al. Factors associated with health-related quality of life in multiple sclerosis. Can. J. Neurol. Sci. 34, 160–166 (2007).
Marrie, R. A., Horwitz, R., Cutter, G. & Tyry, T. Cumulative impact of comorbidity on quality of life in MS. Acta Neurol. Scand. 125, 180–186 (2012).
Feinstein, A. An examination of suicidal intent in patients with multiple sclerosis. Neurology 59, 674–678 (2002).
Sadovnick, A. D., Eisen, K., Ebers, G. C. & Paty, D. W. Cause of death in patients attending multiple sclerosis clinics. Neurology 41, 1193–1196 (1991).
Stenager, E. N. & Stenager, E. Suicide and patients with neurologic diseases. Methodologic problems. Arch. Neurol. 49, 1296–1303 (1992).
Mohr, D. C., Hart, S. L., Fonareva, I. & Tasch, E. S. Treatment of depression for patients with multiple sclerosis in neurology clinics. Mult. Scler. 12, 204–208 (2006).
Kessing, L. V., Harhoff, M. & Andersen, P. K. Increased rate of treatment with antidepressants in patients with multiple sclerosis. Int. Clin. Psychopharmacol. 23, 54–59 (2008).
Cetin, K. et al. Antidepressant use in multiple sclerosis: epidemiologic study of a large community sample. Mult. Scler. 13, 1046–1053 (2007).
Koch, M. W., Glazenborg, A., Uyttenboogaart, M., Mostert, J. & De Keyser, J. Pharmacologic treatment of depression in multiple sclerosis. Cochrane Database of Systematic Reviews, Issue 2. Art. No.: CD007295. http://dx.doi.org/10.1002/14651858.CD007295.pub2.
Schiffer, R. B. & Wineman, N. M. Antidepressant pharmacotherapy of depression associated with multiple sclerosis. Am. J. Psychiatry 147, 1493–1497 (1990).
Ehde, D. M. et al. Efficacy of paroxetine in treating major depressive disorder in persons with multiple sclerosis. Gen. Hosp. Psychiatry 30, 40–48 (2008).
Solaro, C. et al. Duloxetine is effective in treating depression in multiple sclerosis patients: an open-label multicenter study. Clin. Neuropharmacol. 36, 114–116 (2013).
Shafey, H. The effect of fluoxetine in depression associated with multiple sclerosis. Can. J. Psychiatry 37, 147–148 (1992).
Scott, T. F., Nussbaum, P., McConnell, H. & Brill, P. Measurement of treatment response to sertraline in depressed multiple sclerosis patients using the Carroll scale. Neurol. Res. 17, 421–422 (1995).
Barak, Y., Ur, E. & Achiron, A. Moclobemide treatment in multiple sclerosis patients with comorbid depression: an open-label safety trial. J. Neuropsychiatry Clin. Neurosci. 11, 271–273 (1999).
Dean, G. A double-blind trial with an antidepressant drug, imipramine, in multiple sclerosis. S. Afr. Med. J. 43, 86–87 (1969).
Silberberg, D. & Armstrong, R. Tranylcypromine in multiple sclerosis. Lancet 2, 852–853 (1965).
Mohr, D. C. et al. Brain lesion volume and neuropsychological function predict efficacy of treatment for depression in multiple sclerosis. J. Consult. Clin. Psychol. 71, 1017–1024 (2003).
Julian, L. J. & Mohr, D. C. Cognitive predictors of response to treatment for depression in multiple sclerosis. J. Neuropsychiatry Clin. Neurosci. 18, 356–363 (2006).
Thomas, P. W., Thomas, S., Hillier, C., Galvin, K. & Baker, R. Psychological interventions for multiple sclerosis. Cochrane Database of Systematic Reviews, Issue 1, Art. No.: CD004431. http://dx.doi.org/10.1002/14651858.CD004431.pub2.
Mohr, D. C., Boudewyn, A. C., Goodkin, D. E., Bostrom, A. & Epstein, L. Comparative outcomes for individual cognitive–behavior therapy, supportive–expressive group psychotherapy, and sertraline for the treatment of depression in multiple sclerosis. J. Consult. Clin. Psychol. 69, 942–949 (2001).
Askey-Jones, S., David, A. S., Silber, E., Shaw, P. & Chalder, T. Cognitive behaviour therapy for common mental disorders in people with multiple sclerosis: a bench marking study. Behav. Res. Ther. 51, 648–655 (2013).
Hind, D. et al. Cognitive behavioural therapy for the treatment of depression in people with multiple sclerosis: a systematic review and meta-analysis. BMC Psychiatry 14, 5 (2014).
Mohr, D. C. et al. Telephone-administered cognitive–behavioural therapy for the treatment of depressive symptoms in multiple sclerosis. J. Consult. Clin. Psychol. 68, 356–361 (2000).
Hind, D. et al. The acceptability of computerised cognitive behavioural therapy for the treatment of depression in people with chronic physical disease: a qualitative study of people with multiple sclerosis. Psychol. Health 25, 699–712 (2010).
Grossman, P. et al. MS quality of life, depression, and fatigue improve after mindfulness training: a randomized trial. Neurology 75, 1141–1149 (2010).
Mohr, D. C. et al. A randomized trial of stress management for the prevention of new brain lesions in MS. Neurology 79, 412–419 (2012).
Feinstein, A., Rector, N. & Motl, R. Exercising away the blues: can it help multiple sclerosis-related depression? Mult. Scler. 19, 1815–1819 (2013).
Fregni, F. & Pascual-Leone, A. Transcranial magnetic stimulation for the treatment of depression in neurologic disorders. Curr. Psychiatry Rep. 7, 381–390 (2005).
Urban-Kowalczyk, M. et al. Electroconvulsive therapy in patient with psychotic depression and multiple sclerosis. Neurocase 14, 452–455 (2014).
Rasmussen, K. G. & Keegan, B. M. Electroconvulsive therapy in patients with multiple sclerosis. J. ECT 23, 179–180 (2007).
Mattingley, G., Baker, K., Zorumski, C. F. & Fiegiel, G. S. Multiple sclerosis and ECT: possible value of gadolinium-enhanced magnetic resonance scans for identifying high-risk patients. J. Neuropsychiatry Clin. Neurosci. 4, 145–151 (1992).
Acknowledgements
The authors wish to acknowledge the support of the endMS Network and the Multiple Sclerosis Society of Canada.
Author information
Authors and Affiliations
Contributions
All authors contributed equally to researching data for the article, developing the discussions of its content, writing the article, and reviewing and editing the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
A.F. has received honoraria from Biogen, Merck Serono, Novartis and Teva. The other authors declare no competing interests.
PowerPoint slides
Rights and permissions
About this article
Cite this article
Feinstein, A., Magalhaes, S., Richard, JF. et al. The link between multiple sclerosis and depression. Nat Rev Neurol 10, 507–517 (2014). https://doi.org/10.1038/nrneurol.2014.139
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneurol.2014.139
This article is cited by
-
Study protocol: exercise training for treating major depressive disorder in multiple sclerosis
BMC Neurology (2024)
-
Frontal-striatal tract integrity and depression in older adults with and without multiple sclerosis
Neurological Sciences (2024)
-
Monoaminergic network dysfunction and development of depression in multiple sclerosis: a longitudinal investigation
Journal of Neurology (2024)
-
Routine outcomes and evaluation of an 8-week outpatient multidisciplinary rehabilitative therapy program for functional neurological disorder
Journal of Neurology (2024)
-
Nanoparticulate MgH2 ameliorates anxiety/depression-like behaviors in a mouse model of multiple sclerosis by regulating microglial polarization and oxidative stress
Journal of Neuroinflammation (2023)