Key Points
-
Guillain–Barré syndrome (GBS) is a heterogeneous disease characterized by rapidly progressive, symmetrical limb weakness with hyporeflexia or areflexia; sensory disturbances and cranial nerve deficits occur in some patients
-
The clinical diagnosis of GBS can be supported by additional investigations (such as cerebrospinal fluid examination and nerve conduction studies), which are especially useful in patients with atypical features or diagnostic doubt
-
Molecular mimicry, antiganglioside antibodies and, likely, complement activation are involved in the pathogenesis of GBS; a potential role for genetic susceptibility requires further investigation
-
Intravenous immunoglobulin and plasma exchange are proven effective treatments, but improved therapies are needed as ∼25% of patients require artificial ventilation and 20% are unable to walk after 6 months
-
Pain is an important symptom that may be present before onset of weakness, and can impede correct diagnosis, especially in children; other residual features (sensory disturbances and fatigue) may persist for years
-
Prognostic models can predict patient outcomes at 4 weeks, 3 months and 6 months, as well as the probability of respiratory insufficiency, even early in the course of the disease
Abstract
Guillain–Barré syndrome (GBS) is a potentially life-threatening postinfectious disease characterized by rapidly progressive, symmetrical weakness of the extremities. About 25% of patients develop respiratory insufficiency and many show signs of autonomic dysfunction. Diagnosis can usually be made on clinical grounds, but lumbar puncture and electrophysiological studies can help to substantiate the diagnosis and to differentiate demyelinating from axonal subtypes of GBS. Molecular mimicry of pathogen-borne antigens, leading to generation of crossreactive antibodies that also target gangliosides, is part of the pathogenesis of GBS; the subtype and severity of the syndrome are partly determined by the nature of the antecedent infection and specificity of such antibodies. Intravenous immunoglobulin and plasma exchange are proven effective treatments but many patients have considerable residual deficits. Discrimination of patients with treatment-related fluctuations from those with acute-onset chronic inflammatory demyelinating polyneuropathy is important, as these conditions may require different treatments. Novel prognostic models can accurately predict outcome and the need for artificial ventilation, which could aid the selection of patients with a poor prognosis for more-individualized care. This Review summarizes the clinical features of and diagnostic criteria for GBS, and discusses its pathogenesis, treatment and prognosis.
Similar content being viewed by others
Introduction
Guillain–Barré syndrome (GBS) is a common cause of acute flaccid paralysis, characterized by symmetrical weakness of the limbs, and hyporeflexia or areflexia, which reaches a maximum severity within 4 weeks (Figure 1).1,2,3,4 Sensory symptoms, such as paraesthesia or numbness, usually start distally and have a symmetrical pattern. The most common subtypes of GBS are acute inflammatory demyelinating polyneuropathy (AIDP) and acute motor axonal neuropathy (AMAN).1,3,5,6,7,8 A less common subtype is Miller Fisher syndrome (MFS), which is characterized by ophthalmoplegia, ataxia and areflexia.9,10 Overall, the clinical course, severity and outcomes of GBS are highly variable.
The majority of patients with GBS report an infection before the onset of weakness. Antiganglioside antibodies are often detected; their levels decrease over time. Different types of antibodies are related to the preceding infection and the GBS subtype. Progressive weakness reaches its maximum within 4 weeks (often within 2 weeks). The recovery phase may last many weeks, months or even years. Abbreviation: GBS, Guillain–Barré syndrome. Reprinted from Lancet Neurology 7, van Doorn, P. A., Ruts, L. & Jacobs, B. C. Clinical features, pathogenesis, and treatment of Guillain–Barré syndrome, 939–950 © (2008), with permission from Elsevier.
GBS typically occurs after an infectious disease in which the immune response generates antibodies that crossreact with gangliosides at nerve membranes. This autoimmune response results in nerve damage or functional blockade of nerve conduction. The type of preceding infection and the specificity of the antiganglioside antibodies largely determine the subtype and clinical course of GBS. Over the past 10 years, much new information has been gathered about the role of antecedent infections and antiganglioside antibodies in the immunopathology of GBS. We now know that the most common pathogen causing the antecedent infection is Campylobacter jejuni, which is associated with the AMAN subtype of GBS.
Currently, intravenous immunoglobulin (IVIg) and plasma exchange are proven effective treatments for GBS.11,12,13,14,15 However, despite these treatment options, many patients have a severe disease course, pain, and residual deficits. In this Review, we summarize current data on the immune pathogenesis and clinical characteristics of GBS. We describe the current diagnostic criteria for GBS, and discuss the possible additional diagnostic value of cerebrospinal fluid (CSF) examinations and nerve conduction tests. In addition, we review treatment options and prognosis, including novel predictive models, for patients with GBS.
Epidemiology
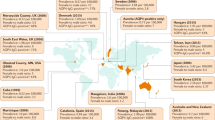
GBS is a rare disease with an incidence of 0.81–1.89 (median 1.11) per 100,000 person–years, and is more common in men than in women (ratio 3:2).1,16 Worldwide, the incidence is variable; for example, a low rate of 0.40 per 100,000 person–years was reported in Brazil, in contrast to a high rate of 2.5 per 100,000 person–years in Curaçao and Bangladesh.16,17,18,19,20 GBS seems to occur less frequently in children (0.34–1.34 per 100,000 person–years) than in adults,18 and its incidence increases with age.16,18 The background incidence of GBS in most studies remains constant over time, although seasonal fluctuations have occasionally been found in studies from Curaçao, Bangladesh and China.17,18,20,21
The proportions of patients with GBS who have AIDP and AMAN vary greatly around the world. AIDP is the predominant subtype (60–80% of patients) in North America and Europe.1,2,6 By contrast, the frequency of AMAN ranges from 6–7% in the UK and Spain to 30–65% in Asia, Central America and South America.6,7,22,23,24 The geographical diversity is probably attributable to differences in exposure to certain types of infection, possibly in combination with different genetic susceptibilities due to varying genetic polymorphisms between individuals or groups of people living in different areas of the world.25,26 These differences may be related not only to the development of a specific GBS subtype, but also to the course and severity of disease. Genetic studies with a high number of patients are required to investigate these relationships.
Pathogenesis
As indicated above, GBS is a postinfectious disorder. Two-thirds of patients report symptoms of a respiratory or gastrointestinal tract infection before the onset of GBS. In about half of patients with GBS, a specific type of preceding infection can be identified,27 and C. jejuni is responsible for at least one-third of these infections.3,24,27 Other pathogens that cause antecedent infections related to GBS are cytomegalovirus, Epstein–Barr virus, Mycoplasma pneumonia, Haemophilus influenzae, and influenza A virus.3,27,28 Notably, a case–control study conducted in the Netherlands showed that 5% of patients with GBS had a hepatitis E virus infection before onset of GBS, compared with 0.5% of matched healthy controls.29 Similarly, 10% of patients with GBS from Bangladesh had an antecedent hepatitis E virus infection, indicating that hepatitis E virus is a worldwide trigger of GBS.30 However, despite the strong association between specific acute infections and GBS, the overall risk of developing this severe postinfectious complication is very small. Only one in 1,000–5,000 patients with Campylobacter enteritis will develop GBS in the subsequent 2 months.31,32 This fact explains why GBS is a sporadic disorder, although outbreaks of GBS after C. jejuni infection have occasionally been reported.33
One of the critical steps in GBS pathogenesis after C. jejuni infection is the generation of antibodies that crossreact with specific gangliosides (Figure 2), which are not produced during uncomplicated C. jejuni gastroenteritis.34,35 However, the production of crossreactive antibodies is only induced in susceptible individuals.35,36 Antibodies that crossreact with various gangliosides have been described in patients with GBS.3,37,38,39 However, only a subset of C. jejuni strains contain lipo-oligosaccharides that mimic the carbohydrate moiety of gangliosides that are present in human peripheral nerves (Figure 2).3 The synthesis of these ganglioside-mimicking carbohydrate structures depends on a set of polymorphic genes and enzymes that vary greatly between different C. jejuni strains.40,41 The Thr51 variant of the C. jejuni cstII gene is associated with the occurrence of GBS, while the Asn51 variant is associated with MFS.42
Infections with pathogens, such as Campylobacter jejuni, can trigger humoral immune and autoimmune responses that result in nerve dysfunction and the symptoms of GBS. Lipo-oligosaccharides on the C. jejuni outer membrane may elicit the production of antibodies that crossreact with gangliosides, such as GM1 and GD1a on peripheral nerves. The antigens targeted in AMAN are located at or near the node of Ranvier. The anti-GM1 and anti-GD1a antibodies bind to the nodal axolemma, leading to complement activation followed by MAC formation and disappearance of voltage-gated sodium channels. This damage can lead to detachment of paranodal myelin, and nerve conduction failure. Macrophages then invade from the nodes into the periaxonal space, scavenging the injured axons. The antigens targeted in AIDP are, presumably, located on the myelin sheath. The antibodies can activate complement, which leads to formation of the MAC on the outer surface of Schwann cells, initiation of vesicular degeneration, and invasion of myelin by macrophages. Abbreviations: AIDP, acute inflammatory demyelinating polyneuropathy; AMAN, acute motor axonal neuropathy; APC, antigen-presenting cell; GBS, Guillain–Barré syndrome; MAC, membrane attack complex.
Some antibody specificities are associated with particular GBS subtypes and related neurological deficits, reflecting the distribution of different gangliosides in human peripheral nerves (Table 1).3,43 C. jejuni infections are predominantly, but not exclusively, related to the AMAN or pure motor subtype of GBS.44 Patients with AMAN frequently have serum antibodies against GM1a, GM1b, GD1a and GalNAc-GD1a gangliosides.3,7,37,45,46,47 Patients with MFS or MFS–GBS overlap syndrome (see below) frequently have antibodies against GD1b, GD3, GT1a and GQ1b gangliosides, which are related to ataxia and ophthalmoplegia.3,9,37,48,49 In a study from the Netherlands, 20% of patients with AIDP related to cytomegalovirus infection had anti-GM2 antibodies, although these antibodies are also found in patients with uncomplicated cytomegalovirus infections.27,50 Interestingly, as well as antibodies against single gangliosides, patients can also have antibodies against combinations of epitopes from ganglioside complexes.38,51,52,53 Such complexes are located in specialized microdomains, or 'lipid rafts', in the cell membrane.54 Antibodies that target ganglioside complexes also crossreact with C. jejuni lipo-oligosaccharides, and are probably induced by a preceding infection with C. jejuni.55 Antibodies against various combinations or complexes of glycolipids have also been reported in patients with AIDP, although the role of these antibodies in its pathogenesis remains to be determined.53
In conjunction with the presence of antiganglioside antibodies, complement activation seems to contribute to nerve degeneration in GBS56,57—a phenomenon that has been studied at the nodes of Ranvier and at the motor nerve terminal in a mouse model of AMAN.58 Sodium channel clusters, as well as paranodal axoglial junctions, the nodal cytoskeleton, and Schwann cell microvilli, all of which stabilize the sodium channel clusters, were disrupted by complement activation in a GBS disease model.7,59,60 Additional studies in a GBS mouse model provided evidence that blockade of complement activation prevents emergence of the clinical signs of antiganglioside-mediated neuropathy.61
The development of GBS after a C. jejuni infection may also depend on patient-related factors that influence the susceptibility to produce crossreactive, carbohydrate-targeted antibodies. This hypothesis is supported by the fact that GBS has a relapse rate of 5%, which is clearly higher than would be expected by chance.62 The initial pathogen–host interaction has a key role in the development of GBS. C. jejuni lipo-oligosaccharides bind to siglec-7 (sialic acid-binding immunoglobulin-like lectin 7) and activate dendritic cells via Toll-like receptor 4 and CD14. These dendritic cells produce type 1 interferon and tumour necrosis factor (TNF), which induce proliferation of B cells.35,63,64 This immune activation could be influenced by genetic polymorphisms but, to date, genetic factors have only been studied in small cohorts of patients. Interestingly, a meta-analysis identified a moderate association between GBS and a particular TNF polymorphism.65 In addition, an association between polymorphisms in the MBL2 gene (encoding mannose-binding protein C) and the severity and outcome of GBS has been confirmed.25 Future genome-wide association studies in large, well-described and adequately controlled cohorts are required to establish the role of host factors in the pathogenesis of GBS.
The potential role of vaccination
A few patients develop GBS shortly after receiving a vaccination. Despite their rarity, such events cause considerable public concern. In the vaccination campaign against influenza A (H1N1) in the USA in 1976, the estimated attributable risk of vaccine-related GBS was about one in 100,000.66 A similar association was suggested for the vaccination campaign against influenza A (H1N1) in 2009, but extensive national and international studies found that vaccination was associated with only a small attributable risk of GBS: 1.6 excess cases of GBS per 1,000,000 vaccine recipients, a frequency similar to that for all seasonal vaccinations.67 In fact, vaccination might even reduce the risk of acquiring GBS, as this condition can be caused by infections such as influenza. The risk of developing GBS after influenza infection is estimated to be 4–7 times higher than after influenza vaccination.68 No relapses of GBS in patients with a history of this disease have been observed after influenza vaccination.68,69
For these reasons, the following practical guideline regarding vaccination of patients with a history of GBS is currently used in the Netherlands: GBS as such is not an indication for influenza vaccination, and vaccination seems to be safe in patients who developed GBS >3 months ago and when onset of GBS was not shortly after vaccination.70
Diagnosis
Diagnostic criteria
In 1978, the US National Institute of Neurological Disorders and Stroke (NINDS) developed case definitions for GBS in the course of investigating the suspected association between GBS and the swine flu vaccination campaign of 1976–1977. The initial diagnostic criteria published in 1981 were modified in 1990.4,71 Though primarily developed for research purposes, they are probably still the most widely used criteria in clinical practice.4 The criteria consist of features that are required for or strongly support the diagnosis of GBS, and features that cast doubt on the diagnosis (Box 1).
In 2011, the Brighton Collaboration published new case definitions for GBS while studying a possible association between GBS and the H1N1 swine flu vaccination campaign of 2009–2010.72 These criteria were specifically developed for retrospective epidemiological and vaccine safety studies and, consequently, are likely to combine high specificity with limited sensitivity. The Brighton criteria identify GBS with four levels of diagnostic certainty, from level 1 (highest) to level 4 (lowest). Use of the Brighton criteria to classify patients with suspected GBS is highly dependent on completeness of the diagnostic data. A study from the Netherlands in 335 patients with GBS with complete sets of diagnostic data—which are required for level 1 certainty according to the Brighton criteria—classified 61% as level 1, 33% as level 2, none as level 3 and 6% as level 4. However, patients diagnosed at different levels of diagnostic certainty did not differ in disease severity or outcome.73 In studies from Korea and India in patients who had GBS, 24% and 14% of patients, respectively, were classified as level 4.74,75 The Brighton criteria are not, however, intended to be used for diagnostic purposes in clinical practice. Further research is needed to develop criteria that can be used to diagnose GBS and its less-frequent variants in the acute phase of the disease. However, in practice, the criteria published in 1990 still provide a good basis for clinicians worldwide to make a diagnosis of GBS.
Clinical symptoms and subtypes of GBS
GBS is characterized by a rapidly progressive, symmetrical weakness of the limbs in combination with hyporeflexia or areflexia.2,4,73 However, GBS is highly diverse with respect to the presence, distribution and extent of cranial nerve deficits, sensory symptoms, weakness, ataxia, pain, autonomic dysfunction, and the course of the disease. Many patients have sensory deficits, such as numbness and/or paraesthesias.4 About half of the patients have cranial nerve deficits, especially bilateral facial weakness, swallowing difficulties or (sometimes) extraocular motor dysfunction.4 A high proportion (54–89%) of patients with GBS experience pain, including painful paraesthesias, backache, muscle pain and meningism, which may even precede the onset of muscle weakness in about one-third of GBS cases.2,4,76,77 Approximately 25% of patients develop respiratory insufficiency requiring artificial ventilation.73,78,79,80 Autonomic dysfunction (predominantly cardiovascular dysregulation) is present in about two-thirds of patients, although its severity is highly variable.2,77,81 About one-third of patients remain able to walk throughout the course of the disease, and are often described as mildly affected.
GBS is a monophasic disease, usually reaching maximum severity (nadir) within 4 weeks.1,2,4 One study showed that 80% of patients with GBS reach the nadir within 2 weeks after onset of weakness, and 97% reach the nadir within 4 weeks.73 A further subset of patients reach the nadir within 4–6 weeks of onset of weakness.73,82 The progressive phase is usually followed by a plateau phase ranging from 2 days to 6 months (median duration 7 days) before patients start to recover (Figure 1).73
Various subtypes of GBS have been reported that differ in their clinical, electrophysiological and histological features (Table 1 and Box 1).1,3,6,7,8,23 The two best-known GBS subtypes are AIDP and AMAN. AIDP is a sensorimotor form of GBS that is often accompanied by cranial nerve deficits, autonomic dysfunction, and pain. This condition is characterized by a demyelinating polyneuropathy at electrophysiological examination.1,3,8 By contrast, AMAN is a pure motor form of GBS, in which the axonal polyneuropathy is not accompanied by sensory deficits at clinical and electrophysiological examination (although 10% of patients with AMAN do have sensory symptoms).6,7,8,46 Cranial nerve deficits are less frequent than in AIDP, but patients with AMAN may have autonomic dysfunction and pain.3,7,77 Usually, disease progresses more rapidly in AMAN than in AIDP, and recovery is often prolonged, owing to axonal degeneration. However, some patients with AMAN recover quickly, even from severe weakness.83 AMAN is frequently associated with an antecedent C. jejuni infection.7,8,46
In some patients with axonal GBS, sensory as well as motor fibres are affected. This subtype, termed acute motor and sensory axonal neuropathy (AMSAN), can be considered a severe variant of AMAN.1,3,7 MFS is an uncommon subtype of GBS characterized by the clinical triad of ophthalmoplegia, ataxia and areflexia.9,10,49,84 In most patients, diplopia is the presenting symptom.9,10,49 Patients with MFS usually have a good clinical outcome but some develop limb weakness and respiratory insufficiency (termed MFS–GBS overlap syndrome). A new electrophysiological technique called compound muscle action potential (CMAP) scanning has shown that some patients with MFS also have subclinical limb motor nerve dysfunction.85 Other local variants of GBS, such as the pharyngeal–cervical–brachial variant, have also been reported.3,84,86
Atypical GBS
About 8% of patients with GBS present with paraparesis, which often complicates the diagnosis and requires extensive diagnostic work-up. Paraparesis may persist in about 70% of these patients during follow-up.73 Definite asymmetrical limb weakness, however, is very uncommon in patients with GBS.73
Although the 1990 GBS criteria require hyporeflexia or areflexia for the diagnosis of GBS, in one cohort of patients with GBS, 9% had normal tendon reflexes in weak arms and 2% had normal tendon reflexes in weak legs at presentation.73 During follow-up, all patients developed hyporeflexia or areflexia in their legs, but in some patients, normal reflexes persisted in the arms.73 For an as yet unknown reason, a small proportion of patients with GBS, especially those with the AMAN subtype, have well-preserved or even exaggerated tendon reflexes.7,87
Additional investigations
Lumbar puncture
A lumbar puncture is often performed in patients with suspected GBS. Importantly, this procedure especially should be done to exclude other diagnoses rather than to confirm GBS. A combination of elevated protein level and normal cell counts in the CSF (termed albuminocytological dissociation) is considered a hallmark of GBS. A frequent misconception, however, is that albuminocytological dissociation must always be present to confirm the diagnosis,1,2,3,88 as only 64% of patients with GBS have this feature. Elevated CSF protein levels are found in approximately 50% of patients in the first 3 days after onset of weakness, which increases to 80% after the first week.73
CSF cell counts >50 cells per μl should cast doubt on the diagnosis of GBS, and other differential diagnoses should be considered, such as leptomeningeal malignancy, lymphoma, cytomegalovirus radiculitis, HIV polyneuropathy and poliomyelitis.1,2,3,73,88 If the protein level in the CSF is normal, repeat lumbar punctures are not usually recommended because albuminocytological dissociation is not necessary to diagnose GBS. In addition, treatment with high-dose IVIg can increase both protein levels and cell counts in the CSF, likely due to transudation or to aseptic meningitis, which can confuse the diagnostic picture in patients who undergo a repeat lumbar puncture.
Muscle and nerve electrophysiology
Nerve conduction studies (NCS) can help to support the clinical diagnosis of GBS and discriminate between axonal and demyelinating subtypes. Diagnosis of GBS can sometimes be difficult in the early phase of the disease, especially when reflexes are still present or the weakness is not distributed according to the classic pattern (for instance, in patients with paraparesis). NCS can demonstrate abnormalities in locations with subclinical disease, such as the arms. NCS findings of peripheral neuropathy or polyradiculopathy can also help to confirm the diagnosis of GBS.
Nerve conduction abnormalities tend to peak >2 weeks after the onset of weakness.6 However, if NCS are required to confirm a diagnosis of suspected GBS, a delay of 2 weeks is often too long. Although NCS can be performed earlier in the disease course, the results might still be normal at this stage. Often, the first-detected NCS abnormalities are prolonged or absent F-waves, although other conduction abnormalities become evident as the disease progresses. To increase the diagnostic yield of NCS, at least four motor nerves, three sensory nerves and F-waves should be investigated.
Abnormalities found on NCS depend on the GBS subtype (AIDP, AMAN or AMSAN). In patients with AIDP, NCS reveal features of demyelination, including prolonged distal motor latency, reduced nerve conduction velocity, prolonged F-wave latency, increased temporal dispersion, and conduction block. The sural sensory potential is often preserved.89 Features of axonal GBS (AMAN or AMSAN) include decreased motor and/or sensory amplitudes, typically in the absence of demyelinating features. Sensory-nerve studies can help to differentiate between AMAN and AMSAN. In AMAN, neurophysiological findings can be very complex, as some patients with this condition have transient conduction block or slowing, which rapidly recovers during the course of the disease—a phenomenon called reversible conduction failure.7,90,91,92,93
Reversible conduction failure can mimic demyelination, and is probably caused by impaired conduction at the node of Ranvier caused by antiganglioside antibodies. Besides reversible conduction failure, other NCS features that suggest demyelination can sometimes be observed in the acute phase of axonal GBS.94 Patients with reversible conduction failure may be falsely diagnosed as having AIDP instead of AMAN. Serial NCS might be needed to reliably distinguish these two subtypes of GBS;95 for example, in an Italian study, 24% of patients initially classified as having AIDP were reclassified as having AMAN when serial NCS were performed.92
Since no consensus exists on which neurophysiological criteria are best for confirming the diagnosis of GBS subtype, multiple classification systems are used.6,23,95 At present, however, subtype classification does not seem to influence treatment choices, as patients with axonal and demyelinating forms of GBS currently receive similar treatment, at least in principle.
Testing for antiganglioside antibodies
Although antiganglioside antibodies are involved in the pathogenesis of GBS, their role in diagnosis has not been established. In general, the frequency of each specific antibody is low, implying that the negative predictive value of detection tests will also be low, and that the negative test findings cannot, therefore, exclude GBS as a diagnosis. In addition, tests for detecting these antibodies have a limited positive predictive value, as antiganglioside antibodies (especially those of the IgM class) also occur in other diseases. Possible exceptions to this rule might be anti-GQ1b antibodies, which are present in the serum of at least 90% of patients with MFS, and anti-GM1 and anti-GD1a IgG antibodies, which are frequently found in patients with AMAN.7,9,37,46,47,48,49 Detection of these specific antibodies might be diagnostically helpful, provided that validated assays are used.96 Moreover, research into antiganglioside antibody detection methods is rapidly progressing, and more-sensitive and more-specific tests may emerge in the near future.
Differential diagnosis
In patients with typical features of GBS, diagnosis is usually straightforward, but in patients with atypical features, GBS can sometimes be difficult to recognize. Even in patients with typical features, a lumbar puncture is recommended to rule out diagnoses other than GBS. The differential diagnosis of GBS includes infectious diseases, malignancy and disorders of the neuromuscular junction.1,2,97,98,99
In patients with an elevated cell count in the CSF, differential diagnoses such as spinal root inflammation due to cytomegalovirus or HIV, transverse myelitis, Lyme disease, leptomeningeal malignancy, or poliomyelitis should be considered.97,98,99 Laboratory investigations can also be helpful to reveal other causes of GBS-like symptoms, such as electrolyte disturbances (especially hypokalaemia) and vitamin B1 deficiency.
In patients with pure motor symptoms, differential diagnoses of myasthenia gravis, polymyositis and dermatomyositis, poliomyelitis, hypermagnesaemia, porphyria, botulism, and lead or organophosphate poisoning should be considered.97,98,99 NCS can be helpful in such individuals to differentiate between polyneuropathy, myopathy, anterior horn cell disease (poliomyelitis), and disorders of the neuromuscular junction.
When a diagnosis of GBS is considered in a patient with paraparesis or abnormal spinal sensory level at neurological examination, MRI of the spinal cord, and possibly also CSF examination, should be performed to exclude spinal cord compression or transverse myelitis. NCS can also be helpful in these patients, especially when they reveal signs of demyelinating polyneuropathy or nerve conduction abnormalities in clinically unaffected arms, as both can be indicative of GBS. MRI findings of nerve root enhancement also support a diagnosis of GBS.100 For patients with bladder or bowel dysfunction at onset or who develop persistent bladder or bowel dysfunction, the differential diagnoses include spinal cord or caudal compression, and transverse myelitis.
If a patient has asymmetric weakness, differential diagnoses such as vasculitic neuropathy, multiple mononeuropathy, Lyme disease, diphtheria, poliomyelitis and leptomeningeal malignancy should be considered.97,98,99 When the severity of respiratory failure is disproportionate to that of limb weakness, disorders such as myasthenia gravis, hypermagnesaemia, hypophosphataemia, high cervical intramedullary lesions, poliomyelitis and botulism should be excluded.97,98,99
Diagnosis of GBS in children
The clinical presentation and outcome of GBS is different in children compared with adults, and diagnosis of childhood GBS can be challenging, especially in young children aged <6 years.101,102,103,104 Pain, difficulty with walking, or refusing to walk are the most frequent presenting symptoms in children, and should raise suspicion of GBS.101,102,103,104 However, only one-third of preschool children with GBS receive a correct diagnosis at admission.103 In young children, GBS may initially be diagnosed as meningitis, coxitis, or malaise caused by viral infections. Moreover, the diagnosis of GBS in children is often delayed. In preschool children (aged <6 years), the delay in diagnosis can be even more than 2 weeks.103 Insufficient monitoring of these children during this period may result in emergency intubation and even death.105
Assessment scales
Over the past few decades, the GBS Disability Scale has been used as an outcome scale in the majority of clinical trials in GBS. The GBS Disability Scale has six levels: 0 (healthy), 1 (minor symptoms and capable of running), 2 (able to walk 10 m without assistance but unable to run), 3 (able to walk 10 m across an open space with help), 4 (bedridden or wheelchair-bound), 5 (requiring assisted ventilation for at least part of the day), and 6 (dead).106
GBS assessment scales must be valid, sensitive, reliable, and able to capture subtle clinical changes over time. The Peripheral Neuropathy Measures Outcome Study (PERINOMS) accordingly investigated a large number of assessment scales.107 In a European Neuromuscular Centre meeting, the PERINOMS study group reached a consensus about the use of a variety of measures for the follow-up of patients with GBS in future trials.107 They recommended using the GBS Disability Scale and the Rasch-built Overall Disability Scale to measure disability, and both the Medical Research Council (MRC) sum score (ranging from 0–60) and the new Rasch-built MRC score to measure muscle strength.106,107,108,109,110
Treatment
Treatment of GBS usually combines multidisciplinary supportive medical care and immunotherapy (Figure 3). Proven effective treatments for GBS are IVIg and plasma exchange.11,12,13 Immunotherapy is usually started if patients are not able to walk 10 m unaided (GBS Disability Scale score ≥3).2,11 Plasma exchange and IVIg have pleiotropic immunomodulatory effects, but we have yet to establish which effects explain their therapeutic efficacy in GBS, and whether the same effects are involved in all patients and all subtypes of GBS.
*If a non-GBS disorder is suspected, target laboratory investigations accordingly. ‡In case of cell count >50 cells per μl, consider spinal nerve root inflammation due to other causes. Normal cell counts and elevated cerebrospinal fluid protein level (albuminocytological dissociation) are indicative of GBS; however, protein level can be normal, especially in the first week.73 §When no other diagnosis could be confirmed by laboratory investigation, lumbar puncture or NCS. Consider performing NCS to subclassify GBS after 1–2 weeks. ||Indications for intensive care unit admission are rapidly progressive weakness with impaired respiration (vital capacity <20 ml/kg), need for artificial ventilation, insufficient swallowing (often with severe weakness), and severe autonomic dysfunction. ¶Or if the treating physician decides that there is an indication for treatment, for example, rapid progressive weakness, mild weakness with severe autonomic dysfunction, or severe swallowing problems. #IVIg: start within 2 weeks of onset: 0.4 g/kg daily for 5 days. PE: start 5 × PE with a total exchange volume of five plasma volumes in 2 weeks. Abbreviations: A-CIDP, acute-onset chronic inflammatory demyelinating polyneuropathy; EGRIS, Erasmus GBS Respiratory Insufficiency Score; GBS, Guillain–Barré syndrome; ICU, intensive care unit; IVIg, intravenous immunoglobulin; NCS, nerve conduction studies; PE, plasma exchange.
IVIg treatment may inhibit Fc-mediated activation of immune cells, binding of antiganglioside antibodies to their neural targets or local complement activation.12,111 Serum IgG Fc glycosylation in patients with GBS seems to be associated with disease severity and could influence the immunomodulatory effects of IVIg.112
Plasma exchange is thought to remove neurotoxic antibodies, complement factors and other humoral mediators of inflammation.11,13 Plasma exchange is beneficial when performed within the first 4 weeks after onset of weakness in patients who are unable to walk unaided (GBS Disability Scale score ≥3), but the largest effect is seen when treatment is started within the first 2 weeks.11,13,113,114 The usual plasma exchange regimen consists of five treatments administered over 2 weeks, involving a total of about five plasma volumes. In mildly affected patients (still able to walk), however, two plasma exchange sessions induced more-rapid onset of motor recovery than did no plasma exchange.115
IVIg is effective in patients who are unable to walk 10 m unaided (GBS Disability Scale score ≥3) and when started within 2 weeks of onset of weakness.11,12 Randomized controlled trials showed that IVIg at a dose of 0.4 g/kg daily for 5 consecutive days (or 1 g/kg daily for 2 days) was as effective as a full course of five plasma exchange sessions applied over 2 weeks.80,116 Whether rapid IVIg treatment over 2 days is superior to treatment with the same total dose (2 g/kg) administered over 5 days has not been fully evaluated. However, one trial demonstrated that children receiving treatment over 2 days more frequently had treatment-related fluctuations than did children receiving treatment over 5 days.117 As IVIg therapy is widely available, does not require special equipment, and generally has only minor adverse effects, it has replaced plasma exchange as the preferred treatment for GBS in many hospitals.11,12 Immunoabsorption, as an alternative to plasma exchange, is occasionally used as a treatment for patients with GBS, and may be equally effective. However, no large-scale randomized controlled trials have shown that treatments other than IVIg or plasma exchange are effective.11,12
The choice of treatment depends on both patient-related and socioeconomic factors. For instance, plasma exchange requires special equipment and is not always available in all hospitals. In addition, plasma exchange can be difficult to perform in young children, and care should be taken in patients with autonomic cardiovascular instability because of the large volume shifts involved in the plasma exchange procedure. However, the direct costs of IVIg treatment can be more than twice those of plasma exchange, making this treatment less attractive in low-income countries.118,119 In this respect, it is important to remember that most clinical trials of these treatments were conducted in Western Europe or North America and, therefore, predominantly involved patients who fulfilled the most commonly used GBS diagnostic criteria.4 The results of these trials might be less applicable in other parts of the world, especially where AMAN is highly prevalent.
Whether patients with AMAN should receive the same treatment as those with AIDP remains uncertain. Results from a small study, which unfortunately had some methodological flaws, suggested that patients with AMAN might have better outcomes after treatment with plasma exchange than after IVIg therapy, and that plasma exchange was also the most cost-effective option.120 However, in countries where plasma exchange machines are not widely available or patients cannot afford this expensive procedure, small-volume plasma exchange or exchange transfusion can be a low-cost therapeutic option.121,122,123,124 Controlled studies of these procedures are currently lacking.
The combination of plasma exchange followed by IVIg is not significantly better than either plasma exchange or IVIg alone.11,80 Oral steroids and intravenous methylprednisolone are not beneficial in patients with GBS.11,15,79 The combination of IVIg and methylprednisolone is no more effective than IVIg alone, although this combined treatment might have some additional short-term benefits when known prognostic factors are taken into account.79 Small randomized placebo-controlled trials of IFN-β1a and brain-derived neurotrophic factor, and one trial studying a 6 week course of mycophenolate mofetil combined with standard IVIg versus IVIg alone, did not indicate beneficial effects of these treatments.14,125
No randomized controlled trials have been performed in patients with MFS.126 A retrospective analysis showed that recovery starts slightly earlier in patients with MFS treated with IVIg than in those who were treated with plasma exchange or received no immunotherapy. However, final outcomes were the same in all three groups.126,127 Indeed, almost all patients with MFS recover fully, irrespective of whether they receive immunotherapy.126,127 Owing to the lack of evidence of a beneficial effect of IVIg or plasma exchange in patients with MFS, combined with the good natural recovery seen in these patients, withholding of immunotherapy in patients with MFS seems currently justified. However, patients with MFS–GBS overlap syndrome can be severely affected, and treatment with IVIg or plasma exchange remains an option for these patients. Notably, no large-scale randomized controlled trials have been performed to determine the optimal treatment strategy in children with GBS and they are, therefore, usually treated in the same manner as adults with GBS.104
Importance of supportive care in GBS
A patient in the progressive phase of GBS requires hospital admission. Important questions are how to monitor progression and how to avoid or treat complications related to weakness, immobility, respiratory insufficiency, autonomic dysfunction, and pain. Patients with GBS need multidisciplinary supportive care to prevent or to manage these diverse complications (Figure 3),128 and to facilitate timely transfer to the intensive care unit (ICU) when indicated.
Care includes monitoring of respiratory function by frequent measurement of vital capacity and other clinical parameters, such as respiratory depth, respiratory frequency and cough strength. The optimal frequency to measure these vital functions has not been investigated, but is probably about once every 1–4 h depending on the rate of deterioration. The duration of ventilation may be shortened by selective digestive tract decontamination.129
Other issues that require attention are prophylaxis against deep vein thrombosis, cardiac and haemodynamic monitoring, pain management, management of possible bladder and bowel dysfunction, physiotherapy, rehabilitation, and psychosocial support.2,128 GBS can be a very challenging disorder for both patients and their relatives, who may benefit from contacting national or international GBS-related patient organizations.
Deterioration after initial improvement
About 10% of patients with GBS who have been treated with IVIg or plasma exchange deteriorate after initial improvement or stabilization—a phenomenon that is termed treatment-related fluctuation (TRF).130,131 These patients usually improve after retreatment with IVIg or plasma exchange, and although the efficacy of retreatment has never been demonstrated in a randomized controlled trial, this approach has become common practice. On the basis of clinical experience, we and others advise retreatment with IVIg (2 g/kg over 5 days) in patients who develop TRF.2 These patients may have a prolonged autoimmune response that causes ongoing nerve damage, or functional blockade that requires prolonged treatment.
GBS with extended progression phase
Some patients experience multiple periods of deterioration or have a progression phase that exceeds 4 weeks. In these patients, the question often arises of whether the patient really has GBS, or whether they have acute-onset chronic inflammatory demyelinating polyneuropathy (A-CIDP).130 A diagnosis of A-CIDP should be considered when patients who were initially diagnosed with GBS have three or more periods of clinical deterioration, or when new deterioration occurs >8 weeks after disease onset (Table 2).130,132 It is vitally important to recognize any late or additional deteriorations, because patients with GBS–TRF may improve after retreatment with IVIg, whereas those with A-CIDP often require chronic maintenance treatment with IVIg or a therapeutic switch to corticosteroids.
Residual deficits
Adult patients with GBS frequently have residual deficits that greatly impair their daily activities and quality of life.133,134,135,136,137,138,139 For example, 6 months after disease onset, about 20% of patients with GBS are still not able to walk unaided.1,2,11 Most improvement occurs within the first year after onset, but can continue after this period.140,141 The most common residual deficits are reduced muscle strength, sensory signs, fatigue, and pain.77,135,138,139 Many patients have to make changes to their lifestyle, work, and social activities.133,135 However, even patients with a good functional outcome (GBS Disability Scale score ≤1) have a reduction in psychosocial health status.134 Some evidence suggests that high-intensity, multidisciplinary rehabilitation reduces disability and improves quality of life in patients with GBS.136,142,143 Children with GBS may have better outcomes than adults, although the long-term residual effects on daily life in children have not been established.102,104
Long-lasting symptoms of fatigue are present in the majority of patients with GBS.138 Fatigue can be assessed using the fatigue severity scale, and the Rasch-built fatigue severity scale.144 The precise pathophysiological mechanisms leading to fatigue are not well understood, but axonal loss seems to be a contributory factor.145 A noncontrolled, nonblinded study showed that physical training is feasible and effective in patients who have, neurologically, recovered well from GBS, but who still have severe fatigue.136
Moderate to severe pain is very common in patients with GBS. A prospective follow-up study showed that two-thirds of patients report pain within the first 3 weeks after onset, and one-third still have pain after 1 year.77 Up to 89% of patients experience pain at some point during their disease course,76 and pain may even precede weakness in about one-third of patients.77 The most common locations of pain are the extremities or the back; patients mainly report muscle pain, painful paraesthesias, radicular pain, arthralgia or meningism.77 Attention must be paid to pain during the entire disease course because although pain can be very severe, it is often under-recognized. Pain can be treated with neuropathic analgesics, but not all patients have a good response to such treatment. A Cochrane review on the pharmacological treatment of pain in patients with GBS showed that evidence to support a pain-relieving effect of analgesics in this condition is scarce.146 The precise causes of pain in GBS are probably diverse, and may vary over the course of the disease.147 Notably, distal intraepidermal nerve fibre density is reduced in patients with GBS, and is associated with both incidence and severity of pain (but not with autonomic dysfunction, as discussed below).148,149
Autonomic dysfunction predominantly occurs in the acute phase of GBS but can also occur in the recovery phase. It can be a serious problem in patients with GBS and may cause sudden death.150,151,152 Tachycardia (38%), hypertension (69%), gastrointestinal dysfunction (45%), and bladder dysfunction (19%) have been reported in a series of 156 GBS patients.77 Patients with severe cardiovascular dysfunction can have rapid changes in blood pressure and cardiac dysrhythmia that sometimes require a cardiac pacemaker. In children, autonomic dysfunction was present in half of the mildly affected patients and seemed not to be related to the severity of the disease,81 which implies that autonomic disturbances are common and may occur throughout the spectrum of severity of GBS.
Autonomic dysfunction in patients with GBS reflects dysfunction of sympathic and/or parasympathic innervation, but the exact immunopathological mechanisms remain to be elucidated. Specifically, the relationship between specific antiganglioside antibodies and autonomic dysfunction needs to be investigated in more detail. We did not observe a correlation between reduction of intraepidermal nerve fibre density and autonomic failure.149 The reason why some patients have severe autonomic dysfunction that can include light-fixed pupils and excessive sweating, whereas others have severe cardiac dysrhythmia, is currently unknown and, unfortunately, cannot be predicted from a clinical point of view. Careful monitoring for the presence of features of autonomic dysfunction is indicated also after a patient is discharged from the ICU.
Prognosis and outcome
As the clinical course and outcomes of GBS are highly variable, their accurate prediction is important to enable clinicians to tailor supportive care and treatment to the individual patient's needs and to inform patients and relatives about the expected clinical course.
Predictors of need for ventilation
Three large studies have been performed to predict the probability of respiratory insufficiency in patients with GBS. A French study including 722 patients found that time from onset to admission of <7 days, inability to cough, inability to stand, inability to lift the elbows or head from the bed, and increased liver enzyme levels were predictors of an increased probability of need for artificial ventilation.153 A second French study found that peroneal nerve conduction block and low vital capacity correlated with a high risk of respiratory failure.154 The third study was conducted in the Netherlands, and used data from a derivation cohort of 397 patients with GBS to identify clinical predictors of mechanical ventilation, which were validated in an independent cohort of 191 patients with GBS.155
The results of the Dutch study led to development of the Erasmus GBS Respiratory Insufficiency Score (EGRIS).155 EGRIS is an accurate prediction model that can be used in the emergency room to predict the probability of respiratory insufficiency in the first week after admission for GBS.155,156 The model incorporates the following parameters: severity of weakness (expressed as the MRC sum score), the number of days between onset of weakness and admission, and facial and/or bulbar weakness (Supplementary Figure 1 online). If a patient's predicted chance of developing respiratory insufficiency is high, it can be advisable to admit the patient to the ICU rather than to a general neurology ward.
Factors that are predictive of successful weaning from the ventilator are age <60 years,157 lack of autonomic dysfunction, and vital capacity >20 ml/kg or an improvement in vital capacity of 4 ml/kg.158 Autonomic dysfunction, advanced age and pulmonary comorbidity are associated with a long duration of mechanical ventilation and the need for tracheostomy.158,159
Predictors of poor long-term outcomes
In almost all studies, poor outcome is defined as a GBS Disability Scale score ≥3 after either 6 months or 12 months.160,161,162,163 Such a high grade on the GBS Disability Scale at neurological examination, diarrhoea preceding GBS onset,28,160,163,164 and advanced age28,78,140,141,154,160,162,163,164,165 are all predictors of poor outcome.
Validated prognostic models have been developed for use in clinical practice to predict long-term outcome in individual patients with GBS. An example is the Erasmus GBS Outcome Score (EGOS), which is based on three clinical characteristics: age, GBS Disability Scale score at 2 weeks after hospital admission, and preceding diarrhoea.156,163 However, the 2-week delay before EGOS can be determined may be too long to adequately tailor treatment according to the patients' predicted outcome. By contrast, the modified EGOS can be used to predict outcomes early in the course of GBS, before irreversible damage occurs.156,166 This model can be used at admission and at 1 week after admission, and is based on age, severity of weakness (expressed as MRC sum score), and preceding diarrhoea (Supplementary Figure 2 online).
Electrophysiological findings
In addition to their diagnostic role, electrophysiological findings might have prognostic relevance. In one NCS study, patients with features of demyelination more often required mechanical ventilation than did patients without this type of damage.154 The most consistent electrophysiological finding predictive of poor outcome is low CMAPs.167 However, some studies demonstrated that an axonal neuropathy is not necessarily a predictor of poor outcome, since patients with AMAN can either improve very slowly and incompletely or recover rapidly.22,168 These observations seem inconsistent, but rapid recovery might be caused by restoration of transient conduction block. Further studies are required to precisely delineate the relationships between conduction block, the presence of antiganglioside antibodies, the effects of treatment, and outcome.
Predictors of mortality
Mortality from GBS varies between 3% and 7%.140,169,170 Predictors of an increased risk of death are advanced age, severe disease, increased comorbidity, pulmonary and cardiac complications, mechanical ventilation, and systemic infection.140,160,169,170,171 Death can occur in all phases of the disease; however, in two studies, a large proportion of the deaths occurred >30 days from onset, and a subsequent study showed that the majority of patients who died were in the recovery phase.160,170,171 Consequently, severely affected patients in the recovery phase of GBS and after discharge from the ICU still require good observation and supportive care.170 The most common causes of death are respiratory insufficiency, pulmonary infection, autonomic dysfunction, and cardiac arrest.78,160,170,171
Ongoing research
Nearly a century after it was first described, GBS is still a life-threatening disorder that results in a poor outcome in at least 20% of patients and has persistent residual effects in the majority. Further research is urgently required to improve this situation. From a clinical perspective, the following are the most challenging needs: to develop improved diagnostic criteria for use in daily clinical practice, trials and vaccine safety studies; to determine the burden of disease caused by GBS worldwide; to develop new and better GBS outcome measures; to establish the precipitating events and patient-related factors that lead to GBS; to define biological and clinical predictors of the clinical course and outcome in individual patients; and, most importantly, to develop more-effective and specific treatments, as well as protocols for supportive care.
These aims can probably only be achieved by large-scale international and multidisciplinary collaborations, such as the International GBS Outcome Study (IGOS), which was launched in 2012. Tissue samples and detailed, standardized clinical data are being collected during a follow-up period of 1–3 years with the intention of including at least 1,000 patients with GBS from all over the world. At present, centres from 17 countries—Argentina, Australia, Bangladesh, Belgium, Canada, Denmark, France, Germany, Italy, Japan, Malaysia, Netherlands, Spain, South Africa, Taiwan, UK and the USA—are recruiting patients. In addition, a randomized controlled trial, the SID-GBS study, is being conducted in the Netherlands. This trial is investigating the effect of a second course of IVIg given shortly after the first course in patients with GBS who have a poor prognosis (defined as a mEGOS score of 6–12 at 1 week after initiation of a standard 5 day course of IVIg). A related international study with an observational prospective design (I-SID-GBS) is investigating the same approach. This study is part of IGOS and is being performed by the Inflammatory Neuropathy Consortium.
In addition, a new randomized placebo-controlled trial of eculizumab in patients with early GBS who are unable to walk is about to start.172 This study is partly based on findings in an animal model of GBS, in which antiganglioside antibodies induce complement-dependent damage at the nodes of Ranvier, nerve terminals, and perisynaptic Schwann cells (Figure 2).59,173 Notably, these deleterious effects of complement on nerve terminals in mice can be blocked by the administration of eculizumab, a humanized monoclonal antibody that binds with high affinity to complement factor C5 and prevents its cleavage to C5a and the proinflammatory, cytolytic C5b-9 complex.61 Many other studies, such as those investigating pain treatment, nerve regeneration, and other factors that may improve the outcomes of patients with GBS, are eagerly awaited.
Conclusions
GBS is a heterogeneous and often severe disorder. Although nonspecific immunotherapy is available and effective in most patients, a need remains for improved treatment and patient care throughout the disease course. Optimal supportive medical care is also essential to prevent or treat disease-related complications. Novel prognostic models have been developed and might enable treatment to be tailored to each patient's requirements.
Although a large amount of information on the immunopathogenesis of the various subtypes of GBS has been collected, further research is still needed. In the past few years, new large-scale clinical studies based on worldwide collaborations have been started and will help us to further define this syndrome and to optimize the care of affected patients.
Review criteria
PubMed was searched for articles published between January 1990 and March 2014. MeSH search terms were “Guillain–Barré syndrome” alone and in combination with “epidemiology”, “immunology”, “genetics”, “therapy”, “drug therapy” or “mortality”. Non-MeSH search terms were “Guillain–Barré syndrome”, “acute inflammatory demyelinating polyneuropathy”, “acute motor axonal polyneuropathy” and “Guillain-Barré syndrome” combined with “epidemiology”, “diagnosis”, “diagnostic criteria”, “infection”, “antibodies”, “immunology”, “nerve conduction studies”, “electrophysiology”, “treatment”, “genetics”, “vaccination”, “autonomic dysfunction” or “pain”. Only papers in English were reviewed. Articles were selected for their relevance, with a preference for new papers. Some other relevant papers known by the authors were also included.
References
Hughes, R. A. & Cornblath, D. R. Guillain–Barré syndrome. Lancet 366, 1653–1666 (2005).
van Doorn, P. A., Ruts, L. & Jacobs, B. C. Clinical features, pathogenesis, and treatment of Guillain–Barré syndrome. Lancet Neurol. 7, 939–950 (2008).
Yuki, N. & Hartung, H. P. Guillain–Barré syndrome. N. Engl. J. Med. 366, 2294–2304 (2012).
Asbury, A. K. & Cornblath, D. R. Assessment of current diagnostic criteria for Guillain–Barré syndrome. Ann. Neurol. 27 (Suppl.), S21–S24 (1990).
Griffin, J. W. et al. Guillain–Barré syndrome in northern China. The spectrum of neuropathological changes in clinically defined cases. Brain 118, 577–595 (1995).
Hadden, R. D. et al. Electrophysiological classification of Guillain–Barré syndrome: clinical associations and outcome. Plasma Exchange/Sandoglobulin Guillain–Barré Syndrome Trial Group. Ann. Neurol. 44, 780–788 (1998).
Kuwabara, S. & Yuki, N. Axonal Guillain–Barré syndrome: concepts and controversies. Lancet Neurol. 12, 1180–1188 (2013).
Van der Meché, F. G., Van Doorn, P. A., Meulstee, J., Jennekens, F. G. & GBS-consensus group of the Dutch Neuromuscular Research Support Centre. Diagnostic and classification criteria for the Guillain–Barré syndrome. Eur. Neurol. 45, 133–139 (2001).
Mori, M. & Kuwabara, S. Fisher syndrome. Curr. Treat. Options Neurol. 13, 71–78 (2011).
Mori, M., Kuwabara, S. & Yuki, N. Fisher syndrome: clinical features, immunopathogenesis and management. Expert Rev. Neurother. 12, 39–51 (2012).
Hughes, R. A. et al. Immunotherapy for Guillain–Barré syndrome: a systematic review. Brain 130, 2245–2257 (2007).
Hughes, R. A., Swan A. V. & van Doorn, P. A. Intravenous immunoglobulin for Guillain–Barré syndrome. Cochrane Database of Systematic Reviews, Issue 12. Art. No.: CD002063. http://dx.doi.org/10.1002/14651858.CD002063.pub5.
Raphael, J. C., Chevret, S., Hughes, R. A. & Annane, D. Plasma exchange for Guillain–Barré syndrome. Cochrane Database of Systematic Reviews, Issue 7. Art. No.: CD001798. http://dx.doi.org/10.1002/14651858.CD001798.pub2.
Hughes, R. A., Pritchard, J. & Hadden, R. D. Pharmacological treatment other than corticosteroids, intravenous immunoglobulin and plasma exchange for Guillain–Barré syndrome. Cochrane Database of Systematic Reviews, Issue 2. Art. No.: CD008630. http://dx.doi.org/10.1002/14651858.CD008630.pub3.
Hughes, R. A. & van Doorn, P. A. Corticosteroids for Guillain–Barré syndrome. Cochrane Database of Systematic Reviews, Issue 8. Art. No.: CD001446. http://dx.doi.org/10.1002/14651858.CD001446.pub4.
Sejvar, J. J., Baughman, A. L., Wise, M. & Morgan, O. W. Population incidence of Guillain–Barré syndrome: a systematic review and meta-analysis. Neuroepidemiology 36, 123–133 (2011).
Islam, Z. et al. High incidence of Guillain–Barré syndrome in children, Bangladesh. Emerg. Infect. Dis. 17, 1317–1318 (2011).
McGrogan, A., Madle, G. C., Seaman, H. E. & de Vries, C. S. The epidemiology of Guillain–Barré syndrome worldwide. A systematic literature review. Neuroepidemiology 32, 150–163 (2009).
Rocha, M. S., Brucki, S. M., Carvalho, A. A. & Lima, U. W. Epidemiologic features of Guillain–Barré syndrome in São Paulo, Brazil. Arq. Neuropsiquiatr. 62, 33–37 (2004).
van Koningsveld, R. et al. Gastroenteritis-associated Guillain–Barré syndrome on the Caribbean island Curaçao. Neurology 56, 1467–1472 (2001).
McKhann, G. M. et al. Clinical and electrophysiological aspects of acute paralytic disease of children and young adults in northern China. Lancet 338, 593–597 (1991).
Hiraga, A. et al. Recovery patterns and long term prognosis for axonal Guillain–Barré syndrome. J. Neurol. Neurosurg. Psychiatry 76, 719–722 (2005).
Ho, T. W. et al. Guillain–Barré syndrome in northern China. Relationship to Campylobacter jejuni infection and anti-glycolipid antibodies. Brain 118, 597–605 (1995).
Islam, Z. et al. Axonal variant of Guillain–Barré syndrome associated with Campylobacter infection in Bangladesh. Neurology 74, 581–587 (2010).
Geleijns, K. et al. Mannose-binding lectin contributes to the severity of Guillain–Barré syndrome. J. Immunol. 177, 4211–4217 (2006).
Sang, D. et al. Fc receptor like 3 in Chinese patients of Han nationality with Guillain–Barré syndrome. J. Neuroimmunol. 246, 65–68 (2012).
Jacobs, B. C. et al. The spectrum of antecedent infections in Guillain–Barré syndrome: a case–control study. Neurology 51, 1110–1115 (1998).
Hadden, R. D. et al. Preceding infections, immune factors, and outcome in Guillain–Barré syndrome. Neurology 56, 758–765 (2001).
van den Berg, B. et al. Guillain–Barré syndrome associated with preceding hepatitis E virus infection. Neurology 82, 491–497 (2014).
Geurtsvankessel, C. H. et al. Hepatitis E and Guillain–Barré syndrome. Clin. Infect. Dis. 57, 1369–1370 (2013).
Tam, C. C. et al. Incidence of Guillain–Barré syndrome among patients with Campylobacter infection: a general practice research database study. J. Infect. Dis. 194, 95–97 (2006).
Nachamkin, I., Allos, B. M. & Ho, T. Campylobacter species and Guillain–Barré syndrome. Clin. Microbiol. Rev. 11, 555–567 (1998).
Jackson, B. R. et al. Binational outbreak of Guillain–Barré syndrome associated with Campylobacter jejuni infection, Mexico and USA, 2011. Epidemiol. Infect. 142, 1089–1099 (2014).
Ang, C. W. et al. Structure of Campylobacter jejuni lipopolysaccharides determines antiganglioside specificity and clinical features of Guillain–Barré and Miller Fisher patients. Infect. Immun. 70, 1202–1208 (2002).
Kuijf, M. L. et al. TLR4-mediated sensing of Campylobacter jejuni by dendritic cells is determined by sialylation. J. Immunol. 185, 748–755 (2010).
Ang, C. W. et al. A case of Guillain–Barré syndrome following a family outbreak of Campylobacter jejuni enteritis. J. Neuroimmunol. 111, 229–233 (2000).
Willison, H. J. & Yuki, N. Peripheral neuropathies and anti-glycolipid antibodies. Brain 125, 2591–2625 (2002).
Kaida, K. & Kusunoki, S. Antibodies to gangliosides and ganglioside complexes in Guillain–Barré syndrome and Fisher syndrome: mini-review. J. Neuroimmunol. 223, 5–12 (2010).
Yuki, N. Guillain–Barré syndrome and anti-ganglioside antibodies: a clinician–scientist's journey. Proc. Jpn Acad. Ser. B Phys. Biol. Sci. 88, 299–326 (2012).
Gilbert, M. et al. The genetic bases for the variation in the lipo-oligosaccharide of the mucosal pathogen, Campylobacter jejuni. Biosynthesis of sialylated ganglioside mimics in the core oligosaccharide. J. Biol. Chem. 277, 327–337 (2002).
van Belkum, A. et al. A Campylobacter jejuni gene associated with immune-mediated neuropathy. Nat. Med. 7, 752–753 (2001).
Godschalk, P. C. et al. Structural characterization of Campylobacter jejuni lipooligosaccharide outer cores associated with Guillain–Barré and Miller Fisher syndromes. Infect. Immun. 75, 1245–1254 (2007).
Kusunoki, S., Kaida, K. & Ueda, M. Antibodies against gangliosides and ganglioside complexes in Guillain–Barré syndrome: new aspects of research. Biochim. Biophys. Acta 1780, 441–444 (2008).
Drenthen, J. et al. Guillain–Barré syndrome subtypes related to Campylobacter infection. J. Neurol. Neurosurg. Psychiatry 82, 300–305 (2011).
Ogawara, K. et al. Axonal Guillain–Barré syndrome: relation to anti-ganglioside antibodies and Campylobacter jejuni infection in Japan. Ann. Neurol. 48, 624–631 (2000).
Visser, L. H. et al. Guillain–Barré syndrome without sensory loss (acute motor neuropathy). A subgroup with specific clinical, electrodiagnostic and laboratory features. Dutch Guillain–Barré Study Group. Brain 118, 841–847 (1995).
Yuki, N. et al. Autoantibodies to GM1b and GalNAc-GD1a: relationship to Campylobacter jejuni infection and acute motor axonal neuropathy in China. J. Neurol. Sci. 164, 134–138 (1999).
Chiba, A., Kusunoki, S., Shimizu, T. & Kanazawa, I. Serum IgG antibody to ganglioside GQ1b is a possible marker of Miller Fisher syndrome. Ann. Neurol. 31, 677–679 (1992).
Yuki, N. Fisher syndrome and Bickerstaff brainstem encephalitis (Fisher–Bickerstaff syndrome). J. Neuroimmunol. 215, 1–9 (2009).
Jacobs, B. C., van Doorn, P. A., Groeneveld, J. H., Tio-Gillen A. P. & van der Meché, F. G. Cytomegalovirus infections and anti-GM2 antibodies in Guillain–Barré syndrome. J. Neurol. Neurosurg. Psychiatry 62, 641–643 (1997).
Kaida, K. et al. Ganglioside complexes as new target antigens in Guillain–Barré syndrome. Ann. Neurol. 56, 567–571 (2004).
Rinaldi, S. Update on Guillain–Barré syndrome. J. Peripher. Nerv. Syst. 18, 99–112 (2013).
Rinaldi, S. et al. Antibodies to heteromeric glycolipid complexes in Guillain–Barré syndrome. PLoS ONE 8, e82337 (2013).
Hakomori, S. I. The glycosynapse. Proc. Natl Acad. Sci. USA 99, 225–232 (2002).
Kuijf, M. L. et al. Origin of ganglioside complex antibodies in Guillain–Barré syndrome. J. Neuroimmunol. 188, 69–73 (2007).
Hafer-Macko, C. et al. Acute motor axonal neuropathy: an antibody-mediated attack on axolemma. Ann. Neurol. 40, 635–644 (1996).
Willison, H. J. The immunobiology of Guillain–Barré syndromes. J. Peripher. Nerv. Syst. 10, 94–112 (2005).
McGonigal, R. et al. Anti-GD1a antibodies activate complement and calpain to injure distal motor nodes of Ranvier in mice. Brain 133, 1944–1960 (2010).
Susuki, K. et al. Anti-GM1 antibodies cause complement-mediated disruption of sodium channel clusters in peripheral motor nerve fibers. J. Neurosci. 27, 3956–3967 (2007).
Susuki, K. et al. Dysfunction of nodes of Ranvier: a mechanism for anti-ganglioside antibody-mediated neuropathies. Exp. Neurol. 233, 534–542 (2012).
Halstead, S. K. et al. Eculizumab prevents anti-ganglioside antibody-mediated neuropathy in a murine model. Brain 131, 1197–1208 (2008).
Kuitwaard, K., van Koningsveld, R., Ruts, L., Jacobs, B. C. & van Doorn, P. A. Recurrent Guillain–Barré syndrome. J. Neurol. Neurosurg. Psychiatry 80, 56–59 (2009).
Huizinga, R. et al. Sialylation of Campylobacter jejuni endotoxin promotes dendritic cell-mediated B cell responses through CD14-dependent production of IFN-β and TNF-α. J. Immunol. 191, 5636–5645 (2013).
Heikema, A. P. et al. Siglec-7 specifically recognizes Campylobacter jejuni strains associated with oculomotor weakness in Guillain–Barré syndrome and Miller Fisher syndrome. Clin. Microbiol. Infect. 19, E106–E112 (2013).
Wu, L. Y., Zhou, Y., Qin, C. & Hu, B. L. The effect of TNF-α, FcγR and CD1 polymorphisms on Guillain–Barré syndrome risk: evidences from a meta-analysis. J. Neuroimmunol. 243, 18–24 (2012).
Schonberger, L. B. et al. Guillain–Barré syndrome following vaccination in the National Influenza Immunization Program, United States, 1976--1977. Am. J. Epidemiol. 110, 105–123 (1979).
Salmon, D. A. et al. Association between Guillain–Barré syndrome and influenza A (H1N1) 2009 monovalent inactivated vaccines in the USA: a meta-analysis. Lancet 381, 1461–1468 (2013).
Poland, G. A., Jacobsen, S. J. Influenza vaccine, Guillain–Barré syndrome, and chasing zero. Vaccine 30, 5801–5803 (2012).
Kuitwaard, K., Bos-Eyssen, M. E., Blomkwist-Markens, P. H. & van Doorn, P. A. Recurrences, vaccinations and long-term symptoms in GBS and CIDP. J. Peripher. Nerv. Syst. 14, 310–315 (2009).
Vereniging Spierziekten Nederland, Nederlandse Vereniging voor Neurologie, Nederlandse Vereniging van Revalidatieartsen. Multidisciplinaire richtlijn Guillain–Barré syndroom [online]. (2010).
Asbury, A. K. Diagnostic considerations in Guillain–Barré syndrome. Ann. Neurol. 9 (Suppl.), 1–5 (1981).
Sejvar, J. J. et al. Guillain–Barré syndrome and Fisher syndrome: case definitions and guidelines for collection, analysis, and presentation of immunization safety data. Vaccine 29, 599–612 (2011).
Fokke, C. et al. Diagnosis of Guillain–Barré syndrome and validation of Brighton criteria. Brain 137, 33–43 (2014).
Choe, Y. J., Cho, H., Bae, G. R., Lee, J. K. Guillain–Barré syndrome following receipt of influenza A (H1N1) 2009 monovalent vaccine in Korea with an emphasis on Brighton Collaboration case definition. Vaccine 29, 2066–2070 (2011).
Mateen, F. J. et al. Guillain–Barré syndrome in India: population-based validation of the Brighton criteria. Vaccine 29, 9697–9701 (2011).
Moulin, D. E., Hagen, N., Feasby, T. E., Amireh, R. & Hahn, A. Pain in Guillain–Barré syndrome. Neurology 48, 328–331 (1997).
Ruts, L. et al. Pain in Guillain–Barré syndrome: a long-term follow-up study. Neurology 75, 1439–1447 (2010).
Winer, J. B., Hughes, R. A., Osmond, C. A prospective study of acute idiopathic neuropathy. I. Clinical features and their prognostic value. J. Neurol. Neurosurg. Psychiatry 51, 605–612 (1988).
van Koningsveld, R. et al. Effect of methylprednisolone when added to standard treatment with intravenous immunoglobulin for Guillain–Barré syndrome: randomised trial. Lancet 363, 192–196 (2004).
[No authors listed] Randomised trial of plasma exchange, intravenous immunoglobulin, and combined treatments in Guillain–Barré syndrome. Plasma Exchange/Sandoglobulin Guillain–Barré Syndrome Trial Group. Lancet 349, 225–230 (1997).
Samadi, M., Kazemi, B., Golzari Oskoui, S. & Barzegar, M. Assessment of autonomic dysfunction in childhood Guillain–Barré syndrome. J. Cardiovasc. Thorac. Res. 5, 81–85 (2013).
Hughes, R. et al. Subacute idiopathic demyelinating polyradiculoneuropathy. Arch. Neurol. 49, 612–616 (1992).
Kuwabara, S. et al. Two patterns of clinical recovery in Guillain–Barré syndrome with IgG anti-GM1 antibody. Neurology 51, 1656–1660 (1998).
Winer, J. B. Guillain–Barré syndrome: clinical variants and their pathogenesis. J. Neuroimmunol. 231, 70–72 (2011).
Drenthen, J. et al. Limb motor nerve dysfunction in Miller Fisher syndrome. J. Peripher. Nerv. Syst. 18, 25–29 (2013).
Wakerley, B. R. & Yuki, N. Pharyngeal–cervical–brachial variant of Guillain–Barré syndrome. J. Neurol. Neurosurg. Psychiatry 85, 339–344 (2014).
Yuki, N. et al. Guillain–Barré syndrome associated with normal or exaggerated tendon reflexes. J. Neurol. 259, 1181–1190 (2012).
van Doorn, P. A. Diagnosis, treatment and prognosis of Guillain–Barré syndrome (GBS). Presse Med. 42, e193–e201 (2013).
Vucic, S., Cairns, K. D., Black, K. R., Chong, P. S. & Cros, D. Neurophysiologic findings in early acute inflammatory demyelinating polyradiculoneuropathy. Clin. Neurophysiol. 115, 2329–2335 (2004).
Capasso, M. et al. Acute motor conduction block neuropathy. Another Guillain–Barré syndrome variant. Neurology 61, 617–622 (2003).
Kuwabara, S. et al. IgG anti-GM1 antibody is associated with reversible conduction failure and axonal degeneration in Guillain–Barré syndrome. Ann. Neurol. 44, 202–208 (1998).
Uncini, A., Manzoli, C., Notturno, F., Capasso, M. Pitfalls in electrodiagnosis of Guillain–Barré syndrome subtypes. J. Neurol. Neurosurg. Psychiatry 81, 1157–1163 (2010).
Kokubun, N. et al. Conduction block in acute motor axonal neuropathy. Brain 133, 2897–2908 (2010).
Kokubun, N., Shahrizaila, N., Koga, M., Hirata, K. & Yuki, N. The demyelination neurophysiological criteria can be misleading in Campylobacter jejuni-related Guillain–Barré syndrome. Clin. Neurophysiol. 124, 1671–1679 (2013).
Uncini, A. & Kuwabara, S. Electrodiagnostic criteria for Guillain–Barré syndrome: a critical revision and the need for an update. Clin. Neurophysiol. 123, 1487–1495 (2012).
Kuijf, M. L. et al. Diagnostic value of anti-GM1 ganglioside serology and validation of the INCAT-ELISA. J. Neurol. Sci. 239, 37–44 (2005).
Parry, G. J. Guillain–Barré Syndrome 42–55 (Thieme Medical Publishers, 1993).
Hughes, R. A. Guillain–Barré Syndrome 124–130 (Springer-Verlag, 1990).
Ropper, A. H., Wijdicks, E. F., Truax, B. T. Guillain–Barré Syndrome 175–224 (F. A. Davis, 1991).
Gorson, K. C., Ropper, A. H., Muriello, M. A. & Blair, R. Prospective evaluation of MRI lumbosacral nerve root enhancement in acute Guillain–Barré syndrome. Neurology 47, 813–817 (1996).
Devos, D. et al. Guillain–Barré syndrome during childhood: particular clinical and electrophysiological features. Muscle Nerve 48, 247–251 (2013).
Korinthenberg, R., Schessl, J. & Kirschner, J. Clinical presentation and course of childhood Guillain–Barré syndrome: a prospective multicentre study. Neuropediatrics 38, 10–17 (2007).
Roodbol, J. et al. Recognizing Guillain–Barré syndrome in preschool children. Neurology 76, 807–810 (2011).
Ryan, M. M. Guillain–Barré syndrome in childhood. J. Paediatr. Child Health 41, 237–241 (2005).
de Wit, M. C., Roodbol, J., de Hoog, M., Catsman-Berrevoets, C. E. & Jacobs, B. C. Imminent respiratory insufficiency in children resulting from Guillain–Barré syndrome [Dutch]. Ned. Tijdschr. Geneeskd. 155, A3808 (2011).
Hughes, R. A., Newsom-Davis, J. M., Perkin, G. D. & Pierce, J. M. Controlled trial prednisolone in acute polyneuropathy. Lancet 2, 750–753 (1978).
Vanhoutte, E. K., Faber, C. G., Merkies, I. S. & PeriNomS study group. 196th ENMC international workshop: outcome measures in inflammatory peripheral neuropathies 8–10 February 2013, Naarden, The Netherlands. Neuromuscul. Disord. 23, 924–933 (2013).
van Nes, S. I. et al. Rasch-built Overall Disability Scale (R-ODS) for immune-mediated peripheral neuropathies. Neurology 76, 337–345 (2011).
Kleyweg, R. P., van der Meché, F. G. & Schmitz, P. I. Interobserver agreement in the assessment of muscle strength and functional abilities in Guillain–Barré syndrome. Muscle Nerve 14, 1103–1109 (1991).
Vanhoutte, E. K. et al. Modifying the Medical Research Council grading system through Rasch analyses. Brain 135, 1639–1649 (2012).
Dalakas, M. C. The use of intravenous immunoglobulin in the treatment of autoimmune neuromuscular diseases: evidence-based indications and safety profile. Pharmacol. Ther. 102, 177–193 (2004).
Fokkink, W. J. et al. IgG Fc N-glycosylation in Guillain–Barré syndrome treated with immunoglobulins. J. Proteome Res. 13, 1722–1730 (2014).
[No authors listed] Plasmapheresis and acute Guillain–Barré syndrome. The Guillain–Barré syndrome Study Group. Neurology 35, 1096–1104 (1985).
[No authors listed] Efficiency of plasma exchange in Guillain–Barré syndrome: role of replacement fluids. French Cooperative Group on Plasma Exchange in Guillain–Barré syndrome. Ann. Neurol. 22, 753–761 (1987).
[No authors listed] Appropriate number of plasma exchanges in Guillain–Barré syndrome. The French Cooperative Group on Plasma Exchange in Guillain–Barré Syndrome. Ann. Neurol. 41, 298–306 (1997).
van der Meché, F. G. & Schmitz, P. I. A randomized trial comparing intravenous immune globulin and plasma exchange in Guillain–Barré syndrome. Dutch Guillain–Barré Study Group. N. Engl. J. Med. 326, 1123–1129 (1992).
Korinthenberg, R., Schessl, J., Kirschner, J. & Monting, J. S. Intravenously administered immunoglobulin in the treatment of childhood Guillain–Barré syndrome: a randomized trial. Pediatrics 116, 8–14 (2005).
Gajjar, M. D. et al. Efficacy and cost effectiveness of therapeutic plasma exchange in patient of Guillain–Barré syndrome—a prospective study. Southeast Asian J. Case Rep. Rev. 2, 218–228 (2013).
Winters, J. L., Brown, D., Hazard, E., Chainani, A. & Andrzejewski, C. Jr. Cost-minimization analysis of the direct costs of TPE and IVIg in the treatment of Guillain–Barré syndrome. BMC Health Serv. Res. 11, 101 (2011).
Dada, M. A. & Kaplan, A. A. Plasmapheresis treatment in Guillain–Barré syndrome: potential benefit over IVIg in patients with axonal involvement. Ther. Apher. Dial. 8, 409–412 (2004).
Baranwal, A. K., Ravi, R. N. & Singh, R. Exchange transfusion: a low-cost alternative for severe childhood Guillain–Barré syndrome. J. Child Neurol. 21, 960–965 (2006).
Meena, A. K., Khadilkar, S. V. & Murthy, J. M. Treatment guidelines for Guillain–Barré syndrome. Ann. Indian Acad. Neurol. 14 (Suppl. 1), S73–S81 (2011).
Netto, A. B. et al. A comparison of immunomodulation therapies in mechanically ventilated patients with Guillain Barré syndrome. J. Clin. Neurosci. 19, 1664–1667 (2012).
Tharakan, J., Jayaprakash, P. A. & Iyer, V. P. Small volume plasma exchange in Guillain–Barré syndrome: experience in 25 patients. J. Assoc. Physicians India 38, 550–553 (1990).
Garssen, M. P. et al. Treatment of Guillain–Barré syndrome with mycophenolate mofetil: a pilot study. J. Neurol. Neurosurg. Psychiatry 78, 1012–1013 (2007).
Overell, J. R., Hsieh, S. T., Odaka, M., Yuki, N. & Willison, H. J. Treatment for Fisher syndrome, Bickerstaff's brainstem encephalitis and related disorders. Cochrane Database of Systematic Reviews, Issue 1. Art. No.: CD004761. http://dx.doi.org/10.1002/14651858.CD004761.pub2.
Mori, M., Kuwabara, S., Fukutake, T. & Hattori, T. Intravenous immunoglobulin therapy for Miller Fisher syndrome. Neurology 68, 1144–1146 (2007).
Hughes, R. A. et al. Supportive care for patients with Guillain–Barré syndrome. Arch. Neurol. 62, 1194–1198 (2005).
Bos Eyssen, M. E. et al. Selective digestive tract decontamination decreases time on ventilator in Guillain–Barré syndrome. Neurocrit. Care 15, 128–133 (2011).
Ruts, L., Drenthen, J., Jacobs, B. C., van Doorn, P. A. & Dutch GBS Study Group. Distinguishing acute-onset CIDP from fluctuating Guillain–Barré syndrome: a prospective study. Neurology 74, 1680–1686 (2010).
Kleyweg, R. P. & van der Meché, F. G. Treatment related fluctuations in Guillain–Barré syndrome after high-dose immunoglobulins or plasma-exchange. J. Neurol. Neurosurg. Psychiatry 54, 957–960 (1991).
Dionne, A., Nicolle, M. W. & Hahn, A. F. Clinical and electrophysiological parameters distinguishing acute-onset chronic inflammatory demyelinating polyneuropathy from acute inflammatory demyelinating polyneuropathy. Muscle Nerve 41, 202–207 (2010).
Bernsen, R. A., de Jager, A. E., Schmitz, P. I. & van der Meché, F. G. Residual physical outcome and daily living 3 to 6 years after Guillain–Barré syndrome. Neurology 53, 409–410 (1999).
Bernsen, R. A., Jacobs, H. M., de Jager, A. E. & van der Meché, F. G. Residual health status after Guillain–Barré syndrome. J. Neurol. Neurosurg. Psychiatry 62, 637–640 (1997).
Bersano, A. et al. Long term disability and social status change after Guillain–Barré syndrome. J. Neurol. 253, 214–218 (2006).
Garssen, M. P. et al. Physical training and fatigue, fitness, and quality of life in Guillain–Barré syndrome and CIDP. Neurology 63, 2393–2395 (2004).
Merkies, I. S. & Faber, C. G. Fatigue in immune-mediated neuropathies. Neuromuscul. Disord. 22 (Suppl. 3), S203–S207 (2012).
Merkies, I. S., Schmitz, P. I., Samijn, J. P., van der Meché, F. G. & van Doorn, P. A. Fatigue in immune-mediated polyneuropathies. European Inflammatory Neuropathy Cause and Treatment (INCAT) Group. Neurology 53, 1648–1654 (1999).
Dornonville de la Cour, C. & Jakobsen, J. Residual neuropathy in long-term population-based follow-up of Guillain–Barré syndrome. Neurology 64, 246–253 (2005).
Dhar, R., Stitt, L. & Hahn, A. F. The morbidity and outcome of patients with Guillain–Barré syndrome admitted to the intensive care unit. J. Neurol. Sci. 264, 121–128 (2008).
Fletcher, D. D., Lawn, N. D., Wolter, T. D. & Wijdicks, E. F. Long-term outcome in patients with Guillain–Barré syndrome requiring mechanical ventilation. Neurology 54, 2311–2315 (2000).
Khan, F. & Amatya, B. Rehabilitation interventions in patients with acute demyelinating inflammatory polyneuropathy: a systematic review. Eur. J. Phys. Rehabil. Med. 48, 507–522 (2012).
Khan, F. et al. Outcomes of high- and low-intensity rehabilitation programme for persons in chronic phase after Guillain–Barré syndrome: a randomized controlled trial. J. Rehabil. Med. 43, 638–646 (2011).
van Nes, S. I. et al. Improving fatigue assessment in immune-mediated neuropathies: the modified Rasch-built fatigue severity scale. J. Peripher. Nerv. Syst. 14, 268–278 (2009).
Drenthen, J. et al. Residual fatigue in Guillain–Barré syndrome is related to axonal loss. Neurology 81, 1827–1831 (2013).
Liu, J., Wang, L. N. & McNicol, E. D. Pharmacological treatment for pain in Guillain–Barré syndrome. Cochrane Database of Systematic Reviews, Issue 10. Art. No.: CD009950. http://dx.doi.org/10.1002/14651858.CD009950.pub2.
Gorson, K. C. This disorder has some nerve: chronic pain in Guillain–Barré syndrome. Neurology 75, 1406–1407 (2010).
Pan, C. L. et al. Cutaneous innervation in Guillain–Barré syndrome: pathology and clinical correlations. Brain 126, 386–397 (2003).
Ruts, L. et al. Unmyelinated and myelinated skin nerve damage in Guillain–Barré syndrome: correlation with pain and recovery. Pain 153, 399–409 (2012).
Kalita, J., Misra, U. K., Goyal, G. & Das, M. Guillain–Barré syndrome: subtypes and predictors of outcome from India. J. Peripher. Nerv. Syst. 19, 36–43 (2014).
Samukawa, M. et al. Clinical features in Guillain–Barré syndrome with anti-Gal-C antibody. J. Neurol. Sci. 337, 55–60 (2014).
Zochodne, D. W. Autonomic involvement in Guillain–Barré syndrome: a review. Muscle Nerve 17, 1145–1155 (1994).
Sharshar, T., Chevret, S., Bourdain, F., Raphaël, J. C. & French Cooperative Group on Plasma Exchange in Guillain–Barré Syndrome. Early predictors of mechanical ventilation in Guillain–Barré syndrome. Crit. Care Med. 31, 278–283 (2003).
Durand, M. C. et al. Clinical and electrophysiological predictors of respiratory failure in Guillain–Barré syndrome: a prospective study. Lancet Neurol. 5, 1021–1028 (2006).
Walgaard, C. et al. Prediction of respiratory insufficiency in Guillain–Barré syndrome. Ann. Neurol. 67, 781–787 (2010).
IGOS GBS prognosis tool. IGOS International GBS Outcome Study [online], (2014).
Henderson, R. D., Lawn, N. D., Fletcher, D. D., McClelland, R. L. & Wijdicks, E. F. The morbidity of Guillain–Barré syndrome admitted to the intensive care unit. Neurology 60, 17–21 (2003).
Nguyen, T. N. et al. Factors predicting extubation success in patients with Guillain–Barré syndrome. Neurocrit. Care 5, 230–234 (2006).
Lawn, N. D. & Wijdicks, E. F. Tracheostomy in Guillain–Barré syndrome. Muscle Nerve 22, 1058–1062 (1999).
[No authors listed] The prognosis and main prognostic indicators of Guillain–Barré syndrome. A multicentre prospective study of 297 patients. The Italian Guillain–Barré Study Group. Brain 119, 2053–2061 (1996).
Cheng, B. C. et al. Long-term prognosis for Guillain–Barré syndrome: evaluation of prognostic factors and clinical experience of automated double filtration plasmapheresis. J. Clin. Apher. 18, 175–180 (2003).
Chio, A. et al. Guillain–Barré syndrome: a prospective, population-based incidence and outcome survey. Neurology 60, 1146–1150 (2003).
van Koningsveld, R. et al. A clinical prognostic scoring system for Guillain–Barré syndrome. Lancet Neurol. 6, 589–594 (2007).
Visser, L. H., Schmitz, P. I., Meulstee, J., van Doorn, P. A. & van der Meché, F. G. Prognostic factors of Guillain–Barré syndrome after intravenous immunoglobulin or plasma exchange. Dutch Guillain–Barré Study Group. Neurology 53, 598–604 (1999).
Rees, J. H., Soudain, S. E., Gregson, N. A. & Hughes, R. A. Campylobacter jejuni infection and Guillain–Barré syndrome. N. Engl. J. Med. 333, 1374–1379 (1995).
Walgaard, C. et al. Early recognition of poor prognosis in Guillain–Barré syndrome. Neurology 76, 968–975 (2011).
Cornblath, D. R. et al. Motor conduction studies in Guillain–Barré syndrome: description and prognostic value. Ann. Neurol. 23, 354–359 (1988).
Kuwabara, S., Mori, M., Ogawara, K., Hattori, T. & Yuki, N. Indicators of rapid clinical recovery in Guillain–Barré syndrome. J. Neurol. Neurosurg. Psychiatry 70, 560–562 (2001).
Alshekhlee, A., Hussain, Z., Sultan, B. & Katirji, B. Guillain–Barré syndrome: incidence and mortality rates in US hospitals. Neurology 70, 1608–1613 (2008).
van den Berg, B., Bunschoten, C., van Doorn, P. A. & Jacobs, B. C. Mortality in Guillain–Barré syndrome. Neurology 80, 1650–1654 (2013).
Lawn, N. D. & Wijdicks, E. F. Fatal Guillain–Barré syndrome. Neurology 52, 635–638 (1999).
US National Library of Medicine. ClinicalTrials.gov [online], (2014).
Plomp, J. J. & Willison, H. J. Pathophysiological actions of neuropathy-related anti-ganglioside antibodies at the neuromuscular junction. J. Physiol. 587, 3979–3999 (2009).
Author information
Authors and Affiliations
Contributions
B.v.d.B. and P.v.D. researched data for the article; B.v.d.B., B.J. and P.v.D. made substantial contributions to discussion of content. All authors made substantial contributions to writing, review and/or editing of the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
B.C.J. receives research support from the Netherlands Organization for Health Research and Development, Erasmus MC, Prinses Beatrix Spierfonds and the Guillain–Barré syndrome, chronic inflammatory demyelinating polyneuropathy (GBS–CIDP) Foundation International, and travel support from Baxter Biopharmaceutics. P.A.v.D. receives research support from the Prinses Beatrix Spierfonds, the GBS-CIDP Foundation International, Baxter Biopharmaceutics, Griffols and Sanquin Plasma Products. B.v.d.B., C.W., J.D. and C.F. declare no competing interests.
Supplementary information
Supplementary Figure 1
EGRIS can predict the likelihood of respiratory failure (PDF 219 kb)
Supplementary Figure 2
Modified EGOS predicts the chance of patients with GBS being unable to walk (PDF 786 kb)
Rights and permissions
About this article
Cite this article
van den Berg, B., Walgaard, C., Drenthen, J. et al. Guillain–Barré syndrome: pathogenesis, diagnosis, treatment and prognosis. Nat Rev Neurol 10, 469–482 (2014). https://doi.org/10.1038/nrneurol.2014.121
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrneurol.2014.121
This article is cited by
-
Neurologic pathologies of the vertebral spine
Skeletal Radiology (2024)
-
COVID-19-associated serum and cerebrospinal fluid cytokines in post- versus para-infectious SARS-CoV-2-related Guillain–Barré syndrome
Neurological Sciences (2024)
-
Kinesin-5 inhibition improves neural regeneration in experimental autoimmune neuritis
Journal of Neuroinflammation (2023)
-
Seroprevalence of Campylobacter jejuni infection in common subtypes of Guillain–Barre syndrome in Kashmiri population
The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2023)
-
The early clinical and laboratory predictors of GBS outcome: hospital-based study, Assiut University, Upper Egypt
The Egyptian Journal of Neurology, Psychiatry and Neurosurgery (2023)