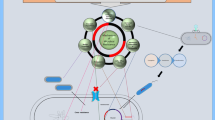
Key Points
-
Antibiotic resistance is a global health emergency.
-
Resistance mechanisms exist for all current antibiotics, and few new drugs are in development.
-
Resistance can occur via a reduction in the intracellular concentration of drug, by target site alteration or protection and by the direct inactivation of antibiotics.
-
The mobilization of resistance genes into pathogens is making the treatment of severe infections challenging owing to a lack of effective antibiotics.
-
Our understanding of the molecular mechanisms of resistance has recently increased as a result of advances in systems biology, genomics and structural biology.
-
New knowledge about antibiotic resistance should be used to inform the design of novel therapeutic agents that might not be subject to, or can circumvent, mechanisms of resistance.
Abstract
Antibiotic-resistant bacteria that are difficult or impossible to treat are becoming increasingly common and are causing a global health crisis. Antibiotic resistance is encoded by several genes, many of which can transfer between bacteria. New resistance mechanisms are constantly being described, and new genes and vectors of transmission are identified on a regular basis. This article reviews recent advances in our understanding of the mechanisms by which bacteria are either intrinsically resistant or acquire resistance to antibiotics, including the prevention of access to drug targets, changes in the structure and protection of antibiotic targets and the direct modification or inactivation of antibiotics.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Walker, D. & Fowler, T. Annual Report of the Chief Medical Officer: Volume Two, 2011: Infections and the Rise of Antimicrobial Resistance (Department of Health, 2011).
World Economic Forum. Global Risks 2013 — Eighth Edition http://www.weforum.org/reports/global-risks-2013-eighth-edition (2013).
World Economic Forum. Global Risks 2014 Report http://www.weforum.org/reports/global-risks-2014-report (2014).
World Health Organization. Antimicrobial Resistance: Global Report on Surveillance 2014 http://www.who.int/drugresistance/documents/surveillancereport/en/ (2014).
Hampton, T. Report reveals scope of US antibiotic resistance threat. JAMA 310, 1661–1663 (2013).
Chuanchuen, R., Karkhoff-Schweizer, R. R. & Schweizer, H. P. High-level triclosan resistance in Pseudomonas aeruginosa is solely a result of efflux. Am. J. Infect. Control 31, 124–127 (2003).
Zhu, L., Lin, J., Ma, J., Cronan, J. E. & Wang, H. Triclosan resistance of Pseudomonas aeruginosa PAO1 is due to FabV, a triclosan-resistant enoyl-acyl carrier protein reductase. Antimicrob. Agents Chemother. 54, 689–698 (2010).
Randall, C. P., Mariner, K. R., Chopra, I. & O'Neill, A. J. The target of daptomycin is absent from Escherichia coli and other Gram-negative pathogens. Antimicrob. Agents Chemother. 57, 637–639 (2013).
Tsuchido, T. & Takano, M. Sensitization by heat treatment of Escherichia coli K-12 cells to hydrophobic antibacterial compounds. Antimicrob. Agents Chemother. 32, 1680–1683 (1988).
Blake, K. L. & O'Neill, A. J. Transposon library screening for identification of genetic loci participating in intrinsic susceptibility and acquired resistance to antistaphylococcal agents. J. Antimicrob. Chemother. 68, 12–16 (2013).
Liu, A. et al. Antibiotic sensitivity profiles determined with an Escherichia coli gene knockout collection: generating an antibiotic bar code. Antimicrob. Agents Chemother. 54, 1393–1403 (2010).
Barbee, L. A., Soge, O. O., Holmes, K. K. & Golden, M. R. In vitro synergy testing of novel antimicrobial combination therapies against Neisseria gonorrhoeae. J. Antimicrob. Chemother. 69, 1572–1578 (2014).
Hornsey, M., Longshaw, C., Phee, L. & Wareham, D. W. In vitro activity of telavancin in combination with colistin versus Gram-negative bacterial pathogens. Antimicrob. Agents Chemother. 56, 3080–3085 (2012).
Principe, L. et al. In vitro activity of doripenem in combination with various antimicrobials against multidrug-resistant Acinetobacter baumannii: possible options for the treatment of complicated infection. Microb. Drug Resist. 19, 407–414 (2013).
Fernández, L. & Hancock, R. E. W. Adaptive and mutational resistance: role of porins and efflux pumps in drug resistance. Clin. Microbiol. Rev. 25, 661–681 (2012).
Nikaido, H. Multidrug resistance in bacteria. Annu. Rev. Biochem. 78, 119–146 (2009).
Wright, G. D. Molecular mechanisms of antibiotic resistance. Chem. Commun. 47, 4055–4061 (2011).
Kojima, S. & Nikaido, H. Permeation rates of penicillins indicate that Escherichia coli porins function principally as nonspecific channels. Proc. Natl Acad. Sci. USA 110, E2629–E2634 (2013).
Vargiu, A. V. & Nikaido, H. Multidrug binding properties of the AcrB efflux pump characterized by molecular dynamics simulations. Proc. Natl Acad. Sci. USA 109, 20637–20642 (2012).
Tran, Q. T., Williams, S., Farid, R., Erdemli, G. & Pearlstein, R. The translocation kinetics of antibiotics through porin OmpC: insights from structure-based solvation mapping using WaterMap. Proteins 81, 291–299 (2013).
Tamber, S. & Hancock, R. E. On the mechanism of solute uptake in Pseudomonas. Front. Biosci. 8, s472–s483 (2003).
Baroud, M. et al. Underlying mechanisms of carbapenem resistance in extended-spectrum β-lactamase-producing Klebsiella pneumoniae and Escherichia coli isolates at a tertiary care centre in Lebanon: role of OXA-48 and NDM-1 carbapenemases. Int. J. Antimicrob. Agents 41, 75–79 (2013).
Lavigne, J. P. et al. An adaptive response of Enterobacter aerogenes to imipenem: regulation of porin balance in clinical isolates. Int. J. Antimicrob. Agents 41, 130–136 (2013).
Poulou, A. et al. Outbreak caused by an ertapenem-resistant, CTX-M-15-producing Klebsiella pneumoniae sequence type 101 clone carrying an OmpK36 porin variant. J. Clin. Microbiol. 51, 3176–3182 (2013).
Wozniak, R. A. & Waldor, M. K. Integrative and conjugative elements: mosaic mobile genetic elements enabling dynamic lateral gene flow. Nature Rev. Microbiol. 8, 552–563 (2010).
Wozniak, A. et al. Porin alterations present in non-carbapenemase-producing Enterobacteriaceae with high and intermediate levels of carbapenem resistance in Chile. J. Med. Microbiol. 61, 1270–1279 (2012).
Novais, Â. et al. Spread of an OmpK36-modified ST15 Klebsiella pneumoniae variant during an outbreak involving multiple carbapenem-resistant Enterobacteriaceae species and clones. Eur. J. Clin. Microbiol. Infecti. Dis. 31, 3057–3063 (2012).
Tangden, T., Adler, M., Cars, O., Sandegren, L. & Lowdin, E. Frequent emergence of porin-deficient subpopulations with reduced carbapenem susceptibility in ESBL-producing Escherichia coli during exposure to ertapenem in an in vitro pharmacokinetic model. J. Antimicrob. Chemother. 68, 1319–1326 (2013).
Papagiannitsis, C. C. et al. OmpK35 and OmpK36 porin variants associated with specific sequence types of Klebsiella pneumoniae. J. Chemother. 25, 250–254 (2013).
Floyd, J. L., Smith, K. P., Kumar, S. H., Floyd, J. T. & Varela, M. F. LmrS is a multidrug efflux pump of the major facilitator superfamily from Staphylococcus aureus. Antimicrob. Agents Chemother. 54, 5406–5412 (2010).
Hu, R. M., Liao, S. T., Huang, C. C., Huang, Y. W. & Yang, T. C. An inducible fusaric acid tripartite efflux pump contributes to the fusaric acid resistance in Stenotrophomonas maltophilia. PLoS ONE 7, e51053 (2012).
Kim, C. et al. The mechanism of heterogeneous β-lactam resistance in MRSA: key role of the stringent stress response. PLoS ONE 8, e82814 (2013).
Ogawa, W., Onishi, M., Ni, R., Tsuchiya, T. & Kuroda, T. Functional study of the novel multidrug efflux pump KexD from Klebsiella pneumoniae. Gene 498, 177–182 (2012).
Dolejska, M., Villa, L., Poirel, L., Nordmann, P. & Carattoli, A. Complete sequencing of an IncHI1 plasmid encoding the carbapenemase NDM-1, the ArmA 16S RNA methylase and a resistance nodulation cell division/multidrug efflux pump. J. Antimicrob. Chemother. 68, 34–39 (2013).
Piddock, L. J. Clinically relevant chromosomally encoded multidrug resistance efflux pumps in bacteria. Clin. Microbiol. Rev. 19, 382–402 (2006).
Hinchliffe, P., Symmons, M. F., Hughes, C. & Koronakis, V. Structure and operation of bacterial tripartite pumps. Annu. Rev. Microbiol. 67, 221–242 (2013).
Ruggerone, P., Murakami, S., Pos, K. M. & Vargiu, A. V. RND efflux pumps: structural information translated into function and inhibition mechanisms. Curr. Top. Med. Chem. 13, 3079–3100 (2013).
Eicher, T. et al. Transport of drugs by the multidrug transporter AcrB involves an access and a deep binding pocket that are separated by a switch-loop. Proc. Natl Acad. Sci. USA 109, 5687–5692 (2012).
Hung, L.-W. et al. Crystal structure of AcrB complexed with linezolid at 3.5 Å resolution. J. Struct. Funct. Genom. 14, 71–75 (2013).
Murakami, S., Nakashima, R., Yamashita, E., Matsumoto, T. & Yamaguchi, A. Crystal structures of a multidrug transporter reveal a functionally rotating mechanism. Nature 443, 173–179 (2006).
Nakashima, R., Sakurai, K., Yamasaki, S., Nishino, K. & Yamaguchi, A. Structures of the multidrug exporter AcrB reveal a proximal multisite drug-binding pocket. Nature 480, 565–569 (2011).
Su, C.-C. et al. Crystal structure of the CusBA heavy-metal efflux complex of Escherichia coli. Nature 470, 558–562 (2011).
Du, D. et al. Structure of the AcrAB-TolC multidrug efflux pump. Nature 509, 512–515 (2014). This article describes the first structure based on data from a complete tripartite efflux system and determines the stoichiometry of the system and key interactions between residues.
Symmons, M. F., Bokma, E., Koronakis, E., Hughes, C. & Koronakis, V. The assembled structure of a complete tripartite bacterial multidrug efflux pump. Proc. Natl Acad. Sci. USA 106, 7173–7178 (2009).
Janganan, T. K., Bavro, V. N., Zhang, L., Borges-Walmsley, M. I. & Walmsley, A. R. Tripartite efflux pumps: energy is required for dissociation, but not assembly or opening of the outer membrane channel of the pump. Mol. Microbiol. 88, 590–602 (2013).
Janganan, T. K. et al. Evidence for the assembly of a bacterial tripartite multidrug pump with a stoichiometry of 3:6:3. J. Biol. Chem. 286, 26900–26912 (2011).
Stegmeier, J. F., Polleichtner, G., Brandes, N., Hotz, C. & Andersen, C. Importance of the adaptor (membrane fusion) protein hairpin domain for the functionality of multidrug efflux pumps. Biochemistry 45, 10303–10312 (2006).
Yum, S. et al. Crystal structure of the periplasmic component of a tripartite macrolide-specific efflux pump. J. Mol. Biol. 387, 1286–1297 (2009).
Everett, M. J., Jin, Y. F., Ricci, V. & Piddock, L. J. Contributions of individual mechanisms to fluoroquinolone resistance in 36 Escherichia coli strains isolated from humans and animals. Antimicrob. Agents Chemother. 40, 2380–2386 (1996).
Kosmidis, C. et al. Expression of multidrug resistance efflux pump genes in clinical and environmental isolates of Staphylococcus aureus. Int. J. Antimicrob. Agents 40, 204–209 (2012).
Pumbwe, L. & Piddock, L. J. V. Two efflux systems expressed simultaneously in multidrug-resistant Pseudomonas aeruginosa. Antimicrob. Agents Chemother. 44, 2861–2864 (2000).
Zalucki, Y. M., Dhulipala, V. & Shafer, W. M. Dueling regulatory properties of a transcriptional activator (MtrA) and repressor (MtrR) that control efflux pump gene expression in Neisseria gonorrhoeae. mBio 3, e00446-12 (2012).
Bailey, A. M. et al. RamA, a member of the AraC/XylS family, influences both virulence and efflux in Salmonella enterica serovar Typhimurium. J. Bacteriol. 192, 1607–1616 (2010).
Abouzeed, Y. M., Baucheron, S. & Cloeckaert, A. ramR mutations involved in efflux-mediated multidrug resistance in Salmonella enterica serovar Typhimurium. Antimicrob. Agents Chemother. 52, 2428–2434 (2008).
Alekshun, M. N. & Levy, S. B. Regulation of chromosomally mediated multiple antibiotic resistance: the mar regulon. Antimicrob. Agents Chemother. 41, 2067–2075 (1997).
Baucheron, S. et al. ramR mutations affecting fluoroquinolone susceptibility in epidemic multidrug-resistant salmonella enterica serovar kentucky ST198. Front. Microbiol. 4, 213 (2013).
Baucheron, S. et al. Bile-mediated activation of the acrAB and tolC multidrug efflux genes occurs mainly through transcriptional derepression of ramA in Salmonella enterica serovar Typhimurium. J. Antimicrob. Chemother. 69, 2400–2406 (2014).
Schindler, B. D. et al. Functional consequences of substitution mutations in MepR, a repressor of the Staphylococcus aureus mepA multidrug efflux pump gene. J. Bacteriol. 195, 3651–3662 (2013).
Pomposiello, P. J., Bennik, M. H. & Demple, B. Genome-wide transcriptional profiling of the Escherichia coli responses to superoxide stress and sodium salicylate. J. Bacteriol. 183, 3890–3902 (2001).
Kaatz, G. W., Thyagarajan, R. V. & Seo, S. M. Effect of promoter region mutations and mgrA overexpression on transcription of norA, which encodes a Staphylococcus aureus multidrug efflux transporter. Antimicrob. Agents Chemother. 49, 161–169 (2005).
Kaczmarek, F. S. et al. Genetic and molecular characterization of β-lactamase-negative ampicillin-resistant Haemophilus influenzae with unusually high resistance to ampicillin. Antimicrob. Agents Chemother. 48, 1630–1639 (2004).
Olliver, A., Vallé, M., Chaslus-Dancla, E. & Cloeckaert, A. Role of an acrR mutation in multidrug resistance of in vitro-selected fluoroquinolone-resistant mutants of Salmonella enterica serovar Typhimurium. FEMS Microbiol. Lett. 238, 267–272 (2004).
van der Straaten, T., Janssen, R., Mevius, D. J. & van Dissel, J. T. Salmonella gene rma (ramA) and multiple-drug-resistant Salmonella enterica serovar typhimurium. Antimicrob. Agents Chemother. 48, 2292–2294 (2004).
Warner, D. M., Shafer, W. M. & Jerse, A. E. Clinically relevant mutations that cause derepression of the Neisseria gonorrhoeae MtrC–MtrD–MtrE efflux pump system confer different levels of antimicrobial resistance and in vivo fitness. Mol. Microbiol. 70, 462–478 (2008).
Webber, M. A. & Piddock, L. J. V. Absence of mutations in marRAB or soxRS in acrB-overexpressing fluoroquinolone-resistant clinical and veterinary isolates of Escherichia coli. Antimicrob. Agents Chemother. 45, 1550–1552 (2001).
Webber, M. A., Talukder, A. & Piddock, L. J. V. Contribution of mutation at amino acid 45 of AcrR to acrB expression and ciprofloxacin resistance in clinical and veterinary Escherichia coli Isolates. Antimicrob. Agents Chemother. 49, 4390–4392 (2005).
Hirakawa, H., Inazumi, Y., Masaki, T., Hirata, T. & Yamaguchi, A. Indole induces the expression of multidrug exporter genes in Escherichia coli. Mol. Microbiol. 55, 1113–1126 (2005).
Nikaido, E. et al. Effects of indole on drug resistance and virulence of Salmonella enterica serovar Typhimurium revealed by genome-wide analyses. Gut Pathog. 4, 5 (2012).
Nikaido, E., Shirosaka, I., Yamaguchi, A. & Nishino, K. Regulation of the AcrAB multidrug efflux pump in Salmonella enterica serovar Typhimurium in response to indole and paraquat. Microbiology 157, 648–655 (2011).
Deng, X. et al. Expression of multidrug resistance efflux pump gene norA is iron responsive in Staphylococcus aureus. J. Bacteriol. 194, 1753–1762 (2012).
Mercante, A. D. et al. MpeR regulates the mtr efflux locus in Neisseria gonorrhoeae and modulates antimicrobial resistance by an iron-responsive mechanism. Antimicrob. Agents Chemother. 56, 1491–1501 (2012).
Wang, K. et al. The expression of ABC efflux pump, Rv1217c–Rv1218c, and its association with multidrug resistance of Mycobacterium tuberculosis in China. Curr. Microbiol. 66, 222–226 (2013).
Kumar, N. et al. Crystal structure of the transcriptional regulator Rv1219c of Mycobacterium tuberculosis. Protein Sci. 23, 423–432 (2014).
Yamasaki, S. et al. The crystal structure of multidrug-resistance regulator RamR with multiple drugs. Nature Commun. 4, 2078 (2013).
Billal, D. S., Feng, J., Leprohon, P., Legare, D. & Ouellette, M. Whole genome analysis of linezolid resistance in Streptococcus pneumoniae reveals resistance and compensatory mutations. BMC Genomics 12, 512 (2011).
Gao, W. et al. Two novel point mutations in clinical Staphylococcus aureus reduce linezolid susceptibility and switch on the stringent response to promote persistent infection. PLoS Pathog. 6, e1000944 (2010).
Leclercq, R. Mechanisms of resistance to macrolides and lincosamides: nature of the resistance elements and their clinical implications. Clin. Infect. Dis. 34, 482–492 (2002).
Unemo, M. et al. High-level cefixime- and ceftriaxone-resistant Neisseria gonorrhoeae in France: novel penA mosaic allele in a successful international clone causes treatment failure. Antimicrob. Agents Chemother. 56, 1273–1280 (2012).
Katayama, Y., Ito, T. & Hiramatsu, K. A new class of genetic element, staphylococcus cassette chromosome mec, encodes methicillin resistance in Staphylococcus aureus. Antimicrob. Agents Chemother. 44, 1549–1555 (2000).
Shore, A. C. et al. Detection of staphylococcal cassette chromosome mec type XI carrying highly divergent mecA, mecI, mecR1, blaZ, and ccr genes in human clinical isolates of clonal complex 130 methicillin-resistant Staphylococcus aureus. Antimicrob. Agents Chemother. 55, 3765–3773 (2011).
Garcia-Ãlvarez, L. et al. Meticillin-resistant Staphylococcus aureus with a novel mecA homologue in human and bovine populations in the UK and Denmark: a descriptive study. Lancet Infect. Dis. 11, 595–603 (2011). This paper reports the identification of a new allele that is undetectable by conventional diagnostic tests.
Shore, A. C. & Coleman, D. C. Staphylococcal cassette chromosome mec: recent advances and new insights. Int. J. Med. Microbiol. 303, 350–359 (2013).
Stegger, M. et al. Rapid detection, differentiation and typing of methicillin-resistant Staphylococcus aureus harbouring either mecA or the new mecA homologue mecALGA251. Clin. Microbiol. Infect. 18, 395–400 (2012).
Cartwright, E. J. P. et al. Use of vitek 2 antimicrobial susceptibility profile to identify mecC in methicillin-resistant Staphylococcus aureus. J. Clin. Microbiol. 51, 2732–2734 (2013).
Skov, R. et al. Phenotypic detection of mecC-MRSA: cefoxitin is more reliable than oxacillin. J. Antimicrob. Chemother. 69, 133–135 (2014).
Long, K. S., Poehlsgaard, J., Kehrenberg, C., Schwarz, S. & Vester, B. The Cfr rRNA methyltransferase confers resistance to Phenicols, Lincosamides, Oxazolidinones, Pleuromutilins, and Streptogramin A antibiotics. Antimicrob. Agents Chemother. 50, 2500–2505 (2006).
Shen, J., Wang, Y. & Schwarz, S. Presence and dissemination of the multiresistance gene cfr in Gram-positive and Gram-negative bacteria. J. Antimicrob. Chemother. 68, 1697–1706 (2013).
Zhang, W. J. et al. Characterization of the IncA/C plasmid pSCEC2 from Escherichia coli of swine origin that harbours the multiresistance gene cfr. J. Antimicrob. Chemother. 69, 385–389 (2014).
Fritsche, T. R., Castanheira, M., Miller, G. H., Jones, R. N. & Armstrong, E. S. Detection of methyltransferases conferring high-level resistance to aminoglycosides in Enterobacteriaceae from Europe, North America, and Latin America. Antimicrob. Agents Chemother. 52, 1843–1845 (2008).
Hidalgo, L. et al. Association of the novel aminoglycoside resistance determinant RmtF with NDM carbapenemase in Enterobacteriaceae isolated in India and the UK. J. Antimicrob. Chemother. 68, 1543–1550 (2013).
Vetting, M. W. et al. Structure of QnrB1, a plasmid-mediated fluoroquinolone resistance factor. J. Biol. Chem. 286, 25265–25273 (2011).
Cai, Y., Chai, D., Wang, R., Liang, B. & Bai, N. Colistin resistance of Acinetobacter baumannii: clinical reports, mechanisms and antimicrobial strategies. J. Antimicrob. Chemother. 67, 1607–1615 (2012).
Lim, L. M. et al. Resurgence of colistin: a review of resistance, toxicity, pharmacodynamics, and dosing. Pharmacotherapy 30, 1279–1291 (2010).
Adams, M. D. et al. Resistance to colistin in Acinetobacter baumannii associated with mutations in the PmrAB two-component system. Antimicrob. Agents Chemother. 53, 3628–3634 (2009).
Beceiro, A. et al. Phosphoethanolamine modification of lipid A in colistin-resistant variants of Acinetobacter baumannii mediated by the pmrAB two-component regulatory system. Antimicrob. Agents Chemother. 55, 3370–3379 (2011).
Fernandez, L. et al. Adaptive resistance to the “last hope” antibiotics polymyxin B and colistin in Pseudomonas aeruginosa is mediated by the novel two-component regulatory system ParR–ParS. Antimicrob. Agents Chemother. 54, 3372–3382 (2010).
Miller, A. K. et al. PhoQ mutations promote lipid A modification and polymyxin resistance of Pseudomonas aeruginosa found in colistin-treated cystic fibrosis patients. Antimicrob. Agents Chemother. 55, 5761–5769 (2011).
Cannatelli, A. et al. In vivo emergence of colistin resistance in Klebsiella pneumoniae producing KPC-type carbapenemases mediated by insertional inactivation of the PhoQ/PhoP mgrB regulator. Antimicrob. Agents Chemother. 57, 5521–5526 (2013).
Cannatelli, A. et al. MgrB inactivation is a common mechanism of colistin resistance in KPC carbapenemase-producing Klebsiella pneumoniae of clinical origin. Antimicrob. Agents Chemother. 58, 5696–5703 (2014).
Mishra, N. N. et al. Emergence of daptomycin resistance in daptomycin-naive rabbits with methicillin-resistant Staphylococcus aureus prosthetic joint infection is associated with resistance to host defense cationic peptides and mprF polymorphisms. PLoS ONE 8, e71151 (2013).
Davlieva, M., Zhang, W., Arias, C. A. & Shamoo, Y. Biochemical characterization of cardiolipin synthase mutations associated with daptomycin resistance in enterococci. Antimicrob. Agents Chemother. 57, 289–296 (2013).
Miller, C. et al. Adaptation of Enterococcus faecalis to daptomycin reveals an ordered progression to resistance. Antimicrob. Agents Chemother. 57, 5373–5383 (2013).
Diaz, L. et al. Whole-genome analyses of Enterococcus faecium isolates with diverse daptomycin MICs. Antimicrob. Agents Chemother. 58, 4527–4534 (2014).
Tran, T. T. et al. Daptomycin-resistant Enterococcus faecalis diverts the antibiotic molecule from the division septum and remodels cell membrane phospholipids. mBio 4, e00281-13 (2013). This study identifies a novel mode of daptomycin resistance in which redistribution of the target away from a key area of the cell results in resistance in enterococci.
Abraham, E. P. & Chain, E. An enzyme from bacteria able to destroy penicillin. 1940. Rev. Infect. Dis. 10, 677–678 (1988).
Livermore, D. M. Defining an extended-spectrum beta-lactamase. Clin. Microbiol. Infect. 14 (Suppl. 1), 3–10 (2008).
Nordmann, P., Poirel, L., Walsh, T. R. & Livermore, D. M. The emerging NDM carbapenemases. Trends Microbiol. 19, 588–595 (2011).
Voulgari, E., Poulou, A., Koumaki, V. & Tsakris, A. Carbapenemase-producing Enterobacteriaceae: now that the storm is finally here, how will timely detection help us fight back? Future Microbiol. 8, 27–39 (2013).
Woodford, N., Turton, J. F. & Livermore, D. M. Multiresistant Gram-negative bacteria: the role of high-risk clones in the dissemination of antibiotic resistance. FEMS Microbiol. Rev. 35, 736–755 (2011).
Johnson, A. P. & Woodford, N. Global spread of antibiotic resistance: the example of New Delhi metallo-β-lactamase (NDM)-mediated carbapenem resistance. J. Med. Microbiol. 62, 499–513 (2013).
Lynch, J. P., 3rd, Clark, N. M. & Zhanel, G. G. Evolution of antimicrobial resistance among Enterobacteriaceae (focus on extended spectrum β-lactamases and carbapenemases). Expert Opin. Pharmacother. 14, 199–210 (2013).
Rossolini, G. M., D'Andrea, M. M. & Mugnaioli, C. The spread of CTX-M-type extended-spectrum β-lactamases. Clin. Microbiol. Infect. 14 (Suppl. 1), 33–41 (2008).
Poirel, L., Bonnin, R. A. & Nordmann, P. Genetic support and diversity of acquired extended-spectrum β-lactamases in Gram-negative rods. Infect. Genet. Evol. 12, 883–893 (2012).
Zhao, W. H. & Hu, Z. Q. Epidemiology and genetics of CTX-M extended-spectrum β-lactamases in Gram-negative bacteria. Crit. Rev. Microbiol. 39, 79–101 (2013).
Dhanji, H. et al. Molecular epidemiology of fluoroquinolone-resistant ST131 Escherichia coli producing CTX-M extended-spectrum β-lactamases in nursing homes in Belfast, UK. J. Antimicrob. Chemother. 66, 297–303 (2011).
Cottell, J. L. et al. Complete sequence and molecular epidemiology of IncK epidemic plasmid encoding blaCTX-M-14. Emerg. Infect. Dis. 17, 645–652 (2011).
Cottell, J. L., Webber, M. A. & Piddock, L. J. Persistence of transferable extended-spectrum-β-lactamase resistance in the absence of antibiotic pressure. Antimicrob. Agents Chemother. 56, 4703–4706 (2012).
Dhanji, H. et al. Dissemination of pCT-like IncK plasmids harboring CTX-M-14 extended-spectrum β-lactamase among clinical Escherichia coli isolates in the United Kingdom. Antimicrob. Agents Chemother. 56, 3376–3377 (2012).
Queenan, A. M. & Bush, K. Carbapenemases: the versatile β-lactamases. Clin. Microbiol. Rev. 20, 440–458 (2007).
Queenan, A. M., Shang, W., Flamm, R. & Bush, K. Hydrolysis and inhibition profiles of β-lactamases from molecular classes A to D with doripenem, imipenem, and meropenem. Antimicrob. Agents Chemother. 54, 565–569 (2010).
Tzouvelekis, L. S., Markogiannakis, A., Psichogiou, M., Tassios, P. T. & Daikos, G. L. Carbapenemases in Klebsiella pneumoniae and other Enterobacteriaceae: an evolving crisis of global dimensions. Clin. Microbiol. Rev. 25, 682–707 (2012).
Yigit, H. et al. Novel carbapenem-hydrolyzing β-lactamase, KPC-1, from a carbapenem-resistant strain of Klebsiella pneumoniae. Antimicrob. Agents Chemother. 45, 1151–1161 (2001).
Deshpande, L. M., Jones, R. N., Fritsche, T. R. & Sader, H. S. Occurrence and characterization of carbapenemase-producing Enterobacteriaceae: report from the SENTRY Antimicrobial Surveillance Program (2000–2004). Microb. Drug Resist. 12, 223–230 (2006).
Qi, Y. et al. ST11, the dominant clone of KPC-producing Klebsiella pneumoniae in China. J. Antimicrob. Chemother. 66, 307–312 (2011).
Leavitt, A., Chmelnitsky, I., Carmeli, Y. & Navon-Venezia, S. Complete nucleotide sequence of KPC-3-encoding plasmid pKpQIL in the epidemic Klebsiella pneumoniae sequence type 258. Antimicrob. Agents Chemother. 54, 4493–4496 (2010).
Woodford, N. et al. Outbreak of Klebsiella pneumoniae producing a new carbapenem-hydrolyzing class A β-lactamase, KPC-3, in a New York Medical Center. Antimicrob. Agents Chemother. 48, 4793–4799 (2004).
Woodford, N. et al. Arrival of Klebsiella pneumoniae producing KPC carbapenemase in the United Kingdom. J. Antimicrob. Chemother. 62, 1261–1264 (2008).
Kumarasamy, K. K. et al. Emergence of a new antibiotic resistance mechanism in India, Pakistan, and the UK: a molecular, biological, and epidemiological study. Lancet Infect. Dis. 10, 597–602 (2010).
Giske, C. G. et al. Diverse sequence types of Klebsiella pneumoniae contribute to the dissemination of blaNDM-1 in India, Sweden, and the United Kingdom. Antimicrob. Agents Chemother. 56, 2735–2738 (2012).
Kumarasamy, K. & Kalyanasundaram, A. Emergence of Klebsiella pneumoniae isolate co-producing NDM-1 with KPC-2 from India. J. Antimicrob. Chemother. 67, 243–244 (2012).
Walsh, T. R., Weeks, J., Livermore, D. M. & Toleman, M. A. Dissemination of NDM-1 positive bacteria in the New Delhi environment and its implications for human health: an environmental point prevalence study. Lancet Infect. Dis. 11, 355–362 (2011).
Nordmann, P., Poirel, L., Carrer, A., Toleman, M. A. & Walsh, T. R. How to detect NDM-1 producers. J. Clin. Microbiol. 49, 718–721 (2011).
Shakil, S. et al. New Delhi metallo-β-lactamase (NDM-1): an update. J. Chemother. 23, 263–265 (2011).
Decousser, J. W. et al. Outbreak of NDM-1-producing Acinetobacter baumannii in France, January to May 2013. Euro Surveill. 18, 20547 (2013).
Wright, G. D. Bacterial resistance to antibiotics: enzymatic degradation and modification. Adv. Drug Delivery Rev. 57, 1451–1470 (2005).
Norris, A. L. & Serpersu, E. H. Ligand promiscuity through the eyes of the aminoglycoside N3 acetyltransferase IIa. Protein Sci. 22, 916–928 (2013).
Romanowska, J., Reuter, N. & Trylska, J. Comparing aminoglycoside binding sites in bacterial ribosomal RNA and aminoglycoside modifying enzymes. Proteins 81, 63–80 (2013).
Qin, S. et al. Identification of a novel genomic island conferring resistance to multiple aminoglycoside antibiotics in Campylobacter coli. Antimicrob. Agents Chemother. 56, 5332–5339 (2012).
Spanogiannopoulos, P., Waglechner, N., Koteva, K. & Wright, G. D. A rifamycin inactivating phosphotransferase family shared by environmental and pathogenic bacteria. Proc. Natl Acad. Sci. USA 111, 7102–7107 (2014).
Bowser, T. E. et al. Novel anti-infection agents: small-molecule inhibitors of bacterial transcription factors. Bioorgan Med. Chem. Lett. 17, 5652–5655 (2007).
Bhullar, K. et al. Antibiotic resistance is prevalent in an isolated cave microbiome. PLoS ONE 7, e34953 (2012).
D'Costa, V. M. et al. Antibiotic resistance is ancient. Nature 477, 457–461 (2011).
Hernandez, J. et al. Human-associated extended-spectrum β-lactamase in the Antarctic. Appl. Environ. Microbiol. 78, 2056–2058 (2012).
Decousser, J. W., Poirel, L. & Nordmann, P. Characterization of a chromosomally encoded extended-spectrum class A β-lactamase from Kluyvera cryocrescens. Antimicrob. Agents Chemother. 45, 3595–3598 (2001).
Humeniuk, C. et al. β-lactamases of Kluyvera ascorbata, probable progenitors of some plasmid-encoded CTX-M types. Antimicrob. Agents Chemother. 46, 3045–3049 (2002).
Wellington, E. M. et al. The role of the natural environment in the emergence of antibiotic resistance in Gram-negative bacteria. Lancet Infect. Dis. 13, 155–165 (2013).
D'Costa, V. M. et al. Inactivation of the lipopeptide antibiotic daptomycin by hydrolytic mechanisms. Antimicrob. Agents Chemother. 56, 757–764 (2012).
Forsberg, K. J. et al. The shared antibiotic resistome of soil bacteria and human pathogens. Science 337, 1107–1111 (2012).
Perry, J. A. & Wright, G. D. The antibiotic resistance “mobilome”: searching for the link between environment and clinic. Front. Microbiol. 4, 138 (2013).
Acknowledgements
The authors would like to acknowledge the Medical Research Council (MRC), Biotechnology and Biological Sciences Research Council (BBSRC), Royal Society, Department for Environment, Food and Rural Affairs (DEFRA) and the National Institute for Health Research (NIHR) for funding their research.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Glossary
- Enoyl-ACP reductase
-
An enzyme key in the production of fatty acids which is the target for triclosan.
- Lipopeptide
-
A natural or semi-synthetic fatty acid-linked peptide chain that targets the cell membrane (for example, daptomycin).
- Glycopeptide
-
A natural or semi-synthetic amino sugar-linked peptide chain that targets terminal D-Ala-D-Ala dipeptides (for example, vancomycin).
- β-lactams
-
An important class of antibiotics, members of which contain a β-lactam ring and inhibit peptidoglycan synthesis by covalent binding to the active-site Ser of penicillin-binding proteins. β-lactam subclasses include carbapenems, cephalosporins, penicillins, monobactams and clavams.
- Fluoroquinolones
-
Synthetic compounds that target topoisomerases. Examples include nalidixic acid and ciprofloxacin.
- Aminoglycosides
-
Natural or semi-synthetic amino sugars that target translation by binding to the 30S subunit of the ribosome. Examples include gentamicin, tobramycin, streptomycin and kanamycin.
- Extended-spectrum β-lactamases
-
(ESBLs). β-lactamase enzymes that are able to hydrolyse extended-spectrum oxyimino cephalosporins.
Rights and permissions
About this article
Cite this article
Blair, J., Webber, M., Baylay, A. et al. Molecular mechanisms of antibiotic resistance. Nat Rev Microbiol 13, 42–51 (2015). https://doi.org/10.1038/nrmicro3380
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrmicro3380
This article is cited by
-
Synthesis and characterization of cellulose derivatives for enhanced antimicrobial activity
Cellulose (2024)
-
Synthesis and antimicrobial activity of new thiomonoterpene carboxylic acids
Russian Chemical Bulletin (2024)
-
An updated review on how biochar may possess potential in soil ARGs control on aspects of source, fate and elimination
Biochar (2024)
-
Bioinspired nanomaterials for the treatment of bacterial infections
Nano Research (2024)
-
Antibacterial effects of quercetagetin are significantly enhanced upon conjugation with chitosan engineered copper oxide nanoparticles
BioMetals (2024)