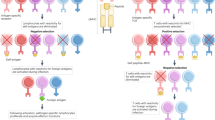
Key Points
-
Self-tolerance of T cells is commonly divided into central (thymic) and peripheral tolerance according to its site of induction. Self-tolerance to most peripheral parenchymal organs has been ascribed to peripheral tolerance. The finding that many tissue-specific genes are expressed by medullary thymic epithelial cells (mTECs) — known as promiscuous gene expression — has changed this view.
-
Tissue-specific self-antigens expressed by mTECs are functionally and structurally highly diverse and encompass essentially all organs. This allows self-antigens, which are expressed in a spatially or temporally restricted manner (such as pregnancy- or puberty-associated self-antigens) to become continuously accessible to developing T cells.
-
mTECs express self-antigens of both large and small organs at similar frequencies, therefore equating possible differences in the tolerogenic potential of organs of varying size.
-
Both genetic and epigenetic mechanisms seem to account for this unorthodox mode of gene expression.
-
Deficiencies in promiscuous gene expression can lead to organ-specific or multi-organ autoimmune syndromes.
-
Promiscuous gene expression might have co-evolved with adaptive immunity in the wake of antigen-receptor diversity early during vertebrate development.
Abstract
The thymus has been viewed as the main site of tolerance induction to self-antigens that are specifically expressed by thymic cells and abundant blood-borne self-antigens, whereas tolerance to tissue-restricted self-antigens has been ascribed to extrathymic (peripheral) tolerance mechanisms. However, the phenomenon of promiscuous expression of tissue-restricted self-antigens by medullary thymic epithelial cells has led to a reassessment of the role of central T-cell tolerance in preventing organ-specific autoimmunity. Recent evidence indicates that both genetic and epigenetic mechanisms account for this unorthodox mode of gene expression. As we discuss here, these new insights have implications for our understanding of self-tolerance in humans, its breakdown in autoimmune diseases and the significance of this tolerance mode in vertebrate evolution.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Ehrlich, P. & Morgenroth, J. II. Ueber Hämolysine. Berl. Klin. Wochenschr. 28, 251–257 (1901).
Hood, L. E., Weissman, I. L., Wood, W. B. & Wilson, J. H. Immunology. 2nd edn. (The Benjamin/Cummings Publishing Company, Inc., Palo Alto, 1978).
Klein, J. Immunology: The Science of Self-Nonself Discrimination. (John Wiley, New York, 1982).
Schwartz, R. H. & Mueller, D. L. in Fundamental Immunology 5th edn (ed. Paul, W. E.) 901–934 (Lippincott Williams & Wilkins, Philadelphia, 2003).
Medzhitov, R. & Janeway, C. A. Jr. Innate immunity, the virtues of a nonclonal system of recognition. Cell 91, 295–298 (1997).
Klein, L. & Kyewski, B. Self-antigen presentation by thymic stromal cells: a subtle division of labor. Curr. Opin. Immunol. 12, 179–186 (2000).
Alferink, J., Aigner, S., Reibke, R., Hämmerling, G. J. & Arnold, B. Peripheral T cell tolerance: the contribution of permissive T cell migration into parenchymal tissues of the neonate. Immunol. Rev. 169, 255–261 (1999).
Walker, L. S. & Abbas, A. K. The enemy within: keeping self-reactive T cells at bay in the periphery. Nature Rev. Immunol. 2, 11–19 (2002).
Derbinski, J., Schulte, A., Kyewski, B. & Klein, L. Promiscuous gene expression in medullary thymic epithelial cells mirrors the peripheral self. Nature Immunol. 2, 1032–1039 (2001).
Gotter, J., Brors, B., Hergenhahn, M. & Kyewski, B. Medullary epithelial cells of the human thymus express a highly diverse selection of tissue-specific genes co-localized in chromosomal clusters. J. Exp. Med. 199, 155–166 (2004). References 9 and 10 define and describe the phenomenon of promiscuous gene expression by purified mouse and human TEC subsets, addressing the expression pattern, scope and co-localization in chromosomal clusters of promiscuously expressed genes.
Sospedra, M. et al. Transcription of a broad range of self-antigens in human thymus suggests a role for central mechanisms in tolerance toward peripheral antigens. J. Immunol. 161, 5918–5929 (1998).
Bruno, R. et al. Multiple sclerosis candidate autoantigens except myelin oligodendrocyte glycoprotein are transcribed in human thymus. Eur. J. Immunol. 32, 2737–2747 (2002).
Bruno, R. et al. Different patterns of nicotinic acetylcholine receptor subunit transcription in human thymus. J. Neuroimmunol. 149, 147–159 (2004).
Kyewski, B., Derbinski, J., Gotter, J. & Klein, L. Promiscuous gene expression and central T-cell tolerance: more than meets the eye. Trends Immunol. 23, 364–371 (2002).
Mathis, D. & Benoist, C. Back to central tolerance. Immunity 20, 509–516 (2004).
Heid, H. W., Moll, I. & Franke, W. W. Patterns of expression of trychocytic and epithelial cytokeratins in mammalian tissue. II. Concomitant and mutually exclusive synthesis of trychocytic and epithelial cytokeratins in diverse human and bovine tissues (hair follicle, nail bed, and matrix, lingua papilla, thymic reticulum). Differentiation 37, 215–230 (1988).
Kirchner, T. et al. Pathogenesis of myasthenia gravis. Acetylcholine receptor-related antigenic determinants in tumor-free thymuses and thymic epithelial tumors. Am. J. Pathol. 130, 268–280 (1988).
Jolicoeur, C., Hanahan, D. & Smith, K. M. T-cell tolerance toward a transgenic β-cell antigen and transcription of endogenous pancreatic genes in thymus. Proc. Natl Acad. Sci. USA 91, 6707–6711 (1994). This paper shows transcription of several self-antigens of the exocrine and endocrine pancreas in the mouse thymus and for the first time promotes the notion that ectopic expression of tissue-restricted antigens is a physiological property of thymic stromal cells.
Pribyl, T. M., Campagnoni, C., Kampf, K., Handley, V. W. & Campagnoni, A. T. The major myelin protein genes are expressed in the human thymus. J. Neurosci. Res. 45, 812–819 (1996).
Geenen, V. & Lefebre, P. J. The intrathymic expression of insulin-related genes: implications for pathophysiology and prevention of type 1 diabetes. Diabetes Metab. Rev. 14, 95–110 (1998).
van Herrath, M. G., Dockter, D. & Oldstone, M. B. How virus induces a rapid or slow onset insulin-dependant diabetes mellitus in a transgenic model. Immunity 1, 231–242 (1994).
Smith, K. M., Olson, D. C., Hirose, R. & Hanahan, D. Pancreatic gene expression in rare cells of thymic medulla: evidence for functional contribution to T cell tolerance. Int. Immunol. 9, 1355–1365 (1997).
Salmon, A. M., Bruand, C., Cardona, A., Changeux, J. P. & Berrih-Aknin, S. An acetylcholine receptor α subunit promoter confers intrathymic expression in transgenic mice. Implications for tolerance of a transgenic self-antigen and for autoreactivity in myasthenia gravis. J. Clin. Invest. 101, 2340–2350 (1998).
Antonia, S. J., Geiger, T., Miller, J. & Flavell, R. A. Mechanisms of immune tolerance induction through the thymic expression of a peripheral tissue-specific protein. Int. Immunol. 7, 715–725 (1995).
Klein, L., Klein, T., Ruether, U. & Kyewski, B. CD4+ T cell tolerance to human C-reactive protein, an inducible serum protein, is mediated by medullary thymic epithelium. J. Exp. Med. 188, 5–16 (1998).
Visan, L. et al. Tolerance induction by intrathymic expressin of P0. J. Immunol. 172, 1364–1370 (2004).
Ham, D. I. et al. Central immunotolerance in transgenic mice expressing a foreign antigen under control of the rhodopsin promotor. Invest. Ophthalmol. Vis. Sci. 45, 857–862 (2004).
Matzinger, P. Tolerance, danger, and the extended family. Annu. Rev. Immunol. 12, 991–1045 (1994).
Volkmann, A., Zal, T. & Stockinger, B. Antigen-presenting cells in the thymus that can negatively select MHC class II-restricted T cells recognizing a circulating self antigen. J. Immunol. 158, 693–706 (1997).
Boehm, T., Scheu, S., Pfeffer, K. & Bleul, C. C. Thymic medullary epithelial cell differentiation, thymocyte emigration, and the control of autoimmunity require lympho–epithelial cross talk via LTβR. J. Exp. Med. 198, 757–769 (2003).
Alonso, L. & Fuchs, E. Stem cells of the skin epithelium. Proc. Natl Acad. Sci. USA 100, 11830–11835 (2003).
Booth, C. & Potten, C. S. Gut instincts: thoughts on intestinal epithelial stem cells. J. Clin. Invest. 105, 1493–1499 (2000).
Kamath, A. T., Henri, S., Battye, F., Tough, D. F. & Shortman, K. Developmental kinetics and lifespan of dendritic cells in mouse lymphoid organs. Blood 100, 1734–1741 (2002).
Farr, A. G. & Rudensky, A. Medullary thymic epithelium: a mosaic of epithelial 'self'? J. Exp. Med. 188, 1–4 (1998).
Farr, A. G., Dooley, J. L. & Erickson, M. Organization of thymic medullary epithelial heterogeneity: implications for mechanisms of epithelial differentiation. Immunol. Rev. 189, 20–27 (2002). A discussion of two competing models possibly underlying promiscuous gene expression, the differentiation model and the mosaic model. The presence of 'islands' of lung epithelium and thyroid follicles in the mouse thymic medulla are interpreted as evidence for the mosaic model.
Chin, R. K. et al. Lymphotoxin pathway directs thymic Aire expression. Nature Immunol. 4, 1121–1127 (2003). This report shows that triggering of LTβR upregulates Aire gene expression by TECs in vivo and in vitro , thereby identifying Aire as a downstream target of this signalling pathway and providing a first clue to its molecular regulation.
Chentoufi, A. A. & Polychronakos, C. Insulin expression levels in the thymus modulate insulin-specific autoreactive T-cell tolerance: the mechanism by which the IDDM2 locus may predispose to diabetes. Diabetes 51, 1383–1390 (2002).
Langbein, L. et al. Tight junction-related structures in the absence of a lumen: occluding, claudins and tight junction plaque proteins in densely packed cell formations of stratified epithelia and squamous cell carcinomas. Eur. J. Cell Biol. 82, 385–400 (2003).
Chentoufi, A. A., Palumbo, M. & Polychronakos, C. Proinsulin expression by Hassall's corpuscles in the mouse thymus. Diabetes 53, 354–359 (2004).
Pitkanen, J. & Peterson, P. Autoimmune regulator: from loss of function to autoimmunity. Genes Immun. 4, 12–21 (2003).
Anderson, M. S. et al. Projection of an immunological self-shadow within the thymus by the aire protein. Science 298, 1395–1401 (2002). This paper shows that the transcriptional regulator AIRE directs the expression of many promiscuously expressed genes and that its deletion leads to a multi-organ autoimmune syndrome similar to APS-1 in humans.
Liston, A., Lesage, S., Wilson, J., Peltonen, L. & Goodnow, C. C. Aire regulates negative selection of organ-specific T cells. Nature Immunol. 4, 350–354 (2003). These authors show that AIRE directs the expression of a neo-self antigen under the control of the rat insulin promoter in a transgenic model and that in the absence of AIRE, deletion of antigen-specific T cells is abolished.
Kumar, P. G. et al. The autoimmune regulator (Aire) is a DNA-binding protein. J. Biol. Chem. 276, 41357–41364 (2001).
Kajiura, F. et al. NF-κB-inducing kinase establishes self-tolerance in a thymic stroma-dependent manner. J. Immunol. 172, 2067–2075 (2004).
Watanabe, N. et al. Human thymic stromal lymphopoietin promotes dendritic cell-mediated CD4+ T cell homeostatic expansion. Nature Immunol. 5, 426–434 (2004).
Pugliese, A. et al. The insulin gene is transcribed in the human thymus and transcription levels correlate with allelic variation at the INS VNTR-IDDM2 susceptibility locus for type 1 diabetes. Nature Genet. 15, 293–297 (1997).
Vafiadis, P. et al. Insulin expression in human thymus is modulated by INS VNTR alleles at the IDDM2 locus. Nature Genet. 15, 289–292 (1997). References 46 and 47 describe a correlation between allelic forms of a genomic region upstream of the insulin promoter (the VNTR- IDDM2 locus), expression levels of insulin in the human thymus and susceptibility to type 1 diabetes mellitus, thereby establishing a link between intrathymic expression levels of a tissue-restricted antigen and susceptibility to organ-specific autoimmunity.
Venanzi, E., Anderson, M. S., Johnnidis, J., Benoist, C. & Mathis, D. Aire influences peripheral antigen expression and the development of autoimmunity. (Keystone Symposia, T Cell Development, 10–15 February 2004) Abstract 334 (Banff, Alberta, Canada).
Schonrich, G., Momburg, F., Hammerling, G. J. & Arnold, B. Anergy induced by thymic medullary epithelium. Eur. J. Immunol. 22, 1687–1691 (1992).
Bonomo, A. & Matzinger, P. Thymus epithelium induces tissue-specific tolerance. J. Exp. Med. 177, 1153–1164 (1993).
Hoffmann, M. W., Allison, J. & Miller, J. F. Tolerance induction by thymic epithelium. Proc. Natl Acad. Sci. USA 89, 2526–2530 (1992).
Sprent, J., Kosaka, H., Gao, E. K., Surh, C. D. & Webb, S. R. Intrathymic and extrathymic tolerance in bone marrow chimeras. Immunol. Rev. 133, 151–176 (1993).
Hoffmann, M. W., Heath, W. R., Ruschmeyer, D. & Miller, J. F. Deletion of high-avidity T cells by thymic epithelium. Proc. Natl Acad. Sci. USA 92, 9851–9855 (1995).
Avichezer, D. et al. An immunologically privileged retinal antigen elicits tolerance: major role for central selection mechanisms. J. Exp. Med. 198, 1665–1676 (2003).
Klein, L., Roettinger, B. & Kyewski, B. Sampling of complementing self-antigen pools by thymic stromal cells maximizes the scope of central T cell tolerance. Eur. J. Immunol. 31, 2476–2486 (2001).
Scollay, R. & Godfrey, D. I. Thymic emigration: conveyor belts or lucky dips? Immunol. Today 16, 268–273 (1995).
Bousso, P. & Robey, E. Dynamics of CD8+ T cell priming by dendritic cells in intact lymph nodes. Nature Immunol. 4, 579–585 (2003).
Witt, C. M. & Robey, E. Characterizing thymocyte migration in an intact thymus using two-photon laser-scanning microscopy. (Keystone Symposia, T Cell Development, 10–15 February 2004) Late abstract (Banff, Alberta, Canada).
Bleul, C. C. & Boehm, T. Chemokines define distinct microenvironments in the developing thymus. Eur. J. Immunol. 30, 3371–3379 (2000).
Annunziato, F., Romagnani, P., Cosmi, L., Lazzeri, E. & Romagnani, S. Chemokines and lymphopoiesis in human thymus. Trends Immunol. 22, 277–281 (2001).
Kwan, J. & Killeen, N. CCR7 directs the migration of thymocytes into the thymic medulla. J. Immunol. 172, 3999–4007 (2004).
Bajenoff, M., Granjeaud, S. & Guerder, S. The strategy of T cell antigen-presenting cell encounter in antigen-draining lymph nodes revealed by imaging of initial T cell activation. J. Exp. Med. 198, 715–724 (2003).
Zhang, M. et al. T cell tolerance to a neo-self antigen expressed by thymic epithelial cells: the soluble form is more effective than the membrane-bound form. J. Immunol. 170, 3954–3962 (2003). This report supports the concept of 'antigen-spreading' from mTECs to DCs by showing that a soluble form of a neo-self antigen produced by mTECs is more effective in deleting autoreactive thymocytes than a membrane-bound form.
Gallegos, A. & Bevan, M. Requirements for antigen presentation in central tolerance to tissue-specific antigens. (Keystone Symposia, T Cell Development, 10–15 February 2004) Abstract 211 (Banff, Alberta, Canada).
Muller, V. & Bonhoeffer, S. Quantitative constraints on the scope of negative selection. Trends Immunol. 24, 132–135 (2003).
Anderson, A. C. & Kuchroo, V. K. Expression of self-antigen in the thymus: a little goes a long way. J. Exp. Med. 198, 1627–1629 (2003).
Le Douarin, N. et al. Evidence for a thymus-dependent form of tolerance that is not based on elimination or anergy of reactive T cells. Immunol. Rev. 149, 35–53 (1996). This review summarizes pioneering studies in the chicken/quail model and in mice by showing that TECs confer transferable tolerance to various non-haematopoietic tissues.
Modigliani, Y., Bandeira, A. & Coutinho, A. A model for developmentally acquired thymus-dependent tolerance to central and peripheral antigens. Immunol. Rev. 149, 155–174 (1996).
Sakaguchi, S. Naturally arising CD4+ regulatory T cells for immunologic self-tolerance and negative control of immune responses. Annu. Rev. Immunol. 22, 531–562 (2004).
Bensinger, S. J., Bandeira, A., Jordan, M. S., Caton, A. J. & Laufer, T. M. Major histocompatibility complex class II-positive cortical epithelium mediates the selection of CD4+CD25+ immunoregulatory T cells. J. Exp. Med. 194, 427–438 (2001).
Jordan, M. S. et al. Thymic selection of CD4+CD25+ regulatory T cells induced by an agonist self-peptide. Nature Immunol. 2, 301–306 (2001).
Apostolou, I., Sarukhan, A., Klein, L. & von Boehmer, H. Origin of regulatory T cells with known specificity for antigen. Nature Immunol. 3, 756–763 (2002). Both studies 71 and 72 show that ectopic expression of neo-self-antigens by mTECs results in efficient intrathymic selection of antigen-specific CD4+CD25+ T Reg cells.
Ramsey, C. et al. Aire deficient mice develop multiple features of APECED phenotype and show altered immune response. Hum. Mol. Genet. 11, 397–409 (2002).
Khattri, R., Cox, T., Yasayko, S. A. & Ramsdell, F. An essential role for Scurfin in CD4+CD25+ T regulatory cells. Nature Immunol. 4, 337–342 (2003).
Fontenot, J. D., Gavin, M. A. & Rudensky, A. Y. Foxp3 programs the development and function of CD4+CD25+ regulatory T cells. Nature Immunol. 4, 330–336 (2003).
Schluesener, H. J. & Wekerle, H. Autoaggressive T lymphocyte lines recognizing the encephalitogenic region of myelin basic protein: in vitro selection from unprimed rat T lymphocyte populations. J. Immunol. 135, 3128–3133 (1985).
Fowell, D. & Mason, D. Evidence that the T cell repertoire of normal rats contains cells with the potential to cause diabetes. Characterization of the CD4+ T cell subset that inhibits this autoimmune potential. J. Exp. Med. 177, 627–636 (1993).
Wucherpfennig, K. W. et al. Clonal expansion and persistence of human T cells specific for an immunodominant myelin basic protein peptide. J. Immunol. 152, 5581–5592 (1994).
Waldmann, H. & Cobbold, S. Regulating the immune response to transplants. A role for CD4+ regulatory cells? Immunity 14, 399–406 (2001).
Vogel, A., Strassburg, C. P., Obermayer-Straub, P., Brabant, G. & Manns, M. P. The genetic background of autoimmune polyendocrinopathy-candidiasis-ectodermal dystrophy and its autoimmune disease components. J. Mol. Med. 80, 201–211 (2002).
Soderbergh, A. et al. Prevalence and clinical associations of 10 defined autoantibodies in autoimmune polyendocrine syndrome type I. J. Clin. Endocrinol. Metab. 89, 557–562 (2004).
Viglietta, V., Kent, S. C., Orban, T. & Hafler, D. A. GAD65-reactive T cells are activated in patients with autoimmune type 1a diabetes. J. Clin. Invest. 109, 895–903 (2002).
Lernmark, A. Controlling the controls: GAD65 autoreactive T cells in type 1 diabetes. J. Clin. Invest. 109, 869–870 (2002).
Baekkeskov, S., Knaani, J., Jaume, J. C. & Kash, S. Does GAD have a unique role in triggering IDDM? J. Autoimmun. 15, 279–286 (2000).
Egwuagu, C. E., Charukamnoetkanok, P. & Gery, I. Thymic expression of autoantigens correlates with resistance to autoimmune disease. J. Immunol. 159, 3109–3112 (1997). One of the first reports to show clearly in different species an inverse relationship between intrathymic expression levels of tissue-restricted self-antigens and susceptibility to experimental organ-specific autoimmune diseases.
Liu, H. et al. Mice resistant to experimental autoimmune encephalomyelitis have increased thymic expression of myelin basic protein and increased MBP specific T cell tolerance. J. Neuroimmunol. 115, 118–126 (2001).
Miyamoto, K., Miyake, S., Schachner, M. & Yamamura, T. Heterozygous null mutation of myelin P0 protein enhances susceptibility to autoimmune neuritis targeting P0 peptide. Eur. J. Immunol. 33, 656–665 (2003).
Thebault-Baumont, K. et al. Acceleration of type 1 diabetes mellitus in proinsulin 2-deficient NOD mice. J. Clin. Invest. 111, 851–857 (2003). References 87 and 88 show that a reduction in the expression level of promiscuously expressed self-antigens tilts the balance towards autoimmunity under experimental conditions.
Klein, L., Klugmann, M., Nave, K. A., Tuohy, V. K. & Kyewski, B. Shaping of the autoreactive T-cell repertoire by a splice variant of self protein expressed in thymic epithelial cells. Nature Med. 6, 56–61 (2000).
Anderson, A. C. et al. High frequency of autoreactive myelin proteolipid protein-specific T cells in the periphery of naive mice: mechanisms of selection of the self-reactive repertoire. J. Exp. Med. 191, 761–770 (2000). Both references 89 and 90 show that self-tolerance to PLP is limited to the shorter splice variant of PLP (DM20) due to its predominant expression by TECs. This finding illustrates an inherent pitfall in central tolerance by promiscuous gene expression as a consequence of differential mRNA splicing between TECs and tissue cells.
Tuohy, V. K. et al. The epitope spreading cascade during progression of experimental autoimmune encephalomyelitis and multiple sclerosis. Immunol. Rev. 164, 93–100 (1998).
Talib, S., Okarma, T. B. & Lebkowski, J. S. Differential expression of human nicotinic acetycholine receptor α subunit variants in muscle and non-muscle tissues. Nucleic Acids Res. 21, 233–237 (1993).
Diez, J. et al. Differential splicing of the IA-2 mRNA in pancreas and lymphoid organs as a permissive genetic mechanism for autoimmunity against the IA-2 type 1 diabetes autoantigen. Diabetes 50, 895–900 (2001).
Backlund, J. et al. Glycosylation of type II collagen is of major importance for T cell tolerance and pathology in collagen-induced arthritis. Eur. J. Immunol. 32, 3776–3784 (2002).
Boon, T. & Old, L. J. Cancer tumor antigens. Curr. Opin. Immunol. 9, 681–683 (1997).
Coulie, P. G. Cancer immunotherapy with MAGE antigens. Suppl. Tumori. 1, S63–S65 (2002).
Renkvist, N., Castelli, C., Robbins, P. F. & Parmiani, G. A listing of human tumor antigens recognized by T cells. Cancer Immunol. Immunother. 50, 3–15 (2001).
Diekman, A. B. et al. Anti-sperm antibodies from infertile patients and their cognate sperm antigens: a review. Identity between SAGA-1, the H6-3C4 antigen, and CD52. Am. J. Reprod. Immunol. 43, 134–143 (2000).
Bellgrau, D. & Duke, R. C. Apoptosis and CD95 ligand in immune privileged sites. Int. Rev. Immunol. 18, 547–562 (1999).
Rijnkels, M., Wheeler, D. A., de Boer, H. A. & Pieper, F. R. Structure and expression of the mouse casein locus. Mamm. Genome 8, 9–15 (1997).
Bonney, E. A. & Matzinger, P. The maternal immune system's interaction with circulating fetal cells. J. Immunol. 158, 40–47 (1997).
von Boehmer, H. et al. Thymic selection revisited: how essential is it? Immunol. Rev. 191, 62–78 (2003).
Gauwerky, C. E. & Croce, C. M. Chromosomal translocations in leukaemia. Semin. Cancer Biol. 4, 333–340 (1993).
Mills, K. D., Ferguson, D. O. & Alt, F. W. The role of DNA breaks in genomic instability and tumorigenesis. Immunol. Rev. 194, 77–95 (2003).
Muller-Hermelink, H. K. & Marx, A. Thymoma. Curr. Opin. Oncol. 12, 426–433 (2000).
Jackson-Grusby, L. et al. Loss of genomic methylation causes p53-dependent apoptosis and epigenetic deregulation. Nature Genet. 27, 31–39 (2001).
Petrie, H. T. Cell migration and the control of post-natal T-cell lymphopoiesis in the thymus. Nature Rev. Immunol. 3, 859–866 (2003).
Nelson, A. J., Hosier, S., Brady, W., Linsley, P. S. & Farr, A. G. Medullary thymic epithelium expresses a ligand for CTLA4 in situ and in vitro. J. Immunol. 151, 2453–2461 (1993).
Surh, C. D. et al. Two subsets of epithelial cells in the thymic medulla. J. Exp. Med. 176, 495–505 (1992).
Blackburn, C. C. & Manley, N. R. Developing a new paradigm for thymus organogenesis. Nature Rev. Immunol. 4, 278–289 (2004).
Humblet, C., Rudensky, A. & Kyewski, B. Presentation and intercellular transfer of self-antigen within the thymic microenvironment: expression of the Eα peptide-I-Ab complex by isolated thymic stromal cells. Int. Immunol. 6, 1949–1958 (1994).
Scheinecker, C., McHugh, R., Shevach, E. M. & Germain, R. N. Constitutive presentation of a natural tissue autoantigen exclusively by dendritic cells in the draining lymph node. J. Exp. Med. 196, 1013–1016 (2002).
Ten, S., New, M. & Maclaren, N. Clinical review 130: Addison's disease 2001. J. Clin. Endocrinol. Metab. 86, 2909–2922 (2001).
Bergman, M. P. et al. Characterization of H+/K+-ATPase T-cell epitopes in human autoimmune gastritis. Eur. J. Immunol. 33, 539–545 (2003).
Gery, L., Nussenblatt, R. B., Chan, C. C. & Caspi, R. R. in The Molecular Pathology of Autoimmune Diseases. 2nd edn (eds Theofilopoulos, A. N. & Bona, C. A.) 978 (Taylor & Francis, New York, 2002).
Vaidya, B., Kendall-Taylor, P. & Pearce, S. H. S. The Genetics of autoimmune thyroid disease. J. Clin. Endocrinol. Metab. 87, 5385–5397 (2002).
Steinman, L. Multiple sclerosis: a coordinated immunological attack against myelin in the central nervous system. Cell 85, 299–302 (1996).
Vincent, A. Unravelling the pathogenesis of myasthenia gravis. Nature Rev. Immunol. 2, 797–804 (2002).
Amagai, M., Klaus-Kovtun, V. & Stanley, J. R. Autoantibodies against a novel epithelial cadherin in pemphigus vulgaris, a disease of cell adhesion. Cell 67, 869–877 (1991).
Backlund, J. et al. Predominant selection of T cells specific for the glycosylated collagen type II epitope (263–270) in humanized transgenic mice and in rheumatoid arthritis. Proc. Natl Acad. Sci. USA 99, 9960–9965 (2002).
Tisch, R. & McDevitt, H. Insulin-dependent diabetes mellitus. Cell 85, 291–297 (1996).
Palermo, B. et al. Specific cytotoxic lymphocyte responses against MelanA/MART1, tyrosinase and gp100 in vitiligo by the use of major histocompatibility complex–peptide tetramers: the role of cellular immunity in the etiopathogenesis of vitiligo. J. Invest. Dermatol. 117, 326–332 (2001).
Mandelcorn-Monson, R. L. et al. Cytotoxic T lymphocyte reactivity to gp100, MelanA/Mart-1, and tyrosinase, in HLA-A2-positive vitiligo patients. J. Invest. Dermatol. 121, 550–556 (2003).
Acknowledgements
We would like to thank J. Gotter and B. Arnold for constructive criticism. The studies by the authors have been supported by the DKFZ, the Deutsche Forschungsgemeinschaft (J.D.) and the Mildred-Scheel Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Related links
DATABASES
Entrez Gene
OMIM
FURTHER INFORMATION
Glossary
- GENE ARRAYS
-
Tools to assess in parallel the expression profile of thousands of coding and non-coding RNAs (or even the transcriptome of whole genomes) by hybridizing labelled RNA or cDNA from cells or tissues to microarrays that contain the known antisense target sequences.
- THYMIC INVOLUTION
-
The thymus reaches its maximal relative weight at birth, the absolute weight and the rate of T-cell production increases until puberty. Then, under the influence of sex hormones, involution begins and the thymus becomes atrophic. The total size is reduced and the stromal compartment is replaced by fibrous and fat tissue. In parallel, thymic T-cell output is proportionally reduced but maintained at low levels.
- PARENCHYMAL ORGANS
-
Organs in which a specialized cell type carries out the physiological function, for example, hepatocytes in the liver, whereas the stromal tissue provides a supporting scaffold. By contrast, in lymphoid organs the stromal network has an indispensable functional role.
- HASSALL'S CORPUSCLES
-
Small clusters or concentric whorls of stratified keratinizing epithelium in the thymic medulla. They probably represent end-stage differentiated epithelial cells either participating in negative selection of thymocytes and/or undergoing apoptosis themselves.
- BI-ALLELIC EXPRESSION
-
Imprinted genes are preferentially expressed from only one allele, depending on their parental origin. Imprinting marks are established during pre-implantation development. However, in rare instances, expression from both alleles is observed in adult tissues.
- SPLIT TOLERANCE
-
Refers to the frequent experimental observations that an allogeneic tissue graft is accepted (tolerated) in vivo, yet peripheral T cells of the host react against allo-antigens of graft type in vitro.
- DOMINANT TOLERANCE
-
Refers to the suppression of an autoimmune response, in vitro or in vivo by suppressor cells including regulatory T cells. By contrast, deletion or anergy induction are referred to as recessive tolerance mechanisms. Dominant tolerance is transferable to naive recipients, whereas recessive tolerance is not.
- SCURFY MICE
-
A mouse strain with a spontaneous mutation in the forkhead box transcription factor P3 (also known as Scurfin), which leads to a rapidly fatal lymphoproliferative disease, causing death by about 4 weeks of age. Scurfin-deficient mice lack regulatory T cells.
- BYSTANDER SUPPRESSION
-
Inhibition of effector T-cell function by suppressor T cells of different antigen specificity, which presumably occurs in T-cell–antigen-presenting cell (APC) clusters, requiring the co-presentation of both antigen specificities by the same APC.
- AUTOIMMUNE POLYGLANDULAR SYNDROME TYPE 1
-
(APS-1). A rare autosomal recessive, autoimmune disorder in humans that is characterized by hypo-parathyroidism, mucocutaneous candidiasis and adrenocortical failure, and is associated with mutations in autoimmune regulator (AIRE). AIRE-deficient mice develop a similar autoimmune phenomena characterized by multi-organ lymphocytic infiltration and circulating autoantibodies.
Rights and permissions
About this article
Cite this article
Kyewski, B., Derbinski, J. Self-representation in the thymus: an extended view. Nat Rev Immunol 4, 688–698 (2004). https://doi.org/10.1038/nri1436
Issue Date:
DOI: https://doi.org/10.1038/nri1436
This article is cited by
-
miR-155 exerts posttranscriptional control of autoimmune regulator (Aire) and tissue-restricted antigen genes in medullary thymic epithelial cells
BMC Genomics (2022)
-
A guide to antigen processing and presentation
Nature Reviews Immunology (2022)
-
Transcriptome profiling of human thymic CD4+ and CD8+ T cells compared to primary peripheral T cells
BMC Genomics (2020)
-
When few survive to tell the tale: thymus and gonad as auditioning organs: historical overview
Theory in Biosciences (2020)
-
An RNA vaccine drives immunity in checkpoint-inhibitor-treated melanoma
Nature (2020)