Key Points
-
Antiviral therapies directed against HBV and HCV are universally effective in primary and secondary prevention of hepatocellular carcinoma (HCC), but are associated with substantial costs and adverse effects
-
Statin use is associated with decreased risk of HCC, potentially by inhibiting Myc activation and through inhibition of the mevalonate pathway
-
In patients with diabetes, the use of metformin might reduce the risk of HCC through mTOR inhibition, whereas insulin and insulin-secreting agents might increase the risk of HCC
-
Aspirin has also been shown to decrease risk of hepatitis-B-associated HCC in animal models, with early epidemiological studies also showing a favourable association
-
Dietary agents, such as coffee, vitamin E, fish rich in n-3 polyunsaturated fatty acids and dietary polyphenols, might also have antineoplastic effects against HCC
-
Randomized controlled trials for chemopreventive agents are logistically and ethically challenging; prospective cohort studies that adjust for relevant confounders might be well-suited to inform us about these agents
Abstract
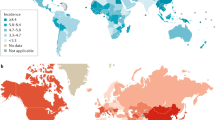
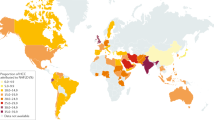
Hepatocellular carcinoma (HCC) is the third most common cause of death from cancer. The incidence and mortality of HCC are increasing in most Western countries as a result of an ageing cohort infected with chronic hepatitis C, and are expected to continue to rise as a consequence of the obesity epidemic. Chemopreventive strategies aimed at decreasing the risk or delaying the onset of HCC are needed. Universal immunization against HBV and antiviral therapy against HBV and HCV in patients with established disease has consistently been associated with reduced HCC risk, especially in patients who achieve sustained virologic response. However, the cost-effectiveness of antiviral therapy for primary HCC prevention is not known. Several commonly prescribed medications seem promising as chemopreventive agents against HCC, including statins, antidiabetic medications and aspirin. Dietary agents such as coffee, vitamin E and fish oil as well as phytochemicals might also be associated with reduced risk of HCC. Though randomized controlled trials are ideally needed to firmly establish efficacy, such chemoprevention trials are logistically and ethically challenging. Well-designed, prospective, population-based cohort studies might provide the best evidence for chemopreventive efficacy of these agents.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Jemal, A. et al. Global cancer statistics. CA Cancer J. Clin. 61, 69–90 (2011).
El-Serag, H. B. Epidemiology of viral hepatitis and hepatocellular carcinoma. Gastroenterology 142, 1264–1273 (2012).
El-Serag, H. B. & Mason, A. C. Rising incidence of hepatocellular carcinoma in the United States. N. Engl. J. Med. 340, 745–750 (1999).
El-Serag, H. B. et al. Treatment and outcomes of treating of hepatocellular carcinoma among Medicare recipients in the United States: a population-based study. J. Hepatol. 44, 158–166 (2006).
Howlader N. et al. SEER Cancer Statistics Review 1975–2010. National Cancer Institute [online], (2013).
Fattovich, G., Bortolotti, F. & Donato, F. Natural history of chronic hepatitis B: special emphasis on disease progression and prognostic factors. J. Hepatol. 48, 335–352 (2008).
Yang, J. D. et al. Cirrhosis is present in most patients with hepatitis B and hepatocellular carcinoma. Clin. Gastroenterol. Hepatol. 9, 64–70 (2011).
Yang, J. D. & Roberts, L. R. Hepatocellular carcinoma: A global view. Nat. Rev. Gastroenterol. Hepatol. 7, 448–458 (2010).
Calle, E. E., Rodriguez, C., Walker-Thurmond, K. & Thun, M. J. Overweight, obesity, and mortality from cancer in a prospectively studied cohort of U. S. adults. N. Engl. J. Med. 348, 1625–1638 (2003).
Rui, R. et al. Excess body mass index and risk of liver cancer: a nonlinear dose-response meta-analysis of prospective studies. PLoS ONE 7, e44522 (2012).
White, D. L., Kanwal, F. & El-Serag, H. B. Association between nonalcoholic fatty liver disease and risk for hepatocellular cancer, based on systematic review. Clin. Gastroenterol. Hepatol. 10, 1342–1359 (2012).
El-Serag, H. B., Hampel, H. & Javadi, F. The association between diabetes and hepatocellular carcinoma: a systematic review of epidemiologic evidence. Clin. Gastroenterol. Hepatol. 4, 369–380 (2006).
Aravalli, R. N., Steer, C. J. & Cressman, E. N. Molecular mechanisms of hepatocellular carcinoma. Hepatology 48, 2047–2063 (2008).
Arzumanyan, A., Reis, H. M. & Feitelson, M. A. Pathogenic mechanisms in HBV- and HCV-associated hepatocellular carcinoma. Nat. Rev. Cancer 13, 123–135 (2013).
Roberts, L. R. & Gores, G. J. Hepatocellular carcinoma: molecular pathways and new therapeutic targets. Semin. Liver Dis. 25, 212–225 (2005).
Villanueva, A., Newell, P., Chiang, D. Y., Friedman, S. L. & Llovet, J. M. Genomics and signaling pathways in hepatocellular carcinoma. Semin. Liver Dis. 27, 55–76 (2007).
Bhat, M., Sonenberg, N. & Gores, G. The mTOR pathway in hepatic malignancies. Hepatology http://dx.doi.org/10.1002/hep.26323.
White, B. D., Chien, A. J. & Dawson, D. W. Dysregulation of Wnt/β-catenin signaling in gastrointestinal cancers. Gastroenterology 142, 219–232 (2012).
Luo, Z., Li, L. & Ruan, B. Impact of the implementation of a vaccination strategy on hepatitis B virus infections in China over a 20-year period. Int. J. Infect. Dis. 16, e82–e88 (2012).
Chang, M. H. et al. Decreased incidence of hepatocellular carcinoma in hepatitis B vaccinees: a 20-year follow-up study. J. Natl Cancer Inst. 101, 1348–1355 (2009).
Lai, C. L. & Yuen, M. F. Prevention of hepatitis B virus-related hepatocellular carcinoma with antiviral therapy. Hepatology 57, 399–408 (2013).
Ikeda, K. et al. Interferon decreases hepatocellular carcinogenesis in patients with cirrhosis caused by the hepatitis B virus: a pilot study. Cancer 82, 827–835 (1998).
Liaw, Y. F. et al. Lamivudine for patients with chronic hepatitis B and advanced liver disease. N. Engl. J. Med. 351, 1521–1531 (2004).
Hosaka, T. et al. Long-term entecavir treatment reduces hepatocellular carcinoma incidence in patients with hepatitis B virus infection. Hepatology 58, 98–107 (2013).
Sung, J. J., Tsoi, K. K., Wong, V. W., Li, K. C. & Chan, H. L. Meta-analysis: Treatment of hepatitis B infection reduces risk of hepatocellular carcinoma. Aliment. Pharmacol. Ther. 28, 1067–1077 (2008).
Papatheodoridis, G. V., Lampertico, P., Manolakopoulos, S. & Lok, A. Incidence of hepatocellular carcinoma in chronic hepatitis B patients receiving nucleos(t)ide therapy: a systematic review. J. Hepatol. 53, 348–356 (2010).
Rein, D. B. et al. Forecasting the morbidity and mortality associated with prevalent cases of pre-cirrhotic chronic hepatitis C in the United States. Dig. Liver Dis. 43, 66–72 (2011).
Thein, H. H., Yi, Q., Dore, G. J. & Krahn, M. D. Estimation of stage-specific fibrosis progression rates in chronic hepatitis C virus infection: a meta-analysis and meta-regression. Hepatology 48, 418–431 (2008).
Yano, M. et al. The long-term pathological evolution of chronic hepatitis C. Hepatology 23, 1334–1340 (1996).
Zhang, C. H. et al. Effects of interferon treatment on development and progression of hepatocellular carcinoma in patients with chronic virus infection: a meta-analysis of randomized controlled trials. Int. J. Cancer 129, 1254–1264 (2011).
Morgan, T. R. et al. Outcome of sustained virological responders with histologically advanced chronic hepatitis C. Hepatology 52, 833–844 (2010).
Morgan, R. L. et al. Eradication of hepatitis C virus infection and the development of hepatocellular carcinoma: a meta-analysis of observational studies. Ann. Intern. Med. 158, 329–337 (2013).
Chou, R. et al. Comparative effectiveness of antiviral treatment for hepatitis C virus infection in adults: a systematic review. Ann. Intern. Med. 158, 114–123 (2013).
Dabbouseh, N. M. & Jensen, D. M. Future therapies for chronic hepatitis C. Nat. Rev. Gastroenterol. Hepatol. 10, 268–276 (2013).
Loomba, R. et al. Synergism between obesity and alcohol in increasing the risk of hepatocellular carcinoma: a prospective cohort study. Am. J. Epidemiol. 177, 333–342 (2013).
Tsan, Y. T. et al. Statins and the risk of hepatocellular carcinoma in patients with hepatitis C virus infection. J. Clin. Oncol. 31, 1514–1521 (2013).
IMS Institute for Healthcare Informatics. The Use of Medicines in the United States: Review of 2010. IMS Institute for Healthcare Informatics [online], (2011).
Demierre, M. F., Higgins, P. D., Gruber, S. B., Hawk, E. & Lippman, S. M. Statins and cancer prevention. Nat. Rev. Cancer 5, 930–942 (2005).
Singh, S., Singh, A. G., Singh, P. P., Murad, M. H. & Iyer, P. G. Statins are associated with reduced risk of esophageal cancer, particularly in patients with Barrett's esophagus: a systematic review and meta-analysis. Clin. Gastroenterol. Hepatol. 11, 620–629 (2013).
Singh, P. P. & Singh, S. Statins are associated with reduced risk of gastric cancer: a systematic review and meta-analysis. Ann. Oncol. 24, 1721–1730 (2013).
Samadder, N. J. et al. Risk of colorectal cancer in self-reported inflammatory bowel disease and modification of risk by statin and NSAID use. Cancer 117, 1640–1648 (2011).
Marcelli, M. et al. Caspase-7 is activated during lovastatin-induced apoptosis of the prostate cancer cell line LNCaP. Cancer Res. 58, 76–83 (1998).
Wu, J., Wong, W. W., Khosravi, F., Minden, M. D. & Penn, L. Z. Blocking the Raf/MEK/ERK pathway sensitizes acute myelogenous leukemia cells to lovastatin-induced apoptosis. Cancer Res. 64, 6461–6468 (2004).
Rao, S. et al. Lovastatin-mediated G1 arrest is through inhibition of the proteasome, independent of hydroxymethyl glutaryl-CoA reductase. Proc. Natl Acad. Sci. USA 96, 7797–7802 (1999).
Cao, Z. et al. MYC phosphorylation, activation, and tumorigenic potential in hepatocellular carcinoma are regulated by HMG-CoA reductase. Cancer Res. 71, 2286–2297 (2011).
Farazi, P. A. & DePinho, R. A. Hepatocellular carcinoma pathogenesis: from genes to environment. Nat. Rev. Cancer 6, 674–687 (2006).
Shachaf, C. M. et al. MYC inactivation uncovers pluripotent differentiation and tumour dormancy in hepatocellular cancer. Nature 431, 1112–1117 (2004).
El-Serag, H. B., Johnson, M. L., Hachem, C. & Morgana, R. O. Statins are associated with a reduced risk of hepatocellular carcinoma in a large cohort of patients with diabetes. Gastroenterology 136, 1601–1608 (2009).
Tsan, Y. T., Lee, C. H., Wang, J. D. & Chen, P. C. Statins and the risk of hepatocellular carcinoma in patients with hepatitis B virus infection. J. Clin. Oncol. 30, 623–630 (2012).
Chiu, H. F., Ho, S. C., Chen, C. C. & Yang, C. Y. Statin use and the risk of liver cancer: a population-based case-control study. Am. J. Gastroenterol. 106, 894–898 (2011).
Hamelin, B. A. & Turgeon, J. Hydrophilicity/lipophilicity: relevance for the pharmacology and clinical effects of HMG-CoA reductase inhibitors. Trends Pharmacol. Sci. 19, 26–37 (1998).
Emberson, J. R. et al. Lack of effect of lowering LDL cholesterol on cancer: meta-analysis of individual data from 175,000 people in 27 randomised trials of statin therapy. PLoS ONE 7, e29849 (2012).
Singh, S., Singh, P. P., Singh, A. G., Murad, M. H. & Sanchez, W. Statins are associated with a reduced risk of hepatocellular cancer: a systematic review and meta-analysis. Gastroenterology 144, 323–332 (2013).
Singh, P. P. & Singh, S. Statins and risk reduction in hepatocellular carcinoma: fact or fiction? J. Clin. Oncol. 30, 2569–2570 (2012).
Decensi, A. et al. Metformin and cancer risk in diabetic patients: a systematic review and meta-analysis. Cancer Prev. Res. (Phila) 3, 1451–1461 (2010).
Chang, C. H., Lin, J. W., Wu, L. C., Lai, M. S. & Chuang, L. M. Oral insulin secretagogues, insulin, and cancer risk in type 2 diabetes mellitus. J. Clin. Endocrinol. Metab. 97, E1170–E1175 (2012).
Zhou, G. et al. Role of AMP-activated protein kinase in mechanism of metformin action. J. Clin. Invest. 108, 1167–1174 (2001).
Chen, H. P. et al. Metformin decreases hepatocellular carcinoma risk in a dose-dependent manner: population-based and in vitro studies. Gut 62, 606–615 (2012).
Blandino, G. et al. Metformin elicits anticancer effects through the sequential modulation of DICER and c-MYC. Nat. Commun. 3, 865 (2012).
Okumura, T. Mechanisms by which thiazolidinediones induce anti-cancer effects in cancers in digestive organs. J. Gastroenterol. 45, 1097–1102 (2010).
Wu, C. W., Farrell, G. C. & Yu, J. Functional role of peroxisome-proliferator-activated receptor γ in hepatocellular carcinoma. J. Gastroenterol. Hepatol. 27, 1665–1669 (2012).
Bowker, S. L., Majumdar, S. R., Veugelers, P. & Johnson, J. A. Increased cancer-related mortality for patients with type 2 diabetes who use sulfonylureas or insulin. Diabetes Care 29, 254–258 (2006).
Ruiter, R. et al. Lower risk of cancer in patients on metformin in comparison with those on sulfonylurea derivatives: results from a large population-based follow-up study. Diabetes Care 35, 119–124 (2012).
Singh, S., Singh, P. P., Singh, A. G., Murad, M. H. & Sanchez, W. Anti-diabetic medications and the risk of hepatocellular cancer: a systematic review and meta-analysis. Am. J. Gastroenterol. 108, 881–891 (2013).
Chang, C. H. et al. Association of thiazolidinediones with liver cancer and colorectal cancer in type 2 diabetes mellitus. Hepatology 55, 1462–1472 (2012).
Kawaguchi, T. et al. Association of exogenous insulin or sulphonylurea treatment with an increased incidence of hepatoma in patients with hepatitis C virus infection. Liver Int. 30, 479–486 (2010).
Oliveria, S. A., Koro, C. E., Yood, M. U. & Sowell, M. Cancer incidence among patients treated with antidiabetic pharmacotherapy. Diabetes and Metabolic Syndrome: Clinical Research and Reviews 2, 47–57 (2008).
Hassan, M. M. et al. Association of diabetes duration and diabetes treatment with the risk of hepatocellular carcinoma. Cancer 116, 1938–1946 (2010).
Suissa, S. & Azoulay, L. Metformin and the risk of cancer: time-related biases in observational studies. Diabetes Care 35, 2665–2673 (2012).
Singh, S. & Singh, P. P. Metformin and risk of hepatocellular carcinoma: are statins the missing link? Gut 62, 951–952 (2013).
Falk, G. W. et al. A combination of esomeprazole and aspirin reduces tissue concentrations of prostaglandin E(2) in patients with Barrett's esophagus. Gastroenterology 143, 917–926 e911 (2012).
Iannacone, M. et al. Platelets mediate cytotoxic T lymphocyte-induced liver damage. Nat. Med. 11, 1167–1169 (2005).
Sitia, G. et al. Antiplatelet therapy prevents hepatocellular carcinoma and improves survival in a mouse model of chronic hepatitis B. Proc. Natl Acad. Sci. USA 109, E2165–E2172 (2012).
Thun, M. J., Jacobs, E. J. & Patrono, C. The role of aspirin in cancer prevention. Nat. Rev. Clin. Oncol. 9, 259–267 (2012).
Sahasrabuddhe, V. V. et al. Nonsteroidal anti-inflammatory drug use, chronic liver disease, and hepatocellular carcinoma. J. Natl Cancer Inst. 104, 1808–1814 (2012).
Singh, P. & Singh, S. Re: nonsteroidal antiinflammatory drug use, chronic liver disease, and hepatocellular carcinoma. J. Natl Cancer Inst. 105, 666–667 (2013).
Gelatti, U. et al. Coffee consumption reduces the risk of hepatocellular carcinoma independently of its aetiology: a case–control study. J. Hepatol. 42, 528–534 (2005).
Inoue, M., Yoshimi, I., Sobue, T. & Tsugane, S. Influence of coffee drinking on subsequent risk of hepatocellular carcinoma: a prospective study in Japan. J. Natl Cancer Inst. 97, 293–300 (2005).
Bravi, F., Bosetti, C., Tavani, A. & La Vecchia, C. Coffee drinking and hepatocellular carcinoma: an update. Hepatology 50, 1317–1318 (2009).
Bravi, F. et al. Coffee drinking and hepatocellular carcinoma risk: a meta-analysis. Hepatology 46, 430–435 (2007).
Tao, K. S. et al. The multifaceted mechanisms for coffee's anti-tumorigenic effect on liver. Med. Hypotheses 71, 730–736 (2008).
Torres, D. M. & Harrison, S. A. Is it time to write a prescription for coffee? Coffee and liver disease. Gastroenterology 144, 670–672 (2013).
Zhang, W. et al. Vitamin intake and liver cancer risk: a report from two cohort studies in China. J. Natl Cancer Inst. 104, 1173–1181 (2012).
Chalasani, N. et al. The diagnosis and management of non-alcoholic fatty liver disease: practice guideline by the American Gastroenterological Association, American Association for the Study of Liver Diseases, and American College of Gastroenterology. Gastroenterology 142, 1592–1609 (2012).
Sawada, N. et al. Consumption of n-3 fatty acids and fish reduces risk of hepatocellular carcinoma. Gastroenterology 142, 1468–1475 (2012).
Bishayee, A. et al. Dietary phytochemicals in the chemoprevention and treatment of hepatocellular carcinoma: in vivo evidence, molecular targets, and clinical relevance. Curr. Cancer Drug Targets. 12, 1191–1232 (2012).
Wogan, G. N., Kensler, T. W. & Groopman, J. D. Present and future directions of translational research on aflatoxin and hepatocellular carcinoma. A review. Food Addit. Contam. Part A Chem. Anal. Control Expo. Risk Assess. 29, 249–257 (2012).
Kensler, T. W. et al. Keap1-nrf2 signaling: a target for cancer prevention by sulforaphane. Top. Curr. Chem. 329, 163–177 (2013).
Kensler, T. W. et al. Effects of glucosinolate-rich broccoli sprouts on urinary levels of aflatoxin-DNA adducts and phenanthrene tetraols in a randomized clinical trial in He Zuo township, Qidong, People's Republic of China. Cancer Epidemiol. Biomarkers Prev. 14, 2605–2613 (2005).
Egner, P. A. et al. Chlorophyllin intervention reduces aflatoxin-DNA adducts in individuals at high risk for liver cancer. Proc. Natl Acad. Sci. USA 98, 14601–14606 (2001).
Soni, K. B., Lahiri, M., Chackradeo, P., Bhide, S. V. & Kuttan, R. Protective effect of food additives on aflatoxin-induced mutagenicity and hepatocarcinogenicity. Cancer Lett. 115, 129–133 (1997).
Anand, P., Sundaram, C., Jhurani, S., Kunnumakkara, A. B. & Aggarwal, B. B. Curcumin and cancer: an “old-age” disease with an “age-old” solution. Cancer Lett. 267, 133–164 (2008).
Bishayee, A., Politis, T. & Darvesh, A. S. Resveratrol in the chemoprevention and treatment of hepatocellular carcinoma. Cancer Treat. Rev. 36, 43–53 (2010).
Kuo, P. L., Chiang, L. C. & Lin, C. C. Resveratrol-induced apoptosis is mediated by p53-dependent pathway in Hep G2 cells. Life Sci. 72, 23–34 (2002).
Sun, Z. J., Pan, C. E., Liu, H. S. & Wang, G. J. Anti-hepatoma activity of resveratrol in vitro. World J. Gastroenterol. 8, 79–81 (2002).
Bishayee, A. & Dhir, N. Resveratrol-mediated chemoprevention of diethylnitrosamine-initiated hepatocarcinogenesis: inhibition of cell proliferation and induction of apoptosis. Chem. Biol. Interact. 179, 131–144 (2009).
Brasnyo, P. et al. Resveratrol improves insulin sensitivity, reduces oxidative stress and activates the Akt pathway in type 2 diabetic patients. Br. J. Nutr. 106, 383–389 (2011).
Poulsen, M. M. et al. High-dose resveratrol supplementation in obese men: an investigator-initiated, randomized, placebo-controlled clinical trial of substrate metabolism, insulin sensitivity, and body composition. Diabetes 62, 1186–1195 (2013).
El-Serag, H. B. Hepatocellular carcinoma. N. Engl. J. Med. 365, 1118–1127 (2011).
Wu, C. Y. et al. Association between nucleoside analogues and risk of hepatitis B virus-related hepatocellular carcinoma recurrence following liver resection. JAMA 308, 1906–1914 (2012).
Hsu, Y. C., Ho, H. J., Wu, M. S., Lin, J. T. & Wu, C. Y. Postoperative peg-interferon plus ribavirin is associated with reduced recurrence of hepatitis C virus-related hepatocellular carcinoma. Hepatology 58, 150–157 (2013).
Zhong, J. H. et al. Postoperative use of the chemopreventive vitamin K2 analog in patients with hepatocellular carcinoma. PLoS ONE 8, e58082 (2013).
Nahon, P. & Zucman-Rossi, J. Single nucleotide polymorphisms and risk of hepatocellular carcinoma in cirrhosis. J. Hepatol. 57, 663–674 (2012).
Wen, C. P. et al. Hepatocellular carcinoma risk prediction model for the general population: the predictive power of transaminases. J. Natl Cancer Inst. 104, 1599–1611 (2012).
Roncalli, M., Terracciano, L., Di Tommaso, L., David, E. & Colombo, M. Liver precancerous lesions and hepatocellular carcinoma: the histology report. Dig. Liver Dis. 43 (Suppl. 4), S361–S372 (2011).
Ghany, M. G., Strader, D. B., Thomas, D. L. & Seeff, L. B. Diagnosis, management, and treatment of hepatitis C: an update. Hepatology 49, 1335–1374 (2009).
Lok, A. S. & McMahon, B. J. Chronic hepatitis B: update 2009. Hepatology 50, 661–662 (2009).
Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults. Executive Summary of The Third Report of the National Cholesterol Education Program (NCEP) Expert Panel on Detection, Evaluation, and Treatment of High Blood Cholesterol in Adults (Adult Treatment Panel III). JAMA 285, 2486–2497 (2001).
US Preventive Services Task Force. Aspirin for the prevention of cardiovascular disease: U. S. Preventive Services Task Force recommendation statement. Ann. Intern. Med. 150, 396–404 (2009).
Acknowledgements
The work of L. R. Roberts is supported by the NIH (grant nos.: CA100882, CA128633, and CA165076), the Mayo Clinic Center for Cell Signaling in Gastroenterology (NIDDK P30DK084567), the Mayo Clinic Cancer Center (CA15083), and the Mayo Foundation.
Author information
Authors and Affiliations
Contributions
S. Singh contributed to researching data for the article, discussion of content, writing and reviewing/editing the manuscript before submission. P. P. Singh and W. Sanchez contributed to researching data, discussion of content and reviewing/editing the manuscript before submission. L. R. Roberts contributed to discussion of content, writing and reviewing/editing the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Table 1
Studies of nucleoside/nucleotide-based antiviral therapies against hepatitis B as primary prevention of hepatocellular cancer. (DOC 28 kb)
Supplementary Table 2
Studies of interferon-based therapies against hepatitis C on primary prevention of hepatocellular carcinoma (DOC 52 kb)
Supplementary Table 3
Summary of observational studies on the chemopreventive effect of statins against hepatocellular cancer in (a) at-risk patients and (b) general population (DOC 28 kb)
Supplementary Table 4
Summary of observational studies on the cancer-modifying effects of antidiabetic medications in primary prevention of hepatocellular carcinoma in patients with diabetes mellitus. (DOC 29 kb)
PowerPoint slides
Rights and permissions
About this article
Cite this article
Singh, S., Singh, P., Roberts, L. et al. Chemopreventive strategies in hepatocellular carcinoma. Nat Rev Gastroenterol Hepatol 11, 45–54 (2014). https://doi.org/10.1038/nrgastro.2013.143
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrgastro.2013.143
This article is cited by
-
Mesenchymal stem cells-based therapy in liver diseases
Molecular Biomedicine (2022)
-
Green tea-derived theabrownin induces cellular senescence and apoptosis of hepatocellular carcinoma through p53 signaling activation and bypassed JNK signaling suppression
Cancer Cell International (2022)
-
Maternal embryonic leucine zipper kinase serves as a potential prognostic marker and leads to sorafenib chemoresistance modified by miR-142-5p in hepatocellular carcinoma
Molecular Biology Reports (2022)
-
Statin use is associated with a lower risk of recurrence after curative resection in BCLC stage 0-A hepatocellular carcinoma
BMC Cancer (2021)
-
Anticancer activity of Nigerian medicinal plants: a review
Future Journal of Pharmaceutical Sciences (2021)