Abstract
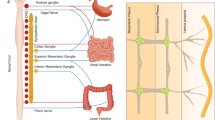
While bidirectional brain–gut interactions are well known mechanisms for the regulation of gut function in both healthy and diseased states, a role of the enteric flora—including both commensal and pathogenic organisms—in these interactions has only been recognized in the past few years. The brain can influence commensal organisms (enteric microbiota) indirectly, via changes in gastrointestinal motility and secretion, and intestinal permeability, or directly, via signaling molecules released into the gut lumen from cells in the lamina propria (enterochromaffin cells, neurons, immune cells). Communication from enteric microbiota to the host can occur via multiple mechanisms, including epithelial-cell, receptor-mediated signaling and, when intestinal permeability is increased, through direct stimulation of host cells in the lamina propria. Enterochromaffin cells are important bidirectional transducers that regulate communication between the gut lumen and the nervous system. Vagal, afferent innervation of enterochromaffin cells provides a direct pathway for enterochromaffin-cell signaling to neuronal circuits, which may have an important role in pain and immune-response modulation, control of background emotions and other homeostatic functions. Disruption of the bidirectional interactions between the enteric microbiota and the nervous system may be involved in the pathophysiology of acute and chronic gastrointestinal disease states, including functional and inflammatory bowel disorders.
Key Points
-
Bidirectional brain–gut interactions have an important role in the modulation of gastrointestinal functions, such as motility, secretion, blood flow, intestinal permeability, mucosal immune activity, and visceral sensations, including pain
-
Evidence suggests that the enteric microbiota has an important role in the above interactions
-
Brain to gut signaling can affect host–bacteria interactions in the gastrointestinal tract indirectly by increasing permeability of the intestinal epithelium, modulating the mucosal immune response and effecting changes in gastrointestinal secretion
-
Evidence supports direct communication between epithelial cells and enteric bacteria via luminal release from neurons, immune cells, Paneth cells and enterochromaffin cells of signaling molecules that can modulate microbial virulence
-
Evidence supports a communication pathway between microbes in the gut lumen and the host's central nervous system via enteric microbiota–enterochromaffin cells–vagal afferent nerves signaling
-
Bidirectional interactions between brain and enteric microbes might have an important role in modulating gut function and may be involved in the modulation of emotions, pain perception and general well-being
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Mayer, E. A. The neurobiology of stress and gastrointestinal disease. Gut 47, 861–869 (2000).
Levenstein, S. et al. Stress and exacerbation in ulcerative colitis: a prospective study of patients enrolled in remission. Am. J. Gastroenterol. 95, 1213–1220 (2000).
Whitehead, W. E., Crowell, M. D., Robinson, J. C., Heller, B. R. & Schuster, M. M. Effects of stressful life events on bowel symptoms: subjects with irritable bowel syndrome compared with subjects without bowel dysfunction. Gut 33, 825–830 (1992).
Urban, M. O. & Gebhart, G. F. Central mechanisms in pain. Med. Clin. North Am. 83, 585–596 (1999).
Castagliuolo, I. et al. Neuronal involvement in the intestinal effects of Clostridium difficile toxin A and Vibrio cholerae enterotoxin in rat ileum. Gastroenterology 107, 657–665 (1994).
Mazmanian, S. K. et al. A microbial symbiosis factor prevents intestinal inflammatory disease. Nature 453, 620–625 (2008).
Guarner, F. & Malagelada, J. R. Gut flora in health and disease. Lancet 361, 512–519 (2003).
Husebye, E., Hellstrom, P. M., Sundler, F., Chen, J. & Midtvedt, T. Influence of microbial species on small intestinal myoelectric activity and transit in germ-free rats. Am. J. Physiol. Gastrointest. Liver Physiol. 280, G368–G380 (2001).
Rhee, S. H. et al. Pathophysiological role of Toll-like receptor 5 engagement by bacterial flagellin in colonic inflammation. Proc. Natl Acad. Sci. USA 102, 13610–13615 (2005).
Ait-Belgnaoui, A. et al. Lactobacillus farciminis treatment suppresses stress induced visceral hypersensitivity: a possible action through interaction with epithelial cell cytoskeleton contraction. Gut 55, 1090–1094 (2006).
Turnbaugh, P. J. et al. The human microbiome project. Nature 449, 804–810 (2007).
Spiller, P. Review article: probiotics and prebiotics in irritable bowel syndrome (IBS). Aliment. Pharmacol. Ther. (2008).
Agrawal, A. et al. Clinical trial: the effects of a fermented milk product containing Bifidobacterium lactis DN-173-010 on abdominal distension and gastrointestinal transit in irritable bowel syndrome with constipation. Aliment. Pharmacol. Ther. (In press).
Vanderpool, C., Yan, F. & Polk, D. B. Mechanisms of probiotic action: implications for therapeutic applications in inflammatory bowel diseases. Inflamm. Bowel Dis. 14, 1585–1596 (2008).
Schaedler, R. W. & Dubos, R. J. The fecal flora of various strains of mice. Its bearing on their susceptibility to endotoxin. J. Exp. Med. 115, 1149–1160 (1962).
Bailey, M. T. & Coe, C. L. Maternal separation disrupts the integrity of the intestinal microflora in infant rhesus monkeys. Dev. Psychobiol. 35, 146–155 (1999).
Bailey, M. T. et al. Prenatal stress alters bacterial colonization of the gut in infant monkeys. J. Pediatr. Gastroenterol. Nutr. 38, 414–421 (2004).
Holstege, G. et al. The Emotional Motor System (Elsevier, Amsterdam, 1996).
Macfarlane, S. & Dillon, J. F. Microbial biofilms in the human gastrointestinal tract. J. Appl. Microbiol. 102, 1187–1196 (2007).
Van Felius, I. D. et al. Interdigestive small bowel motility and duodenal bacterial overgrowth in experimental acute pancreatitis. Neurogastroenterol. Motil. 15, 267–276 (2003).
Lembo, A. & Camilleri, M. Chronic constipation. N. Engl. J. Med. 349, 1360–1368 (2003).
Chey, W. Y. et al. Colonic motility abnormality in patients with irritable bowel syndrome exhibiting abdominal pain and diarrhea. Am. J. Gastroenterol. 96, 1499–1506 (2001).
Kiliaan, A. J. et al. Stress stimulates transepithelial macromolecular uptake in rat jejunum. Am. J. Physiol. 275, G1037–G1044 (1998).
Groot, J. et al. Stress-induced decrease of the intestinal barrier function. The role of muscarinic receptor activation. Ann. NY Acad. Sci. 915, 237–246 (2000).
Yates, D. A., Santos, J., Soderholm, J. D. & Perdue, M. H. Adaptation of stress-induced mucosal pathophysiology in rat colon involves opioid pathways. Am. J. Physiol. Gastrointest. Liver Physiol. 281, G124–G128 (2001).
Soderholm, J. D. et al. Neonatal maternal separation predisposes adult rats to colonic barrier dysfunction in response to mild stress. Am. J. Physiol. Gastrointest. Liver Physiol. 283, G1257–G1263 (2002).
Jacob, C. et al. Mast cell tryptase controls paracellular permeability of the intestine. Role of protease-activated receptor 2 and beta-arrestins. J. Biol. Chem. 280, 31936–31948 (2005).
Demaude, J. et al. Phenotypic changes in colonocytes following acute stress or activation of mast cells in mice: implications for delayed epithelial barrier dysfunction. Gut 55, 655–661 (2006).
Salzman, N. H., Underwood, M. A. & Bevins, C. L. Paneth cells, defensins, and the commensal microbiota: a hypothesis on intimate interplay at the intestinal mucosa. Semin. Immunol. 19, 70–83 (2007).
Alonso, C. et al. Maladaptive intestinal epithelial responses to life stress may predispose healthy women to gut mucosal inflammation. Gastroenterology 135, 163–172 (2008).
Stephens, R. L. & Tache, Y. Intracisternal injection of a TRH analogue stimulates gastric luminal serotonin release in rats. Am. J. Physiol. 256, G377–G383 (1989).
Yang, H. et al. TRH analogue microinjected into specific medullary nuclei stimulates gastric serotonin secretion in rats. Am. J. Physiol. 262, G216–G222 (1992).
Santos, J. et al. Release of mast cell mediators into the jejunum by cold pain stress in humans. Gastroenterology 114, 640–648 (1998).
Hughes, D. T. & Sperandio, V. Inter-kingdom signalling: communication between bacteria and their hosts. Nat. Rev. Microbiol. 6, 111–120 (2008).
Alverdy, J. et al. Gut-derived sepsis occurs when the right pathogen with the right virulence genes meets the right host: evidence for in vivo virulence expression in Pseudomonas aeruginosa. Ann. Surg. 232, 480–489 (2000).
Cogan, T. A. et al. Norepinephrine increases the pathogenic potential of Campylobacter jejuni. Gut 56, 1060–1065 (2007).
Dunlop, S. P., Jenkins, D. & Spiller, R. C. Distinctive clinical, psychological, and histological features of postinfective irritable bowel syndrome. Am. J. Gastroenterol. 98, 1578–1583 (2003).
Barbara, G. et al. Interactions between commensal bacteria and gut sensorimotor function in health and disease. Am. J. Gastroenterol. 100, 2560–2568 (2005).
Dass, N. B. et al. The relationship between the effects of short-chain fatty acids on intestinal motility in vitro and GPR43 receptor activation. Neurogastroenterol. Motil. 19, 66–74 (2007).
Malbert, C. H. The ileocolonic sphincter. Neurogastroenterol. Motil. 17 (Suppl. 1), 41–49 (2005).
Nealson, K. H., Platt, T. & Hastings, J. W. Cellular control of the synthesis and activity of the bacterial luminescent system. J. Bacteriol. 104, 313–322 (1970).
Mayer, E. A. & Baldi, J. P. Can regulatory peptides be regarded as words of a biological language? Am. J. Physiol. 261, G171–G184 (1991).
Roth, J. et al. Molecules of intercellular communication in vertebrates, invertebrates and microbes: do they share common origins? Prog. Brain Res. 68, 71–79 (1986).
Reading, N. C. et al. A novel two-component signaling system that activates transcription of an enterohemorrhagic Escherichia coli effector involved in remodeling of host actin. J. Bacteriol. 189, 2468–2476 (2007).
Sperandio, V., Torres, A. G., Jarvis, B., Nataro, J. P. & Kaper, J. B. Bacteria–host communication: the language of hormones. Proc. Natl Acad. Sci. USA 100, 8951–8956 (2003).
Irie, Y. & Parsek, M. R. Quorum sensing and microbial biofilms. Curr. Top. Microbiol. Immunol. 322, 67–84 (2008).
Callaway, T. R. et al. Social stress increases fecal shedding of Salmonella typhimurium by early weaned piglets. Curr. Issues Intest. Microbiol. 7, 65–71 (2006).
Rhee, S. H., Keates, A. C., Moyer, M. P. & Pothoulakis, C. MEK is a key modulator for TLR5-induced interleukin-8 and MIP3alpha gene expression in non-transformed human colonic epithelial cells. J. Biol. Chem. 279, 25179–25188 (2004).
Rhee, S. H., Kim, H., Moyer, M. P. & Pothoulakis, C. Role of MyD88 in phosphatidylinositol 3-kinase activation by flagellin/Toll-like receptor 5 engagement in colonic epithelial cells. J. Biol. Chem. 281, 18560–18568 (2006).
Charrier, L. et al. hPepT1 mediates bacterial tripeptide fMLP uptake in human monocytes. Lab. Invest. 86, 490–503 (2006).
Valet, P. et al. Characterization and distribution of alpha 2-adrenergic receptors in the human intestinal mucosa. J. Clin. Invest. 91, 2049–2055 (1993).
Walsh, J. H. & Mayer, E. A. Gastrointestinal peptide hormones and signal transduction. In Gastrointestinal Disease: Pathophysiology, Diagnosis, Management 5th edn (Eds Sleizenger, M. & Fordtran, J.) 18–44 (WB Saunders, Philadelphia, 1993).
Braun, T., Voland, P., Kunz, L., Prinz, C. & Gratzl, M. Enterochromaffin cells of the human gut: sensors for spices and odorants. Gastroenterology 132, 1890–1901 (2007).
Gershon, M. D. & Tack, J. The serotonin signaling system: from basic understanding to drug development for functional GI disorders. Gastroenterology 132, 397–414 (2007).
Gershon, M. D. Nerves, reflexes, and the enteric nervous system: athogenesis of the irritable bowel syndrome. J. Clin. Gastroenterol. 39, S184–S193 (2005).
Grider, J. R., Kuemmerle, J. F. & Jin, J. G. 5-HT released by mucosal stimuli initiates peristalsis by activating 5-HT4/5-HT1p receptors on sensory CGRP neurons. Am. J. Physiol. 270, G778–G782 (1996).
Peregrin, A. T., Ahlman, H., Jodal, M. & Lundgren, O. Involvement of serotonin and calcium channels in the intestinal fluid secretion evoked by bile salt and cholera toxin. Br. J. Pharmacol. 127, 887–894 (1999).
Raybould, H. E. Visceral perception: sensory transduction in visceral afferents and nutrients. Gut 51 (Suppl. 1), i11–i14 (2002).
Hansen, M. B. & Witte, A. B. The role of serotonin in intestinal luminal sensing and secretion. Acta Physiol. (Oxf.) 193, 311–323 (2008).
Bogunovic, M. et al. Enteroendocrine cells express functional Toll-like receptors. Am. J. Physiol. Gastrointest. Liver Physiol. 292, G1770–G1783 (2007).
Lencer, W. I. Microbes and microbial toxins: paradigms for microbial-mucosal toxins. V. Cholera: invasion of the intestinal epithelial barrier by a stably folded protein toxin. Am. J. Physiol. Gastrointest. Liver Physiol. 280, G781–G786 (2001).
Costedio, M. M. et al. Serotonin and its role in colonic function and in gastrointestinal disorders. Dis. Colon Rectum 50, 376–388 (2007).
Spiller, R. C. Role of infection in irritable bowel syndrome. J. Gastroenterol. 42 (Suppl. 17), 41–47 (2007).
Grondahl, M. L. et al. Effects of nitric oxide in 5-hydroxytryptamine-, cholera toxin-, enterotoxigenic Escherichia coli and Salmonella typhimurium-induced secretion in the porcine small intestine. Comp. Biochem. Physiol. A Mol. Integr. Physiol. 141, 476–484 (2005).
Xue, J., Askwith, C., Javed, N. H. & Cooke, H. J. Autonomic nervous system and secretion across the intestinal mucosal surface. Auton. Neurosci. 133, 55–63 (2007).
Wheatcroft, J. et al. Enterochromaffin cell hyperplasia and decreased serotonin transporter in a mouse model of postinfectious bowel dysfunction. Neurogastroenterol. Motil. 17, 863–870 (2005).
Raybould, H. E., Cooke, H. J. & Christofi, F. L. Sensory mechanisms: transmitters, modulators and reflexes. Neurogastroenterol. Motil. 16 (Suppl. 1), 60–63 (2004).
Schonhoff, S. E., Giel-Moloney, M. & Leiter, A. B. Minireview: development and differentiation of gut endocrine cells. Endocrinology 145, 2639–2644 (2004).
O'Hara, J. R., Ho, W., Linden, D. R., Mawe, G. M. & Sharkey, K. A. Enteroendocrine cells and 5-HT availability are altered in mucosa of guinea pigs with TNBS ileitis. Am. J. Physiol. Gastrointest. Liver Physiol. 287, G998–G1007 (2004).
Li, Y. Sensory signal transduction in the vagal primary afferent neurons. Curr. Med. Chem. 14, 2554–2563 (2007).
Watkins, L. R. & Maier, S. F. Immune regulation of central nervous system functions: from sickness responses to pathological pain. J. Intern. Med. 257, 139–155 (2005).
Watkins, L. R. & Maier, S. F. The pain of being sick: implications of immune-to-brain communication for understanding pain. Annu. Rev. Psychol. 51, 29–57 (2000).
Lyte, M., Li, W., Opitz, N., Gaykema, R. P. & Goehler, L. E. Induction of anxiety-like behavior in mice during the initial stages of infection with the agent of murine colonic hyperplasia Citrobacter rodentium. Physiol. Behav. 89, 350–357 (2006).
Jänig, W., Khasar, S. G., Levine, J. D. & Miao, F. J. P. The role of visceral afferents in the control of nociception. In The Biological Basis for Mind Body Interactions 1st edn ( Eds Mayer, E. A. & Saper, C. B. ) 273–287 (Elsevier Science, Amsterdam, 2000).
Amaral, F. A. et al. Commensal microbiota is fundamental for the development of inflammatory pain. Proc. Natl Acad. Sci. USA 105, 2193–2197 (2008).
Sudo, N. et al. Postnatal microbial colonization programs the hypothalamic–pituitary–adrenal system for stress response in mice. J. Physiol. 558, 263–275 (2004).
Rousseaux, C. et al. Lactobacillus acidophilus modulates intestinal pain and induces opioid and cannabinoid receptors. Nat. Med. 13, 35–37 (2007).
Turnbaugh, P. J. et al. An obesity-associated gut microbiome with increased capacity for energy harvest. Nature 444, 1027–1031 (2006).
Kassinen, A. et al. The fecal microbiota of irritable bowel syndrome patients differs significantly from that of healthy subjects. Gastroenterology 133, 24–33 (2007).
Moayyedi, P. et al. The efficacy of probiotics in the therapy of irritable bowel syndrome: a systematic review. Gut [doi:10.1136/gut.2008.167270] (2008).
Gwee, K. A. et al. The role of psychological and biological factors in postinfective gut dysfunction. Gut 44, 400–406 (1999).
Bailey, M. T. et al. In vivo adaptation of attenuated Salmonella typhimurium results in increased growth upon exposure to norepinephrine. Physiol. Behav. 67, 359–364 (1999).
O'Mahony, L. et al. Lactobacillus and bifidobacterium in irritable bowel syndrome: symptom responses and relationship to cytokine profiles. Gastroenterology 128, 541–551 (2005).
Elenkov, I. J. & Chrousos, G. P. Stress system—organization, physiology and immunoregulation. Neuroimmunomodulation 13, 257–267 (2006).
Elenkov, I. J. et al. The sympathetic nerve—an interface between two supersystems: the brain and the immune system. Pharmacol. Rev. 52, 595–638 (2000).
Acknowledgements
This work was supported in part by the National Institute of Health/National Institute of Diabetes and Digestive and Kidney Diseases grants R01 DK 48,351, P50 DK64539 and R24 AT002681, RO1 DK47343, P01 DK 33,506, R01 DK072471, and RO1 DK060729. The authors thank Jennifer Drader for excellent editorial services.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
E. A. Mayer declared association with the following companies: Eli Lilly and Company as consultant, GlaxoSmithKline as consultant and recipient of grant/research support, Groupe Danone as consultant and recipient of grant/research support, Johnson & Johnson as recipient of grant/research support, Nestlé and Prometheus Laboratories as consultant. C. Pothoulakis and S. H. Rhee declared no competing interests.
Rights and permissions
About this article
Cite this article
Rhee, S., Pothoulakis, C. & Mayer, E. Principles and clinical implications of the brain–gut–enteric microbiota axis. Nat Rev Gastroenterol Hepatol 6, 306–314 (2009). https://doi.org/10.1038/nrgastro.2009.35
Issue Date:
DOI: https://doi.org/10.1038/nrgastro.2009.35
This article is cited by
-
Gut microbiota of Parkinson’s disease in an appendectomy cohort: a preliminary study
Scientific Reports (2023)
-
Fresh Washed Microbiota Transplantation Alters Gut Microbiota Metabolites to Ameliorate Sleeping Disorder Symptom of Autistic Children
Journal of Microbiology (2023)
-
Unveiling the gut-brain axis: structural and functional analogies between the gut and the choroid plexus vascular and immune barriers
Seminars in Immunopathology (2022)
-
Effects of different probiotic strains B. lactis, L. rhamnosus and L. reuteri on brain-intestinal axis immunomodulation in an endotoxin-induced inflammation
Molecular Neurobiology (2022)
-
The role and molecular mechanism of gut microbiota in Graves’ orbitopathy
Journal of Endocrinological Investigation (2022)