Key Points
-
Complex and diverse mechanisms have evolved to regulate the immune system and prevent it from inappropriately turning against the self. Overall, autoimmunity can be viewed as an alteration in the normal homeostatic mechanisms that regulate self–non-self discrimination.
-
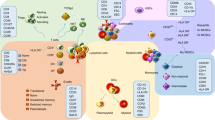
The immune system comprises two interacting systems that are based on innate and adaptive immune responses. Innate responses are immediate and generally use pre-formed recognition structures, whereas adaptive immunity involves the production and selection of specific recognition structures that develop following exposure and persist as a memory response.
-
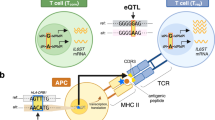
A number of genes involved in adaptive immunity have been implicated in autoimmune diseases. Several of these genes regulate T-cell tolerance to self, and give rise to rare and highly penetrant Mendelian disorders. Other genes are common and have more subtle 'threshold' effects on T-cell reactivity. In general, T-cell tolerance is effected 'centrally' in the thymus, or peripherally through the action of regulatory T cells or other mechanisms.
-
The genetic variants involved in regulating T-cell and B-cell tolerance predispose to multiple autoimmune disorders. This demonstrates that there are common underlying mechanisms for many of these diseases, such as type 1 diabetes, systemic lupus erythematosus and rheumatoid arthritis, among others.
-
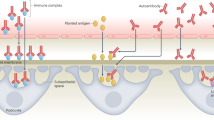
Recent studies have also demonstrated the involvement of the innate immune system in autoimmunity. In particular, Toll-like receptors have been implicated in the development of B-cell autoimmunity, and genetic associations in Toll-receptor signalling pathways have been found in systemic lupus erythematosus.
-
New gene-identification strategies, such as whole-genome association studies, are likely to reveal many additional genes that predispose to autoimmunity. A consideration of gene–gene and gene–environment interactions will be essential for the proper interpretation of these new genetic findings.
Abstract
In the past few years, our extensive knowledge of the mammalian immune system and our increasing ability to understand the genetic causes of complex human disease have opened a window onto the pathways that lead to autoimmune disorders. In addition to the well-established role of genetic variation that affects the major histocompatibility complex, a number of rare and common variants that affect a range of immunological pathways are now known to have important influences on the phenotypic diversity that is seen among autoimmune diseases. Recent studies have also highlighted a previously unanticipated interplay between the innate and adaptive immune system, providing a new direction for research in this field.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$189.00 per year
only $15.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
References
Silverstein, A. M. Paul Ehrlich, archives and the history of immunology. Nature Immunol. 6, 639 (2005).
Jacobson, D. L., Gange, S. J., Rose, N. R. & Graham, N. M. Epidemiology and estimated population burden of selected autoimmune diseases in the United States. Clin. Immunol. Immunopathol. 84, 223–243 (1997).
Hallert, E., Husberg, M., Jonsson, D. & Skogh, T. Rheumatoid arthritis is already expensive during the first year of the disease (the Swedish TIRA project). Rheumatology 43, 1374–1382 (2004).
Kobelt, G., Berg, J., Atherly, D. & Hadjimichael, O. Costs and quality of life in multiple sclerosis: a cross-sectional study in the United States. Neurology 66, 1696–1702 (2006).
Ashwood, P., Wills, S. & Van de Water, J. The immune response in autism: a new frontier for autism research. J. Leukoc. Biol. 80, 1–15 (2006).
Arbuckle, M. R. et al. Development of autoantibodies before the clinical onset of systemic lupus erythematosus. N. Engl. J. Med. 349, 1526–1533 (2003).
Hoppu, S., Ronkainen, M. S., Kulmala, P., Akerblom, H. K. & Knip, M. GAD65 antibody isotypes and epitope recognition during the prediabetic process in siblings of children with type I diabetes. Clin. Exp. Immunol. 136, 120–128 (2004).
Strieder, T. G., Prummel, M. F., Tijssen, J. G., Endert, E. & Wiersinga, W. M. Risk factors for and prevalence of thyroid disorders in a cross-sectional study among healthy female relatives of patients with autoimmune thyroid disease. Clin. Endocrinol. 59, 396–401 (2003).
Hugot, J. P. et al. Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn's disease. Nature 411, 599–603 (2001).
Ogura, Y. et al. A frameshift mutation in NOD2 associated with susceptibility to Crohn's disease. Nature 411, 603–606. (2001).
Shiina, T., Inoko, H. & Kulski, J. K. An update of the HLA genomic region, locus information and disease associations: 2004. Tissue Antigens 64, 631–649 (2004).
Criswell, L. A. et al. Analysis of families in the multiple autoimmune disease genetics consortium (MADGC) collection: the PTPN22 620W allele associates with multiple autoimmune phenotypes. Am. J. Hum. Genet. 76, 561–571 (2005).
Michel, M. et al. Familial lupus erythematosus. Clinical and immunologic features of 125 multiplex families. Medicine 80, 153–158 (2001).
Kyewski, B. & Klein, L. A central role for central tolerance. Annu. Rev. Immunol. 24, 571–606 (2006).
Liston, A., Lesage, S., Gray, D. H., Boyd, R. L. & Goodnow, C. C. Genetic lesions in T-cell tolerance and thresholds for autoimmunity. Immunol. Rev. 204, 87–101 (2005).
Sakaguchi, S., Setoguchi, R., Yagi, H. & Nomura, T. Naturally arising FOXP3-expressing CD25+CD4+ regulatory T cells in self-tolerance and autoimmune disease. Curr. Top. Microbiol. Immunol. 305, 51–66 (2006). References 14–16 provide a comprehensive discussion of the various mechanisms of T-cell tolerance. Sakaguchi, a pioneer in defining regulatory T cells, provides an up-to-date discussion of this fast-moving field.
Sakaguchi, S. & Sakaguchi, N. Regulatory T cells in immunologic self-tolerance and autoimmune disease. Int. Rev. Immunol. 24, 211–226 (2005).
Apostolou, I. & von Boehmer, H. In vivo instruction of suppressor commitment in naive T cells. J. Exp. Med. 199, 1401–1408 (2004).
Chen, W. et al. Conversion of peripheral CD4+CD25− naive T cells to CD4+CD25+ regulatory T cells by TGFβ induction of transcription factor FOXP3. J. Exp. Med. 198, 1875–1886 (2003).
Hori, S., Nomura, T. & Sakaguchi, S. Control of regulatory T-cell development by the transcription factor FOXP3. Science 299, 1057–1061 (2003).
Fontenot, J. D., Gavin, M. A. & Rudensky, A. Y. FOXP3 programs the development and function of CD4+CD25+ regulatory T cells. Nature. Immunol. 4, 330–336 (2003).
Fontenot, J. D., Rasmussen, J. P., Gavin, M. A. & Rudensky, A. Y. A function for interleukin 2 in FOXP3-expressing regulatory T cells. Nature. Immunol. 6, 1142–1151 (2005).
Bluestone, J. A. & Tang, Q. How do CD4+CD25+ regulatory T cells control autoimmunity? Curr. Opin. Immunol. 17, 638–642 (2005).
Anderson, M. S. et al. Projection of an immunological self shadow within the thymus by the AIRE protein. Science 298, 1395–1401 (2002). This seminal paper demonstrates the importance of AIRE in regulating the thymic expression of self antigens and its role in autoimmunity.
Anderson, M. S. et al. The cellular mechanism of AIRE control of T-cell tolerance. Immunity 23, 227–239 (2005).
Nagamine, K. et al. Positional cloning of the APECED gene. Nature Genet. 17, 393–398 (1997).
Eisenbarth, G. S. & Gottlieb, P. A. Autoimmune polyendocrine syndromes. N. Engl. J. Med. 350, 2068–2079 (2004).
Takase, H. et al. Thymic expression of peripheral tissue antigens in humans: a remarkable variability among individuals. Int. Immunol. 17, 1131–1140 (2005).
Barratt, B. J. et al. Remapping the insulin gene/IDDM2 locus in type 1 diabetes. Diabetes 53, 1884–1889 (2004).
Pugliese, A. et al. The insulin gene is transcribed in the human thymus and transcription levels correlated with allelic variation at the INS VNTR–IDDM2 susceptibility locus for type 1 diabetes. Nature Genet. 15, 293–297 (1997).
Vafiadis, P. et al. Insulin expression in human thymus is modulated by INS VNTR alleles at the IDDM2 locus. Nature Genet. 15, 289–292 (1997).
Chentoufi, A. A. & Polychronakos, C. Insulin expression levels in the thymus modulate insulin-specific autoreactive T-cell tolerance: the mechanism by which the IDDM2 locus may predispose to diabetes. Diabetes 51, 1383–1390 (2002).
Kent, S. C. et al. Expanded T cells from pancreatic lymph nodes of type 1 diabetic subjects recognize an insulin epitope. Nature 435, 224–228 (2005).
Giraud, M. et al. Transcriptional control of CHRNA1 gene in thymus by a promoter SNP associated with onset of autoimmune myasthenia gravis. Clinical Immunol. 119, 512 (2006).
Dechairo, B. M. et al. Association of the TSHR gene with Graves' disease: the first disease specific locus. Eur. J. Hum. Genet. 13, 1223–1230 (2005).
Sakaguchi, N. et al. Altered thymic T-cell selection due to a mutation of the ZAP70 gene causes autoimmune arthritis in mice. Nature 426, 454–460 (2003).
Wildin, R. S., Smyk-Pearson, S. & Filipovich, A. H. Clinical and molecular features of the immunodysregulation, polyendocrinopathy, enteropathy, X linked (IPEX) syndrome. J. Med. Genet. 39, 537–545 (2002).
Wildin, R. S. et al. X-linked neonatal diabetes mellitus, enteropathy and endocrinopathy syndrome is the human equivalent of mouse scurfy. Nature Genet. 27, 18–20 (2001).
Brunkow, M. E. et al. Disruption of a new forkhead/winged-helix protein, scurfin, results in the fatal lymphoproliferative disorder of the scurfy mouse. Nature Genet. 27, 68–73 (2001).
Khattri, R., Cox, T., Yasayko, S. A. & Ramsdell, F. An essential role for Scurfin in CD4+CD25+ T regulatory cells. Nature Immunol. 4, 337–342 (2003).
Sakaguchi, S., Fukuma, K., Kuribayashi, K. & Masuda, T. Organ-specific autoimmune diseases induced in mice by elimination of T cell subset. I. Evidence for the active participation of T cells in natural self-tolerance; deficit of a T cell subset as a possible cause of autoimmune disease. J. Exp. Med. 161, 72–87 (1985).
Sakaguchi, S. Naturally arising CD4+ regulatory T cells for immunologic self-tolerance and negative control of immune responses. Annu. Rev. Immunol. 22, 531–562 (2004).
Setoguchi, R., Hori, S., Takahashi, T. & Sakaguchi, S. Homeostatic maintenance of natural FOXP3(+) CD25(+) CD4(+) regulatory T cells by interleukin (IL)-2 and induction of autoimmune disease by IL-2 neutralization. J. Exp. Med. 201, 723–735 (2005).
Fehervari, Z., Yamaguchi, T. & Sakaguchi, S. The dichotomous role of IL-2: tolerance versus immunity. Trends Immunol. 27, 109–111 (2006).
Vella, A. et al. Localization of a type 1 diabetes locus in the IL2RA/CD25 region by use of tag single-nucleotide polymorphisms. Am. J. Hum. Genet. 76, 773–779 (2005).
Keir, M. E. & Sharpe, A. H. The B7/CD28 costimulatory family in autoimmunity. Immunol. Rev. 204, 128–143 (2005).
van Berkel, M. E. & Oosterwegel, M. A. CD28 and ICOS: similar or separate costimulators of T cells? Immunol. Lett. 105, 115–122 (2006).
Chen, L. Co-inhibitory molecules of the B7-CD28 family in the control of T-cell immunity. Nature Rev. Immunol. 4, 336–347 (2004).
Tivol, E. A. et al. Loss of CTLA-4 leads to massive lymphoproliferation and fatal multiorgan tissue destruction, revealing a critical negative regulatory role of CTLA-4. Immunity 3, 541–547 (1995).
Waterhouse, P. et al. Lymphoproliferative disorders with early lethality in mice deficient in CTLA-4. Science 270, 985–988 (1995).
Gough, S. C., Walker, L. S. & Sansom, D. M. CTLA4 gene polymorphism and autoimmunity. Immunol. Rev. 204, 102–115 (2005).
Yanagawa, T., Hidaka, Y., Guimaraes, V., Soliman, M. & DeGroot, L. J. CTLA-4 gene polymorphism associated with Graves' disease in a Caucasian population. J. Clin. Endocrinol. Metab. 80, 41–45 (1995).
Nistico, L. et al. The CTLA-4 gene region of chromosome 2q33 is linked to, and associated with, type 1 diabetes. Belgian Diabetes Registry. Hum. Mol. Genet. 5, 1075–1080 (1996).
Ueda, H. et al. Association of the T-cell regulatory gene CTLA4 with susceptibility to autoimmune disease. Nature 423, 506–511 (2003). The first detailed, although still incomplete, analysis of the molecular basis of CTLA associations with autoimmune disease. See reference 51 for a more recent review.
Plenge, R. M. et al. Replication of putative candidate-gene associations with rheumatoid arthritis in >4,000 samples from North America and Sweden: association of susceptibility with PTPN22, CTLA4, and PADI4. Am. J. Hum. Genet. 77, 1044–1060 (2005).
Nishimura, H., Nose, M., Hiai, H., Minato, N. & Honjo, T. Development of lupus-like autoimmune diseases by disruption of the PD-1 gene encoding an ITIM motif-carrying immunoreceptor. Immunity 11, 141–151 (1999).
Nishimura, H. et al. Autoimmune dilated cardiomyopathy in PD-1 receptor-deficient mice. Science 291, 319–322 (2001).
Prokunina, L. et al. A regulatory polymorphism in PDCD1 is associated with susceptibility to systemic lupus erythematosus in humans. Nature Genet. 32, 666–669 (2002).
Martin-Orozco, N. & Dong, C. New battlefields for costimulation. J. Exp. Med. 203, 817–820 (2006).
Holets, L. M., Hunt, J. S. & Petroff, M. G. Trophoblast CD274 (B7-H1) is differentially expressed across gestation: influence of oxygen concentration. Biol. Reprod. 74, 352–358 (2006).
Keir, M. E. et al. Tissue expression of PD-L1 mediates peripheral T cell tolerance. J. Exp. Med. 203, 883–895 (2006).
Greenwald, R. J., Freeman, G. J. & Sharpe, A. H. The B7 family revisited. Annu. Rev. Immunol. 23, 515–548 (2005).
Bottini, N., Vang, T., Cucca, F. & Mustelin, T. Role of PTPN22 in type 1 diabetes and other autoimmune diseases. Semin. Immunol. 18, 207–213 (2006).
Wu, J. et al. Identification of substrates of human protein tyrosine phosphatase PTPN22. J. Biol. Chem. 281, 11002–11010 (2006).
Bottini, N. et al. A functional variant of lymphoid tyrosine phosphatase is associated with type I diabetes. Nature Genet. 36, 337–338 (2004).
Begovich, A. B. et al. A missense single-nucleotide polymorphism in a gene encoding a protein tyrosine phosphatase (PTPN22) is associated with rheumatoid arthritis. Am. J. Hum. Genet. 75, 330–337 (2004).
Smyth, D. et al. Replication of an association between the lymphoid tyrosine phosphatase locus (LYP/PTPN22) with type 1 diabetes, and evidence for its role as a general autoimmunity locus. Diabetes 53, 3020–3023 (2004).
Kyogoku, C. et al. Genetic association of the R620W polymorphism of protein tyrosine phosphatase PTPN22 with human SLE. Am. J. Hum. Genet. 75, 504–507 (2004).
Vandiedonck, C. et al. Association of the PTPN22*R620W polymorphism with autoimmune myasthenia gravis. Ann. Neurol. 59, 404–407 (2006).
Vang, T. et al. Autoimmune-associated lymphoid tyrosine phosphatase is a gain-of-function variant. Nature Genet. 37, 1317–1319 (2005).
Hasegawa, K. et al. PEST domain-enriched tyrosine phosphatase (PEP) regulation of effector/memory T cells. Science 303, 685–689 (2004). These two papers present contrasting evidence for the mechanisms by which PTPN22 alleles predispose to autoimmunity. Vang et al . provide evidence for the gain of function of PTPN22 risk alleles, whereas studies in knockout mice (Hasegawa et al .) indicate that PTPN22 has predominantly negative regulatory effects in T cells.
Gregersen, P. K., Lee, H. S., Batliwalla, F. & Begovich, A. B. PTPN22: setting thresholds for autoimmunity. Semin. Immunol. 18, 214–223 (2006).
Siminovitch, K. A. PTPN22 and autoimmune disease. Nature Genet. 36, 1248–1249 (2004).
Gregersen, P. K. Gaining insight into PTPN22 and autoimmunity. Nature Genet. 37, 1300–1302 (2005).
Begovich, A. B. et al. The R620W polymorphism of the protein tyrosine phosphatase PTPN22 is not associated with multiple sclerosis. Am. J. Hum. Genet. 76, 184–187 (2005).
van Oene, M. et al. Association of the lymphoid tyrosine phosphatase R620W variant with rheumatoid arthritis, but not Crohn's disease, in Canadian populations. Arthritis Rheum. 52, 1993–1998 (2005).
Carlton, V. E. et al. PTPN22 genetic variation: evidence for multiple variants associated with rheumatoid arthritis. Am. J. Hum. Genet. 77, 567–581 (2005).
Marchini, J., Cardon, L. R., Phillips, M. S. & Donnelly, P. The effects of human population structure on large genetic association studies. Nature Genet. 36, 512–517 (2004).
Seldin, M. et al. European population substructure: clustering of northern and southern populations. PLoS Genet. 2, 1339–1351 (2006).
Price, A. L. et al. Principal components analysis corrects for stratification in genome-wide association studies. Nature Genet. 38, 904–909 (2006).
Nimmerjahn, F. & Ravetch, J. V. Fcγ receptors: old friends and new family members. Immunity 24, 19–28 (2006).
Takai, T. Fc receptors and their role in immune regulation and autoimmunity. J. Clin. Immunol. 25, 1–18 (2005).
Su, K. et al. A promoter haplotype of the immunoreceptor tyrosine-based inhibitory motif-bearing FcγRIIb alters receptor expression and associates with autoimmunity. II. Differential binding of GATA4 and Yin-Yang1 transcription factors and correlated receptor expression and function. J. Immunol. 172, 7192–7199 (2004).
Blank, M. C. et al. Decreased transcription of the human FCGR2B gene mediated by the-343 G/C promoter polymorphism and association with systemic lupus erythematosus. Hum. Genet. 117, 220–227 (2005).
Chadha, S. et al. Haplotype structure of TNFRSF5–TNFSF5 (CD40–CD40L) and association analysis in systemic lupus erythematosus. Eur. J. Hum. Genet. 13, 669–676 (2005).
Sontheimer, R. D., Racila, E. & Racila, D. M. C1Q: its functions within the innate and adaptive immune responses and its role in lupus autoimmunity. J. Invest. Dermatol. 125, 14–23 (2005).
Akira, S., Uematsu, S. & Takeuchi, O. Pathogen recognition and innate immunity. Cell 124, 783–801 (2006).
Meylan, E., Tschopp, J. & Karin, M. Intracellular pattern recognition receptors in the host response. Nature 442, 39–44 (2006).
Schreiber, S., Rosenstiel, P., Albrecht, M., Hampe, J. & Krawczak, M. Genetics of Crohn disease, an archetypal inflammatory barrier disease. Nature Rev. Genet. 6, 376–388 (2005).
Leadbetter, E. A. et al. Chromatin-IgG complexes activate B cells by dual engagement of IgM and Toll-like receptors. Nature 416, 603–607 (2002). This groundbreaking study demonstrates that TLRs can co-stimumlate B-cell activation in the absence of T-cell help.
Rifkin, I. R., Leadbetter, E. A., Busconi, L., Viglianti, G. & Marshak-Rothstein, A. Toll-like receptors, endogenous ligands, and systemic autoimmune disease. Immunol. Rev. 204, 27–42 (2005).
Baechler, E. C. et al. Interferon-inducible gene expression signature in peripheral blood cells of patients with severe lupus. Proc. Natl Acad. Sci. USA 100, 2610–2615 (2003).
Ronnblom, L., Eloranta, M. L. & Alm, G. V. The type I interferon system in systemic lupus erythematosus. Arthritis Rheum. 54, 408–420 (2006).
Baechler, E. C., Gregersen, P. K. & Behrens, T. W. The emerging role of interferon in human systemic lupus erythematosus. Curr. Opin. Immunol. 16, 801–807 (2004).
Sigurdsson, S. et al. Polymorphisms in the tyrosine kinase 2 and interferon regulatory factor 5 genes are associated with systemic lupus erythematosus. Am. J. Hum. Genet. 76, 528–537 (2005).
Graham, R. R. et al. A common haplotype of interferon regulatory factor 5 (IRF5) regulates splicing and expression and is associated with increased risk of systemic lupus erythematosus. Nature Genet. 38, 550–555 (2006). These two studies provide definitive evidence for the involvement of IRF5 in genetic susceptibility to SLE, therefore linking TLR signalling with abnormalities of interferon regulation in this disease (also see reference 93 for a review).
Morley, M. et al. Genetic analysis of genome-wide variation in human gene expression. Nature 430, 743–747 (2004).
Thurman, J. M. & Holers, V. M. The central role of the alternative complement pathway in human disease. J. Immunol. 176, 1305–1310 (2006).
Pickering, M. C., Botto, M., Taylor, P. R., Lachmann, P. J. & Walport, M. J. Systemic lupus erythematosus, complement deficiency, and apoptosis. Adv. Immunol. 76, 227–324 (2000).
Russell, A. I. et al. Polymorphism at the C-reactive protein locus influences gene expression and predisposes to systemic lupus erythematosus. Hum. Mol. Genet. 13, 137–147 (2004).
Werth, V. P., Berlin, J. A., Callen, J. P., Mick, R. & Sullivan, K. E. Mannose binding lectin (MBL) polymorphisms associated with low MBL production in patients with dermatomyositis. J. Invest. Dermatol. 119, 1394–1399 (2002).
Kravitz, M. S., Pitashny, M. & Shoenfeld, Y. Protective molecules — C-reactive protein (CRP), serum amyloid P (SAP), pentraxin3 (PTX3), mannose-binding lectin (MBL), and apolipoprotein A1 (Apo A1), and their autoantibodies: prevalence and clinical significance in autoimmunity. J. Clin. Immunol. 25, 582–591 (2005).
Subramanian, S. et al. A Tlr7 translocation accelerates systemic autoimmunity in murine lupus. Proc. Natl Acad. Sci. USA 103, 9970–9975 (2006).
Pisitkun, P. et al. Autoreactive B cell responses to RNA-related antigens due to TLR7 gene duplication. Science 312, 1669–1672 (2006). These two recent studies provide direct evidence for the involvement of TLRs ( Tlr7 ) in mouse models of autoimmunity, setting the stage for a further investigation of the role of TLR7 in humans, and further supporting the involvement of innate immune mechanisms in the development of autoimmunity.
Suzuki, A. et al. Functional haplotypes of PADI4, encoding citrullinating enzyme peptidylarginine deiminase 4, are associated with rheumatoid arthritis. Nature Genet. 34, 395–402 (2003).
Alarcon, G. S. et al. Systemic lupus erythematosus in a multi-ethnic cohort (LUMINA) XXXII: [corrected] contributions of admixture and socioeconomic status to renal involvement. Lupus 15, 26–31 (2006).
Krishnan, E. & Hubert, H. B. Ethnicity and mortality from systemic lupus erythematosus in the US. Ann. Rheum. Dis. 65, 1500–1505 (2006).
Ioannidis, J. P., Ntzani, E. E., Trikalinos, T. A. & Contopoulos-Ioannidis, D. G. Replication validity of genetic association studies. Nature Genet. 29, 306–309 (2001).
International HapMap Consortium. A haplotype map of the human genome. Nature 437, 1299–320 (2005).
Klein, R. J. et al. Complement factor H polymorphism in age-related macular degeneration. Science 308, 385–389 (2005).
Pritchard, J. K. & Cox, N. J. The allelic architecture of human disease genes: common disease-common variant. or not? Hum. Mol. Genet. 11, 2417–2423 (2002).
Hirschhorn, J. N. & Daly, M. J. Genome-wide association studies for common diseases and complex traits. Nature Rev. Genet. 6, 95–108 (2005).
Wang, W. Y., Barratt, B. J., Clayton, D. G. & Todd, J. A. Genome-wide association studies: theoretical and practical concerns. Nature Rev. Genet. 6, 109–118 (2005).
Costenbader, K. H., Feskanich, D., Mandl, L. A. & Karlson, E. W. Smoking intensity, duration, and cessation, and the risk of rheumatoid arthritis in women. Am. J. Med. 119, 503.e1–503.e9 (2006).
Klareskog, L. et al. A new model for an etiology of rheumatoid arthritis: smoking may trigger HLA-DR (shared epitope)-restricted immune reactions to autoantigens modified by citrullination. Arthritis Rheum. 54, 38–46 (2006). This report provides a compelling recent example of a gene–environment interaction in the development of autoimmunity.
Schellekens, G. A. et al. The diagnostic properties of rheumatoid arthritis antibodies recognizing a cyclic citrullinated peptide. Arthritis Rheum. 43, 155–163 (2000).
Irigoyen, P. et al. Regulation of anti-cyclic citrullinated peptide antibodies in rheumatoid arthritis: contrasting effects of HLA–DR3 and the shared epitope alleles. Arthritis Rheum. 52, 3813–3818 (2005).
Berglin, E. et al. A combination of autoantibodies to cyclic citrullinated peptide (CCP) and HLA–DRB1 locus antigens is strongly associated with future onset of rheumatoid arthritis. Arthritis Res. Ther. 6, R303–R308 (2004).
Kuhn, K. A. et al. Antibodies against citrullinated proteins enhance tissue injury in experimental autoimmune arthritis. J. Clin. Invest. 116, 961–973 (2006).
James, J. A. et al. Systemic lupus erythematosus in adults is associated with previous Epstein–Barr virus exposure. Arthritis Rheum. 44, 1122–1126 (2001).
Manolio, T. A., Bailey-Wilson, J. E. & Collins, F. S. Genes, environment, and the value of prospective cohort studies. Nature Rev. Genet. 7, 812–820 (2006).
Vyse, T. J. & Todd, J. A. Genetic analysis of autoimmune disease. Cell 85, 311–318 (1996).
Redondo, M. J. & Eisenbarth, G. S. Genetic control of autoimmunity in type I diabetes and associated disorders. Diabetologia 45, 605–622 (2002).
Ban, Y. & Tomer, Y. Susceptibility genes in thyroid autoimmunity. Clin. Dev. Immunol. 12, 47–58 (2005).
Barcellos, L. F. et al. HLA–DR2 dose effect on susceptibility to multiple sclerosis and influence on disease course. Am. J. Hum. Genet. 72, 710–716 (2003).
Graham, R. R. et al. Visualizing human leukocyte antigen class II risk haplotypes in human systemic lupus erythematosus. Am. J. Hum. Genet. 71, 543–553 (2002).
Hall, F. C. et al. Influence of the HLA–DRB1 locus on susceptibility and severity in rheumatoid arthritis. QJM 89, 821–829 (1996).
Prokunina, L. et al. Association of the PD-1.3A allele of the PDCD1 gene in patients with rheumatoid arthritis negative for rheumatoid factor and the shared epitope. Arthritis Rheum. 50, 1770–1773 (2004).
Acknowledgements
Some of the work described in this Review has been supported by grants from the National Institutes of Health and the National Arthritis Foundation. P.K.G. receives additional support from the Boas family and from the Eileen Ludwig Greenland Center for Rheumatoid Arthritis.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Related links
DATABASES
OMIM
FURTHER INFORMATION
Glossary
- Innate immune system
-
Nonspecific and phylogenetically ancient mechanisms that form the first line of defence against infection. Innate immune defence is inborn and does not involve memory; it uses a limited set of molecules that generally recognize common molecular patterns found in microorganisms.
- Adaptive immune system
-
A flexible and specific immune response that can adjust to new structures and that retains a memory of prior exposure to these structures. A large and diverse set of recognition molecules — antibodies (produced by B cells) and T-cell receptors — mediate adaptive immune recognition.
- Linkage analysis
-
A method for tracking the transmission of genetic information across generations to identify the map location of genetic loci on the basis of co-inheritance of genetic markers and discernable phenotypes.
- Gene association study
-
A study in which a genetic variant is genotyped in a population for which phenotypic information (such as disease occurrence, or a range of different trait values) is available. If a correlation is observed between the genotype and phenotype, there is said to be an association between the variant and the disease or trait.
- Candidate gene
-
A gene for which there is evidence of its possible role in the trait or disease that is under study.
- T cells
-
Lymphocytes that have important roles in the primary immune response. Effector T cells fall into two classes — CD8+ killer or cytotoxic T cells, which destroy infected cells, and CD4+ or helper T cells, which regulate the function of other lymphocytes. A third class, regulatory T cells, regulate the self reactivity of effector T cells in the periphery.
- Systemic lupus erythematosus
-
The prototypical autoimmune disease in which antibodies are produced to DNA and a variety of other self constituents. The disease has highly variable manifestations and can be mild or lead to widespread inflammation and tissue destruction of important organ systems.
- Tolerance
-
A specific unresponsiveness of the adaptive immune system to particular antigens in an otherwise immunocompetent organism. In the absence of autoimmunity, tolerance to self antigens is characteristic of the normal immune system.
- Type I diabetes
-
An autoimmune disorder in which insulin-producing islet cells are destroyed by the immune system, leading to insulin deficiency. Onset is usually in childhood or adolescence.
- Myasthenia gravis
-
An autoimmune disorder in which antibodies to the acetylcholine receptor disrupt neuromuscular transmission leading to symptoms of weakness.
- Rheumatoid arthritis
-
A chronic inflammatory disorder of synovial joints and surrounding tissues. It often leads to bone and cartilage destruction if left untreated.
- Whole-genome association studies
-
Studies in which associations between genetic variation and a phenotype of interest (for example, disease) are identified by genotyping cases and controls for a set of polymorphic markers that capture genetic variation across the entire genome.
- Florid lymphoproliferation
-
Extensive proliferation of lymphoid elements, usually either T cells or B cells.
- Odds ratio
-
A measure of relative risk that is usually estimated from case–control studies.
- Addison disease
-
A condition resulting from inadequate production of cortisol by the adrenal glands owing to adrenal destruction by autoimmune mechanisms.
- Coeliac disease
-
An autoimmune disorder induced by exposure to gluten and characterized by damage to all or part of the villi lining the small intestine, leading to malabsorption.
- Macrophage
-
A specialized type of white blood cell that can engulf foreign particles and microorganisms.
- Dendritic cells
-
These cells present antigen to T cells, and stimulate cell proliferation and the immune response.
- Memory T cells
-
T lymphocytes that have been previously exposed to specific antigen and are primed to have an increased response following re-exposure to the same antigen.
- Natural killer cell
-
Large granular non-T, non-B-type lymphocytes. Natural killer cells are important for the early response to viruses. They produce cytokines, kill certain tumour cells and have appropriate receptors for antibody-dependent cell-mediated cytotoxicity.
- Humoral
-
In mammals, humoral immunity describes B-cell-mediated immunity that fights bacteria and viruses in body fluids with antibodies that circulate in blood plasma and lymph.
- Ancestry informative markers
-
A locus with several polymorphisms that exhibit substantially different frequencies between ancestral populations. For example, the Duffy null allele has a frequency of almost 100% of sub-Saharan Africans, but occurs rarely in other populations.
- Complement system
-
A complex protein cascade that is involved in both innate and adaptive immunity. Three biochemical pathways activate the complement system: the classical complement pathway, the alternative complement pathway, and the mannose-binding lectin pathway.
- Penetrance
-
The proportion of individuals with a specific genotype who manifest the genotype at the phenotypic level. For example, if all individuals with a specific disease genotype show the disease phenotype, then the genotype is said to be 'completely penetrant'.
- Multiple-hypothesis testing
-
Testing more than one hypothesis within an experiment. As a result, the probability of an unusual result from within the entire experiment occurring by chance is higher than the individual P-value associated with that result.
- Prospective cohorts
-
Individuals who are selected for certain exposure characteristics and can be followed up over time to assess who develops a certain outcome (often disease).
Rights and permissions
About this article
Cite this article
Gregersen, P., Behrens, T. Genetics of autoimmune diseases — disorders of immune homeostasis. Nat Rev Genet 7, 917–928 (2006). https://doi.org/10.1038/nrg1944
Issue Date:
DOI: https://doi.org/10.1038/nrg1944
This article is cited by
-
The brain structure, immunometabolic and genetic mechanisms underlying the association between lifestyle and depression
Nature Mental Health (2023)
-
Modic change is associated with increased BMI but not autoimmune diseases in TwinsUK
European Spine Journal (2023)
-
The Adaptive and Innate Immune Cell Landscape of Uterine Leiomyosarcomas
Scientific Reports (2020)
-
HLA in transplantation
Nature Reviews Nephrology (2018)
-
Influence of genetic polymorphisms of IL23R, STAT3, IL12B, and STAT4 on the risk of aplastic anemia and the effect of immunosuppressive therapy
Annals of Hematology (2018)