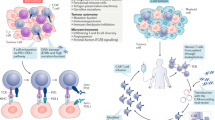
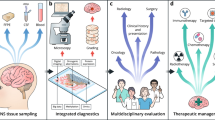
Abstract
Improvements in protocol-driven clinical trials and supportive care for children and adolescents with cancer have reduced mortality rates by more than 50% over the past three decades. Overall, the 5-year survival rate for patients with pediatric cancer has increased to approximately 80%. Recognition of the biological heterogeneity within specific subtypes of cancer, the discovery of genetic lesions that drive malignant transformation and cancer progression, and improved understanding of the basis of drug resistance will undoubtedly catalyze further advances in risk-directed treatments and the development of targeted therapies, boosting the cure rates further. Emerging new treatments include novel formulations of existing chemotherapeutic agents, monoclonal antibodies against cancer-associated antigens, and molecular therapies that target genetic lesions and their associated signaling pathways. Recent findings that link pharmacogenomic variations with drug exposure, adverse effects, and efficacy should accelerate efforts to develop personalized therapy for individual patients. Finally, palliative care should be included as an essential part of cancer management to prevent and relieve the suffering and to improve the quality of life of patients and their families.
Key Points
-
Prophylactic cranial irradiation can be omitted from the treatment of patients with acute lymphoblastic or myeloid leukemia, with the use of effective systemic and intrathecal therapy
-
Vigilant supportive care can reduce morbidity and mortality, and improve event-free survival of acute myeloid leukemia
-
The next generation of treatment for brain tumors will be tailored to specific molecular subtypes of disease to improve the cure rates and reduce the long-term sequela of therapy
-
The cure rates have improved dramatically over the past three decades for patients with localized solid tumors and hematologic cancers
-
Patients with disseminated disease continue to fare poorly and some are now receiving targeted therapies against specific molecular alterations
-
Integration of palliative care into the ongoing care of children with cancer improves the quality of pediatric oncology care
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
The cancer genome census. Wellcome Trust Sanger Institute [online], (2011).
Stratton, M. R., Campbell, P. J. & Futreal, P. A. The cancer genome. Nature 458, 719–724 (2009).
National Cancer Institute. Surveillance Epidemiology and End Results. Previous Version: SEER Cancer Statistics Review, 1975–2007 [online], (2010).
Pui, C. H., Carroll, W. L., Meshinchi, S. & Arceci, R. J. Biology, risk stratification and therapy of pediatric acute leukemias: an update. J. Clin. Oncol. 29, 551–565 (2011).
Nachman, J. B. et al. Young adults with acute lymphoblastic leukemia have an excellent outcome with chemotherapy alone and benefit from intensive postinduction treatment: a report from the Children's Oncology Group. J. Clin. Oncol. 27, 5189–5194 (2009).
Pui, C. H. et al. Improved prognosis for older adolescents with acute lymphoblastic leukemia. J. Clin. Oncol. 29, 386–391 (2011).
Schultz, K. R. et al. Improved early event-free survival with imatinib in Philadelphia chromosome-positive acute lymphoblastic leukemia: a Children's Oncology Group study. J. Clin. Oncol. 27, 5175–5181 (2009).
Pui, C. H. & Jeha, S. New therapeutic strategies for the treatment of acute lymphoblastic leukaemia. Nat. Rev. Drug. Discov. 6, 149–165 (2007).
Pui, C. H. & Howard, S. C. Current management and challenges of malignant disease in the CNS in paediatric leukaemia. Lancet Oncol. 9, 257–268 (2008).
Pui, C. H. et al. Treating childhood acute lymphoblastic leukemia without cranial irradiation. N. Engl. J. Med. 360, 2730–2741 (2009).
Veerman, A. J. et al. Dexamethasone-based therapy for childhood acute lymphoblastic leukaemia: results of the prospective Dutch Childhood Oncology Group (DCOG) protocol ALL-9 (1997–2004). Lancet Oncol. 10, 957–966 (2009).
Coustan-Smith, E. et al. Early T-cell precursor leukaemia: a subtype of very high-risk acute lymphoblastic leukaemia. Lancet Oncol. 10, 147–156 (2009).
Schrappe, M. et al. Dexamethasone in induction can eliminate one third of all relapses in childhood acute lymphoblastic leukemia (ALL): Results of an international randomized trial in 3655 patients (Trial AEIOP-BFM ALL 2000) [abstract]. Am. Soc. Hematol. Ann. Meeting 112, a7 (2008).
Pui, C. H. et al. Outcome of treatment in childhood acute lymphoblastic leukaemia with rearrangements of the 11q23 chromosomal region. Lancet 359, 1909–1915 (2002).
Pieters, R. et al. A treatment protocol for infants younger than 1 year with acute lymphoblastic leukaemia (Interfant-99): an observational study and a multicentre randomised trial. Lancet 370, 240–250 (2007).
Dreyer, Z. E. et al. Analysis of the role of hematopoietic stem-cell transplantation in infants with acute lymphoblastic leukemia in first remission and MLL gene rearrangements: a report from the Children's Oncology Group. J. Clin. Oncol. 29, 214–222 (2011).
Brown, P., Levis, M., McIntyre, E., Griesemer, M. & Small, D. Combinations of the FLT3 inhibitor CEP-701 and chemotherapy synergistically kill infant and childhood MLL-rearranged ALL cells in a sequence-dependent manner. Leukemia 20, 1368–1376 (2006).
Schafer, E. et al. Promoter hypermethylation in MLL-r infant acute lymphoblastic leukemia: biology and therapeutic targeting. Blood 115, 4798–4809 (2010).
Mullighan, C. G. et al. BCR-ABL1 lymphoblastic leukaemia is characterized by the deletion of Ikaros. Nature 453, 110–114 (2008).
Mullighan, C. G. et al. Deletion of IKZF1 and prognosis in acute lymphoblastic leukemia. N. Engl. J. Med. 360, 470–480 (2009).
Den Boer, M. L. et al. A subtype of childhood acute lymphoblastic leukaemia with poor treatment outcome: a genome-wide classification study. Lancet Oncol. 10, 125–134 (2009).
Mullighan, C. G. et al. Rearrangement of CRLF2 in B-progenitor- and Down syndrome-associated acute lymphoblastic leukemia. Nat. Genet. 41, 1243–1246 (2009).
Cario, G. et al. Presence of the P2RY8-CRLF2 rearrangement is associated with a poor prognosis in non-high-risk precursor B-cell acute lymphoblastic leukemia in children treated according to the ALL-BFM 2000 protocol. Blood 115, 5393–5397 (2010).
Mullighan, C. G. et al. CREBBP mutations in relapsed acute lymphoblastic leukaemia. Nature 471, 235–239 (2011).
Pui, C. H., Robison, L. L. & Look, A. T. Acute lymphoblastic leukaemia. Lancet 371, 1030–1043 (2008).
Lee-Sherick, A. B. et al. Targeting paediatric acute lymphoblastic leukaemia: novel therapies currently in development. Br. J. Haematol. 151, 295–311 (2010).
Kawedia, J. D. et al. Pharmacokinetic, pharmacodynamic and pharmacogenetic determinants of osteonecrosis in children with acute lymphoblastic leukemia. Blood 117, 2340–2347 (2011).
Rubnitz, J. E. et al. Minimal residual disease-directed therapy for childhood acute myeloid leukaemia: results of the AML02 multicentre trial. Lancet Oncol. 11, 543–552 (2010)
Harrison, C. J. et al. Cytogenetics of childhood acute myeloid leukemia: United Kingdom Medical Research Council Treatment trials AML 10 and 12. J. Clin. Oncol. 28, 2674–2681 (2010).
Pratz, K. W. et al. FLT3-mutant allelic burden and clinical status are predictive of response to FLT3 inhibitors in AML. Blood 115, 1425–1432 (2010).
Rubnitz, J. E. et al. NKAML: a pilot study to determine the safety and feasibility of haploidentical natural killer cell transplantation in childhood acute myeloid leukemia. J. Clin. Oncol. 28, 955–959 (2010).
Hudson, M. M. et al. Noninvasive evaluation of late anthracycline cardiac toxicity in childhood cancer survivors. J. Clin. Oncol. 25, 3635–3643 (2007).
Jeha, S. et al. Phase II study of clofarabine in pediatric patients with refractory or relapsed acute myeloid leukemia. J. Clin. Oncol. 27, 4392–4397 (2009).
Kurt, B. et al. Prophylactic antibiotics reduce morbidity due to septicemia during intensive treatment for pediatric acute myeloid leukemia. Cancer 113, 376–382 (2008).
Cornely, O. A. et al. Posaconazole vs. fluconazole or itraconazole prophylaxis in patients with neutropenia. N. Engl. J. Med. 356, 348–359 (2007).
Ehlers, S. et al. Granulocyte colony-stimulating factor (G-CSF) treatment of childhood acute myeloid leukemias that overexpress the differentiation-defective G-CSF receptor isoform IV is associated with a higher incidence of relapse. J. Clin. Oncol. 28, 2591–2597 (2010).
Gajjar, A. et al. Risk-adapted craniospinal radiotherapy followed by high-dose chemotherapy and stem-cell rescue in children with newly diagnosed medulloblastoma (St Jude Medulloblastoma-96): long-term results from a prospective, multicentre trial. Lancet Oncol. 7, 813–820 (2006).
Hughes, E. N. et al. Medulloblastoma at the joint center for radiation therapy between 1968 and 1984. The influence of radiation dose on the patterns of failure and survival. Cancer 61, 1992–1998 (1988).
Thompson, M. C. et al. Genomics identifies medulloblastoma subgroups that are enriched for specific genetic alterations. J. Clin. Oncol. 24, 1924–1931 (2006).
Kool, M. et al. Integrated genomics identifies 5 medulloblastoma subtypes with distinct molecular profiles, pathway signatures and clinicopathological features. PLoS ONE 3, e3068 (2008).
Northcott, P. A. et al. Medulloblastoma comprises four distinct molecular variants. J. Clin. Oncol. 29, 1408–1414 (2011).
Rudin, C. M. et al. Treatment of medulloblastoma with hedgehog pathway inhibitor GDC-0449. N. Engl. J. Med. 361, 1173–1178 (2009).
Tamburrini, G. et al. Survival following treatment for intracranial ependymoma: a review. Childs Nerv. Syst. 25, 1303–1312 (2009).
Merchant, T. E. et al. Conformal radiotherapy after surgery for paediatric ependymoma: a prospective study. Lancet Oncol. 10, 258–266 (2009).
Korshunov, A. et al. Molecular staging of intracranial ependymoma in children and adults. J. Clin. Oncol. 28, 3182–3190 (2010).
Johnson, R. A. et al. Cross-species genomics matches driver mutations and cell compartments to model ependymoma. Nature 466, 632–636 (2010).
Puget, S. et al. Candidate genes on chromosome 9q33–34 involved in the progression of childhood ependymomas. J. Clin. Oncol. 27, 1884–1892 (2009).
Kilday, J. P. et al. Pediatric ependymoma: biological perspectives. Mol. Cancer Res. 7, 765–786 (2009).
Broniscer, A. Past, present, and future strategies in the treatment of high-grade glioma in children. Cancer Invest. 24, 77–81 (2006).
Broniscer, A. et al. Temozolomide after radiotherapy for newly diagnosed high-grade glioma and unfavorable low-grade glioma in children. J. Neurooncol. 76, 313–319 (2006).
Gururangan, S. et al. Lack of efficacy of bevacizumab plus irinotecan in children with recurrent malignant glioma and diffuse brainstem glioma: a Pediatric Brain Tumor Consortium study. J. Clin. Oncol. 28, 3069–3075 (2010).
Parsons, D. W. et al. An integrated genomic analysis of human glioblastoma multiforme. Science 321, 1807–1812 (2008).
Cancer Genome Atlas Research Network. Comprehensive genomic characterization defines human glioblastoma genes and core pathways. Nature 455, 1061–1068 (2008).
Zarghooni, M. et al. Whole genome profiling of pediatric intrinsic diffuse pontine gliomas highlight platelet derived growth factor receptor α and poly (ADP-ribose) polymerase as potential therapeutic targets. J. Clin. Oncol. 28, 1337–1344 (2010).
Paugh, B. S. et al. Integrated molecular genetic profiling of pediatric high-grade gliomas reveals key differences with the adult disease. J. Clin. Oncol. 28, 3061–3068 (2010).
Gajjar, A. et al. Low-grade astrocytoma: a decade of experience at St. Jude Children's Research Hospital. J. Clin. Oncol. 15, 2792–2799 (1997).
Armstrong, G. T. et al. Survival and long-term health and cognitive outcomes after low-grade glioma. Neuro Oncol. 13, 223–234 (2011).
Forshew, T. et al. Activation of the ERK/MAPK pathway: a signature genetic defect in posterior fossa pilocytic astrocytomas. J. Pathol. 218, 172–181 (2009).
Pfister, S. et al. BRAF gene duplication constitutes a mechanism of MAPK pathway activation in low-grade astrocytomas. J. Clin. Invest. 118, 1739–1749 (2008).
Jones, D. T. et al. Tandem duplication producing a novel oncogenic BRAF fusion gene defines the majority of pilocytic astrocytomas. Cancer Res. 68, 8673–8677 (2008).
Bar, E. E., Lin, A., Tihan, T., Burger, P. C. & Eberhart, C. G. Frequent gains at chromosome 7q34 involving BRAF in pilocytic astrocytoma. J. Neuropathol. Exp. Neurol. 67, 878–887 (2008).
Rutkowski, S. et al. Treatment of early childhood medulloblastoma by postoperative chemotherapy alone. N. Engl. J. Med. 352, 978–986 (2005).
Sanders, R. P. et al. High-grade astrocytoma in very young children. Pediatr. Blood Cancer 49, 888–893 (2007).
Tekautz, T. M. et al. Atypical teratoid/rhabdoid tumors (ATRT): improved survival in children 3 years of age and older with radiation therapy and high-dose alkylator-based chemotherapy. J. Clin. Oncol. 23, 1491–1499 (2005).
Judkins, A. R. et al. Immunohistochemistry analysis of hSNFS/INI 1 in pediatric CNS neoplasms. Am. J. Surg. Path. 26, 644-650 (2004).
Biegel, J. A. et al. Alterations of the hSNFS/INI 1 gene in central nervous system atypical teratoid tumors and renal and extra renal rhabdoid tumors. Clin. Cancer. Res. 8, 3461–3467 (2002).
Maris, J. M. Recent advances in neuroblastoma. N. Engl. J. Med. 362, 2202–2211 (2010).
Baker, D. L. et al. Outcome after reduced chemotherapy for intermediate-risk neuroblastoma. N. Engl. J. Med. 363, 1313–1323 (2010).
Yu, A. L. et al. Anti-GD2 Antibody with GM-CSF, interleukin-2, and isotretinoin for neuroblastoma. N. Engl. J. Med. 363, 1324–1334 (2010).
Mossé, Y. P., Wood, A. & Maris, J. M. Inhibition of ALK signaling for cancer therapy. Clin. Cancer Res. 15, 5609–5614 (2009).
Maris, J. M. et al. Initial testing of the aurora kinase A inhibitor MLN8237 by the Pediatric Preclinical Testing Program (PPTP). Pediatr. Blood Cancer 55, 26–34 (2010).
Morton, C. L. et al. Initial testing of the replication competent Seneca Valley virus (NTX-010) by the pediatric preclinical testing program. Pediatr. Blood Cancer 55, 295–303 (2010).
Oberlin, O. et al. Prognostic factors in metastatic rhabdomyosarcomas: results of a pooled analysis from United States and European cooperative groups. J. Clin. Oncol. 26, 2384–2389 (2008).
Cao, L. et al. Addiction to elevated insulin-like growth factor I receptor and initial modulation of the AKT pathway define the responsiveness of rhabdomyosarcoma to the targeting antibody. Cancer Res. 68, 8039–8048 (2008).
Zibat, A. et al. Activation of the hedgehog pathway confers a poor prognosis in embryonal and fusion gene-negative alveolar rhabdomyosarcoma. Oncogene 29, 6323–6330 (2010).
Davicioni, E. et al. Identification of a PAX-FKHR gene expression signature that defines molecular classes and determines the prognosis of alveolar rhabdomyosarcomas. Cancer Res. 66, 6936–6946 (2006).
Taylor, J. G. 6th et al. Identification of FGFR4-activating mutations in human rhabdomyosarcomas that promote metastasis in xenotransplanted models. J. Clin. Invest. 119, 3395–3407 (2009).
Wachtel, M. & Schäfer, B. W. Targets for cancer therapy in childhood sarcomas. Cancer Treat. Rev. 36, 318–327 (2010).
Zeng, F. Y. et al. Glycogen synthase kinase 3 regulates PAX3–FKHR-mediated cell proliferation in human alveolar rhabdomyosarcoma cells. Biochem. Biophys. Res. Commun. 391, 1049–1055 (2010).
Davicioni, E. et al. Gene expression profiling for survival prediction in pediatric rhabdomyosarcomas: a report from the Children's Oncology Group. J. Clin. Oncol. 28, 1240–1246 (2010).
Demetri, G. D. et al. Efficacy and safety of imatinib mesylate in advanced gastrointestinal stromal tumors. N. Engl. J. Med. 347, 472–480 (2002).
Butrynski, J. E. et al. Crizotinib in ALK-rearranged inflammatory myofibroblastic tumor. N. Engl. J. Med. 363, 1727–1733 (2010).
Agaram, N. P. et al. Molecular characterization of pediatric gastrointestinal stromal tumors. Clin. Cancer Res. 14, 3204–3215 (2008).
Loh, M. L. et al. Treatment of infantile fibrosarcoma with chemotherapy and surgery: results from the Dana-Farber Cancer Institute and Children's Hospital, Boston. J. Pediatr. Hematol. Oncol. 24, 722–726 (2002).
Pappo, A. S. & Janeway, K. A. Pediatric gastrointestinal stromal tumors. Hematol. Oncol. Clin. North Am. 23, 15–34 (2009).
Janeway, K. A. et al. Defects in succinate dehydrogenase in gastrointestinal stromal tumors lacking KIT and PDGFRA mutation. Proc. Natl Acad. Sci. USA 108, 314–318 (2011).
Balamuth, N. J. & Womer, R. B. Ewing's sarcoma. Lancet Oncol. 11, 184–192 (2010).
Pappo, A. S. et al. Activity of R1507, a monoclonal antibody to the insulin-like growth factor-1 receptor (IGF1R) in patients with recurrent or refractory Ewing's sarcoma family of tumors (ESFT): results of a phase II SARC study [abstract]. J. Clin. Oncol. 28, a10000 (2010).
Carol, H. et al. Initial testing (stage 1) of the kinesin spindle protein inhibitor ispinesib by the pediatric preclinical testing program. Pediatr. Blood Cancer 53, 1255–1263 (2009).
Meyers, P. A. et al. Osteosarcoma: a randomized, prospective trial of the addition of ifosfamide and/or muramyl tripeptide to cisplatin, doxorubicin, and high-dose methotrexate. J. Clin. Oncol. 23, 2004–2011 (2005).
Khanna, C. Novel targets with potential therapeutic applications in osteosarcoma. Curr. Oncol. Rep. 10, 350–358 (2008).
Kolb, E. A. et al. R1507, a fully human monoclonal antibody targeting IGF-1R, is effective alone and in combination with rapamycin in inhibiting growth of osteosarcoma xenografts. Pediatr. Blood Cancer 55, 67–75 (2010).
Ahmed, N. et al. Immunotherapy for osteosarcoma: genetic modification of T cells overcomes low levels of tumor antigen expression. Mol. Ther. 17, 1779–1787 (2009).
Dunkel, I. J. et al. Intensive multimodality therapy for patients with stage 4a metastatic retinoblastoma. Pediatr. Blood Cancer 55, 55–59 (2010).
Broaddus, E., Topham, A. & Singh, A. D. Survival with retinoblastoma in the USA: 1975–2004. Br. J. Ophthalmol. 93, 24–27 (2009).
Shields, C. L. & Shields, J. A. Retinoblastoma management: advances in enucleation, intravenous chemoreduction, and intra-arterial chemotherapy. Curr. Opin. Ophthalmol. 21, 203–212 (2010).
Woo, K. I. & Harbour, J. W. Review of 676 second primary tumors in patients with retinoblastoma: association between age at onset and tumor type. Arch. Ophthalmol. 128, 865–870 (2010).
Nemeth, K. M. et al. Subconjunctival carboplatin and systemic topotecan treatment in preclinical models of retinoblastoma. Cancer 117, 421–434 (2010).
Abramson, D. H., Dunkel, I. J., Brodie, S. E., Marr, B. & Gobin, Y. P. Superselective ophthalmic artery chemotherapy as primary treatment for retinoblastoma (chemosurgery). Ophthalmology 117, 1623–1629 (2010).
Chévez-Barrios, P. et al. Response of retinoblastoma with vitreous tumor seeding to adenovirus-mediated delivery of thymidine kinase followed by ganciclovir. J. Clin. Oncol. 23, 7927–7935 (2005).
Carcaboso, A. M. et al. Episcleral implants for topotecan delivery to the posterior segment of the eye. Invest. Ophthalmol. Vis. Sci. 51, 2126–2134 (2010).
Laurie, N. A. et al. Inactivation of the p53 pathway in retinoblastoma. Nature 444, 61–66 (2006).
DiGiammarino, E. L. et al. A novel mechanism of tumorigenesis involving pH-dependent destabilization of a mutant p53 tetramer. Nat. Struct. Biol. 9, 12–16 (2002).
Hill, D. A. et al. DICER1 mutations in familial pleuropulmonary blastoma. Science 325, 965 (2009).
Collins, J. J. et al. The measurement of symptoms in children with cancer. J. Pain Symptom Manage. 19, 363–377 (2000).
Ullrich, C. K. et al. End-of-life experience of children undergoing stem cell transplantation for malignancy: parent and provider perspectives and patterns of care. Blood 115, 3879–3885 (2010).
Klassen, A. F. et al. Impact of caring for a child with cancer on parents' health-related quality of life. J. Clin. Oncol. 26, 5884–5889 (2008).
Maurer, S. H. et al. Decision making by parents of children with incurable cancer who opt for enrollment on a phase I trial compared with choosing a do not resuscitate/terminal care option. J. Clin. Oncol. 28, 3292–3298 (2010).
Dussel, V. et al. Looking beyond where children die: determinants and effects of planning a child's location of death. J. Pain Symptom Manage. 37, 33–43 (2009).
Kreicbergs, U. et al. Anxiety and depression in parents 4–9 years after the loss of a child owing to a malignancy: a population-based follow-up. Psychol. Med. 34, 1431–1441 (2004).
Bluebond-Langner, M., Belasco, J. B., Goldman, A. & Belasco, C. Understanding parents' approaches to care and treatment of children with cancer when standard therapy has failed. J. Clin. Oncol. 25, 2414–2419 (2007).
Mack, J. W. et al. Parents' views of cancer-directed therapy for children with no realistic chance for cure. J. Clin. Oncol. 26, 4759–4764 (2008).
Vickers, J., Thompson, A., Collins, G. S., Childs, M. & Hain, R. Place and provision of palliative care for children with progressive cancer: a study by the Paediatric Oncology Nurses' Forum/United Kingdom Children's Cancer Study Group Palliative Care Working Group. J. Clin. Oncol. 25, 4472–4476 (2007).
Wolfe, J. et al. Easing of suffering in children with cancer at the end of life: is care changing? J. Clin. Oncol. 26, 1717–1723 (2008).
Ferris, F. D. et al. Palliative cancer care a decade later: accomplishments, the need, next steps—from the American Society of Clinical Oncology. J. Clin. Oncol. 27, 3052–3058 (2009).
Kane, J. R. Pediatric palliative care moving forward: empathy, competence, quality, and the need for systematic change. J. Palliat. Med. 9, 847–849 (2006).
Temel, J. et al. Early palliative care for patients with metastatic non-small-cell lung cancer. N. Engl. J. Med. 363, 733–742 (2010).
Baker, J. N., Barfield, R., Hinds, P. S. & Kane, J. R. A process to facilitate decision making in pediatric stem cell transplantation: the individualized care planning and coordination model. Biol. Blood Marrow Transplant. 13, 245–254 (2007).
Baker, J. N. et al. Integration of palliative care practices into the ongoing care of children with cancer: individualized care planning and coordination. Pediatr. Clin. North Am. 55, 223–250 (2008).
Hui, D. et al. Availability and integration of palliative care at US cancer centers. JAMA 303, 1054–1061 (2010).
Acknowledgements
This project was supported in part by grant CA21765 and GM092666 from the National Institutes of Health, and by the American Lebanese Syrian Associated charities. C. P. Vega, University of California, Irvine, CA, is the author of and is solely responsible for the content of the learning objectives, questions and answers of the Medscape, LLC-accredited continuing medical education activity associated with this article.
Author information
Authors and Affiliations
Contributions
All authors were involved in the research of data, discussion of content, writing the Review and revising the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Pui, CH., Gajjar, A., Kane, J. et al. Challenging issues in pediatric oncology. Nat Rev Clin Oncol 8, 540–549 (2011). https://doi.org/10.1038/nrclinonc.2011.95
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrclinonc.2011.95
This article is cited by
-
Comprehensive analysis of mutational signatures reveals distinct patterns and molecular processes across 27 pediatric cancers
Nature Cancer (2023)
-
3D genome mapping identifies subgroup-specific chromosome conformations and tumor-dependency genes in ependymoma
Nature Communications (2023)
-
Circulating tumor DNA profiling for childhood brain tumors: Technical challenges and evidence for utility
Laboratory Investigation (2022)
-
Central nervous system tumors in children under 5 years of age: a report on treatment burden, survival and long-term outcomes
Journal of Neuro-Oncology (2022)
-
Systems pharmacogenomics identifies novel targets and clinically actionable therapeutics for medulloblastoma
Genome Medicine (2021)