Key Points
-
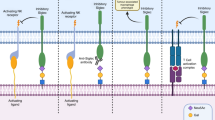
Heparan-sulphate glycosaminoglycans (HSGAGs) act at the cell–extracellular-matrix (ECM) interface to modulate cell signalling, thereby regulating how a cell perceives its environment.
-
HSGAGs interact with various extracellular signalling molecules: growth factors, morphogens, enzymes and chemokines. The specificity of these interactions is dependent on HSGAG sequence, spacing of binding sites and the three-dimensional structure of the HSGAG chain.
-
HSGAGs, depending on location and sequence, impinge on tumour onset and progression in various ways, some of which are pro-tumorigenic and others of which are anti-tumorigenic.
-
HSGAGs at the tumour-cell surface actively modulate the tumorigenic process by regulating autocrine signalling loops that lead to unregulated cell growth.
-
HSGAGs impinge on how an organism responds to a growing tumour, including the recruitment of cells of the immune system to the tumour site, formation of a fibrin shell around the tumour that acts as a protective barrier and development of new blood vessels to the site of the growing tumour.
-
Compelling clinical evidence indicates that pharmacological doses of heparin, a highly sulphated HSGAG, can have a marked effect on tumour metastasis. Clinical trials have been designed to determine the exact benefits of heparin therapy in cancer.
-
In addition, the low-molecular-weight heparins (LMWHs) — a series of heparin fragments that share many of heparin's activities, including its anticoagulant effect, but lack several of its side effects — might show even greater antitumour activity.
-
The advent of HSGAG sequencing technologies promises to usher in a new generation of LMWHs with potent antitumour activity.
Abstract
Cell-surface/extracellular-matrix heparan-sulphate glycosaminoglycans (HSGAGs) are complex polysaccharides that are ubiquitous in nature, and that regulate several aspects of cancer biology, including tumorigenesis, tumour progression and metastasis. Recently gained insights into the structure of HSGAGs have extended our understanding of their role in the oncogenic process. At present, clinical trials are examining the anticancer properties of exogenous highly sulphated HSGAGs, including heparin and low-molecular-weight heparins, in addition to small oligosaccharide heparin mimetics. Combined with our more intricate understanding of HSGAG structure, this emerging structure–activity approach opens exciting avenues for the generation of polysaccharide-based anticancer therapeutics.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Perrimon, N. & Bernfield, M. Specificities of heparan sulphate proteoglycans in developmental processes. Nature 404, 725–728 (2000).
Conrad, H. E. Heparin-Binding Proteins (Academic Press, San Diego, 1998).This book describes what is known about the structure and function of HSGAGs, as well as tools that have been developed to study structure–function relationships.
Liu, D., Shriver, Z., Qi, Y., Venkataraman, G. & Sasisekharan, R. Dynamic regulation of tumor growth and metastasis by heparan sulfate glycosaminoglycans. Semin. Thromb. Hemost. 28, 67–78 (2002).
Gallagher, J. T. Heparan sulfate: growth control with a restricted sequence menu. J. Clin. Invest. 108, 357–361 (2001).
Esko, J. D. & Lindahl, U. Molecular diversity of heparan sulfate. J. Clin. Invest. 108, 169–173 (2001).
Turnbull, J., Powell, A. & Guimond, S. Heparan sulfate: decoding a dynamic multifunctional cell regulator. Trends Cell Biol. 11, 75–82 (2001).
Sasisekharan, R. & Venkataraman, G. Heparin and heparan sulfate: biosynthesis, structure and function. Curr. Opin. Chem. Biol. 4, 626–631 (2000).
Faham, S., Linhardt, R. J. & Rees, D. C. Diversity does make a difference: fibroblast growth factor-heparin interactions. Curr. Opin. Struct. Biol. 8, 578–586 (1998).
Jin, L. et al. The anticoagulant activation of antithrombin by heparin. Proc. Natl Acad. Sci. USA 94, 14683–14688 (1997).
Schlessinger, J. et al. Crystal structure of a ternary FGF–FGFR–heparin complex reveals a dual role for heparin in FGFR binding and dimerization. Mol. Cell 6, 743–750 (2000).
DiGabriele, A. D. et al. Structure of a heparin-linked biologically active dimer of fibroblast growth factor. Nature 393, 812–817 (1998).
Mulloy, B. & Linhardt, R. J. Order out of complexity: protein structures that interact with heparin. Curr. Opin. Struct. Biol. 11, 623–628 (2001).
Chang, Z., Meyer, K., Rapraeger, A. C. & Friedl, A. Differential ability of heparan sulfate proteoglycans to assemble the fibroblast growth factor receptor complex in situ. FASEB J. 14, 137–144 (2000).
Nurcombe, V., Ford, M. D., Wildschut, J. A. & Bartlett, P. F. Developmental regulation of neural response to FGF1 and FGF2 by heparan sulfate proteoglycan. Science 260, 103–106 (1993).
Dhoot, G. K. et al. Regulation of Wnt signaling and embryo patterning by an extracellular sulfatase. Science 293, 1663–1666 (2001).Shows that cells actively modulate their HSGAG coat to influence morphogen gradients and, therefore, pattern formation.
Cosgrove, R. H., Zacharski, L. R., Racine, E. & Andersen, J. C. Improved cancer mortality with low-molecular-weight heparin treatment: a review of the evidence. Semin. Thromb. Hemost. 28, 79–88 (2002).
Vlodavsky, I. & Friedmann, Y. Molecular properties and involvement of heparanase in cancer metastasis and angiogenesis. J. Clin. Invest. 108, 341–347 (2001).
Varki, N. M. & Varki, A. Heparin inhibition of selectin-mediated interactions during the hematogenous phase of carcinoma metastasis: rationale for clinical studies in humans. Semin. Thromb. Hemost. 28, 53–66 (2002).
Liu, D., Shriver, Z., Venkataraman, G., El Shabrawi, Y. & Sasisekharan, R. Tumor cell surface heparan sulfate as cryptic promoters or inhibitors of tumor growth and metastasis. Proc. Natl Acad. Sci. USA 99, 568–573 (2002).Presents the novel observation that HSGAGs of differing structure can have opposing roles in mediating the processes of primary tumour growth and metastasis.
Blackhall, F. H., Merry, C. L., Davies, E. J. & Jayson, G. C. Heparan sulfate proteoglycans and cancer. Br. J. Cancer 85, 1094–1098 (2001).
Xiang, Y. Y., Ladeda, V. & Filmus, J. Glypican-3 expression is silenced in human breast cancer. Oncogene 20, 7408–7412 (2001).
Filmus, J. Glypicans in growth control and cancer. Glycobiology 11, 19R–23R (2001).
Sanderson, R. D. Heparan sulfate proteoglycans in invasion and metastasis. Semin. Cell Dev. Biol. 12, 89–98 (2001).
Jayson, G. C. et al. Heparan sulfate undergoes specific structural changes during the progression from human colon adenoma to carcinoma in vitro. J. Biol. Chem. 273, 51–57 (1998).
DeBaun, M. R., Ess, J. & Saunders, S. Simpson–Golabi–Behmel syndrome: progress toward understanding the molecular basis for overgrowth, malformation, and cancer predisposition. Mol. Genet. Metab. 72, 279–286 (2001).
Mundhenke, C., Meyer, K., Drew, S. & Friedl, A. Heparan sulfate proteoglycans as regulators of fibroblast growth factor-2 receptor binding in breast carcinomas. Am. J. Pathol. 160, 185–194 (2002).
Kreuger, J., Salmivirta, M., Sturiale, L., Gimenez-Gallego, G. & Lindahl, U. Sequence analysis of heparan sulfate epitopes with graded affinities for fibroblast growth factors 1 and 2. J. Biol. Chem. 276, 30744–30752 (2001).
Iozzo, R. V. & San Antonio, J. D. Heparan sulfate proteoglycans: heavy hitters in the angiogenesis arena. J. Clin. Invest. 108, 349–355 (2001).
Folkman, J. Angiogenesis-dependent diseases. Semin. Oncol. 28, 536–542 (2001).
Sasisekharan, R., Moses, M. A., Nugent, M. A., Cooney, C. L. & Langer, R. Heparinase inhibits neovascularization. Proc. Natl Acad. Sci. USA 91, 1524–1528 (1994).
Karumanchi, S. A. et al. Cell surface glypicans are low-affinity endostatin receptors. Mol. Cell 7, 811–822 (2001).
Smorenburg, S. M. & Van Noorden, C. J. The complex effects of heparins on cancer progression and metastasis in experimental studies. Pharmacol. Rev. 53, 93–105 (2001).
Tovari, J. et al. Role of sinusoidal heparan sulfate proteoglycan in liver metastasis formation. Int. J. Cancer 71, 825–831 (1997).
Hulett, M. D. et al. Cloning of mammalian heparanase, an important enzyme in tumor invasion and metastasis. Nature Med. 5, 803–809 (1999).
Vlodavsky, I. et al. Mammalian heparanase: gene cloning, expression and function in tumor progression and metastasis. Nature Med. 5, 793–802 (1999).These two studies report the cloning and characterization of the human heparanase gene. Heparanase is an enzyme that is produced by cancer cells that was found to be a key factor or switch by which a tumour becomes metastatic. This has led to a substantial effort to identify inhibitors of human heparanase as a therapeutic strategy to combat metastasis.
Kakkar, A. K. & Williamson, R. C. Antithrombotic therapy in cancer. BMJ 318, 1571–1572 (1999).
Zacharski, L. R. & Ornstein, D. L. Heparin and cancer. Thromb. Haemost. 80, 10–23 (1998).
Zacharski, L. R., Ornstein, D. L. & Mamourian, A. C. Low-molecular-weight heparin and cancer. Semin. Thromb. Hemost. 26, 69–77 (2000).Definitive review of the effects of low-molecular-weight heparin on cancer progression.
Goger, B. et al. Different affinities of glycosaminoglycan oligosaccharides for monomeric and dimeric interleukin-8: a model for chemokine regulation at inflammatory sites. Biochemistry 41, 1640–1646 (2002).
Koopmann, W., Ediriwickrema, C. & Krangel, M. S. Structure and function of the glycosaminoglycan binding site of chemokine macrophage-inflammatory protein-1β. J. Immunol. 163, 2120–2127 (1999).
Vlodavsky, I. et al. Mammalian heparanase: involvement in cancer metastasis, angiogenesis and normal development. Semin. Cancer Biol. 12, 121–129 (2002).
Iversen, P. O., Sorensen, D. R. & Benestad, H. B. Inhibitors of angiogenesis selectively reduce the malignant cell load in rodent models of human myeloid leukemias. Leukemia 16, 376–381 (2002).
Parish, C. R., Freeman, C., Brown, K. J., Francis, D. J. & Cowden, W. B. Identification of sulfated oligosaccharide-based inhibitors of tumor growth and metastasis using novel in vitro assays for angiogenesis and heparanase activity. Cancer Res. 59, 3433–3441 (1999).
Bentolila, A. et al. Poly(N-acryl amino acids): a new class of biologically active polyanions. J. Med. Chem. 43, 2591–2600 (2000).
Naggi, A. et al. Toward a biotechnological heparin through combined chemical and enzymatic modification of the Escherichia coli K5 polysaccharide. Semin. Thromb. Hemost. 27, 437–443 (2001).
Belting, M. et al. Tumor attenuation by combined heparan sulfate and polyamine depletion. Proc. Natl Acad. Sci. USA 99, 371–376 (2002).
Merry, C. L., Lyon, M., Deakin, J. A., Hopwood, J. J. & Gallagher, J. T. Highly sensitive sequencing of the sulfated domains of heparan sulfate. J. Biol. Chem. 274, 18455–18462 (1999).
Turnbull, J. E., Hopwood, J. J. & Gallagher, J. T. A strategy for rapid sequencing of heparan sulfate and heparin saccharides. Proc. Natl Acad. Sci. USA 96, 2698–2703 (1999).
Vives, R. R. et al. Sequence analysis of heparan sulphate and heparin oligosaccharides. Biochem. J. 339, 767–773 (1999).
Venkataraman, G., Shriver, Z., Raman, R. & Sasisekharan, R. Sequencing complex polysaccharides. Science 286, 537–542 (1999).
Keiser, N., Venkataraman, G., Shriver, Z. & Sasisekharan, R. Direct isolation and sequencing of specific protein-binding glycosaminoglycans. Nature Med. 7, 123–128 (2001).
Borsig, L. et al. Heparin and cancer revisited: mechanistic connections involving platelets, P-selectin, carcinoma mucins, and tumor metastasis. Proc. Natl Acad. Sci. USA 98, 3352–3357 (2001).Anecdotal evidence has indicated that pharmacological doses of low-molecular-weight heparins serve a protective role against metastasis. This paper proposes that heparins interfere with the selectin-mediated interaction of cancer cells with their stroma.
Petitou, M. et al. Experimental proof for the structure of a thrombin-inhibiting heparin molecule. Chemistry 7, 858–873 (2001).
Ho, G., Broze, G. J. Jr & Schwartz, A. L. Role of heparan sulfate proteoglycans in the uptake and degradation of tissue factor pathway inhibitor-coagulation factor Xa complexes. J. Biol. Chem. 272, 16838–16844 (1997).
Nugent, M. A. & Iozzo, R. V. Fibroblast growth factor-2. Int. J. Biochem. Cell Biol. 32, 115–120 (2000).
Derksen, P. W. et al. Cell surface proteoglycan syndecan-1 mediates hepatocyte growth factor binding and promotes Met signaling in multiple myeloma. Blood 99, 1405–1410 (2002).
Lin, X. & Perrimon, N. Dally cooperates with Drosophila Frizzled 2 to transduce Wingless signalling. Nature 400, 281–284 (1999).
Tsuda, M. et al. The cell-surface proteoglycan Dally regulates Wingless signalling in Drosophila. Nature 400, 276–280 (1999).
Ma, Y. Q. & Geng, J. G. Heparan sulfate-like proteoglycans mediate adhesion of human malignant melanoma A375 cells to P-selectin under flow. J. Immunol. 165, 558–565 (2000).
Hoffman, M. P. et al. Cell type-specific differences in glycosaminoglycans modulate the biological activity of a heparin-binding peptide (RKRLQVQLSIRT) from the G domain of the laminin-α1 chain. J. Biol. Chem. 276, 22077–22085 (2001).
Utani, A. et al. A unique sequence of the laminin-α 3G domain binds to heparin and promotes cell adhesion through syndecan-2 and -4. J. Biol. Chem. 276, 28779–28788 (2001).
Lundmark, K. et al. Perlecan inhibits smooth muscle cell adhesion to fibronectin: role of heparan sulfate. J. Cell Physiol. 188, 67–74 (2001).
Acknowledgements
The authors would like to acknowledge financial assistance from the Burroughs Wellcome Foundation, the Arnold and Mabel Beckman Foundation, the CapCure Foundation and the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Related links
Related links
DATABASES
Cancer.gov
LocusLink
platelet-derived growth factor
OMIM
Simpson–Golabi–Behmel syndrome
FURTHER INFORMATION
Glossary
- PROTEOGLYCAN
-
A glycoprotein that consists of a core protein sequence and glycosaminoglycan extensions. Proteoglycans that contain heparan-sulphate glycosaminoglycan side chains are called heparan-sulphate proteoglycans.
- SYNDECAN
-
A membrane-bound proteoglycan that contains a large extracellular domain with attached heparan-sulphate glycosaminoglycan chains, a conserved transmembrane domain and a small cytoplasmic domain.
- GLYPICAN
-
A heparan-sulphate proteoglycan that is tethered to the membrane by a glycosylphosphatidylinositol anchor. The core protein contains a conserved cysteine-rich globular region and several glycosaminoglycan attachment sites.
- PERLECAN
-
A proteoglycan that is typically extruded into the extracellular space.
- HEPARIN
-
A highly sulphated member of the heparan-sulphate glycosaminoglycan family. Typically present in mast cells, where it acts as a storage depot for proteases, heparin is used pharmacologically as an anticoagulant.
- PROPERTY-ENCODED NOMENCLATURE
-
(PEN). A rational system for defining a polymer that is based on the properties of its monomeric units. This system forms the basis for a computationally aided sequencing approach for heparan-sulphate glycosaminoglycan complex oligosaccharides.
- ANTITHROMBIN III
-
(AT-III). An inhibitor of the coagulation cascade, specifically Factor Xa and Factor IIa (thrombin). Binding of AT-III to a specific pentasaccharide sequence in heparan sulphate results in a conformational change in AT-III, increasing its anticoagulant activity by orders of magnitude. Factor Xa is a serine protease of the coagulation cascade. Factor Xa activates thrombin — the penultimate step of the coagulation cascade.
- MACROGLOSSIA
-
Tongue enlargement, leading to functional and cosmetic problems.
- MACROSOMIA
-
Atypically large body size.
- SULPHATION PATTERN
-
Each HSGAG disaccharide unit can be differentially sulphated at four possible positions. On the uronic acid, the 2-O position might be sulphated or unsulphated. For the glucosamine, the 6-O and 3-O positions might also be sulphated or unsulphated. Finally, the N-position of the glucosamine can be N-sulphated, acetylated or unsubstituted.
- LOW-MOLECULAR-WEIGHT HEPARIN
-
(LMWH). Developed to maintain the potent anticoagulant affect of heparin but to reduce the number of side effects. LMWHs are generated by enzymatic or chemical means.
- THROMBIN
-
Also known as Factor IIa, it is the penultimate factor of the coagulation cascade. Thrombin converts fibrinogen into fibrin, which is ultimately responsible for clot formation.
Rights and permissions
About this article
Cite this article
Sasisekharan, R., Shriver, Z., Venkataraman, G. et al. Roles of heparan-sulphate glycosaminoglycans in cancer. Nat Rev Cancer 2, 521–528 (2002). https://doi.org/10.1038/nrc842
Issue Date:
DOI: https://doi.org/10.1038/nrc842
This article is cited by
-
Xylosyltransferase I mediates the synthesis of proteoglycans with long glycosaminoglycan chains and controls chondrocyte hypertrophy and collagen fibers organization of in the growth plate
Cell Death & Disease (2023)
-
Discrimination of deletion to point cytokine mutants based on an array of cross-reactive receptors mimicking protein recognition by heparan sulfate
Analytical and Bioanalytical Chemistry (2022)
-
Heparanase (HPSE) gene polymorphism (rs12503843) contributes as a risk factor for hepatocellular carcinoma (HCC): a pilot study among Egyptian patients
Journal of Genetic Engineering and Biotechnology (2021)
-
Heparanase: a potential marker of worse prognosis in estrogen receptor-positive breast cancer
npj Breast Cancer (2021)
-
Endocan, a novel inflammatory marker, is upregulated in human chondrocytes stimulated with IL-1 beta
Molecular and Cellular Biochemistry (2021)