Key Points
-
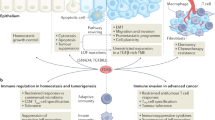
TGFβ signalling is tumour suppressive in epithelial cells, whereas it can promote invasion and metastasis during the later stages of carcinoma progression.
-
During tumour progression, tumour cells frequently lose the growth-inhibitory response to TGFβ, and this is associated with an increased expression of TGFβ in the microenvironment.
-
TGFβ-mediated regulation in the tumour microenvironment can be attributed to many factors, including those that involve cell-autonomous signalling, stromal–epithelial interactions, inflammation, immune evasion and angiogenesis.
-
Cell-autonomous TGFβ signalling can cause epithelial–mesenchymal transitions (EMT) in carcinoma cells, which increase invasion and metastasis.
-
Conversely, the abrogation of carcinoma-cell-autonomous TGFβ signalling can increase metastasis in the apparent absence of EMT.
-
Together, the cell-type-dependent and context-dependent effects of TGFβ signalling contribute to the regulation of tumour initiation, progression and metastasis.
-
Despite the complex nature of TGFβ-mediated regulatory signalling in the tumour microenvironment, many aspects of signalling through this pathway have been targeted for therapeutic intervention using systemic and cell-specific strategies, with some indications of efficacy.
Abstract
Transforming growth factor-β (TGFβ) signalling regulates cancer through mechanisms that function either within the tumour cell itself or through host–tumour cell interactions. Studies of tumour-cell-autonomous TGFβ effects show clearly that TGFβ signalling has a mechanistic role in tumour suppression and tumour promotion. In addition, factors in the tumour microenvironment, such as fibroblasts, immune cells and the extracellular matrix, influence the ability of TGFβ to promote or suppress carcinoma progression and metastasis. The complex nature of TGFβ signalling and crosstalk in the tumour microenvironment presents a unique challenge, and an opportunity to develop therapeutic intervention strategies for targeting cancer.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Siegel, P. M. & Massague, J. Cytostatic and apoptotic actions of TGF-β in homeostasis and cancer. Nature Rev. Cancer 3, 807–821 (2003).
Derynck, R. & Zhang, Y. E. Smad-dependent and Smad-independent pathways in TGF-β family signalling. Nature 425, 577–584 (2003).
Bierie, B. & Moses, H. L. TGF-β and cancer. Cytokine Growth Factor Rev 17, 29–40 (2006).
Lin, H. Y., Wang, X. F., Ng-Eaton, E., Weinberg, R. A. & Lodish, H. F. Expression cloning of the TGF-β type II receptor, a functional transmembrane serine/threonine kinase. Cell 68, 775–785 (1992). Describes the initial cloning and characterization of the type II TGFβ receptor. The binding affinity of TGFβ1 and TGFβ2 was shown, along with an analysis of this receptor as a functional serine and threonine kinase.
Wang, X. F. et al. Expression cloning and characterization of the TGF-β type III receptor. Cell 67, 797–805 (1991). Describes the initial cloning and characterization of a type III TGFβ receptor. It was shown that the cloned type III receptor was able to bind TGFβ1 and increase the ligand affinity for the type II TGFβ receptor.
Yu, Q. & Stamenkovic, I. Cell surface-localized matrix metalloproteinase-9 proteolytically activates TGF-β and promotes tumor invasion and angiogenesis. Genes Dev. 14, 163–176 (2000).
Munger, J. S. et al. The integrin-α v β 6 binds and activates latent TGF β 1: a mechanism for regulating pulmonary inflammation and fibrosis. Cell 96, 319–328 (1999).
Lin, H. Y. et al. The soluble exoplasmic domain of the type II transforming growth factor (TGF)-β receptor. A heterogeneously glycosylated protein with high affinity and selectivity for TGF-β ligands. J. Biol. Chem. 270, 2747–2754 (1995).
Crawford, S. E. et al. Thrombospondin-1 is a major activator of TGF-β1 in vivo. Cell 93, 1159–1170 (1998).
Moustakas, A. et al. The transforming growth factor-β receptors types I, II, and III form hetero-oligomeric complexes in the presence of ligand. J. Biol. Chem. 268, 22215–22218 (1993).
Gilboa, L., Wells, R. G., Lodish, H. F. & Henis, Y. I. Oligomeric structure of type I and type II transforming growth factor-β receptors: homodimers form in the ER and persist at the plasma membrane. J. Cell. Biol. 140, 767–777 (1998).
Goumans, M. J. et al. Activin receptor-like kinase (ALK)1 is an antagonistic mediator of lateral TGFβ/ALK5 signaling. Mol. Cell 12, 817–828 (2003).
Wrana, J. L. et al. TGF β signals through a heteromeric protein kinase receptor complex. Cell 71, 1003–1014 (1992).
Luo, K. & Lodish, H. F. Signaling by chimeric erythropoietin-TGF-β receptors: homodimerization of the cytoplasmic domain of the type I TGF-β receptor and heterodimerization with the type II receptor are both required for intracellular signal transduction. EMBO J. 15, 4485–4496 (1996).
Feng, X. H. & Derynck, R. Ligand-independent activation of transforming growth factor (TGF) β signaling pathways by heteromeric cytoplasmic domains of TGF-β receptors. J. Biol. Chem. 271, 13123–13129 (1996).
Olivey, H. E., Mundell, N. A., Austin, A. F. & Barnett, J. V. Transforming growth factor-β stimulates epithelial-mesenchymal transformation in the proepicardium. Dev. Dyn. 235, 50–59 (2006).
Shi, Y. & Massague, J. Mechanisms of TGF-β signaling from cell membrane to the nucleus. Cell 113, 685–700 (2003).
Moustakas, A. & Heldin, C. H. Non-Smad TGF-β signals. J. Cell Sci. 118, 3573–3584 (2005).
Barrios-Rodiles, M. et al. High-throughput mapping of a dynamic signaling network in mammalian cells. Science 307, 1621–1625 (2005). The TGFβ pathway has been targeted for interactome mapping. This paper and supplementary material outlines the results from approximately 12,000 individual experimental reactions that resulted in the identification of a large number of new interactions.
Feng, X. H. & Derynck, R. Specificity and versatility in tgf-β signaling through Smads. Annu. Rev. Cell Dev. Biol. 21, 659–693 (2005).
Massague, J. How cells read TGF-β signals. Nature Rev. Mol. Cell Biol. 1, 169–178 (2000).
Akhurst, R. J. & Derynck, R. TGF-β signaling in cancer-a double-edged sword. Trends Cell Biol. 11, S44–S51 (2001).
Derynck, R., Akhurst, R. J. & Balmain, A. TGF-β signaling in tumor suppression and cancer progression. Nature Genet. 29, 117–129 (2001).
Lin, H. K., Bergmann, S. & Pandolfi, P. P. Cytoplasmic PML function in TGF-β signalling. Nature 431, 205–211 (2004).
Zhang, L. et al. A role for MEK kinase 1 in TGF-β/activin-induced epithelium movement and embryonic eyelid closure. EMBO J. 22, 4443–4454 (2003).
Chiu, C. et al. TGF-β-induced p38 activation is mediated by Rac1-regulated generation of reactive oxygen species in cultured human keratinocytes. Int. J. Mol. Med. 8, 251–255 (2001).
Edlund, S., Landstrom, M., Heldin, C. H. & Aspenstrom, P. Smad7 is required for TGF-β-induced activation of the small GTPase Cdc42. J. Cell Sci. 117, 1835–1847 (2004).
Perlman, R., Schiemann, W. P., Brooks, M. W., Lodish, H. F. & Weinberg, R. A. TGF-β-induced apoptosis is mediated by the adapter protein Daxx that facilitates JNK activation. Nature Cell Biol. 3, 708–714 (2001).
Wilkes, M. C., Murphy, S. J., Garamszegi, N. & Leof, E. B. Cell-type-specific activation of PAK2 by transforming growth factor-β independent of Smad2 and Smad3. Mol. Cell Biol. 23, 8878–8889 (2003).
Mulder, K. M. & Morris, S. L. Activation of p21ras by transforming growth factor-β in epithelial cells. J. Biol. Chem. 267, 5029–5031 (1992).
Yi, J. Y., Shin, I. & Arteaga, C. L. Type I transforming growth factor-β receptor binds to and activates phosphatidylinositol 3-kinase. J. Biol. Chem. 280, 10870–10876 (2005).
Ozdamar, B. et al. Regulation of the polarity protein Par6 by TGFβ receptors controls epithelial cell plasticity. Science 307, 1603–1609 (2005).
Bhowmick, N. A. et al. Transforming growth factor-β1 mediates epithelial to mesenchymal transdifferentiation through a RhoA-dependent mechanism. Mol. Biol. Cell 12, 27–36 (2001).
Shibuya, H. et al. TAB1: an activator of the TAK1 MAPKKK in TGF-β signal transduction. Science 272, 1179–1182 (1996).
Yamaguchi, K. et al. Identification of a member of the MAPKKK family as a potential mediator of TGF-β signal transduction. Science 270, 2008–2011 (1995).
Petritsch, C., Beug, H., Balmain, A. & Oft, M. TGF-β inhibits p70 S6 kinase via protein phosphatase 2A to induce G(1) arrest. Genes Dev. 14, 3093–3101 (2000).
Levy, L. & Hill, C. S. Alterations in components of the TGF-β superfamily signaling pathways in human cancer. Cytokine Growth Factor Rev. 17, 41–58 (2006).
Markowitz, S. et al. Inactivation of the type II TGF-β receptor in colon cancer cells with microsatellite instability. Science 268, 1336–1338 (1995). This is the first conclusive study that links inactivation of the type II TGFβ receptor to cancer.
Grady, W. M. Genomic instability and colon cancer. Cancer Metastasis Rev. 23, 11–27 (2004).
Pasche, B. Role of transforming growth factor-β in cancer. J. Cell. Physiol. 186, 153–168 (2001).
Bacon, A. L., Farrington, S. M. & Dunlop, M. G. Mutation frequency in coding and non-coding repeat sequences in mismatch repair deficient cells derived from normal human tissue. Oncogene 20, 7464–7471 (2001).
Kim, S. J., Im, Y. H., Markowitz, S. D. & Bang, Y. J. Molecular mechanisms of inactivation of TGF-β receptors during carcinogenesis. Cytokine Growth Factor Rev. 11, 159–168 (2000).
Kang, S. H. et al. Transcriptional repression of the transforming growth factor-β type I receptor gene by DNA methylation results in the development of TGF-β resistance in human gastric cancer. Oncogene 18, 7280–7286 (1999).
Lebrin, F., Deckers, M., Bertolino, P. & Ten Dijke, P. TGF-β receptor function in the endothelium. Cardiovasc Res. 65, 599–608 (2005).
Pangas, S. A. & Matzuk, M. M. Genetic models for transforming growth factor-β superfamily signaling in ovarian follicle development. Mol. Cell. Endocrinol. 225, 83–91 (2004).
Guy, C. T. et al. Expression of the neu proto-oncogene in the mammary epithelium of transgenic mice induces metastatic disease. Proc. Natl Acad. Sci. USA 89, 10578–10582 (1992).
Guy, C. T., Cardiff, R. D. & Muller, W. J. Induction of mammary tumors by expression of polyomavirus middle T oncogene: a transgenic mouse model for metastatic disease. Mol. Cell Biol. 12, 954–961 (1992).
Matsui, Y., Halter, S. A., Holt, J. T., Hogan, B. L. & Coffey, R. J. Development of mammary hyperplasia and neoplasia in MMTV-TGF-α transgenic mice. Cell 61, 1147–1155 (1990).
Hennighausen, L. & Robinson, G. W. Information networks in the mammary gland. Nature Rev. Mol. Cell Biol. 6, 715–725 (2005).
Shackleton, M. et al. Generation of a functional mammary gland from a single stem cell. Nature 439, 84–88 (2006). Although it is not directly related to TGFβ signalling in cancer, this high-impact paper outlines a new method whereby a single mammary stem cell can be isolated that is able to produce myoepithelium, ductal and alveolar epithelium. A single cell from this population was able to reconstitute all the epithelial and myoepithelial cell types necessary to reconstitute a functional mammary gland when transplanted into a cleared mammary fat pad.
Joseph, H., Gorska, A. E., Sohn, P., Moses, H. L. & Serra, R. Overexpression of a kinase-deficient transforming growth factor-β type II receptor in mouse mammary stroma results in increased epithelial branching. Mol. Biol. Cell 10, 1221–1234 (1999).
Nguyen, A. V. & Pollard, J. W. Transforming growth factor β3 induces cell death during the first stage of mammary gland involution. Development 127, 3107–3118 (2000).
Pierce, D. F., Jr. et al. Inhibition of mammary duct development but not alveolar outgrowth during pregnancy in transgenic mice expressing active TGF-β 1. Genes Dev. 7, 2308–2317 (1993).
Boulanger, C. A. & Smith, G. H. Reducing mammary cancer risk through premature stem cell senescence. Oncogene 20, 2264–2272 (2001).
Boulanger, C. A., Wagner, K. U. & Smith, G. H. Parity-induced mouse mammary epithelial cells are pluripotent, self-renewing and sensitive to TGF-β1 expression. Oncogene 24, 552–560 (2005).
Jhappan, C. et al. Targeting expression of a transforming growth factor β 1 transgene to the pregnant mammary gland inhibits alveolar development and lactation. EMBO J. 12, 1835–1845 (1993).
Kordon, E. C. et al. Ectopic TGF-β1 expression in the secretory mammary epithelium induces early senescence of the epithelial stem cell population. Dev. Biol. 168, 47–61 (1995).
Pierce, D. F., Jr. et al. Mammary tumor suppression by transforming growth factor-β1 transgene expression. Proc. Natl Acad. Sci. USA 92, 4254–4258 (1995).
Muraoka, R. S. et al. Increased malignancy of Neu-induced mammary tumors overexpressing active transforming growth factor β1. Mol. Cell. Biol. 23, 8691–8703 (2003).
Muraoka-Cook, R. S. et al. Conditional overexpression of active transforming growth factor β1 in vivo accelerates metastases of transgenic mammary tumors. Cancer Res. 64, 9002–9011 (2004).
Gorska, A. E. et al. Transgenic mice expressing a dominant-negative mutant type II transforming growth factor-β receptor exhibit impaired mammary development and enhanced mammary tumor formation. Am. J. Pathol. 163, 1539–1549 (2003).
Lenferink, A. E., Magoon, J., Pepin, M. C., Guimond, A. & O'Connor-McCourt, M. D. Expression of TGF-β type II receptor antisense RNA impairs TGF-β signaling in vitro and promotes mammary gland differentiation in vivo. Int. J. Cancer 107, 919–928 (2003).
Muraoka, R. S. et al. Blockade of TGF-β inhibits mammary tumor cell viability, migration, and metastases. J. Clin. Invest. 109, 1551–1559 (2002).
Forrester, E. et al. Effect of conditional knockout of the type II TGF-β receptor gene in mammary epithelia on mammary gland development and polyomavirus middle T antigen induced tumor formation and metastasis. Cancer Res. 65, 2296–2302 (2005). Outlined for the first time the effect of complete conditional type II TGFβ receptor ablation in the context of mammary development and tumourigenesis.
Ewan, K. B. et al. Latent transforming growth factor-β activation in mammary gland: regulation by ovarian hormones affects ductal and alveolar proliferation. Am. J. Pathol. 160, 2081–2093 (2002).
Ewan, K. B. et al. Proliferation of estrogen receptor-α-positive mammary epithelial cells is restrained by transforming growth factor-β1 in adult mice. Am. J. Pathol. 167, 409–417 (2005).
Tang, B. et al. TGF-β switches from tumor suppressor to prometastatic factor in a model of breast cancer progression. J. Clin. Invest. 112, 1116–1124 (2003).
Muraoka-Cook, R. S. et al. Activated type I TGFβ receptor kinase enhances the survival of mammary epithelial cells and accelerates tumor progression. Oncogene (2005).
Oft, M., Heider, K. H. & Beug, H. TGFβ signaling is necessary for carcinoma cell invasiveness and metastasis. Curr. Biol. 8, 1243–1252 (1998).
Siegel, P. M., Shu, W., Cardiff, R. D., Muller, W. J. & Massague, J. Transforming growth factor β signaling impairs Neu-induced mammary tumorigenesis while promoting pulmonary metastasis. Proc. Natl Acad. Sci. USA 100, 8430–8435 (2003).
Deckers, M. et al. The tumor suppressor Smad4 is required for transforming growth factor-β-induced epithelial to mesenchymal transition and bone metastasis of breast cancer cells. Cancer Res. 66, 2202–2209 (2006).
Cui, W. et al. TGFβ1 inhibits the formation of benign skin tumors, but enhances progression to invasive spindle carcinomas in transgenic mice. Cell 86, 531–542 (1996).
Fowlis, D. J., Cui, W., Johnson, S. A., Balmain, A. & Akhurst, R. J. Altered epidermal cell growth control in vivo by inducible expression of transforming growth factor β 1 in the skin of transgenic mice. Cell Growth Differ. 7, 679–687 (1996).
Cui, W. et al. Concerted action of TGF-β1 and its type II receptor in control of epidermal homeostasis in transgenic mice. Genes Dev. 9, 945–955 (1995).
Amendt, C., Schirmacher, P., Weber, H. & Blessing, M. Expression of a dominant negative type II TGF-β receptor in mouse skin results in an increase in carcinoma incidence and an acceleration of carcinoma development. Oncogene 17, 25–34 (1998).
Go, C. et al. Aberrant cell cycle progression contributes to the early-stage accelerated carcinogenesis in transgenic epidermis expressing the dominant negative TGFβRII. Oncogene 19, 3623–3631 (2000).
Go, C., Li, P. & Wang, X. J. Blocking transforming growth factor-β signaling in transgenic epidermis accelerates chemical carcinogenesis: a mechanism associated with increased angiogenesis. Cancer Res. 59, 2861–2868 (1999).
Wang, X. J., Liefer, K. M., Tsai, S., O'Malley, B. W. & Roop, D. R. Development of gene-switch transgenic mice that inducibly express transforming growth factor β1 in the epidermis. Proc. Natl Acad. Sci. USA 96, 8483–8488 (1999).
Weeks, B. H., He, W., Olson, K. L. & Wang, X. J. Inducible expression of transforming growth factor β1 in papillomas causes rapid metastasis. Cancer Res. 61, 7435–7443 (2001).
Han, G. et al. Distinct mechanisms of TGF-β1-mediated epithelial-to-mesenchymal transition and metastasis during skin carcinogenesis. J. Clin. Invest. 115, 1714–1723 (2005). Showed the effect of increased TGFβ expression with the concurrent expression of a dominant-negative type II receptor in the skin epithelium during carcinogenesis. The data show that the expression of TGFβ with a reduction in the tumour-cell-autonomous response to this pathway promotes progression to metastasis.
Wang, X. J. et al. Expression of a dominant-negative type II transforming growth factor-β (TGF-β) receptor in the epidermis of transgenic mice blocks TGF-β-mediated growth inhibition. Proc. Natl Acad. Sci. USA 94, 2386–2391 (1997).
Bhowmick, N. A. et al. TGF-β signaling in fibroblasts modulates the oncogenic potential of adjacent epithelia. Science 303, 848–851 (2004). Showed that TGFβ signalling in some fibroblast subpopulations can regulate the initiation of carcinoma in adjacent epithelia.
Cheng, N. et al. Loss of TGF-β type II receptor in fibroblasts promotes mammary carcinoma growth and invasion through upregulation of TGF-α-, MSP- and HGF-mediated signaling networks. Oncogene 24, 5053–5068 (2005). Showed that TGFβ signalling in fibroblasts can regulate tumour progression in adjacent epithelium through distinct molecular mechanisms.
Hayward, S. W. et al. Malignant transformation in a nontumorigenic human prostatic epithelial cell line. Cancer Res. 61, 8135–8142 (2001).
Barcellos-Hoff, M. H. & Ravani, S. A. Irradiated mammary gland stroma promotes the expression of tumorigenic potential by unirradiated epithelial cells. Cancer Res. 60, 1254–1260 (2000).
Chang, H. Y. et al. Diversity, topographic differentiation, and positional memory in human fibroblasts. Proc. Natl Acad. Sci. USA 99, 12877–12882 (2002). Showed that fibroblasts isolated from different parts of the body have distinct molecular profiles. The unique molecular identity of each fibroblast subpopulation was used to accurately identify the tissue from which it was derived.
Giannouli, C. C. & Kletsas, D. TGF-β regulates differentially the proliferation of fetal and adult human skin fibroblasts via the activation of PKA and the autocrine action of FGF-2. Cell. Signal. 14 Dec 2005 [epub ahead of print].
Chen, W. & Wahl, S. M. TGF-β: the missing link in CD4+CD25+ regulatory T cell-mediated immunosuppression. Cytokine Growth Factor Rev. 14, 85–89 (2003).
de Visser, K. E. & Kast, W. M. Effects of TGF-β on the immune system: implications for cancer immunotherapy. Leukemia 13, 1188–1199 (1999).
Gorelik, L. & Flavell, R. A. Transforming growth factor-β in T-cell biology. Nature Rev. Immunol. 2, 46–53 (2002).
Wahl, S. M., Swisher, J., McCartney-Francis, N. & Chen, W. TGF-β: the perpetrator of immune suppression by regulatory T cells and suicidal T cells. J. Leukoc. Biol. 76, 15–24 (2004).
Goumans, M. J., Lebrin, F. & Valdimarsdottir, G. Controlling the angiogenic switch: a balance between two distinct TGF-β receptor signaling pathways. Trends Cardiovasc. Med. 13, 301–307 (2003).
Muraoka-Cook, R. S., Dumont, N. & Arteaga, C. L. Dual role of transforming growth factor β in mammary tumorigenesis and metastatic progression. Clin. Cancer Res. 11, 937s–943s (2005).
Gorelik, L. & Flavell, R. A. Abrogation of TGFβ signaling in T cells leads to spontaneous T cell differentiation and autoimmune disease. Immunity 12, 171–181 (2000).
Kulkarni, A. B. et al. Transforming growth factor-β1 null mutation in mice causes excessive inflammatory response and early death. Proc. Natl Acad. Sci. USA 90, 770–774 (1993).
Leveen, P. et al. Induced disruption of the transforming growth factor-β type II receptor gene in mice causes a lethal inflammatory disorder that is transplantable. Blood 100, 560–568 (2002).
Shull, M. M. et al. Targeted disruption of the mouse transforming growth factor-β1 gene results in multifocal inflammatory disease. Nature 359, 693–699 (1992).
Ruzek, M. C. et al. Minimal effects on immune parameters following chronic anti-TGF-β monoclonal antibody administration to normal mice. Immunopharmacol. Immunotoxicol. 25, 235–257 (2003).
Yang, Y. A. et al. Lifetime exposure to a soluble TGF-β antagonist protects mice against metastasis without adverse side effects. J. Clin. Invest. 109, 1607–1615 (2002). Before this study it was not known if the systemic inhibition of TGFβ signalling would be a viable strategy for administration over a sustained duration in vivo . However, this report indicates that in mice, a sustained systemic inhibition of TGFβ does not result in any observed adverse effects.
Yingling, J. M., Blanchard, K. L. & Sawyer, J. S. Development of TGF-β signalling inhibitors for cancer therapy. Nature Rev. Drug Discov. 3, 1011–1022 (2004).
Smyth, M. J. et al. CD4+CD25+ T regulatory cells suppress NK cell-mediated immunotherapy of cancer. J. Immunol. 176, 1582–1587 (2006).
Fontana, A., Constam, D. B., Frei, K., Malipiero, U. & Pfister, H. W. Modulation of the immune response by transforming growth factor-β. Int. Arch. Allergy Immunol. 99, 1–7 (1992).
Fontana, A., Bodmer, S., Frei, K., Malipiero, U. & Siepl, C. Expression of TGF-β2 in human glioblastoma: a role in resistance to immune rejection? Ciba Found. Symp. 157, 232–238; discussion 238–241 (1991).
Gorelik, L. & Flavell, R. A. Immune-mediated eradication of tumors through the blockade of transforming growth factor-β signaling in T cells. Nature Med. 7, 1118–1122 (2001). Blockade of TGFβ signalling in T cells resulted in a marked resistance to cancer when mice were challenged with live tumour cells. The resistance was shown to be the result of an efficient eradication of tumour cells owing to a robust immune response after the attenuation of TGFβ signalling in T cells.
Thomas, D. A. & Massague, J. TGF-β directly targets cytotoxic T cell functions during tumor evasion of immune surveillance. Cancer Cell 8, 369–380 (2005).
Zhang, Q. et al. Adoptive transfer of tumor-reactive transforming growth factor-β-insensitive CD8+ T cells: eradication of autologous mouse prostate cancer. Cancer Res. 65, 1761–1769 (2005).
Peng, S. B. et al. Kinetic characterization of novel pyrazole TGF-β receptor I kinase inhibitors and their blockade of the epithelial-mesenchymal transition. Biochemistry 44, 2293–2304 (2005).
Tojo, M. et al. The ALK-5 inhibitor A-83–01 inhibits Smad signaling and epithelial-to-mesenchymal transition by transforming growth factor-β. Cancer Sci. 96, 791–800 (2005).
Ge, R. et al. Selective inhibitors of type I receptor kinase block cellular transforming growth factor-β signaling. Biochem. Pharmacol. 68, 41–50 (2004).
DaCosta Byfield, S., Major, C., Laping, N. J. & Roberts, A. B. SB-505124 is a selective inhibitor of transforming growth factor-β type I receptors ALK4, ALK5, and ALK7. Mol. Pharmacol. 65, 744–752 (2004).
Uhl, M. et al. SD-208, a novel transforming growth factor-β receptor I kinase inhibitor, inhibits growth and invasiveness and enhances immunogenicity of murine and human glioma cells in vitro and in vivo. Cancer Res. 64, 7954–7961 (2004).
Inman, G. J. et al. SB-431542 is a potent and specific inhibitor of transforming growth factor-β superfamily type I activin receptor-like kinase (ALK) receptors ALK4, ALK5, and ALK7. Mol. Pharmacol. 62, 65–74 (2002).
Landis, M. D., Seachrist, D. D., Montanez-Wiscovich, M. E., Danielpour, D. & Keri, R. A. Gene expression profiling of cancer progression reveals intrinsic regulation of transforming growth factor-β signaling in ErbB2/Neu-induced tumors from transgenic mice. Oncogene 24, 5173–5190 (2005).
Yoshinaga, K. et al. Clinical significance of the expression of activin A in esophageal carcinoma. Int. J. Oncol. 22, 75–80 (2003).
Subramanian, G. et al. Targeting endogenous transforming growth factor-β receptor signaling in SMAD4-deficient human pancreatic carcinoma cells inhibits their invasive phenotype1. Cancer Res. 64, 5200–5211 (2004).
Cosgrove, D. et al. Integrin α1β1 and transforming growth factor-β1 play distinct roles in alport glomerular pathogenesis and serve as dual targets for metabolic therapy. Am. J. Pathol. 157, 1649–1659 (2000).
Bandyopadhyay, A. et al. A soluble transforming growth factor β type III receptor suppresses tumorigenicity and metastasis of human breast cancer MDA-MB-231 cells. Cancer Res. 59, 5041–5046 (1999).
Bandyopadhyay, A. et al. Antitumor activity of a recombinant soluble betaglycan in human breast cancer xenograft. Cancer Res. 62, 4690–4695 (2002).
Dasch, J. R., Pace, D. R., Waegell, W., Inenaga, D. & Ellingsworth, L. Monoclonal antibodies recognizing transforming growth factor-β. Bioactivity neutralization and transforming growth factor-β 2 affinity purification. J. Immunol. 142, 1536–1541 (1989).
Cordeiro, M. F., Gay, J. A. & Khaw, P. T. Human anti-transforming growth factor-β2 antibody: a new glaucoma anti-scarring agent. Invest. Ophthalmol. Vis. Sci. 40, 2225–2234 (1999).
Thompson, J. E. et al. A fully human antibody neutralising biologically active human TGFβ2 for use in therapy. J. Immunol. Methods 227, 17–29 (1999).
Lucas, C. et al. The autocrine production of transforming growth factor-β1 during lymphocyte activation. A study with a monoclonal antibody-based ELISA. J. Immunol. 145, 1415–1422 (1990).
Arteaga, C. L., Carty-Dugger, T., Moses, H. L., Hurd, S. D. & Pietenpol, J. A. Transforming growth factor β1 can induce estrogen-independent tumorigenicity of human breast cancer cells in athymic mice. Cell Growth Differ. 4, 193–201 (1993).
Arteaga, C. L., Dugger, T. C., Winnier, A. R. & Forbes, J. T. Evidence for a positive role of transforming growth factor-β in human breast cancer cell tumorigenesis. J. Cell. Biochem. Suppl. 17G, 187–193 (1993).
Arteaga, C. L. et al. Anti-transforming growth factor (TGF)-β antibodies inhibit breast cancer cell tumorigenicity and increase mouse spleen natural killer cell activity. Implications for a possible role of tumor cell/host TGF-β interactions in human breast cancer progression. J. Clin. Invest. 92, 2569–2576 (1993).
Fakhrai, H. et al. Eradication of established intracranial rat gliomas by transforming growth factor-β antisense gene therapy. Proc. Natl Acad. Sci. USA 93, 2909–2914 (1996).
Liau, L. M., Fakhrai, H. & Black, K. L. Prolonged survival of rats with intracranial C6 gliomas by treatment with TGF-β antisense gene. Neurol. Res. 20, 742–747 (1998).
Schlingensiepen, K. H. et al. Targeted tumor therapy with the TGF-β2 antisense compound AP 12009. Cytokine Growth Factor Rev. 17, 729–139 (2005).
Schlingensiepen, R. et al. Intracerebral and intrathecal infusion of the TGF-β2-specific antisense phosphorothioate oligonucleotide AP 12009 in rabbits and primates: toxicology and safety. Oligonucleotides 15, 94–104 (2005).
Rajagopalan, H., Nowak, M. A., Vogelstein, B. & Lengauer, C. The significance of unstable chromosomes in colorectal cancer. Nature Rev. Cancer 3, 695–701 (2003).
Vogelstein, B. & Kinzler, K. W. Cancer genes and the pathways they control. Nature Med. 10, 789–799 (2004).
Hanahan, D. & Weinberg, R. A. The hallmarks of cancer. Cell 100, 57–70 (2000).
Hill, R., Song, Y., Cardiff, R. D. & Van Dyke, T. Selective evolution of stromal mesenchyme with p53 loss in response to epithelial tumorigenesis. Cell 123, 1001–1011 (2005).
Desgrosellier, J. S., Mundell, N. A., McDonnell, M. A., Moses, H. L. & Barnett, J. V. Activin receptor-like kinase 2 and Smad6 regulate epithelial-mesenchymal transformation during cardiac valve formation. Dev. Biol. 280, 201–210 (2005).
Lai, Y. T. et al. Activin receptor-like kinase 2 can mediate atrioventricular cushion transformation. Dev. Biol. 222, 1–11 (2000).
Miettinen, P. J., Ebner, R., Lopez, A. R. & Derynck, R. TGF-β induced transdifferentiation of mammary epithelial cells to mesenchymal cells: involvement of type I receptors. J. Cell Biol. 127, 2021–2036 (1994).
Adams, D. H. et al. Transforming growth factor-β induces human T lymphocyte migration in vitro. J. Immunol. 147, 609–6012 (1991).
Ahmadzadeh, M. & Rosenberg, S. A. TGF-β1 attenuates the acquisition and expression of effector function by tumor antigen-specific human memory CD8 T cells. J. Immunol. 174, 5215–5223 (2005).
Bogdan, C. & Nathan, C. Modulation of macrophage function by transforming growth factor β, interleukin-4, and interleukin-10. Ann. NY Acad. Sci. 685, 713–739 (1993).
Wahl, S. M. et al. Transforming growth factor-β is a potent immunosuppressive agent that inhibits IL-1-dependent lymphocyte proliferation. J. Immunol. 140, 3026–3032 (1988).
Bombara, C. & Ignotz, R. A. TGF-β inhibits proliferation of and promotes differentiation of human promonocytic leukemia cells. J. Cell. Physiol. 153, 30–37 (1992).
Kitamura, M. Identification of an inhibitor targeting macrophage production of monocyte chemoattractant protein-1 as TGF-β 1. J. Immunol. 159, 1404–1411 (1997).
Feinberg, M. W. et al. Essential role for Smad3 in regulating MCP-1 expression and vascular inflammation. Circ. Res. 94, 601–608 (2004).
Fadok, V. A. et al. Macrophages that have ingested apoptotic cells in vitro inhibit proinflammatory cytokine production through autocrine/paracrine mechanisms involving TGF-β, PGE2, and PAF. J. Clin. Invest. 101, 890–898 (1998).
McDonald, P. P., Fadok, V. A., Bratton, D. & Henson, P. M. Transcriptional and translational regulation of inflammatory mediator production by endogenous TGF-β in macrophages that have ingested apoptotic cells. J. Immunol. 163, 6164–6172 (1999).
Xiao, Y. Q. et al. Cross-talk between ERK and p38 MAPK mediates selective suppression of pro-inflammatory cytokines by transforming growth factor-β. J. Biol. Chem. 277, 14884–14893 (2002).
Wang, J. et al. Role of tyrosine phosphorylation in ligand-independent sequestration of CXCR4 in human primary monocytes-macrophages. J. Biol. Chem. 276, 49236–49243 (2001).
Franitza, S. et al. TGF-β1 enhances SDF-1α-induced chemotaxis and homing of naive T cells by up-regulating CXCR4 expression and downstream cytoskeletal effector molecules. Eur. J. Immunol. 32, 193–202 (2002).
Orimo, A. et al. Stromal fibroblasts present in invasive human breast carcinomas promote tumor growth and angiogenesis through elevated SDF-1/CXCL12 secretion. Cell 121, 335–348 (2005).
Geiser, A. G. et al. Transforming growth factor β1 (TGF-β1) controls expression of major histocompatibility genes in the postnatal mouse: aberrant histocompatibility antigen expression in the pathogenesis of the TGF-β1 null mouse phenotype. Proc. Natl Acad. Sci. USA 90, 9944–9948 (1993).
Lee, Y. J. et al. TGF-β suppresses IFN-γ induction of class II MHC gene expression by inhibiting class II transactivator messenger RNA expression. J. Immunol. 158, 2065–2075 (1997).
Johns, L. D. et al. Transforming growth factor-β 1 differentially regulates proliferation and MHC class-II antigen expression in forebrain and brainstem astrocyte primary cultures. Brain Res. 585, 229–236 (1992).
Ma, D. & Niederkorn, J. Y. Transforming growth factor-β down-regulates major histocompatibility complex class I antigen expression and increases the susceptibility of uveal melanoma cells to natural killer cell-mediated cytolysis. Immunology 86, 263–269 (1995).
Witham, T. F. et al. Expression of a soluble transforming growth factor-β (TGFβ) receptor reduces tumorigenicity by regulating natural killer (NK) cell activity against 9L gliosarcoma in vivo. J. Neurooncol. 64, 63–69 (2003).
Reibman, J. et al. Transforming growth factor β1, a potent chemoattractant for human neutrophils, bypasses classic signal-transduction pathways. Proc. Natl Acad. Sci. USA 88, 6805–6809 (1991).
Chen, J. J., Sun, Y. & Nabel, G. J. Regulation of the proinflammatory effects of Fas ligand (CD95L). Science 282, 1714–1717 (1998).
Hahne, M. et al. Melanoma cell expression of Fas(Apo-1/CD95) ligand: implications for tumor immune escape. Science 274, 1363–1366 (1996).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Related links
Glossary
- Loss of heterozygosity
-
Tumour cells often lose large genomic regions at loci that often contain tumour-suppressor genes. In cells that carry a mutated allele of a tumour-suppressor gene, the loss of a large region from a chromosome that carries the wild-type allele can result in a complete loss of function.
- Microsatellite instability
-
A condition associated with some cancers whereby a tumours associated genetic instability is due to defects in mismatch-repair gene products. The mutations associated with this type of genomic instability often occur in short nucleotide repeats.
- Dominant-negative
-
A defective protein product that effectively inhibits the function of a wild-type counterpart by retaining essential interaction capabilities without a desired effector function.
- Lobular-alveolar
-
Mammary epithelial cells that are able to differentiate into functional secretory units during pregnancy, and that can produce milk proteins during lactation.
- Bigenic mice
-
Transgenic mice that concurrently express two minigene constructs.
- Major histocompatibility complex
-
Genes that encode products that are necessary for the regulation of immune function. Class I and class II MHC genes are involved in antigen presentation and the regulation of self recognition.
- Convection-enhanced delivery
-
A method of delivering compounds to the brain that circumvents the blood–brain barrier. This method enables a compound to be infused directly into a brain tumour under a controlled pressure and rate of release.
Rights and permissions
About this article
Cite this article
Bierie, B., Moses, H. TGFβ: the molecular Jekyll and Hyde of cancer. Nat Rev Cancer 6, 506–520 (2006). https://doi.org/10.1038/nrc1926
Issue Date:
DOI: https://doi.org/10.1038/nrc1926
This article is cited by
-
SPAG6 regulates cell proliferation and apoptosis via TGF-β/Smad signal pathway in adult B-cell acute lymphoblastic leukemia
International Journal of Hematology (2024)
-
New gold(III) complexes TGS 121, 404, and 702 show anti-tumor activity in colitis-induced colorectal cancer: an in vitro and in vivo study
Pharmacological Reports (2024)
-
Identification and verification of a BMPs-related gene signature for osteosarcoma prognosis prediction
BMC Cancer (2023)
-
“Stromal cells in prostate cancer pathobiology: friends or foes?”
British Journal of Cancer (2023)
-
Copper chelation suppresses epithelial-mesenchymal transition by inhibition of canonical and non-canonical TGF-β signaling pathways in cancer
Cell & Bioscience (2023)