Key Points
-
Cannabinoids, the active components of Cannabis sativa and their derivatives, act in the organism by mimicking endogenous substances, the endocannabinoids, that activate specific cannabinoid receptors.
-
Cannabinoids exert palliative effects in patients with cancer and inhibit tumour growth in laboratory animals.
-
The best-established palliative effect of cannabinoids in cancer patients is the inhibition of chemotherapy-induced nausea and vomiting. Today, capsules of Δ9-tetrahydrocannabinol (dronabinol (Marinol)) and its synthetic analogue nabilone (Cesamet) are approved for this purpose.
-
Other potential palliative effects of cannabinoids in cancer patients — supported by Phase III clinical trials — include appetite stimulation and pain inhibition. In relation to the former, dronabinol is now prescribed for anorexia associated with weight loss in patients with AIDS.
-
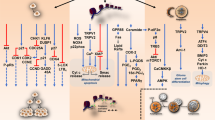
Cannabinoids inhibit tumour growth in laboratory animals. They do so by modulating key cell-signalling pathways, thereby inducing direct growth arrest and death of tumour cells, as well as by inhibiting tumour angiogenesis and metastasis.
-
Cannabinoids are selective antitumour compounds, as they can kill tumour cells without affecting their non-transformed counterparts. It is probable that cannabinoid receptors regulate cell-survival and cell-death pathways differently in tumour and non-tumour cells.
-
Cannabinoids have favourable drug-safety profiles and do not produce the generalized toxic effects of conventional chemotherapies. The use of cannabinoids in medicine, however, is limited by their psychoactive effects, and so cannabinoid-based therapies that are devoid of unwanted side effects are being designed.
-
Further basic and preclinical research on cannabinoid anticancer properties is required. It would be desirable that clinical trials could accompany these laboratory studies to allow us to use these compounds in the treatment of cancer.
Abstract
Cannabinoids — the active components of Cannabis sativa and their derivatives — exert palliative effects in cancer patients by preventing nausea, vomiting and pain and by stimulating appetite. In addition, these compounds have been shown to inhibit the growth of tumour cells in culture and animal models by modulating key cell-signalling pathways. Cannabinoids are usually well tolerated, and do not produce the generalized toxic effects of conventional chemotherapies. So, could cannabinoids be used to develop new anticancer therapies?
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Gaoni, Y. & Mechoulam, R. Isolation, structure and partial synthesis of an active constituent of hashish. J. Am. Chem. Soc. 86, 1646–1647 (1964).
Howlett, A. C. et al. International Union of Pharmacology. XXVII. Classification of cannabinoid receptors. Pharmacol. Rev. 54, 161–202 (2002). A comprehensive update on cannabinoid receptors and their biochemistry and pharmacology.
Herkenham, M. et al. Characterization and localization of cannabinoid receptors in rat brain: a quantitative in vitro autoradiographic study. J. Neurosci. 11, 563–583 (1991).
Porter, A. C. & Felder, C. C. The endocannabinoid nervous system. Unique opportunities for therapeutic intervention. Pharmacol. Ther. 90, 45–60 (2001).
Pertwee, R. G. Cannabinoid receptor ligands: clinical and neuropharmacological considerations, relevant to future drug discovery and development. Expert Opin. Investig. Drugs 9, 1553–1571 (2000).
Di Carlo, G. & Izzo, A. A. Cannabinoids for gastrointestinal diseases: potential therapeutic applications. Expert Opin. Investig. Drugs 12, 39–49 (2003).
Croxford, J. L. Therapeutic potential of cannabinoids in CNS disease. CNS Drugs 17, 179–202 (2003).
Robson, P. Therapeutic aspects of cannabis and cannabinoids. Br. J. Psychiatry 178, 107–115 (2001).
Tramer, M. R. et al. Cannabinoids for control of chemotherapy induced nausea and vomiting: quantitative systematic review. BMJ 323, 16–21 (2001). A detailed review on the best palliative action of cannabinoids in cancer therapy that has been established so far.
Walsh, D., Nelson, K. A. & Mahmoud, F. A. Established and potential therapeutic applications of cannabinoids in oncology. Support Care Cancer 11, 137–143 (2003).
Barann, M. et al. Direct inhibition by cannabinoids of human 5-HT3A receptors: probable involvement of an allosteric modulatory site. Br. J. Pharmacol. 137, 589–596 (2002).
Tisdale, M. J. Cachexia in cancer patients. Nature Rev. Cancer 2, 862–871 (2002).
Berry, E. M. & Mechoulam, R. Tetrahydrocannabinol and endocannabinoids in feeding and appetite. Pharmacol. Ther. 95, 185–190 (2002). An authoritative review on the physiological role and therapeutic potential of cannabinoids in appetite stimulation.
Cota, D. et al. Endogenous cannabinoid system as a modulator of food intake. Int. J. Obes. Relat. Metab. Disord. 27, 289–301 (2003).
Gomez, R. et al. A peripheral mechanism for CB1 cannabinoid receptor-dependent modulation of feeding. J. Neurosci. 22, 9612–9617 (2002).
Bensaid, M. et al. The cannabinoid CB1 receptor antagonist SR141716 increases Acrp30 mRNA expression in adipose tissue of obese fa/fa rats and in cultured adipocyte cells. Mol. Pharmacol. 63, 908–914 (2003).
Cota, D. et al. The endogenous cannabinoid system affects energy balance via central orexigenic drive and peripheral lipogenesis. J. Clin. Invest. 112, 423–431 (2003).
Nelson, K., Walsh, D., Deeter, P. & Sheehan, F. A phase II study of δ-9-tetrahydrocannabinol for appetite stimulation in cancer-associated anorexia. J. Palliat. Care 10, 14–18 (1994).
Jatoi, A. et al. Dronabinol versus megestrol acetate versus combination therapy for cancer-associated anorexia: a North Central Cancer Treatment Group study. J. Clin. Oncol. 20, 567–573 (2002).
Mantyh, P. W., Clohisy, D. R., Koltzenburg, M. & Hunt, S. P. Molecular mechanisms of cancer pain. Nature Rev. Cancer 2, 201–209 (2002).
Pertwee, R. G. Cannabinoid receptors and pain. Prog. Neurobiol. 63, 569–611 (2001).
Walker, J. & Huang, S. Cannabinoid analgesia. Pharmacol. Ther. 95, 127–135 (2002).
Calignano, A., LaRana, G., Giuffrida, A. & Piomelli, D. Control of pain initiation by endogenous cannabinoids. Nature 394, 277–281 (1998).
Campbell, F. A. et al. Are cannabinoids an effective and safe treatment option in the management of pain? A qualitative systematic review. BMJ 323, 13–16 (2001). A lively discussion on the possible therapeutic value of cannabinoids as analgesic agents.
Noyes, R. Jr, Brunk, S. F., Avery, D. A. H. & Canter, A. C. The analgesic properties of delta-9-tetrahydrocannabinol and codeine. Clin. Pharmacol. Ther. 18, 84–89 (1975).
Iversen, L. & Chapman, V. Cannabinoids: a real prospect for pain relief. Curr. Opin. Pharmacol. 2, 50–55 (2002).
Manzanares, J. et al. Pharmacological and biochemical interactions between opioids and cannabinoids. Trends Pharmacol. Sci. 20, 287–294 (1999).
Baker, D. & Pryce, G. The therapeutic potential of cannabis in multiple sclerosis. Expert Opin. Investig. Drugs 12, 561–567 (2003).
Munson, A. E., Harris, L. S., Friedman, M. A., Dewey, W. L. & Carchman, R. A. Antineoplastic activity of cannabinoids. J. Natl Cancer Inst. 55, 597–602 (1975). The seminal demonstration that THC inhibits tumour-cell growth in culture and in mice.
Guzman, M., Sanchez, C. & Galve-Roperh, I. Cannabinoids and cell fate. Pharmacol. Ther. 95, 175–184 (2002).
Bouaboula, M. et al. Activation of mitogen-activated protein kinases by stimulation of the central cannabinoid receptor CB1. Biochem. J. 312, 637–641 (1995).
Bouaboula, M. et al. Signaling pathway associated with stimulation of CB2 peripheral cannabinoid receptor. Involvement of both mitogen-activated protein kinase and induction of Krox-24 expression. Eur. J. Biochem. 237, 704–711 (1996).
Liu, J. et al. Functional CB1 cannabinoid receptors in human vascular endothelial cells. Biochem. J. 346, 835–840 (2000).
Rueda, D., Galve-Roperh, I., Haro, A. & Guzman, M. The CB1 cannabinoid receptor is coupled to the activation of c-Jun N-terminal kinase. Mol. Pharmacol. 58, 814–820 (2000).
Derkinderen, P., Ledent, C., Parmentier, M. & Girault, J. A. Cannabinoids activate p38 mitogen-activated protein kinases through CB1 receptors in hippocampus. J. Neurochem. 77, 957–960 (2001).
Chang, L. & Karin, M. Mammalian MAP kinase signalling cascades. Nature 410, 37–40 (2001).
Rueda, D., Navarro, B., Martinez-Serrano, A., Guzman, M. & Galve-Roperh, I. The endocannabinoid anandamide inhibits neuronal progenitor cell differentiation through attenuation of the Rap1/B-Raf/ERK pathway. J. Biol. Chem. 277, 46645–46650 (2002).
Gomez del Pulgar, T., Velasco, G. & Guzman, M. The CB1 cannabinoid receptor is coupled to the activation of protein kinase B/Akt. Biochem. J. 347, 369–373 (2000).
Sanchez, M. G., Ruiz-Llorente, L., Sanchez, A. M. & Diaz-Laviada, I. Activation of phosphoinositide 3-kinase/PKB pathway by CB1 and CB2 cannabinoid receptors expressed in prostate PC-3 cells. Involvement in Raf-1 stimulation and NGF induction. Cell. Signal. 15, 851–859 (2003).
Vivanco, I. & Sawyers, C. L. The phosphatidylinositol 3-kinase AKT pathway in human cancer. Nature Rev. Cancer 2, 489–501 (2002).
Samson, M. T. et al. Differential roles of CB1 and CB2 cannabinoid receptors in mast cells. J. Immunol. 170, 4953–4962 (2003).
Gomez del Pulgar, T., Velasco, G., Sanchez, C., Haro, A. & Guzman, M. De novo-synthesized ceramide is involved in cannabinoid-induced apoptosis. Biochem. J. 363, 183–188 (2002).
Bouaboula, M. et al. A selective inverse agonist for central cannabinoid receptor inhibits mitogen-activated protein kinase activation stimulated by insulin or insulin-like growth factor 1. Evidence for a new model of receptor/ligand interactions. J. Biol. Chem. 272, 22330–22339 (1997).
Galve-Roperh, I., Rueda, D., Gomez Del Pulgar, T., Velasco, G. & Guzman, M. Mechanism of extracellular signal-regulated kinase activation by the CB1 cannabinoid receptor. Mol. Pharmacol. 62, 1385–1392 (2002).
Derkinderen, P. et al. Regulation of extracellular signal-regulated kinase by cannabinoids in hippocampus. J. Neurosci. 23, 2371–2382 (2003).
Sanchez, C., Galve-Roperh, I., Rueda, D. & Guzman, M. Involvement of sphingomyelin hydrolysis and the mitogen-activated protein kinase cascade in the Δ9–tetrahydrocannabinol-induced stimulation of glucose metabolism in primary astrocytes. Mol. Pharmacol. 54, 834–843 (1998).
Hannun, Y. A. & Obeid, L. M. The Ceramide-centric universe of lipid-mediated cell regulation: stress encounters of the lipid kind. J. Biol. Chem. 277, 25847–25850 (2002).
Kolesnick, R. The therapeutic potential of modulating the ceramide/sphingomyelin pathway. J. Clin. Invest. 110, 3–8 (2002).
Sanchez, C. et al. The CB1 cannabinoid receptor of astrocytes is coupled to sphingomyelin hydrolysis through the adaptor protein fan. Mol. Pharmacol. 59, 955–959 (2001).
Galve-Roperh, I. et al. Anti-tumoral action of cannabinoids: involvement of sustained ceramide accumulation and extracellular signal-regulated kinase activation. Nature Med. 6, 313–319 (2000). The first identification of a signalling mechanism for the apoptotic action of cannabinoids on tumour cells.
Sanchez, C., Galve-Roperh, I., Canova, C., Brachet, P. & Guzman, M. Δ9–Tetrahydrocannabinol induces apoptosis in C6 glioma cells. FEBS Lett. 436, 6–10 (1998).
Guzman, M., Galve-Roperh, I. & Sanchez, C. Ceramide: a new second messenger of cannabinoid action. Trends Pharmacol. Sci. 22, 19–22 (2001).
Sanchez, C. et al. Inhibition of glioma growth in vivo by selective activation of the CB2 cannabinoid receptor. Cancer Res. 61, 5784–5789 (2001).
Mimeault, M., Pommery, N., Wattez, N., Bailly, C. & Henichart, J. P. Anti-proliferative and apoptotic effects of anandamide in human prostatic cancer cell lines: implication of epidermal growth factor receptor down-regulation and ceramide production. Prostate 56, 1–12 (2003).
Sarker, K. P., Obara, S., Nakata, M., Kitajima, I. & Maruyama, I. Anandamide induces apoptosis of PC-12 cells: involvement of superoxide and caspase-3. FEBS Lett. 472, 39–44 (2000).
Sarker, K. P. et al. ASK1-p38 MAPK/JNK signaling cascade mediates anandamide-induced PC12 cell death. J. Neurochem. 85, 50–61 (2003).
De Petrocellis, L. et al. The endogenous cannabinoid anandamide inhibits human breast cancer cell proliferation. Proc. Natl Acad. Sci. USA 95, 8375–8380 (1998).
Melck, D. et al. Involvement of the cAMP/protein kinase A pathway and of mitogen-activated protein kinase in the anti-proliferative effects of anandamide in human breast cancer cells. FEBS Lett. 463, 235–240 (1999).
Melck, D. et al. Suppression of nerve growth factor trk receptors and prolactin receptors by endocannabinoids leads to inhibition of human breast and prostate cancer cell proliferation. Endocrinology 141, 118–126 (2000).
Bifulco, M. et al. Control by the endogenous cannabinoid system of ras oncogene-dependent tumor growth. FASEB J. 15, 2745–2747 (2001).
Casanova, M. L. et al. Inhibition of skin tumor growth and angiogenesis in vivo by activation of cannabinoid receptors. J. Clin. Invest. 111, 43–50 (2003).
Kerbel, R. & Folkman, J. Clinical translation of angiogenesis inhibitors. Nature Rev. Cancer 2, 727–739 (2002).
Blazquez, C. et al. Inhibition of tumor angiogenesis by cannabinoids. FASEB J. 17, 529–531 (2003). The first paper showing that cannabinoid administration to mice impairs tumour angiogenesis.
Portella, G. et al. Inhibitory effects of cannabinoid CB1 receptor stimulation on tumor growth and metastatic spreading: actions on signals involved in angiogenesis and metastasis. FASEB J. 3 Jul 2003 (doi:10.1096/fj.02-1129fje).
Gomez Del Pulgar, T., De Ceballos, M. L., Guzman, M. & Velasco, G. Cannabinoids protect astrocytes from ceramide-induced apoptosis through the phosphatidylinositol 3-kinase/protein kinase B pathway. J. Biol. Chem. 277, 36527–36533 (2002).
Molina-Holgado, E. et al. Cannabinoids promote oligodendrocyte progenitor survival: involvement of cannabinoid receptors and phosphatidylinositol-3 kinase/Akt signaling. J. Neurosci. 22, 9742–9753 (2002).
Blazquez, C., Galve-Roperh, I. & Guzman, M. De novo-synthesized ceramide signals apoptosis in astrocytes via extracellular signal-regulated kinase. FASEB J. 14, 2315–2322 (2000).
Glass, M. & Felder, C. C. Concurrent stimulation of cannabinoid CB1 and dopamine D2 receptors augments cAMP accumulation in striatal neurons: evidence for a Gs linkage to the CB1 receptor. J. Neurosci. 17, 5327–5333 (1997).
Vasquez, C. & Lewis, D. L. The CB1 cannabinoid receptor can sequester G-proteins, making them unavailable to couple to other receptors. J. Neurosci. 19, 9271–9280 (1999).
Mukhopadhyay, S., McIntosh, H. H., Houston, D. B. & Howlett, A. C. The CB1 cannabinoid receptor juxtamembrane C-terminal peptide confers activation to specific G proteins in brain. Mol. Pharmacol. 57, 162–170 (2000).
Mechoulam, R., Panikashvili, D. & Shohami, E. Cannabinoids and brain injury: therapeutic implications. Trends Mol. Med. 8, 58–61 (2002).
van der Stelt, M. et al. Acute neuronal injury, excitotoxicity, and the endocannabinoid system. Mol. Neurobiol. 26, 317–346 (2002).
Maccarrone, M., Lorenzon, T., Bari, M., Melino, G. & Finazzi-Agro, A. Anandamide induces apoptosis in human cells via vanilloid receptors. Evidence for a protective role of cannabinoid receptors. J. Biol. Chem. 275, 31938–31945 (2000).
Guzman, M., Sanchez, C. & Galve-Roperh, I. Control of the cell survival/death decision by cannabinoids. J. Mol. Med. 78, 613–625 (2001).
Schwarz, H., Blanco, F. J. & Lotz, M. Anadamide, an endogenous cannabinoid receptor agonist inhibits lymphocyte proliferation and induces apoptosis. J. Neuroimmunol. 55, 107–115 (1994).
Zhu, W., Friedman, H. & Klein, T. W. Δ9-tetrahydrocannabinol induces apoptosis in macrophages and lymphocytes: involvement of Bcl-2 and caspase-1. J. Pharmacol. Exp. Ther. 286, 1103–1109 (1998).
Zhu, L. X. et al. Δ-9-tetrahydrocannabinol inhibits antitumor immunity by a CB2 receptor-mediated, cytokine-dependent pathway. J. Immunol. 165, 373–380 (2000).
Derocq, J. M., Segui, M., Marchand, J., Le Fur, G. & Casellas, P. Cannabinoids enhance human B-cell growth at low nanomolar concentrations. FEBS Lett. 369, 177–182 (1995).
Valk, P. et al. Anandamide, a natural ligand for the peripheral cannabinoid receptor is a novel synergistic growth factor for hematopoietic cells. Blood 90, 1448–1457 (1997).
Tashkin, D. R., Baldwin, G. C., Sarafian, T., Dubinett, S. & Roth, M. D. Respiratory and immunologic consequences of marijuana smoking. J. Clin. Pharmacol. 42, 71S–81S (2002).
Adams, I. B. & Martin, B. R. Cannabis: pharmacology and toxicology in animals and humans. Addiction 91, 1585–1614 (1996).
Grotenhermen, F. Pharmacokinetics and pharmacodynamics of cannabinoids. Clin. Pharmacokinet. 42, 327–360 (2003).
Chan, P. C., Sills, R. C., Braun, A. G., Haseman, J. K. & Bucher, J. R. Toxicity and carcinogenicity of Δ9–tetrahydrocannabinol in Fischer rats and B6C3F1 mice. Fund. Appl. Toxicol. 30, 109–117 (1996).
Malan, T. P. et al. CB2 cannabinoid receptor agonists: pain relief without psychoactive effects? Curr. Opin. Pharmacol. 3, 62–67 (2003).
Jacobsson, S. O., Rongard, E., Stridh, M., Tiger, G. & Fowler, C. J. Serum-dependent effects of tamoxifen and cannabinoids upon C6 glioma cell viability. Biochem. Pharmacol. 60, 1807–1813 (2000).
Mechoulam, R., Parker, L. A. & Gallily, R. Cannabidiol: an overview of some pharmacological aspects. J. Clin. Pharmacol. 42, 11S–19S (2002).
Pop, E. Dexanabinol Pharmos. Curr. Opin. Investig. Drugs 1, 494–503 (2000).
Recht, L. D. et al. Antitumor effects of ajulemic acid (CT3), a synthetic non-psychoactive cannabinoid. Biochem. Pharmacol. 62, 755–763 (2001).
Rhee, M. H. et al. Cannabinol derivatives: binding to cannabinoid receptors and inhibition of adenylylcyclase. J. Med. Chem. 40, 3228–3233 (1997).
Bifulco, M. & Di Marzo, V. Targeting the endocannabinoid system in cancer therapy: a call for further research. Nature Med. 8, 547–550 (2002). An enjoyable commentary about the possible antitumour action of the endogenous cannabinoid system.
Gallily, R. et al. γ-Irradiation enhances apoptosis induced by cannabidiol, a non-psychotropic cannabinoid, in cultured HL–60 myeloblastic leukemia cells. Leukemia Lymphoma 44, 1767–1773 (2003).
Radin, N. S. Killing tumours by ceramide-induced apoptosis: a critique of available drugs. Biochem. J. 371, 243–256 (2003).
Maurer, B. J., Melton, L., Billups, C., Cabot, M. C. & Reynolds, C. P. Synergistic cytotoxicity in solid tumor cell lines between N-(4- hydroxyphenyl)retinamide and modulators of ceramide metabolism. J. Natl Cancer Inst. 92, 1897–1909 (2000).
Maher, E. A. et al. Malignant glioma: genetics and biology of a grave matter. Genes Dev. 15, 1311–1333 (2001).
Louis, D. N., Pomeroy, S. L. & Cairncross, J. G. Focus on central nervous system neoplasia. Cancer Cell 1, 125–128 (2002).
McKallip, R. J. et al. Targeting CB2 cannabinoid receptors as a novel therapy to treat malignant lymphoblastic disease. Blood 100, 627–634 (2002).
Mon, M. J., Jansing, R. L., Doggett, S., Stein, J. L. & Stein, G. S. Influence of Δ9–tetrahydrocannabinol on cell proliferation and macromolecular biosynthesis in human cells. Biochem. Pharmacol. 27, 1759–1765 (1978).
Blevins, R. D. & Smith, D. P. Effects of Δ-9-tetrahydrocannabinol on cultured HeLa cell growth and development. Growth 44, 133–138 (1980).
Ruiz, L., Miguel, A. & Diaz-Laviada, I. Δ9–tetrahydrocannabinol induces apoptosis in human prostate PC-3 cells via a receptor-independent mechanism. FEBS Lett. 458, 400–404 (1999).
Devane, W. et al. Isolation and structure of a brain constituent that binds to the cannabinoid receptor. Science 258, 1946–1949 (1992). The discovery of anandamide, the first endogenous ligand of cannabinoid receptors.
Mechoulam, R. et al. Identification of an endogenous 2-monoglyceride, present in canine gut, that binds to cannabinoid receptors. Biochem. Pharmacol. 50, 83–90 (1995).
Sugiura, T. et al. 2-Arachidonoylglycerol: a possible endogenous cannabinoid receptor ligand in brain. Biochem. Biophys. Res. Commun. 215, 89–97 (1995).
Matsuda, L. A., Lolait, S. J., Brownstein, M. J., Young, A. C. & Bonner, T. I. Structure of a cannabinoid receptor and functional expression of the cloned cDNA. Nature 346, 561–564 (1990). The molecular characterization of CB 1 — the first specific cannabinoid receptor.
Munro, S., Thomas, K. L. & Shaar, M. Molecular characterization of a peripheral receptor for cannabinoids. Nature 365, 61–65 (1993).
Di Marzo, V. et al. Formation and inactivation of endogenous cannabinoid anandamide. Nature 372, 686–691 (1994). The discovery of the currently accepted molecular mechanism of endocannabinoid biosynthesis.
Stella, N., Schweitzer, P. & Piomelli, D. A second endogenous cannabinoid that modulates long-term potentiation. Nature 388, 773–778 (1997).
Beltramo, M. et al. Functional role of high-affinity anandamide transport, as revealed by selective inhibition. Science 277, 1094–1097 (1997).
Cravatt, B. F. et al. Molecular characterization of an enzyme that degrades neuromodulatory fatty-acid amides. Nature 384, 83–87 (1996).
Piomelli, D., Giuffrida, A., Calignano, A. & Rodríguez de Fonseca, F. The endocannabinoid system as a target for therapeutic drugs. Trends Pharmacol. Sci. 21, 218–224 (2000).
Wilson, R. I. & Nicoll, R. A. Endogenous cannabinoids mediate retrograde signaling at hippocampal synapses. Nature 410, 588–592 (2001).
Schlicker, E. & Kathmann, M. Modulation of transmitter release via presynaptic cannabinoid receptors. Trends Pharmacol. Sci. 22, 565–572 (2001).
Maldonado, R. & Rodriguez de Fonseca, F. Cannabinoid addiction: behavioral models and neural correlates. J. Neurosci. 22, 3326–3331 (2002).
Calhoun, S. R., Galloway, G. P. & Smith, D. E. Abuse potential of dronabinol (Marinol). J. Psychoactive Drugs 30, 187–196 (1998).
Acknowledgements
I am indebted to all my laboratory colleagues, in particular to I. Galve-Roperh, G. Velasco and C. Sanchez for their continuous support and for making our research projects possible. This work was funded by 'Fundación Científica de la Asociación Española Contra el Cáncer' and 'Ministerio de Ciencia y Tecnología'.
Author information
Authors and Affiliations
Related links
Related links
DATABASES
Cancer.gov
LocusLink
FURTHER INFORMATION
British Medical Association (Therapeutic uses of cannabis)
GW Pharmaceuticals clinical trials
House of Lords Committee on Science and Technology (therapeutic uses of cannabis)
House of Lords Committee on Science and Technology (therapeutic uses of cannabis)
House of Lords Committee on Science and Technology (therapeutic uses of cannabis)
International Cannabinoid Research Society
MRC multiple sclerosis clinical trial
Glossary
- CANNABINOIDS
-
Compounds with tetrahydrocannabinol (THC)-like structures and/or THC-like pharmacological properties. Many compounds with a THC-like structure are present in cannabis, but not all of them have THC-like pharmacological properties. In addition, some natural or synthetic compounds have THC-like pharmacological properties but not THC-like structure.
- CANNABIMIMETIC
-
Tetrahydrocannabinol (THC)-like in pharmacological terms. A compound is usually accepted as cannabimimetic if it produces four characteristic THC effects in an in vivo assay known as the 'mouse tetrad model': hypomotility, hypothermia, analgesia and a sustained immobility of posture (catalepsy).
- CANNABIDIOL
-
A non-psychoactive cannabinoid present in cannabis that inhibits convulsions, anxiety, vomiting and inflammation; it is now in Phase III clinical trials in combination with tetrahydrocannabinol for the treatment of multiple-sclerosis-associated muscle disorders.
- MYENTERIC AND SUBMUCOSAL PLEXUS
-
A network of sympathetic and parasympathetic nerve fibres and neuron cell bodies that are tucked in among the interstices of the smooth-muscle layer surrounding the digestive mucosa (myenteric plexus) or just underneath the digestive mucosa (submucosal plexus) and that coordinately control gastrointestinal contractions.
- META-ANALYSIS
-
Statistical analysis of a large collection of results from individual studies for the purpose of integrating their findings.
- IONOTROPIC RECEPTORS
-
Channel-like receptors that are opened by agonist binding and through which ions such as Na+, K+ and/or Ca2+ can pass. Ionotropic glutamate receptors are usually divided into three groups: N-methyl-D-aspartic acid (NMDA) receptors, kainate receptors and α-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid (AMPA) receptors.
- METABOTROPIC RECEPTORS
-
Seven-transmembrane (heptahelical) receptors that couple to heterotrimeric G proteins, thereby modulating pathways such as cyclic AMP–protein kinase A (via Gs or Gi), diacylglycerol–protein kinase C (via Gq) and inositol 1,4,5-trisphosphate–Ca2+ (via Gq). At least eight subtypes of glutamate metabotropic receptors are known.
- INTRAOCULAR PRESSURE
-
Pressure inside the eye. When it increases — for example, in glaucoma — damage to the optic nerve of the eye can result in blindness. Cannabinoids decrease intraocular pressure.
- NOCICEPTIVE
-
A stimulus that causes pain or a reaction that is caused by pain.
- HYPERALGESIA
-
An increased sensitivity and lowered threshold to a stimulus — such as burn of the skin — that is normally painful.
- ALLODYNIA
-
Pain caused by a stimulus — such as touch, pressure and warmth — that does not normally provoke pain.
- SENSORY-MOTOR PERIPHERAL NEUROPATHIES
-
Diseases or abnormalities of the peripheral nervous system that affect senses and movement.
- MYASTHENIC
-
Abnormal muscle weakness or fatigue.
- FORKHEAD TRANSCRIPTION FACTORS
-
A family of proteins that regulate the expression of genes that are involved in the control of cell survival, death, growth, differentiation and stress responses. Their activity is tightly controlled by AKT, so that phosphorylated forkhead transcription factor FOXO is retained in the cytoplasm and remains transcriptionally inactive.
- PHEOCHROMOCYTOMA
-
A relatively severe tumour of adrenal-gland chromaffin cells that causes excess release of adrenaline and noradrenaline and is therefore characterized by hypertension and tachycardia.
- PHARMACODYNAMICS
-
Mechanisms by which drugs affect their target sites in the body to produce their desired therapeutic effects and their adverse side effects.
- PHARMACOKINETICS
-
Time course of drug and metabolite levels in different fluids, tissues and excreta of the body, and of the mathematical relationships required to develop models to interpret such data.
- FIRST-PASS METABOLISM
-
Pre-systemic metabolism of a drug that limits its exposure to the body. For example, chemical or enzymatic breakdown of a drug in the gastrointestinal lumen or in the stomach, intestine or liver cells can greatly reduce the amount of drug that ends up in the bloodstream.
- DEXANABINOL
-
(HU-211). A non-psychoactive synthetic derivative of tetrahydrocannabinol that blocks ionotropic glutamate receptors and has antioxidant and anti-inflammatory properties; it is now in Phase III clinical trials for the management of brain trauma.
- AJULEMIC ACID
-
(CT3). A synthetic derivative of the tetrahydrocannabinol metabolite 11-carboxy-THC that inhibits pain and inflammation; it is entering Phase II clinical trials for the treatment of pain and spasticity in multiple sclerosis.
Rights and permissions
About this article
Cite this article
Guzmán, M. Cannabinoids: potential anticancer agents. Nat Rev Cancer 3, 745–755 (2003). https://doi.org/10.1038/nrc1188
Issue Date:
DOI: https://doi.org/10.1038/nrc1188
This article is cited by
-
Advances in blood–brain barrier-crossing nanomedicine for anti-glioma
Cancer Nanotechnology (2023)
-
Tetrahydrocannabinols: potential cannabimimetic agents for cancer therapy
Cancer and Metastasis Reviews (2023)
-
Therapeutic and Supportive Effects of Cannabinoids in Patients with Brain Tumors (CBD Oil and Cannabis)
Current Treatment Options in Oncology (2023)
-
Synthon-based ligand discovery in virtual libraries of over 11 billion compounds
Nature (2022)
-
Potential cannabidiol (CBD) repurposing as antibacterial and promising therapy of CBD plus polymyxin B (PB) against PB-resistant gram-negative bacilli
Scientific Reports (2022)