Abstract
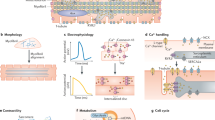
Pluripotent stem cells (PSCs), including induced PSCs, hold great potential for personalized disease modeling, drug testing and cell-based therapeutics. However, cells differentiated from PSCs remain immature in a dish, and thus there are serious caveats to their use in modeling adult-onset diseases such as cardiomyopathies and Alzheimer's disease. By taking advantage of knowledge gained about mammalian development and from bioinformatics analyses, we recently developed a neonatal rat system that enables maturation of PSC-derived cardiomyocytes into cardiomyocytes analogous to those seen in adult animals. Here we describe a detailed protocol that describes how to initiate the in vitro differentiation of mouse and human PSCs into cardiac progenitor cells, followed by intramyocardial delivery of the progenitor cells into neonatal rat hearts, in vivo incubation and analysis. The entire process takes ∼6 weeks, and the resulting cardiomyocytes can be analyzed for morphology, function and gene expression. The neonatal system provides a valuable tool for understanding the maturation and pathogenesis of adult human heart muscle cells, and this concept may be expanded to maturing other PSC-derived cell types, including those containing mutations that lead to the development of diseases in the adult.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout





Similar content being viewed by others
References
Takahashi, K. et al. Induction of pluripotent stem cells from adult human fibroblasts by defined factors. Cell 131, 861–872 (2007).
Burridge, P.W., Keller, G., Gold, J.D. & Wu, J.C. Production of de novo cardiomyocytes: human pluripotent stem cell differentiation and direct reprogramming. Cell Stem Cell 10, 16–28 (2012).
Bellin, M., Marchetto, M.C., Gage, F.H. & Mummery, C.L. Induced pluripotent stem cells: the new patient? Nat. Rev. Mol. Cell Biol. 13, 713–726 (2012).
Moretti, A., Laugwitz, K.L., Dorn, T., Sinnecker, D. & Mummery, C. Pluripotent stem cell models of human heart disease. Cold Spring Harb. Perspect. Med. 3 http://dx.doi.org/10.1101/cshperspect.a014027 (2013).
Yang, X., Pabon, L. & Murry, C.E. Engineering adolescence: maturation of human pluripotent stem cell-derived cardiomyocytes. Circ. Res. 114, 511–523 (2014).
Tabar, V. & Studer, L. Pluripotent stem cells in regenerative medicine: challenges and recent progress. Nat. Rev. Genet. 15, 82–92 (2014).
Uosaki, H. et al. Transcriptional landscape of cardiomyocyte maturation. Cell Rep. 13, 1705–1716 (2015).
Cho, G.S., Fernandez, L. & Kwon, C. Regenerative medicine for the heart: perspectives on stem-cell therapy. Antioxid. Redox Signal. 21, 2018–2031 (2014).
Finegold, J.A., Asaria, P. & Francis, D.P. Mortality from ischaemic heart disease by country, region, and age: statistics from World Health Organisation and United Nations. Int. J. Cardiol. 168, 934–945 (2013).
Yoshida, Y. & Yamanaka, S. iPS cells: a source of cardiac regeneration. J. Mol. Cell. Cardiol. 50, 327–332 (2011).
Robertson, C., Tran, D.D. & George, S.C. Concise review: maturation phases of human pluripotent stem cell-derived cardiomyocytes. Stem Cells 31, 829–837 (2013).
Smolich, J.J. Ultrastructural and functional features of the developing mammalian heart: a brief overview. Reprod. Fertil. Dev. 7, 451–461 (1995).
Kane, C., Couch, L. & Terracciano, C.M. Excitation-contraction coupling of human induced pluripotent stem cell-derived cardiomyocytes. Front. Cell Dev. Biol. 3, 59 (2015).
Knollmann, B.C. Induced pluripotent stem cell-derived cardiomyocytes: boutique science or valuable arrhythmia model? Circ. Res. 112, 969–976 (2013).
Nunes, S.S. et al. Biowire: a platform for maturation of human pluripotent stem cell-derived cardiomyocytes. Nat. Methods 10, 781–787 (2013).
Chun, Y.W. et al. Combinatorial polymer matrices enhance in vitro maturation of human induced pluripotent stem cell-derived cardiomyocytes. Biomaterials 67, 52–64 (2015).
Ruan, J.L. et al. Mechanical stress promotes maturation of human myocardium from pluripotent stem cell-derived progenitors. Stem Cells 33, 2148–2157 (2015).
Rog-Zielinska, E.A. et al. Glucocorticoids promote structural and functional maturation of foetal cardiomyocytes: a role for PGC-1alpha. Cell Death Differ. 22, 1106–1116 (2015).
Yang, X. et al. Tri-iodo-l-thyronine promotes the maturation of human cardiomyocytes-derived from induced pluripotent stem cells. J. Mol. Cell. Cardiol. 72, 296–304 (2014).
Kadota, S., Pabon, L., Reinecke, H. & Murry, C.E. In vivo maturation of human induced pluripotent stem cell-derived cardiomyocytes in neonatal and adult rat hearts. Stem Cell Rep. 8, 278–289 (2017).
Cho, G.S. et al. Neonatal transplantation confers maturation of PSC-derived cardiomyocytes conducive to modeling cardiomyopathy. Cell Rep. 18, 571–582 (2017).
Laugwitz, K.L. et al. Postnatal isl1+ cardioblasts enter fully differentiated cardiomyocyte lineages. Nature 433, 647–653 (2005).
Genead, R. et al. Islet-1 cells are cardiac progenitors present during the entire lifespan: from the embryonic stage to adulthood. Stem Cells Dev. 19, 1601–1615 (2010).
Uosaki, H. & Taguchi, Y.H. Comparative gene expression analysis of mouse and human cardiac maturation. Genomics Proteomics Bioinformatics 14, 207–215 (2016).
Espuny-Camacho, I. et al. Hallmarks of Alzheimer's disease in stem-cell-derived human neurons transplanted into mouse brain. Neuron 93, 1066–1081 (2017).
Shenje, L.T. et al. Precardiac deletion of Numb and Numblike reveals renewal of cardiac progenitors. ELife 3, e02164 (2014).
Lee, D.I. et al. PDE5A suppression of acute beta-adrenergic activation requires modulation of myocyte beta-3 signaling coupled to PKG-mediated troponin I phosphorylation. Basic Res. Cardiol. 105, 337–347 (2010).
Tandon, N. et al. Electrical stimulation systems for cardiac tissue engineering. Nat. Protoc. 4, 155–173 (2009).
Shin, J. et al. Single-cell RNA-Seq with waterfall reveals molecular cascades underlying adult neurogenesis. Cell Stem Cell 17, 360–372 (2015).
Laflamme, M.A. et al. Cardiomyocytes derived from human embryonic stem cells in pro-survival factors enhance function of infarcted rat hearts. Nat. Biotechnol. 25, 1015–1024 (2007).
Acknowledgements
We thank Kwon laboratory members for critical reading and discussions. E.T. was supported by a Johns Hopkins School of Medicine Clinician Scientist Award. This work was supported by the Magic that Matters Fund and grants from the MSCRF (2015-MSCRFI-1622), NHLBI/NIH (R01HL111198) and NICHD/NIH (R01HD086026) to C.K.
Author information
Authors and Affiliations
Contributions
G.-S.C. and C.K. designed the experiments. G.-S.C., E.T. and P.A. performed the experiments. G.-S.C., E.T. and P.A. analyzed the data. E.T. and P.A. created the figures. E.T., G.-S.C., P.A. and C.K. wrote the manuscript. All authors approved the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 FACS gating strategy
A. FACS gating strategy for the sorting of live Isl-1+ mouse CPCs. First plot gating for live cells, then second plot for single and then only for Isl1-1+ RFP cells. B. FACS gating strategy for the analysis of human CPCs. The cells were fixed and stained with a primary mouse anti-Islet-1 antibody and a secondary far red (647 nm emission wavelength) conjugated antibody. First plot gating for fixed cells, then single cells and then Isl-1+ Far Red CPCs.
Supplementary Figure 2 Teratoma formation (asterisk) after injection of unsorted mouse ESC-derived cells
Arrow points to the dissected part of the heart.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1 and 2. (PDF 411 kb)
Rights and permissions
About this article
Cite this article
Cho, GS., Tampakakis, E., Andersen, P. et al. Use of a neonatal rat system as a bioincubator to generate adult-like mature cardiomyocytes from human and mouse pluripotent stem cells. Nat Protoc 12, 2097–2109 (2017). https://doi.org/10.1038/nprot.2017.089
Published:
Issue Date:
DOI: https://doi.org/10.1038/nprot.2017.089
This article is cited by
-
PGC1/PPAR drive cardiomyocyte maturation at single cell level via YAP1 and SF3B2
Nature Communications (2021)
-
Approaches to Optimize Stem Cell-Derived Cardiomyocyte Maturation and Function
Current Stem Cell Reports (2021)
-
Genome-wide association and multi-omic analyses reveal ACTN2 as a gene linked to heart failure
Nature Communications (2020)
-
Precardiac organoids form two heart fields via Bmp/Wnt signaling
Nature Communications (2018)
-
Harnessing cell pluripotency for cardiovascular regenerative medicine
Nature Biomedical Engineering (2018)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.