Abstract
The influence of cannabis on mental health receives growing scientific and political attention. An increasing demand for treatment of cannabis dependence has refueled the discussion about the addictive potential of cannabis. A key feature of all addictive drugs is the ability to increase synaptic dopamine levels in the striatum, a mechanism involved in their rewarding and motivating effects. However, it is currently unknown if cannabis can stimulate striatal dopamine neurotransmission in humans. Here we show that Δ9-tetrahydrocannabinol (THC), the main psychoactive component in cannabis, induces dopamine release in the human striatum. Using the dopamine D2/D3 receptor tracer [11C]raclopride and positron emission tomography in seven healthy subjects, we demonstrate that THC inhalation reduces [11C]raclopride binding in the ventral striatum and the precommissural dorsal putamen but not in other striatal subregions. This is consistent with an increase in dopamine levels in these regions. These results suggest that THC shares a potentially addictive property with other drugs of abuse. Further, it implies that the endogenous cannabinoid system is involved in regulating striatal dopamine release. This allows new directions in research on the effects of THC in neuropsychiatric disorders, such as schizophrenia.
Similar content being viewed by others
INTRODUCTION
The debate whether cannabis can be characterized as an addictive drug has been ongoing for many years (Grinspoon et al, 1997). Recently, a substantial increase in the demand for treatment of cannabis dependence has intensified this discussion (Hall, 2006). The rewarding properties of addictive drugs are thought to be mediated by their action on the mesolimbic dopamine system (for review see Wise, 2004; Hyman et al, 2006). This dopamine system originates in the ventral tegmental area and projects to the ventral striatum, which predominantly comprises the nucleus accumbens. Addictive drugs probably induce their rewarding effects by enhancement of synaptic dopamine levels in the ventral striatum (Wise, 2004; Hyman et al, 2006). In the human striatum, increased dopamine levels have been found with the use of neuroimaging techniques after the administration of amphetamine (Laruelle et al, 1996; Breier et al, 1997; Drevets et al, 2001; Martinez et al, 2003, 2007), cocaine (Schlaepfer et al, 1997), alcohol (Boileau et al, 2003), and nicotine (Brody et al, 2004, 2006). In animals, it has been demonstrated that cannabinoid substances such as Δ9-tetrahydrocannabinol (THC), the main psychoactive component in cannabis (Gaoni and Mechoulam, 1964), also stimulate striatal dopamine neurotransmission (for review see Tanda and Goldberg, 2003; Lupica et al, 2004; Gardner, 2005). Cannabinoids enhance neuronal firing of mesolimbic dopamine neurons (French, 1997; French et al, 1997; Gessa et al, 1998) and elevate striatal dopamine levels (Ng Cheong Ton et al, 1988; Chen et al, 1990; Tanda et al, 1997; Malone and Taylor, 1999; Fadda et al, 2006), both through activation of cannabinoid CB1 receptors (French, 1997; French et al, 1997; Tanda et al, 1997; Gessa et al, 1998; Malone and Taylor, 1999). However, whether THC affects the human striatal dopamine system is currently unknown.
The purpose of the present study was to investigate whether THC can induce dopamine release in the striatum of healthy human subjects. This was assessed using positron emission tomography (PET) and the dopamine D2/D3 receptor ligand [11C]raclopride. With this method, an increase in striatal synaptic dopamine concentrations can be determined by a reduction in [11C]raclopride binding (Breier et al, 1997; Laruelle et al, 1997). On the basis of findings from animal studies, our hypothesis was that THC should reduce [11C]raclopride binding in the human striatum, consistent with striatal dopamine release.
MATERIALS AND METHODS
Subjects
Healthy male subjects were recruited through advertisements on the Internet. All subjects had a history of mild cannabis use for at least 1 year, defined as using cannabis more than four times a year and at most once a week. In addition, it was required that they never experienced psychotic effects after cannabis use and did not meet criteria for ‘Paranoid Ideation’ or ‘Psychoticism’ on the self-report symptom checklist SCL-90 (Derogatis, 1983). Mild cannabis users were selected as they a priori could be expected to tolerate the THC challenge used in this experiment although not having long-term effects associated with frequent cannabis use. All subjects were in good physical health as assessed by medical history, physical examination, electrocardiogram (ECG), and routine laboratory tests. Urine screening for cannabis, amphetamine, cocaine, and morphine was performed at screening and on both study days. Subjects with a positive drug test on other drugs than cannabis were excluded from the study. Subjects with a positive cannabis test at screening were tested again, and were required to be negative before the first study day. Subjects were excluded from participation in case of history of alcohol or drug abuse and in case of major current psychiatric diagnosis. In addition, subjects were excluded if they, or a first- or second-degree relative, had a lifetime history of a clinically significant psychiatric or neurological illness. Use of medication at the time of the study was not allowed. All volunteers gave written informed consent before entry into the study. The study was approved by the Medical Research Ethics Committee of the University Medical Center Utrecht, the Netherlands.
Design and Procedure
In a double-blind, randomized, placebo-controlled, crossover study, subjects had two PET scans after either administration of THC or placebo. Scanning sessions were separated by at least 2 weeks to allow for complete clearance of drug between both occasions. Subjects arrived 2 h before the start of the scanning procedure at the Department of Nuclear Medicine and PET Research of the VU University Medical Center in Amsterdam, the Netherlands, having fasted for at least 4 h before their arrival. Subjects refrained from cannabis for at least 2 weeks before the first study day until study completion and from alcohol for 24 h before each study day. Caffeine intake and smoking were not allowed on study days. Use of drugs of abuse, including cannabis, was checked with urine drug screenings, which had to be negative on the day of the PET scans. Use of alcohol, caffeine, and nicotine was checked by self-report. A standard breakfast or lunch was served and venous catheters were placed in each arm, one for [11C]raclopride infusion and the other for venous blood sampling.
Drugs and Administration
Preparation and administration of drugs was performed according to Zuurman et al (2008). THC was purified from Cannabis sativa according to GMP-compliant procedures (Farmalyse BV, Zaandam, the Netherlands) and was dissolved in 200 μl 100 vol% alcohol. The solvent was used as placebo. Drugs were administered using a Volcano® vaporizer (Storz–Bickel GmbH, Tuttlingen, Germany). Five minutes before administration, 8 mg of THC was vaporized into an opaque polythene bag equipped with a valved mouthpiece, preventing the loss of THC in between inhalations. Subjects inhaled the volume of this bag in three or four subsequent breaths, holding their breath for 10 s after each inhalation. They were not allowed to speak during the inhalation process, which was practiced at screening using placebo.
Production of [11C]raclopride
[11C]Raclopride was synthesized by methylation of O-desmethyl raclopride (obtained from ABX, Radeberg, Germany) with 11CH3I in dimethylsulfoxide at 80°C for 5 min, utilizing a Nuclear Interface methylation synthesis module. The resulting product was purified from the reaction mixture by HPLC (μbondapak 7.8 × 300; 0.01 M H3PO4/MeCN 70 : 30, 5 ml/min, UV at 254 nm). The collected fraction containing [11C]raclopride was diluted with 40 ml of 1 mM NaOH in water and this mixture was subsequently passed over a tC18 SepPak. After washing the SepPak with 20 ml of water for injection, [11C]raclopride was eluted from the SepPak with 1.2 ml of sterile ethanol and a sterile solution of NaH2PO4 in saline (7.1 mM, pH 5.4). The final solution was transferred to a sterile product vial by a sterile 0.22 μm MIllex GV filter, yielding a sterile, pyrogen free solution of [11C]raclopride with a (radio)chemical purity of >98% whereas the specific activity ranged from 26 to 104 GBq/μmol at time of injection. The complete production procedure was performed in accordance with the EU guideline ‘Eudralex volume 4: Good Manufacturing Practices’ and were approved by the Dutch health authorities (license number 107627A).
Positron Emission Tomography
PET scans were performed on an ECAT EXACT HR+ scanner (Siemens/CTI, Knoxville, TN, USA), which is located at the Department of Nuclear Medicine and PET Research of the VU University Medical Center in Amsterdam, the Netherlands. This scanner enables the acquisition of 63 transaxial planes over a 15.5 cm axial field of view, thus allowing the whole brain to be imaged.
Five minutes after inhalation of placebo or THC, [11C]raclopride was given as a bolus plus constant infusion. [11C]Raclopride was delivered in a 50 ml volume and administered by a computer operated infusion pump (Med-Rad, Beek, the Netherlands). First, a bolus dose of 28 ml was given over 3.1 min, followed by constant infusion of 22 ml at 0.15 ml/h for 88 min. Thus, the bolus to infusion ratio (Kbol) was 112 min (Carson et al, 1997). A 40 min scanning period with eight successive frames of 5 min was initiated 40 min after the start of [11C]raclopride administration. Finally, a transmission scan of 10 min was performed to correct for photon attenuation. Correction for emission contamination was performed using the dwell profile method (van der Weerdt et al, 2004).
Image Reconstruction
All PET sinograms were corrected for dead time, decay, randoms, scatter, and tissue attenuation. All PET emission scans were reconstructed with FORE+2D FBP using a 0.5 Hanning filter, resulting in a transaxial spatial resolution of ∼7 mm in the center of the field of view. Images were then transferred to workstations (Sun Microsystems, Santa Clara, CA, USA) for further analysis.
Behavioral, Subjective, and Physiological Measurements
Behavioral ratings were assessed with the 18-item Brief Psychiatric Rating Scale (BPRS; Overall and Gorham, 1962). This structured interview was performed at baseline and 21 and 102 min after THC administration. Total BPRS scores were analyzed together with scores for the factors thinking disorder (BPRS items: conceptual disorganization, hallucinatory behavior, and unusual thought content), withdrawal–retardation (BPRS items: blunted affect and emotional withdrawal), anxiety–depression (BPRS items: anxiety, guilt feelings, and depressive mood), and hostility–suspiciousness (BPRS items: hostility, suspiciousness, and uncooperativeness) (Hedlund and Vieweg, 1980).
A rating scale consisting of 16 visual analogue scales was used to determine subjective effects. From these analogue scales three factors were calculated, corresponding to alertness, contentedness, and calmness (Bond and Lader, 1974). Psychedelic effects were assessed using an adapted version of a 13-item visual analogue rating scale, originally described by Bowdle and colleagues (Bowdle et al, 1998; Zuurman et al, 2008). The visual analogue scale (VAS) ‘feeling high’ was analyzed individually and composite scores of ‘external perception’ and ‘internal perception’ were calculated (Zuurman et al, 2008). Both rating scales were performed consecutively at baseline and 7, 12, 17, 32, and 100 min after THC administration.
ECG was monitored continuously whereas blood pressure and heart rate were measured at baseline and 6, 11, 15, 19, 34, 49, 64, 79, and 94 min after start of THC administration.
Blood Sampling
Venous blood samples were collected to determine plasma concentrations of THC and its two most important metabolites, 11-OH-THC and 11-nor-9-carboxy-THC. Blood samples were withdrawn 5, 10, 20, 35, 55, and 90 min after THC administration and processed according to Zuurman et al (2008). Additional venous blood samples were withdrawn 40, 60, 70, and 80 min after start of [11C]raclopride administration to measure [11C]raclopride metabolism. These samples were processed according to Schuit et al (2007).
Magnetic Resonance Imaging
Magnetic resonance imaging (MRI) of all subjects was performed at the Department of Radiology of the University Medical Center in Utrecht, the Netherlands, for anatomical definition. MRI scans were acquired using a 1.5 T scanner (Philips Gyroscan; Philips Medical Systems, Best, the Netherlands). T1-weighted, 3D, fast field echo scans with 160–180 1.2 mm contiguous coronal slices (echo time, 4.6 ms; repetition time, 30 ms; flip angle 301; field of view 256 mm; Hulshoff Pol et al, 2001) were used.
Regions of Interest
All MRI scans were rotated to acquire horizontal lines between anterior and posterior commissures (AC–PC line) in the sagittal plane. Then the striatum was divided into five anatomical regions of interest (ROI; see Figure 1; Table 1), according to published criteria (Mawlawi et al, 2001; Martinez et al, 2003). These ROIs were delineated on MRI scans oriented in the coronal plane using DISPLAY. ROIs were defined for ventral striatum, precommissural dorsal caudate, precommissural dorsal putamen, postcommisural caudate, and postcommissural putamen. These ROIs were classified into three functional subdivisions: limbic striatum (ventral striatum), associative striatum (consisting of precommissural dorsal caudate, precommissural dorsal putamen, and postcommisural caudate), and sensorimotor striatum (postcommissural putamen; Mawlawi et al, 2001; Martinez et al, 2003). Cerebellar hemispheres were also defined on the MRI scans. After reconstruction, individual PET frames were co-registered to the first frame to correct for motion and summed over all frames. These summed PET images were co-registered to the rotated MRI scan using VINCI software (Cizek et al, 2004). After projection of the ROIs on the co-registered summed PET images, activity was calculated for each ROI as the volume weighted average of left and right regions. Activity in associative striatum was derived as the volume weighted average of precommissural dorsal caudate, precommissural dorsal putamen, and postcommisural caudate, whereas activity in striatum as a whole was calculated as the volume weighted average of all five ROIs (Table 1).
Coronal slices of (left) PET [11C]raclopride and (right) co-registered magnetic resonance imaging (MRI) scans at the level of the striatum, (a) anterior and (b) posterior to the AC-plane. Striatal subregions are indicated on the MRI scans: ventral striatum (yellow), precommissural dorsal putamen (green), precommissural dorsal caudate (red), postcommissural putamen (purple), and postcommissural caudate (blue).
Outcome Measures
Nondisplaceable binding potential (BPND; Innis et al, 2007) was used as measure of dopamine D2/D3 receptor availability. BPND was defined as the distribution volume ratio (DVR) minus 1 (Lammertsma et al, 1996). As scans were performed during steady state, DVR could be obtained using the average activity concentration in a ROI divided by that of the cerebellum ROI, which was used as reference. In this way, BPND was calculated for all ROIs for both scanning sessions.
Statistical Analysis
Group differences in BPND between placebo and THC were analyzed using repeated measures ANOVA with ROI and drug as factors. Post hoc analysis was performed for each ROI using paired t-tests. Behavioral, subjective, psychedelic, and physiological effects were corrected for baseline values and also analyzed using repeated measures ANOVA with drug and time as factors. Post hoc analysis was performed using paired t-tests. Therefore, a mean score was calculated for each parameter and compared between placebo and THC. Differences in PET scan parameters and [11C]raclopride concentrations were measured using paired t-tests. A p-value less than 0.05 was considered statistically significant.
RESULTS
Subjects
Nine healthy male subjects gave informed consent for this study. Seven volunteers completed the study procedure. One subject was excluded because of positive urine drug screening on the first study day. Another subject did not complete the second scanning session because of anxiety. Mean age of the seven subjects was 21.9±2.7 years (range 20–27). Mean height, weight, and BMI were 183±8 cm (range 172–196), 80±9 kg (range 72–98), and 23.8±0.9 kg/m2 (range 22.9–25.5), respectively. All subjects were familiar with the effects of cannabis. Two subjects used cannabis less than once a month, one subject three times a month, three subjects twice a month and one subject used cannabis once a week. They all showed negative urine screening at both study days.
PET Scan Parameters
Mean injected dose of [11C]raclopride was similar between placebo (770±30 MBq) and THC sessions (810±90 MBq; p=0.254). In addition, total mass of administered raclopride (6.1±2.3 and 4.6±1.5 μmol for placebo and THC sessions, respectively; p=0.181) was not significantly different between sessions.
There were no significant changes in equilibrium levels of striatal activity, expressed by percentage change of activity concentration over time, between placebo (−0.10±0.16% per min) and THC (−0.12±0.08% per min) sessions (p=0.633). In addition, the slope (ie change over time during scanning) of the ratio between striatum and cerebellum [11C]raclopride concentrations was not significantly different between sessions (−0.0011±0.0030 and −0.0010±0.0025 for placebo and THC sessions, respectively; p=0.967).
Blood Sample Analysis
THC plasma concentration reached a maximum of 143±91 ng/ml 5 min after inhalation, decreasing rapidly thereafter. Plasma concentrations of the main metabolites of THC, 11-OH-THC, and 11-nor-9-carboxy-THC, peaked at 10 min (6±2 ng/ml) and 20 min (18±5 ng/ml) after inhalation, respectively (Figure 2).
[11C]Raclopride concentrations were not significantly different between placebo and THC sessions in both whole blood (0.59±0.25 and 0.61±0.28 kBq/g, respectively; p=0.717) and plasma (1.02±0.42 and 1.06±0.43 kBq/g, respectively; p=0.687), normalized to the effectively injected dose. In addition, the fraction of parent [11C]raclopride was not significantly different (p=0.191) between placebo (80.4±5.6%) and THC (77.5±4.3%).
Dopamine D2/D3 Receptor Availability
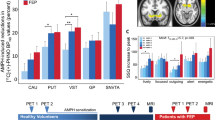
BPND of [11C]raclopride, reflecting dopamine D2/D3 receptor availability, was significantly reduced in the ventral striatum and the precommissural dorsal putamen after inhalation of THC compared to placebo (−3.43±3.70%, p=0.029 and −3.88±4.07%, p=0.042, respectively; Figure 3). In other subdivisions of the striatum no significant differences were found between THC and placebo (Table 1).
Behavioral, Subjective, and Physiological Measurements
Analysis of variance revealed a significant drug × time effect on the BPRS total score (F(2,12)=11.28, p=0.002) and on the BPRS composite score withdrawal–retardation (F(2,12)=18.23, p<0.001). THC-induced significant increases in VAS scores of ‘feeling high’ (F(5,30)=3.88, p=0.008), ‘external perception’ (F(5,30)=2.91, p=0.029) and ‘calmness’ (F(5,30)=3.22, p=0.019), and a decrease on ‘alertness’ (F(5,30)=3.07, p=0.024). Heart rate increased significantly after THC compared with placebo (F(9,54)=9.36, p<0.001). Behavioral, subjective, and physiological measurements are summarized in Table 2 and Table 3. No significant associations between measures of dopamine release and behavioral, subjective or physiological effects were demonstrated.
DISCUSSION
This study examined the effects of THC inhalation on [11C]raclopride specific binding in seven healthy volunteers, finding a reduction in the ventral striatum and precommissural dorsal putamen. The reduction in [11C]raclopride specific binding is consistent with an increase in dopamine levels in these regions.
This is the first study demonstrating THC-induced dopamine release in the human striatum. This result is in line with animal findings, showing enhanced neuronal firing of mesolimbic dopamine neurons after administration of cannabinoids (French, 1997; French et al, 1997; Gessa et al, 1998). In addition, it is consistent with microdialysis studies demonstrating that cannabinoids induce elevated striatal dopamine levels (Ng Cheong Ton et al, 1988; Chen et al, 1990; Tanda et al, 1997; Malone and Taylor, 1999; Fadda et al, 2006). These effects are dependent on the activation of cannabinoid CB1 receptors (French, 1997; French et al, 1997; Tanda et al, 1997; Gessa et al, 1998; Malone and Taylor, 1999).
The ability of THC to induce dopamine release in the human striatum suggests that THC shares addictive properties with other drugs of abuse. Dopamine release in the striatum is a key feature of all addictive drugs, specifically involved in their rewarding effects and in the formation of reward related associations (Wise, 2004; Hyman et al, 2006). However, whereas amphetamine (Drevets et al, 2001; Martinez et al, 2003, 2007), cocaine (Schlaepfer et al, 1997), alcohol (Boileau et al, 2003), and nicotine (Brody et al, 2004, 2006) cause reductions in dopamine D2/D3 receptor availability in the range of 10–30%, we found a relatively modest THC-induced decrease of 3.4 and 3.9% in the ventral striatum and the precommissural dorsal putamen, respectively. Interestingly, this modest decrease in [11C]raclopride binding is consistent with the moderate increase in striatal dopamine levels measured after administration of THC in animals (Ng Cheong Ton et al, 1988; Chen et al, 1990; Tanda et al, 1997; Malone and Taylor, 1999). Assuming a ratio between increase in dopamine levels and reduction in [11C]raclopride binding of approximately 40 : 1 (Breier et al, 1997; Laruelle et al, 1997), our data indicate an increase in dopamine concentrations in the ventral striatum of 136%. This is in line with the THC-induced increase in striatal dopamine levels as demonstrated in microdialysis studies (Ng Cheong Ton et al, 1988; Chen et al, 1990; Tanda et al, 1997; Malone and Taylor, 1999).
As THC was dissolved in 100 vol% alcohol and the solvent was used as placebo, we cannot exclude that the inhalation of alcohol has caused dopamine release. However, this is very unlikely, as only 200 μl alcohol was administered. Please note that the placebo scan was subtracted from the THC scan and both conditions contained the same amount of alcohol.
THC-induced well-known behavioral, subjective, and physiological effects (D’Souza et al, 2004; Ilan et al, 2005) in our subjects, replicating effects caused by the highest dose of THC administered in previous research using the same vaporizing device (Strougo et al, 2008; Zuurman et al, 2008). In addition, THC plasma concentrations in this study were comparable with or even higher than those obtained after smoking of high-potency cannabis (Huestis et al, 1992; Ramaekers et al, 2006). Thus, our results indicate that a relatively high dose of THC induces a moderate degree of dopamine release in the human striatum. This effect may be explained by the indirect effects of THC on striatal dopamine levels through cannabinoid CB1 receptors on glutamate and GABA neurons in the nucleus accumbens and the ventral tegmental area (Schlicker and Kathmann, 2001; Lupica et al, 2004). Other drugs of abuse have more direct effects on the dopamine system (Koob et al, 1998; Hyman et al, 2006).
As the PET scan was performed around 45–85 min after inhalation of THC it could be argued that most of the effect of THC on dopamine release had dissipated at the time of the scan. By this time, plasma concentrations of THC were only 2.0–4.4% of the maximum concentration. However, pharmacokinetic/pharmacodynamic (PK/PD) models that have been described recently indicate that central nervous system effects of THC last much longer than suggested by the rapid decline of plasma concentrations (Strougo et al, 2008). Application of these PK/PD-models to this study showed that 84.5–95.9% of the maximum CNS-effects were still present during acquisition of the PET scan. These findings suggest that it is unlikely that striatal dopamine release immediately after THC administration has been much larger than the modest levels of 3.4–3.9% that were observed around 45 min after administration. Indeed, effects on VAS ‘feeling high’ that were reported 101 min after inhalation were still significant.
Moreover, it is known that drug-induced effects on dopamine D2/D3 receptor availability last longer than changes in synaptic dopamine concentrations (Breier et al, 1997; Laruelle et al, 1997). In humans, [11C]raclopride BP was still decreased 6 h after amphetamine administration (Cardenas et al, 2004). This is probably because of an internalization of dopamine receptors (Laruelle, 2000), indicating that a drug-induced effect on striatal dopamine release can be detected for a long time after administration.
Our finding of THC-induced release of dopamine in the striatum suggests that human striatal dopamine release is under control of the endogenous cannabinoid system. The exact mechanism is still unclear, but cannabinoid CB1 receptors on glutamate and GABA terminals in both the nucleus accumbens and the ventral tegmental area are involved in the regulation of dopamine release in the striatum (Schlicker and Kathmann, 2001; Lupica et al, 2004). Interestingly, it is known that cannabis use increases the risk for developing schizophrenia (Arseneault et al, 2004; Moore et al, 2007) and worsens its clinical outcome (Linszen et al, 1994; D’Souza et al, 2005). Schizophrenia is an illness that has consistently been related to increased dopamine function in the striatum (Seeman and Lee, 1975; Angrist and Van Kammen, 1984), possibly caused by disinhibition of striatal dopamine transmission (Laruelle et al, 1996; Breier et al, 1997). Thus, elevated striatal dopamine release after the use of cannabis may explain how cannabis use contributes to the development and pathophysiology of schizophrenia.
In conclusion, we have demonstrated that Δ9-THC, the main psychoactive component of cannabis, induces dopamine release in the human striatum. This finding implies that THC may share a putatively addictive property with other drugs of abuse and that the endogenous cannabinoid system is involved in regulating striatal dopamine release, possibly explaining some of the detrimental effects of THC in neuropsychiatric disorders such as schizophrenia.
References
Angrist B, Van Kammen DP (1984). CNS stimulants as tools in the study of schizophrenia. Trends Neurosci 7: 388–390.
Arseneault L, Cannon M, Witton J, Murray RM (2004). Causal association between cannabis and psychosis: examination of the evidence. Br J Psychiatry 184: 110–117.
Boileau I, Assaad JM, Pihl RO, Benkelfat C, Leyton M, Diksic M et al (2003). Alcohol promotes dopamine release in the human nucleus accumbens. Synapse 49: 226–231.
Bond A, Lader M (1974). The use of analogue scales in rating subjective feelings. Br J Med Psychol 47: 211–218.
Bowdle TA, Radant AD, Cowley DS, Kharasch ED, Strassman RJ, Roy-Byrne PP (1998). Psychedelic effects of ketamine in healthy volunteers: relationship to steady-state plasma concentrations. Anesthesiology 88: 82–88.
Breier A, Su TP, Saunders R, Carson RE, Kolachana BS, De Bartolomeis A et al (1997). Schizophrenia is associated with elevated amphetamine-induced synaptic dopamine concentrations: evidence from a novel positron emission tomography method. Proc Natl Acad Sci USA 94: 2569–2574.
Brody AL, Mandelkern MA, Olmstead RE, Scheibal D, Hahn E, Shiraga S et al (2006). Gene variants of brain dopamine pathways and smoking-induced dopamine release in the ventral caudate/nucleus accumbens. Arch Gen Psychiatry 63: 808–816.
Brody AL, Olmstead RE, London ED, Farahi J, Meyer JH, Grossman P et al (2004). Smoking-induced ventral striatum dopamine release. Am J Psychiatry 161: 1211–1218.
Cardenas L, Houle S, Kapur S, Busto UE (2004). Oral D-amphetamine causes prolonged displacement of [11C]raclopride as measured by PET. Synapse 51: 27–31.
Carson RE, Breier A, de Bartolomeis A, Saunders RC, Su TP, Schmall B et al (1997). Quantification of amphetamine-induced changes in [11C]raclopride binding with continuous infusion. J Cereb Blood Flow Metab 17: 437–447.
Chen JP, Paredes W, Li J, Smith D, Lowinson J, Gardner EL (1990). Delta 9-tetrahydrocannabinol produces naloxone-blockable enhancement of presynaptic basal dopamine efflux in nucleus accumbens of conscious, freely-moving rats as measured by intracerebral microdialysis. Psychopharmacology (Berl) 102: 156–162.
Cizek J, Herholz K, Vollmar S, Schrader R, Klein J, Heiss WD (2004). Fast and robust registration of PET and MR images of human brain. NeuroImage 22: 434–442.
D’Souza DC, Abi-Saab WM, Madonick S, Forselius-Bielen K, Doersch A, Braley G et al (2005). Delta-9-tetrahydrocannabinol effects in schizophrenia: implications for cognition, psychosis, and addiction. Biol Psychiatry 57: 594–608.
D’Souza DC, Perry E, MacDougall L, Ammerman Y, Cooper T, Wu YT et al (2004). The psychotomimetic effects of intravenous delta-9-tetrahydrocannabinol in healthy individuals: implications for psychosis. Neuropsychopharmacology 29: 1558–1572.
Derogatis JR (1983). SCL-90-R: Administration, Scoring, and Procedures Manual—II. Clinical Psychometric Research: Townson.
Drevets WC, Gautier C, Price JC, Kupfer DJ, Kinahan PE, Grace AA et al (2001). Amphetamine-induced dopamine release in human ventral striatum correlates with euphoria. Biol Psychiatry 49: 81–96.
Fadda P, Scherma M, Spano MS, Salis P, Melis V, Fattore L et al (2006). Cannabinoid self-administration increases dopamine release in the nucleus accumbens. Neuroreport 17: 1629–1632.
French ED (1997). Delta9-tetrahydrocannabinol excites rat VTA dopamine neurons through activation of cannabinoid CB1 but not opioid receptors. Neurosci Lett 226: 159–162.
French ED, Dillon K, Wu X (1997). Cannabinoids excite dopamine neurons in the ventral tegmentum and substantia nigra. Neuroreport 8: 649–652.
Gaoni Y, Mechoulam R (1964). Isolation, structure and partial synthesis of an active constituent of hashish. J Am Chem Soc 86: 1646–1647.
Gardner EL (2005). Endocannabinoid signaling system and brain reward: emphasis on dopamine. Pharmacol Biochem Behav 81: 263–284.
Gessa GL, Melis M, Muntoni AL, Diana M (1998). Cannabinoids activate mesolimbic dopamine neurons by an action on cannabinoid CB1 receptors. Eur J Pharmacol 341: 39–44.
Grinspoon L, Bakalar JB, Zimmer L, Morgan JP (1997). Marijuana addiction. Science 277: 749.
Hall W (2006). The mental health risks of adolescent cannabis use. PLoS Med 3: 159–162.
Hedlund JL, Vieweg BW (1980). The Brief Psychiatric Rating Scale (BPRS): a comprehensive review. J Oper Psychiatry 11: 48–65.
Huestis MA, Henningfield JE, Cone EJ (1992). Blood cannabinoids. I. Absorption of THC and formation of 11-OH-THC and THCCOOH during and after smoking marijuana. J Anal Toxicol 16: 276–282.
Hulshoff Pol HE, Schnack HG, Mandl RC, van Haren NE, Koning H, Collins DL et al (2001). Focal gray matter density changes in schizophrenia. Arch Gen Psychiatry 58: 1118–1125.
Hyman SE, Malenka RC, Nestler EJ (2006). Neural mechanisms of addiction: the role of reward-related learning and memory. Annu Rev Neurosci 29: 565–598.
Ilan AB, Gevins A, Coleman M, ElSohly MA, De Wit H (2005). Neurophysiological and subjective profile of marijuana with varying concentrations of cannabinoids. Behav Pharmacol 16: 487–496.
Innis RB, Cunningham VJ, Delforge J, Fujita M, Gjedde A, Gunn RN et al (2007). Consensus nomenclature for in vivo imaging of reversibly binding radioligands. J Cereb Blood Flow Metab 27: 1533–1539.
Koob GF, Sanna PP, Bloom FE (1998). Neuroscience of addiction. Neuron 21: 467–476.
Lammertsma AA, Bench CJ, Hume SP, Osman S, Gunn K, Brooks DJ et al (1996). Comparison of methods for analysis of clinical [11C]raclopride studies. J Cereb Blood Flow Metab 16: 42–52.
Laruelle M (2000). Imaging synaptic neurotransmission with in vivo binding competition techniques: a critical review. J. Cereb. Blood Flow Metab 20: 423–451.
Laruelle M, Abi-Dargham A, van Dyck CH, Gil R, D'Souza CD, Erdos J et al (1996). Single photon emission computerized tomography imaging of amphetamine-induced dopamine release in drug-free schizophrenic subjects. Proc Natl Acad Sci USA 93: 9235–9240.
Laruelle M, Iyer RN, Al-Tikriti MS, Zea-Ponce Y, Malison R, Zoghbi SS et al (1997). Microdialysis and SPECT measurements of amphetamine-induced dopamine release in nonhuman primates. Synapse 25: 1–14.
Linszen DH, Dingemans PM, Lenior ME (1994). Cannabis abuse and the course of recent-onset schizophrenic disorders. Arch Gen Psychiatry 51: 273–279.
Lupica CR, Riegel AC, Hoffman AF (2004). Marijuana and cannabinoid regulation of brain reward circuits. Br J Pharmacol 143: 227–234.
Malone DT, Taylor DA (1999). Modulation by fluoxetine of striatal dopamine release following Delta9-tetrahydrocannabinol: a microdialysis study in conscious rats. Br J Pharmacol 128: 21–26.
Martinez D, Narendran R, Foltin RW, Slifstein M, Hwang DR, Broft A et al (2007). Amphetamine-induced dopamine release: markedly blunted in cocaine dependence and predictive of the choice to self-administer cocaine. Am J Psychiatry 164: 622–629.
Martinez D, Slifstein M, Broft A, Mawlawi O, Hwang DR, Huang Y et al (2003). Imaging human mesolimbic dopamine transmission with positron emission tomography. Part II: amphetamine-induced dopamine release in the functional subdivisions of the striatum. J Cereb Blood Flow Metab 23: 285–300.
Mawlawi O, Martinez D, Slifstein M, Broft A, Chatterjee R, Hwang DR et al (2001). Imaging human mesolimbic dopamine transmission with positron emission tomography: I. Accuracy and precision of D(2) receptor parameter measurements in ventral striatum. J Cereb Blood Flow Metab 21: 1034–1057.
Moore TH, Zammit S, Lingford-Hughes A, Barnes TR, Jones PB, Burke M et al (2007). Cannabis use and risk of psychotic or affective mental health outcomes: a systematic review. Lancet 370: 319–328.
Ng Cheong Ton JM, Gerhardt GA, Friedemann M, Etgen AM, Rose GM, Sharpless NS et al (1988). The effects of delta 9-tetrahydrocannabinol on potassium-evoked release of dopamine in the rat caudate nucleus: an in vivo electrochemical and in vivo microdialysis study. Brain Res 451: 59–68.
Overall JE, Gorham DR (1962). The Brief Psychiatric Rating Scale. Psychol Rep 10: 799–812.
Ramaekers JG, Kauert G, van Ruitenbeek P, Theunissen EL, Schneider E, Moeller MR (2006). High-potency marijuana impairs executive function and inhibitory motor control. Neuropsychopharmacology 31: 2296–2303.
Schlaepfer TE, Pearlson GD, Wong DF, Marenco S, Dannals RF (1997). PET study of competition between intravenous cocaine and [11C]raclopride at dopamine receptors in human subjects. Am J Psychiatry 154: 1209–1213.
Schlicker E, Kathmann M (2001). Modulation of transmitter release via presynaptic cannabinoid receptors. Trends Pharmacol Sci 22: 565–572.
Schuit RC, Luurtsema G, Greuter HNJM, Hendrikse NH, Windhorst AD, van Berckel BN et al (2007). Intravenous amphetamine administration does not affect metabolism of [11C]raclopride. J Labelled Compd Rad 50: S471.
Seeman P, Lee T (1975). Antipsychotic drugs: direct correlation between clinical potency and presynaptic action on dopamine neurons. Science 188: 1217–1219.
Strougo A, Zuurman L, Roy C, Pinquier JL, van Gerven JM, Cohen AF et al (2008). Modelling of the concentration–effect relationship of THC on central nervous system parameters and heart rate—insight into its mechanisms of action and a tool for clinical research and development of cannabinoids. J Psychopharmacol. 2008 June 26 [E-pub ahead of print].
Tanda G, Goldberg SR (2003). Cannabinoids: reward, dependence, and underlying neurochemical mechanisms—a review of recent preclinical data. Psychopharmacology (Berl) 169: 115–134.
Tanda G, Pontieri FE, Di Chiara G (1997). Cannabinoid and heroin activation of mesolimbic dopamine transmission by a common mu1 opioid receptor mechanism. Science 276: 2048–2050.
van der Weerdt AP, Boellaard R, Knaapen P, Visser CA, Lammertsma AA, Visser FC (2004). Postinjection transmission scanning in myocardial 18F-FDG PET studies using both filtered backprojection and iterative reconstruction. J Nucl Med 45: 169–175.
Wise RA (2004). Dopamine, learning and motivation. Nat Rev Neurosci 5: 483–494.
Zuurman L, Roy C, Schoemaker RC, Hazekamp A, Den Hartigh J, Bender JC et al (2008). Effect of intrapulmonary THC administration in humans. J Psychopharmacol. 2008 May 30 [E-pub ahead of print].
Acknowledgements
We thank Storz and Bickel for kindly supplying the Volcano vaporizer, the BV Cyclotron VU for providing 11CO2 and Reina Kloet for help with data analysis.
Author information
Authors and Affiliations
Corresponding author
Additional information
DISCLOSURE/CONFLICT OF INTEREST
The authors declare that no financial support or compensation has been received from any individual or corporate entity over the past 3 years for research or professional service and there are no personal financial holdings that could be perceived as constituting a potential conflict of interest.
Rights and permissions
About this article
Cite this article
Bossong, M., van Berckel, B., Boellaard, R. et al. Δ9-Tetrahydrocannabinol Induces Dopamine Release in the Human Striatum. Neuropsychopharmacol 34, 759–766 (2009). https://doi.org/10.1038/npp.2008.138
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/npp.2008.138
Keywords
This article is cited by
-
Associations between cannabis use, cannabis use disorder, and mood disorders: longitudinal, genetic, and neurocognitive evidence
Psychopharmacology (2022)
-
Cannabinoids, reward processing, and psychosis
Psychopharmacology (2022)
-
Is resting-state functional connectivity altered in regular cannabis users? A systematic review of the literature
Psychopharmacology (2022)
-
Dopamine, behavior, and addiction
Journal of Biomedical Science (2021)
-
A systematic review of neuroimaging and acute cannabis exposure in age-of-risk for psychosis
Translational Psychiatry (2021)