Abstract
Lung stem/progenitor cells are potentially useful for regenerative therapy, for example in repairing damaged or lost lung tissue in patients. Several optical imaging methods and probes have been used to track how stem cells incorporate and regenerate themselves in vivo over time. However, these approaches are limited by photobleaching, toxicity and interference from background tissue autofluorescence. Here we show that fluorescent nanodiamonds, in combination with fluorescence-activated cell sorting, fluorescence lifetime imaging microscopy and immunostaining, can identify transplanted CD45–CD54+CD157+ lung stem/progenitor cells in vivo, and track their engraftment and regenerative capabilities with single-cell resolution. Fluorescent nanodiamond labelling did not eliminate the cells’ properties of self-renewal and differentiation into type I and type II pneumocytes. Time-gated fluorescence imaging of tissue sections of naphthalene-injured mice indicates that the fluorescent nanodiamond-labelled lung stem/progenitor cells preferentially reside at terminal bronchioles of the lungs for 7 days after intravenous transplantation.
Similar content being viewed by others
Main
The lung is a complex organ consisting of at least 40 different cell lineages1. Following postnatal growth, the lung epithelium slowly turns over under normal conditions, but its regenerative capacity can be activated substantially after injury2. Resident lung stem/progenitor cells (referred to collectively as LSCs throughout this Article) are responsible for this epithelial repair and tissue homeostasis. Several stem cell niches have been identified as being located in terminal bronchioles or bronchoalveolar junctions3,4,5,6. These putative LSCs are susceptible to infection by severe acute respiratory syndrome (SARS) associated coronavirus6,7, leading to deterioration of lung tissue and loss of lung repair capacity. LSCs have also been found to be able to renew and proliferate to form epithelial cells in vivo4. They are potentially useful in regenerative therapy, for example, in repairing damaged lung tissue in patients. The advances and obstacles of using various strategies and assays to establish the regenerative potential of endogenous LSCs have been reviewed recently8,9.
To enable the aforementioned therapeutic applications of LSCs, it is crucial to determine their tissue-specific engraftment and regenerative capacity in animals. Achieving this goal requires the use of a highly sensitive imaging modality, together with a highly stable (both biologically and photophysically) imaging probe, to allow tracking of the transplanted cells in vivo over an extended period of time. Compared with magnetic resonance imaging (MRI), optical imaging offers the advantages of higher sensitivity, larger in vitro and in vivo throughputs, and greater potential for clinical translation10. However, existing fluorescence-based technologies such as dye labelling11 and in vitro transfection of cells with plasmids to express fluorescent proteins (for example, GFP)12,13 or non-fluorescent compounds (for example, luciferase)14 often suffer from the problems of photobleaching, interference from background tissue autofluorescence and/or low transfection efficiency for primary cells. Although quantum dots have been adopted and highly regarded as alternatives15,16, their application is hampered by their potential toxicity and facile degradation in vitro17 as well as in vivo18.
Fluorescent nanodiamonds (FNDs)19, a new member of the nanocarbon family20, have emerged recently as a novel nanotechnology imaging probe for biological applications21,22. The nanoscale diamond material is chemically robust, biologically inert, and non-toxic at both cellular23,24 and whole-organism levels25,26. A number of experiments have demonstrated that bare FND particles can be readily taken up by cells through clathrin-mediated endocytosis27, but with an exceptionally low exocytosis activity28,29. When excited by green-yellow light, the fluorophores (for example, negatively charged nitrogen–vacancy centres, NV−) built into the FND emit perfectly stable far-red emission (∼600–800 nm) with a fluorescence lifetime (τ) greater than 15 ns, even in cells30,31. This lifetime is substantially longer than that (τ ≈ 1–4 ns) of the endogenous and exogenous fluorophores commonly used in cell biology32, making it possible to separate FND emission from the strong autofluorescence background of host tissue using fluorescence lifetime imaging microscopy (FLIM) and various nanosecond time-gating techniques31,33. In this work, we show that primary cells such as LSCs can be spontaneously labelled with FNDs by endocytosis, and that the labelling does not eliminate cellular functions such as division, proliferation and differentiation. By combining FND–FLIM with fluorescence-activated cell sorting (FACS) and immunostaining analysis, we have been able to identify, unequivocally, transplanted cells in histological lung sections after intravenous (i.v.) injection of the FND-labelled LSCs into mice for more than a week, with single-cell resolution. The tissue-specific engraftment capacity of these cells is further elucidated with lung injury models.
Isolation and characterization of LSCs
Single-cell suspensions of pulmonary cells were prepared from the proteolytic digestion of neonatal mouse lung tissues, and removal of red blood cells by lysis6. Viable LSC candidates were isolated by FACS through staining with two specific cell surface markers (CD54 and CD157), propidium iodide and the CD45 antibody to exclude haematopoietic lineage cells. Flow cytometric analysis with CD31 and immunostaining with von Willebrand factor and isolectin showed that the sorted CD45−CD54+CD157+ cells did not express any of these endothelial markers, indicating that they were not contaminated with endothelial cells (Supplementary Fig. S1). Only a few cells of the subpopulation expressed α6-integrin, CD24 and EpCAM (Supplementary Fig. S2). The expression pattern of these epithelial markers suggests that the presently isolated CD45−CD54+CD157+ cells markedly differ from the LSC cohorts reported in the literature34,35 (see Supplementary section, ‘Results and Discussion’ for details).
To fully characterize the sorted CD45−CD54+CD157+ cells, immunofluorescence analysis was first performed at the time of isolation. Through a careful assessment for the specificity of the detection using isotype control antibodies (Supplementary Figs S3, S4), we found that these cells expressed the undifferentiated embryonic stem cell markers (Oct-4 and Nanog), the epithelial cell marker (cytokeratin-7), and the club cell marker (CCSP), but not the differentiated type II and type I pneumocyte markers (SP-C and Aqp-5, respectively) (Fig. 1a). There were no changes in the expression of these markers after cell culture on collagen I-coated plates using DMEM medium supplemented with 10% fetal bovine serum (FBS), 1% insulin–transferrin–selenium (ITS) and 10 ng ml−1 epithelial growth factor (EGF) for 10 days (Supplementary Fig. S5).
a, Immunofluorescence staining of the sorted CD45−CD54+CD157+ cells at the time of isolation against various types of undifferentiated and differentiated markers, including Oct-4 and Nanog (red), and cytokeratin-7, CCSP, SP-C and Aqp-5 (green). The cells expressed neither type II nor type I pneumocyte markers (SP-C and Aqp-5, respectively). Cell nuclei were stained in blue by DAPI. Scale bar, 10 µm. b, Examination for the differentiation of cultured CD45−CD54+CD157+ cells in vitro. The cells were induced to undergo differentiation by incubation in MCDB201 for 7 days, before being stained with antibodies against the type II pneumocyte marker, SP-C (green). Cells were then stained with antibodies against the type I pneumocyte marker, Aqp-5 (green), after incubation in MCDB201 for 14 days. Scale bar, 50 µm. Data are representative images from three independent experiments.
We next examined whether the cultured CD45−CD54+CD157+ cells had the capacity for cell differentiation. Cells were incubated in MCDB201 medium supplemented with 1% FBS, 1% ITS and 10 ng ml−1 EGF for ∼1–2 weeks. After 7 days of incubation, the cells became flattened and larger, and SP-C expression was detected in the cytoplasm close to the perinuclear region, which is indicative of cell differentiation into type II pneumocytes (Fig. 1b). Extension of the incubation to 14 days led to further flattening and enlargement of the cells (approximately fivefold greater than that of the original undifferentiated cells). These morphological changes were accompanied with a decrease in SP-C expression and an increase in Aqp-5 expression, an indication that the prospectively isolated CD45−CD54+CD157+ cells have the potential to differentiate into type II and then type I pneumocytes in a sequential manner.
Labelling of LSCs with FNDs
FNDs with dimensions of ∼100 nm were produced by ion irradiation and thermal annealing of type Ib diamond powders21,30. To carry out FND labelling, the cultured CD45−CD54+CD157+ cells (identified hereafter as LSCs) were incubated with 100 nm FNDs in DMEM at 37 °C with 5% CO2 for 4 h, after which the cells were washed thoroughly with phosphate-buffered saline (PBS) to remove free FNDs, and then collected by trypsin treatment. Flow cytometric analysis showed that the amount of 100 nm FNDs taken up by the LSCs reached a plateau at a concentration of 100 µg ml−1 (Supplementary Fig. S6). This behaviour closely resembles that of many other cell types including HeLa cells, 3T3-L1 pre-adipocytes and 489-2.1 multipotent stromal cells27,29. An extraordinary feature of the FND labelling is that in addition to far-red fluorescence, data collected in the side scatter (SSC) channel also provide useful information on FND uptake (Fig. 2a)29. This is attributable to the fact that diamond has the highest refractive index of all transparent minerals36, and diamond nanocrystallites scatter light strongly in the visible region and thus produce strong SSC signals. By properly gating the bivariate plot (SSC versus Far-Red) in quadrants, two distinct separate populations of FND-labelled and unlabelled cells could be detected in these two channels (Fig. 2a). The double-positive cell population, denoted SSC+Far-Red+, was subsequently identified as FND-labelled cells without additional staining.
a,b, Flow cytometric analysis of FND-labelled LSCs (red) and control LSCs without FND labelling (grey), showing two distinct populations in the side scatter (SSC) and far-red fluorescence channels (a), and that the FND-labelled LSCs cultured in DMEM could be continuously monitored for 15 days post-labelling (b). D0, D2, D6 and D15 in b denote days 0, 2, 6 and 15 after FND labelling, respectively. c,d, Representative wide-field fluorescence images of differentiated type II pneumocytes derived from the control LSCs (c) and FND-labelled LSCs (d) after induction in MCDB201 medium for 7 days, followed by immunostaining with SP-C (DAPI in blue, SP-C in green and FND in red). The FND image was acquired by excitation at 515–560 nm and collection of emission at >590 nm. No FNDs were found in cell nuclei. Scale bars, 10 µm. Experiments were repeated in triplicate.
Primary cells like LSCs divide slowly (∼2 days for one division). Moreover, they are sensitive and fragile, and properties such as growth rate and differentiation capacity are likely to be affected by the nanoparticle-based labelling. To address this issue, we tracked the proliferation of the FND-labelled LSCs continuously over two weeks by flow cytometry (Fig. 2b). Immediately after FND labelling, the mean fluorescence intensity of the LSCs was ∼45-fold greater than that of the unlabelled control cells. A successive decrease in fluorescence intensity by half occurred approximately every 48 h due to cell division. LSCs labelled with FNDs at 100 µg ml−1 could be identified for more than a week (approximately four divisions), after which the cells became confluent and stopped proliferating. The identification of LSCs in the cell culture up to day 15 revealed that the extent of FND exocytosis was low29. Further analysis by fluorescence microscopy showed that both untreated and FND-labelled LSCs were able to undergo morphological alterations and express SP-C on day 7 after induction (Fig. 2c,d). The expression of SP-C in the cytoplasm of the FND-labelled cells implies that the endocytic FNDs do not eliminate the apparent biological functions of the LSCs.
Tracking of FND-labelled LSCs in vivo
The performance of this nanodiamond-based optical imaging platform for in vivo stem cell tracking was first tested with healthy normal mice. Approximately 5 × 105 FND-labelled LSCs were injected into the tail veins of adult mice (four weeks old). Mice injected with saline served as controls. Organs and tissues including lungs, kidneys, liver and spleen were collected for examination on days 1, 4 and 7 after injection. Flow cytometric analysis confirmed that the injected LSCs preferentially resided in the lungs, and not in other organs (Supplementary Fig. S7). On day 1, ∼1.64% of the total population of viable pulmonary cells appeared as FND-labelled LSCs (Fig. 3a). This fraction, however, markedly decreased to 0.22% and 0.12% on days 4 and 7, respectively. In this analysis, the gating thresholds in the bivariate plots were carefully chosen by referring to the in vitro result (Fig. 2a) as well as the profiles of the saline controls (Supplementary Fig. S8) to ensure good reliability. With a false positive rate of less than 0.05%, as determined from the controls, the observed approximately tenfold decline in the SSC+Far-Red+ subpopulation was a reflection of the fact that most of the transplanted cells were not functionally engrafted. It is most likely that they were only initially trapped in the lung microvasculature and were eventually lost during the first week following transplantation.
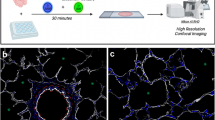
a, Flow cytometric analysis of total lung cells collected from uninjured mice receiving an i.v. injection of FND-labelled LSCs for 1, 4 and 7 days (n = 3 per group). b, Representative FLIM, TGF and bright-field H&E staining images of the same lung tissue sections from mice in a. The merged H&E and TGF images show that the FND-labelled cells (denoted by black arrows) are primarily located in the subepithelium of bronchiolar airways. Scale bar, 50 µm. c, Co-localization examination of FND-labelled LSCs and macrophages in a typical lung tissue section immunostained with macrophage-specific antigen F4/80 and haematoxylin counterstain. The enlarged view in the last panel shows that the transplanted FND-labelled cells (red, denoted by red arrows) and alveolar macrophages (brown, denoted by black arrows) are located at different positions. Scale bar, 10 µm. Experiments were repeated in triplicate.
To exclude the possibility that the sorted SSC+Far-Red+ cells were false positives, lung tissue sections were stained with haematoxylin and eosin (H&E) for morphological analysis, and then fluorescently imaged. However, when searching for FND-labelled LSCs in the tissue sections using confocal fluorescence microscopy, the images acquired using a continuous-wave 561 nm laser as the light source were overwhelmed by tissue autofluorescence and by the fluorescence derived from photoexcitation of the stain (Fig. 3b,c). With the aid of FLIM, the background noises and FND fluorescence signals could be readily distinguished. Gating the fluorescence signal at τ = 9–18 ns clearly revealed the location of FND-labelled LSCs with an enhancement in the signal-to-noise ratio of more than an order of magnitude (Fig. 3b). The identity of the FNDs was also confirmed by prolonged excitation, which did not result in any significant decrease in fluorescence intensity, consistent with the unique characteristic of the NV− fluorophores.
We further examined whether our observation was a consequence of FND engulfment by resident macrophages. To address this issue, lung tissue sections were stained with the macrophage-specific antibody, F4/80, followed by haematoxylin counterstaining and fluorescence imaging. Overlapping of the bright-field and time-gated fluorescence images (Fig. 3c) showed no sign of FND co-localization with the F4/80-stained macrophages, suggesting that the observed FND-labelled LSCs were not phagocytosed after i.v. injection. Such identification could not have been made using organic dyes such as carboxyfluorescein succinimidyl ester (CFSE)37, because of the similarity in lifetime between CFSE and the background fluorescence (Supplementary Fig. S9).
Engraftment of FND-labelled LSCs in lung injury models
It is known that the regenerative capacity of LSCs is determined not only by their intrinsic developmental potential, but also by their interaction with other cell elements in their niches38. This capacity could be substantially activated after tissue injury2. To illustrate this effect, we tracked LSCs in vivo using mice pretreated with naphthalene, which selectively ablated club cells in the epithelium of terminal and respiratory bronchioles39. Club cells (or Clara cells) are secretory cells that play a protective role in the bronchial tissue against damage. In this experiment, 5 × 105 FND-labelled LSCs were injected into the mice after lung injury for 2 days. Because LSCs express CCSP (Fig. 1a), the extent of the injury and the repair of the bronchiolar epithelium could be examined by immunostaining against CCSP (club cell secretory protein). On day 1, the bronchiolar epithelium in the lung-injured mice was sparsely surrounded by CCSP+ cells in both the control and treatment groups (Fig. 4a), showing low degrees of lung repair. Although some progress in club cell regeneration occurred in the control on day 7, the bronchiolar epithelium of the mice injected with FND–LSCs displayed a significantly greater repopulation of CCSP+ cells, that is, a greater regenerative capacity or a more rapid restoration of the lung epithelium (Fig. 4a).
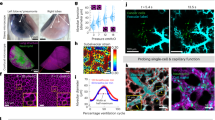
a,b, Immunohistochemical analysis of lung tissue sections (a) and flow cytometric analysis of total lung cells (b) collected from naphthalene-injured mice receiving an i.v. injection of saline (control) or FND-labelled LSCs for 1 and 7 days (n = 3 per group). The tissue sections in a were stained with CCSP for club cells (brown). c, Representative FLIM, TGF and bright-field H&E staining images of the same lung tissue sections, showing the location of FND-labelled LSCs (denoted by white and black arrows) in terminal bronchioles of the lungs. d, FLIM and H&E/TGF images of the lung tissue section of a naphthalene-injured mouse on day 7, showing engraftment of the transplanted FND-labelled LSCs (denoted by white and black arrows) to terminal bronchioles in cluster form. Scale bars, 50 µm. Experiments were repeated in triplicate.
The almost complete restoration of the CCSP+ cells strongly suggests that both endogenous LSCs and the transplanted FND-labelled LSCs were involved in lung repair and homeostasis. The suggestion was corroborated by flow cytometric analysis, where ∼0.91% and 0.80% of the viable pulmonary cells were identified as SSC+Far-Red+ on days 1 and 7, respectively (Fig. 4b). In comparison, the percentages of transplanted non-LSCs (such as mouse embryonic fibroblasts, MEFs) in the recipient lungs of the injured mice were significantly lower (0.33% and 0.17% on days 1 and 7, respectively) and should be attributed to non-specific entrapment (Supplementary Fig. S10). Further analysis by compound imaging with H&E staining and time-gated fluorescence (τ = 9–18 ns) revealed that the FND-labelled LSCs were preferentially localized in the terminal bronchioles of the lung-injured mice (Fig. 4c), in contrast to the localization of the cells in the subepithelium of bronchiolar airways in uninjured mice (Fig. 3b).
In the lung-injured mice, although most of the transplanted FND-labelled LSCs were monodispersed or in singlet form (Fig. 4c), they also exhibited different degrees of clustering in the terminal bronchioles (Fig. 4d). It is therefore speculated that the pattern of the distribution of these FND-labelled cells may reflect different degrees of injury in the lung tissues. For instance, the clustered cells may represent regions that have sustained more injury from the naphthalene. A close examination for the co-localization of the FND-labelled cells with the CCSP (Fig. 5a) and pan-cytokeratin (Fig. 5b) epithelial markers by high-power fluorescence imaging with single-cell resolution confirmed that the transplanted LSCs were not entrapped in the microvascular network of the lung, but rather had been functionally engrafted and integrated in the bronchiolar epithelium.
a,b, Club cell markers (CCSP, a) and epithelial markers (pan-cytokeratin, b) examined by FLIM and immunostaining of lung tissue sections prepared from naphthalene-injured mice on day 7 after i.v. injection of FND-labelled LSCs. The enlarged, merged immunostaining and TGF images in the red dashed boxes show that the FND-labelled LSCs (red) co-localize with CCSP+ (brown) and pan-cytokeratin+ (brown) cells and reside at the bronchiolar epithelial region of the lung. Scale bars, 10 µm. c, Histomorphometric distribution measured by visually counting the numbers of FND-labelled LSCs nested in terminal bronchioles (black) or alveoli (white) of the lungs of uninjured and injured mice on day 7 after i.v. injection. Results are averages of more than 30 visual fields per section, with error bars representing standard deviations of the measurements (n = 6 per group).
Our results have shown that the lung epithelia of the injured mice were restored more rapidly after transplantation of the FND-labelled LSCs than with saline control (Fig. 4a). To provide a semi-quantitative estimate40, we calculated the percentage (Ph) of the transplanted LSCs engrafted to the lung based on the total number (Nv) of viable (PI−) cells isolated from the mouse lung tissue, the percentage (Ps) of the FND-labelled cells identified in FACS analysis, and the number (Nt) of the cells actually transplanted, as Ph = NvPs/Nt. With Nv ≈ 7 × 106, Ps = 1.64% and Nt ≈ 5 × 105, the Ph for normal mice was estimated to be ∼23% on day 1. This percentage, however, markedly declined to 1.7% on day 7 (Fig. 3a). In contrast, the Ph for the lung injury model exhibited a much smaller decrease, with Ph ≈ 13% on day 1 and Ph ≈ 11% on day 7 (Fig. 4b). The distinct contrast between these two results provides compelling evidence that the lodgement of the transplanted FND-labelled cells in the injury models represents a ‘pro-active’ tissue-specific engraftment, instead of non-specific (or passive) entrapment.
A merit of the FND labelling technique is that it allows quantitative assessment of the distribution of transplanted LSCs in tissue due to the excellent chemical stability and photostability of the nanomaterial. We conducted this analysis by acquiring images of H&E staining using a bright-field section scanner. From these images, the cells showing FND labelling were counted visually in randomly selected regions. To reduce potential biases in the quantitative assessment, measurements were performed for more than 30 visual fields per section for six randomly selected sections of each sample, by independent workers. The results show that the percentages of FND-labelled LSCs nested in the terminal bronchioles and alveoli of the lung-injured mice are 59 ± 5% and 41 ± 5%, respectively, compared with 24 ± 3% and 76 ± 3% for the uninjured mice (Fig. 5c). The marked difference in the histomorphometric distributions of the FND-labelled LSC population between these two animal models serves as additional evidence that the transplanted LSCs preferentially engraft to the terminal bronchioles of the mice after lung injury. Although the mechanisms by which the injected LSCs reach lung tissues and further engraft to the terminal bronchioles are still not yet fully understood38, our findings support the contention that specific microenvironments (or niches) in lungs play important roles in the regulation of tissue-specific engraftment, structural support and the signals for self-renewal and differentiation of the stem cells41,42.
Conclusions
We have developed a novel nanodiamond-based platform that enables long-term imaging and tracking of transplanted stem/progenitor cells in vivo. The platform consists of FND labelling, FLIM and FACS technologies, with many unique features including simple labelling, high throughput and unequivocal detection of fluorescence signals that are not confounded by tissue autofluorescence and/or fluorescence derived from exogenous stains. Moreover, the FND labelling does not eliminate the cells’ in vitro differentiation and in vivo migration. Using the combined techniques, we have been able to follow the fate of FND-labelled LSCs in vivo after transplantation, precisely locate their position in tissue with single-cell resolution, and quantify their engraftment capacity over a week for the first time. The platform is particularly suitable for the study of rare stem cells that are difficult to transfect to express fluorescent proteins or non-fluorescent compounds. The method is general and also has broad applicability to other stem cell systems (such as haematopoietic stem/progenitor cells43,44).
Methods
Cell isolation and immunofluorescence staining
Viable LSCs were isolated from neonatal CD-1 (ICR) mice by proteolytic digestion of lung tissues and lysis of red blood cells, followed by sorting with FACS after staining with propidium iodide, CD54, CD157 and CD45 antibodies. Cells were then cultured through several passages and seeded at a density of 2 × 105 cells ml−1 in a collagen I-coated plate using DMEM supplemented with 10% FBS, 1% ITS and 10 ng ml−1 EGF. To perform immunofluorescence staining, cells in primary culture were first fixed in 4% paraformaldehyde/PBS at room temperature, permeabilized, and blocked with 0.5% Triton X-100 in 3% bovine serum albumin (BSA)/PBS. Cells were then incubated at 4 °C with the primary antibodies against antigens including SP-C, Aqp-5, cytokeratin-7 (all from Millipore), CCSP and Oct-4 (both from Santa Cruz). After overnight incubation, the cells were washed and incubated with respective FITC- or Cy3-labelled secondary antibodies (Jackson ImmunoResearch), and then counterstained with 4′,6-diamidino-2-phenylindole (DAPI). Photomicrographs of the cells were immediately taken after staining with a Zeiss fluorescence microscope.
FND production and labelling
FNDs were produced by radiation damage of type Ib diamond powders (Micron+ MDA M0.10, Element Six) using a 40 keV He+ ion beam, followed by thermal annealing at 800 °C, air oxidation at 450 °C and purification in concentrated H2SO4–HNO3 (3:1, vol/vol) solution at 100 °C (ref. 30). LSCs after cell attachment were labelled by FNDs through endocytosis at 37 °C with 5% CO2 for 4 h (ref. 29). The FND-labelled LSCs were then thoroughly washed by PBS to remove free FNDs and then analysed by using a FACSAria flow cytometer (BD Bioscience) equipped with a 594 nm laser and a 670LP emission filter in the far-red channel. To conduct differentiation studies, attached FND-labelled LSCs were incubated in MCDB201 medium supplemented with 1% FBS, 1% ITS and 10 ng ml−1 EGF. Cells were then fixed, permeabilized, and stained with primary antibodies against SP-C.
Confocal fluorescence microscopy and FLIM
Confocal imaging was carried out using a SP5 inverted microscope (Leica) equipped with three solid-state lasers operating separately at 561, 488 and 405 nm for the excitation of FND, SP-C and DAPI, respectively. Fluorescence was collected through an oil-immersion objective (×100, NA 1.4) and detected with either a photomultiplier tube (PMT) for SP-C and DAPI or an avalanche photodiode (APD) for FND. To conduct FLIM, an external frequency-doubled picosecond Nd:YAG laser (IC-532-30, High Q Laser), operating at 532 nm with a pulse width of 7 ps and a repetition rate of 50 MHz, was coupled through a single-mode optical fibre into the Leica microscope featuring a FLIM system (Supplementary Fig. S11). FND fluorescence was collected using a ×63 oil-immersion objective and detected with an APD at a wavelength of 650–850 nm through a bandpass filter (OS019606-HQ750/210m, Chroma). A time-correlated single-photon counting system (Pico-Harp 300, Pico Quant) was used to measure the fluorescence lifetimes, from which time-gated images were obtained with the SymPhoTime software.
In vivo tracking
Mouse LSCs were labelled with bare FNDs for 4 h at 100 µg ml−1. After washing away excess FNDs, 5 × 105 cells in 100 µl PBS were i.v. injected into adult mice (four weeks old) through tail veins. Mice were maintained until being killed on days 1, 4 and 7 (n = 3 per group), after which organs were collected for analysis with FACS and FLIM. All assays were repeated for at least three independent experiments. For fluorescence imaging, tissues were first fixed in 10% formalin overnight and then embedded in paraffin and sectioned. Sections (5 µm) were deparaffinized in xylene, rehydrated in a graded ethanol series, and incubated in blocking buffer. Sections were incubated overnight with antibodies against antigens including F4/80 (eBioscience), CCSP and pan-cytokeratin (both from Santa Cruz) and then analysed immunohistochemically with a peroxidase detection kit (Vector Laboratories) using diaminobenzene as the substrate according to the manufacturer's instructions. All sections were counterstained with Mayer's haematoxylin. Images of lung tissues after H&E staining or immunostaining were acquired using a bright-field scanner (Aperio Digital Pathology System) equipped with a ×40 objective. In separate experiments with lung injury models (n = 3 per group), naphthalene dissolved in Mazola corn oil was injected intraperitoneally at 275 mg kg−1 into sex- and background-matched adult (four weeks old) CD-1 (ICR) mice. FND-labelled LSCs were then administered 52 h after the naphthalene treatment and subsequently analysed following the procedures described above. All assays were repeated in triplicate.
References
Morrisey, E. E. & Hogan, B. L. Preparing for the first breath: genetic and cellular mechanisms in lung development. Dev. Cell 18, 8–23 (2010).
Giangreco, A. et al. Stem cells are dispensable for lung homeostasis but restore airways after injury. Proc. Natl Acad. Sci. USA 106, 9286–9291 (2009).
Giangreco, A., Reynolds, S. D. & Stripp, B. R. Terminal bronchioles harbor a unique airway stem cell population that localizes to the bronchoalveolar duct junction. Am. J. Pathol. 161, 173–182 (2002).
Kim, C. F. et al. Identification of bronchioalveolar stem cells in normal lung and lung cancer. Cell 121, 823–835 (2005).
Kim, C. F. Paving the road for lung stem cell biology: bronchioalveolar stem cells and other putative distal lung stem cells. Am. J. Physiol. Lung Cell Mol. Physiol. 293, L1092–L1098 (2007).
Ling, T. Y. et al. Identification of pulmonary Oct-4+ stem/progenitor cells and demonstration of their susceptibility to SARS coronavirus (SARS-CoV) infection in vitro. Proc. Natl Acad. Sci. USA 103, 9530–9535 (2006).
Chen, Y. X. et al. A novel subset of putative stem/progenitor CD34+Oct-4+ cells is the major target for SARS coronavirus in human lung. J. Exp. Med. 204, 2529–2536 (2007).
Lau, A. N., Goodwin, M., Kim, C. F. & Weiss, D. J. Stem cells and regenerative medicine in lung biology and diseases. Mol. Ther. 20, 1116–1130 (2012).
McQualter, J. L. & Bertoncello, I. Concise review: deconstructing the lung to reveal its regenerative potential. Stem Cells 30, 811–816 (2012).
Kircher, M. F., Gambhir, S. S. & Grimm, J. Noninvasive cell-tracking methods. Nature Rev. Clin. Oncol. 8, 677–688 (2011).
Weir, C. et al. Mesenchymal stem cells: isolation, characterisation and in vivo fluorescent dye tracking. Heart Lung Circ. 17, 395–403 (2008).
Chalfie, M., Tu, Y., Euskirchen, G., Ward, W. W. & Prasher, D. C. Green fluorescent protein as a marker for gene-expression. Science 263, 802–805 (1994).
Kajstura, J. et al. Evidence for human lung stem cells. N. Engl. J. Med. 364, 1795–1806 (2011).
Wang, H. et al. Trafficking mesenchymal stem cell engraftment and differentiation in tumor-bearing mice by bioluminescence imaging. Stem Cells 27, 1548–1558 (2009).
Ferreira, L., Karp, J. M., Nobre, L. & Langer, R. New opportunities: the use of nanotechnologies to manipulate and track stem cells. Cell Stem Cell 3, 136–146 (2008).
Solanki, A., Kim, J. D. & Lee, K. B. Nanotechnology for regenerative medicine: nanomaterials for stem cell imaging. Nanomedicine (Lond.) 3, 567–578 (2008).
Pi, Q. M., Zhang, W. J., Zhou, G. D., Liu, W. & Cao, Y. Degradation or excretion of quantum dots in mouse embryonic stem cells. BMC Biotechnol. 10, 36 (2010).
Rosen, A. B. et al. Finding fluorescent needles in the cardiac haystack: tracking human mesenchymal stem cells labeled with quantum dots for quantitative in vivo three-dimensional fluorescence analysis. Stem Cells 25, 2128–2138 (2007).
Yu, S-J., Kang, M-W., Chang, H-C., Chen, K-M. & Yu, Y-C. Bright fluorescent nanodiamonds: no photobleaching and low cytotoxicity. J. Am. Chem. Soc. 127, 17604–17605 (2005).
Mochalin, V. N., Shenderova, O., Ho, D. & Gogotsi, Y. The properties and applications of nanodiamonds. Nature Nanotech. 7, 11–23 (2012).
Chang, Y-R. et al. Mass production and dynamic imaging of fluorescent nanodiamonds. Nature Nanotech. 3, 284–288 (2008).
McGuinness, L. P. et al. Quantum measurement and orientation tracking of fluorescent nanodiamonds inside living cells. Nature Nanotech. 6, 358–363 (2011).
Huang, H., Pierstorff, E., Osawa, E. & Ho, D. Active nanodiamond hydrogels for chemotherapeutic delivery. Nano Lett. 7, 3305–3314 (2007).
Schrand, A. M. et al. in Safety of Nanoparticles (ed. Webster, T. J.) Ch. 8, 159–187 (Springer, 2009).
Mohan, N., Chen, C-S., Hsieh, H-H., Wu, Y-C. & Chang, H-C. In vivo imaging and toxicity assessments of fluorescent nanodiamonds in Caenorhabditis elegans. Nano Lett. 10, 3692–3699 (2010).
Vaijayanthimala, V. et al. The long-term stability and biocompatibility of fluorescent nanodiamond as an in vivo contrast agent. Biomaterials 33, 7794–7802 (2012).
Vaijayanthimala, V., Tzeng, Y-K., Chang, H-C. & Li, C-L. The biocompatibility of fluorescent nanodiamonds and their mechanism of cellular uptake. Nanotechnology 20, 425103 (2009).
Liu, K-K., Wang, C-C., Cheng, C-L. & Chao, J-I. Endocytic carboxylated nanodiamond for the labeling and tracking of cell division and differentiation in cancer and stem cells. Biomaterials 30, 4249–4259 (2009).
Fang, C-Y. et al. The exocytosis of fluorescent nanodiamond and its use as a long-term cell tracker. Small 7, 3363–3370 (2011).
Fu, C-C. et al. Characterization and application of single fluorescent nanodiamonds as cellular biomarkers. Proc. Natl Acad. Sci. USA 104, 727–732 (2007).
Faklaris, O. et al. Detection of single photoluminescent diamond nanoparticles in cells and study of the internalization pathway. Small 4, 2236–2239 (2008).
Billinton, N. & Knight, A. W. Seeing the wood through the trees: a review of techniques for distinguishing green fluorescent protein from endogenous autofluorescence. Anal. Biochem. 291, 175–197 (2001).
Chang, C. W., Sud, D. & Mycek, M. A. Fluorescence lifetime imaging microscopy. Methods Cell Biol. 81, 495–524 (2007).
McQualter, J. L., Yuen, K., Williams, B. & Bertoncello, I. Evidence of an epithelial stem/progenitor cell hierarchy in the adult mouse lung. Proc. Natl Acad. Sci. USA 107, 1414–1419 (2010).
Chen, H. et al. Airway epithelial progenitors are region specific and show differential responses to bleomycin-induced lung injury. Stem Cells 30, 1948–1960 (2012).
Edwards, D. F. & Philipp, H. R. in Handbook of Optical Constants of Solids (ed. Polik, E. D.) 665–673 (Academic, 1985).
Lyons, A. B. Analysing cell division in vivo and in vitro using flow cytometric measurement of CFSE dye dilution. J. Immunol. Methods 243, 147–154 (2000).
Chavakis, E., Urbich, C. & Dimmeler, S. Homing and engraftment of progenitor cells: a prerequisite for cell therapy. J. Mol. Cell. Cardiol. 45, 514–522 (2008).
Stripp, B. R., Maxson, K., Mera, R. & Singh, G. Plasticity of airway cell proliferation and gene expression after acute naphthalene injury. Am. J. Physiol. Lung Cell Mol. Physiol. 269, L791–L799 (1995).
Szilvassy, S. I., Meyerrose, T. E., Ragland, P. L. & Grimes, B. Differential homing and engraftment properties of hematopoietic progenitor cells from murine bone marrow, mobilized peripheral blood, and fetal liver. Blood 98, 2108–2115 (2001).
Chistiakov, D. A. Endogenous and exogenous stem cells: a role in lung repair and use in airway tissue engineering and transplantation. J. Biomed. Sci. 17, 92 (2010).
Andersson-Sjoland, A., Nihlberg, K., Eriksson, L., Bjermer, L. & Westergren-Thorsson, G. Fibrocytes and the tissue niche in lung repair. Respir. Res. 12, 76 (2011).
Lo Celso, C. et al. Live-animal tracking of individual haematopoietic stem/progenitor cells in their niche. Nature 457, 92–96 (2009).
Xie, Y. et al. Detection of functional haematopoietic stem cell niche using real-time imaging. Nature 457, 97–101 (2009).
Acknowledgements
This work was supported by Academia Sinica and the National Science Council, Taiwan (grants nos. 100-2119M-001-028 and 100-2321-B-001-036). The authors thank the Division of Medical Biology, Genomics Research Center, for providing facilities and support for cell imaging and flow cytometric analysis.
Author information
Authors and Affiliations
Contributions
T.J.W. and Y.K.T. conceived the study, conducted the experiments, interpreted the results, and wrote the manuscript. T.J.W. performed the tissue-culture work, cell sorting and tracking experiments, and data analysis. Y.K.T. and Y.K. assembled the FLIM systems and produced the image acquisition scripts. W.W.C. helped with the isolation of LSCs and carried out data analysis. C.A.C. prepared FNDs and performed the cell tracking experiments. C.H.C., H.C.C. and J.Y. supervised and planned the project, analysed the data, and wrote the manuscript. All authors designed the experiments and edited the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary information
Supplementary information (PDF 22544 kb)
Rights and permissions
About this article
Cite this article
Wu, TJ., Tzeng, YK., Chang, WW. et al. Tracking the engraftment and regenerative capabilities of transplanted lung stem cells using fluorescent nanodiamonds. Nature Nanotech 8, 682–689 (2013). https://doi.org/10.1038/nnano.2013.147
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nnano.2013.147
This article is cited by
-
Nanomaterial-based contrast agents
Nature Reviews Methods Primers (2023)
-
Mechanoporation enables rapid and efficient radiolabeling of stem cells for PET imaging
Scientific Reports (2022)
-
Loss of core-fucosylation of SPARC impairs collagen binding and contributes to COPD
Cellular and Molecular Life Sciences (2022)
-
Fluorescent nanodiamond for nanotheranostic applications
Microchimica Acta (2022)
-
Synthesis, Characterization, Properties, and Novel Applications of Fluorescent Nanodiamonds
Journal of Fluorescence (2022)