Abstract
Although multiple sclerosis is a common neurological disorder, the origin of the autoimmune response against myelin, which is the characteristic feature of the disease, remains unclear. To investigate whether oligodendrocyte death could cause this autoimmune response, we examined the oligodendrocyte ablation Plp1-CreERT;ROSA26-eGFP-DTA (DTA) mouse model. Approximately 30 weeks after recovering from oligodendrocyte loss and demyelination, DTA mice develop a fatal secondary disease characterized by extensive myelin and axonal loss. Strikingly, late-onset disease was associated with increased numbers of T lymphocytes in the CNS and myelin oligodendrocyte glycoprotein (MOG)-specific T cells in lymphoid organs. Transfer of T cells derived from DTA mice to naive recipients resulted in neurological defects that correlated with CNS white matter inflammation. Furthermore, immune tolerization against MOG ameliorated symptoms. Overall, these data indicate that oligodendrocyte death is sufficient to trigger an adaptive autoimmune response against myelin, suggesting that a similar process can occur in the pathogenesis of multiple sclerosis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
References
Nylander, A. & Hafler, D.A. Multiple sclerosis. J. Clin. Invest. 122, 1180–1188 (2012).
Nakahara, J., Aiso, S. & Suzuki, N. Autoimmune versus oligodendrogliopathy: the pathogenesis of multiple sclerosis. Arch. Immunol. Ther. Exp. (Warsz.) 58, 325–333 (2010).
McFarland, H.F. & Martin, R. Multiple sclerosis: a complicated picture of autoimmunity. Nat. Immunol. 8, 913–919 (2007).
Stys, P.K., Zamponi, G.W., van Minnen, J. & Geurts, J.J. Will the real multiple sclerosis please stand up? Nat. Rev. Neurosci. 13, 507–514 (2012).
Barnett, M.H. & Prineas, J.W. Relapsing and remitting multiple sclerosis: pathology of the newly forming lesion. Ann. Neurol. 55, 458–468 (2004).
Henderson, A.P., Barnett, M.H., Parratt, J.D. & Prineas, J.W. Multiple sclerosis: distribution of inflammatory cells in newly forming lesions. Ann. Neurol. 66, 739–753 (2009).
Rodriguez, M. & Scheithauer, B. Ultrastructure of multiple sclerosis. Ultrastruct. Pathol. 18, 3–13 (1994).
Traka, M. et al. A genetic mouse model of adult-onset, pervasive central nervous system demyelination with robust remyelination. Brain 133, 3017–3029 (2010).
Doerflinger, N.H., Macklin, W.B. & Popko, B. Inducible site-specific recombination in myelinating cells. Genesis 35, 63–72 (2003).
Feil, R. et al. Ligand-activated site-specific recombination in mice. Proc. Natl. Acad. Sci. USA 93, 10887–10890 (1996).
Bailey, S.L., Schreiner, B., McMahon, E.J. & Miller, S.D. CNS myeloid DCs presenting endogenous myelin peptides 'preferentially' polarize CD4+ TH-17 cells in relapsing EAE. Nat. Immunol. 8, 172–180 (2007).
Bettelli, E., Baeten, D., Jäger, A., Sobel, R.A. & Kuchroo, V.K. Myelin oligodendrocyte glycoprotein-specific T and B cells cooperate to induce a Devic-like disease in mice. J. Clin. Invest. 116, 2393–2402 (2006).
McMahon, E.J., Bailey, S.L., Castenada, C.V., Waldner, H. & Miller, S.D. Epitope spreading initiates in the CNS in two mouse models of multiple sclerosis. Nat. Med. 11, 335–339 (2005).
Mombaerts, P. et al. RAG-1-deficient mice have no mature B and T lymphocytes. Cell 68, 869–877 (1992).
Butovsky, O. et al. Microglia activated by IL-4 or IFN-gamma differentially induce neurogenesis and oligodendrogenesis from adult stem/progenitor cells. Mol. Cell. Neurosci. 31, 149–160 (2006).
Pusic, A.D., Pusic, K.M., Clayton, B.L. & Kraig, R.P. IFNγ-stimulated dendritic cell exosomes as a potential therapeutic for remyelination. J. Neuroimmunol. 266, 12–23 (2014).
Schwartz, M. & Raposo, C. Protective autoimmunity: a unifying model for the immune network involved in CNS repair. Neuroscientist 20, 343–358 (2014).
Yednock, T.A. et al. Prevention of experimental autoimmune encephalomyelitis by antibodies against α4β1 integrin. Nature 356, 63–66 (1992).
Polman, C.H. et al. A randomized, placebo-controlled trial of natalizumab for relapsing multiple sclerosis. N. Engl. J. Med. 354, 899–910 (2006).
Podojil, J.R. et al. B7-H4Ig inhibits mouse and human T-cell function and treats EAE via IL-10/Treg-dependent mechanisms. J. Autoimmun. 44, 71–81 (2013).
Hunter, Z. et al. A biodegradable nanoparticle platform for the induction of antigen-specific immune tolerance for treatment of autoimmune disease. ACS Nano 8, 2148–2160 (2014).
Bjartmar, C., Wujek, J.R. & Trapp, B.D. Axonal loss in the pathology of MS: consequences for understanding the progressive phase of the disease. J. Neurol. Sci. 206, 165–171 (2003).
Maña, P. et al. Demyelination caused by the copper chelator cuprizone halts T cell mediated autoimmune neuroinflammation. J. Neuroimmunol. 210, 13–21 (2009).
Manrique-Hoyos, N. et al. Late motor decline after accomplished remyelination: impact for progressive multiple sclerosis. Ann. Neurol. 71, 227–244 (2012).
Blakemore, W.F. Demyelination of the superior cerebellar peduncle in the mouse induced by cuprizone. J. Neurol. Sci. 20, 63–72 (1973).
Emerson, M.R., Biswas, S. & LeVine, S.M. Cuprizone and piperonyl butoxide, proposed inhibitors of T-cell function, attenuate experimental allergic encephalomyelitis in SJL mice. J. Neuroimmunol. 119, 205–213 (2001).
Locatelli, G. et al. Primary oligodendrocyte death does not elicit anti-CNS immunity. Nat. Neurosci. 15, 543–550 (2012).
Buch, T. et al. A Cre-inducible diphtheria toxin receptor mediates cell lineage ablation after toxin administration. Nat. Methods 2, 419–426 (2005).
Ghosh, A. et al. Targeted ablation of oligodendrocytes triggers axonal damage. PLoS One 6, e22735 (2011).
Pohl, H.B. et al. Genetically induced adult oligodendrocyte cell death is associated with poor myelin clearance, reduced remyelination, and axonal damage. J. Neurosci. 31, 1069–1080 (2011).
Oluich, L.J. et al. Targeted ablation of oligodendrocytes induces axonal pathology independent of overt demyelination. J. Neurosci. 32, 8317–8330 (2012).
Gritsch, S. et al. Oligodendrocyte ablation triggers central pain independently of innate or adaptive immune responses in mice. Nat. Commun. 5, 5472 (2014).
Rumah, K.R., Linden, J., Fischetti, V.A. & Vartanian, T. Isolation of Clostridium perfringens type B in an individual at first clinical presentation of multiple sclerosis provides clues for environmental triggers of the disease. PLoS One 8, e76359 (2013).
Linden, J.R. et al. Clostridium perfringens epsilon toxin causes selective death of mature oligodendrocytes and central nervous system demyelination. MBio 6, e02513 (2015).
Caprariello, A.V., Mangla, S., Miller, R.H. & Selkirk, S.M. Apoptosis of oligodendrocytes in the central nervous system results in rapid focal demyelination. Ann. Neurol. 72, 395–405 (2012).
Kassmann, C.M. et al. Axonal loss and neuroinflammation caused by peroxisome-deficient oligodendrocytes. Nat. Genet. 39, 969–976 (2007).
Ip, C.W. et al. Immune cells contribute to myelin degeneration and axonopathic changes in mice overexpressing proteolipid protein in oligodendrocytes. J. Neurosci. 26, 8206–8216 (2006).
Ohno, M., Komiyama, A., Martin, P.M. & Suzuki, K. MHC class II antigen expression and T-cell infiltration in the demyelinating CNS and PNS of the twitcher mouse. Brain Res. 625, 186–196 (1993).
Suzuki, K. Twenty five years of the “psychosine hypothesis”: a personal perspective of its history and present status. Neurochem. Res. 23, 251–259 (1998).
Suzuki, K. Globoid cell leukodystrophy (Krabbe's disease): update. J. Child Neurol. 18, 595–603 (2003).
Hafler, D.A. et al. Risk alleles for multiple sclerosis identified by a genomewide study. N. Engl. J. Med. 357, 851–862 (2007).
Sawcer, S. et al. Genetic risk and a primary role for cell-mediated immune mechanisms in multiple sclerosis. Nature 476, 214–219 (2011).
Ivanova, A. et al. In vivo genetic ablation by Cre-mediated expression of diphtheria toxin fragment A. Genesis 43, 129–135 (2005).
Srinivas, S. et al. Cre reporter strains produced by targeted insertion of EYFP and ECFP into the ROSA26 locus. BMC Dev. Biol. 1, 4 (2001).
Traka, M. et al. Nur7 is a nonsense mutation in the mouse aspartoacylase gene that causes spongy degeneration of the CNS. J. Neurosci. 28, 11537–11549 (2008).
Shen, S. et al. Age-dependent epigenetic control of differentiation inhibitors is critical for remyelination efficiency. Nat. Neurosci. 11, 1024–1034 (2008).
Acknowledgements
We thank E. Liu, A. Solanki, A.X. Tang and S. Labak for technical assistance, G. Wright for assistance with the morphometric analysis of the EM images using the ImageJ software and V. Bindokas from the University of Chicago Integrated Light Microscopy Core Facility for help with image acquisition and image processing. The work was supported by awards from the Myelin Repair Foundation and the National Multiple Sclerosis Society (RG 4952-A-5) to B.P. and S.D.M.
Author information
Authors and Affiliations
Contributions
M.T. and J.R.P. designed the studies, performed the experiments, analyzed and interpreted the data and wrote the manuscript. D.P.M. assisted with the induction and completion of the MOG35–55 specific tolerance experiments. B.P. and S.D.M. supervised the project, assisted with experimental design, data interpretation and manuscript preparation.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 T cell infiltration in the CNS of tamoxifen-treated DTA mice during the late-onset disease.
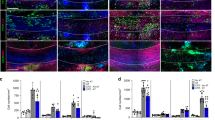
Staining for CD3 (green) revealed increased T cell infiltration in different areas of the CNS in tamoxifen-treated PLP/CreERT;ROSA26-eGFP-DTA (DTA) mice (lower panel) at 53 weeks post-injection (p.i.) compared with that in control (ROSA26-eGFP-DTA) mice (upper panel). Higher magnification of the CD3+ cells is shown in the inset (lower panel, corpus callosum). Images are representative of three mice/genotype. Scale bar: 100 μm. Sections were counterstained with DAPI (blue) to show cell nuclei.
Supplementary Figure 2 Tamoxifen-independent recombination in oligodendrocytes of the reporter mice.
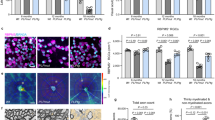
(a) Expression of the reporter gene protein YFP (green) was detected in a subpopulation of oligodendrocytes stained for CC-1 (red) in all CNS areas examined of the untreated PLP/CreERT;RosaEYFP (reporter w/o 4-HT; lower panel) mice at the age of 52 weeks. CC1/YFP stainings in corresponding areas of control littermate mice (RosaEYFP) are shown in the upper panel. The CC1/YFP double positive cells (yellow) are marked by arrows. Images are representative of three mice/genotype. Scale bar: 100 μm. (b) Counts of the CC1/YFP double positive cells labeled in different CNS areas of the untreated reporter mice showed that tamoxifen-independent recombination occurs in ~ 6%-14% of oligodendrocytes at 26 weeks and it tends to be increased in most areas (6%-20%) at 52 weeks (brain stem p =0.0084). Graph in b shows means (+ SEM), n=4 mice per group, two-tailed unpaired Student’s t test, **p <0.01.
Supplementary Figure 3 Tamoxifen-independent demyelination in untreated DTA mice.
(a) Electron microscopy analysis demonstrated normal myelin levels in the cervical cord and milder demyelination in the cerebellum, corpus callosum, optic nerve and brain stem areas of the untreated PLP/CreERT;ROSA26-eGFP-DTA (DTA w/o 4-HT) mice as compared to tamoxifen-treated PLP/CreERT;ROSA26-eGFP-DTA (DTA) mice, which showed more severe myelin loss in the same areas. Images are representative of three mice/genotype. Scale bars: 2 μm. (b) Morphometric analysis of the corpus callosum area showed that numbers of unmyelinated axons were significantly lower (~ 30%) in the 52-week old untreated DTA mice as compared to tamoxifen-treated DTA mice at 53 weeks post-injection suggesting milder myelin loss in the former animals. Control versus tamoxifen-treated DTA mice: p<0.0001, control vs. untreated DTA mice: p=0.0001, tamoxifen-treated DTA mice versus untreated DTA mice: p=0.0013. Graph in b shows means (+ SEM), n=3 for control and tamoxifen-treated DTA mice, n=4 for untreated DTA mice. ***p <0.001, **p <0.01, one-way ANOVA with Tukey’s post-hoc test. (c) Scatter plots of g-ratios versus axon diameters indicate significantly increased g-ratios (thinner myelin) in axons of the corpus callosum in both the tamoxifen-treated DTA (mean g ratio of 0.80 ± 0.004) and the untreated DTA mice (mean g ratio of 0.82 ± 0.005) as compared to controls (ROSA26-eGFP-DTA, mean g ratio of 0.77 ± 0.005). Control versus tamoxifen-treated DTA mice: p<000.1 and control versus untreated DTA mice: p<000.1, one-way Anova followed by Tukey’s post-hoc analysis test. Forty axons/mouse, n=3 mice per group.
Supplementary Figure 4 The untreated DTA mice do not develop a late-onset clinical phenotype.
(a-b) The untreated PLP/CreERT;ROSA26-eGFP-DTA (DTA w/o 4-HT) mice displayed normal coordination skills on the rotarod (a) and they did not show significant weight loss (b) as compared to control littermate (ROSA26-eGFP-DTA) mice during the time points that the tamoxifen-treated DTA mice were severely affected. Data are presented as the mean (± SEM), n= 5 mice/genotype for each data point shown in the graphs in a and b, p >0.05; two-way ANOVA with Bonferroni post-hoc analysis.
Supplementary Figure 5 Tamoxifen-independent demyelination in untreated DTA mice does not elicit an immune response against myelin.
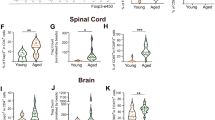
(a) Staining for the pan T cell marker CD3 showed similar, low numbers of T cells in different CNS areas of the 52-week old untreated PLP/CreERT;ROSA26-eGFP-DTA (DTA w/o 4-HT) mice and in corresponding CNS areas of their littermate controls (ROSA26-eGFP-DTA mice). Images are representative of three mice/genotype. Scale bar: 100 μm. Spleen, cervical lymph nodes, and CNS samples were collected from age matched control littermate mice and untreated DTA mice. (b) Total splenoctyes (1x106 cells per well) were cultured in the presence of medium alone, anti-CD3 (1μg/ml), OVA323-339, PLP139-151, PLP178-191, MBP84-104, MOG35-55, and whole recombinant rat MOG protein (10 μg/ml). The cultures were pulsed with tritiated thymidine (1 μCi) at 24 hours and cultures were harvested at 72 hours post culture to determine the level of cellular proliferation. Cells from (c) spleen, (d) cervical lymph nodes, and (e) CNS were stained for the presence of total infiltrating lymphocytes (CD45hi), microglia (CD45lo/CD11b+), total CD3+, total CD4+ T cells (CD3+/CD4+), Treg cells (CD3+/CD4+/CD25+/FoxP3+), effector CD4+ T cells (CD3+/CD4+/CD44hi/FoxP3-), total monocytes (Mθ; CD3-/CD11b+/CD11c-), and total dendritic cells (DC; CD3-/CD11b-/CD11c+). No significant difference in the number of the various immune cells populations were found within the spleen, cervical lymph nodes, or the CNS (n=3) via two-way ANOVA with Bonferroni post-hoc analysis for differences between control mice and tamoxifen-treated DTA mice. The data are presented as the means (+ SEM). Sections in a were counterstained with DAPI (blue) to visualize cell nuclei. Abbreviations: CPM, counts per minute.
Supplementary Figure 6 Adoptive transfer of MOG-specific T cells derived from tamoxifen-treated DTA mice and 2D2 TCR transgenic mice into naive Rag1−/− mice versus wild-type C57BL/6 mice.
Splenic cells from tamoxifen-treated PLP/CreERT;ROSA26-eGFP-DTA (DTA) mice at 40-52 weeks post-injection or age-matched control (ROSA26-eGFP-DTA) mice were cultured for 72 h at in the presence of MOG35–55 peptide (20 μg/ml) plus IL-12 (10 ng/ml) and IL-2 (100 U/ml). Cultured cells (10x106 blast cells) from tamoxifen-treated DTA mice were transferred into either naïve Rag1−/− recipient mice (n=7) (a) or naïve wildtype C57BL/6 recipient mice (n=7) (b). Naïve CD4+ T cells were isolated from 2D2 MOG35–55-specific TCR transgenic mice, and activated in the presence plate-bound anti-CD3 (1ug/ml) plus various Teff cell lineage promoting conditions as indicated. 2D2 T cells (3x106 cells per mouse) activated in the presence of Th1 cell- [IL-12 (10ng/ml), IL-2 (100 U/ml), and anti-IL-4 (1 μg/ml)] or Th17 cell- [TGF-β (10 ng/ml), IL-6 (50ng/ml), IL-23 (10 ng/ml), anti-IL-4 (1 μg/ml), and anti-IFN-γ (1 μg/ml)] promoting conditions were transferred into Rag1-/- mice versus wildtype C57BL/6 mice (n=5), and the recipient mice were followed for disease (c). 2D2 T cells (3x106 cells per mouse) activated in the presence of Th0- [IL-2 (100 U/ml)], Th1 cell- or Th17 cell-promoting conditions were transferred into Rag1-/- mice (n=5), and the recipient mice were followed for disease (d). One representative experiment of three is presented. The data is presented as the mean Clinical Score (± SEM).
Supplementary Figure 7 Adoptive transfer of MOG-specific T cells derived from tamoxifen-treated DTA mice causes mild demyelination in naive Rag1−/− mice.
Splenic cells from tamoxifen-treated (PLP/CreERT;ROSA26-eGFP-DTA) DTA mice at 40-52 weeks post-injection or age-matched control (ROSA26-eGFP-DTA) mice were cultured for 72 h at in the presence of MOG35–55 peptide (20 μg/ml). Cultured cells from tamoxifen-treated DTA mice (2x106 blast cells) were transferred into naïve Rag1−/− recipient mice (a) Forty-two days after transfer, Electron microscopy analysis revealed foci of myelin loss in the lower lumbar spinal cord and cerebellar white matter in Rag1−/− mice inoculated with T cells from tamoxifen-treated DTA mice (DTA recipient) as compared with those inoculated with cells from control mice (littermate recipient). Inflammatory cells were also frequently detected in the cerebellum (asterisk). More-extensive demyelination was seen in the brain stem gray matter. Images are representative of three mice/genotype. Scale bars: 2 μm. (b) Demyelination in the brain stem of Rag1−/− mice inoculated with cells from tamoxifen-treated DTA mice was shown by significantly reduced mean (+ SEM) numbers of myelinated axons (~30% fewer, p=0.0363). N=3 mice/group; *p <0.05 with two-tailed unpaired Student’s t test.
Supplementary Figure 8 MOG35–55-PLG-induced tolerance inhibits activated DTA mouse-derived MOG35–55-specific T cell entry into the CNS.
Representative flow plots for the data presented in Fig. 7c and e are presented. The data is presented as the (a) IFN-γ+, (b) IL-17+, and (c) Ki67+ singlet live CD45hi/CD4+ T cells within the CNS from control (ROSA26-eGFP-DTA) or tamoxifen-treated PLP/CreERT;ROSA26-eGFP-DTA (DTA)-derived cell recipient mice that received OVA323-339-PLG (Red line) versus MOG35-55-PLG treatment (Blue line). Similar analyses were completed for splenocyte samples assessing (d) IFN-γ+, (e) IL-17+, and (f) Ki67+ singlet live CD45hi/CD4+ T cells.
Supplementary Figure 9 MOG35–55 tolerance inhibits CD4+ T cell infiltration, proliferation and production of the proinflammatory cytokines in the CNS of the tamoxifen-treated DTA mice.
Representative flow plots of cells isolated from the CNS (a-g) and the spleens (h-m) of the tamoxifen-treated PLP/CreERT;ROSA26-eGFP-DTA (DTA) mice at 39 weeks post-injection after receiving a single treatment with the MOG35-55-PLG or the OVA323-339-PLG control peptide at 32 weeks post-injection. Lower numbers of the total infiltrating lymphocytes (CD45hi+ stained cells) were detected in the CNS of the MOG35-55-tolerized DTA mice, as compared to the OVA323-339-tolerized (control) DTA mice (n=6). The later mice also showed, lower numbers of the effector T cells (CD3+/CD4+ double positive cells) and proliferating interferon-γ-positive effector T cells (Ki67+/INF-γ+ stained cells) and no changes for the proliferating IL-17-positive effector T cells (Ki67+/IL-17+ stained cells). No differences were detected in the numbers of the different immune cell populations in the spleens between the two groups of mice.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–9 (PDF 2108 kb)
Rights and permissions
About this article
Cite this article
Traka, M., Podojil, J., McCarthy, D. et al. Oligodendrocyte death results in immune-mediated CNS demyelination. Nat Neurosci 19, 65–74 (2016). https://doi.org/10.1038/nn.4193
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nn.4193
This article is cited by
-
Infection and inflammation: radiological insights into patterns of pediatric immune-mediated CNS injury
Neuroradiology (2023)
-
CXCL13 expressed on inflamed cerebral blood vessels recruit IL-21 producing TFH cells to damage neurons following stroke
Journal of Neuroinflammation (2022)
-
The landscape of targets and lead molecules for remyelination
Nature Chemical Biology (2022)
-
Epidermal Growth Factor in the CNS: A Beguiling Journey from Integrated Cell Biology to Multiple Sclerosis. An Extensive Translational Overview
Cellular and Molecular Neurobiology (2022)
-
Targeted Oligodendrocyte Apoptosis in Optic Nerve Leads to Persistent Demyelination
Neurochemical Research (2020)