Abstract
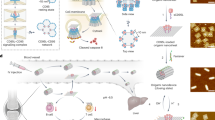
Host recognition and immune-mediated foreign body response to biomaterials can compromise the performance of implanted medical devices. To identify key cell and cytokine targets, here we perform in-depth systems analysis of innate and adaptive immune system responses to implanted biomaterials in rodents and non-human primates. While macrophages are indispensable to the fibrotic cascade, surprisingly neutrophils and complement are not. Macrophages, via CXCL13, lead to downstream B cell recruitment, which further potentiated fibrosis, as confirmed by B cell knockout and CXCL13 neutralization. Interestingly, colony stimulating factor-1 receptor (CSF1R) is significantly increased following implantation of multiple biomaterial classes: ceramic, polymer and hydrogel. Its inhibition, like macrophage depletion, leads to complete loss of fibrosis, but spares other macrophage functions such as wound healing, reactive oxygen species production and phagocytosis. Our results indicate that targeting CSF1R may allow for a more selective method of fibrosis inhibition, and improve biomaterial biocompatibility without the need for broad immunosuppression.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout






Similar content being viewed by others
Change history
19 May 2021
A Correction to this paper has been published: https://doi.org/10.1038/s41563-021-01023-1
References
Kurtz, S., Ong, K., Lau, E., Mowat, F. & Halpern, M. Projections of primary and revision hip and knee arthroplasty in the United States from 2005 to 2030. J. Bone Joint Surg. Am. Vol. 89, 780–785 (2007).
Med, I. Medical Devices and the Public’s Health: The FDA 510(k) Clearance Process at 35 Years 1–298 (National Academies, 2011).
Cobelli, N., Scharf, B., Crisi, G. M., Hardin, J. & Santambrogio, L. Mediators of the inflammatory response to joint replacement devices. Nat. Rev. Rheumatol. 7, 600–608 (2011).
Hubbell, J. A. & Langer, R. Translating materials design to the clinic. Nat. Mater. 12, 963–966 (2013).
Fattahi, P., Yang, G., Kim, G. & Abidian, M. R. A review of organic and inorganic biomaterials for neural interfaces. Adv. Mater. 26, 1846–1885 (2014).
Farra, R. et al. First-in-human testing of a wirelessly controlled drug delivery microchip. Sci. Transl. Med. 4, 122ra121 (2012).
Rosen, M. R., Robinson, R. B., Brink, P. R. & Cohen, I. S. The road to biological pacing. Nat. Rev. Cardiol. 8, 656–666 (2011).
Nichols, S. P., Koh, A., Storm, W. L., Shin, J. H. & Schoenfisch, M. H. Biocompatible materials for continuous glucose monitoring devices. Chem. Rev. 113, 2528–2549 (2013).
Perez-Cambrodi, R. J., Pinero, D. P., Ferrer-Blasco, T., Cervino, A. & Brautaset, R. The posterior chamber phakic refractive lens (PRL): a review. Eye 27, 14–21 (2013).
Kearney, C. J. & Mooney, D. J. Macroscale delivery systems for molecular and cellular payloads. Nat. Mater. 12, 1004–1017 (2013).
Anderson, J. M., Rodriguez, A. & Chang, D. T. Foreign body reaction to biomaterials. Semin. Immunol. 20, 86–100 (2008).
Wynn, T. A. & Ramalingam, T. R. Mechanisms of fibrosis: therapeutic translation for fibrotic disease. Nat. Med. 18, 1028–1040 (2012).
Kenneth Ward, W. A review of the foreign-body response to subcutaneously-implanted devices: the role of macrophages and cytokines in biofouling and fibrosis. J. Diabetes Sci. Technol. Online 2, 768–777 (2008).
Gordon, S. Alternative activation of macrophages. Nat. Rev. Immunol. 3, 23–35 (2003).
Grainger, D. W. All charged up about implanted biomaterials. Nat. Biotechnol. 31, 507–509 (2013).
Sussman, E. M., Halpin, M. C., Muster, J., Moon, R. T. & Ratner, B. D. Porous implants modulate healing and induce shifts in local macrophage polarization in the foreign body reaction. Ann. Biomed. Eng. 42, 1508–1516 (2014).
Kyriakides, T. R. et al. The CC chemokine ligand, CCL2/MCP1, participates in macrophage fusion and foreign body giant cell formation. Am. J. Pathol. 165, 2157–2166 (2004).
Rodriguez, A., Meyerson, H. & Anderson, J. M. Quantitative in vivo cytokine analysis at synthetic biomaterial implant sites. J. Biomed. Mater. Res. Part A 89, 152–159 (2009).
Lee, K. Y. & Mooney, D. J. Alginate: properties and biomedical applications. Progr. Polym. Sci. 37, 106–126 (2012).
de Vos, P., Faas, M. M., Strand, B. & Calafiore, R. Alginate-based microcapsules for immunoisolation of pancreatic islets. Biomaterials 27, 5603–5617 (2006).
Jacobs-Tulleneers-Thevissen, D. et al. Sustained function of alginate-encapsulated human islet cell implants in the peritoneal cavity of mice leading to a pilot study in a type 1 diabetic patient. Diabetologia 56, 1605–1614 (2013).
Tuch, B. E. et al. Safety and viability of microencapsulated human islets transplanted into diabetic humans. Diabetes Care 32, 1887–1889 (2009).
Weir, G. C. Islet encapsulation: advances and obstacles. Diabetologia 56, 1458–1461 (2013).
Dang, T. T. et al. Enhanced function of immuno-isolated islets in diabetes therapy by co-encapsulation with an anti-inflammatory drug. Biomaterials 34, 5792–5801 (2013).
Robitaille, R. et al. Inflammatory response to peritoneal implantation of alginate-poly-L-lysine microcapsules. Biomaterials 26, 4119–4127 (2005).
Vegas, A. J. et al. Combinatorial hydrogel library enables identification of materials that mitigate the foreign body response in primates. Nat. Biotechnol. 34, 345–352 (2016).
Veiseh, O. et al. Size- and shape-dependent foreign body immune response to materials implanted in rodents and non-human primates. Nat. Mater. 14, 643–651 (2015).
Harding, J. L. & Reynolds, M. M. Combating medical device fouling. Trends Biotechnol. 32, 140–146 (2014).
Langer, R. Perspectives and challenges in tissue engineering and regenerative medicine. Adv. Mater. 21, 3235–3236 (2009).
Rhen, T. & Cidlowski, J. A. Antiinflammatory action of glucocorticoids—new mechanisms for old drugs. N. Engl. J. Med. 353, 1711–1723 (2005).
Khan, W., Muntimadugu, E., Jaffe, M. & Domb, A. J. Focal Controlled Drug Delivery 33–59 (Springer, 2014).
Attur, M. G. et al. Differential anti-inflammatory effects of immunosuppressive drugs: cyclosporin, rapamycin and FK-506 on inducible nitric oxide synthase, nitric oxide, cyclooxygenase-2 and PGE 2 production. Inflamm. Res. 49, 20–26 (2000).
King, A., Sandler, S. & Andersson, A. The effect of host factors and capsule composition on the cellular overgrowth on implanted alginate capsules. J. Biomed. Mater. Res. 57, 374–383 (2001).
Manoury, B., Caulet-Maugendre, S., Guenon, I., Lagente, V. & Boichot, E. TIMP-1 is a key factor of fibrogenic response to bleomycin in mouse lung. Int. J. Immunopathol. Pharmacol. 19, 471–487 (2006).
Paredes-Juarez, G. A., de Haan, B. J., Faas, M. M. & de Vos, P. The role of pathogen-associated molecular patterns in inflammatory responses against alginate based microcapsules. J. Control Release 172, 983–992 (2013).
Jhunjhunwala, S. et al. Neutrophil responses to sterile implant materials. PLoS ONE 10, e0137550 (2015).
Shi, C. & Pamer, E. G. Monocyte recruitment during infection and inflammation. Nat. Rev. Immunol. 11, 762–774 (2011).
Wood, K. J., Bushell, A. & Hester, J. Regulatory immune cells in transplantation. Nat. Rev. Immunol. 12, 417–430 (2012).
Bratlie, K. M. et al. Rapid biocompatibility analysis of materials via in vivo fluorescence imaging of mouse models. PLoS ONE 5, e10032 (2010).
Ito, M. et al. NOD/ID/gamma(c)(null) mouse: an excellent recipient mouse model for engraftment of human cells. Blood 100, 3175–3182 (2002).
Diel, I. J., Bergner, R. & Grotz, K. A. Adverse effects of bisphosphonates: current issues. J. Support. Oncol. 5, 475–482 (2007).
Pyonteck, S. M. et al. CSF-1R inhibition alters macrophage polarization and blocks glioma progression. Nat. Med. 19, 1264–1272 (2013).
Conway, J. G. et al. Inhibition of colony-stimulating-factor-1 signaling in vivo with the orally bioavailable cFMS kinase inhibitor GW2580. Proc. Natl Acad. Sci. USA 102, 16078–16083 (2005).
Laskin, D. L., Sunil, V. R., Gardner, C. R. & Laskin, J. D. Macrophages and tissue injury: agents of defense or destruction? Ann. Rev. Pharmacol. Toxicol. 51, 267–288 (2011).
Arnold, L. et al. CX3CR1 deficiency promotes muscle repair and regeneration by enhancing macrophage ApoE production. Nat. Commun. 6, 8972 (2015).
Pesce, J. et al. The IL-21 receptor augments Th2 effector function and alternative macrophage activation. J. Clin. Investig. 116, 2044–2055 (2006).
Carlsen, H. S., Baekkevold, E. S., Morton, H. C., Haraldsen, G. & Brandtzaeg, P. Monocyte-like and mature macrophages produce CXCL13 (B cell-attracting chemokine 1) in inflammatory lesions with lymphoid neogenesis. Blood 104, 3021–3027 (2004).
Affara, N. I. et al. B cells regulate macrophage phenotype and response to chemotherapy in squamous carcinomas. Cancer Cell 25, 809–821 (2014).
Vuga, L. J. et al. C-X-C motif chemokine 13 (CXCL13) is a prognostic biomarker of idiopathic pulmonary fibrosis. Am. J. Respir. Crit. Care Med. 189, 966–974 (2014).
Neale, S. D. & Athanasou, N. A. Cytokine receptor profile of arthroplasty macrophages, foreign body giant cells and mature osteoclasts. Acta Orthop. Scand. 70, 452–458 (1999).
Acknowledgements
This work was supported by the Juvenile Diabetes Research Foundation (JDRF) (Grant 17-2007-1063), the Leona M. and Harry B. Helmsley Charitable Trust Foundation (Grants 09PG-T1D027 and 2015PG-T1D063), the National Institutes of Health (Grants EB000244, EB000351, DE013023 and CA151884), and through a generous gift from the Tayebati Family Foundation. J.C.D. was supported by JDRF postdoctoral fellowship (Grant 3-PDF-2015-91-A-N). O.V. was supported by JDRF and DOD/CDMRP postdoctoral fellowships (Grants 3-2013-178 and W81XWH-13-1-0215, respectively). J.O. is supported by the National Institutes of Health (NIH/NIDDK) R01DK091526 and the Chicago Diabetes Project. D.L.G. is supported by the National Institutes of Health (NIH/NIDDK) UC4 DK104218. The authors would like to acknowledge the use of resources at W. M. Keck Biological Imaging Facility (Whitehead Institute), and Microscopy, Histology, Whole Animal Imaging, and Flow Cytometry Core Facilities (Swanson Biotechnology Center, David H. Koch Institute for Integrative Cancer Research at MIT).
Author information
Authors and Affiliations
Contributions
J.C.D. and D.G.A. designed experiments, analysed data and wrote the manuscript. J.C.D., O.V., A.J.V., H.H.T., S.F., M.M., J.L., A.B., A.C., S.A.-D., M.G., A.S., S.J., M.W., S.S., K.T., M.C., E.L., N.D., R.T., M.Q. and J.O. performed experiments. J.C.D. and H.H.T. performed statistical analyses of data sets and aided in the preparation of displays communicating data sets. J.O. and D.L.G. provided conceptual advice and technical support. R.L. and D.G.A. supervised the study. All authors discussed the results and assisted in the preparation of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Information (PDF 7377 kb)
Rights and permissions
About this article
Cite this article
Doloff, J., Veiseh, O., Vegas, A. et al. Colony stimulating factor-1 receptor is a central component of the foreign body response to biomaterial implants in rodents and non-human primates. Nature Mater 16, 671–680 (2017). https://doi.org/10.1038/nmat4866
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nmat4866
This article is cited by
-
Screening hydrogels for antifibrotic properties by implanting cellularly barcoded alginates in mice and a non-human primate
Nature Biomedical Engineering (2023)
-
Tracing immune cells around biomaterials with spatial anchors during large-scale wound regeneration
Nature Communications (2023)
-
Intragraft immune cells: accomplices or antagonists of recipient-derived macrophages in allograft fibrosis?
Cellular and Molecular Life Sciences (2023)
-
Advancing cardiac regeneration through 3D bioprinting: methods, applications, and future directions
Heart Failure Reviews (2023)
-
Allometrically scaling tissue forces drive pathological foreign-body responses to implants via Rac2-activated myeloid cells
Nature Biomedical Engineering (2023)