Abstract
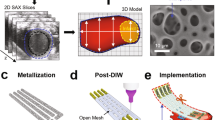
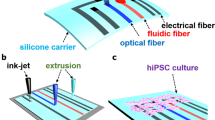
Biomedical research has relied on animal studies and conventional cell cultures for decades. Recently, microphysiological systems (MPS), also known as organs-on-chips, that recapitulate the structure and function of native tissues in vitro, have emerged as a promising alternative1. However, current MPS typically lack integrated sensors and their fabrication requires multi-step lithographic processes2. Here, we introduce a facile route for fabricating a new class of instrumented cardiac microphysiological devices via multimaterial three-dimensional (3D) printing. Specifically, we designed six functional inks, based on piezo-resistive, high-conductance, and biocompatible soft materials that enable integration of soft strain gauge sensors within micro-architectures that guide the self-assembly of physio-mimetic laminar cardiac tissues. We validated that these embedded sensors provide non-invasive, electronic readouts of tissue contractile stresses inside cell incubator environments. We further applied these devices to study drug responses, as well as the contractile development of human stem cell-derived laminar cardiac tissues over four weeks.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Bhatia, S. N. & Ingber, D. E. Microfluidic organs-on-chips. Nat. Biotechnol. 32, 760–772 (2014).
Mammoto, A. et al. Control of lung vascular permeability and endotoxin-induced pulmonary oedema by changes in extracellular matrix mechanics. Nat. Commun. 4, 1759 (2013).
Feinberg, A. W. et al. Muscular thin films for building actuators and powering devices. Science 317, 1366–1370 (2007).
Boudou, T. et al. A microfabricated platform to measure and manipulate the mechanics of engineered cardiac microtissues. Tissue Eng. A 18, 910–919 (2011).
Wang, G. et al. Modeling the mitochondrial cardiomyopathy of Barth syndrome with induced pluripotent stem cell and heart-on-chip technologies. Nat. Med. 20, 616–623 (2014).
Hinson, J. T. et al. Titin mutations in iPS cells define sarcomere insufficiency as a cause of dilated cardiomyopathy. Science 349, 982–986 (2015).
Agarwal, A. et al. Micropatterning alginate substrates for in vitro cardiovascular muscle on a chip. Adv. Funct. Mater. 23, 3738–3746 (2013).
Grosberg, A., Alford, P. W., McCain, M. L. & Parker, K. K. Ensembles of engineered cardiac tissues for physiological and pharmacological study: heart on a chip. Lab Chip 11, 4165–4173 (2011).
Park, S.-J. et al. Phototactic guidance of a tissue-engineered soft-robotic ray. Science 353, 158–162 (2016).
Lewis, J. A. Direct ink writing of 3D functional materials. Adv. Funct. Mater. 16, 2193–2204 (2006).
Hardin, J. O., Ober, T. J., Valentine, A. D. & Lewis, J. A. Microfluidic printheads for multimaterial 3D printing of viscoelastic inks. Adv. Mater. 27, 3279–3284 (2015).
Sun, K. et al. 3D printing of interdigitated Li-Ion microbattery architectures. Adv. Mater. 25, 4539–4543 (2013).
Miller, J. S. et al. Rapid casting of patterned vascular networks for perfusable engineered three-dimensional tissues. Nat. Mater. 11, 768–774 (2012).
Kolesky, D. B., Homan, K. A., Skylar-Scott, M. A. & Lewis, J. A. Three-dimensional bioprinting of thick vascularized tissues. Proc. Natl Acad. Sci. USA 113, 3179–3184 (2016).
Matsuhisa, N. et al. Printable elastic conductors with a high conductivity for electronic textile applications. Nat. Commun. 6, 7461 (2015).
Lipomi, D. J. et al. Skin-like pressure and strain sensors based on transparent elastic films of carbon nanotubes. Nat. Nanotech. 6, 788–792 (2011).
Berthier, E., Young, E. W. & Beebe, D. Engineers are from PDMS-land, biologists are from polystyrenia. Lab Chip 12, 1224–1237 (2012).
Kléber, A. G. & Rudy, Y. Basic mechanisms of cardiac impulse propagation and associated arrhythmias. Physiol. Rev. 84, 431–488 (2004).
Pasqualini, F. S., Sheehy, S. P., Agarwal, A., Aratyn-Schaus, Y. & Parker, K. K. Structural phenotyping of stem cell-derived cardiomyocytes. Stem Cell Rep. 4, 340–347 (2015).
Feinberg, A. W. et al. Controlling the contractile strength of engineered cardiac muscle by hierarchal tissue architecture. Biomaterials 33, 5732–5741 (2012).
Sheehy, S. P. et al. Quality metrics for stem cell-derived cardiac myocytes. Stem Cell Rep. 2, 282–294 (2014).
OštIádalová, I. et al. Early postnatal development of contractile performance and responsiveness to Ca2+, verapamil and ryanodine in the isolated rat heart. J. Mol. Cell. Cardiol. 25, 733–740 (1993).
Zhang, D. et al. Tissue-engineered cardiac patch for advanced functional maturation of human ESC-derived cardiomyocytes. Biomaterials 34, 5813–5820 (2013).
Zimmermann, W. H. et al. Three-dimensional engineered heart tissue from neonatal rat cardiac myocytes. Biotechnol. Bioeng. 68, 106–114 (2000).
Reiser, P. J., Portman, M. A., Ning, X.-H. & Moravec, C. S. Human cardiac myosin heavy chain isoforms in fetal and failing adult atria and ventricles. Am. J. Physiol. 280, H1814–H1820 (2001).
Lundy, S. D., Zhu, W-Z., Regnier, M. & Laflamme, M. A. Structural and functional maturation of cardiomyocytes derived from human pluripotent stem cells. Stem Cells Dev. 22, 1991–2002 (2013).
Nunes, S. S. et al. Biowire: a platform for maturation of human pluripotent stem cell-derived cardiomyocytes. Nat. Methods 10, 781–787 (2013).
Xiao, Y. et al. Microfabricated perfusable cardiac biowire: a platform that mimics native cardiac bundle. Lab Chip 14, 869–882 (2014).
Zimmermann, W.-H. et al. Tissue engineering of a differentiated cardiac muscle construct. Circ. Res. 90, 223–230 (2002).
LeGrice, I. J. et al. Laminar structure of the heart: ventricular myocyte arrangement and connective tissue architecture in the dog. Am. J. Physiol. 269, H571–H582 (1995).
Acknowledgements
The authors thank L. K. Sanders for her work on photography and time-lapse movies, J. A. Goss for his assistance with fabrication of the device holder and J. Minardi for his development of Mecode, and his help with machine automation. This work was performed in part at the Center for Nanoscale Systems (CNS), a member of the National Nanotechnology Infrastructure Network (NNIN), which is supported by the National Science Foundation under NSF award no. ECS-0335765. CNS is part of Harvard University. This work was also supported by the National Center For Advancing Translational Sciences of the National Institutes of Health under Award Number UH3TR000522, the US Army Research Laboratory and the US Army Research Office under Contract No. W911NF-12-2-0036, the Air Force Research Laboratory under Contract No. FA8650-09-D-5037-0004, and the Harvard University Materials Research Science and Engineering Center (MRSEC) award no. DMR-1420570. J.U.L. gratefully acknowledges support from the Villum Foundation. J.A.L. gratefully acknowledges support from the Office of Naval Research, Vannevar Bush National Security Science and Engineering Faculty Fellowship (Award No. N00014-16-1-2823).
Author information
Authors and Affiliations
Contributions
J.U.L., T.A.B., J.A.L. and K.K.P. designed the study. J.U.L. and T.A.B. designed the device. T.A.B. coded the 3D-print procedure and automation. J.U.L., T.A.B., A.K. and A.D.V. developed and characterized the printable materials. J.U.L., A.D.V. and T.A.B., optimized and printed devices. P.H.C. performed NRVM harvesting and prepared culturing media. J.U.L., M.Y. and A.P.N. performed NRVM culture, drug-dose experiments, and data analysis. M.Y. and J.U.L. conducted hiPS-CM culture, experiments and data analysis. F.S.P. and J.U.L. performed tissue staining, confocal imaging, and OOP analysis. S.-J.P. and J.U.L. conducted optical mapping experiments and analysis. H.Y. and J.J.V. developed the mechanical model of the device. J.U.L., T.A.B., J.A.L. and K.K.P. prepared illustrations and wrote the manuscript. F.S.P. and A.D.V. contributed to writing the manuscript.
Corresponding authors
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Information
Supplementary Information (PDF 5849 kb)
Supplementary Information
Supplementary movie 1 (MOV 8624 kb)
Supplementary Information
Supplementary movie 2 (MOV 4801 kb)
Supplementary Information
Supplementary movie 3 (MOV 8813 kb)
Supplementary Information
Supplementary movie 4 (MOV 164 kb)
Supplementary Information
Supplementary movie 5 (MOV 151 kb)
Supplementary Information
Supplementary movie 6 (MOV 104 kb)
Supplementary Information
Supplementary movie 7 (MOV 148 kb)
Supplementary Information
Supplementary movie 8 (MOV 9398 kb)
Supplementary Information
Supplementary movie 9 (MOV 1207 kb)
Supplementary Information
Supplementary movie 10 (MOV 2084 kb)
Supplementary Information
Supplementary movie 11 (MOV 1382 kb)
Supplementary Information
Supplementary movie 12 (MOV 1674 kb)
Supplementary Information
Supplementary movie 13 (MOV 1631 kb)
Supplementary Information
Supplementary movie 14 (MOV 638 kb)
Supplementary Information
Supplementary movie 15 (MOV 2341 kb)
Rights and permissions
About this article
Cite this article
Lind, J., Busbee, T., Valentine, A. et al. Instrumented cardiac microphysiological devices via multimaterial three-dimensional printing. Nature Mater 16, 303–308 (2017). https://doi.org/10.1038/nmat4782
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nmat4782
This article is cited by
-
Versatile human cardiac tissues engineered with perfusable heart extracellular microenvironment for biomedical applications
Nature Communications (2024)
-
Graphene-integrated mesh electronics with converged multifunctionality for tracking multimodal excitation-contraction dynamics in cardiac microtissues
Nature Communications (2024)
-
Three-Dimensional Tumor Models to Study Cancer Stemness-Mediated Drug Resistance
Cellular and Molecular Bioengineering (2024)
-
Nanomaterials-incorporated hydrogels for 3D bioprinting technology
Nano Convergence (2023)
-
Recent advances in 3D printable conductive hydrogel inks for neural engineering
Nano Convergence (2023)