Abstract
Human immunodeficiency virus (HIV) and Mycobacterium tuberculosis annually cause 3 million and 2 million deaths, respectively. Last year, 600,000 individuals, doubly infected with HIV and M. tuberculosis, died. Since World War I, approximately 150 million people have succumbed to these two infections—more total deaths than in all wars in the last 2,000 years. Although the perceived threats of new infections such as SARS, new variant Creutzfeldt-Jakob disease and anthrax are real, these outbreaks have caused less than 1,000 deaths globally, a death toll AIDS and tuberculosis exact every 2 h. In 2003, 40 million people were infected with HIV, 2 billion with M. tuberculosis, and 15 million with both. Last year, 5 million and 50 million were newly infected with HIV or M. tuberculosis, respectively, with 2 million new double infections. Better control measures are urgently needed.
Similar content being viewed by others
Main
The two culprits
M. tuberculosis infection does not necessarily transform into disease. Of the more than 2 billion individuals infected with M. tuberculosis, only approximately 10% will develop tuberculosis1,2. The pathogen is not eradicated, but is contained in distinct foci by the immune system. Critical for protection are CD4+ T lymphocytes. When disease develops, it generally manifests in the lung and is transmitted through the air. Hence, active tuberculosis is highly contagious and prevention of infection is nearly impossible. A vaccine against tuberculosis was developed in the early twentieth century by the French scientists Albert Calmette and Camille Guérin3, consisting of an attenuated strain of M. bovis, the etiologic agent of tuberculosis in cattle. The bacille Calmette-Guérin (BCG) vaccine protects against severe forms of childhood tuberculosis, but unfortunately, does not lead to eradication of M. tuberculosis and protective activity of the vaccine weakens during adolescence. As a consequence, BCG does not protect against the most prevalent disease form, pulmonary tuberculosis, in adults. Tuberculosis can be cured by chemotherapy, but the complex and long-lasting treatment, involving at least three drugs for 6 months, means compliance is often incomplete, resulting in a rising incidence of multidrug-resistant (MDR) strains. In several countries such as Estonia, the Russian Federation, Israel and Uzbekistan, more than 10% of all tuberculosis cases are caused by MDR strains1. In low-income countries MDR tuberculosis results in no treatment and often leads to death and further spread.
Infection with HIV, in contrast, consistently transforms into disease, and is contagious at all stages. HIV predominantly resides in CD4+ T lymphocytes. Infected and noninfected T cells are damaged, causing immunodeficiency. With new antiretroviral drugs, HIV infection can be controlled, but not eradicated. Treatment, however, is expensive and less than 5% of individuals infected with HIV in developing countries have access to effective treatment. Anti-HIV drugs target HIV reverse transcriptase, protease, integrase or the coiled coil domain of gp41. Used in combinations of three or more, they are very effective at treating HIV infection: patients with advanced AIDS have shown dramatic albeit incomplete recovery of CD4+ T cell counts and immune function, though sometimes the revitalized immune response causes severe problems by reacting to previously silent infecting pathogens. Yet even when virus loads have become undetectable for several years, cessation of drugs results in rapid rebound of virus and return to the pretreatment levels4. This implies that patients need to take these drugs for life. But because of serious side effects and expense, indefinite treatment is not possible for most of the world. Drug resistance by virus mutation is well described5 and although triple therapy reduces the risk substantially, imperfect adherence to treatment regimes may result in selection of resistant virus. As is the case for tuberculosis, this could limit treatment options in the near future. Transmission, however, can be reduced by 'safer sex' practices. Such behavior changes may account for the reduction in prevalence of HIV-1 infection from >20% to 8% in Uganda over 10 years6.
The dangerous liaison between AIDS and tuberculosis
In South Africa, more than 10% of the 40 million inhabitants are infected with HIV and more than 5% suffer from active tuberculosis. In this country, more than half of all individuals with tuberculosis have concurrent HIV infection. Immunodeficiency caused by HIV infection increases the risk of developing tuberculosis dramatically—10% of double-infected individuals will develop active tuberculosis within a year of coinfection, as compared to the 10% lifelong risk in individuals infected with M. tuberculosis alone. Despite the availability of effective chemotherapy to cure tuberculosis and the successful development of antiretroviral drugs that control HIV, vaccines provide the only realistic hope of effective prevention.
Host response to tuberculosis
Tuberculosis most frequently develops in the lung (Fig. 1). Once tubercle bacilli have reached the lung alveoli, they are taken up by alveolar macrophages and probably dendritic cells (DCs) in the lung interstitium (Fig. 1). M. tuberculosis is protected by a recalcitrant cell wall rich in waxes and other glycolipids7, which is responsible for the unique staining characteristics of these microbes and contributes significantly to resistance against host defense. Infected macrophages and DCs, therefore, do not destroy their bacterial prey and thus serve as a mobile habitat, transporting the microbes to the lung parenchyma and eventually to the draining lymph nodes8,9. Infected macrophages attract monocytes and a lesion develops. DCs in the lymph nodes present mycobacterial antigens to T cells. At this early stage of infection, secreted proteins such as early secreted antigen for T cells (ESAT-6) and antigen 85 (Ag85) presumably serve as dominant antigens for CD4+ T cells, which accumulate in great numbers in lesions early after infection. At later stages of infection, CD8+ T cells also become stimulated10. In addition, unconventional T cells are activated, including T cells expressing a γδ T cell receptor with specificity for small phosphorylated ligands and T cells with specificity for glycolipids, which are presented by major histocompatibility complex (MHC) class I–like molecules of the CD1 family11,12,13,14. Studies in nonhuman primates support a role for γδ T cells in protective immunity against tuberculosis13. The CD1-restricted T cells presumably evolved as a result of the evolutionary cross-talk between mycobacteria and the mammalian host, as they are specific for glycolipids abundant in mycobacteria but not found in other microbial pathogens11.
M. tuberculosis enters the host within inhaled droplets. Three outcomes are possible. (i) Immediate eradication of M. tuberculosis by the pulmonary immune system. This alternative is rare to absent. (ii) Infection transforms into tuberculosis. This frequently occurs in immunodeficient individuals, with the notable example of HIV infection increasing the risk of developing tuberculosis 800-fold. (iii) Infection does not transform into disease because M. tuberculosis is contained inside granulomas. In the diseased individual, M. tuberculosis is no longer contained because caseation of the lesion results in dissemination and transmission of M. tuberculosis. After inhalation, M. tuberculosis is engulfed by alveolar macrophages and DCs. In draining lymph nodes, these cells present mycobacterial antigens to different T cell populations. Antigen presentation probably involves cross-priming, allowing transfer of mycobacterial antigens from infected macrophages to dendritic cells. Antigen-specific CD4+ T cells, CD8+ T cells, γδT cells and CD1-restricted T cells participate in protection. Most importantly, macrophages are activated by IFN-γ and TNF-α. In addition, T cells may kill mycobacteria present in macrophages by means of perforin and granulysin.
Antigen-specific T cells induce the formation of a granuloma around infected macrophages, primarily composed of monocyte-derived macrophages (some of which transform into multinucleated giant cells), CD4+ T cells and an outer ring of CD8+ T cells. At later stages, the granuloma is surrounded by a fibrotic wall and lymphoid follicular structures develop in the vicinity, probably orchestrating the local immune response15.
In the granulomatous lesion, macrophages are activated by T lymphocytes through production of type I cytokines, notably interferon (IFN)-γ and tumor necrosis factor (TNF)-α16. IFN-γ activates the capacity to control M. tuberculosis in macrophages17,18. Moreover, IFN-γ and TNF-α are instrumental in walling off M. tuberculosis inside granulomatous lesions. The importance of these cytokines in the containment of mycobacteria is well illustrated by the observation that individuals with deficient IFN-γ signaling suffer from rapid onset of mycobacterial diseases, and that treatment with antibodies that neutralize TNF-α in individuals with rheumatoid arthritis reactivates tuberculosis in those with latent infection19.
The granuloma persists for years and efficiently contains tubercle bacilli as long as the individual remains immunocompetent. The granuloma deprives the arrested mycobacteria of oxygen and nutrients and as a direct consequence, the microbes survive, probably in a state of dormancy20,21,22,23. The gene expression profile of M. tuberculosis is altered in response to the restricted growth conditions in the granulomatous lesion. It is highly probable that some of these dormancy-related gene products serve as the major antigens of dormant M. tuberculosis and hence represent promising candidate antigens for a postexposure vaccine aimed at preventing reactivation tuberculosis. The best-known dormancy antigen is the α-crystallin, a small heat-shock protein (Hsp) also termed HspX23.
Host resistance, latency and tuberculosis outbreak
The mechanisms that determine latency and disease outbreak in tuberculosis remain elusive. Although the risk of reactivation is understood to be determined by both host and microbial factors in addition to environmental components, virtually nothing is known about the responsible genes. Increasing epidemiologic evidence that strains of the M. tuberculosis Beijing/W genotype family, many of which are of the MDR type, are spreading throughout the world suggests that this family of M. tuberculosis evolved against the evolutionary pressure of BCG vaccination and chemotherapy24,25.
A careful histologic analysis of lung autopsy material performed from 284 cadavers more than 100 years ago in Zürich showed almost 100% M. tuberculosis infection in individuals over 21 years of age, who had died of unrelated reasons26. We can assume similarly high incidences nowadays for individuals living in tuberculosis 'hot spots' (e.g., prisons in some countries) and infection rates between 10% and 50% in areas with high M. tuberculosis incidences.
How and why disease outbreak occurs after a period of latency are unclear27,28. Increased risk of tuberculosis as a result of unique environmental and behavioral factors such as alcohol abuse or dietary iron overload emphasizes the importance of these components, but again provides little explanation of specific control mechanisms29. A considerable proportion of individuals with tuberculosis develop disease within the first year after infection. Moreover, superinfection as well as reinfection after successful tuberculosis chemotherapy have been described30. It is probable that these individuals develop an insufficient immune response against natural infection with M. tuberculosis because of genetic host susceptibility, immune suppression by the pathogen or both. Elucidation of the genetic mechanisms underlying susceptibility and protective immune mechanisms in resistant individuals that prevent disease outbreak in face of ongoing infection, as well as identification of the pathogen genes that promote transformation of latent infection into active tuberculosis, will facilitate rational design of a postexposure vaccine27,28,31.
Of equal importance will be the careful analysis of the efficacy of BCG vaccination. BCG was found to protect against adult tuberculosis in the UK and against leprosy in Malawi, but did not provide any protection in the World Health Organization trial in south India32. Overall, a 50% protective efficacy has been estimated for BCG33. Although environmental factors, notably frequent infection with atypical mycobacteria, probably have a role, contribution of genetic host factors should be assessed more carefully. It is possible that a small proportion of BCG-vaccinated individuals develops a long-lasting immune response against tuberculosis, whereas the majority does not. Because any new vaccine has to protect individuals who do not mount an appropriate immune response to natural infection with M. tuberculosis or to vaccination with BCG, the susceptible and resistant target populations and the criteria that distinguish them from each other need to be defined carefully.
Vaccination strategies against tuberculosis
Subunit vaccines given alone or in addition to BCG. New subunit vaccines against M. tuberculosis comprise antigen-adjuvant formulations, naked DNA vaccine constructs or recombinant carriers expressing antigen (Table 1)34. They are mainly based on protein antigens. Unfortunately, reliable rules for defining protective antigens for T cells do not exist. Most vaccine antigens investigated thus far are early produced secreted antigens such as Ag85, a shared antigen with BCG, and Esat-6, which is an antigen unique to M. tuberculosis (Fig. 2)35,36. Such antigens are probably adequate for pre-exposure vaccination. For individuals latently infected with M. tuberculosis, a postexposure vaccine composed of dormancy-related antigens such as HspX seems more suitable (Fig. 2)21,22,23.
(a,b) A pre-exposure vaccine should comprise the set of antigens that are rapidly secreted early after infection, but would be ineffective in latent infection because its antigenic composition does not match the dormancy-induced antigenic repertoire. (c) A postexposure vaccine composed of dormancy-induced proteins should match the antigenic repertoire of dormant M. tuberculosis. (d) Ideally, a combination of both types of antigens would protect against both early childhood tuberculosis and adult reactivation tuberculosis because the antigenic repertoire would reflect the different stages of infection. Red line, nonvaccinated; blue line, vaccinated.
A recent screen has assessed the protective efficacy in mice of more than 30 antigens that are differentially expressed in the proteomes of M. tuberculosis versus BCG37. From these, only one antigen was identified that induced a robust protection similar to that of BCG, arguing against a unique role in protection of proteins exclusively present in the proteome of M. tuberculosis.
Although proteins will constitute the major antigens of subunit vaccines, glycolipid antigens can be included in these vaccine formulations. Such glycolipids could serve both as antigen in the context of CD1 and as adjuvant for Toll-like receptors (TLRs)11. Generally, subunit vaccines crucially depend on appropriate adjuvants38 that stimulate T helper type 1 (TH1) immune responses by the different T cell populations required for protection against tuberculosis.
Naked DNA constructs can stimulate CD4+ and CD8+ T cells. Although they have proven their high immunogenicity in small-rodent animal models, human studies are thus far mostly disappointing. But new carrier systems such as polylactide glycolyde microparticles may facilitate application of naked DNA vaccines in humans39. Recombinant bacterial and recombinant viral carriers expressing defined mycobacterial antigens have been constructed and their vaccine efficacy against tuberculosis have been determined in experimental animal models. These vectors induce potent CD8+ and CD4+ TH1 responses. The most advanced vaccine of this type is recombinant modified vaccinia virus Ankara (r-MVA) expressing Ag85, which has already entered phase 1 clinical trials40,41.
Vaccination with Mtb 72F protein in AS02A adjuvant or in the form of naked DNA induces protective immunity in both mice and guinea pigs42. Mtb 72F is a recombinant fusion protein composed of Rv0125 and Rv1196 with a predicted size of 70 kDa. The adjuvant AS02A is composed of a nontoxic lipopolysaccharide derivative and QS21 from quillaja saponaria (a triterpene glycoside) as an oil-in-water emulsion. The Mtb 72F-AS02A vaccine formulation has now entered a phase 1 clinical trial in healthy M. tuberculosis-uninfected volunteers (Table 2). Another protein-based vaccine comprising a fusion protein of Esat-6 and Ag85 in a mixture of oligodeoxynucleotides and a polycationic peptide (IC31) as an adjuvant has shown promising results in experimental animals and hence is aimed at entering a phase 1 clinical trial later in 2005 (Table 2)36.
Generally heterologous prime-boost schemes are composed of a relatively simple first component (e.g., DNA) that primes a focused immune response, and a second boost vaccine that induces an inflammatory response (e.g., using a recombinant virus) to magnify the initial response. To achieve a proper prime-boost effect, shared antigens are required for the subunit boost vaccination. In tuberculosis, however, heterologous prime-boost vaccination schemes starting with a BCG prime followed by a subunit boost are considered most promising, not only for scientific reasons but also because BCG vaccination of newborns cannot be given up prematurely. The recently discovered antigen Rv3407 is encoded in the BCG genome but is undetectable in its proteome37. The increased protection seen in BCG-primed mice after boost vaccination with naked DNA encoding Rv3407 indicates that this protein is an important antigen of M. tuberculosis that is suboptimally expressed in BCG. Similarly, boost with Mtb 72F in AS02A adjuvant increased protection induced by BCG prime43. The r-MVA expressing Ag85 induced substantial protection both when given alone or as booster vaccination on top of BCG prime41. A recent clinical phase 1 trial showed that r-MVA-Ag85 induced Ag85-specific IFN-γ–secreting T cells (Table 2)40. More profound effects were observed in the BCG prime–r-MVA-Ag85 boost group, underlining the importance of heterologous prime-boost vaccination in the rational delineation of future tuberculosis vaccination strategies.
Attenuated gene deletion mutants of M. tuberculosis as vaccine candidates. Vaccine efficacy data of mutant M. tuberculosis are still limited. During the early stage of infection, M. tuberculosis replicates actively. Accordingly, M. tuberculosis knockout mutants, in which synthesis of essential amino acids is prohibited, will not grow in lungs of experimentally infected mice. Typically, these are auxotrophic mutants that die of starvation in the absence of the required nutrients (Table 1)44,45. A second group of M. tuberculosis knockout mutants show reduced growth in lungs of experimentally infected mice, but persist at a lower level than wild-type microorganisms. These mutations include deficient regulatory proteins, such as the phoP/phoQ two-component regulatory system and a variety of mutants with deficient lipid metabolism or transport46,47. Although genes of this group include virulence factors, it is also possible that the gene products are needed for persistence rather than harming the host directly. M. tuberculosis knockout mutants deficient in genes expressed during dormancy replicate in the lungs of experimental mice in an unconstrained manner early after infection, but cease to grow at later stages because of their impaired dormancy gene program. One of the best described genes of this group is that which encodes isocitrate lyase48. M. tuberculosis knockout mutants, which grow as well as wild-type microorganisms but induce weaker pathology, lack true virulence factors. Some knockout mutants behave like wild-type M. tuberculosis in the lung but do not disseminate to other organs. The heparin-binding hemagglutinin adhesion molecule seems to participate in the dissemination of M. tuberculosis to extrapulmonary sites and hence qualifies as a member of this group49. Factors that facilitate dissemination to other tissues should be deleted in a viable vaccine in order to focus the response on the lymph nodes. A recently defined group of M. tuberculosis knockout mutants comprises strains that grow as well as wild-type microorganisms in normal mice, but do not persist in mouse knockout mutants with defined immunodeficiency50.
Vaccine candidates based on M. tuberculosis knockout mutants will probably face strong objections against use in human clinical trials largely because of the genetic stability of the mutants. Reversion is best prevented by having two independent chromosomal gene deletions. The advantage of M. tuberculosis knockout mutants is their profound stimulation of all T cell populations relevant to protective immunity. On the other hand, M. tuberculosis is known to impair the host immune response. Therefore, it is probably not sufficient to reduce the virulence of M. tuberculosis knockout mutants. Additional genetic modifications improving the immune response and reducing pathology will be required. Although these vaccines will have a long way to go, a rationally designed M. tuberculosis mutant lacking a defined set of virulence genes in the long run could have great potential as a tuberculosis vaccine.
Improved recombinant BCG as vaccine candidates. As compared to M. tuberculosis, the current vaccine BCG lacks approximately 130 genes that are clustered in 16 regions of difference (RD)51 and are at least in part involved in pathogenicity and persistence. Reintroduction of selected genes may increase immunogenicity, antigenicity or both of BCG without reverting it to a pathogen (Table 1). Improved immunogenicity results in the stimulation of a profound immune response. Antigenicity can be improved by introduction of additional antigens or by overexpression of antigens expressed at suboptimal level.
Pym et al. have introduced the entire RD1 region of M. tuberculosis into BCG, comprising at least 11 genes52. Although it remains to be clarified whether the recombinant BCG (r-BCG) expressing RD1 genes is endowed with improved immunogenicity, antigenicity or both, it was claimed that this vaccine candidate provided slightly better protection than parental BCG in mice. Not unexpectedly, however, this r-BCG candidate showed higher virulence in immunocompromised mice as compared to wild-type BCG.
Reintroduction of genes missing in BCG that do not confer virulence might increase vaccine efficacy of BCG without decreasing its safety. Horwitz et al. introduced the gene encoding Ag85 into BCG, an abundant secreted protein in M. tuberculosis53. Although the gene is also expressed in BCG, it was assumed that overexpression of this immunodominant antigen would increase protective immune responses. Indeed, in guinea pigs, r-BCG expressing Ag85 induced substantially higher protection than parental BCG against tuberculosis. This vaccine was at least as safe as BCG and has recently entered a phase 1 clinical trial (Table 2).
The r-BCG vaccine candidates with higher immunogenicity comprise strains that express human cytokines such as IFN-γ, IFN-α, interleukin (IL)-2, IL-12 and granulocyte macrophage colony stimulating factor (GM-CSF)54,55,56. However, these cytokine-secreting r-BCG have yet to prove superior protection in animal models against tuberculosis, as they have not yet been compared to parental strains.
Another approach to improving immunogenicity of BCG takes advantage of the biological activity of listeriolysin (Hly)57. In its natural host, Listeria monocytogenes, this cytolysin forms pores in the phagosomal membrane, promoting listerial egression into the cytosol58. In the cytosol, listerial antigens are readily introduced into the MHC class I pathway, causing preferential stimulation of CD8+ T cells. Compelling evidence suggests that BCG is insufficiently equipped for stimulating CD8+ T cells, whereas CD4+ T cell stimulation is satisfactory59, the gene encoding Hly was introduced into BCG to improve CD8+ T cell stimulation. Indeed, such vaccine constructs induced better protection than parental BCG in mice (Grode, L. et al; unpublished data). Production of this vaccine under good manufacturing practices (GMP) conditions has been initiated and this candidate is aimed at entering a phase 1 clinical trial in 2005 (Table 2).
Pros and cons of subunit and viable vaccines
The use of subunit vaccines is based on the assumption that one or a few protective antigens and T cell clones will suffice for efficacious protection16. In contrast, attenuated viable vaccines utilize the whole spectrum of expressed antigens to stimulate an optimal combination of T cell subtypes. Genetically engineered viable vaccines are therefore best suited as replacements for BCG. Despite previous reluctance, a recent expert group meeting has strongly advocated development of viable recombinant vaccines against tuberculosis because they are the most potent stimulators of protective immune responses that perform better than BCG in experimental animal models60. As an essential requirement, any new viable vaccine should be at least as safe as BCG in immunocompetent and safer than BCG in immunocompromised individuals.
Cross-reactive immune responses against atypical mycobacteria might prematurely eradicate an improved r-BCG or attenuated recombinant M. tuberculosis and thereby impair efficacy of genetically engineered viable vaccines. Although subunit vaccines are probably not affected by the preexisting cross-reactive immunity to environmental bacteria, generally immunity induced by subunit vaccines is short-lived. Given the complementary strength of both types of new vaccine candidates, a heterologous prime-boost regimen comprising a prime with a viable vaccine candidate superior to BCG and a boost with a subunit vaccine candidate will probably be the most promising combination to ensure long-lasting efficacy.
AIDS: infection, pathogenesis, immune response and disease
HIV is a member of the lentivirus subgroup of the retrovirus family, so named because of a long period of clinical latency after infection. Its envelope is derived from cell membrane and expresses the glycoproteins gp120 (responsible for virus attachment to cells) and gp41 (responsible for membrane fusion). Internally, matrix (gag p17) and capsid (gag p24) proteins enclose the viral RNA. Other viral proteins include the reverse transcriptase, protease, integrase and regulatory proteins nef, tat, rev, vif, vpr and vpu. The virus infects by attaching gp120 to the CD4 molecule and either the chemokine receptor CCR5 or CXCR4 present on T cells61. Gp41 mediates fusion and in the cytosol the RNA is reverse transcribed and the preintegration complex moves to the nucleus, where the cDNA is integrated as provirus into host DNA in activated cells. Gene expression is normally immediate; first regulatory and then structural proteins are made, regulated by tat and rev proteins. New virus particles bud from the surface of infected cells about 24 h after infection. Virus is shed for a further day or so before the cell dies62.
Pathogenesis, immune response and disease. AIDS is insidious. HIV-1 infection often causes a transient acute febrile illness shortly after infection, when virus levels in the blood peak, but after that, infection is silent. A degree of immune control by CD8+ T cells is achieved, and neutralizing antibodies eventually appear, although too late to prevent infection, and are easily evaded by viral mutation. T cell immunity seems to control the infection over several years but with a dynamic process of immune selection and escape occurring63. CD4+ T cells are both deleted and functionally impaired early64, with HIV-specific T cells preferentially infected and depleted65. However, in some cells (e.g., long-lived memory T cells and macrophages), gene expression is delayed and the infection becomes latent. The progressive loss of CD4+ T cells leads to clinical immunodeficiency, which is manifested by opportunistic infections and, often, reactivation of tuberculosis. These infections rapidly cause death if untreated.
HIV infects CD4+ T cells and monocytes and macrophages. The virus is cytopathic in activated T cells, but less so in macrophages, and not at all in latently infected cells with integrated provirus. These different forms of infection present problems for vaccines. Those that stimulate and maintain high levels of neutralizing antibodies could prevent initial infection, but once that has occurred, it is almost impossible to eliminate HIV. Under prolonged antiretroviral drug therapy, virus is eliminated from the activated T cells that express the enzymes targeted by the drugs, but not from cells in which virus turns over slowly or is latent66. Thus if an HIV vaccine does not prevent infection, it is unlikely to eliminate the virus but may be able to control the ongoing infection and prevent disease.
There is no known protective immunity against HIV, in the sense that virus is never eradicated from those infected so that it is impossible to find people protected by previous infection, as is the case for many other viruses, such as measles, mumps and influenza. This poses serious problems for vaccine development, although it is not unique (Epstein-Barr virus is another such example). Adult monkeys infected with attenuated SIV (e.g., with deletions in nef) do not become sick, and are protected from challenge with pathogenic SIV67. This protection is probably, but not certainly, immunological68. Some highly HIV-exposed individuals resist HIV infection; others develop T cell responses to HIV69 but not serum antibodies, and their immunity depends on continuing exposure to the virus70. This may represent immune resistance, although it is hard to prove. Another clue may come from the rarity of superinfection in people infected with HIV who are repeatedly exposed to further infection. Although there are elegant studies of superinfection71, it is suspected that it is rare; if so, its rarity probably reflects immune protection.
The spread of HIV-1 infection around the world in 20 years has been alarming. The worst epidemics are in sub-Saharan Africa, where more than 50% of young adults are infected. Mortality from HIV infection without drug treatment is close to 100%, although infected people usually survive from 5 to 10 years before developing AIDS. The introduction of effective antiretroviral drugs in high-income countries has reduced mortality without reducing infection.
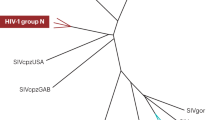
Virus variability. HIV is the most variable virus known. There are six major subtypes, A, BC, D, E, F and G, which are 'ancient' (in the HIV context of 30–50 years) and have distinct geographical distribution (Fig. 3)72. The complexity is even greater because of recombinations between subtypes and within subtypes. Each subtype differs by >20% in amino-acid sequence, so that T cells specific for one subtype are unlikely to cross-react substantially with the others; each epitope of 9–15 amino acids will probably have two or more mutations, and this level of variability is known to adversely affect T cell recognition73. Although there are a few cross-reactive T cell epitopes, as well as conserved segments of HIV, it may be necessary to match any virus subtype with that of the circulating viruses in the population to be vaccinated. It is less certain that subtype-specific vaccines will be necessary for stimulating neutralizing antibodies, although sequence variability is known to be a major problem.
A further complication is the variability within each subtype and within each individual. It is clear that both antibodies and CD8+ T cells are very effective at selecting virus escape mutants74,75,76,77. As human leukocyte antigen (HLA) type controls the epitopes recognized by T cells, it is not surprising that HLA type influences virus sequence in individuals as a consequence of T cell–driven escape78. However, the mutant virus may be less fit and the escape can offer advantages to the host. The constraints on the virus probably account for the overall conservation of virus sequence in primary infection, before the immune response evolves. Therefore, vaccines that focus on conserved consensus sequences may have the best chance, at minimum selecting slightly less fit viruses during primary infection.
A T cell vaccine that permits infection and induces selection of escape mutants could undermine vaccine effectiveness, as has been seen in macaques79. But selection of less fit virus has also been observed in macaques in whom SIV infection remains controlled, so this could favor the host80.
Vaccination strategies against AIDS
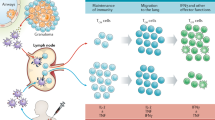
Challenges. For HIV there are two major challenges: to find (i) immunogens that can stimulate broadly cross-reacting neutralizing antibodies and (ii) immunogens that stimulate high levels of persisting CD8+ and CD4+ T cells. Both humoral and cellular immunity may be needed, but they require different types of immunogens; eventually vaccines could be mixed to achieve both (Fig. 4).
A prophylactic vaccine will be given months or years before exposure and, hopefully, prevent or ameliorate infection. An antibody-inducing vaccine could prevent infection81, but as indicated above, a vaccine that stimulates T cell immunity cannot stop virus infecting cells. The latter vaccination might enable the host to suppress the infection for long periods and prevent disease. Thus, macaques vaccinated to stimulate T cell immunity against SIV became infected when challenged with virus, but had very low virus loads and experienced little effect on their health as compared to unvaccinated controls82,83,84. Because it is almost impossible to eliminate HIV infection, this may be the best that can be achieved. However, many chronic virus infections as well as latent M. tuberculosis infection are controlled effectively in the long term by cellular immunity without causing disease. HIV-2 does not cause disease in more than 80% of those infected in West Africa85, suggesting that the immune response and the virus are in balance in the infected but healthy individual.
Antibody-stimulating vaccines. At present there is no realistic candidate HIV vaccine. It was thought that gp120 preparations would stimulate neutralizing antibodies, and they do against tissue culture–adapted HIV strains. However, all such vaccines have failed to neutralize primary virus isolates and one tested in two large efficacy trials failed to protect (NAM, http://www.aidsmap.com/). Now the aim is to design HIV envelope protein immunogens that will stimulate protective antibodies. Unfortunately the dice are loaded against this: (i) the envelope is heavily glycosylated, making it largely nonimmunogenic; (ii) it is conformationally variable, so that the most sensitive site, the chemokine receptor binding site, is not exposed unless CD4+ has bound; (iii) the CD4+ binding site is deeply recessed and hard to access by antibodies; (iv) besides the carbohydrates, crucial parts of the gp120 surface are protected by hypervariable loops, which can and do vary by mutation at no cost to the virus, thereby escaping neutralizing antibodies86,87. Real novelty in immunogen design is needed to get around these problems.
T cell–stimulating vaccines. As an alternative, much effort is being made to create vaccines that stimulate T cell immunity, particularly CD8+ T cells. In mice, several approaches comprising plasmid DNA and various recombinant viruses and recombinant bacteria have given promising results88,89,90. Also particulate proteins and peptide-pulsed DCs can efficiently stimulate CD8+ T cells91,92. But these findings are not easily transferable to primates. DNA vaccines stimulate only weak responses in humans93 and recombinant viruses give mixed results. The poxviruses (canary pox, the attenuated vaccinia virus (NYVAC) and MVA) induce weak primary responses94,95, possibly because the recombinant immunogen is swamped by more than 200 poxvirus proteins. Also, these viruses may be too attenuated, with little or no proliferation after infection. However, they may be better at boosting T cell responses that have already been primed (e.g., BCG; Table 1). The most promising results to date come from recombinant adenovirus 5, which has stimulated strong and sustained T cell responses, but its applicability is constrained by the high frequency of antibodies to this virus in most human populations. Alternate candidates in trial include other strains of adenovirus, adeno-associated virus, alphaviruses and r-BCG as vectors for HIV.
As for tuberculosis, heterologous prime-boost regimes offer enhanced T cell immune responses96,97 and have been observed in macaques and humans94. It seems that in humans, recombinant adenoviruses are good at both priming and boosting, whereas recombinant poxviruses such as MVA are better at boosting than priming (McMichael, A.J., Goonetilleke, N., Guimaeres-Walker, A., Dorrell, L., Yan, H., Hanke, T., unpublished data).
Vaccine-induced T cell responses should include both CD4+ and CD8+ T cells, even though the former are targets for the virus. CD4+ T cell help is important for optimal CD8+ T cell responses98,99,100,101—an issue of particular importance to HIV vaccine development because natural infection results in impaired CD4+ T cell immunity.
Protein immunogens typically elicit antibody responses and T helper cell responses, but the latter may be of the TH2 type, especially when alum is used as an adjuvant102; TH2 responses have little or no antiviral activity. Live intracellular infections generally elicit TH1 responses and CD8+ T cell responses, hence the use of live attenuated vectors to mimic a virus infection. These deliver the required immunogen into the cytosol, from which it can enter the MHC class I antigen presentation pathway directly, or indirectly when the cell dies and virus protein is taken up by DCs for 'cross-priming' of CD8+ T cells103,104,105,106.
People who are homozygous for the δ32 variant of CCR5 do not express an intact chemokine receptor and are resistant to HIV infection107. Immune resistance is suspected for people who are highly exposed, yet uninfected. Many generate CD8+ and/or CD4+ T cell responses, but without any serum antibody69. It is not certain that the T cell responses are responsible for resistance. If they are, it is encouraging because the levels of T cell response seen in current vaccine trials could be sufficient.
HIV vaccines and mucosal immunity
HIV enters the host through (usually genital) mucosa. HIV infects, or attaches to, mucosal Langerhans cells first and then migrates to local lymphoid sites108 to set up systemic infection with a predominance of early virus in intestinal tract CD4+ T cells109. Mucosal IgA and T cells may have an important role in control of this infection.
An HIV vaccine should stimulate B and T cell as well as mucosal and innate immunity. Live attenuated HIV probably provokes all of these, but because it will set up a persistent infection, there are insoluble safety issues that render its use unlikely in humans. Therefore, it may be necessary to build a set of vaccines to stimulate each component separately and administer them in combination.
Degree of protection
If control equivalent to that of chronic Epstein-Barr virus or cytomegalovirus or latent M. tuberculosis infection could be achieved for HIV, with reduced or negligible further transmission, it would represent a considerable advance. Measuring the efficacy of the vaccine would be problematic, being dependent on reduced virus load at set point, the time at around 6 months after primary infection when virus level stabilizes. The set-point level is inversely correlated with time of survival. Only neutralizing antibodies, stimulated by vaccines, offer any real chance of sterile immunity and such vaccines are a long way off.
A prophylactic vaccine for HIV is badly needed. Unless current trials of vaginal microbicides are unexpectedly successful, there is no other way of controlling the infection and both antibody- and T cell–inducing vaccines need a total rethink. The most advanced of these vaccines is the Merck recombinant adenovirus 5 (Ad5) vaccine that is about to enter clinical trials. But even if successful, a different vector will be needed to deal with the problem of pre-existing antibody immunity to Ad5. The Merck trial may, however, indicate whether vaccines that stimulate T cell immunity offer any benefit, and that type of news is to be welcomed. Could AIDS and tuberculosis vaccines be given together? Probably, but this may be decades away. In parts of Africa, BCG is given at birth. Combining BCG with an AIDS vaccine, with a boost at puberty, may be feasible in the distant future.
From animal models to clinical trials
Preclinical studies: tuberculosis and AIDS vaccine testing. Most tuberculosis vaccine candidates have been tested in mice or guinea pigs. Studies in mice take advantage of the in-depth knowledge of the mouse immune system, whereas guinea pigs have the advantage of developing a pathology that highly resembles human tuberculosis. These experimental animal studies form the starting point of the tedious pipeline leading to a new vaccine candidate110. The US National Institutes of Health, through their preclinical tuberculosis screening program, and the European Union, through its TBVac integrated project in the Framework Program 6, sponsor vaccine testing in experimental animals under standardized conditions. Thus far, the two programs utilize different screening procedures, which need to be harmonized in order to achieve comparability of different vaccine candidates. However animal models cannot unequivocally predict the efficacy of a vaccine candidate against tuberculosis or HIV and immunogenicity results in mice often do not predict responses in humans. Although nonhuman primate studies can be bypassed before phase 1 and phase 2 clinical trials, they may become necessary before embarking on phase 3 trials.
Phase 1 and phase 2 clinical trials should also be exploited for determination of immunological correlates of protection (i.e., markers that unequivocally predict protective efficacy of a vaccine candidate). Currently, IFN-γ produced by T cells with specificity for defined antigens is probably the best marker of protection111 for tuberculosis, but this is much less clear for HIV. In the most impressive vaccine protections studies, using attenuated SIV as a vaccine it is not known what confers protection68,112 and the IFN-γ ELISPOT assay for T cells does not correlate with protection in vaccine-protected macaques68. Additional markers are required.
The SIV challenge model in macaques has been very useful for HIV vaccine development67, but there are limitations. In these experiments, the virus challenge dose is always large, compared to repeated low-dose exposures in humans. In addition, the vaccine is nearly always homologous to the challenge virus, giving good chances of success that are unrealistic in humans. Attempts are being made to introduce more representative challenges113. Finally the SIV or SIV-HIV hybrid (SHIV) challenges may be slightly misleading; it seems easier to protect against the aggressive hybrid virus SHIV 89.6P compared to the less virulent SIV mac 239. It is unclear which will be closer to an HIV exposure in humans. Despite these problems, the existing data suggest vaccine-induced protection is possible.
Therapeutic vaccination for HIV is rarely discussed, but must be considered as recent studies in macaques and humans114,115,116 give it some credibility. In humans, therapeutic vaccination would probably be used to stimulate T cell responses in HIV-infected people whose virus was well controlled by antiretroviral drugs, with the aim of terminating antiretroviral therapy (ART) once the T cell levels were boosted. The rationale is that T cells, particularly CD8+ T cells, are known to be effective in long-term control of the virus in the absence of drug treatment, but T cell responses decline in patients on effective ART117. When ART is stopped, virus rebounds to pretreatment levels4. If the T cell levels were already boosted, this might lead to lower virus levels at the new set point. At its best, this treatment could enable withdrawal of ART for prolonged periods and offer new options in low-income countries in particular. Patients whose virus was controlled in this way might also be less likely to transmit virus.
Clinical trials. The earliest vaccine trials are small and are concerned with vaccine safety and immunogenicity. Then immunogenicity is optimized by finding the best vaccine dose and route of delivery. Finally, the vaccine efficacy trials involve several thousand volunteers who are at high risk for infection. Translation of vaccine candidates from bench science into clinical trials is relatively straightforward scientifically but complicated logistically and extremely expensive (Box 1).
Phase 1 trials can be done in the country of origin of the vaccine, but increasingly good sites are being established in developing countries and several countries have HIV vaccine trial experience. In contrast, experience with tuberculosis vaccine trials is marginal and currently only a few phase 1 trials have been initiated. Two phase 3 trials of Vaxgen gp120 in 10,000 people showed clearly that the AIDS vaccine candidate offered no protection (e.g., reported at http://www.hivandhepatitis.com/vaccines/022503a.html). A phase 2b trial has now been proposed before phase 3. Here, between 1,000 and 2,000 high-risk volunteers are given placebo or vaccine and all are followed for evidence of infection. Once 30 trial participants are infected, a detailed analysis of the relationship between infection and immunity is made. In the case of AIDS, virus load, subtype and T cell and humoral immune responses are determined and correlated and the degree of protection ascertained. It is arguable that such an approach might have obtained a result for the Vaxgen trial in a shorter time at lower cost. It would be worthwhile to consider a similar strategy for tuberculosis vaccine efficacy trials.
Vaccine recipients for phase 1 trials are volunteers who are at negligible risk of infection. Nevertheless, they have to be counseled about the implications of testing, which adds some burden to all parties. It has proved relatively easy to recruit such volunteers in the UK and in Kenya and Uganda for AIDS vaccine testing. For efficacy trials, phase 2b and phase 3, it will be necessary to work with individuals with high risk for HIV infection. Sex-worker cohorts are usually too small and follow up can be difficult. In a high-risk region in Africa, the annual incidence may be 1–10%, but the implementation of trials inevitably raises awareness and the best possible advice must be given to volunteers, particularly concerning condom use. Therefore, it should be expected that incidence might decrease by half. This is important to realize in determining statistical powers before embarking on the trial. The population of high-risk volunteers is less well circumscribed for tuberculosis than for AIDS.
There are major ethical issues in efficacy trials. Double blinding and placebo controls are essential, but a difficult question is what to offer in terms of chemotherapy to trial participants in low-income countries such as Africa. It is now generally agreed that the best possible (rather than best regional) therapy should be offered to all trial participants who become infected; the unresolved questions are for how long and when, given that drugs may not be required for 5–10 years. Although it is desirable to insist on the highest safety standards for any vaccine candidate as defined by the FDA and the EMEA it may be worthwhile to carefully assess whether risk-benefit relationships differ for countries with low or high tuberculosis or AIDS prevalence. Side effects of new vaccine candidates may be tolerable for a vaccine that can prevent tuberculosis or AIDS mortality and morbidity in countries where incidences are skyrocketing, but not for countries with low tuberculosis or AIDS prevalence118.
HIV and tuberculosis vaccine trials will probably need multiple sites. A trial involving 2,000 volunteers with detailed prescreening, individual counseling and careful follow up will probably necessitate at least 20 sites. Although in theory such sites would have the infrastructure and could also conduct trials for both tuberculosis and HIV, it is unlikely that this would be possible at the same time because of high cost, a requirement for multiple vaccine groups and complicated data analysis.
Concluding remarks
AIDS and tuberculosis rampage most freely in low-income countries where the total annual budget for public health is below US $5 per capita119,120,121,122. Currently available therapeutic regimes exceed such budgets by several fold. Similarly, vaccine development from the bench to the field consumes huge amounts of financial resources. Consequently development of vaccines against tuberculosis and AIDS will be most successful as joint public-private enterprise with support from governmental and nongovernmental funding organizations and philanthropic foundations. Such a consortium would be best equipped to bring forward vaccine development by a combination of 'push' and 'pull' programs. Although support for preclinical research will be best directed by classical push programs, incentives should be made available for alternative approaches118. The removal of roadblocks serves as a good example for a support strategy emphasizing innovation and not restrictive in the experimental approach. Unconventional research areas, such as therapeutic HIV-1 and tuberculosis vaccination, could be further stimulated by pull programs rewarding a vaccine candidate that proves successful in preclinical studies. At the transition from the preclinical to the clinical phase, pull programs providing incentives for the market-ready final product would be most appropriate118. These include tax reduction for vaccine production, secured future markets in developing countries, a tiered price system, and reduced interest rates or debt release by the World Bank for vaccine purchase and distribution. In the absence of such incentives, even the best vaccine candidate may fail to reach the desired goal of unrestricted distribution in countries affected most by AIDS and tuberculosis.
Lack of financial incentive may provide some unique opportunities for vaccine development against AIDS and tuberculosis. Notably, low-to-absent competition for financial profits can promote comparative clinical trials under the umbrella of governmental, nongovernmental or philanthropic organizations either alone or together with the aim first to select the most promising candidates, and second to proceed by 'learning by doing' (i.e., continuous vaccine improvement of candidates in iterative clinical trial processes). Analysis of the immune responses of vaccine trial participants may provide new information that can be further explored in experimental animal models and help to define the next clinical trial step. Strong efforts are required to harmonize vaccine trials and accompanying vaccine efficacy testing. It is rewarding that several major organizations including the US National Institutes of Health though their intramural and extramural programs, the Bill and Melinda Gates Foundation through Aeras for tuberculosis and their Vaccine Enterprise for AIDS as well as the European Union through their European & Developing Countries Clinical Trials Partnerships program have committed themselves to bring vaccines against AIDS and tuberculosis from the bench to the field.
Vaccination strategies against these two diseases need to be integrated as soon as possible, considering the intimate interdependence of the two deadly pathogens and the consequences of their liaison. Obviously, numerous hurdles need to be overcome. Yet, even if only partially protective vaccines can be developed, return on investment will be enormous. This is not only true for the most impoverished countries, for which a rapid solution is vital, but also for industrialized countries, which may suffer significantly from global economic and social regressions and further weakening of unstable states.
References
World Health Organization. Global Tuberculosis Control: Surveillance, Planning, Financing (World Health Organization, Geneva, 2004).
Kaufmann, S.H.E. Is the development of a new tuberculosis vaccine possible? Nat. Med. 6, 955–960 (2000).
Calmette, A. Die Schutzimpfung gegen Tuberkulose mit “BCG” (F.C.W. Vogel, Leipzig, 1928).
Rosenberg, E.S. et al. Immune control of HIV-1 after early treatment of acute infection. Nature 407, 523–526 (2000).
Dybul, M., Fauci, A.S., Bartlett, J.G., Kaplan, J.E. & Pau, A.K. Guidelines for using antiretroviral agents among HIV-infected adults and adolescents. Ann. Intern. Med. 137, 381–433 (2002).
White, R.G. et al. Can Population Differences Explain the Contrasting Results of the Mwanza, Rakai, and Masaka HIV/Sexually Transmitted Disease Intervention Trials?: A Modeling Study. J. Acquir. Immune Defic. Syndr. 37, 1500–1513 (2004).
Kremer, L. & Besra, G.S. A waxy tale by Mycobacterium tuberculosis. in Tuberculosis and the Tubercle Bacillus (eds. Cole, S.T., Eisenach, K.D., McMurray, D.N. & Jacobs, W.R., Jr.) 287–305 (ASM Press, Washington, DC, 2005).
Chan, J., Silver, R.F., Kampmann, B. & Wallis, R.S. Intracelluar models of Mycobacterium tuberculosis infection. in Tuberculosis and the Tubercle Bacillus (eds. Cole, S.T., Eisenach, K.D., McMurray, D.N. & Jacobs, W.R., Jr.) 437–449 (ASM Press, Washington, DC, 2005).
Russell, D.G. Mycobacterium tuberculosis: the indigestible microbe. in Tuberculosis and the Tubercle Bacillus (eds. Cole, S.T., Eisenach, K.D., McMurray, D.N. & Jacobs, W.R., Jr.) 427–435 (ASM Press, Washington, DC, 2005).
Kaufmann, S.H.E. & Flynn, J.L. CD8 T cells in tuberculosis. in Tuberculosis and the Tubercle Bacillus (eds. Cole, S.T., Eisenach, K.D., McMurray, D.N. & Jacobs, W.R., Jr.) 465–474 (ASM Press, Washington, DC, 2005).
Dascher, C.C. & Brenner, M.B. CD1 and tuberculosis. in Tuberculosis and the Tubercle Bacillus (eds. Cole, S.T., Eisenach, K.D., McMurray, D.N. & Jacobs, W.R., Jr.) 475–487 (ASM Press, Washington, DC, 2005).
Kaufmann, S.H.E. gamma/delta and other unconventional T lymphocytes: What do they see and what do they do? Proc. Natl. Acad. Sci. USA 93, 2272–2279 (1996).
Shen, Y. et al. Adaptive immune response of V gamma 2V delta 2(+) T cells during mycobacterial infections. Science 295, 2255–2258 (2002).
Fischer, K. et al. Mycobacterial phosphatidylinositol mannoside is a natural antigen for CD1d-restricted T cells. Proc. Natl. Acad. Sci. USA 101, 10685–10690 (2004).
Ulrichs, T. et al. Human tuberculous granulomas induce peripheral lymphoid follicle-like structures to orchestrate local host defence in the lung. J. Pathol. 204, 217–228 (2004).
Kaufmann, S.H.E. How can immunology contribute to the control of tuberculosis? Nat. Rev. Immunol. 1, 20–30 (2001).
Cooper, A.M. et al. Disseminated tuberculosis in interferon gamma gene-disrupted mice. J. Exp. Med. 178, 2243–2247 (1993).
Flynn, J.L. et al. An essential role for interferon gamma in resistance to Mycobacterium tuberculosis infection. J. Exp. Med. 178, 2249–2254 (1993).
Maini, R. et al. Infliximab (chimeric anti-tumour necrosis factor alpha monoclonal antibody) versus placebo in rheumatoid arthritis patients receiving concomitant methotrexate: a randomised phase III trial. ATTRACT Study Group. Lancet 354, 1932–1939 (1999).
Chan, J. & Flynn, J. The immunological aspects of latency in tuberculosis. Clin. Immunol. 110, 2–12 (2004).
Boon, C. & Dick, T. Mycobacterium bovis BCG response regulator essential for hypoxic dormancy. J. Bacteriol. 184, 6760–6767 (2002).
Voskuil, M.I. et al. Inhibition of respiration by nitric oxide induces a Mycobacterium tuberculosis dormancy program. J. Exp. Med. 198, 705–713 (2003).
Sherman, D.R. et al. Regulation of the Mycobacterium tuberculosis hypoxic response gene encoding alpha -crystallin. Proc. Natl. Acad. Sci. USA 98, 7534–7539 (2001).
Bifani, P.J., Mathema, B., Kurepina, N.E. & Kreiswirth, B.N. Global dissemination of the Mycobacterium tuberculosis W-Beijing family strains. Trends Microbiol. 10, 45–52 (2002).
Glynn, J.R., Whiteley, J., Bifani, P.J., Kremer, K. & van Soolingen, D. Worldwide occurrence of Beijing/W strains of Mycobacterium tuberculosis: a systematic review. Emerg. Infect. Dis. 8, 843–849 (2002).
Naegeli, O. Ueber Häufigkeit, Localisation und Ausheilung der Tuberculose. Archiv für pathologische Anatomie und Physiologie und für klinische Medizin 160, 426–472 (1900).
Casanova, J.-L. & Abel, L. Genetic dissection of immunity to Mycobacteria: the human model. Annu. Rev. Immunol. 20, 581–620 (2002).
Cooke, G.S. & Hill, A.V. Genetics of susceptibility to human infectious disease. Nat. Rev. Genet. 2, 967–977 (2001).
Schaible, U.E. & Kaufmann, S.H. Iron and microbial infection. Nat. Rev. Microbiol. 2, 946–953 (2004).
Van Rie, A. et al. Exogenous reinfection as a cause of recurrent tuberculosis after curative treatment. N. Engl. J. Med. 341, 1174–1179 (1999).
Hingley-Wilson, S.M., Sambandamurthy, V.K. & Jacobs, W.R., Jr. Survival perspectives from the world's most successful pathogen, Mycobacterium tuberculosis. Nat. Immunol. 4, 949–955 (2003).
Fine, P.E.M. The BCG story - lessons from the past and implications for the future. Rev. Infect. Dis. 11, S353–S359 (1989).
Colditz, G.A. et al. Efficacy of BCG vaccine in the prevention of tuberculosis. Meta-analysis of the published literature. JAMA 271, 698–702 (1994).
Okkels, L.M., Doherty, T.M. & Andersen, P. Selecting the components for a safe and efficient tuberculosis subunit vaccine—recent progress and post-genomic insights. Curr. Pharm. Biotechnol. 4, 69–83 (2003).
Huygen, K. et al. Immunogenicity and protective efficacy of a tuberculosis DNA vaccine. Nat. Med. 2, 893–898 (1996).
Olsen, A.W., van Pinxteren, L.A.H., Okkels, L.M., Rasmussen, P.B. & Andersen, P. Protection of mice with a tuberculosis subunit vaccine based on a fusion protein of antigen 85B and ESAT-6. Infect. Immun. 69, 2773–2778 (2001).
Mollenkopf, H.J. et al. Application of mycobacterial proteomics to vaccine design: improved protection by Mycobacterium bovis BCG prime-Rv3407 DNA boost vaccination against tuberculosis. Infect. Immun. 72, 6471–6479 (2004).
Kaufmann, S.H.E. (ed.) Novel Vaccination Strategies (John Wiley & Sons, Weinheim, 2004).
O'Hagan, D.T. & Singh, M. Microparticles as vaccine adjuvants and delivery systems. in Novel Vaccination Strategies (ed. Kaufmann, S.H.E.) 147–172 (John Wiley & Sons, Weinheim, 2004).
McShane, H. et al. Recombinant modified vaccinia virus Ankara expressing antigen 85A boosts BCG-primed and naturally acquired antimycobacterial immunity in humans. Nat. Med. 10, 1240–1244 (2004).
McShane, H., Brookes, R., Gilbert, S.C. & Hill, A.V. Enhanced immunogenicity of CD4(+) t-cell responses and protective efficacy of a DNA-modified vaccinia virus Ankara prime-boost vaccination regimen for murine tuberculosis. Infect. Immun. 69, 681–686 (2001).
Skeiky, Y.A. et al. Differential immune responses and protective efficacy induced by components of a tuberculosis polyprotein vaccine, Mtb72F, delivered as naked DNA or recombinant protein. J. Immunol. 172, 7618–7628 (2004).
Brandt, L. et al. The protective effect of the Mycobacterium bovis BCG vaccine is increased by coadministration with the Mycobacterium tuberculosis 72-kilodalton fusion polyprotein Mtb72F in M. tuberculosis-infected guinea pigs. Infect. Immun. 72, 6622–6632 (2004).
Guleria, I. et al. Auxotrophic vaccines for tuberculosis. Nat. Med. 2, 334–337 (1996).
Smith, D.A., Parish, T., Stoker, N.G. & Bancroft, G.J. Characterization of auxotrophic mutants of Mycobacterium tuberculosis and their potential as vaccine candidates. Infect. Immun. 69, 1142–1150 (2001).
Perez, E. et al. An essential role for phoP in Mycobacterium tuberculosis virulence. Mol. Microbiol. 41, 179–187 (2001).
Cox, J.S., Chen, B., McNeil, M. & Jacobs, W.R. Complex lipid determine tissue specific replication of Mycobacterium tuberculosis in mice. Nature 402, 79–83 (1999).
McKinney, J.D. et al. Persistence of Mycobacterium tuberculosis in macrophages and mice requires the glyoxylate shunt enzyme isocitrate lyase. Nature 406, 735–738 (2000).
Pethe, K. et al. The heparin-binding haemagglutinin of M. tuberculosis is required for extrapulmonary dissemination. Nature 412, 190–194 (2001).
Hisert, K.B. et al. Identification of Mycobacterium tuberculosis counterimmune (cim) mutants in immunodeficient mice by differential screening. Infect. Immun. 72, 5315–5321 (2004).
Behr, M.A. et al. Comparative genomics of BCG vaccines by whole-genome DNA microarray. Science 284, 1520–1523 (1999).
Pym, A.S. et al. Recombinant BCG exporting ESAT-6 confers enhanced protection against tuberculosis. Nat. Med. 9, 533–539 (2003).
Horwitz, M.A., Harth, G., Dillon, B.J. & Maslesa-Galic, S. Recombinant bacillus Calmette-Guerin (BCG) vaccines expressing the Mycobacterium tuberculosis 30-kDa major secretory protein induce greater protective immunity against tuberculosis than conventional BCG vaccines in a highly susceptible animal model. Proc. Natl. Acad. Sci. USA 97, 13853–13858 (2000).
Murray, P.J., Aldovini, A. & Young, R.A. Manipulation and potentiation of antimycobacterial immunity using recombinant bacille Calmette-Guerin strains that secrete cytokines. Proc. Natl. Acad. Sci. USA 93, 934–939 (1996).
Wangoo, A. et al. Bacille Calmette-Guerin (BCG)-associated inflammation and fibrosis: modulation by recombinant BCG expressing interferon-gamma (IFN-gamma). Clin. Exp. Immunol. 119, 92–98 (2000).
Luo, Y., Chen, X., Han, R. & O'Donnell, M.A. Recombinant bacille Calmette-Guerin (BCG) expressing human interferon-alpha 2B demonstrates enhanced immunogenicity. Clin. Exp. Immunol. 123, 264–270 (2001).
Hess, J. et al. Mycobacterium bovis bacille Calmette-Guerin strains secreting listeriolysin of Listeria monocytogenes. Proc. Natl. Acad. Sci. USA 95, 5299–5304 (1998).
Portnoy, D.A., Chakraborty, T., Goebel, W. & Cossart, P. Molecular determinants of Listeria monocytogenes pathogenesis. Infect. Immun. 60, 1263–1267 (1992).
Kaufmann, S.H.E. & Nasser, A. Improved protection by recombinant BCG. Microbes Infect. (in the press).
Kamath, A.T. et al. New live mycobacterial vaccines: The Geneva consensus on essential steps towards clinical development. Vaccine in the press.
Markovic, I. & Clouse, K.A. Recent advances in understanding the molecular mechanisms of HIV-1 entry and fusion: revisiting current targets and considering new options for therapeutic intervention. Curr. HIV Res. 2, 223–234 (2004).
Simon, V. & Ho, D.D. HIV-1 dynamics in vivo: implications for therapy. Nat. Rev. Microbiol. 1, 181–190 (2003).
McMichael, A.J. & Phillips, R.E. Escape of human immunodeficiency virus from immune control. Annu. Rev. Immunol. 15, 271–296 (1997).
Younes, S.A. et al. HIV-1 viremia prevents the establishment of interleukin 2-producing HIV-specific memory CD4+ T cells endowed with proliferative capacity. J. Exp. Med. 198, 1909–1922 (2003).
Douek, D.C. et al. HIV preferentially infects HIV-specific CD4+ T cells. Nature 417, 95–98 (2002).
Blankson, J.N., Persaud, D. & Siliciano, R.F. The challenge of viral reservoirs in HIV-1 infection. Annu. Rev. Med. 53, 557–593 (2002).
Daniel, M.D., Kirchhoff, F., Czajak, S.C., Sehgal, P.K. & Desrosiers, R.C. Protective effects of a live attenuated SIV vaccine with a deletion in the nef gene. Science 258, 1938–1941 (1992).
Desrosiers, R.C. Prospects for an AIDS vaccine. Nat. Med. 10, 221–223 (2004).
Rowland-Jones, S.L. et al. Cytotoxic T cell responses to multiple conserved HIV epitopes in HIV-resistant prostitutes in Nairobi. J. Clin. Invest. 102, 1758–1765 (1998).
Kaul, R. et al. Late seroconversion in HIV-resistant Nairobi prostitutes despite pre-existing HIV-specific CD8+ responses. J. Clin. Invest. 107, 341–349 (2001).
Altfeld, M. et al. HIV-1 superinfection despite broad CD8+ T-cell responses containing replication of the primary virus. Nature 420, 434–439 (2002).
Korber, B. et al. Timing the ancestor of the HIV-1 pandemic strains. Science 288, 1789–1796 (2000).
Lee, J.K. et al. T cell cross-reactivity and conformational changes during TCR engagement. J. Exp. Med. 200, 1455–1466 (2004).
Altman, J.D. & Feinberg, M.B. HIV escape: there and back again. Nat. Med. 10, 229–230 (2004).
Derdeyn, C.A. et al. Envelope-constrained neutralization-sensitive HIV-1 after heterosexual transmission. Science 303, 2019–2022 (2004).
Goulder, P.J. & Watkins, D.I. HIV and SIV CTL escape: implications for vaccine design. Nat. Rev. Immunol. 4, 630–640 (2004).
Richman, D.D., Wrin, T., Little, S.J. & Petropoulos, C.J. Rapid evolution of the neutralizing antibody response to HIV type 1 infection. Proc. Natl. Acad. Sci. USA 100, 4144–4149 (2003).
Moore, C.B. et al. Evidence of HIV-1 adaptation to HLA-restricted immune responses at a population level. Science 296, 1439–1443 (2002).
Barouch, D.H. et al. Eventual AIDS vaccine failure in a rhesus monkey by viral escape from cytotoxic T lymphocytes. Nature 415, 335–339 (2002).
Friedrich, T.C. et al. Reversion of CTL escape-variant immunodeficiency viruses in vivo. Nat. Med. 10, 275–281 (2004).
Nishimura, Y. et al. Transfer of neutralizing IgG to macaques 6 h but not 24 h after SHIV infection confers sterilizing protection: implications for HIV-1 vaccine development. Proc. Natl. Acad. Sci. USA 100, 15131–15136 (2003).
Amara, R.R. et al. Control of a mucosal challenge and prevention of AIDS by a multiprotein DNA/MVA vaccine. Science 292, 69–74 (2001).
Barouch, D.H. et al. Control of viremia and prevention of clinical AIDS in rhesus monkeys by cytokine-augmented DNA vaccination. Science 290, 486–492 (2000).
Shiver, J.W. et al. Replication-incompetent adenoviral vaccine vector elicits effective anti-immunodeficiency-virus immunity. Nature 415, 331–335 (2002).
Alabi, A.S. et al. Plasma viral load, CD4 cell percentage, HLA and survival of HIV-1, HIV-2, and dually infected Gambian patients. AIDS 17, 1513–1520 (2003).
Burton, D.R. et al. HIV vaccine design and the neutralizing antibody problem. Nat. Immunol. 5, 233–236 (2004).
Wyatt, R. et al. The antigenic structure of the HIV gp120 envelope glycoprotein. Nature 393, 705–711 (1998).
Aldovini, A. & Young, R.A. Humoral and cell-mediated immune responses to live recombinant BCG-HIV vaccines. Nature 351, 479–482 (1991).
Liu, M.A. Vaccine developments. Nat. Med. 4, 515–519 (1998).
Sutter, G., Wyatt, L.S., Foley, P.L., Bennink, J.R. & Moss, B. A recombinant vector derived from the host range-restricted and highly attenuated MVA strain of vaccinia virus stimulates protective immunity in mice to influenza virus. Vaccine 12, 1032–1040 (1994).
Huang, X.L. et al. Priming of human immunodeficiency virus type 1 (HIV-1)-specific CD8+ T cell responses by dendritic cells loaded with HIV-1 proteins. J. Infect. Dis. 187, 315–319 (2003).
Nabel, G.J. HIV vaccine strategies. Vaccine 20, 1945–1947 (2002).
MacGregor, R.R., Boyer, J.D., Ciccarelli, R.B., Ginsberg, R.S. & Weiner, D.B. Safety and immune responses to a DNA-based human immunodeficiency virus (HIV) type I env/rev vaccine in HIV-infected recipients: follow-up data. J. Infect. Dis. 181, 406 (2000).
McConkey, S.J. et al. Enhanced T-cell immunogenicity of plasmid DNA vaccines boosted by recombinant modified vaccinia virus Ankara in humans. Nat. Med. 9, 729–735 (2003).
Paris, R. et al. HLA class I serotypes and cytotoxic T-lymphocyte responses among human immunodeficiency virus-1-uninfected Thai volunteers immunized with ALVAC-HIV in combination with monomeric gp120 or oligomeric gp160 protein boosting. Tissue Antigens 64, 251–256 (2004).
Hanke, T. et al. Enhancement of MHC class I-restricted peptide-specific T cell induction by a DNA prime/MVA boost vaccination regime. Vaccine 16, 439–445 (1998).
Schneider, J. et al. Enhanced immunogenicity for CD8+ T cell induction and complete protective efficacy of malaria DNA vaccination by boosting with modified vaccinia virus Ankara. Nat. Med. 4, 397–402 (1998).
Sun, J.C., Williams, M.A. & Bevan, M.J. CD4+ T cells are required for the maintenance, not programming, of memory CD8+ T cells after acute infection. Nat. Immunol. 5, 927–933 (2004).
Shedlock, D.J. & Shen, H. Requirement for CD4 T cell help in generating functional CD8 T cell memory. Science 300, 337–339 (2003).
Ridge, J.P., Di Rosa, F. & Matzinger, P. A conditioned dendritic cell can be a temporal bridge between a CD4+ T-helper and a T-killer cell. Nature 393, 474–478 (1998).
Liu, H., Andreansky, S., Diaz, G., Hogg, T. & Doherty, P.C. Reduced functional capacity of CD8+ T cells expanded by post-exposure vaccination of gamma-herpesvirus-infected CD4-deficient mice. J. Immunol. 168, 3477–3483 (2002).
Brewer, J.M., Conacher, M., Satoskar, A., Bluethmann, H. & Alexander, J. In interleukin-4-deficient mice, alum not only generates T helper 1 responses equivalent to freund's complete adjuvant, but continues to induce T helper 2 cytokine production. Eur. J. Immunol. 26, 2062–2066 (1996).
Norbury, C.C. et al. CD8+ T cell cross-priming via transfer of proteasome substrates. Science 304, 1318–1321 (2004).
Wolkers, M.C., Brouwenstijn, N., Bakker, A.H., Toebes, M. & Schumacher, T.N. Antigen bias in T cell cross-priming. Science 304, 1314–1317 (2004).
Beignon, A.S., Skoberne, M. & Bhardwaj, N. Type I interferons promote cross-priming: more functions for old cytokines. Nat. Immunol. 4, 939–941 (2003).
Le Bon, A. et al. Cross-priming of CD8+ T cells stimulated by virus-induced type I interferon. Nat. Immunol. 4, 1009–1015 (2003).
Liu, R. et al. Homozygous defect in HIV-1 coreceptor accounts for resistance of some multiply-exposed individuals to HIV-1 infection. Cell 86, 367–377 (1996).
Haase, A.T. The pathogenesis of sexual mucosal transmission and early stages of infection: obstacles and a narrow window of opportunity for prevention. AIDS 15 Suppl 1, S10–S11 (2001).
Brenchley, J.M. et al. CD4+ T cell depletion during all stages of HIV disease occurs predominantly in the gastrointestinal tract. J. Exp. Med. 200, 749–759 (2004).
Orme, I.M. & Izzo, A.A. in Tuberculosis and the Tubercle Bacillus (eds. Cole, S.T., Eisenach, K.D., McMurray, D.N. & Jacobs, W.R., Jr.) 561–571 (ASM Press, Washington, DC, 2005).
Pai, M., Riley, L.W. & Colford, J.M. Jr. Interferon-gamma assays in the immunodiagnosis of tuberculosis: a systematic review. Lancet Infect. Dis. 4, 761–776 (2004).
Stebbings, R.J. et al. Mechanisms of protection induced by attenuated simian immunodeficiency virus. Virology 296, 338–353 (2002).
McDermott, A.B. et al. Repeated low-dose mucosal simian immunodeficiency virus SIVmac239 challenge results in the same viral and immunological kinetics as high-dose challenge: a model for the evaluation of vaccine efficacy in nonhuman primates. J. Virol. 78, 3140–3144 (2004).
Hel, Z. et al. Viremia control following antiretroviral treatment and therapeutic immunization during primary SIV251 infection of macaques. Nat. Med. 6, 1140–1146 (2000).
Lu, W., Arraes, L.C., Ferreira, W.T. & Andrieu, J.M. Therapeutic dendritic-cell vaccine for chronic HIV-1 infection. Nat. Med. 10, 1359–1365 (2004).
Tryniszewska, E. et al. Vaccination of macaques with long-standing SIVmac251 infection lowers the viral set point after cessation of antiretroviral therapy. J. Immunol. 169, 5347–5357 (2002).
Ogg, G.S. et al. Decay kinetics of human immunodeficiency virus-specific effector cytotoxic T lymphocytes after combination antiretroviral therapy. J. Virol. 73, 797–800 (1999).
Kremer, M. & Glennerster, R. Strong Medicine: Creating Incentives For Pharmaceutical Research on Neglected Diseases (Princeton University Press, Princeton, Oxford, 2004).
World Health Organization. Global Atlas of infectious diseases. http://globalatlas.who.int/. (World Health Organization, Geneva, 2004).
UNAIDS. 2004 Report on the global AIDS epidemic. 2004. Geneva.
World Health Organization. The World Health Report 2004 - Changing History. 2004. Switzerland. (World Health Organization, Geneva, 2004).
Corbett, E.L. et al. HIV-1/AIDS and the control of other infectious diseases in Africa. Lancet 359, 2177–2187 (2002).
Temmerman, S. et al. Methylation-dependent T cell immunity to Mycobacterium tuberculosis heparin-binding hemagglutinin. Nat. Med. 10, 935–941 (2004).
Lowrie, D.B. et al. Therapy of tuberculosis in mice by DNA vaccination. Nature 400, 269–271 (1999).
Brooks, J.V., Frank, A.A., Keen, M.A., Bellisle, J.T. & Orme, I.M. Boosting vaccine for tuberculosis. Infect. Immun. 69, 2714–2717 (2001).
Acknowledgements
S.H.E. Kaufmann acknowledges financial support for his work on tuberculosis vaccination from: the Fonds Chemie, EU FP6 TB-VAC, EU FP6 MUVAPRED, Bundeministerium für Bildung und Forschung Competence Network “Structural Genomics of M. tuberculosis”, BMBF joint project “Genomics of M. tuberculosis”, EU project “X-TB”, Deutsche Forschungsgemeinschaft Priority Program “Novel Vaccination Strategies”. A.J. McMichael acknowledges grant support from the UK Medical Research Council and the International AIDS Vaccine Initiative. We thank A. von Gabain, J. Cohen, H. McShane, P. Andersen, T. Ottenhoff, M. Klein, T. Hanke and L. Castello-Branco for discussions, T. Walker and A. Ozin for reading this manuscript, D. Schad for graphical work and S. Sibaei for secretarial help.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Kaufmann, S., McMichael, A. Annulling a dangerous liaison: vaccination strategies against AIDS and tuberculosis. Nat Med 11 (Suppl 4), S33–S44 (2005). https://doi.org/10.1038/nm1221
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm1221
This article is cited by
-
Anti-tubercular activity evaluation of natural compounds by targeting Mycobacterium tuberculosis resuscitation promoting factor B inhibition: An in silico study
Molecular Diversity (2023)
-
Transcriptional response to the host cell environment of a multidrug-resistant Mycobacterium tuberculosis clonal outbreak Beijing strain reveals its pathogenic features
Scientific Reports (2021)
-
Depriving Iron Supply to the Virus Represents a Promising Adjuvant Therapeutic Against Viral Survival
Current Clinical Microbiology Reports (2020)
-
COVID-19 as part of the hyperferritinemic syndromes: the role of iron depletion therapy
Immunologic Research (2020)
-
The role of host miRNAs on Mycobacterium tuberculosis
ExRNA (2019)